IMI Assessment Class Brian John Piccolo BA MA

IMI: Assessment Class Brian John Piccolo, BA, MA, NCTMB Updated 05/06/2010 IMI

Contents Part 1: Value of Assessment Part 2: What to Assess Part 3. Class Room Activities IMI: Assessment Class IMI

Part-1 The Value of Assessment IMI

Part-2 Provides a Baseline 1. Provides a baseline from which to judge progress. 2. What is your pain level today? 3. What was your pain level yesterday? 4. Is there numbness or pain down your arms or legs? 5. Is the pain greater on the right or on the left? Value of Assessment

Part-2 Effectiveness of Treatment 1. Provides a way to determine the effectiveness of treatment. 2. What therapies has the patient had in the past? Did anything work or not? 3. Is what you did as a therapist last time accomplish anything or not? 4. Was trigger point therapy effective last time or was myofascial release better? Value of Assessment

Part-2 Safe and Effective 1. Provides for the development of a safe and effective treatment. 2. If a client has a fusion in their spine then distraction of their spine is contraindicated. 3. If a client has disk degeneration disease then traction of the spine is beneficial. 4. Accurate assessments dictate procedures in a safe manner. Value of Assessment

Part-2 Soap Notes & History Value of Assessment

Part-2 Treat the Cause 1. Provides treatment for the cause of the client’s problem. 2. Chasing pain does not provide long-term relief for the client. 3. The cause of the pain must be understood through the assessment process. 4. Is the clients pain sharp from a nerve root or a dull ache from a ligament? Value of Assessment
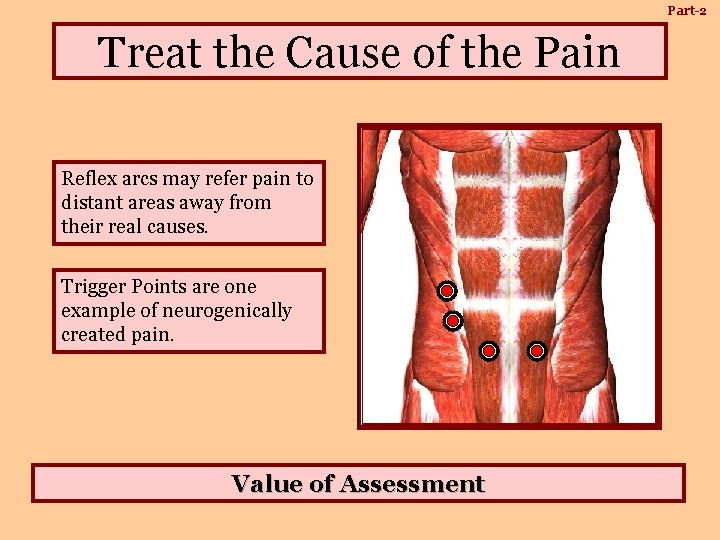
Part-2 Treat the Cause of the Pain Reflex arcs may refer pain to distant areas away from their real causes. Trigger Points are one example of neurogenically created pain. Value of Assessment

Part-2 Basis for Communication 1. Provides a basis of communication (with permission) with other healthcare professionals. 2. Knowing our scope of limitation and practice is a sign of a good therapist. 3. There is a time to send your client to a D. O. of a D. C. for high velocity manipulations. 4. Keep a file of business cards of other professionals on hand. Value of Assessment

Part-2 Client Education 1. Provides a basis for communication with the client so they can better understand their problem? 2. Informed clients do their homework. 3. Informed clients show up more regularly for therapy because they understand its benefits. 4. Rehabilitation is always important in a clients recovery from physical trauma. Value of Assessment
Part-2 What to Assess IMI

Part-3 Client’s Health History 1. Clients condition via a Health History. 2. Have they had any operations in the last three months? If so, what kind? 3. Do they have a heart condition? 4. What medicines are they currently taking? 5. Have they had a hip or knee replacement or a lumbar vertebrae fusion operation? What to Assess

Part-3 Client’s Chief Complaint 1. What is the clients chief complaint? 2. Does the client have numbness, short of breath, shooting pain? 3. Is there numbness in the both hands? What makes it better or worse? 4. When does the pain hurt most, AM or PM or when standing too long? 5. Is the condition Chronic or Acute? 6. Is the client depressed psychologically? What to Assess

