Immunity Dr Spandana Charles MD Immunity Resistance to





















- Slides: 37

Immunity Dr. Spandana Charles MD

Immunity • Resistance to disease • Immune system – Two intrinsic systems • Innate (nonspecific) defense system • Adaptive (specific) defense system © 2013 Pearson Education, Inc.

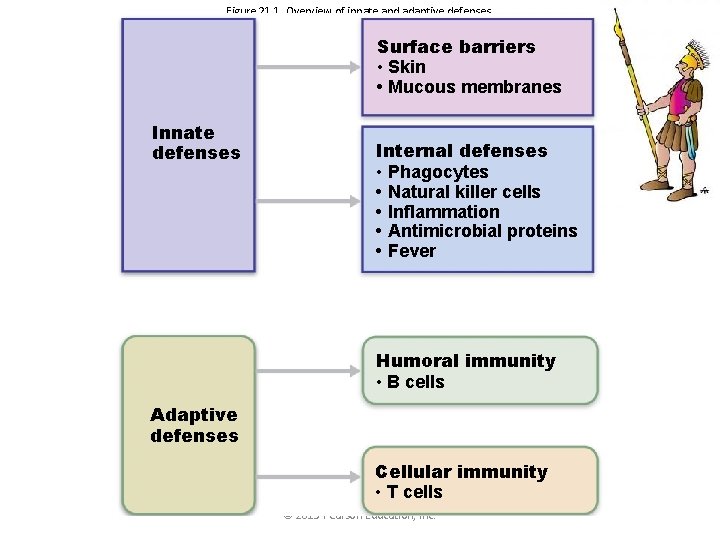
Figure 21. 1 Overview of innate and adaptive defenses. Surface barriers • Skin • Mucous membranes Innate defenses Internal defenses • Phagocytes • Natural killer cells • Inflammation • Antimicrobial proteins • Fever Humoral immunity • B cells Adaptive defenses Cellular immunity • T cells © 2013 Pearson Education, Inc.

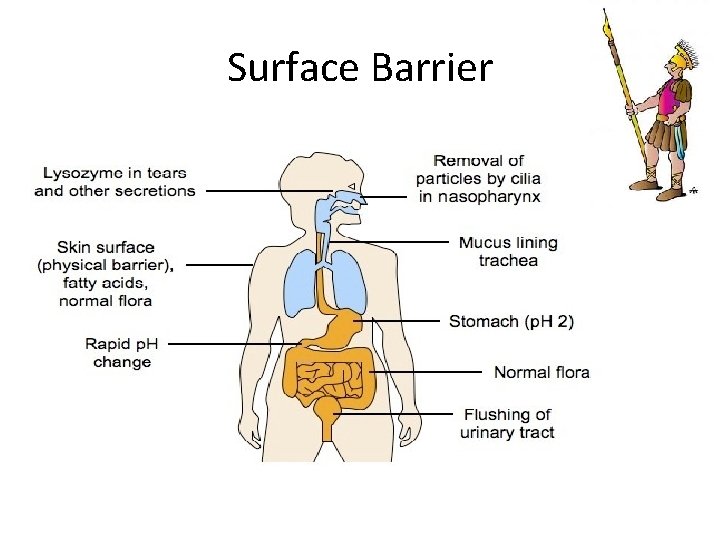
Surface Barrier

Internal Defenses: Cells and Chemicals • Necessary if microorganisms invade deeper tissues – Phagocytes – Natural killer (NK) cells – Antimicrobial proteins (interferons and complement proteins) – Fever – Inflammatory response (macrophages, mast cells, WBCs, and inflammatory chemicals) © 2013 Pearson Education, Inc.

Phagocytes • Neutrophils most abundant but die fighting Become phagocytic on exposure to infectious material • Macrophages develop from monocytes – chief phagocytic cells – robust cells • Free macrophages wander through tissue spaces, e. g. , alveolar macrophages • Fixed macrophages -permanent residents of some organs; e. g. , Kupffer cells (liver) and microglia (brain) © 2013 Pearson Education, Inc.

