Immunodeficiencies Martin Lika Basic immunological terms Immune system

Immunodeficiencies Martin Liška
Basic immunological terms Immune system provides 3 basic functions: a) Defense against infection b) Homeostasis – elimination of old or impaired cells c) Immunological surveillance - elimination of mutated cells Endocrine system Immune system Nervous system Disorders – detectable by laboratory or histological methods, without clinical manifestation Clinical manifestation – decreased function - immunodeficiencies - increased function – allergy, autoimmunity

Immunodeficiencies • Humoral – innate immunity - complement, MBL acquired immunity – immunoglobulins (B lymphocytes) • Cell mediated immunity – innate immunity – phagocytes - acquired immunity – T lymphocytes • Primary – congenital, genetically defined, symptoms predominantly at an early age • Secondary – the onset of symptoms at any age chronic diseases the effects of irradiation immunosuppression surgery, injuries stress

Immunodeficiencies – critical life periods in respect to symptoms onset • Newborn age - severe primary disorders of cell mediated immunity • 6 mth. – 2 yrs. – severe humoral immunodeficiencies cong. /transient • 3 - 5 yrs. – transient and selective humoral immunodeficiencies, secondary immunodeficiencies • 15 – 20 yrs. – hormonal instability, thymus involution, life-style changes, some typical infections first symptoms of CVID • Middleage – often excessive workload, stress first symptoms of autoimmune disorders (also immunodeficiency) • Advanced and old age – rather symptoms of severe secondary immunodeficiencies, repercussion of functional disorders

Immunodeficiencies – major clinical features • Antibodies - microbial infections (encapsulated bacterias) respiratory - pneumonia, sinusitis, otitis GIT – diarrhea • Complement – microbial infections (pyogenic), sepsis various systems affection edema (HAE) – C 1 -INH deficiency • T lymphocytes - bacterial, fungal, viral GIT – diarrhoea respiratory – pneumonia, sinusitis • Phagocytes - abscesses, recurrent purulent skin infections granulomatous inflammations
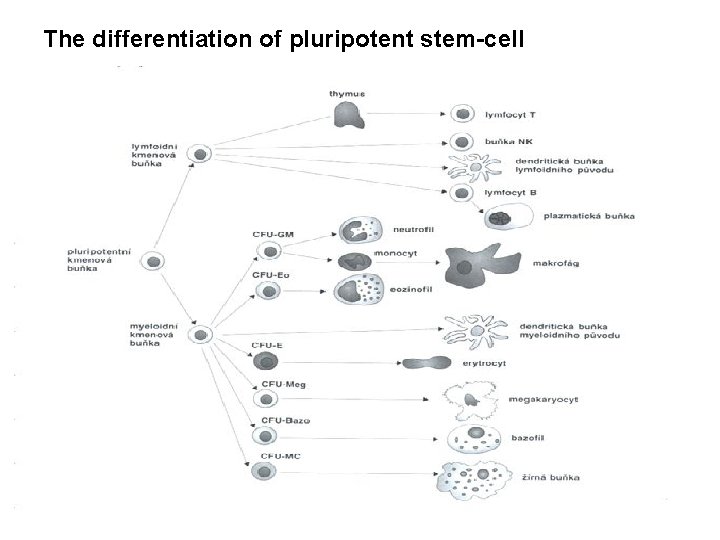
The differentiation of pluripotent stem-cell

I. Primary immunodeficiencies – phagocytic cell defects 1/ Quantitative – decreased numbers of granulocytes – neutrophil elastase mutation Congenital chronic agranulocytosis Cyclic agranulocytosis (neutropenia) • Systemic manifestation, fevers in 3 -weeks cycles in cyclic form • Treatment with granulocyte growth factors, ATB

I. Primary immunodeficiencies – phagocytic cell defects 2/ Qualitative – phagocytes functional disorders, various enzyme deficits, inability of phagocytes to degrade the ingested material Chronic Granulomatous Disease (CGD) • Approximately in 60% X-linked • Enzymatic inability to generate toxic oxygen metabolites (H 2 O 2) during oxygen consumption) - result of defect in neutrophilic cytochrome b (part of complex containing NADPH oxidase) • Inability to kill bacteria such as Staph. aureus, Pseud. aeruginosa that produce the enzyme catalase • Clinical features: granulomas in many organs • Treatment: long-term ATB administration • Myeloperoxidase deficiency • Recurrent microbial infections, susceptibility to Candida albicans and Staph. aureus infections

