Immunopathology Lecture 1 Mays Ibrahim Arab board of

Immunopathology Lecture 1 Mays Ibrahim, Arab board of pathology, CABP University of Al-Mustansiriyah, college of medicine


Immunity � Is defense against infectious pathogens, it accomplishes this by distinguishing self from nonself (exogenous or foreign) molecules. � Immunity classified into: 1. Innate immunity (natural, or native, immunity) 2. Adaptive immunity (acquired, or specific, immunity) � Any derangement in the regulatory mechanism leads to one of the followings: 1. Hypersensitivity and Autoimmune Disorders 2. Deficiency states, congenital or acquired 3. Amyloidosis, a disorder of extracellular protein accumulation

The immune system organs � Primary organs: ◦ Bone marrow- immune cell production, B cell maturation. ◦ Thymus-T cell maturation. � Secondary organs: ◦ Spleen, lymph nodes, tonsils, peyers patches- Allow immune cells to interact with antigens.

Innate immunity � Innate immunity It is the first line of non-specific defense that occur rapidly (minutes to hours) after exposure to antigen, and does not demonstrate immune memory. � � The components of innate immunity are: 1. 2. 3. � Epithelial barriers Phagocytic cells (neutrophils, macrophage), dendritic cells, natural killer (NK) cells. Several plasma proteins, including the proteins of the complement system. The two most important cellular reactions of innate immunity are: 1. 2. Inflammation Anti-viral defense, mediated by dendritic cells and NK cells. The cellular receptors of the innate immune cells that recognize the stimulus are called Toll-like receptors (TLRs). �
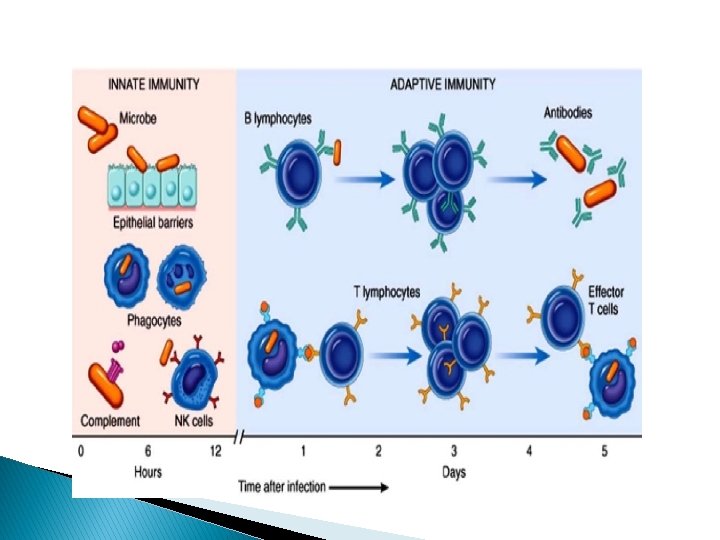

Adaptive immunity It is more powerful than innate immunity, activated by exposing to microbes that are not killed by innate immunity. � � Types of adaptive immune response Humoral immunity: mediated by antibodies produced by Blymphocyte; provide protection against extracellular microbes Cellular immunity: mediated by T-lymphocytes; provide protection against intracellular microbes � Component of adaptive immunity: Lymphocytes and their products
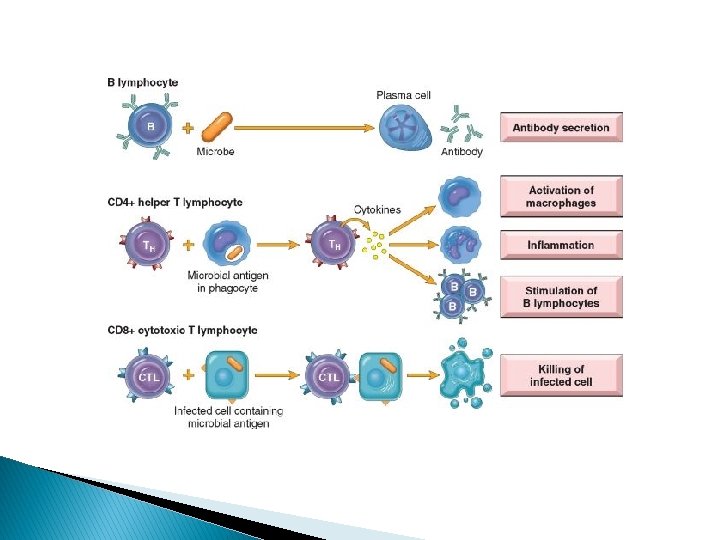

