Immunity General Physiology Tony Serino Ph D Biology
Immunity General Physiology Tony Serino, Ph. D. Biology Department Misericordia University

Immune System • Provide defense of the body against infectious agents, toxins, foreign bodies, and cancers • Two types of defenses: – General (Non-specific or Innate) Defense • • Barriers Normal Flora and Fauna Fever Surveillance Inflammation Non-specific Phagocytic WBCs and NK cells Protective Chemicals – Specific (Adaptive) Defense --Lymphocytes

Barriers • Prevent infectious agents from penetrating internal environment – Epithelium ( thickness, tight junctions, keratin) -especially the skin – Cilia and mucus – Watery secretions (tears, saliva) – Acidity (stomach, urine, vaginal secretions) • Normal Flora and Fauna –resident bacteria prevent infectious agents from growing on body surfaces

Fever • Rise in Body Temperature – Inhibits invading cell growth; increase body metabolism to increase defense/repair cell activity – Produced by release of pyrogens from leukocytes – Low grade fever is beneficial in fighting infection, high sustained fever may be life threatening

Surveillance • Number of cells and organs to detect invading agents • Langerhans cells of skin, Mast cells, Dendritic cells, and organs like: Tonsils, GALT cells • Gather antigens and present them to lymphocytes

Inflammation • Allows more blood defenses into damaged areas • Triggered by release of paracrines from damaged tissues (PG), attacking WBCs (cytokines), mast cells (heparin and histamine), and activation of blood protective chemicals (complement and bradykinins) • Increases: – blood flow through vasodilation (hyperemia) – capillary permeability – Both lead to local edema • If prolonged or systemic, can become life threatening
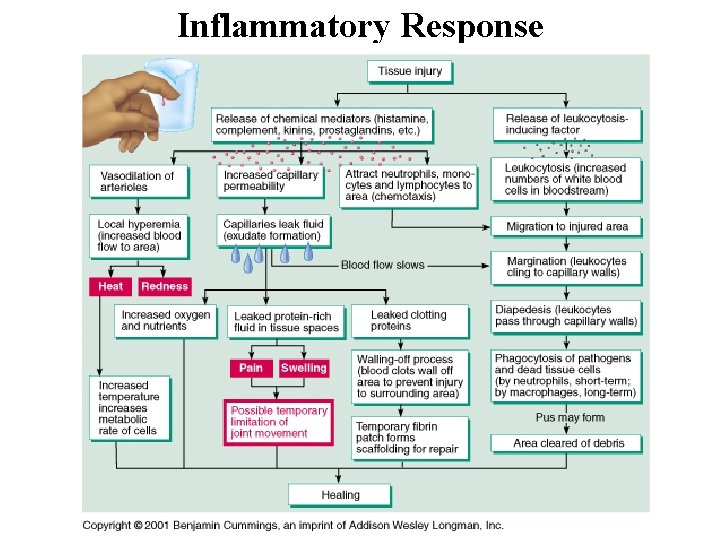
Inflammatory Response

Phagocytic WBC and NK cells • WBCs can distinguish the sugars in mammalian cells and those found on bacteria or other parasites – PMNs, macrophage, and mast cells can injure or destroy cells that do not display normal sugars • NK cells –related to T-cells but attack any cell not displaying MHC I proteins – Kill by secreting perforins and other chemicals