I. Primary immunodeficiencies – phagocytic cell defects Chédiak-Higashi syndrome • Clinical features: recurrent, severe, pyogenic infections (streptococcal, staphylococcal) • Defective intracellular killing of bacteria (neutrophils contain abnormal giant lysosomes Hyper. Ig. E (Job’s) syndrome • Mutation of STAT 3 gene • Recurrent “cold” staphylococcal abscesses, chronic eczema, otitis media • Extremely high serum Ig. E levels • Treatment: ATB LAD syndrome – Leukocyte Adhesion Deficiency (neutrophil adhesion molecules deficiency) • LAD I – integrins expression deficiency • LAD II – selectins expression deficiency

II. Primary immunodeficiencies – B cell disorders • • • Bruton’s X-linked hypogamaglobulinemia Blockage in the maturation of pre-B lymphocytes into B lymphocytes (tyrosine kinase defect) Frequency 1: 50 -100 thousands Undetectable or very low serum levels of Ig Clinical symptoms in 5 -9 mth. of age Pneumonia, pyogenic otitis, complicated sinusitis, increased occurrence of pulmonary fibrosis Treatment: life-long IVIG substitution CVID – Common Variable Immuno. Deficiency B cell functional disorder, mostly low levels of Ig. G and Ig. A Frequency 1: 100 -200 thousands. Symptoms’ onset between 2 nd and 3 rd decade Recurrent respiratory tract infections (pneumonia) Treatment: IVIG substitution

II. Primary immunodeficiencies – B cell disorders • • • Selective Ig. A deficiency Disorder of B cell function Frequency 1: 500 -700, manifestation mostly at pre-school age Recurrent mild/moderate infections (respiratory, GIT, urinary tract) or asymptomatic Risk of reaction to live attenuated vaccines or generation of anti-Ig. A antibodies after a blood transfusion Laboratory criterion: Ig. A < 0, 07 g/l (age > 4 years) Selective Ig. G subclasses or specific Ig. G deficiency • B cell function disorder • Frequency ? • Onset of symptoms in childhood, mostly respiratory tract infections caused by encapsulated bacteria (H. influenzae, Pneumococci) Transient hypogammaglobulinemia of infancy

III. Primary immunodeficiencies – T cell disorders di. George syndrome • Disorder of prethymocytes maturation due to absence of thymus • Disorder of development of 3 rd and 4 th branchial pouch – absence of parathyroid glands • Congenital heart diseases • Frequency 1 : 100 thousands • The onset of symptoms after the birth – hypocalcemic spasms and manifestations of cong. heart disease • Immunodeficiency could be only mild, the numbers of T lymphocytes later usually become normal • Treatment symptomatic

III. Primary immunodeficiencies – T cell disorders Lymphoproliferative syndrome • Malignant proliferation of activated T lymphocytes • Hypogamaglobulinaemia, lymphoma • Its development is induced by EBV infection Chronic mucocutaneous candidiasis • Impaired ability of T cells to produce macrophage migration inhibiting factor (MIF) in response to Candida antigen Bare lymphocyte sy. • Disorder of antigen presentation – defect of MHC I and/or MHC II expression leads to the dysfunction of CD 4 and CD 8 lymphocytes IFN-g Receptor deficiency • Th 1 lymphocytes differentiation disorder inability of intracellular killing of Mycobacteria (fatal BCG itis)
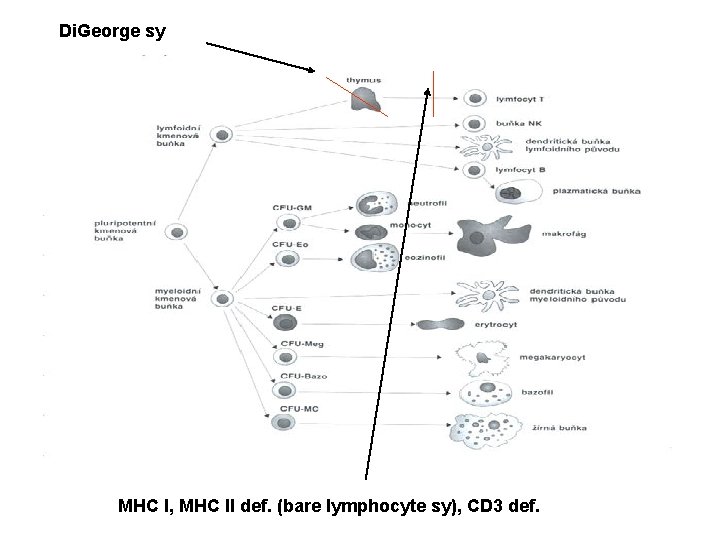
Di. George sy MHC I, MHC II def. (bare lymphocyte sy), CD 3 def.

