IMMUNE SYSTEM FOR STUDENT COPY Key attributes of

IMMUNE SYSTEM FOR STUDENT COPY

Key attributes of immune system • 4 attributes that characterize the immune system as a whole – specificity • antigen-antibody specificity – diversity • react to millions of antigens – memory • rapid 2° response – ability to distinguish self vs. non-self • maturation & training process to reduce autoimmune disease

Immune System • must be able to identify nonself from self • detection determined by molecular recognition of receptor & cell-identity markers molecules

Innate Immunity • nonspecific defense that is active immediately upon infection • found in all animals & plants • includes: – outer covering • skin – chemical secretions • @ openings to interior of body – Mucous membranes – Sweat glands

Innate Immunity • defenses that body naturally has: – Skin – Secretions – Phagocytes – Natural killer cells

Barrier Defenses • epithelial tissues block entry of many pathogens – skin – mucous membranes • line organs that have opening to outside of body • mucus: viscous fluid that blocks microbes & other particles • saliva, tears have “washing” action keeping microbes from colonizing

Barrier Defenses • cellular secretions – lysozyme kills by breaking down cell walls – saliva, tears dilute & prevent colonization – sweat p. H 3 – 4 – stomach p. H 2

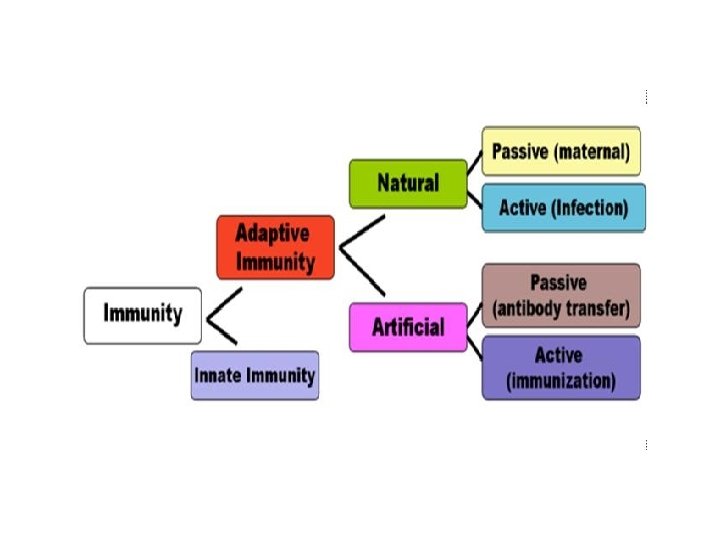
Adaptive Immunity • • found only in vertebrates very specific aka acquired immune response activated after innate responses & develops more slowly
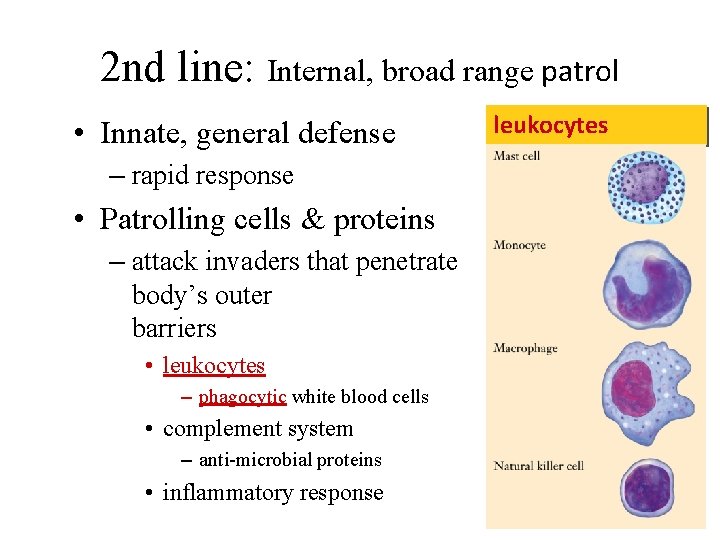
2 nd line: Internal, broad range patrol • Innate, general defense – rapid response • Patrolling cells & proteins – attack invaders that penetrate body’s outer barriers • leukocytes – phagocytic white blood cells • complement system – anti-microbial proteins • inflammatory response leukocytes

Internal Innate Defenses 1. phagocytes • cells that can detect fungi & bacteria then engulf them
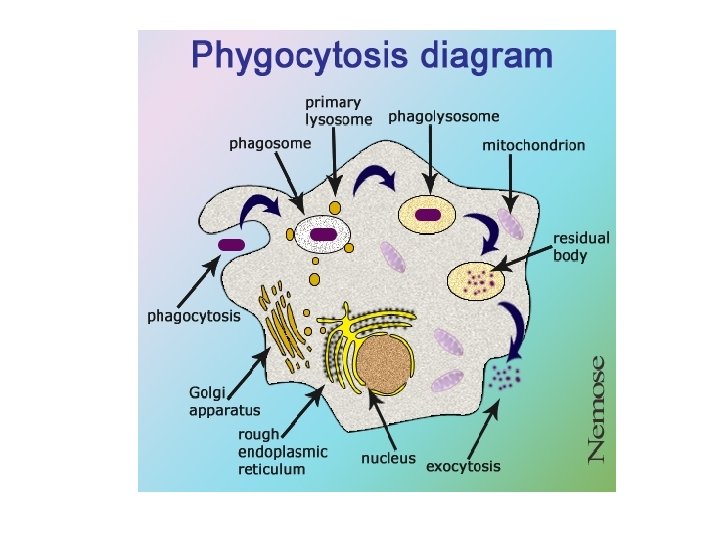

Types of Phagocytic Cells(#4) 1. Neutrophils – circulate in blood – attracted by signals sent from infected cells 2. Macrophages – larger cells migrate thru tissues or reside permanently in organs/tissues likely to have invaders