Fig. 18. 03
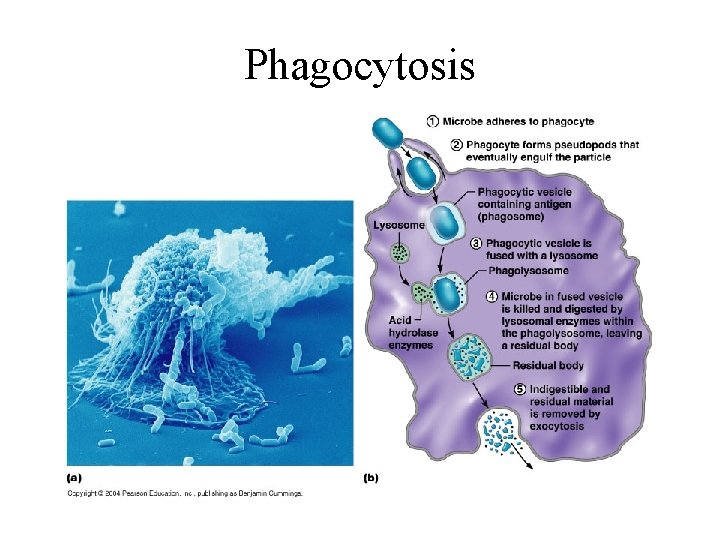
Phagocytosis
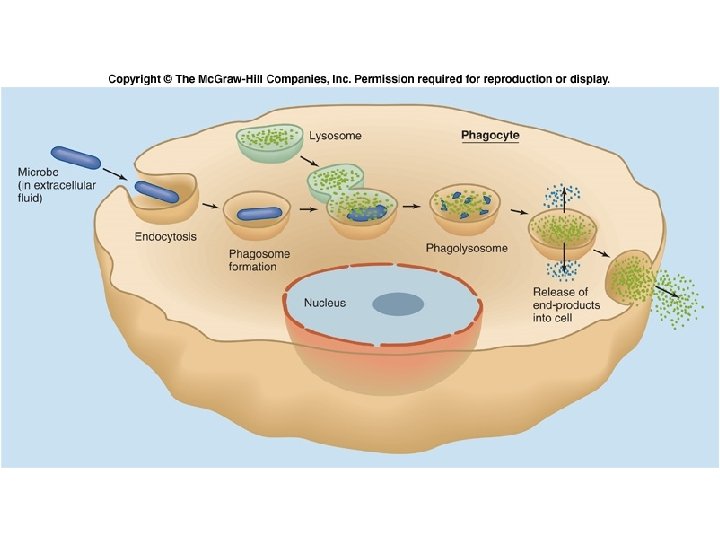
Fig. 18. 02
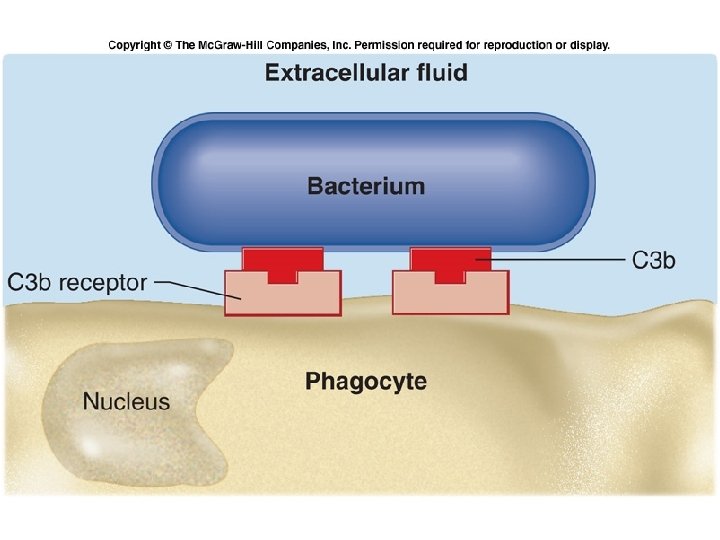
Fig. 18. 05
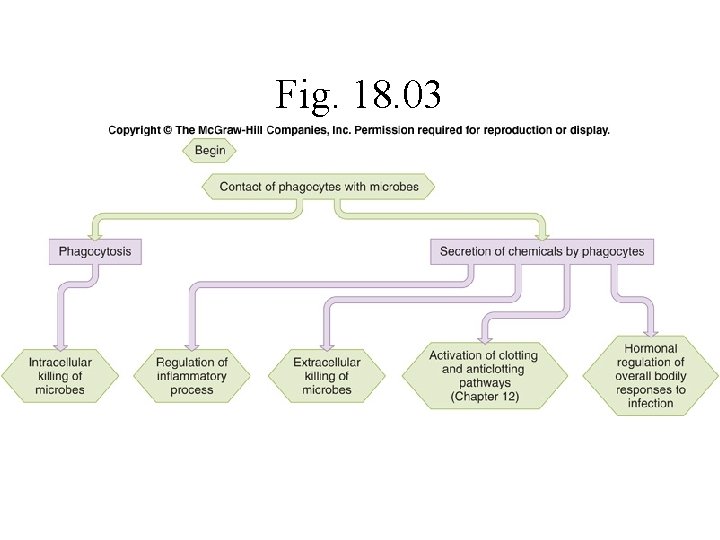
Fig. 18. 03
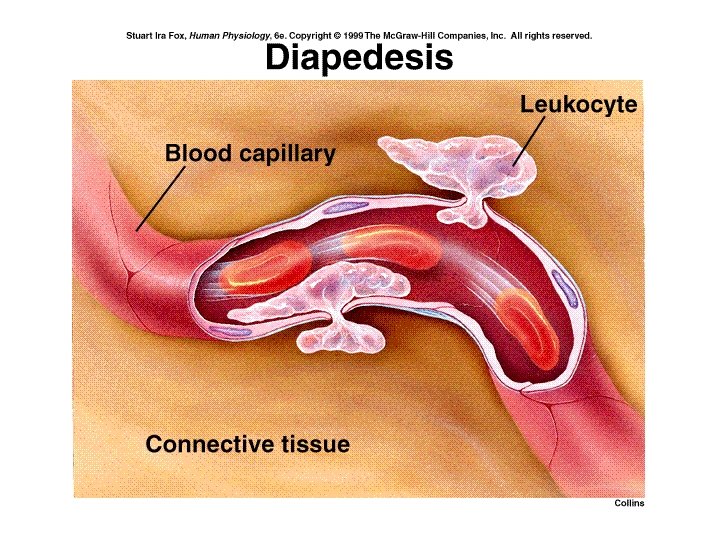
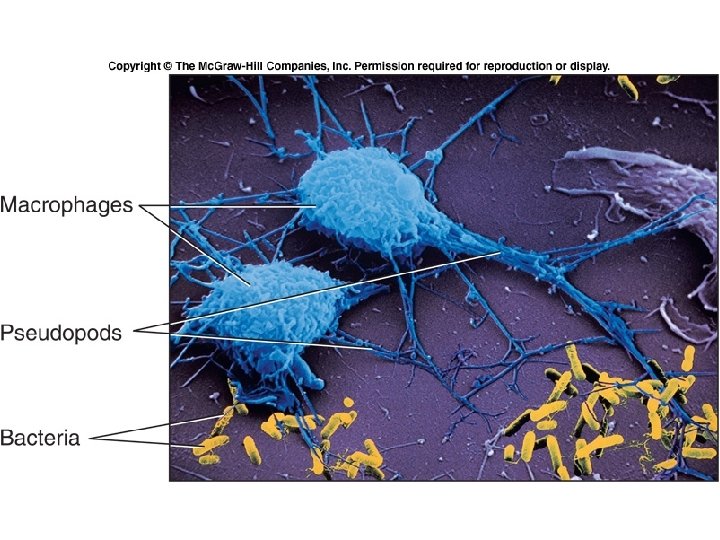
Fig. 18. 01
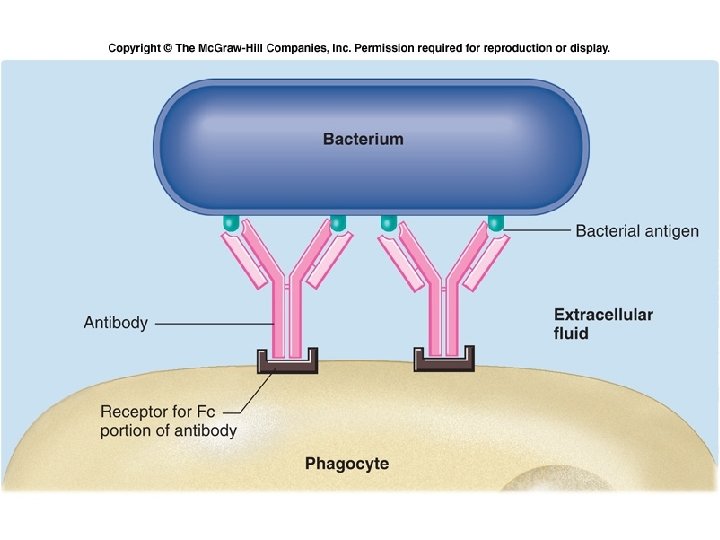
Fig. 18. 15
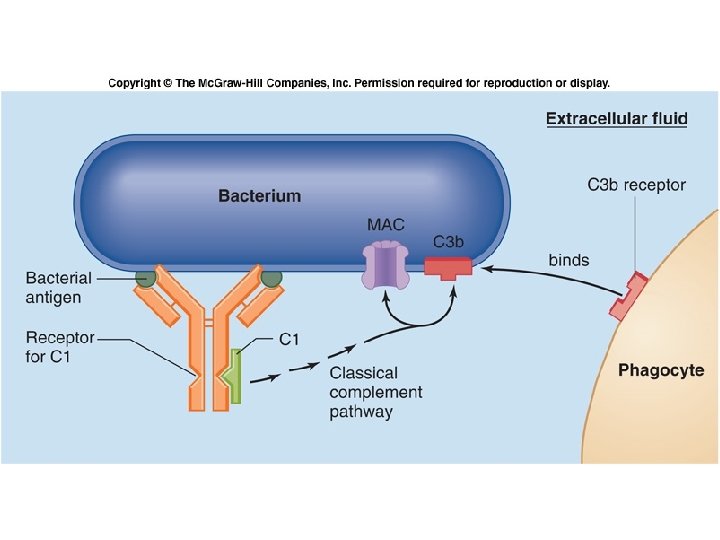
Fig. 18. 16
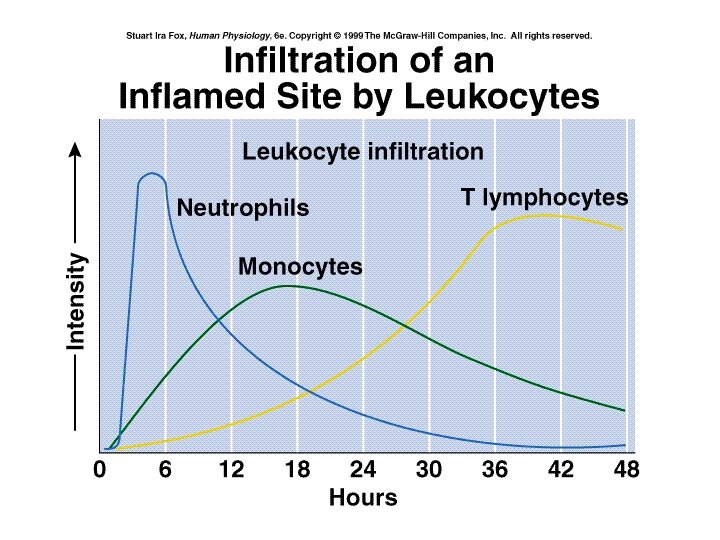