Cells of the immune system � Lymphocytes The three major types of lymphocytes, namely T, B and NK cells, account for 25% of peripheral blood leukocyte. Lymphocyte produced in B. M. → mature in B. M. to be B lymphocytes or → mature in thymus → T-Lymphocyte � Each Ag. T or B lymphocyte expresses receptor for single

T-lymphocytes 70% of lymphocytes in blood. Responsible for Cell mediated immunity. Each T cell has a specific T-cell receptor (TCR) that recognizes an antigen displayed by major histocompatibility complex (MHC) molecules on the surfaces of antigen-presenting cells (APCs). CD 3 present on all T cells surfaces CD 4 and CD 8 are co-receptors. T cells are either CD 4+or CD 8+ CD 4 attach to MHCII and CD 8 to MHC I (rule of 8). Normally CD 4: CD 8 ratio=2: 1 CD 4+ cells called helper cells I. Help the activation of immune cells by releasing T cells cytokines CD 8+ cells called cytotoxic cells: I. kills viral infected cells by inducing apoptosis II. Binds to MHC I, and release cytotoxic perforin and granzyme B
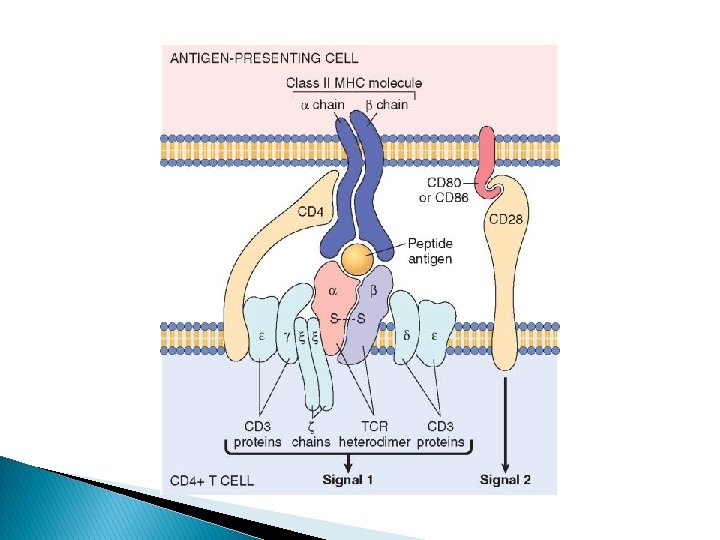

B-lymphocytes 10% to 20% of the circulating peripheral lymphocyte Humoral immunity. Present in lymph nodes, spleen, and mucosaassociated lymphoid tissues. Recognize antigen via the B-cell antigen receptor complex (Ig. M or Ig. D). B cells develop into plasma cells that secrete antibodies
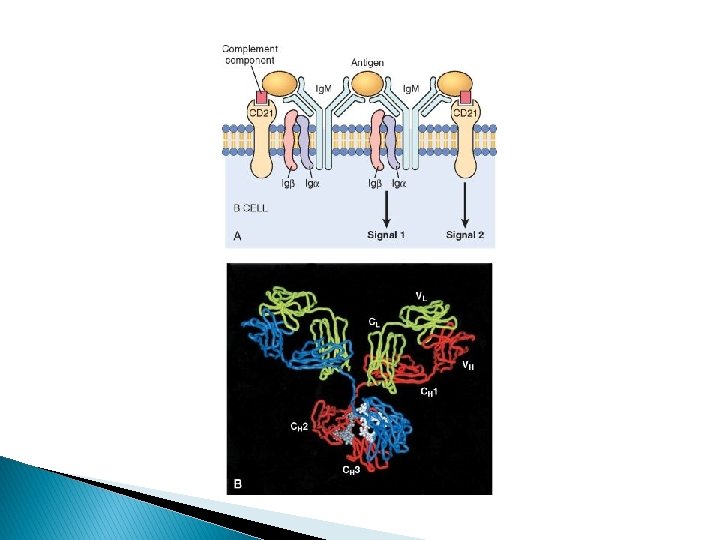