Types of Phagocytic Cells 3. Dendritic cells • mainly found in tissues with contact to outside (skin) – stimulate adaptive immunity after engulfing pathogen 4. Eosinophils – found beneath mucous membranes – low phagocytic activity – speciality: able to defend against parasitic worms secrete enzymes

Neutrophils ü 60 to 70 % of all WBCs üActive phagocytes üNumber increases rapidly during short term or acute infections
Eosinophils ü 2 to 4 % of all WBCs üIncrease during allergy attacks üReact to parasitic worms üInactivate some inflammatory chemicals
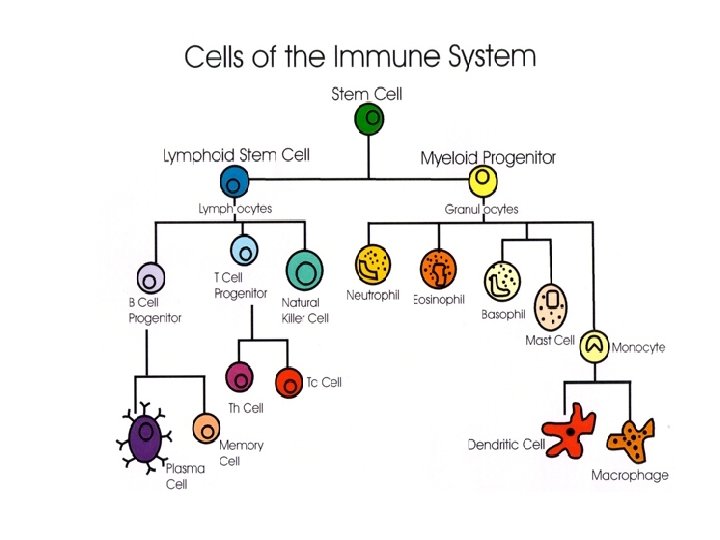

Lymphocytes ü 20 to 25 % of all WBCs üProvides Immunity (eg. Killer T-Cell) üProduces antibodies üNucleus fills most of the cell

Inflammatory Response • innate immune defense triggered by physical injury or infection of tissue involving the release of substances that promote swelling, enhance the infiltration of WBCs, & aid in tissue repair & destruction of invading pathogens
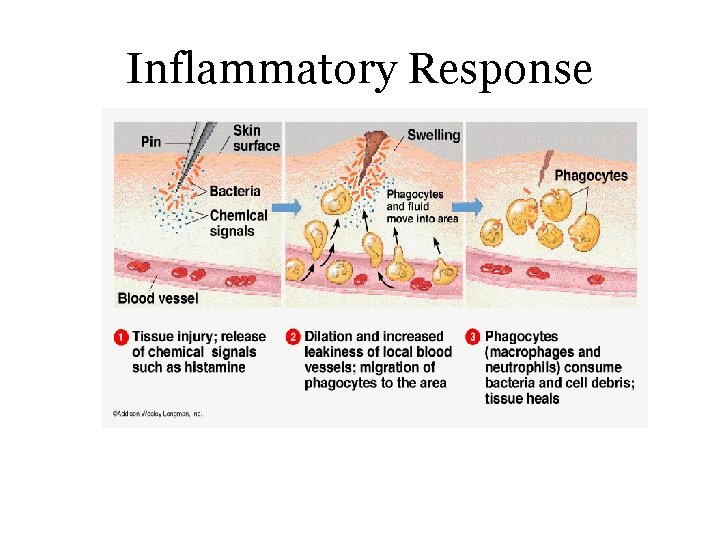
Inflammatory Response
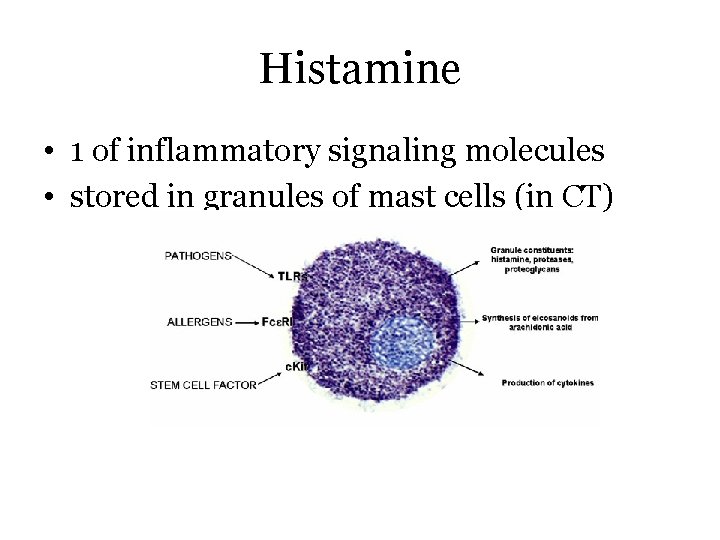
Histamine • 1 of inflammatory signaling molecules • stored in granules of mast cells (in CT)

Fever: Abnormally High Body Temperature • Hypothalamus normally set at 37°C. • Gram-negative endotoxin cause phagocytes to release interleukin– 1 (IL– 1). • Hypothalamus releases prostaglandins that reset the hypothalamus to a high temperature. • Body increases rate of metabolism and shivering which raise temperature. • When IL– 1 is eliminated, body temperature falls (crisis).

