Illness Management and Recovery IMR Presented by NHBBH

Illness Management and Recovery (IMR) Presented by NH-BBH June 14, 2007 Harry Cunningham cunningh@mhcgm. org

The Day the Voices Stopped • “I have a vision that goes like this: In this new century, mentally ill people will have the science…, and the means to leave our ghettos of isolation behind us. ” – Ken Steele

What’s the Big Deal? “A wide variety of effective, communitybased services, carefully refined through years of research, exist for even the most severe mental illness yet are not being translated into community settings. ” A Report of the Surgeon General on Mental Health, 1999

The five current Evidence Based Practices (EBPs) • Assertive Community Treatment (ACT) • Integrated Dual Disorders Treatment (IDDT) • Family Psychoeducation (FPE) • Supported Employment (SE) • Illness Management and Recovery (IMR)

Potential future EBPs • Peer support programming • Treatment for people with borderline personality disorders (DBT? ) • Trauma services • Supported housing • ?

Overview of Training • • • What is Illness Management and Recovery? The importance of recovery Core values in IMR 8 key strategies to doing IMR Research behind the practice Engagement and orientation of clients On-the-job-training of some of the 10 topic areas Doing IMR in a group Where do you go from here?

What Is Illness Management and Recovery? • Illness Management and Recovery is a program that helps people set meaningful goals for themselves, acquire information and skills to develop more mastery over their psychiatric illness, and make progress towards their own personal recovery.

Core Ingredients of the Illness Management and Recovery Program: • 6 to 12 months of weekly sessions conducted by trained practitioners • 10 educational handouts that contain practical information and strategies • A practitioners’ guide with tips for teaching people about mental illness and helping them implement strategies

Focus of Services to SMI Consumers in Recent Decades • • 1960 s- Get clients out of the Hospital 1970 s- Keep clients out of the Hospital 1980 s- Rehabilitate clients (Do to them) 1990 s&2000 s- Help clients toward Recovery (Do with them)

EBPs are a Movement in Mental Health • Increase access for consumers to recoverybased services that have demonstrated effectiveness • Help administrators and providers of mental health services to set up and maintain services that have demonstrated effectiveness

The Importance of Recovery “Recovery involves the development of new meaning and purpose in one’s life as one grows beyond the catastrophic effects of mental illness. ” (Anthony, 1993).

Characteristics of Recovery • • Is defined and accomplished by the person Can be viewed as a process or outcome Distinguished from rehabilitation Involves personal and social success in areas the consumer defines as important to them • Is a universal human experience • Includes themes of hope, self-confidence, expectations, well-being, & optimism • “A life worth living” (Patricia Deegan video)
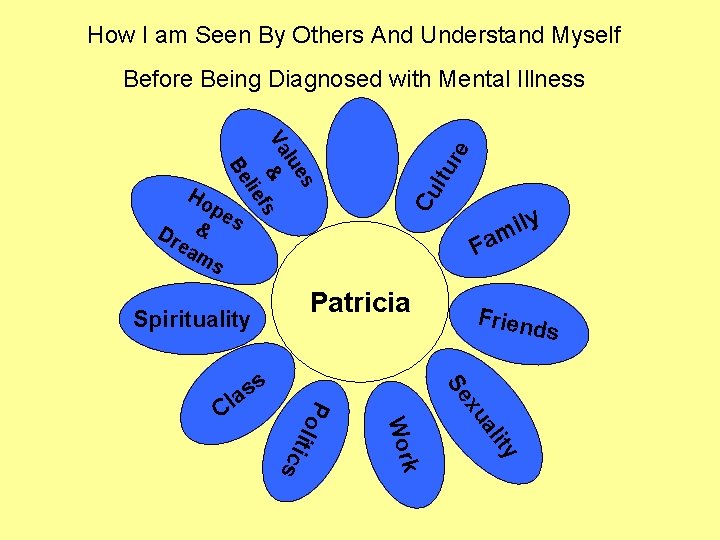
How I am Seen By Others And Understand Myself es lu Va & s f Frien ds Se xu al i ty l i ti c k s Wor Po Cl ly i m Fa Patricia Spirituality s s a Cu lie Ho pe s Dr & ea ms l tu Be re Before Being Diagnosed with Mental Illness

Recovery Is Related to Motivation • Motivation: “an inner urge that prompts a person to action. ” • Illness management and recovery can best happen when a consumer is motivated to act. • Motivation sources: * Hold the hope for someone. * Peer support. * Relationship to professional. * Inner urge. * Mystery? ? ?