Part-3 Therapist Observation 1. How is the clients posture? 2. Do they have uneven shoulders? 3. How do they walk, pigeon toed or like a duck? 4. Do they have a head forward posture? Is the neck or head too far forward? 5. What is the condition of their skin? 6. Are their shoes’ heels worn out on the lateral posterior corner? What to Assess
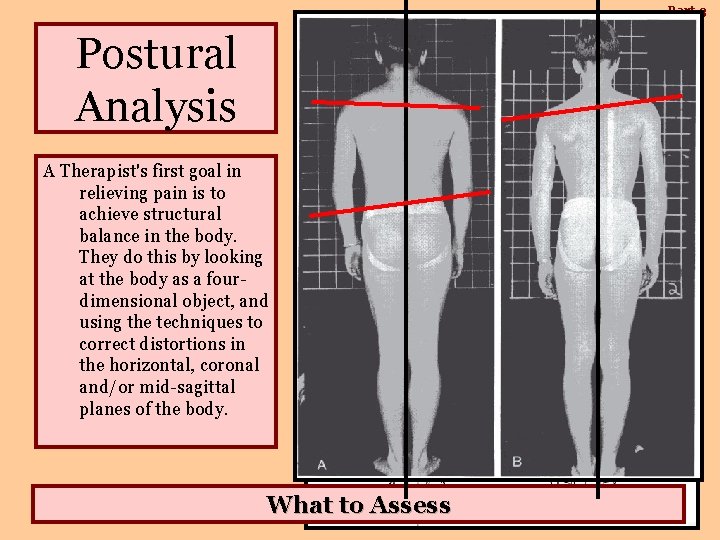
Part-3 Postural Analysis A Therapist's first goal in relieving pain is to achieve structural balance in the body. They do this by looking at the body as a fourdimensional object, and using the techniques to correct distortions in the horizontal, coronal and/or mid-sagittal planes of the body. What to Assess

Part-3 Therapist Palpitation 1. Is there tenderness or pain? 2. Is there swelling or edema? 3. Is there differences in heat or cold? 4. Are there any trigger points to release? 5. Are there any energy blocks in their energy field or structure? 6. Does their fascia feel tight in some areas more than others when skin rolling? What to Assess
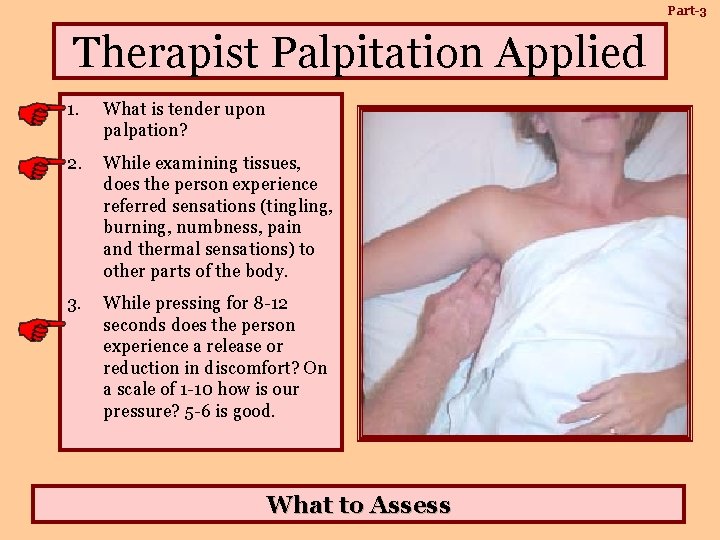
Part-3 Therapist Palpitation Applied 1. What is tender upon palpation? 2. While examining tissues, does the person experience referred sensations (tingling, burning, numbness, pain and thermal sensations) to other parts of the body. 3. While pressing for 8 -12 seconds does the person experience a release or reduction in discomfort? On a scale of 1 -10 how is our pressure? 5 -6 is good. What to Assess