Natural killer cells Part of innate immunity Kills viral infected cells and tumor cells They have inhibitory receptor recognize MHC I Induced to kill when exposed to cell with absence of MHC I on target cell surface( viral infected cell, and stressed cell).

Antigen presenting cells � Are immune cells that specialized to capture Ags and display them to lymphocytes. Dendritic cells (like Langerhans cells in the epithelia) and macrophages Effector cells NK are first line of defense B lymph are humoral immunity T lymph both CD 4 and CD 8 are effector of cell mediated immunity Macrophages are effectors of both humoral immunity( through phagocytizing opsonized cells) and cell mediated immunity( through improving their ability to destroy phagocytized microbes in response to T helper cells signal).

Major Histocompatibility Complex (MHC) Molecules: Are glycoproteins found on the surface of the cells and arencoded by HLA gene Presents antigens to T cells and bind TCRs � Encoded by HLA A, B, C PRESENT ON ALL NUCLEATED CELLS. Function: present endogenous antigens (e. g. virus) to CD 8 cytotoxic T cells. � MHC class II ENCODED BY HLA DQ, DR PRESENT ON APC( DENDRITIC CELLS), MACRPHAGES AND B CELLS Function: present exogenously antigens (e. g. bacteria) to CD 4 helper T cells.

� NOTES: � The combination of HLA alleles in each individual is called the HLA haplotype. Any given individual inherits one set of HLA genes from each parent � Because of the polymorphism of the HLA loci, virtually innumerable combinations of molecules exist in the population � Polymorphism means that no two individuals (other than identical twins) are likely to express the same MHC molecules, � So the implication of HLA polymorphism is obvious in the context of transplantation, and therefore grafts exchanged between these individuals are recognized as foreign and attacked by the immune system. �

� HLA subtypes associated with diseases: examples � � 1. HLA-B 27: Psoriatic arthritis, Ankylosing spondylitis, IBD associated atrthritis, Reactive arthritis. (PAIR) 2. DQ 2/DQ 8: Celiac disease.

Hypersensitivity reaction � Reactions imply an excessive response to an antigenic stimulus.