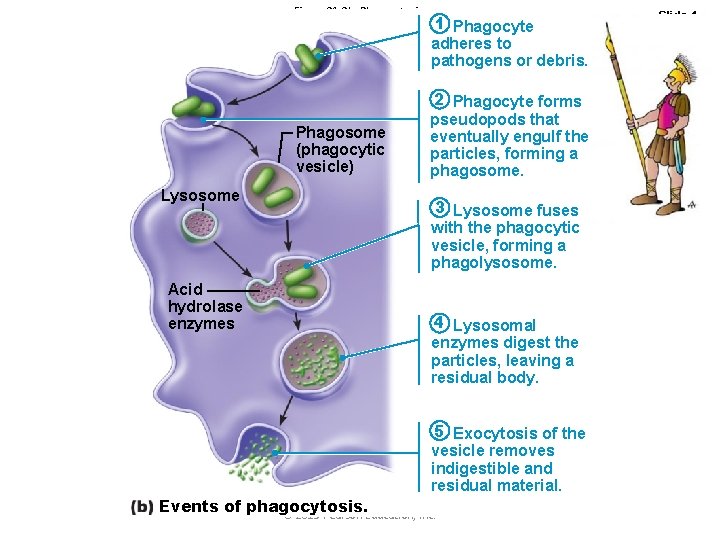
Figure 21. 2 b Phagocytosis. Phagosome (phagocytic vesicle) Lysosome Acid hydrolase enzymes 1 Phagocyte adheres to pathogens or debris. 2 Phagocyte forms pseudopods that eventually engulf the particles, forming a phagosome. 3 Lysosome fuses with the phagocytic vesicle, forming a phagolysosome. 4 Lysosomal enzymes digest the particles, leaving a residual body. 5 Exocytosis of the vesicle removes indigestible and residual material. Events of phagocytosis. © 2013 Pearson Education, Inc. Slide 1

Inflammatory Response • • • Triggered whenever body tissues injured Prevents spread of damaging agents Disposes of cell debris and pathogens Alerts adaptive immune system Sets the stage for repair Cardinal signs of acute inflammation: 1. Redness 2. Heat 3. Swelling 4. Pain (Sometimes 5. Impairment of function) © 2013 Pearson Education, Inc.

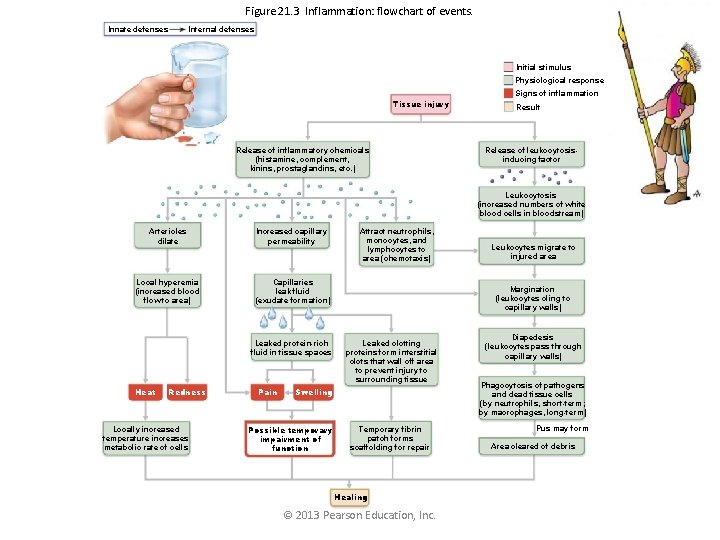
Figure 21. 3 Inflammation: flowchart of events. Innate defenses Internal defenses Initial stimulus Physiological response Tissue injury Release of inflammatory chemicals (histamine, complement, kinins, prostaglandins, etc. ) Signs of inflammation Result Release of leukocytosisinducing factor Leukocytosis (increased numbers of white blood cells in bloodstream) Arterioles dilate Increased capillary permeability Local hyperemia (increased blood flow to area) Capillaries leak fluid (exudate formation) Leaked protein-rich fluid in tissue spaces Heat Redness Locally increased temperature increases metabolic rate of cells Pain Attract neutrophils, monocytes, and lymphocytes to area (chemotaxis) Margination (leukocytes cling to capillary walls) Leaked clotting proteins form interstitial clots that wall off area to prevent injury to surrounding tissue Swelling Possible temporary impairment of function Leukocytes migrate to injured area Temporary fibrin patch forms scaffolding for repair Healing © 2013 Pearson Education, Inc. Diapedesis (leukocytes pass through capillary walls) Phagocytosis of pathogens and dead tissue cells (by neutrophils, short-term; by macrophages, long-term) Pus may form Area cleared of debris

Phagocyte Mobilization • Neutrophils lead; macrophages follow – As attack continues, monocytes arrive • 12 hours after leaving bloodstream macrophages • These "late-arrivers" replace dying neutrophils and remain for clean up prior to repair • If inflammation due to pathogens, complement activated; adaptive immunity elements arrive © 2013 Pearson Education, Inc.

