Illuminating the Path Becoming a Respiratory Nurse Practitioner

Illuminating the Path: Becoming a Respiratory Nurse Practitioner John Serginson NP Respiratory Caboolture Hospital RN BN MCN MNPS GD Nur Sc (crit care). Rhona Mac. Donald NP Respiratory Lung Health Unit Ipswich P&CHS RGN, MNPS.

Outline Reflections on our different journeys from CNC to NP. Themes, observations & lessons
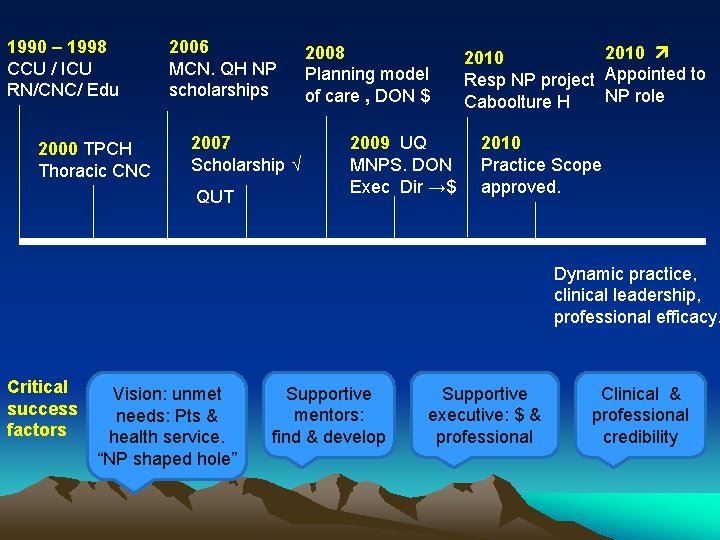
1990 – 1998 CCU / ICU RN/CNC/ Edu 2000 TPCH Thoracic CNC 2006 MCN. QH NP scholarships 2007 Scholarship QUT 2008 Planning model of care , DON $ 2009 UQ MNPS. DON Exec Dir →$ 2010 Resp NP project Appointed to NP role Caboolture H 2010 Practice Scope approved. Dynamic practice, clinical leadership, professional efficacy. Critical success factors Vision: unmet needs: Pts & health service. “NP shaped hole” Supportive mentors: find & develop Supportive executive: $ & professional Clinical & professional credibility
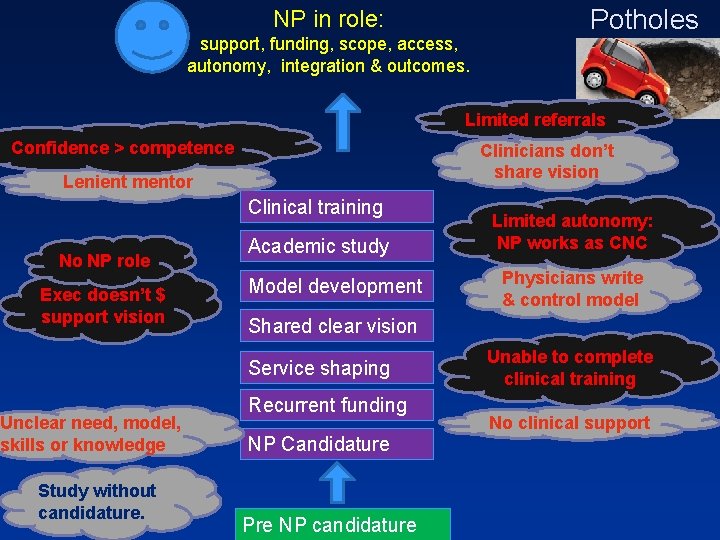
NP in role: support, funding, scope, access, autonomy, integration & outcomes. Potholes Limited referrals Confidence > competence Clinicians don’t share vision Lenient mentor Clinical training No NP role Exec doesn’t $ support vision Academic study Model development Study without candidature. Physicians write & control model Shared clear vision Service shaping Unclear need, model, skills or knowledge Limited autonomy: NP works as CNC Recurrent funding NP Candidature Pre NP candidature Unable to complete clinical training No clinical support

Evolution of Clinical Reasoning CNC Diagnosis & Mx plan clear → Assess, educate, support, behaviour NP Patients are undifferentiated. → Assess (Hx, PE, tests) → Diagnose / clarify Dx Focused on resp. issues, symptom impacts & support needs. Resp. focus & other issues found: address or refer each. Strategies developed with pts , Communicate → specialists in team to discuss findings / suggest changes. Develop MX plan. Communicate →physicians / GPs outside team: evidence to support recommendations.


Primary & Community Health Service (Ipswich) • Employed as a CNC within Lung Health Service • Completed NP course in June 2010 • Employed as NP from February 2011 • How to add value to our existing service? • How to change from CNC to NP? • How are the staff in our service going to respond?

Service looked at: ED presentations with asthma • N= 605 in 12 months • No formal follow up for patients who presented • Some presenting to ED several times • Strain on ED & the hospital • Ipswich general has 341 beds (soon to be 431) • Significant numbers in rural locations (could benefit from home visits but too far to travel).

Resp NP Patients • Rapid access asthma clinic • Rural clinics • Smoking cessation clinics • Patients referred from no formal diagnosis (request & interpret investigations). • Patients referred from physician teams for action plans • Commencing appropriate medications • Problem solving with lung health team

Rapid access Asthma clinic: • Weekly clinic: 14 patients per week. • referrals from ED, GP or wards • also phone or write to all ED visits in month. • SB nurse practitioner – Investigations ordered (spiro, CXR, bloods as needed) – Medications ordered or adjusted – Action plans completed • IF NP can gain control (NP patient only) • If issues: S/B specialist for further investigations & follow up

Rural clinic • 3 rural hospitals in district • 1 clinic / month at each • Generally more severe patients • Referrals from main hospital, GP, rural hosp. • May not have definite diagnosis (patients need work up) • Clinic done with exercise physiologist: modified exercise programs can be done up.

Value Add by NP within service NP completes all Action Plans COPD/Asthma Pulmonary Rehab NP Rural clinics 3 Rural hospitals: Assessment, Diagnosis & Treatment NP Service Referrals from GP’s, ED, MAPU, Inreach & LH team, Lung Health Service NP Aboriginal & Torres Strait Islander Smoking Cessation Clinic COPD / Asthma / Bronchiectasis / ILD education & support NP Rapid Access Asthma Clinic After hours Weekly 4 -8. 30 pm Referrals from Specialist, Inreach OPD and GP

How to change CNC to NP • 2 -3 yrs of hard work • Think holistically • Work autonomously • Take your team with you • Good communication with all

Hurdles & stress • PBS versus LAM (QH List of approved medicines) • No provider number for state (Qld Health) funded NPs • Unable to refer out from Qld Health • Poor understanding of the NP role

End of day stress relief.

Does your service need one of us?
- Slides: 16