Protective Chemicals • Chemicals that aid in destroying or retarding infectious agents – Interferon –cytokine released when cell attacked by virus; warns other cells in area – Lysozyme –antibacterial enzyme present in tears and saliva – Complement –blood proteins which can detect and destroy bacteria
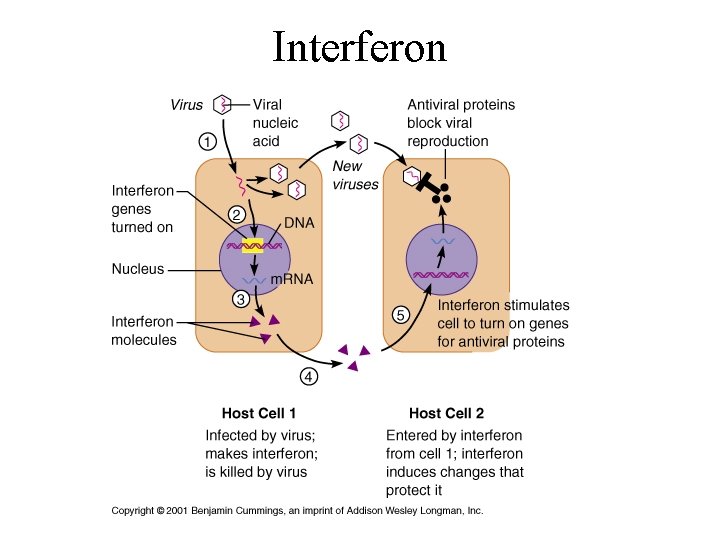
Interferon
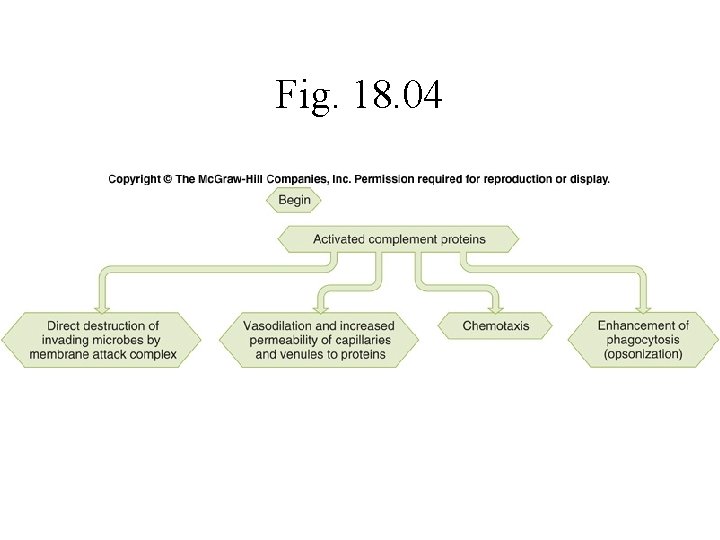
Fig. 18. 04
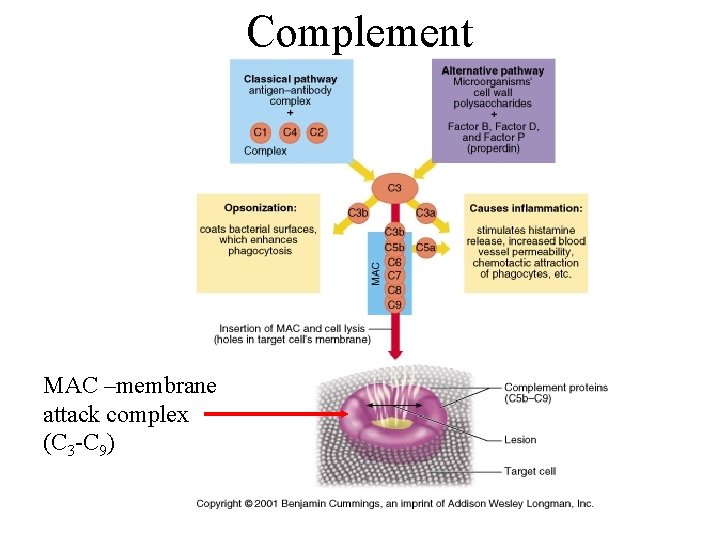
Complement MAC –membrane attack complex (C 3 -C 9)

Specific (Adaptive) Immunity • Individual targets are selected for attack by the lymphocytes that can bind that target (antigen) • Antigens (Ag) – any large substance not normally found in the body; these illicit an immune response (immunogenic and immuno-reactive) • Haptens are small molecules that can trigger an immune response only if bound to larger molecules (like: pollen, some cosmetics, detergent fragrances, poison ivy animal dander and drugs); they are immuno-reactive but not immunogenic by themselves
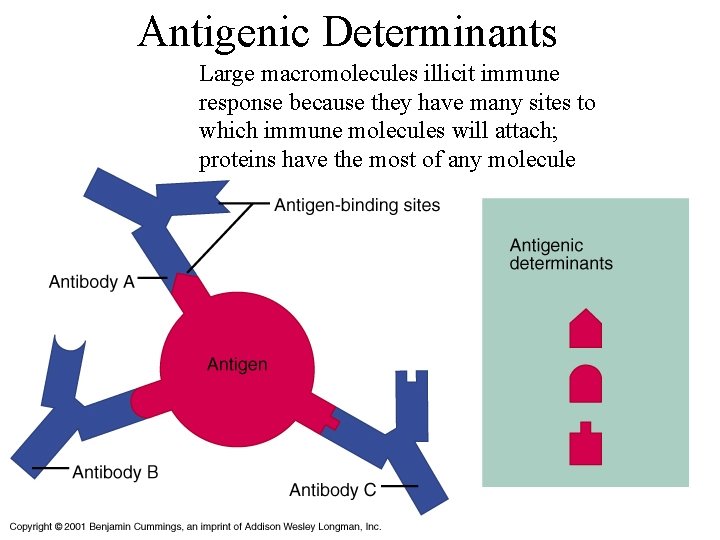
Antigenic Determinants Large macromolecules illicit immune response because they have many sites to which immune molecules will attach; proteins have the most of any molecule

Identifying “Self” from “Non-self” • T-cells migrate to thymus, B-cells remain in bone marrow (the primary lymphoid tissues) • Become immunocompetent -selected for their ability to produce a surface receptor against an antigen and to tolerate self antigens • Those that bind weakly to self-antigens are selected, the others are eliminated • The strongest self-antigens are the MHC proteins • Once competent, the cells are released to move through the blood and aggregate in the secondary lymphoid tissues
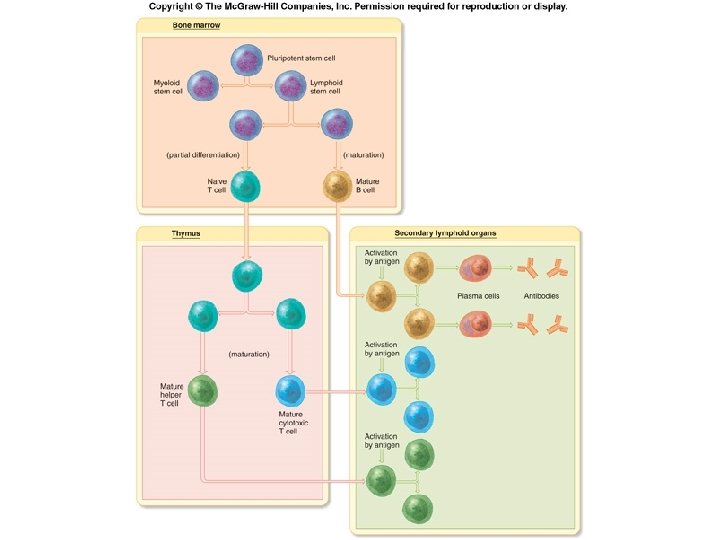
Fig. 18. 08
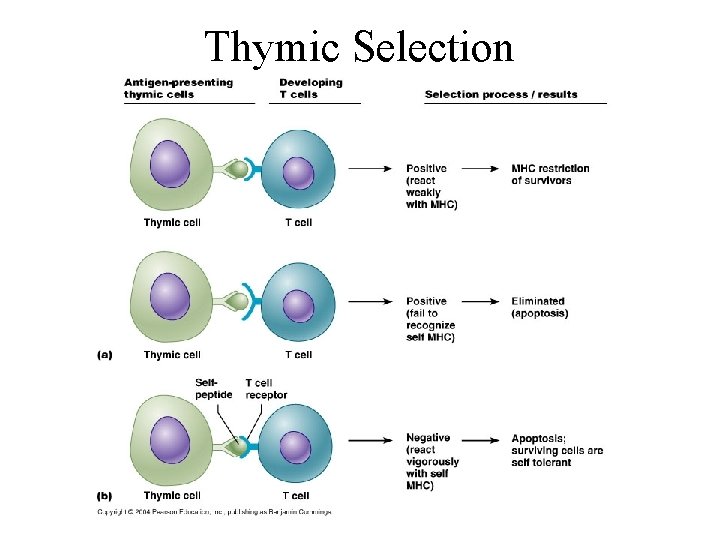
Thymic Selection
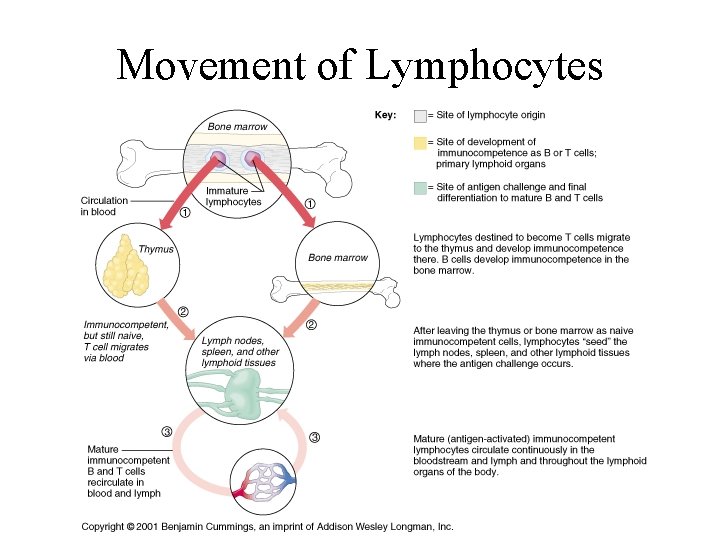
Movement of Lymphocytes