What Might Motivate Consumers to Practice IMR?

What Would Motivate You to Practice IMR?

Core Values In IMR § Hope is the Key Ingredient The long term course of MI cannot be predicted Being able to influence one’s own destiny is the basis for future hope and optimism Having other people believe in us is empowering; we sometimes have to “hold” hope for others § Consumers don’t fail the practice, the practice fails them Consumers should be given unconditional support for their participation Programs should work under easy re-entry and “fail-safe” principles § The person is the expert in his or her own experience of mental illness On what strategies have worked for them On what has been helpful and what has not

CORE VALUES IN IMR (Continued) • Personal Choice is Paramount The ability and right of people to make their own decisions, including when those decisions differ from recommendations made by their treatment providers The task then becomes to work with them to evaluate the consequences of decisions in terms of their hopes and dreams. Acceptance is also paramount. • Practitioners are Collaborators Practitioner as consultant in a non-hierarchal relationship • Practitioners demonstrate Respect for people who experience psychiatric symptoms As capable decision-makers and active participants in their own treatment Respect for differing values and opinions To seek common ground when there is a difference in point of view

How Is IMR Different From the Ways I Am Already Working With Consumers?

8 Key Strategies to Doing IMR

Key 1. Client Centered goal setting toward recovery • Focus on client’s context of life rather than just on their symptoms • Strengths vs. Problems • Mutual responsibility in planning and pursuing goals rather than “following” treatment • Constant reassessment and adjustment of plan
Moving From a Disease Model of Mental Illness • Examples of disease goals *Take medications * Reduce voices * Stop reacting to delusions * Maintain housing * Manage finances

Examples of Goals That Go Beyond a Focus on Symptoms • To get closer to 2 current friends who I value. • To improve the appearance of my apartment so I can have friends over. • To play a larger role in the operations of my church. • To own my own car so I can hike in the mountains. • To go to the movies once a month.

Key 2: Good Basic Knowledge About Mental Health: – Origin and course of MI – Symptoms and diagnosis – Medications – Recovery – Community resources

Key 3: A Monitor~Response to Identified Symptoms and Unhealthy Behavior • Increased awareness of “I can effect it” • Choices of things that make it better and make it worse • Relapse prevention plan • Wellness plan • Even though I may not have caused it, I can have the most effect on it • Acceptance of mutual responsibility: Shared Decision Making

Key 4: A Strength-Based Approach • People with severe and persistent mental illness can learn, grow and change. • The focus of the helping process is upon the consumer’s strengths, interests and abilities, not upon their deficits or pathology. People who are successful in living have goals and dreams. They use their strengths to attain their aspirations.

Key 5: Educational Teaching Strategies Interactive teaching, not lecturing • Asking “open-ended” questions to review information and check comprehension • Using a variety of methods to present the handout material: – – summarizing the key points, giving examples taking turns reading aloud asking people to read on their own • Adopting participants’ language to facilitate comprehension of material

Key 6: Motivational Teaching Strategies • Help person see how learning information and skills is related to achieving personal goals • Convey hope, belief, and confidence that person can make desired changes and accomplish goals • Help person explore costs and benefits of maintaining the status quo vs. costs and benefits of change
Key 7: Cognitive-Behavioral Teaching Strategies • • • Reinforcement Shaping Modeling Role playing Cognitive restructuring

Key 8: Emphasis on Stages of Change in Ongoing Assessment • Pre-Engagement Task: Outreach, raise awareness, increase hope • Contemplation Task: Weigh pros and cons, help imagine a better life • Preparation Task: Collect information about alternative actions. • Action Task: Modify lifestyle, staff as consultant(not expert) • Maintenance Task: Maintain new balance, monitor against old habits

IMR Intro Video

IMR Materials (Cont. ) IMR Workbook The basics of Illness Management and Recovery • Educational Handouts with ample worksheets and checklists are provided to participants • Practitioners’ Guide provides guidelines for each topic in the educational handouts

IMR Materials (Cont. ) IMR Videos • Short video introduces the program to participants • Practice demonstration video illustrates the teaching strategies for practitioners

