Immediate Antiretroviral Therapy for Better Patient Health and

Immediate Antiretroviral Therapy for Better Patient Health and HIV Prevention Oliver Bacon, MD, MPH 2 February 2016

Disclaimer Views expressed in this talk do not necessarily reflect those of the San Francisco Department of Public Health or UCSF

Getting to Zero San Francisco: The Power of Collective Impact—and guided by data By 2020: 90% fewer HIV infections 90% fewer HIV deaths Zero stigma and discrimination
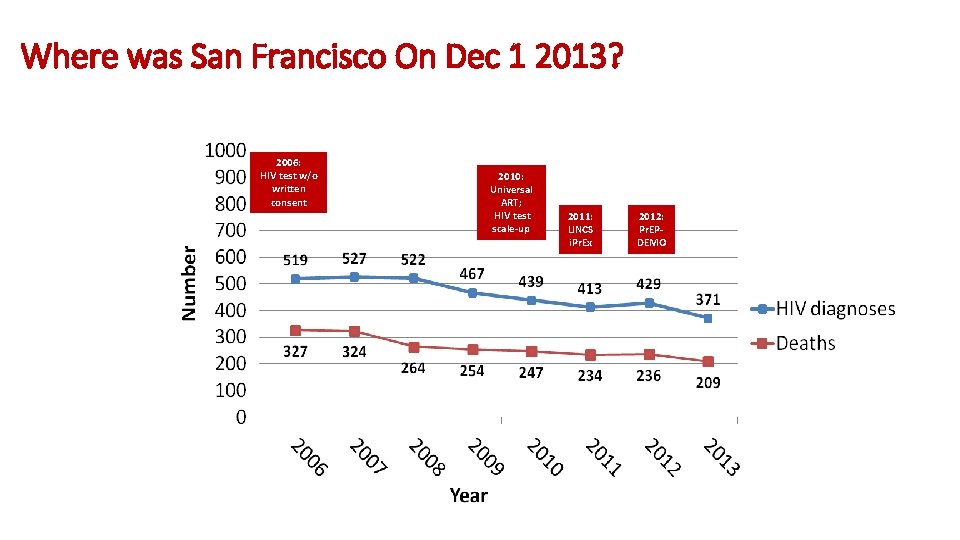
Where was San Francisco On Dec 1 2013? 2006: HIV test w/o written consent 2010: Universal ART; HIV test scale-up 2011: LINCS i. Pr. Ex 2012: Pr. EPDEMO
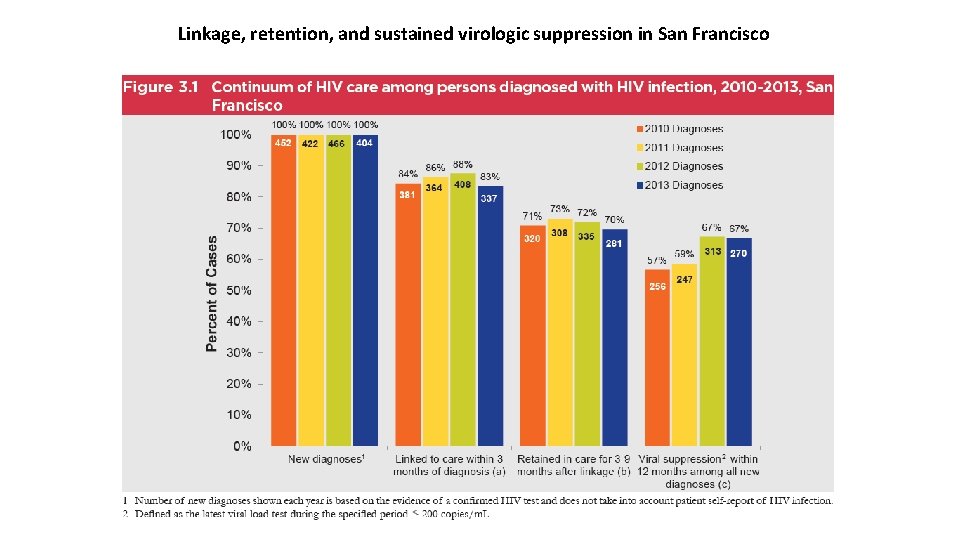
Linkage, retention, and sustained virologic suppression in San Francisco