Cells Involved in Specific Immunity • Lymphocytes (B and T cells) -attack antigen bearing agents either chemically (humoral immunity –the B-cells) or physically (cellular immunity –the T-cells) • T and B-cell activation to an antigen works best when they are presented with the antigen by another cell • APCs (Antigen Presenting Cells) (macrophage, surveillance cells, B-cells, infected cells) display foreign antigenic determinants on their MHC II cell surface proteins to activate the lymphocytes
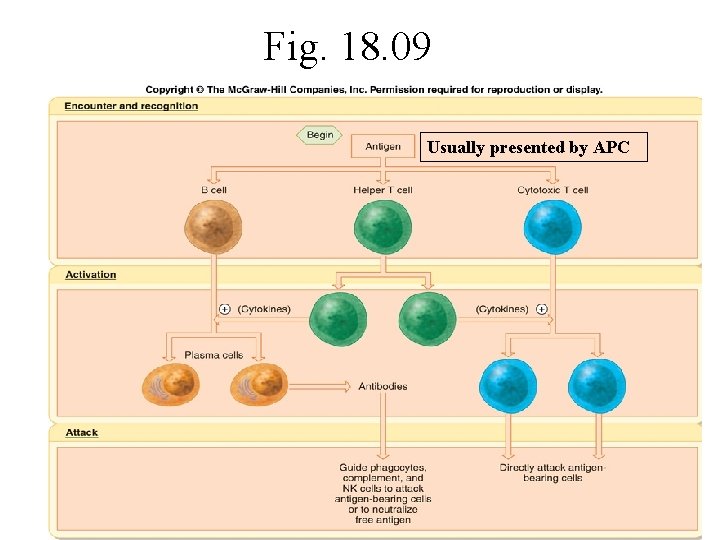
Fig. 18. 09 Usually presented by APC
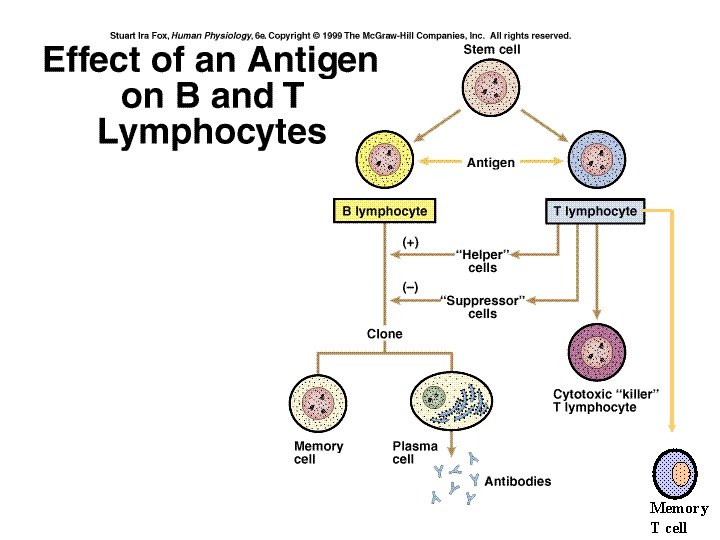
Memory T cell
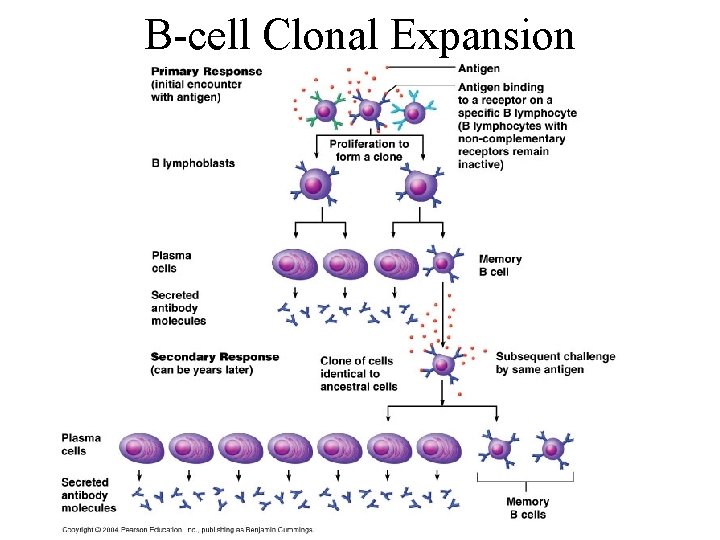
B-cell Clonal Expansion
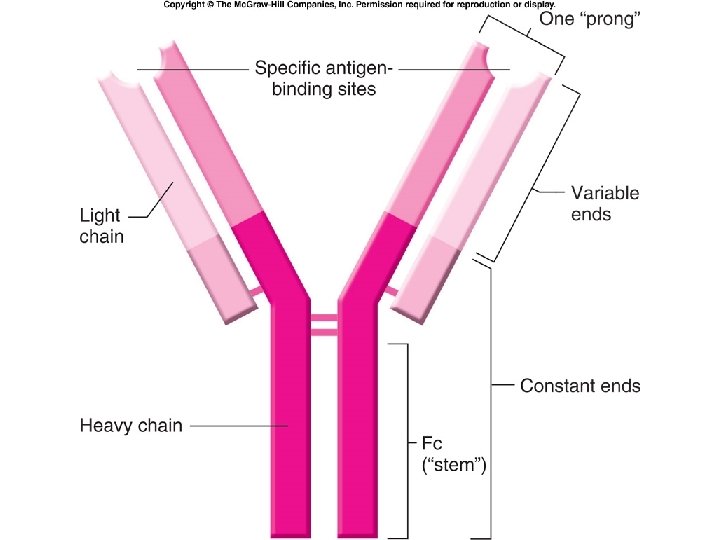
Fig. 18. 10
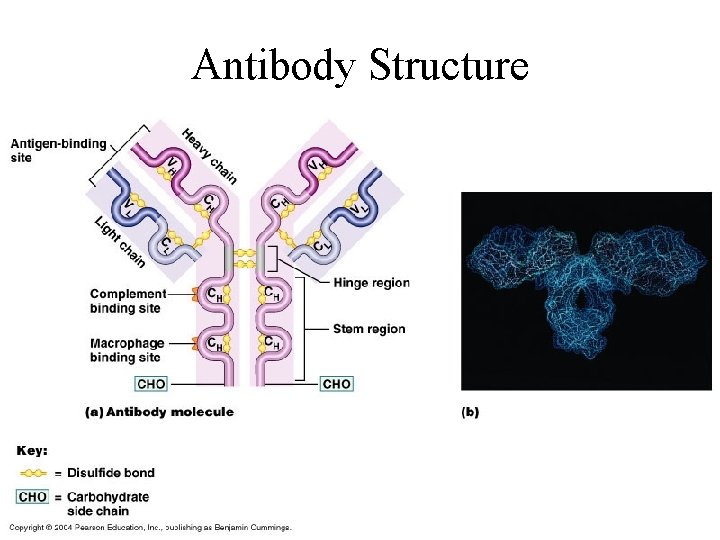
Antibody Structure
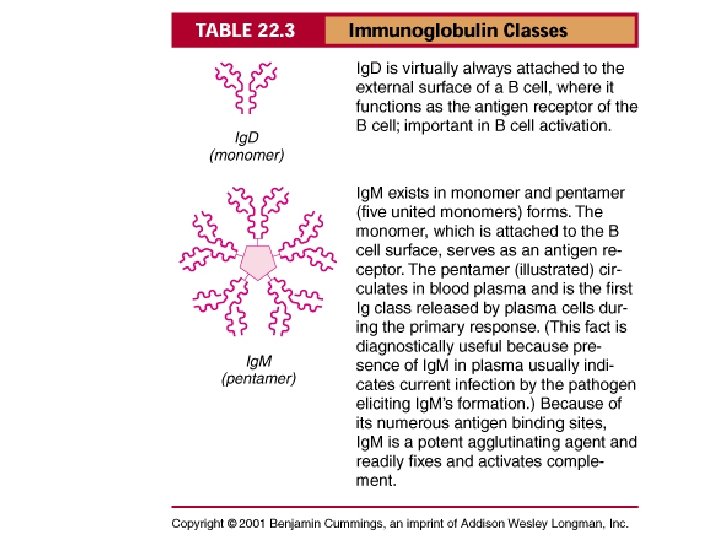

