Immunopathology lec 2 By Dr Mays Ibrahim Types

Immunopathology lec 2 By Dr. Mays Ibrahim

Types of hypersensitivity reactions � hypersensitivity type I � hypersensitivity typre III � hypersensitivity typre IV

Type III hypersensitivity (immune complex disease) Definition: hypersensitivity reaction characterized by the formation of in-situ or circulating antibody-antigen immune complexes, which deposit in tissue resulting in complement activation, inflammation and tissue injury. Examples: Serum sickness Systemic lupus erythematosus(SLE) Glomerulonephritis
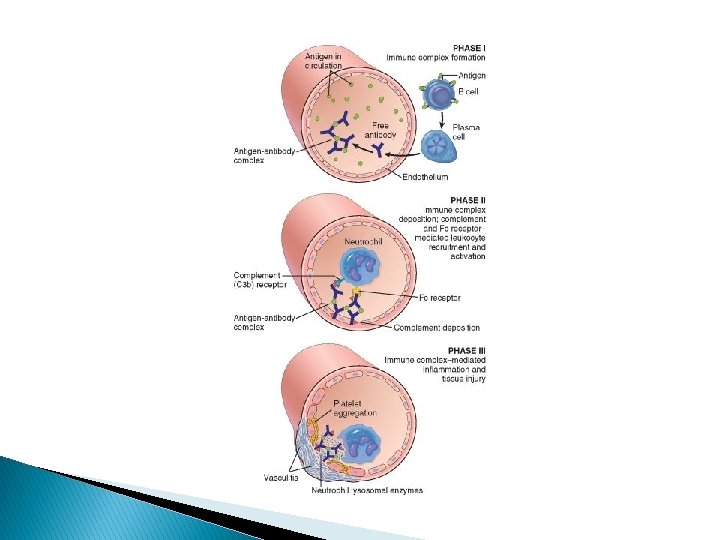

Type IV hypersensitivity (cell mediated type) Definition: hypersensitivity reaction mediated by sensitized T lymphocyte Delayed type hypersensitivity CD 4+ T-cell lymphocyte mediated granuloma formation Cytotoxic T cell mediated CD 8+ T cell lymphocyte destroy antigen-containing cells • Examples � PPD skin test and tuberculosis � Viral infections, immune reaction to tumors, contact dermatitis, type 1 diabetes
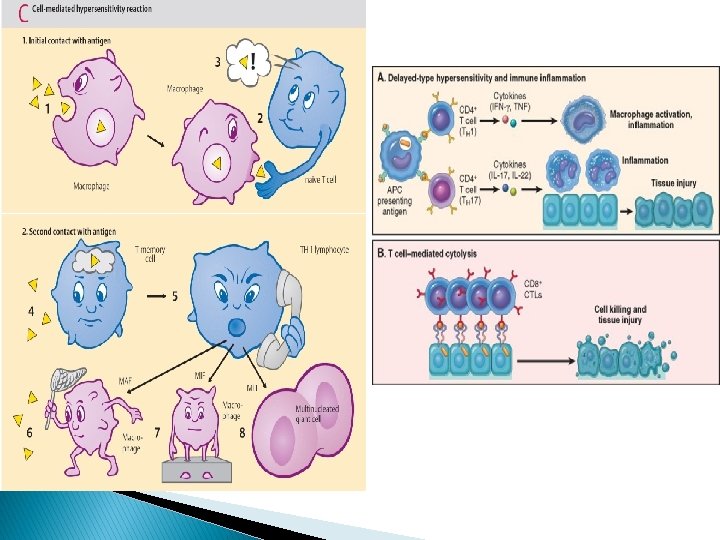

Autoimmune disease: � is an immune reaction to self-antigens result from loss of self-tolerance. � Self-tolerance: is the normal state of non-responsiveness to one’s own antigens. � The mechanisms of self-tolerance can be either central or peripheral: I. Central Tolerance: This refers to the process by which T and B cells that recognize self antigens are either killed (negative selection) or rendered harmless. Negative selection: T cell expressing TCR with high affinity for self-antigens undergo apoptosis. This happens in the thymic medulla. Peripheral Tolerance Auto-reactive cells that escape central regulatory mechanisms can be removed or inactivated in the periphery through Anergy: is irreversible functional inactivation of T cells when they recognize self-antigen

Autoimmune diseases: Systemic lupus erythematosus (SLE): Definition: chronic systemic autoimmune disease characterized by loss of self tolerance and production of autoantibodies. Epidemiology: Female more than male Age 20 -45 I. II. III. Types of Autoantibodies present: Antinuclear antibody(ANA) (more than 95%) Anti-ds. DNA (40 -60%) Anti-Sm(20 -30%) Mechanism of injury: type II and III hypersensitivity reactions � Cell injury (e. g. , UV light and other environmental insults) leads to apoptosis and an increased burden of nuclear antigens. � Defective B and T-cell tolerance leads to autoantibodies directed against the nuclear antigens, with the resulting immune complexes being ingested by B cells and dendritic cells; subsequent TLR engagement causes further cellular activation, cytokine production, and augmented autoantibody synthesis, which causes more apoptosis in a self-amplifying loop.