Part-3 Functional Ability & Tests 1. Do they feel restricted in their everyday functions, work, recreation? 2. Do they have limited endurance, or tire easily? 3. Do they have limited Range of Motion? 4. What is their strength level? 5. What special orthopedic test can we do to ascertain more precise knowledge? (Clinical Massage Therapy, pages 1061 -1127) What to Assess
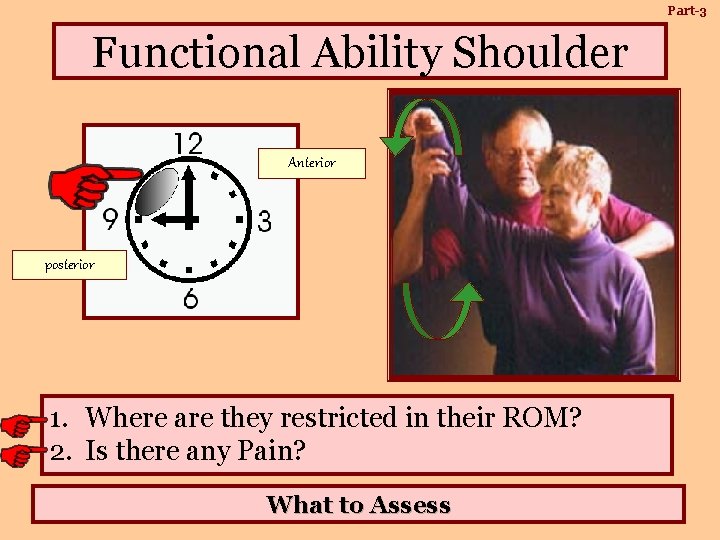
Part-3 Functional Ability Shoulder Anterior posterior 1. Where are they restricted in their ROM? 2. Is there any Pain? What to Assess

Part-3 Contraindications 1. 2. 3. 4. 5. 6. 7. 8. Are there contagious or infectious problems? Do they have Cancer? Do they have acute inflammation? Do they have a fever? Do they have an aneurysm or osteoporosis? Do they have varicose veins? Do you need a Doctor’s approval to proceed? When in doubt, do without! Do no harm! (Clinical Massage Therapy, pages 147 -154) What to Assess

Part-3 Referral Sources 1. Chiropractor: for high velocity spinal adjustments. 2. Osteopath: for more sophisticated manipulations of the body. 3. Physical Therapist: for rehabilitation work and rebuilding of atrophied muscles. 4. Medical Doctor: for general diagnosis and Rx. 5. Homeopath or Nutritionist: for allergies and etc. 6. Psychologist: for emotional needs, depression. What to Assess

Part-3 Class Room Activities IMI

Part-4 Case Studies 1. Put the students in to 5 groups. 2. Each group gets one Case Study only. 3. Each student gets a Case Study form to be completed working as a group (45 min). 4. Each Group will present their assessment findings to the class (about 5’ each group). 5. Next divide the class into groups of 2 only and let them treat each other according to the findings in their assessment (1. 5 hours). 6. Gather for last 10’ for group feedback. Classroom Activities