Demographics of the 306 New HIV Infections in SF in 2014 HIV Infections by Race/Ethnicity: 2014 HIV Infections by Transmission Category: 2014 Race/Ethnicity Transmission Category No. (%) White 135 (44. 1) African American 33 (10. 8) Latino 85 API/NA Multiple Races No. (%) MSM 231 (75. 5) IDU 20 (27. 8) MSM IDU 33 (10. 8) 40 (13. 1) Heterosexual 8 (2. 6) 13 (4. 2) TFN/Hemophilia 0 (0) Perinatal 0 (0) 14 (4. 6) Other/Unknown HIV Semi-Annual Surveillance Report, SFDPH, June 2015 (6. 5)

Data Highlight the Gaps • If the goal is virologic suppression, 67% is insufficient • Need better, faster Linkage • Need better Retention • Need something to prevent HIV(-)s from getting infected by unknown HIV (+)s • Need to decrease stigma, psychosocioeconomic discrimination as a barrier to care, prevention

Strategic Plan: Signature Initiatives • Pr. EP: Expand access to pre-exposure prophylaxis for San Franciscans at-risk for HIV infection • RAPID ART: Early diagnosis, with immediate linkage to care and treatment of HIV • RETENTION in HIV care • STIGMA reduction interventions Committee for each initiative is developing action plan, metrics and milestones, budget

Universal ART…………Faster • Delivering ART as early as possible after a new diagnosis of HIV: • improves morbidity and mortality in all stages of infection (START Trial 2015) • reduces transmission by 96% (HPTN 052 2011) • in acute HIV infection: limits reservoirs and hyper-infectivity • Typical interval of weeks to months between diagnosis, ART, and virologic suppression=lost opportunities • Delayed or dropped linkage, retention • Immunologic dysfunction • Onward Transmission Why can’t ART be started at diagnosis?
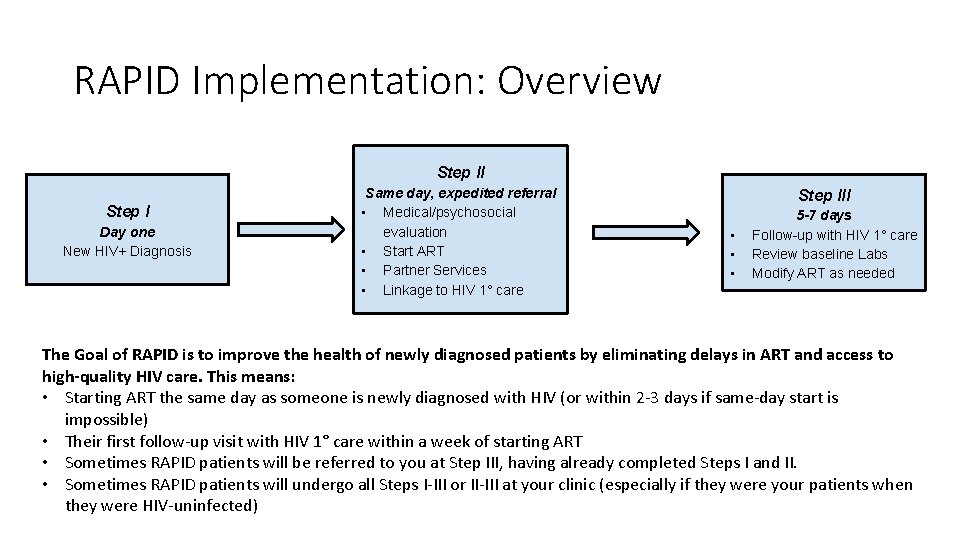
RAPID Implementation: Overview Step II Step I Day one New HIV+ Diagnosis Same day, expedited referral • Medical/psychosocial evaluation • Start ART • Partner Services • Linkage to HIV 1° care Step III • • • 5 -7 days Follow-up with HIV 1° care Review baseline Labs Modify ART as needed The Goal of RAPID is to improve the health of newly diagnosed patients by eliminating delays in ART and access to high-quality HIV care. This means: • Starting ART the same day as someone is newly diagnosed with HIV (or within 2 -3 days if same-day start is impossible) • Their first follow-up visit with HIV 1° care within a week of starting ART • Sometimes RAPID patients will be referred to you at Step III, having already completed Steps I and II. • Sometimes RAPID patients will undergo all Steps I-III or II-III at your clinic (especially if they were your patients when they were HIV-uninfected)