Phagocyte Mobilization • Steps for phagocyte mobilization 1. Leukocytosis: release of neutrophils from bone marrow in response to leukocytosis-inducing factors from injured cells 2. Margination: neutrophils cling to walls of capillaries in inflamed area in response to CAMs 3. Diapedesis of neutrophils 4. Chemotaxis: inflammatory chemicals (chemotactic agent) promote positive chemotaxis of neutrophils © 2013 Pearson Education, Inc.

Antimicrobial Proteins • Interferons (IFNs) and complement proteins – Attack microorganisms directly – Hinder microorganisms' ability to reproduce © 2013 Pearson Education, Inc.

Interferons • Family of immune modulating proteins – Have slightly different physiological effects • Viral-infected cells secrete IFNs (e. g. , IFN alpha and beta) to "warn" neighboring cells – IFNs enter neighboring cells produce proteins that block viral reproduction and degrade viral RNA – IFN alpha and beta also activate NK cells • Artificial IFNs used to treat hepatitis C, genital warts, multiple sclerosis, hairy cell leukemia © 2013 Pearson Education, Inc.

Complement • Unleashes inflammatory chemicals that amplify all aspects of inflammatory response • Kills bacteria and certain other cell types by cell lysis • Enhances both innate and adaptive defenses © 2013 Pearson Education, Inc.

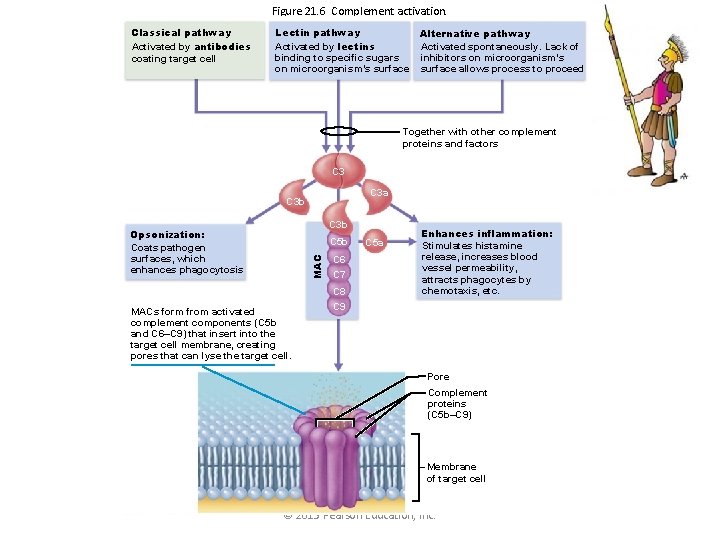
Figure 21. 6 Complement activation. Classical pathway Activated by antibodies coating target cell Lectin pathway Activated by lectins binding to specific sugars on microorganism’s surface Alternative pathway Activated spontaneously. Lack of inhibitors on microorganism’s surface allows process to proceed Together with other complement proteins and factors C 3 a C 3 b Opsonization: Coats pathogen surfaces, which enhances phagocytosis MAC C 5 b MACs form from activated complement components (C 5 b and C 6–C 9) that insert into the target cell membrane, creating pores that can lyse the target cell. C 6 C 7 C 8 C 9 C 5 a Enhances inflammation: Stimulates histamine release, increases blood vessel permeability, attracts phagocytes by chemotaxis, etc. Pore Complement proteins (C 5 b–C 9) Membrane of target cell © 2013 Pearson Education, Inc.

Fever • Abnormally high body temperature • Systemic response to invading microorganisms • Leukocytes and macrophages exposed to foreign substances secrete pyrogens • Pyrogens act on body's thermostat in hypothalamus, raising body temperature © 2013 Pearson Education, Inc.

Adaptive Immunity • Immunity against specific antigens • Is of two types – Humoral Immunity – Cell mediated immunity

Cells of the Adaptive Immune System • Three types of cells – Two types of lymphocytes • B lymphocytes (B cells)—Humoral immunity • T lymphocytes (T cells)—Cell-mediated immunity – Antigen-presenting cells (APCs) • Do not respond to specific antigens • Play essential auxiliary roles in immunity © 2013 Pearson Education, Inc.