Part-4 Five Case Studies Group 1: Shoulder Impingement (p. 457). Group 2: Planter Fasciitis (p. 417). Group 3: Thoracic Outlet Syndrome (p. 825). Group 4: Osteoarthritis Knee (p. 637). Group 5: Herniated/Degenerative Disk (p. 617). Classroom Activities
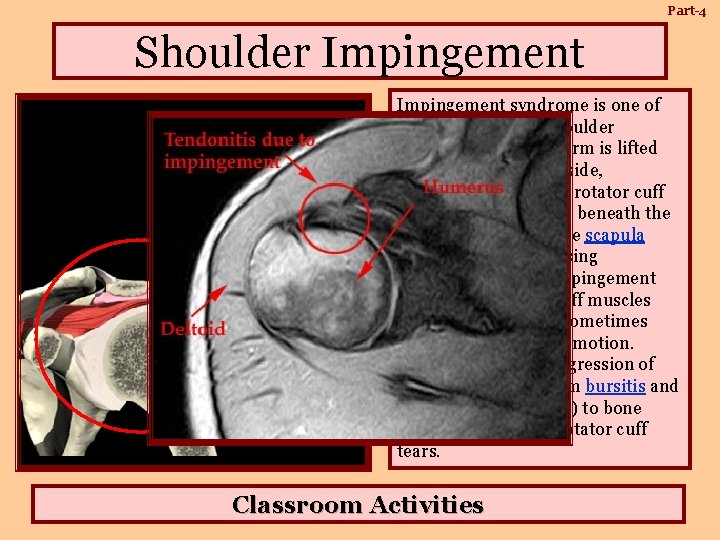
Part-4 Shoulder Impingement syndrome is one of the most common shoulder problems. When the arm is lifted forward or out to the side, structures such as the rotator cuff and bursa get pinched beneath the acromial process of the scapula (shoulder blade), causing inflammation. The impingement pinches the rotator cuff muscles and causes pain and sometimes weakness and limited motion. Impingement is a progression of problems ranging from bursitis and tendonitis (tendinosis) to bone spurs and complete rotator cuff tears. Classroom Activities
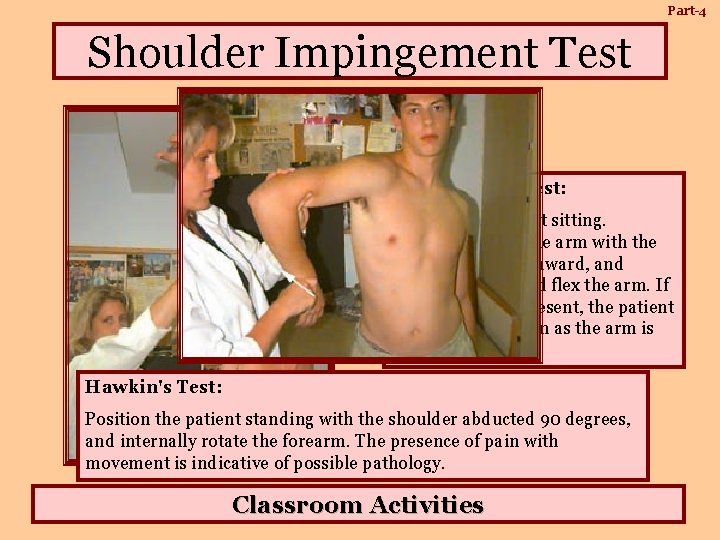
Part-4 Shoulder Impingement Test: Position the patient sitting. Internally rotate the arm with the thumb facing downward, and abduct and forward flex the arm. If impingement is present, the patient will experience pain as the arm is abducted. Hawkin's Test: Position the patient standing with the shoulder abducted 90 degrees, and internally rotate the forearm. The presence of pain with movement is indicative of possible pathology. Classroom Activities