Fever • Advantages – Increase transferrins – Increase IL– 1 activity • Disadvantages – Tachycardia – Acidosis – Dehydration
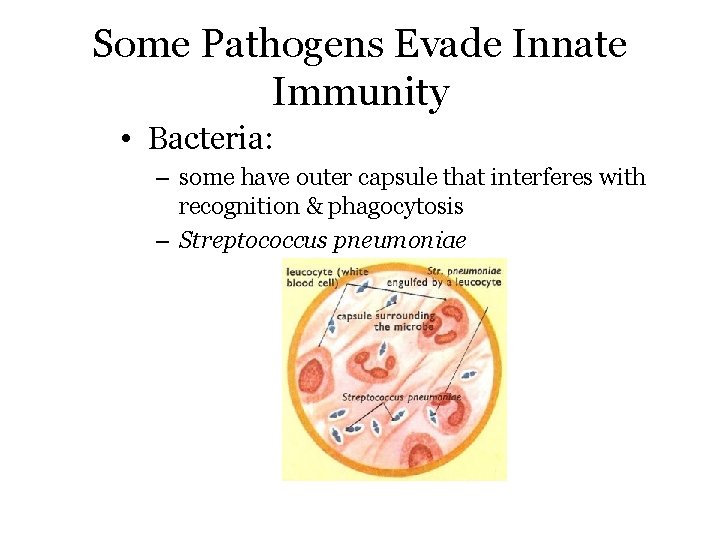
Some Pathogens Evade Innate Immunity • Bacteria: – some have outer capsule that interferes with recognition & phagocytosis – Streptococcus pneumoniae

Natural Killer Cells • circulate thru body detecting abnl surface proteins of cells infected with virus or cancer cells • on detection secrete chemicals that kill affected cell

Destroying cells gone bad! • Natural Killer Cells perforate cells – release perforin protein – insert into membrane of target cell – forms pore allowing fluid to flow into cell natural killer cell – cell ruptures (lysis) • apoptosis perforin punctures cell membrane vesicle cell membrane virus-infected cell
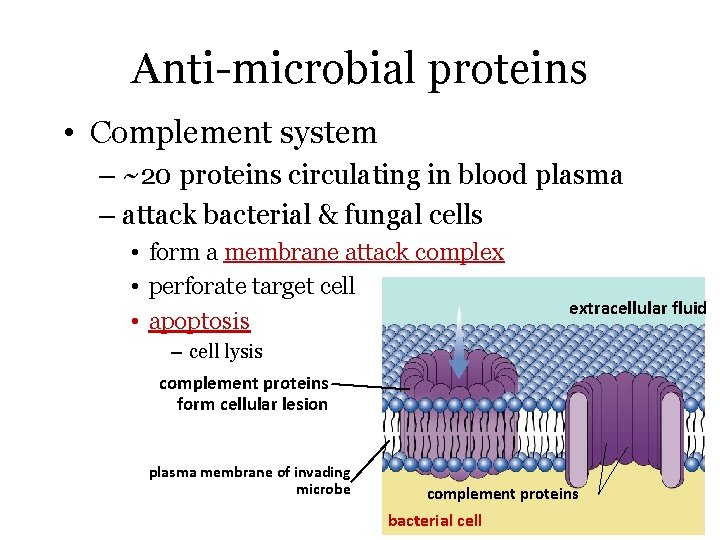
Anti-microbial proteins • Complement system – ~20 proteins circulating in blood plasma – attack bacterial & fungal cells • form a membrane attack complex • perforate target cell • apoptosis extracellular fluid – cell lysis complement proteins form cellular lesion plasma membrane of invading microbe complement proteins bacterial cell
3 rd line: Acquired (active) Immunity • Specific defense – lymphocytes • B lymphocytes (B cells) • T lymphocytes (T cells) – antibodies • immunoglobulins • Responds to… – antigens • specific pathogens • specific toxins • abnormal body cells (cancer)

4 Major Characteristics of Acquired Immunity 1. immense diversity of lymphocytes & receptors – enables immune system to detect pathogens never before encountered 2. adaptive immunity normally has “self” tolerance – arises as B cell matures

4 Major Characteristics of Adaptive Immunity 3. cell proliferation triggered by activation greatly increases the # of B and T cells 4. there is a stronger & more rapid response to agn previously encountered – immunological memory occurs after mature lymphocyte encounters & binds to a specific agn

How are invaders recognized: antigens • Antigens – proteins that serve as cellular name tags • foreign antigens cause response from WBCs – viruses, bacteria, protozoa, parasitic worms, fungi, toxins – non-pathogens: pollen & transplanted tissue • B cells & T cells respond to different antigens – B cells recognize intact antigens • pathogens in blood & lymph – T cells recognize antigen fragments • pathogens which have already infected cells “self” “foreign”