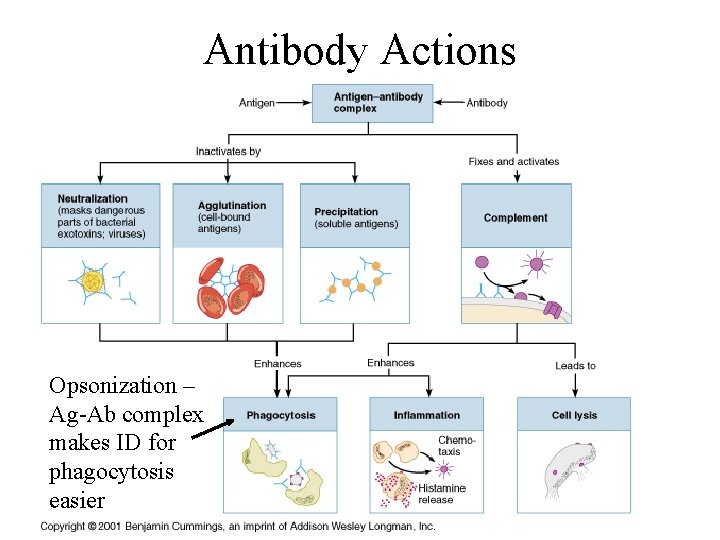
Antibody Actions Opsonization – Ag-Ab complex makes ID for phagocytosis easier
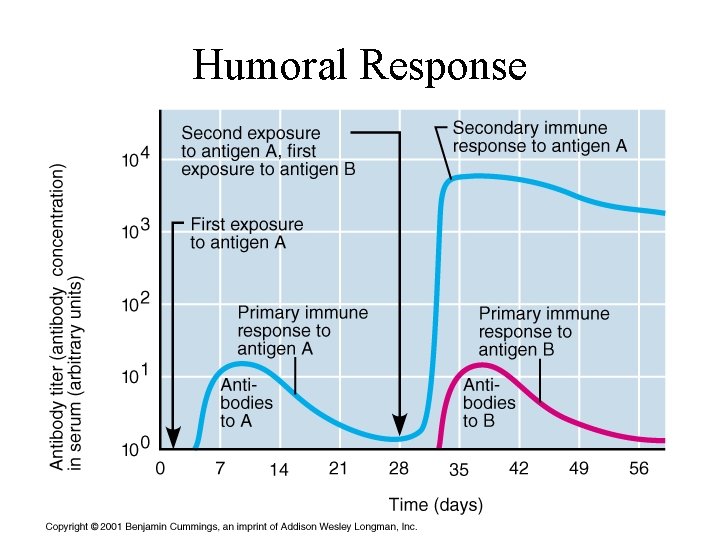
Humoral Response
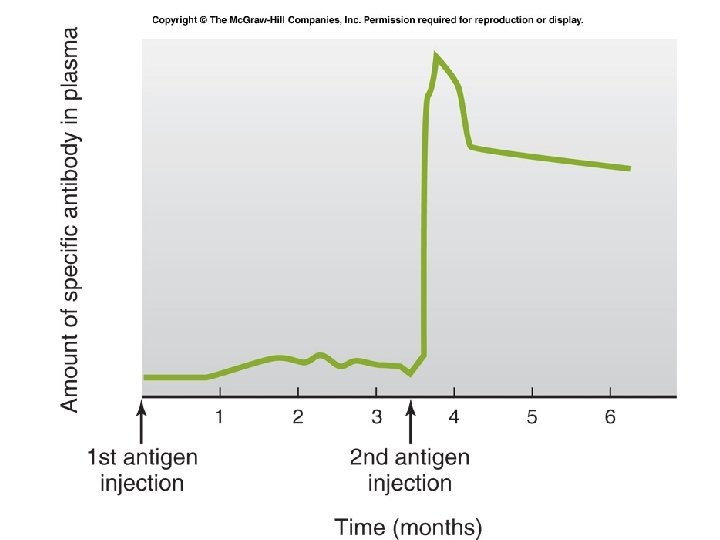
Fig. 18. 17