IV. Primary immunodeficiencies – combined defects of T and B cells • SCID – Severe Combined Immuno. Deficiency • X-linked recessive or AR disease, combined disorder of humoral and cell mediated immunity • Severe disorder (patients often die during first 2 years of life), symptoms’ onset soon after the birth (severe diarrhoea, pneumonia, meningitis, BCGitis) • Immunological features: typically lymphopenia and thymus hypoplasia • Forms: AR form – often enzymatic deficiency (ADA, PNP) that leads to accumulation of metabolites toxic to DNA synthesis (lymphocytes) X-linked form – disorder of stem-cell Treatment: ATB, IVIG BMT is of critical significance in ADA deficiency the gene therapy was tested successfully • Reticular dysgenesis • • Stem-cell differentiation is blocked Very rare Symptoms immediately after the birth – severe diarrhoea, infections of deep layers Fatal, BMT is the only treatment
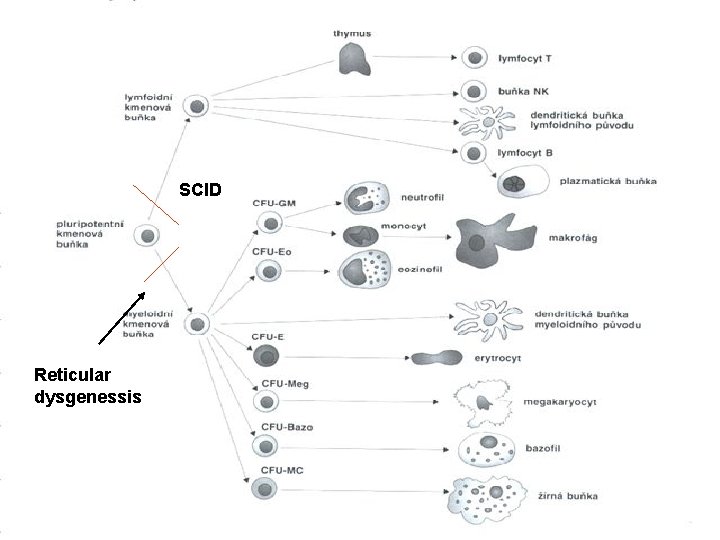
SCID Reticular dysgenessis

IV. Primary immunodeficiencies – combined defects of T and B cells Ataxia teleangiectasia • Increased radiation induced chromosomal breakage, ataxia, dilatation of small blood vessels (teleangiectasia) • Neurological disorders, immunodeficiency is not necessary (if present, Ig. A deficiency or T lymphocytes function disorders are most common) • Treatment: ATB, IVIG Hyper Ig. M syndrome • CD 40 L expression disorder, poor cooperation of B and T cells, impaired isotype switching, increased Ig. M levels Wiskott-Aldrich syndrome • thrombocytopenia, eczema, recurrent infections (encapsulated microbes), decreased Ig. M levels
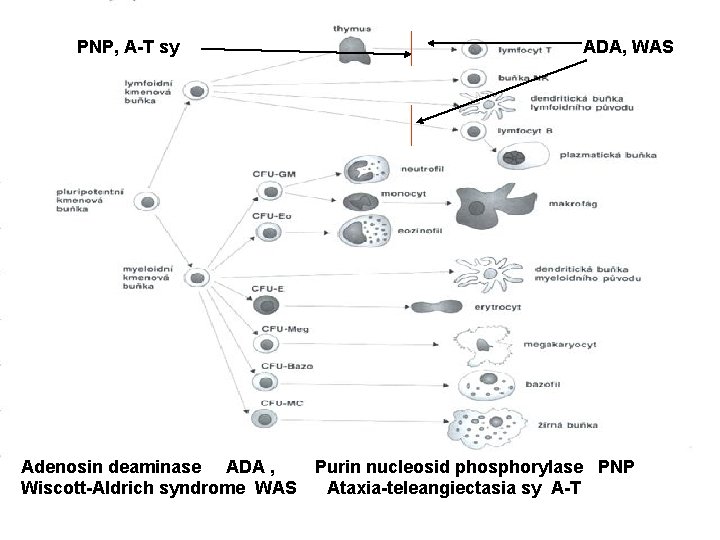
PNP, A-T sy Adenosin deaminase ADA , Wiscott-Aldrich syndrome WAS ADA, WAS Purin nucleosid phosphorylase PNP Ataxia-teleangiectasia sy A-T