Thymus • organ in thoracic cavity • some new lymphocytes travel from bone marrow thymus & are “taught” how to respond in immune attack mature into T cells
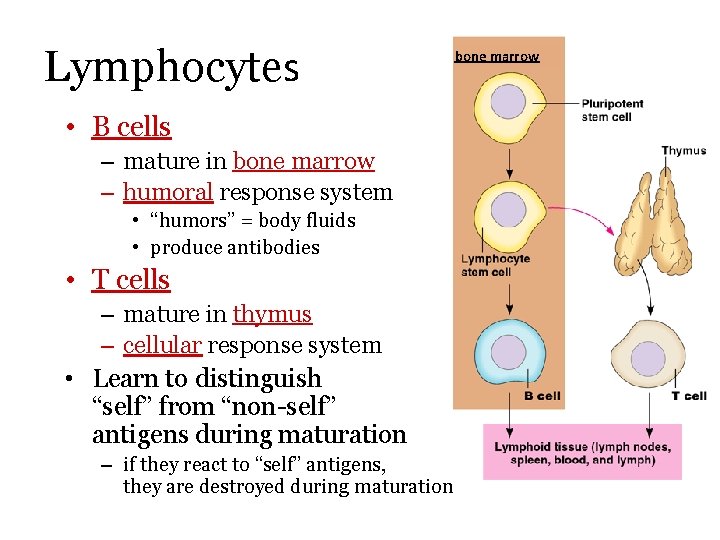
Lymphocytes • B cells – mature in bone marrow – humoral response system • “humors” = body fluids • produce antibodies • T cells – mature in thymus – cellular response system • Learn to distinguish “self” from “non-self” antigens during maturation – if they react to “self” antigens, they are destroyed during maturation bone marrow
B cells • Humoral response = “in fluid” – defense against attackers circulating freely in blood & lymph • Specific response – produce specific antibodies against specific antigen • Types of B cells • plasma cells – immediate production of antibodies – rapid response, short term release • memory cells – long term immunity
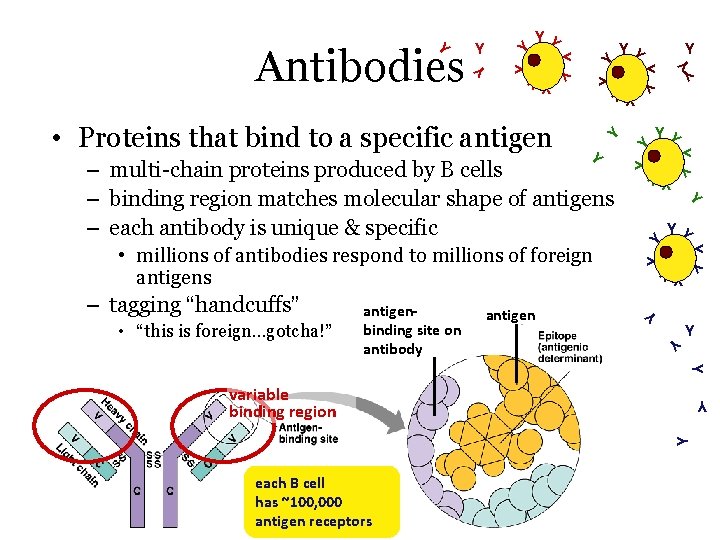
Y Y Y Y Y Y YY Y • “this is foreign…gotcha!” Y • millions of antibodies respond to millions of foreign antigens antigen Y Y Y – multi-chain proteins produced by B cells – binding region matches molecular shape of antigens – each antibody is unique & specific antigenbinding site on antibody YY YY • Proteins that bind to a specific antigen – tagging “handcuffs” Y Y Y Antibodies Y Y Y variable binding region Y Y each B cell has ~100, 000 antigen receptors
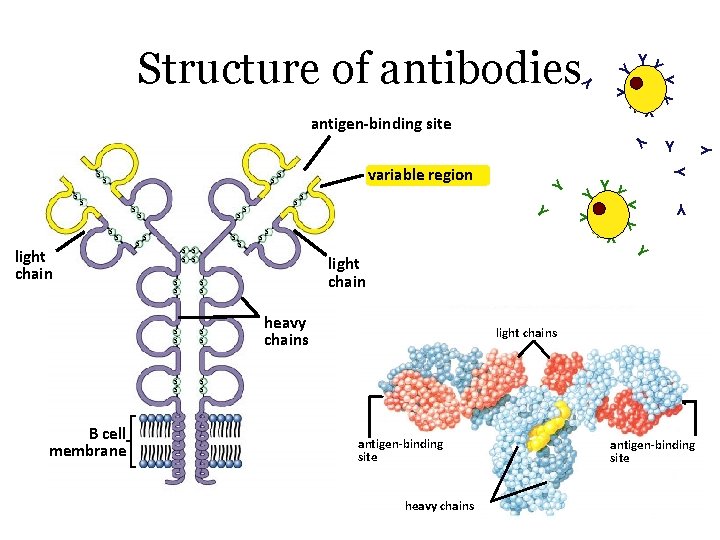
Structure of antibodies Y YY Y Y s B cell membrane s s s s s Y Y s s Y light chain s s Y Y s s YY s variable region s Y s s Y Y antigen-binding site light chain heavy chains light chains antigen-binding site heavy chains antigen-binding site
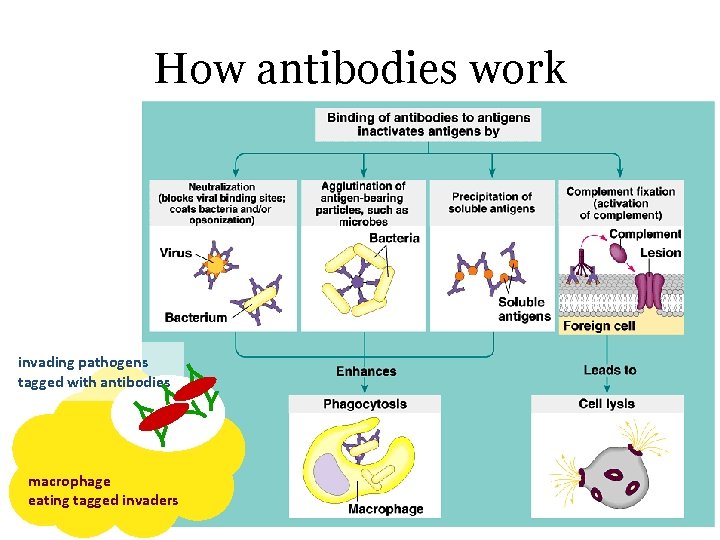
How antibodies work Y invading pathogens tagged with antibodies Y Y Y macrophage eating tagged invaders

B Cell Activation • starts when agn binds to a B cell agn receptor • ends with B cell secreting soluble form of its agn receptor = antibody (aby) or immunoglobulin (Ig) • abys have same “Y” shaped organization as the B cell agn receptor
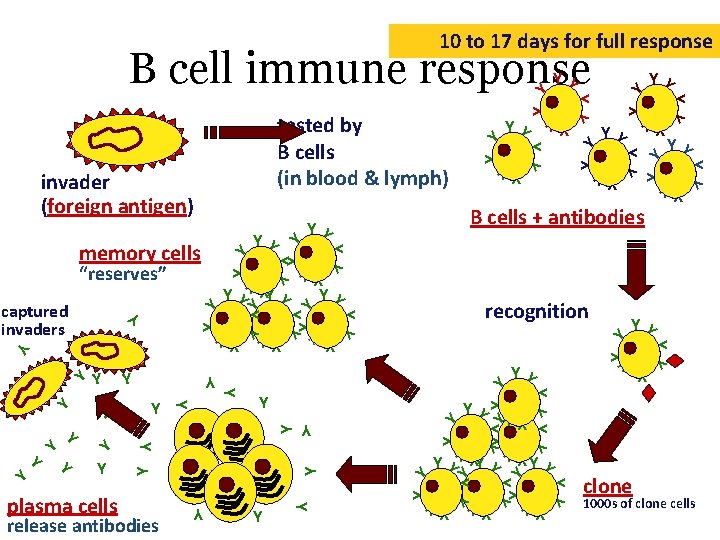
10 to 17 days for full response B cell immune response Y Y Y Y Y Y Y Y Y Y Y Y Y Y Y Y Y Y YY Y Y YY YY Y Y Y Y YY YY YY YY recognition Y Y release antibodies Y Y plasma cells YY Y Y YY Y Y captured invaders Y “reserves” Y B cells + antibodies Y Y memory cells Y Y invader (foreign antigen) Y tested by B cells (in blood & lymph) Y clone 1000 s of clone cells