Control of Lymphocyte Response • B-cells can be activated by the antigen alone, but it is more effective if they are presented the antigen by APCs or stimulated by T-helper cells • Activation of T-helper cells stimulates complete lymphocyte response
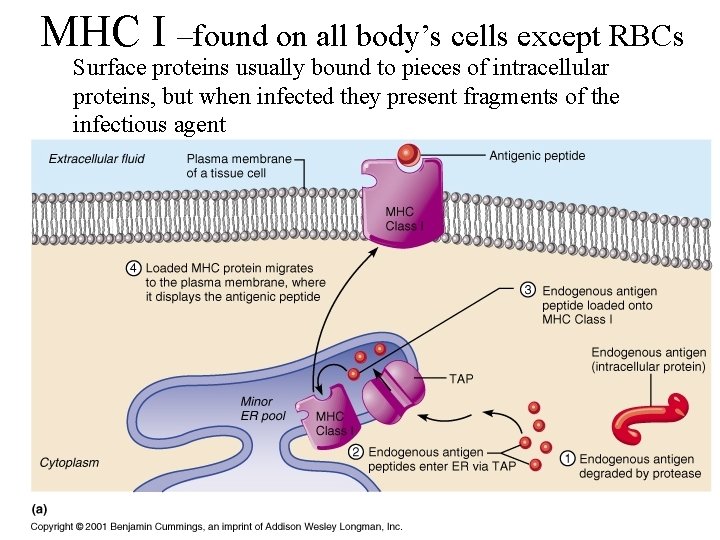
MHC I –found on all body’s cells except RBCs Surface proteins usually bound to pieces of intracellular proteins, but when infected they present fragments of the infectious agent
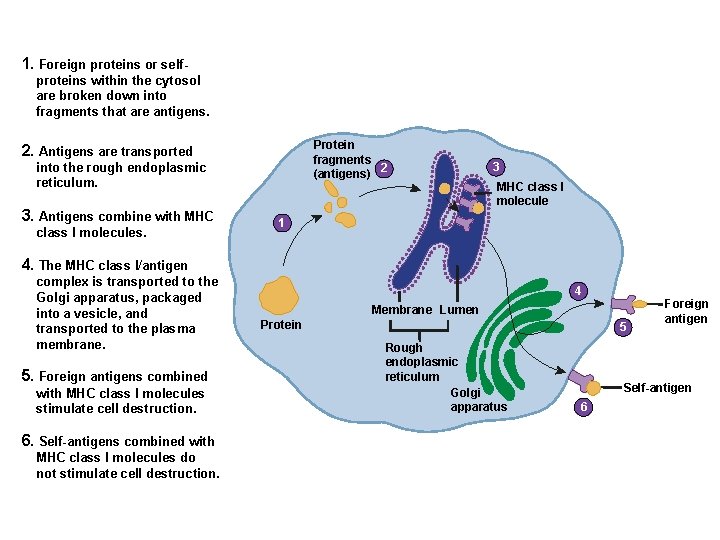
1. Foreign proteins or selfproteins within the cytosol are broken down into fragments that are antigens. Protein fragments (antigens) 2 2. Antigens are transported into the rough endoplasmic reticulum. 3. Antigens combine with MHC class I molecules. 3 MHC class I molecule 1 4. The MHC class I/antigen complex is transported to the Golgi apparatus, packaged into a vesicle, and transported to the plasma membrane. 5. Foreign antigens combined with MHC class I molecules stimulate cell destruction. 6. Self-antigens combined with MHC class I molecules do not stimulate cell destruction. 4 Membrane Lumen Protein 5 Rough endoplasmic reticulum Golgi apparatus Foreign antigen Self-antigen 6