V. Primary immunodeficiencies – complement system disorders Deficiency of: • C 1, C 2, C 3, C 4 – impaired opsonization, susceptibility to infections, autoimunity, SLE–like syndrome • C 6, C 7, C 8, C 9 – SLE–like syndrome, increased susceptibility to neisserial infections • MBL deficiency – mannan binding lectin (lectin way of complement activation), various infections, susceptibility to autoimmunity, association with allergy.

V. Primary immunodeficiencies – complement system disorders Hereditary angioedema (HAE) • Absence or functional deficiency of C 1 -inhibitor • Anaphylactoid reactions with skin and/or mucosal (oral, laryngeal, gut) edemas caused by overproduced bradykinin • Injuries or surgical/stomatological operations are mostly the triggering factor • Laryngeal edemas could be life-threatening, immediate treatment is necessary ! • Treatment: preventive – androgens, EACA immediate – C 1 -INH concentrate or fresh frozen plasma administration, icatibant • Secondary forms also exist !

Secondary immunodeficiencies • Acute and chronic viral infections – infectious mononucleosis, influenza • Metabolic disorders – diabetes mellitus, uremia • Autoimmune diseases – autoantibodies against immunocompetent cells (neutrophils, lymphocytes); autoimmune phenomena also after administration of certain drugs (e. g. oxacilin, quinidine) • Allergic diseases • Chronic GIT diseases • Malignant diseases (leukemia) • Hypersplenism/asplenia • Burn, postoperative status, injuries • Severe nutritional disorders • Chronic infections • Ionizing radiation • Drug induced immunodeficiencies (chemotherapy) • Immunosupression • Chronic stress • Chronic exposure to harmful chemical substances

Secondary immunodeficiencies • Splenectomy – deficiency in generation of antibodies against encapsulated microorganisms (Pneumococci, Neisseria) • A loss of immunoglobulins – nephrotic syndrome - lymphangiectasies • Lymphomas, myelomas, CLL • Chronic fatigue syndrome • First, it is necessary to exclude all chronic diseases which can lead to fatigue: • autoimunity • malignancy • focal infection • neurological disorders • metabolic disorders • depression

Secondary immunodeficiencies - A. I. D. S. • Caused by retrovirus HIV 1 or HIV 2 • Current incidence 40 mil. people, predominantly in central Africa, 5 mil. of new infections per year, 3 mil. deaths per year • CZ: 10/06 - HIV+ 904/248, AIDS 204/14, deaths 23/2 • Virus has a tropism for cells bearing CD 4 surface marker (Th CD 4+ lymphocytes); also affects macrophages and CNS cells • Viral genome transcribes into human DNA and infected cell provides viral replication • Transmission: sexual intercourse contact with blood endouterine (mother – fetus, breast milk) • Phases: acute (flu-like sy) asymptomatic – several years, viral replication symptomatic – infections, autoimmunity, malignancy, allergy final – systemic breakdown, opportune infections

A. I. D. S. - Treatment • Reverse transcriptase inhibitors (zidovudine, dideoxyinosine, dideoxycytosine, 3 -thiacytosine) • Protease inhibitors - block the viral protease enzyme • Combined drug therapy • Antimicrobial agents

Substitution therapy with immunoglobulins • Prepared by fractionation of pooled human plasma from huge amount of donors (1000) • Examination of donors, inactivating procedures to minimize the risk of infection transmission • Mainly Ig. G, minimal content of Ig. A • i. v. (Octagam, Gammagard) or s. c. use (Subcuvia, Gammanorm)

Indications • Primary humoral immunodeficiencies • Ig. G subclasses deficiencies, deficiencies of generation of specific antibodies, secondary humoral immunodeficiencies, combined immunodeficiencies

Dosage • agamaglobulinemia – IVIG 400 -600 mg/kg/month • regular substitution in outpatient’s room every 3 -4 weeks • „home therapy“ (s. c. administration by infusion pump)

Adverse effects • Allergic reactions, or even anaphylaxis [in minor reactions (chill, headache) only slowing down of infusion is usually needed]
- Slides: 28