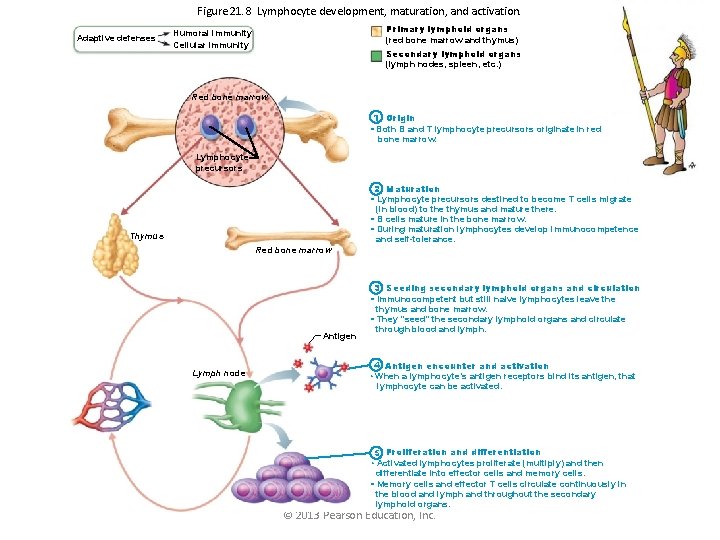
Figure 21. 8 Lymphocyte development, maturation, and activation. Adaptive defenses Primary lymphoid organs (red bone marrow and thymus) Humoral immunity Cellular immunity Secondary lymphoid organs (lymph nodes, spleen, etc. ) Red bone marrow 1 Origin • Both B and T lymphocyte precursors originate in red bone marrow. Lymphocyte precursors 2 Maturation • Lymphocyte precursors destined to become T cells migrate (in blood) to the thymus and mature there. • B cells mature in the bone marrow. • During maturation lymphocytes develop immunocompetence and self-tolerance. Thymus Red bone marrow Antigen Lymph node 3 Seeding secondary lymphoid organs and circulation • Immunocompetent but still naive lymphocytes leave thymus and bone marrow. • They “seed” the secondary lymphoid organs and circulate through blood and lymph. 4 Antigen encounter and activation • When a lymphocyte’s antigen receptors bind its antigen, that lymphocyte can be activated. 5 Proliferation and differentiation • Activated lymphocytes proliferate (multiply) and then differentiate into effector cells and memory cells. • Memory cells and effector T cells circulate continuously in the blood and lymph and throughout the secondary lymphoid organs. © 2013 Pearson Education, Inc. Slide 1

Humoral Immunity – Antibody-Mediated Immunity – Involves production of antibodies against foreign antigens – Produced by B cells – Defense against bacteria, bacterial toxins, and viruses that circulate freely in body fluids, before they enter cells

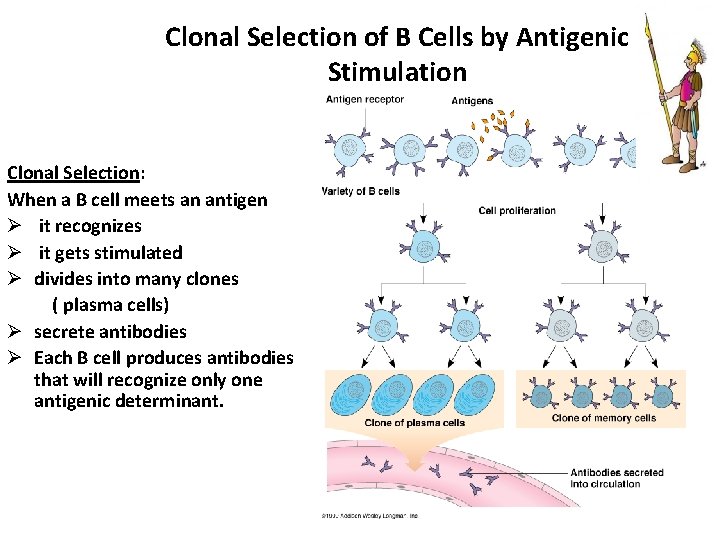
Clonal Selection of B Cells by Antigenic Stimulation Clonal Selection: When a B cell meets an antigen Ø it recognizes Ø it gets stimulated Ø divides into many clones ( plasma cells) Ø secrete antibodies Ø Each B cell produces antibodies that will recognize only one antigenic determinant.