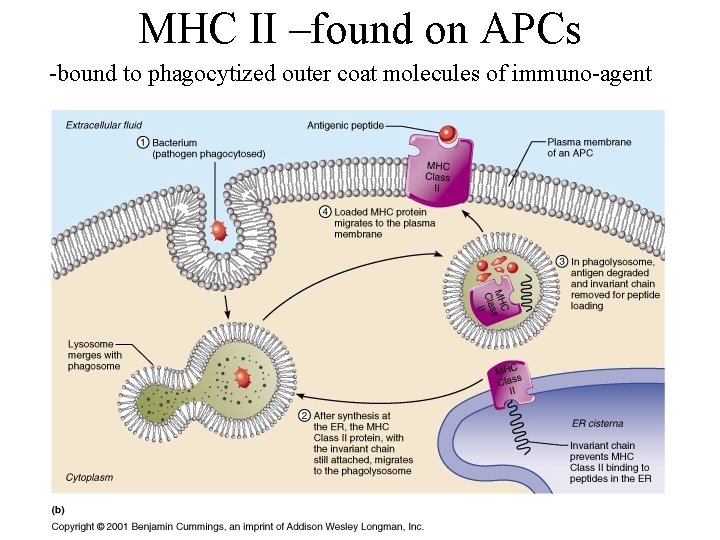
MHC II –found on APCs -bound to phagocytized outer coat molecules of immuno-agent
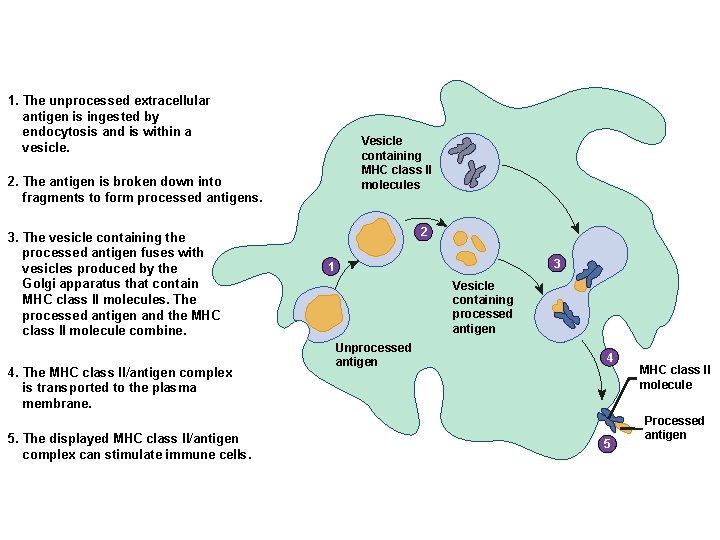
1. The unprocessed extracellular antigen is ingested by endocytosis and is within a vesicle. Vesicle containing MHC class II molecules 2. The antigen is broken down into fragments to form processed antigens. 3. The vesicle containing the processed antigen fuses with vesicles produced by the Golgi apparatus that contain MHC class II molecules. The processed antigen and the MHC class II molecule combine. 4. The MHC class II/antigen complex is transported to the plasma membrane. 5. The displayed MHC class II/antigen complex can stimulate immune cells. 2 3 1 Vesicle containing processed antigen Unprocessed antigen 4 5 MHC class II molecule Processed antigen
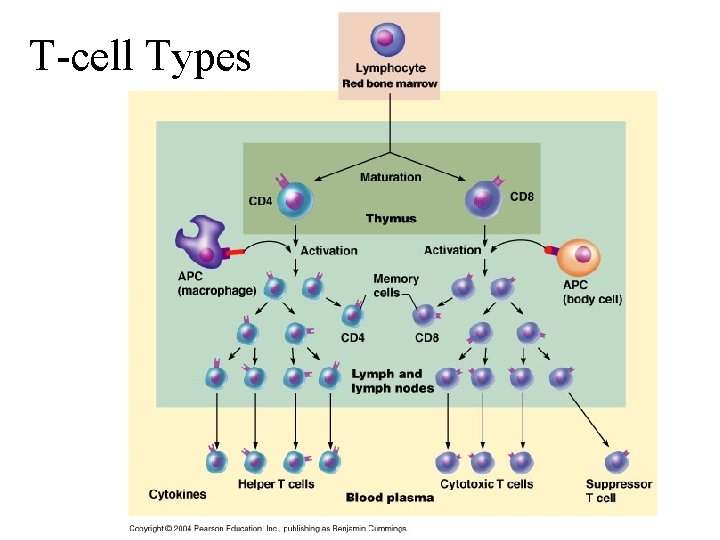
T-cell Types
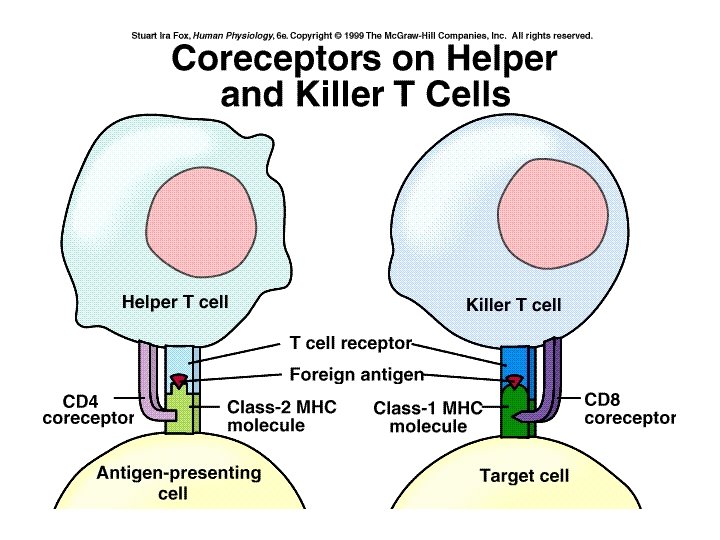
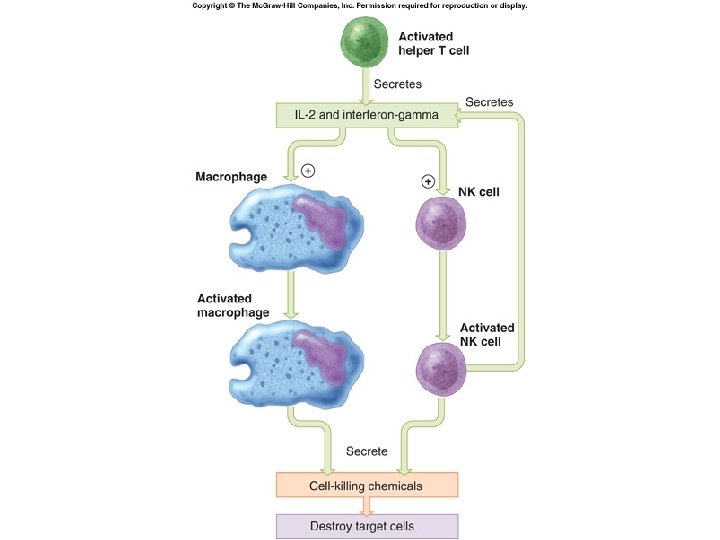
Fig. 18. 19
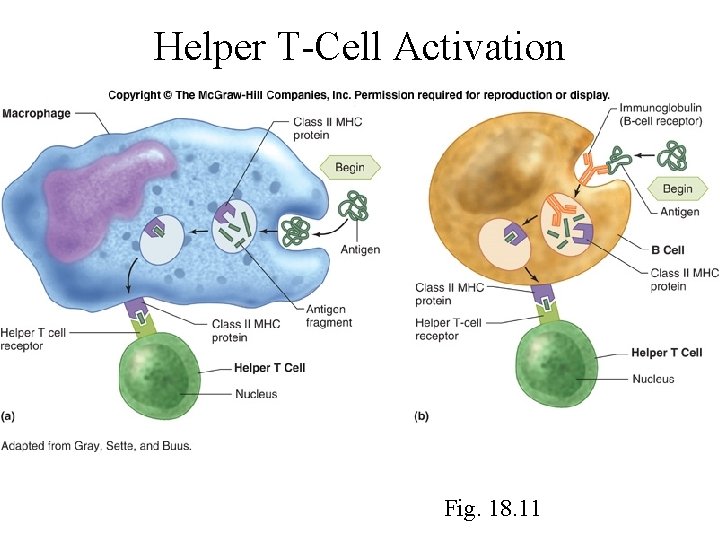
Helper T-Cell Activation Fig. 18. 11
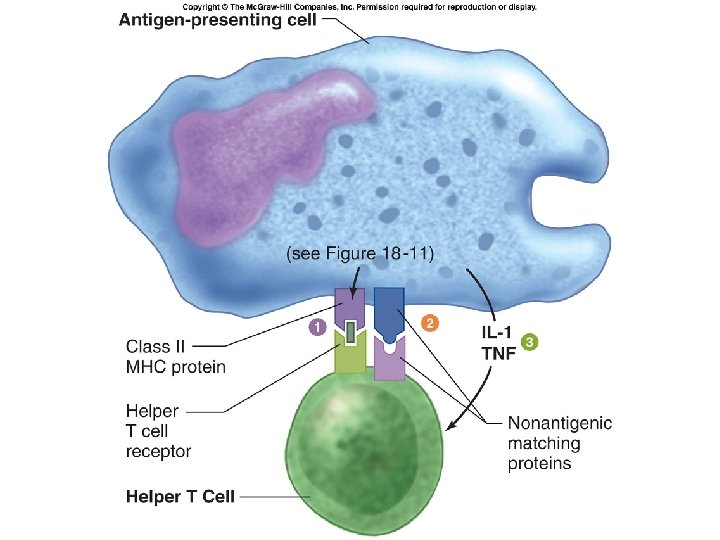
Fig. 18. 12
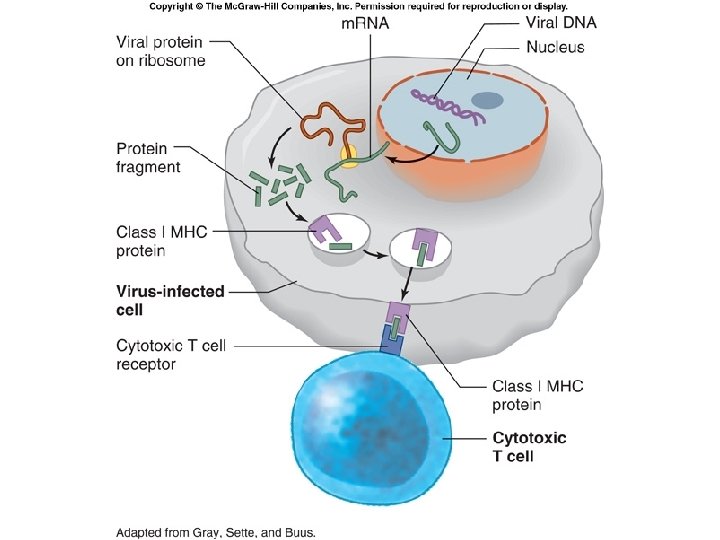