Part-4 Shoulder Impingement Signs and Symptoms: There is a slow restriction of movement of the arm to the point of affecting daily activities such as combing the hair. The patient finds it difficult to abduct and flex the arm and has difficulty in moving the arm back. There is a limit in external rotation, abduction, flexion and internal rotation. Risk Factors: This condition is more common in women over 50 years of age. Recommendations to Therapist: In Acute frozen shoulder, ice or superficial heat reduces pain and muscle guarding. Use capsular stretching procedures with the client's arm hanging over the side of the table. In chronic stage, the aim is to stretch the capsule-especially the anterior-inferior area. Work in conjunction with physical therapist and encourage the client to do stretches. Classroom Activities
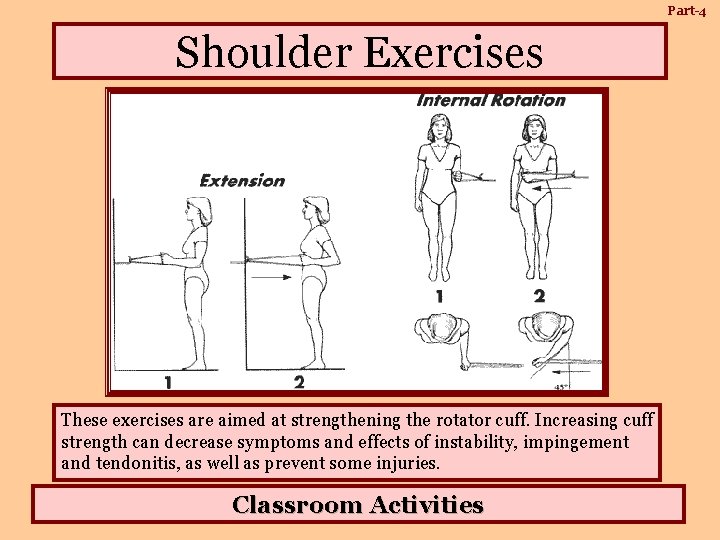
Part-4 Shoulder Exercises These exercises are aimed at strengthening the rotator cuff. Increasing cuff strength can decrease symptoms and effects of instability, impingement and tendonitis, as well as prevent some injuries. Classroom Activities
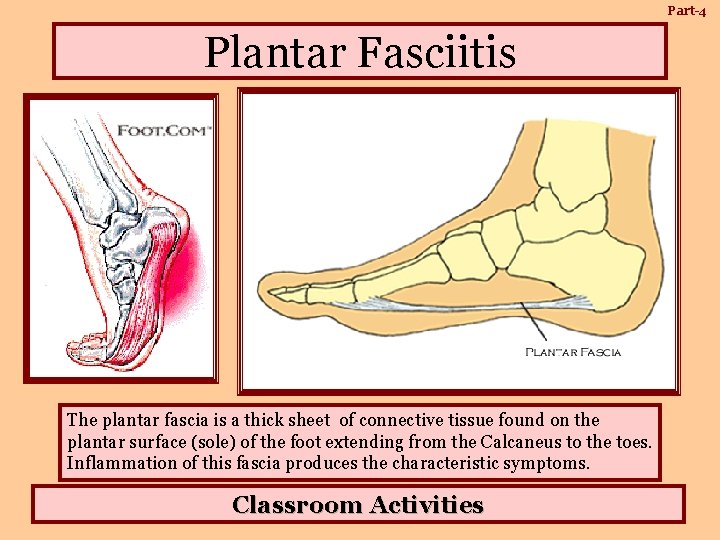
Part-4 Plantar Fasciitis The plantar fascia is a thick sheet of connective tissue found on the plantar surface (sole) of the foot extending from the Calcaneus to the toes. Inflammation of this fascia produces the characteristic symptoms. Classroom Activities

Part-4 Planter Fasciitis Signs and Symptoms: The person complains of pain in the heel that is made worse on climbing stairs, walking or running. The pain is relieved by rest. There is tenderness near the attachment of the fascia to the Calcaneus, medial aspect of the foot and tin the abductor Hallucis muscle. Risk Factors: It is common in individuals with high arched feet and those over the age of 40. In the younger group it can occur in those who are active in sports. People who are in occupations that involve prolonged standing or walking are also prone. Recommendations to Therapist: Ice massage is used initially. In the sub acute or chronic stage, friction massage at the origin of the Calcaneus is given to reduce adhesions. Mobilize the joints of the foot, to reduce stiffness. Lymphatic massage and drainage techniques can be used in the leg and ankle. Remedial exercises to stretch the Gastrocnemius and the plantar fascia should also be done. Classroom Activities