RAPID Pilot at SFGH: 2013 -15 • PHAST Team paged with any new confirmed new HIV+ patients on SFGH campus • PHAST Team paged by testing sites in SF with any new HIV+ with no/public insurance • Expedited intake at Ward 86 (UCSF HIV Clinic at SFGH) • Comparison of linkage, virologic outcomes, by era: • CD 4 -guided ART • Universal ART • RAPID (immediate ART)
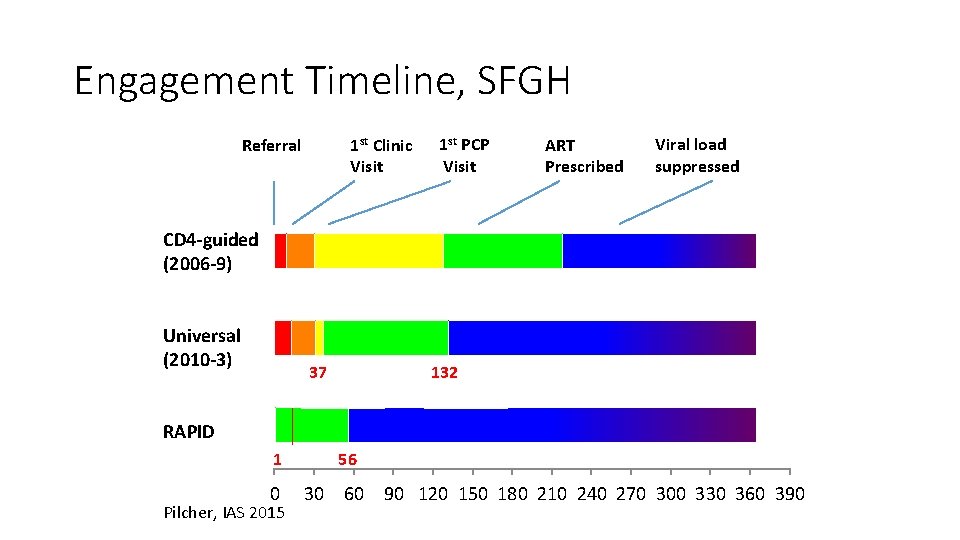
Engagement Timeline, SFGH 1 st Clinic Visit Referral 1 st PCP Visit ART Prescribed Viral load suppressed CD 4 -guided (2006 -9) Universal (2010 -3) 37 132 RAPID 1 0 Pilcher, IAS 2015 56 30 60 90 120 150 180 210 240 270 300 330 360 390
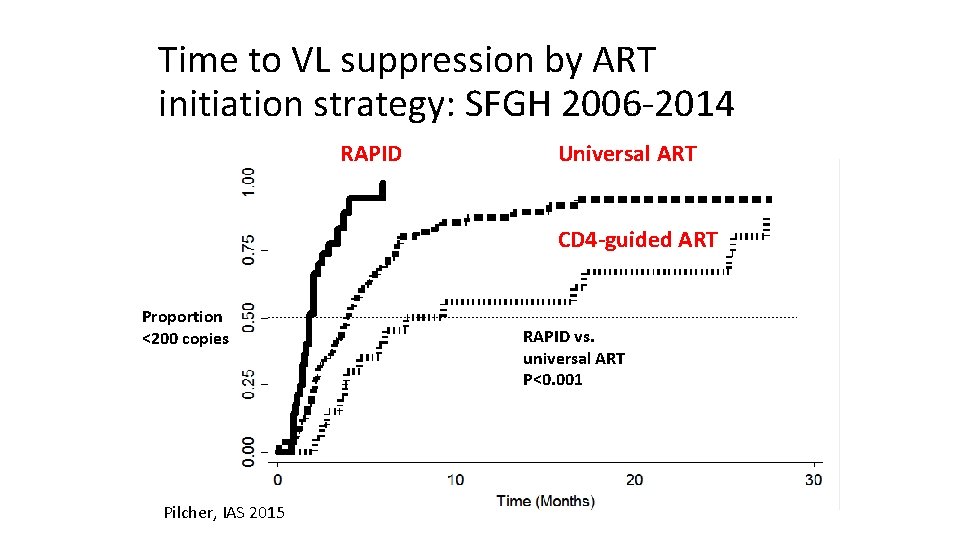
Time to VL suppression by ART initiation strategy: SFGH 2006 -2014 RAPID Universal ART CD 4 -guided ART Proportion <200 copies Pilcher, IAS 2015 RAPID vs. universal ART P<0. 001