Humoral Immunity B-Cells • Long Term Memory • B-Cells make antibodies which trigger a TCell reaction to kill the invader • Vaccines, Chicken Pox, Viral Infections Humoral Immunity (Go animation)

Types of Antibodies • Ig. G – major immunoglobulin in extra vascular spaces – crosses placenta • Ig. A – in secretions • Ig. M – 1 st immunoglobulin to be made by fetus – very good at clumping microorganisms

Types of Antibodies • Ig. D – mostly found on B cell surfaces • Ig. E – involved in allergic reactions – levels rise in helminthic parasitic infections (worms)

Antibody Function • do not kill pathogens • bind to agns inactivation or destruction

Immunological Memory • gives individual long term protection from an infection or vaccination • Primary Immune Response – produces effector cells from a clone of lymphocytes – peaks 10 -17 days after initial exposure
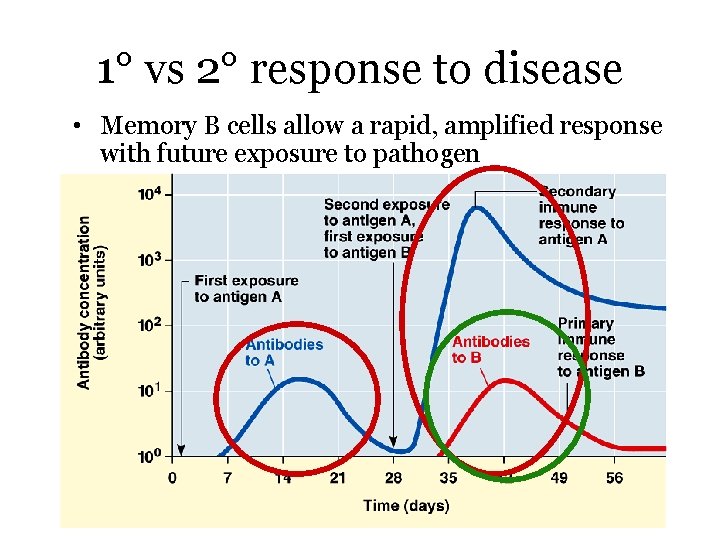
1° vs 2° response to disease • Memory B cells allow a rapid, amplified response with future exposure to pathogen
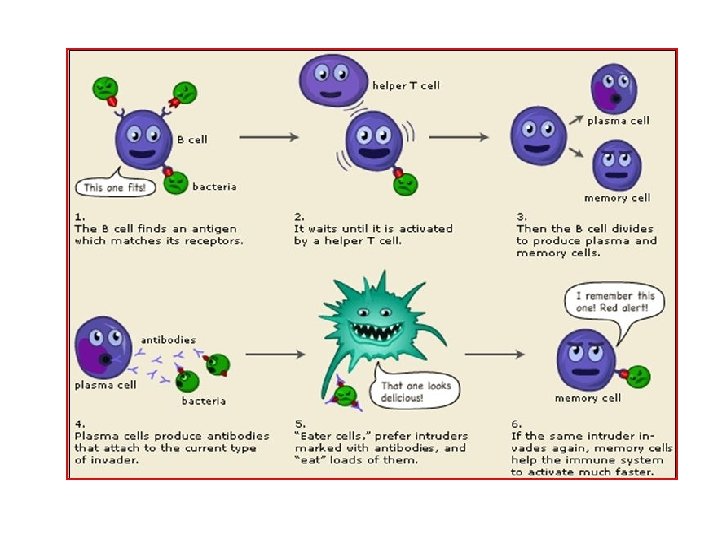
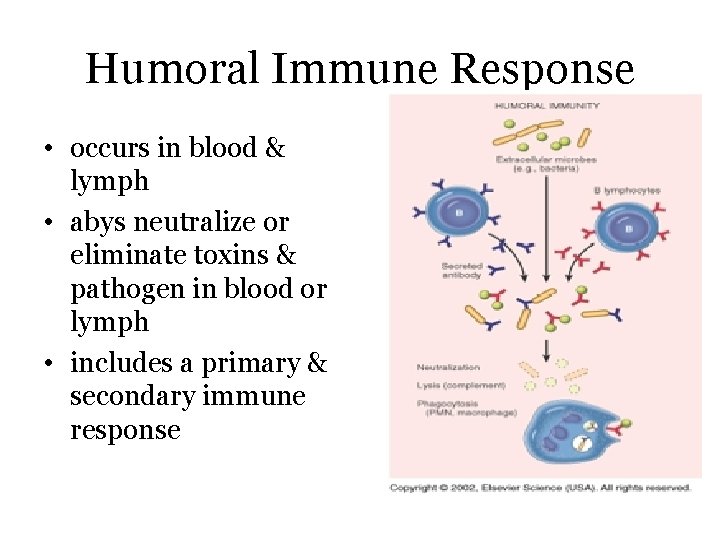
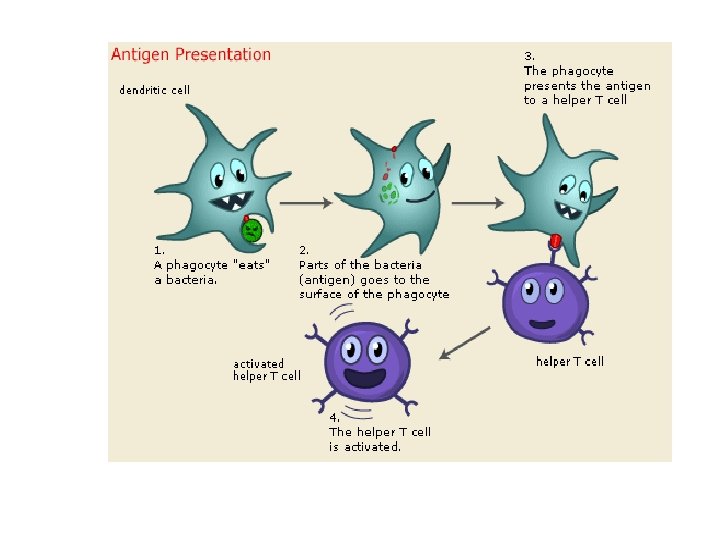
Humoral Immune Response • occurs in blood & lymph • abys neutralize or eliminate toxins & pathogen in blood or lymph • includes a primary & secondary immune response
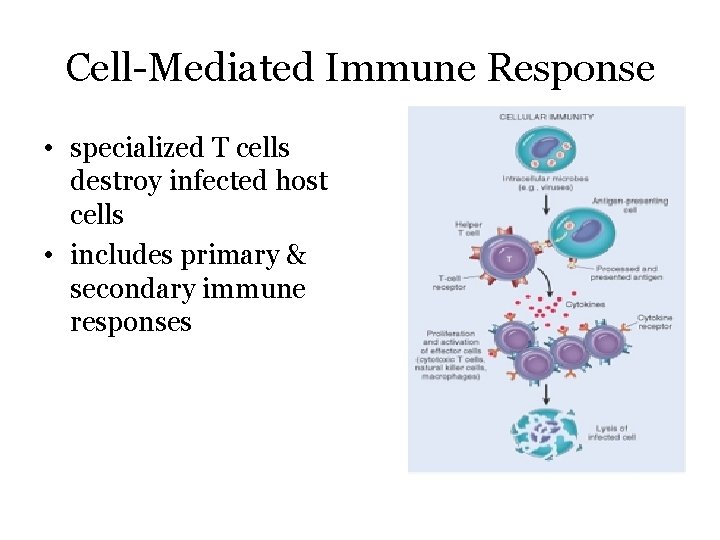