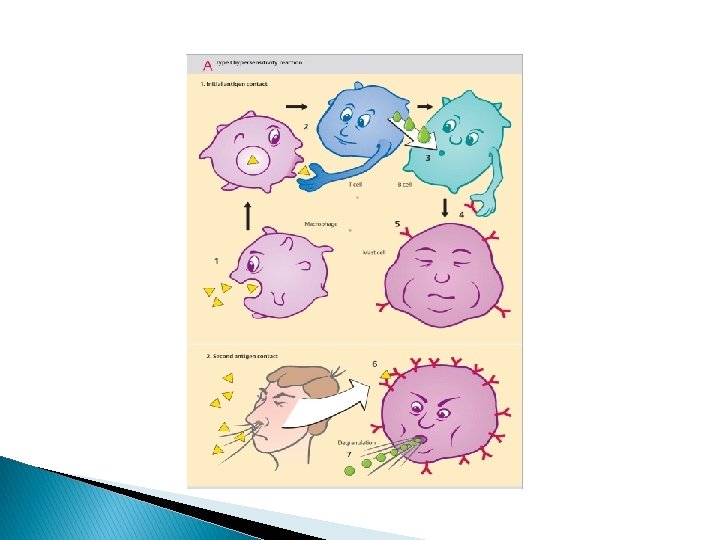
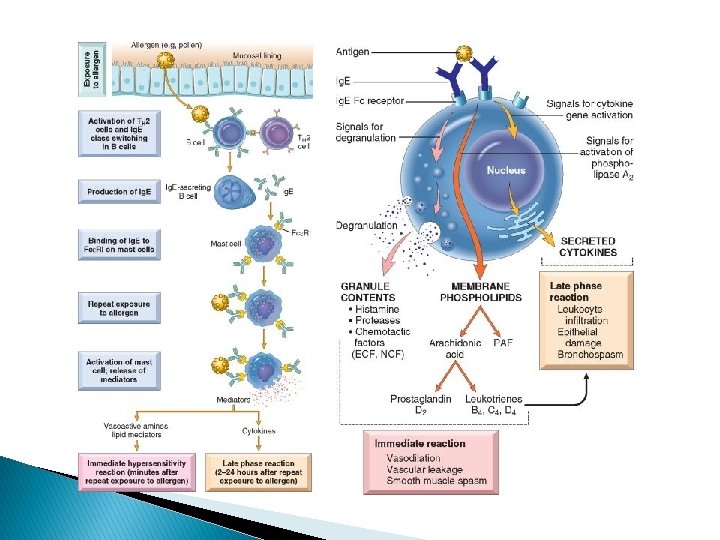
Type I hypersensitivity reaction: Definition: hypersensitivity reaction characterized by Ig. E related release of chemical mediators from mast cells and basophils. The release is triggered by exposure to an Ag. Require prior sensitization to Ag Require cross linking of Ig. E Fc receptor on the surface of mast cells and basophils Release of chemical mediators 1. 2. 3. 4. Histamine Eosinophil chemotactic factor LB 4 (neutrophil chemotactic). PAF Immediate phase: Reaction develops rapidly after Ag exposure because of preformed antibodies. Delayed phase: result from mast cells and basophils releasing cytokines that induce cellular inflammation. Effects may be localized or systemic 1. Systemic: anaphylaxis(e. g: bee sting and drugs) 2. Localized: food allergies, atopy, and asthma.

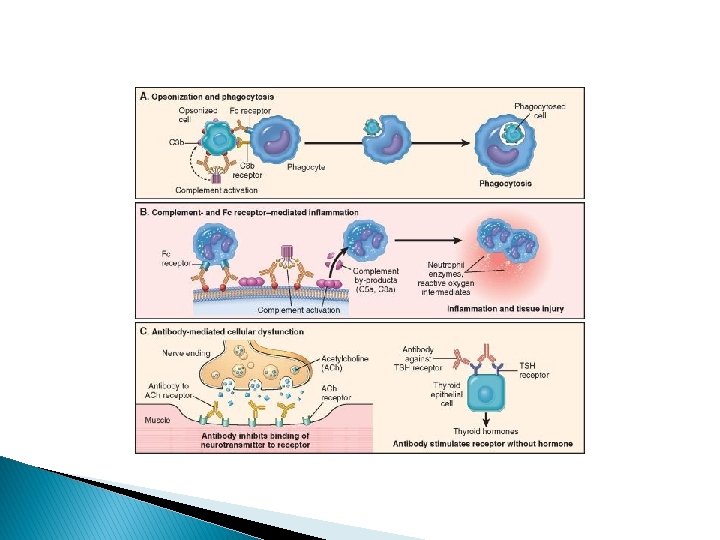
Type II hypersensitivity (cytotoxic type) Definition: hypersensitivity reaction characterized by production of an Ig. G or Ig. M antibody directed against a specific target cell or tissue. Complement dependent cytotoxicity 1. Fixation of complement results in osmotic lysis or opsonization of antibody coated cells 2. Example: autoimmune hemolytic anemia Antibody dependent cell mediated cytotoxicity 1. Cytotoxic killing of an antibody coated cell (opsonizes) 2. Example: Goodpasture's syndrome Anti-receptor antibodies: 1. Antibodies activate or interfere with receptors 2. Example: Graves disrease

Thank you for your attention
- Slides: 25