Qualitative Lessons from Interviews with RAPID Pilot Team Members: Keys to Success 1. 2. 3. 4. 5. Single point-of-contact for referrals activates the team (PHAST Pager) Committed team is essential (Counseling, Benefits Navigation, Clinical) Minimize handoffs: Every handoff is a warm handoff Talk about Care first, Insurance later Have a plan for medication access • Emergency ADAP • Presumptive Medi-Cal • Pharma Patient Assistance Cards 6. Check in with patient in the 1 -2 days after he/she leaves the appointment

Taking ART Citywide • Develop a RAPID Protocol • Develop a capacity-building strategy • Clinic-wide education Sessions • Public Health Detailing of Individual Clinicians, with RAPID Guide for Providers • Target High Prevalence Testing Sites • Target HIV Clinics where newly HIV+ persons are linked (referral sites) • Develop an Evaluation Plan
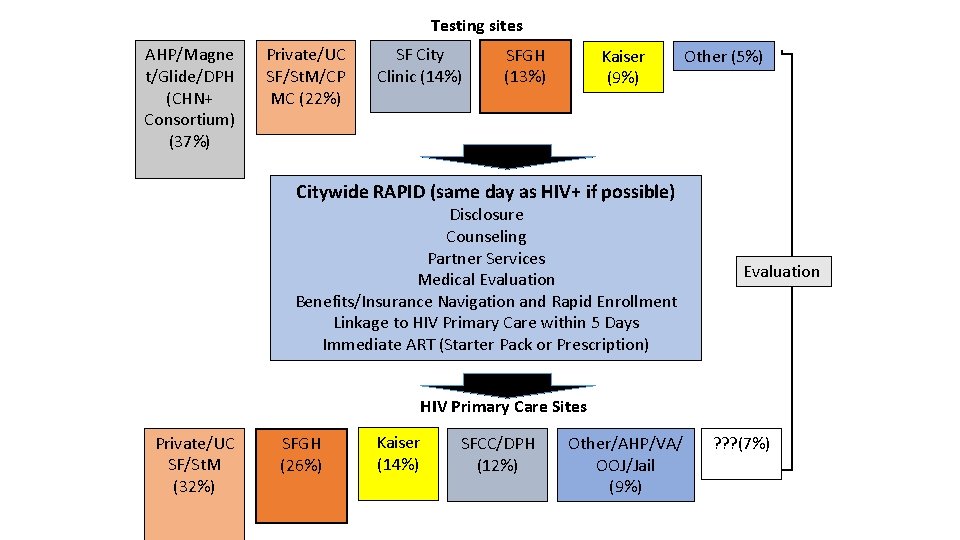
Testing sites AHP/Magne t/Glide/DPH (CHN+ Consortium) (37%) Private/UC SF/St. M/CP MC (22%) SF City Clinic (14%) SFGH (13%) Kaiser (9%) Other (5%) Citywide RAPID (same day as HIV+ if possible) Disclosure Counseling Partner Services Medical Evaluation Benefits/Insurance Navigation and Rapid Enrollment Linkage to HIV Primary Care within 5 Days Immediate ART (Starter Pack or Prescription) Evaluation HIV Primary Care Sites Private/UC SF/St. M (32%) SFGH (26%) Kaiser (14%) SFCC/DPH (12%) Other/AHP/VA/ OOJ/Jail (9%) ? ? ? (7%)