Part-4 Planter Fasciitis Exercises In the second exercise, you lean forward In one exercise, you lean forward against onto a countertop, spreading your feet a wall with one knee straight and heel on apart with one foot in front of the other. the ground. Your other knee is bent. Your Flex your knees and squat down, keeping heel cord and foot arch stretch as your heels on the ground as long as lean. Hold for 10 seconds, relax and possible. Your heel cords and foot arches straighten up. Repeat 20 times for each will stretch as the heels come up in the sore heel. stretch. Hold for 10 seconds, relax and straighten up. Repeat 20 times. Classroom Activities
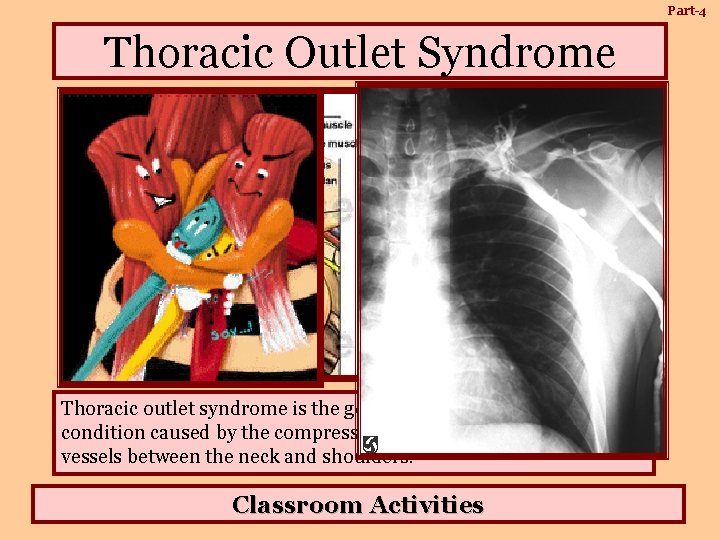
Part-4 Thoracic Outlet Syndrome Thoracic outlet syndrome is the general term used to describe a condition caused by the compressing of the nerves and blood vessels between the neck and shoulders. Classroom Activities

Part-4 Thoracic Outlet Syndrome Signs and Symptoms: Edema or heaviness of the arms, numbness, tingling or weakness of the upper limb are some of the symptoms. Risk Factors: It could be familial if cervical rib is present in other members of the family. Kyphosis and bad posture may also predispose to this condition. Pressure in the armpit as in the use of crutches can damage the nerves going to the limb. Whiplash injury or similar trauma that produces spasm of the neck muscles are other predisposing factors. Recommendations to Therapist: Assess the range of motion of neck and upper limbs. The pulse may weaken and symptoms may be precipitated or reduced on changing the position of the limb. This indicates the presence of this syndrome. Initially with the client supine, massage the chest, shoulder and neck using broad strokes of effleurage and pretrissage. Then concentrate on the muscles of the neck and shoulder. The scalene muscles and anterior neck muscles are important. Classroom Activities

Part-4 TOS Exercises Stretching: • Serratus Anterior • Levator Scapula • Chest Muscles • P/A Neck Muscles. Classroom Activities
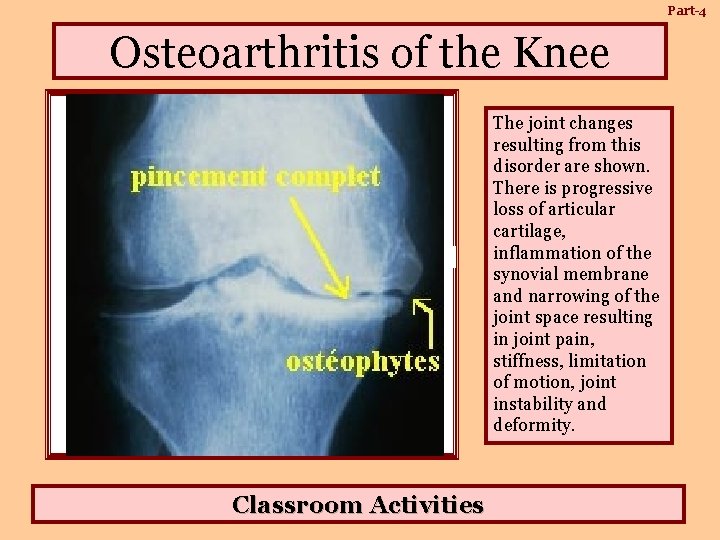
Part-4 Osteoarthritis of the Knee Bone Cysts Osteophyte Narrowing of Joint Space Erosion of Cartilage & Bone Classroom Activities The joint changes resulting from this disorder are shown. There is progressive loss of articular cartilage, inflammation of the synovial membrane and narrowing of the joint space resulting in joint pain, stiffness, limitation of motion, joint instability and deformity.