Distribution of the disease: I. II. III. IV. hematologic I. Hemolytic anemia II. Thrombocytopenia III. Neutropenia IV. Lymphopenia Arthritis: polyarthralgia and synovitis without joint deformity. Skin: I. II. Malar “butterfly” rash, sunlight exacerbates the lesions Maculopapular rash I. glomerulonephritis I. Libman sacks endocarditis(no bacterial endocarditis): numerous small, warty vegetations (1 to 3 mm) on the inflow or outflow surfaces (or both) of the mitral and tricuspid valves Kidney diseases: Heart Serosal surfaces: pericarditis, pleuritis, and pleural effusions VI. CNS: focal neurologic symptoms, seizure, and psychosis. Treatment: steroid and immunosuppressive agents. Prognosis: V. I. Chronic unpredictable course with remission and relapse. II. Death is frequently due to renal failure and infectioins


Sjo"gren Syndrome Definition: autoimmune disorder characterized by destruction of the lacrimal and salivary glands resulting in inability to produce tears and saliva. Epidemiology: I. Female more than male II. age range 30 -50 Clinical features: dry eyes-keratoconjunctivitis sicca dry mouth-xerostomia mikulicz syndrome: enlargement of the salivary and lacrimal glands often associated with rheumatoid arthritis and other autoimmune disease anti-ribonucleoprotein antibodies I. III. I. SS-A(Ro) II. SS-B(La) Complication: increased risk of developing lymphoma.

Scleroderma(progressive systemic sclerosis) Definition: autoimmune disease characterized by triad of autoimmunity, non-inflammatory vasculopathy and collagen deposition with fibrosis(fibroblast stimulation and deposition of collagen in the skin and internal organs) Female more than male Age range 20 -55 Pathogenesis: Vascular damage: microvascular injury is the hallmark of the systemic sclerosis it is thought to be due to chronic perivascular fibrosis or by direct autoimmune attack. The end process of repeated injuries lead to vascular lumen narrowing. activation of fibroblast by cytokines, interleukin-1(IL-1), platelet derived growth factor(PDGF), and /or fibroblast growth factor(FGF) leads to fibrosis.
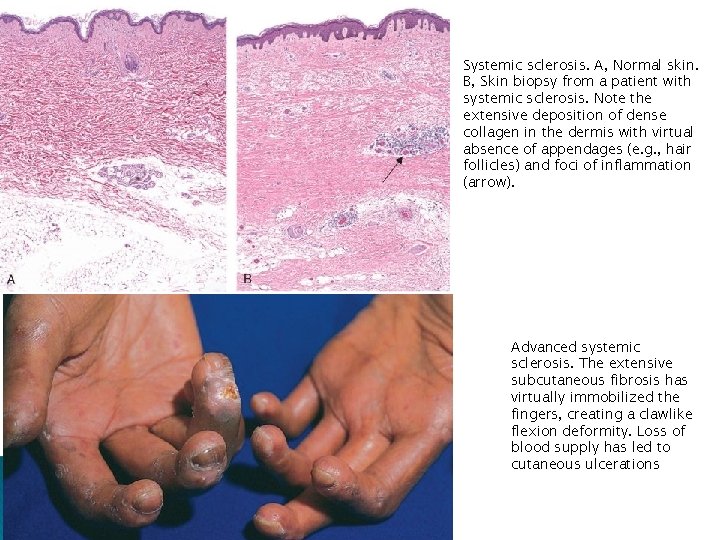
Systemic sclerosis. A, Normal skin. B, Skin biopsy from a patient with systemic sclerosis. Note the extensive deposition of dense collagen in the dermis with virtual absence of appendages (e. g. , hair follicles) and foci of inflammation (arrow). Advanced systemic sclerosis. The extensive subcutaneous fibrosis has virtually immobilized the fingers, creating a clawlike flexion deformity. Loss of blood supply has led to cutaneous ulcerations

� IT IS OF TWO TYPES Diffuse scleroderma: characterized by Anti-DNA topoisomerase I antibodies(Scl-70) 70% Widespread skin involovement of Early involvement of visceral organs a) b) c) Esophagus-dysphagia GI tract- malabsorption Pulmonary fibrosis-dyspnea on exertion Cardiac fibrosis-arrythmias Kidney fibrosis-renal insufficiency Localized scleroderma: characterized by Anti-centromere antibodies Limited Skin involvement of the face and hand Late involovement of visceral organs Relatively benign clinical course Can ssociate with -CREST syndrome: Calcinosis, Raynaud phenomenon, Esophageal dysmotility, Sclerodatyly, Telangiectasia

Rheumatoid arthritis (RA) Is a chronic autoimmune inflammatory disease that affects mainly the joints, especially small joints (digits before wrist, ankles, elbows, and knees) in a bilaterally symmetric pattern), but can affect multiple tissues (blood vessels, skin, heart, lungs, and muscles). RA is caused by an autoimmune response against self-antigen(s), which leads to T cell reactions in the joint with production of cytokines that activate phagocytes that damage tissues and stimulate proliferation of synovial cells (synovitis). Antibodies may also contribute to the disease. About 80% of patients have serum immunoglobulin M (Ig. M) (and, less frequently, Ig. A) autoantibodies that bind to the Fc portions of their own (self ) Ig. G. � These autoantibodies are called rheumatoid factor. They may form immune complexes with self-Ig. G that deposit in joints and other tissues, leading to inflammation and tissue damage
- Slides: 15