Cell-Mediated Immune Response • specialized T cells destroy infected host cells • includes primary & secondary immune responses
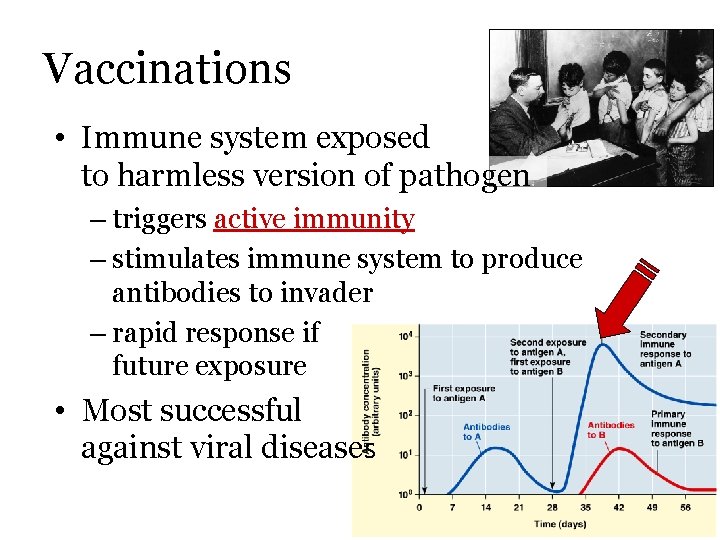
Vaccinations • Immune system exposed to harmless version of pathogen – triggers active immunity – stimulates immune system to produce antibodies to invader – rapid response if future exposure • Most successful against viral diseases

Jonas Salk April 12, 1955 • Developed first vaccine – against polio • attacks motor neurons Albert Sabin 1962 oral vaccine 1914 – 1995

Passive Immunity • Obtaining antibodies from another individual • Maternal immunity – antibodies pass from mother to baby across placenta or in mother’s milk – critical role of breastfeeding in infant health • mother is creating antibodies against pathogens baby is being exposed to • Injection – injection of antibodies – short-term immunity

Artificial Active Immunity • Immunizations: introduce agns to body abys develop giving immunity to person receiving vaccination • Jenner: took cowpox virus to induce adaptive immunity against small pox (closely related viruses)
Small Pox Vaccination

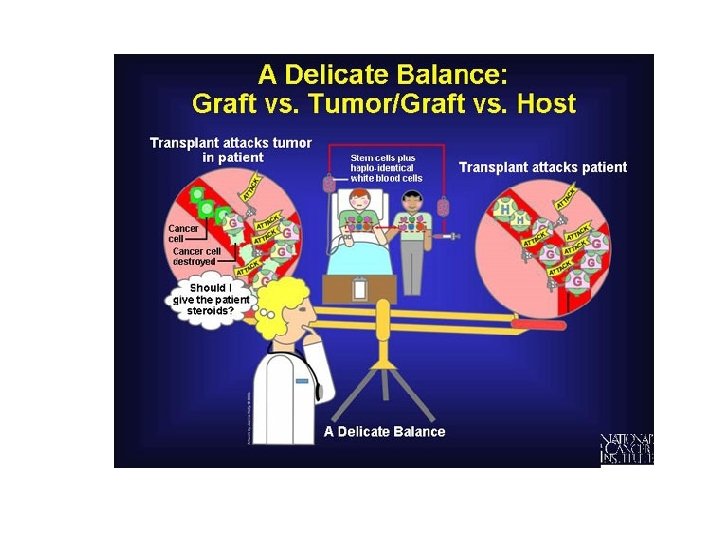
Tissue & Organ Transplants • MHC molecules stimulate the immune response that rejection • MHC molecules have many alleles and any 1 individual has many that vary in shape & charge • for most transplant recipients there will be some MHC molecules seen as foreign