Part-4 Osteoarthritis of the Knee Signs and Symptoms: Osteoarthritis affects the single large synovial joints. There is a progressive loss of articular cartilage and inflammation of the synovial membrane. There is joint stiffness and muscle spasm. Risk Factors: The incidence increases with age. There is a genetic predisposition in some individuals. Immunologic factors have also been implicated in accelerating the changes in the pirmary type. Trauma to and repetitive use of a joint can predispose to Osteoarthritis. Recommendations to Therapist: Deep moist heat application improves the circulation around the joints. Passive movement and friction of the joint are indicated when pain is minimal. Trigger point therapy, lymphatic drainage techniques and other forms of treatment that have been used. Therapeutic exercise is an important component that is used to increase flexibility, strength, and endurance to reduce pain. Classroom Activities
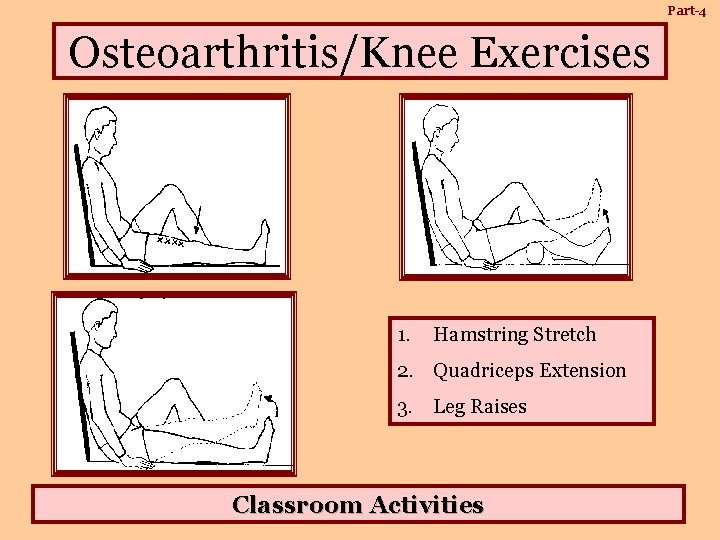
Part-4 Osteoarthritis/Knee Exercises 1. Hamstring Stretch 2. Quadriceps Extension 3. Leg Raises Classroom Activities
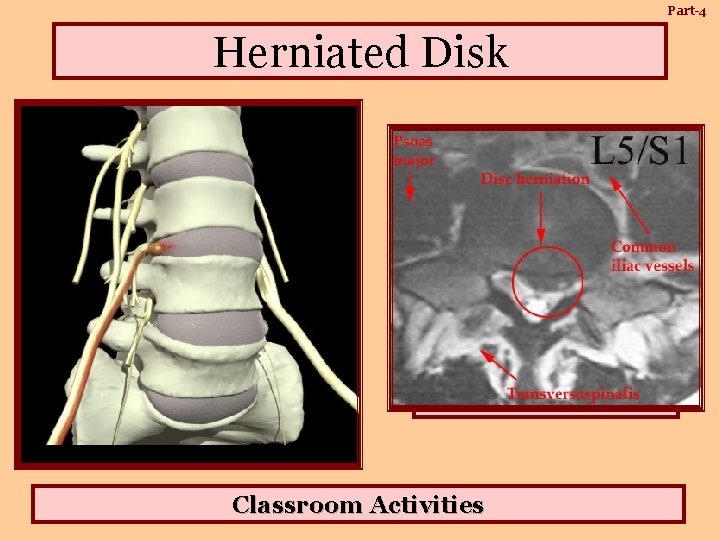
Part-4 Herniated Disk As a disc between two vertebrae degenerates, its inner nucleus may penetrate the surrounding annulus (ring). This causes the disc to protrude (herniate) into the spinal nerves. The weakest portion of the disc is right under the nerve root. A herniation may put pressure on the nerve, which can cause pain to radiate toward the leg, foot, arm, or hand. Classroom Activities
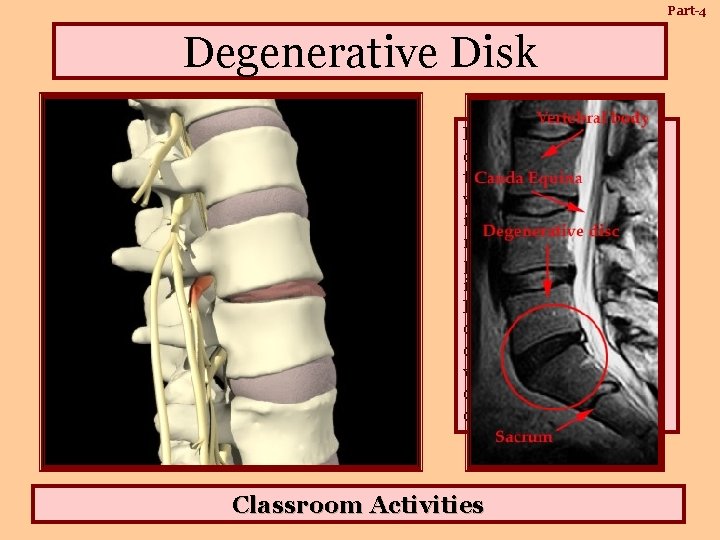
Part-4 Degenerative Disk Lumbar and cervical disc degeneration cause the discs to collapse, which results in nerve impingement (due to the narrowing of nerve pathways/foramina), inflammation, and pain. In severe cases, the discs can degenerate so completely that the vertebrae actually rub directly against each other. Classroom Activities