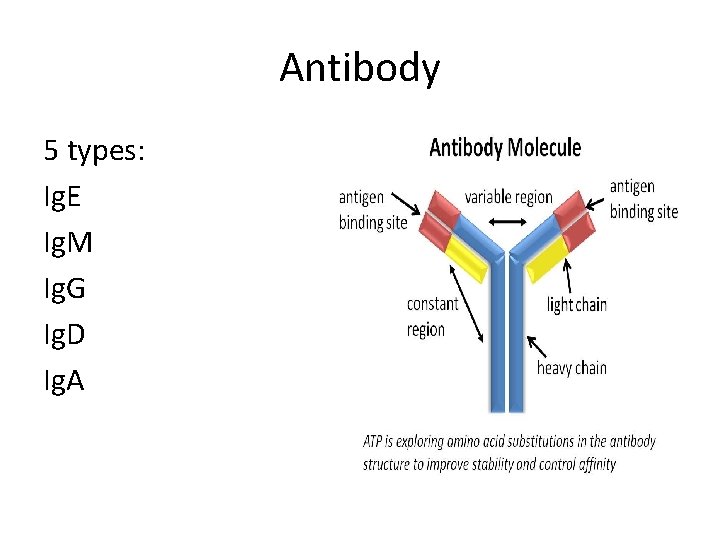
Antibody 5 types: Ig. E Ig. M Ig. G Ig. D Ig. A

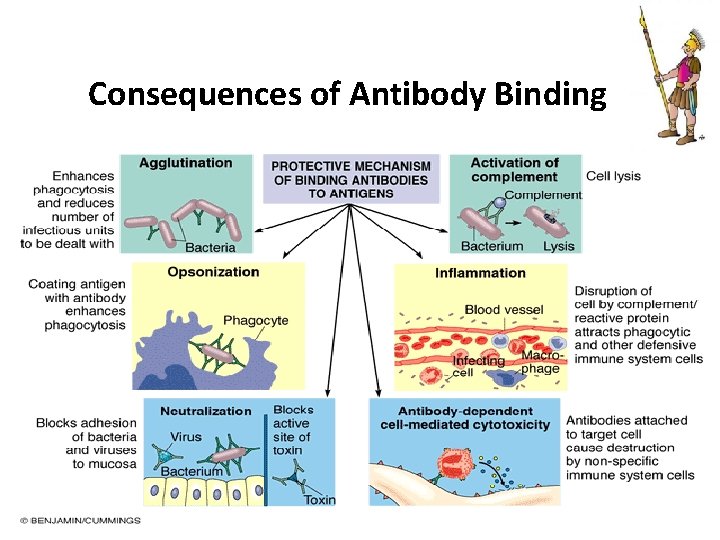
Consequences of Antibody Binding

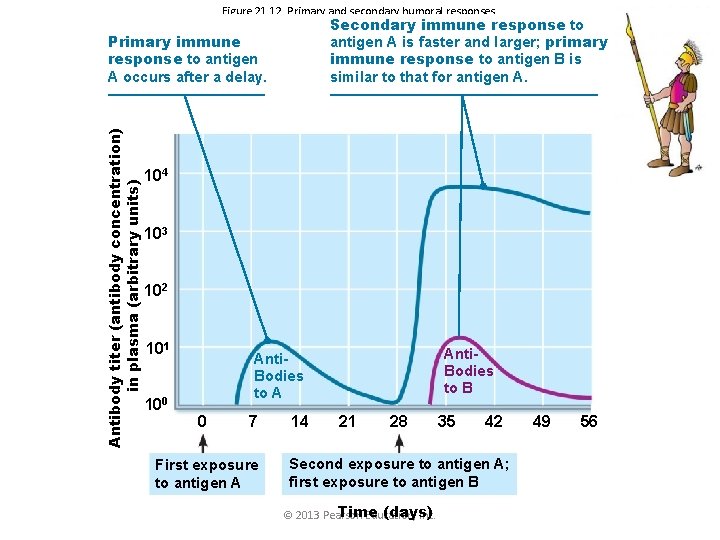
Figure 21. 12 Primary and secondary humoral responses. Secondary immune response to antigen A is faster and larger; primary immune response to antigen B is similar to that for antigen A. Antibody titer (antibody concentration) in plasma (arbitrary units) Primary immune response to antigen A occurs after a delay. 104 103 102 101 100 Anti. Bodies to B Anti. Bodies to A 0 7 First exposure to antigen A 14 21 28 35 42 Second exposure to antigen A; first exposure to antigen B Time (days) © 2013 Pearson Education, Inc. 49 56