Moon Face

Graft Versus Host Rejection • seen in bone marrow transplants • recipient’s bone marrow radiated b/4 to get rid of abnl cells also wipes out their immune system • lymphocytes in donor’s marrow react to “foreign” recipients tissues and cells
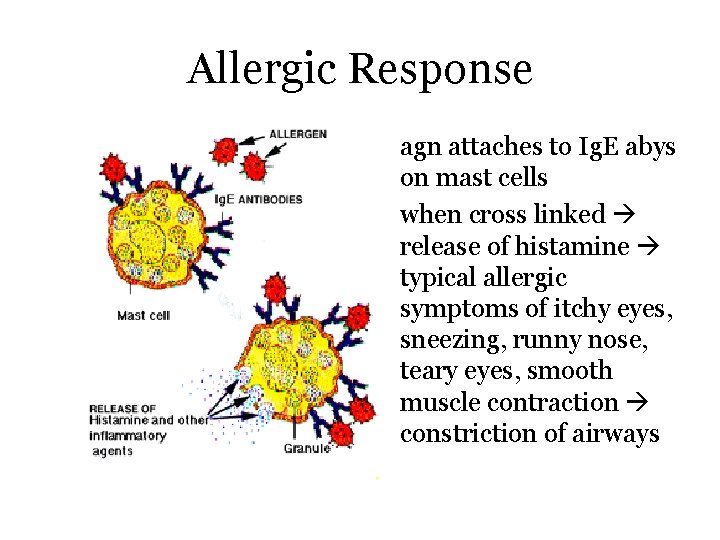
Allergic Response • agn attaches to Ig. E abys on mast cells • when cross linked release of histamine typical allergic symptoms of itchy eyes, sneezing, runny nose, teary eyes, smooth muscle contraction constriction of airways
What if the attacker gets past the B cells in the blood & actually infects some of your cells? You need trained assassins to kill off these infected cells! T Attack of the Killer T cells! 2007 -2008
T cells • Cell-mediated response – immune response to infected cells • viruses, bacteria & parasites (pathogens) within cells – defense against “non-self” cells • cancer & transplant cells • Types of T cells – helper T cells • alerts immune system – killer (cytotoxic) T cells • attack infected body cells
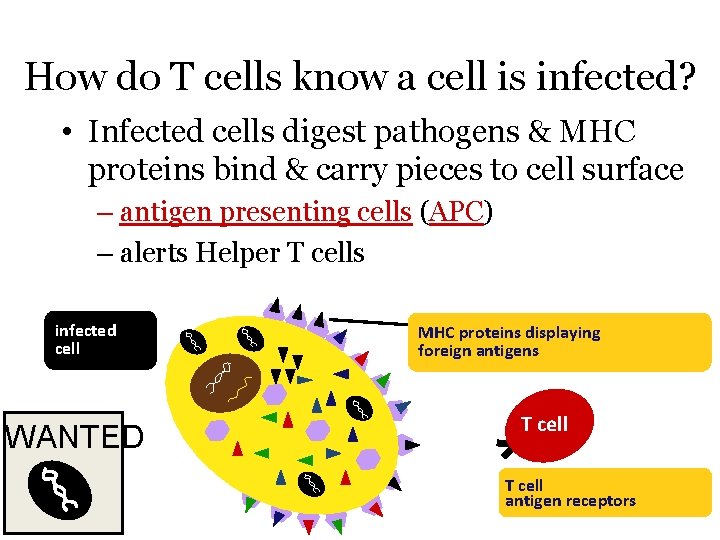
How do T cells know a cell is infected? • Infected cells digest pathogens & MHC proteins bind & carry pieces to cell surface – antigen presenting cells (APC) – alerts Helper T cells infected cell WANTED MHC proteins displaying foreign antigens T cell antigen receptors