Part-4 Herniated Disk Signs and Symptoms: Disk prolapse is more common in the lumbar and cervical regions. In most patients, herniated disk occurs in the L 5 -S 1 or L 4 -L 5 regions. In the neck, it is most frequent in the C 6 -C 7 level. Risk Factors: Trauma (eg. Whiplash injury) degenerative disease of the spine (eg. Anklosing spondylitis) predispose to this problem. Recommendations to Therapist: If a person with acute low back pain complains of tingling numbness or weakness of the muscles or if the pain radiates or increases on coughing or straining, do not massage, but advise the client to seek medical help. Work in conjunction with the Physiotherapist on those under treatment for this condition. Identify the muscles that have gone into spasm. Trigger Point therapy is very effective with chronically tight muscles. Patient needs rehabilitative program under the direction of a doctor or physical therapist. Classroom Activities

Part-4 Herniated Disk Exercises Lumbar Extension Back Flexion Gluteus Stretch These back exercises should never be performed if they cause irritation to your back or any other condition while they are being performed! Classroom Activities
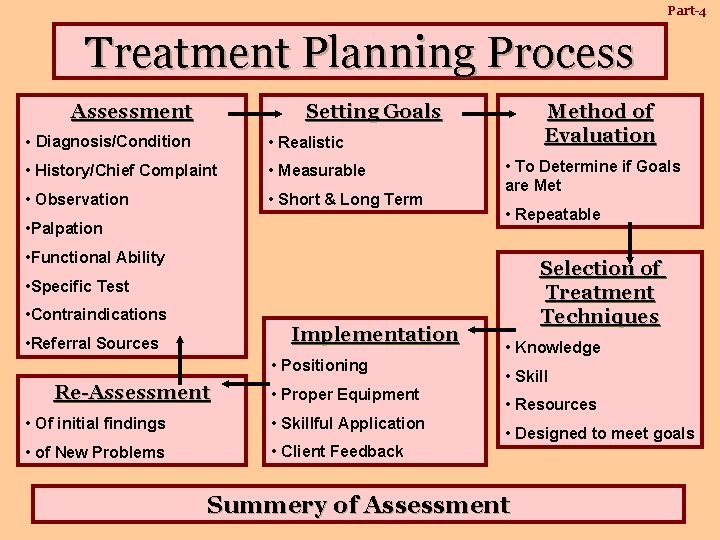
Part-4 Treatment Planning Process Setting Goals Assessment • Diagnosis/Condition • Realistic • History/Chief Complaint • Measurable • Observation • Short & Long Term • Palpation Method of Evaluation • To Determine if Goals are Met • Repeatable • Functional Ability Selection of Treatment Techniques • Specific Test • Contraindications Implementation • Referral Sources • Positioning Re-Assessment • Proper Equipment • Of initial findings • Skillful Application • of New Problems • Client Feedback • Knowledge • Skill • Resources • Designed to meet goals Summery of Assessment

End of Presentation The Value of Assessment IMI
- Slides: 44