Fig. 18. 13
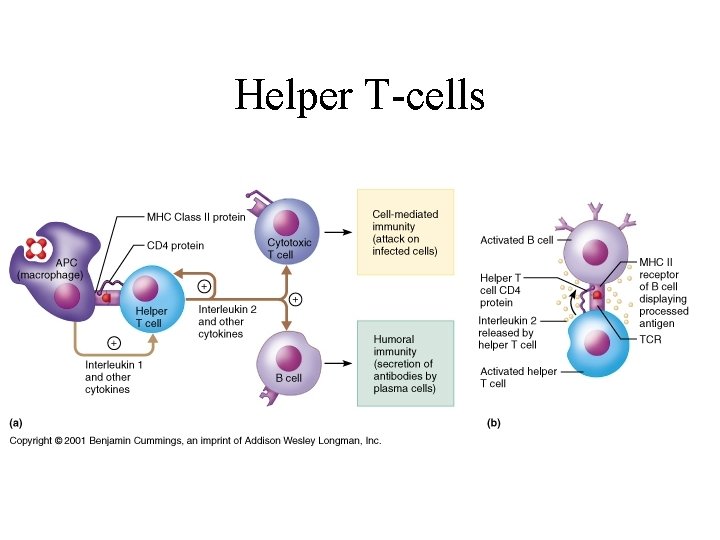
Helper T-cells
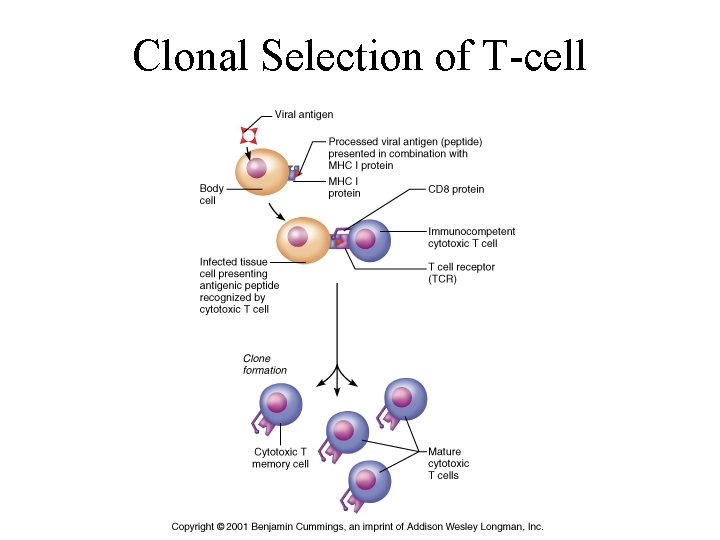
Clonal Selection of T-cell
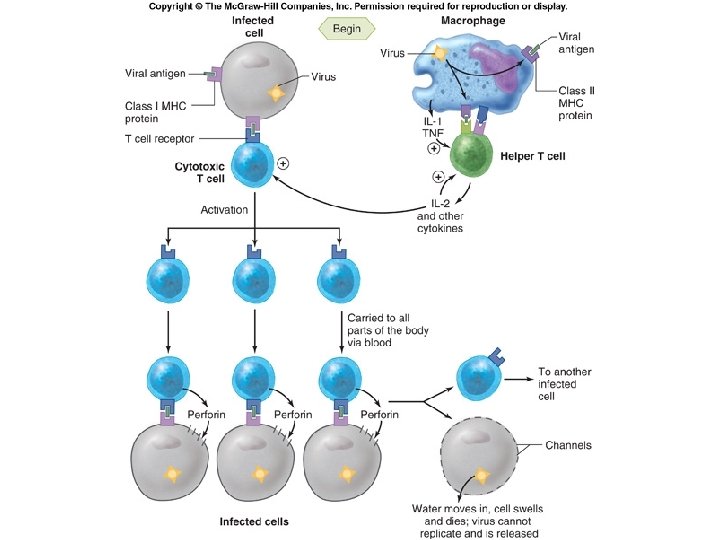
Fig. 18
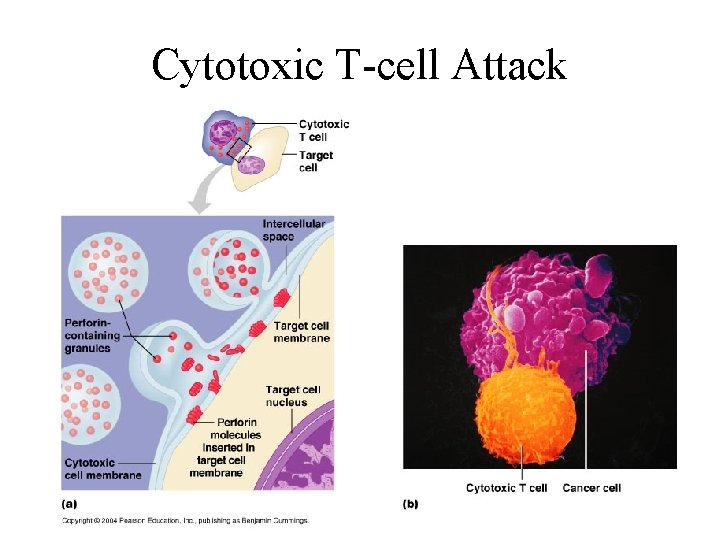
Cytotoxic T-cell Attack
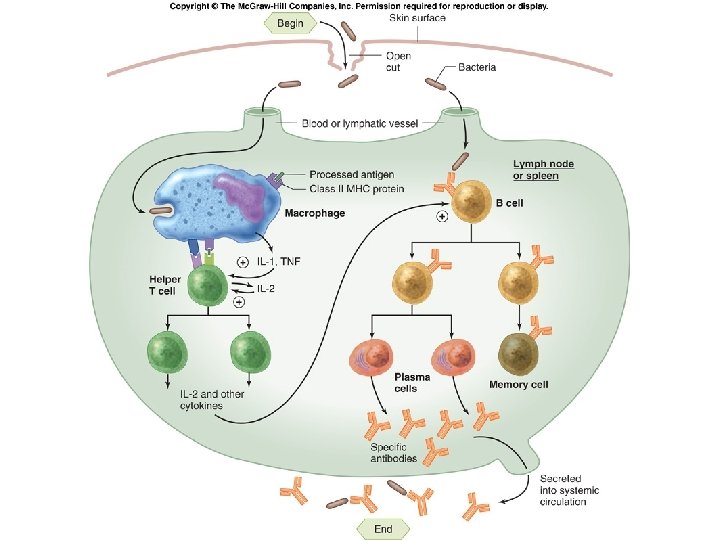
Fig. 18. 14
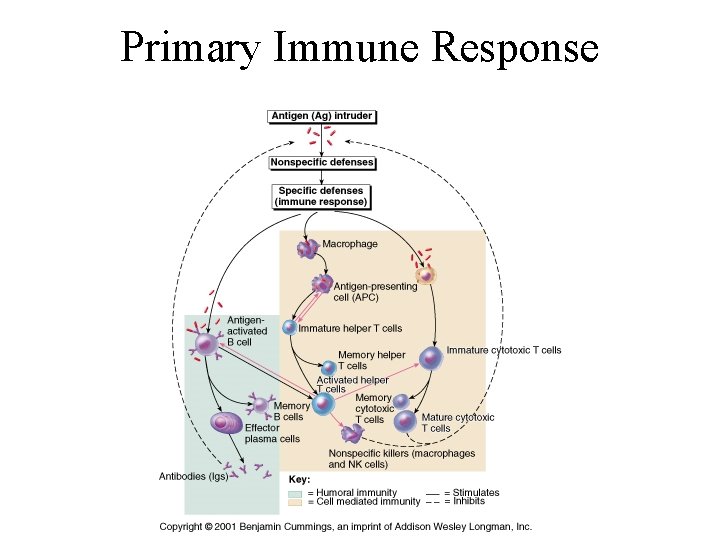
Primary Immune Response
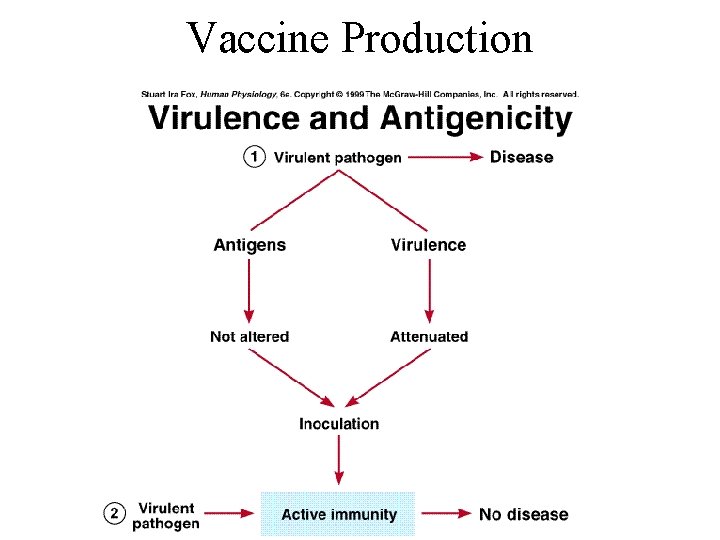
Vaccine Production
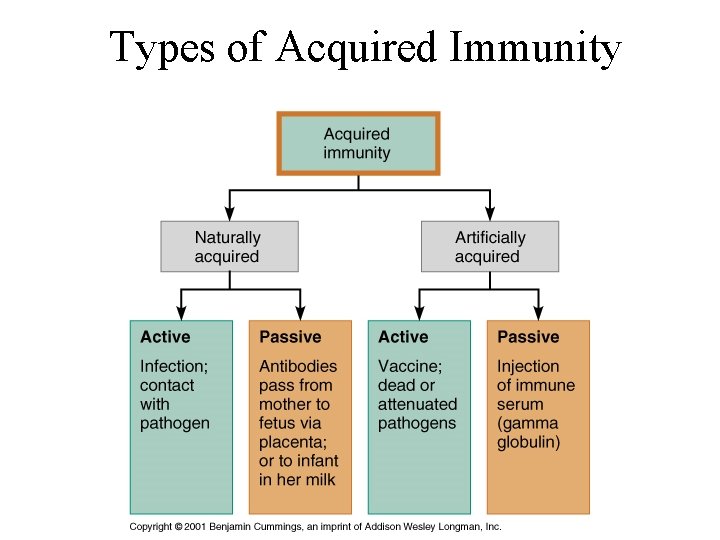
Types of Acquired Immunity
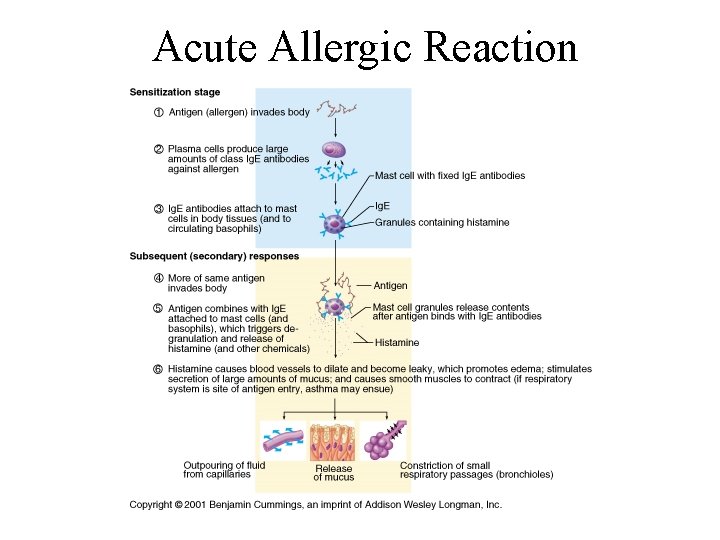
Acute Allergic Reaction
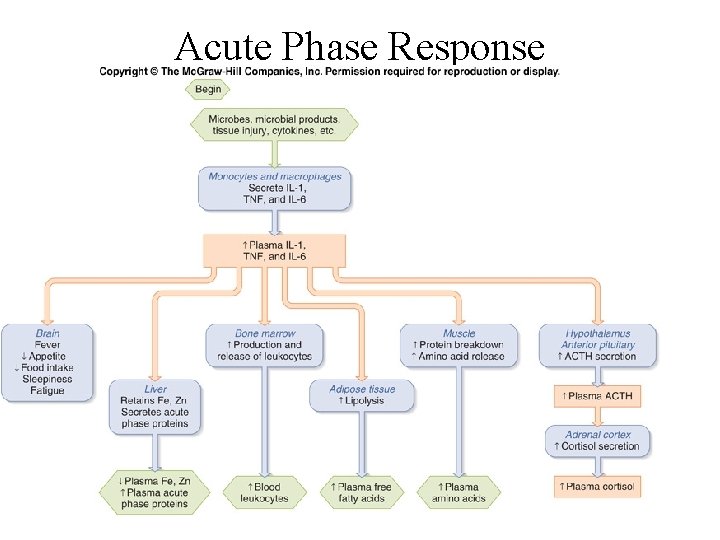
Acute Phase Response
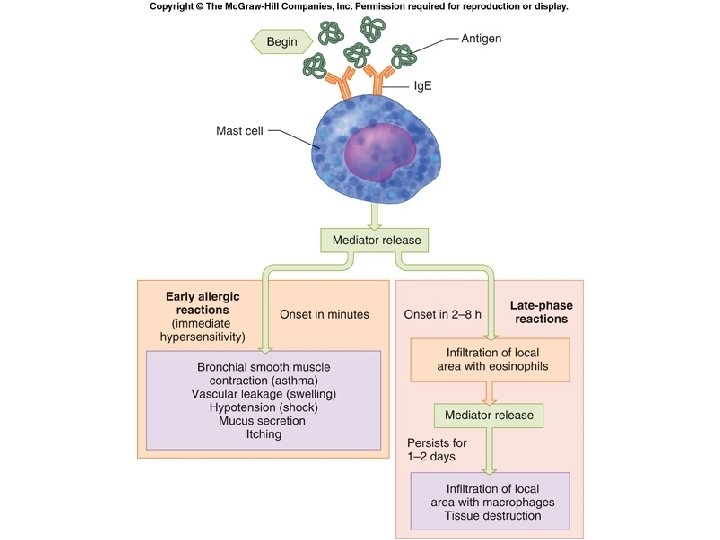
Fig. 18. 21

Fig. 18. 05

Fig. 18. 10

Pathologies • AIDS –HIV invades T-helper cells, diminishing effectiveness of immune response; may have as long as 8 year incubation time, 100% fatal • Autoimmune Diseases –Immune system targets naturally occurring compounds of the body (usually sequestered proteins) MS, rheumatoid arthritis, Diabetes mellitus (I), etc. • Cancer –cancers cells spontaneously form during life, but the immune system keeps them in check; failure results in tumors and metastasis
- Slides: 64