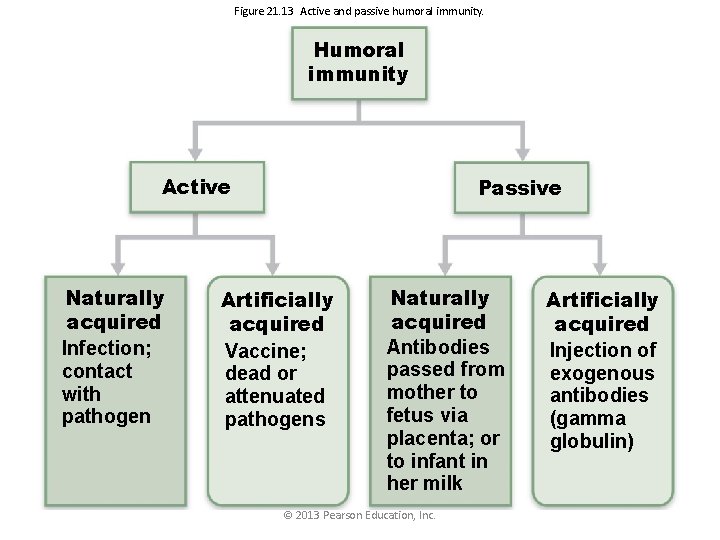
Figure 21. 13 Active and passive humoral immunity. Humoral immunity Active Naturally acquired Infection; contact with pathogen Passive Artificially acquired Vaccine; dead or attenuated pathogens Naturally acquired Antibodies passed from mother to fetus via placenta; or to infant in her milk © 2013 Pearson Education, Inc. Artificially acquired Injection of exogenous antibodies (gamma globulin)

Humoral Immunity • Active Humoral Immunity-Vaccines – Most of dead or attenuated pathogens – Spare us symptoms of primary response – Provide antigenic determinants that are immunogenic and reactive. • Passive Humoral Immunity-Antibodies are injected into a person © 2013 Pearson Education, Inc.

Cellular Immunity • Lymphocytes act against target cell – Directly – by killing infected cells – Indirectly – by releasing chemicals that enhance inflammatory response; or activating other lymphocytes or macrophages © 2013 Pearson Education, Inc.

T cells • T cells mature in thymus under negative and positive selection pressures ("tests") – Positive selection • Selects T cells capable of recognizing self-MHC proteins (MHC restriction); failures destroyed by apoptosis – Negative selection • Prompts apoptosis of T cells that bind to self-antigens displayed by self-MHC • Ensures self-tolerance © 2013 Pearson Education, Inc.

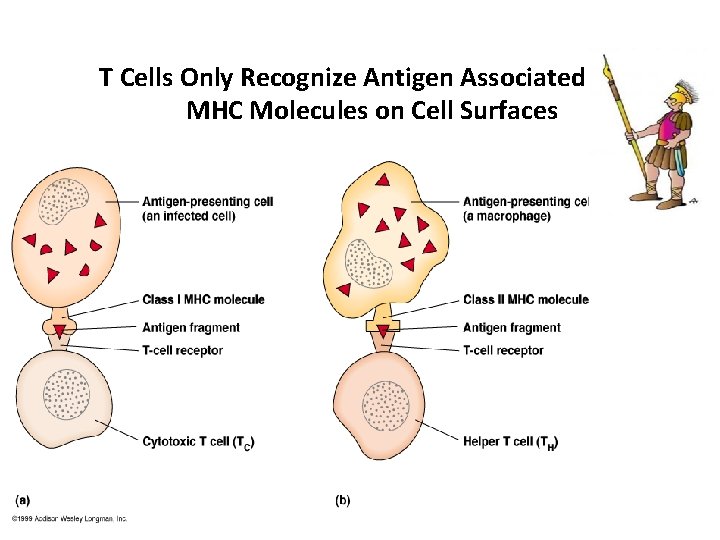
Cellular Components of CMI T cells are key cellular component of immunity – T cells have an antigen receptor (T cell receptor) that recognizes & reacts to a specific antigen – Antigens that stimulate this response are mainly intracellular – T cell receptor only recognize antigens combined with major histocompatability (MHC) proteins on the surface of cells. • MHC Class I: Found on all cells. • MHC Class II: Found on phagocytes. – Clonal selection increases number of T cells.