Cytotoxic T Cells • in cell-mediated immune response • role: effector cells – synthesize toxic gene products that kill infected cells • activated by signaling molecules from helper T cells + interaction with APC
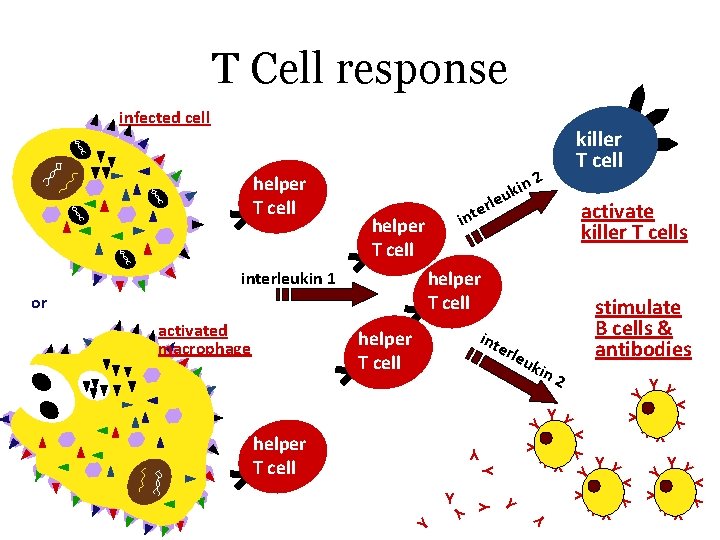
T Cell response infected cell activate killer T cells helper T cell rle uki n 2 Y Y YY Y Y YY helper T cell Y Y Y int e helper T cell stimulate B cells & antibodies Y Y or Y Y i helper T cell interleukin 1 activated macrophage eu rl nte 2 n i k Y helper T cell killer T cell
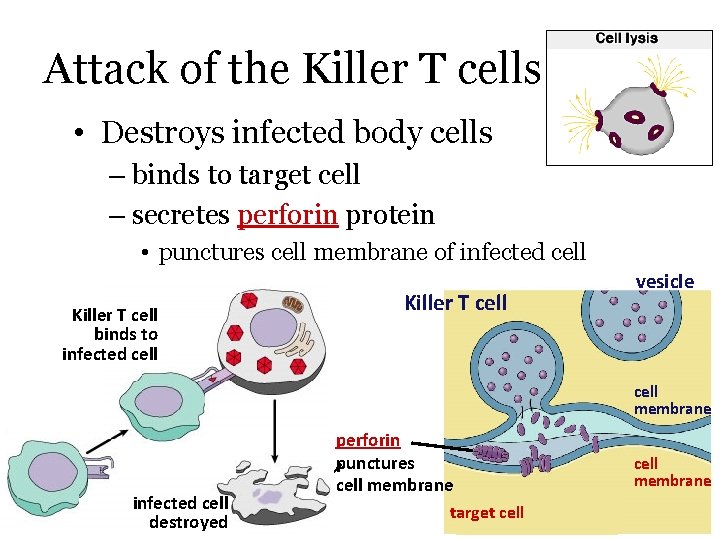
Attack of the Killer T cells • Destroys infected body cells – binds to target cell – secretes perforin protein • punctures cell membrane of infected cell Killer T cell binds to infected cell Killer T cell vesicle cell membrane infected cell destroyed perforin punctures cell membrane target cell membrane

HIV & AIDS • Human Immunodeficiency Virus – virus infects helper T cells – helper T cells don’t activate rest of immune system: T cells & B cells • also destroy T cells • Acquired Immuno. Deficiency Syndrome – infections by opportunistic diseases – death usually from other infections • pneumonia, cancer

How to protect yourself…

Immune system malfunctions • Auto-immune diseases – immune system attacks own molecules & cells • lupus – antibodies against many molecules released by normal breakdown of cells • rheumatoid arthritis – antibodies causing damage to cartilage & bone • diabetes – beta-islet cells of pancreas attacked & destroyed • multiple sclerosis – T cells attack myelin sheath of brain & spinal cord nerves • Allergies – over-reaction to environmental antigens • allergens = proteins on pollen, dust mites, in animal saliva • stimulates release of histamine

Allergies • exaggerated hypersensitivity reactions to allergens: agn that triggers exaggerated immune response • most involve aby of Ig. E class • example: – hayfever • agn on surface of pollen grains
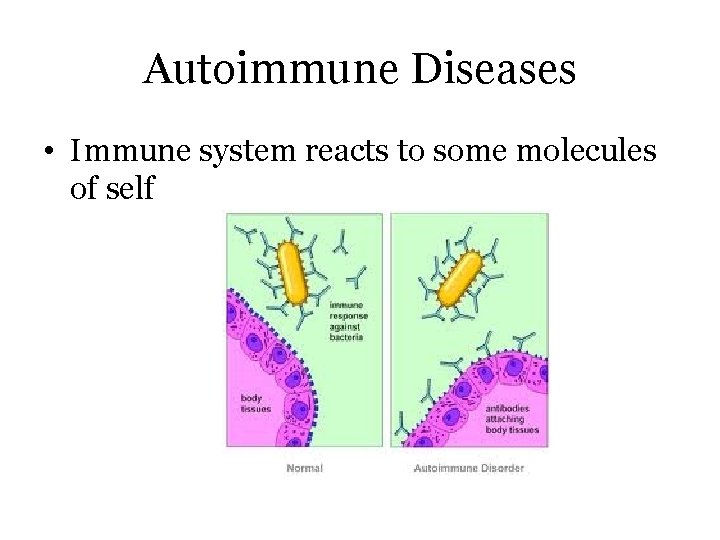
Autoimmune Diseases • Immune system reacts to some molecules of self

Stress & the Immune System • psychological stress disrupts immune system by altering interplay of the nervous system endocrine system & immune system • rest important for immunity – adults with < 7 hrs sleep/nite : 3 x more likely to get sick when exposed to cold virus as those who average 8 hrs sleep/nite

Lymphatic System • network of vessels that connect lymphatic tissues thru out body – ECF lymph vessels lymph nodes lymph vessels venous drainage • some macrophages in lymph nodes
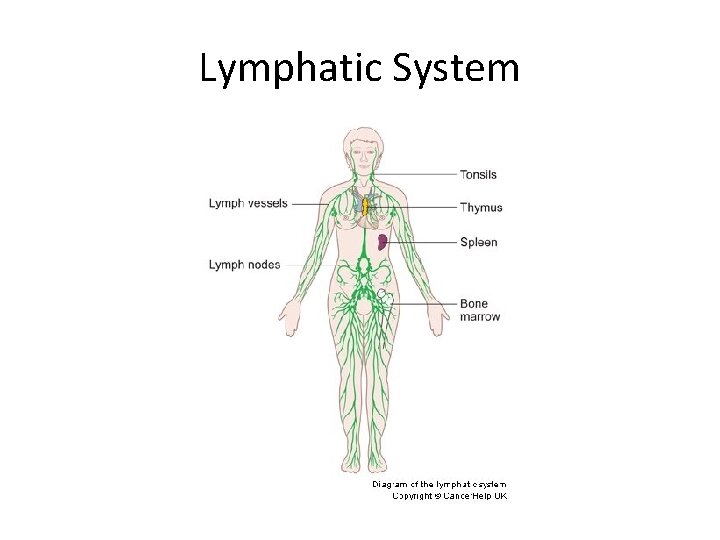
Lymphatic System
- Slides: 73