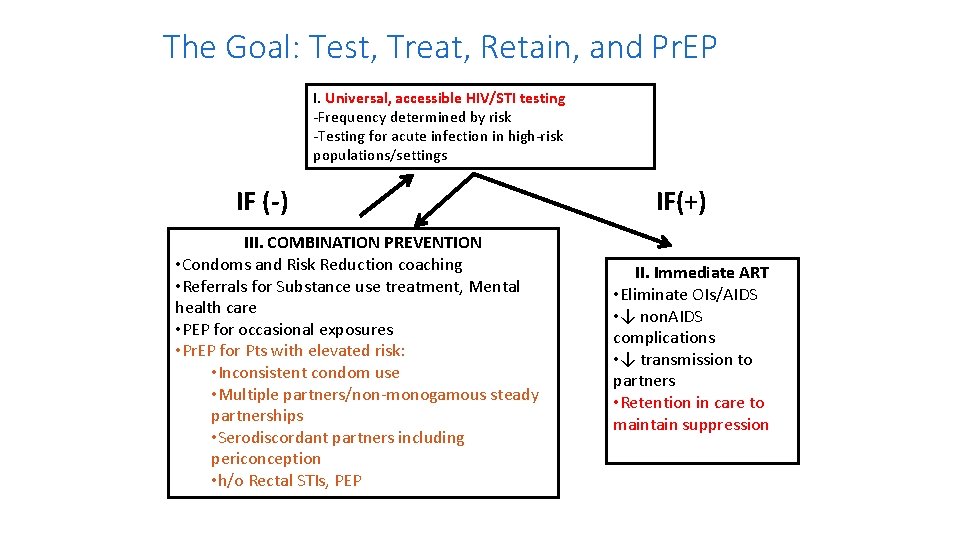
The Goal: Test, Treat, Retain, and Pr. EP I. Universal, accessible HIV/STI testing -Frequency determined by risk -Testing for acute infection in high-risk populations/settings IF (-) III. COMBINATION PREVENTION • Condoms and Risk Reduction coaching • Referrals for Substance use treatment, Mental health care • PEP for occasional exposures • Pr. EP for Pts with elevated risk: • Inconsistent condom use • Multiple partners/non-monogamous steady partnerships • Serodiscordant partners including periconception • h/o Rectal STIs, PEP IF(+) II. Immediate ART • Eliminate OIs/AIDS • ↓ non. AIDS complications • ↓ transmission to partners • Retention in care to maintain suppression

Acknowledgments • G 2 Z Rapid Committee • • Diane Havlir Diane Jones Stephanie Cohen Chris Pilcher Hiroyu Hatano Susa Coffey Tim Patriarca Janet Grochowski • G 2 Z Steering Committee • Shannon Weber • PHAST • Clarissa Ospina-Norvell • Sandra Torres • Fabi Calderon • Kaiser-SF • Brad Hare • Marc Solomon • Ed Chitty • SFDPH • • Jonathan Fuchs Darpun Sachdev Andy Scheer Susan Scheer
- Slides: 18