T Cells Only Recognize Antigen Associated with MHC Molecules on Cell Surfaces

T cells Helper T cells • Activate macrophages • Induce formation of cytotoxic T cells • Stimulate B cells to produce antibodies. Cytotoxic T cells. Release protein called perforin which forms a pore in target cell, causing lysis of infected cells. • Destroy target cells • Supressor T cells Inhibit the immune response

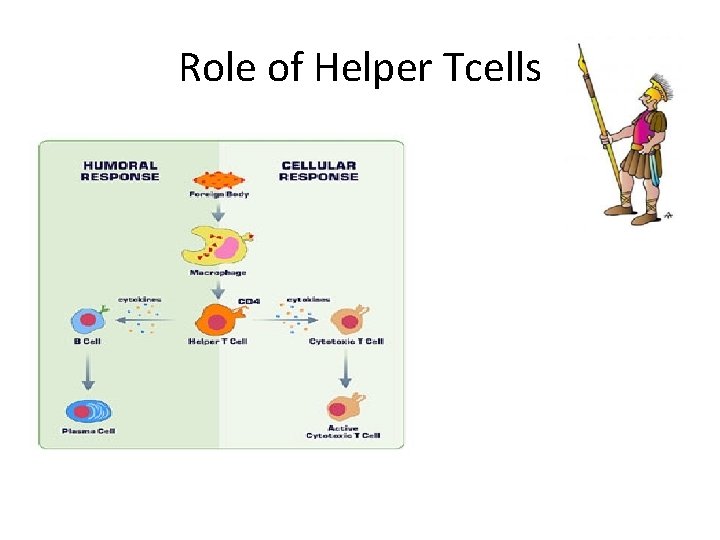
Role of Helper Tcells

Organ Transplants • Four varieties – Autografts: from one body site to another in same person – Isografts: between identical twins – Allografts: between individuals who are not identical twins – Xenografts: from another animal species © 2013 Pearson Education, Inc.

Acquired Immune Deficiency Syndrome (AIDS) • Caused by human immunodeficiency virus (HIV) transmitted via body fluids—blood, semen, and vaginal secretions • Attacks the helper T cells- Depresses Cell mediated Immunity • HIV enters cell and uses reverse transcriptase to produce DNA from its viral RNA • The DNA copy (a provirus) directs host cell to make viral RNA and proteins, enabling virus to reproduce

Autoimmune Diseases • Immune system loses ability to distinguish self from foreign • Production of autoantibodies and sensitized TC cells that destroy body tissues • Examples include multiple sclerosis, myasthenia gravis, Graves' disease, type 1 diabetes mellitus, systemic lupus erythematosus (SLE), glomerulonephritis, and rheumatoid arthritis © 2013 Pearson Education, Inc.

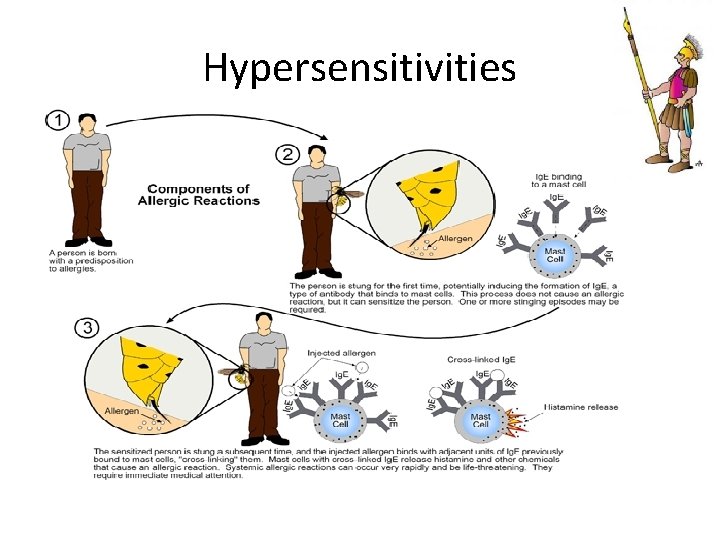
Hypersensitivities

Thank You!