Evidenced-Based Components of Illness Management • Education about mental illness and its treatment • Relapse prevention training • Behavioral tailoring for medication • Coping skills training • Social skills training • Dual Disorder strategies

10 Topic Areas 1. Recovery Strategies 2. Practical Facts about Mental Illness (schizophrenia, bipolar disorder, major depression) 3. The Stress-Vulnerability Model and Treatment Strategies 4. Building Social Support 5. Using Medication Effectively

10 Topic Areas (cont. ) 6. Alcohol and Drug Use 7. Reducing relapses 8. Coping with stress 9. Coping with problems and symptoms 10. Getting your needs met in the mental health system

Learning IMR On-The-Job • Start with 2 -3 clients ASAP • Keep 1 -2 sessions ahead of client • The curriculum and teaching strategies can be learned as you go • Biweekly training/supervision allows practitioners to gain the knowledge

IMR is Structured yet Flexible Not intended to be presented as a “cookie cutter” practice! The ideal is to integrate: – best available research – your individual clinical expertise – with consumer’s preferences

Seeing and Doing IMR

Who is IMR Designed For? • Almost anyone with a severe mental illness • Research and educational materials cover 4 areas of symptoms: schizophrenia, schizoaffective disorder, bipolar disorder, major depression • You often can’t predict who will benefit and who won’t • Customize to the unique needs of the consumer

Examples of consumers who may benefit from IMR • People with distressing persistent symptoms • People who experience frequent hospitalizations • People who have frequent crises • People wanting to live more independently • People wanting to improve employment skills • People wanting to increase friendships

Engagement Barriers: Staff • • She’s too high/low functioning He doesn’t show up for anything She’s got too many crises going on He never sticks around for more than 3 months She needs maintenance, not recovery I already do this with clients I don’t have time for extra work

Engagement Barriers: Client • • • Nothing really helps, why try IMR It’s too risky to risk It’s too much commitment It sounds too much like school I’m not mentally ill, or schizophrenic, or… I know all of that stuff already

Approaches to Engage Clients How would you like to learn more about: § recovery, future possibilities for you § medications, support from medical staff § mental illness, diagnosis § reducing relapses § coping with stress § support from family and other people § reduce/manage symptoms § leaving the hospital

Approaches to Clients (cont. ) How would you like to be more involved: • Play more of a role in the treatment team • Set goals that reflect personal and social success that are important to you Can you use your relationship with client? • Find ways to help staff work more with you • Have staff better understand you • Trust me! Trial Offer • Come this week and decide if you want to continue

Orientation for Clients (Page 39) • Usually lasts one meeting • Expectations made clear – Attendance – Roles of consumer and practitioner – Homework – Mutual responsibility – Sets positive expectations of change • Reduces treatment drop-out rate!

Homework • Collaboratively agreed upon by the practitioner and the person at the end of each session • Related to the person’s goal and/or the curriculum topic • Individually tailored to the person

Homework (continued) • Behaviorally specific • May involve significant others or treatment team members • Followed up at the next session • Analyze and problem-solve any difficulties in doing assignments.

Examples of Homework • Reviewing a handout, checklist, or plan with significant other • Practicing a skill (e. g. , striking up a conversation) • Getting more information about achieving a goal (e. g. , checking out costs of local health clubs) • Taking a step towards a personal goal • Practicing a coping strategy at home (e. g. , relaxation exercises)

Knowledge and Skills Inventory • Strengths Assessment Or • Knowledge and Skills Inventory (Page 41) Your choice!

Involvement of Family & Other Supportive People • Encourage family members and other supportive people to participate • With the participant’s permission • Supportive people can help in a variety of ways: • • • Assisting with homework Reading handouts Role in relapse prevention plan Achieving specific goals Attending some sessions

Structure of Sessions • Informal socializing and identification of any major problems (1 -3 minutes) • Review previous sessions (1 -3 minutes) • Review homework (3 -5 minutes) • Follow-up on goals (1 -3 minutes) • Set agenda for current session (1 -2 minutes)

Structure of Sessions (continued) • Teach new material or review previously taught material (20 -30 minutes) • Agree on new homework assignment (3 -5 minutes) • Summarize progress made in current session (3 -5 minutes)

Topic Area 1: Recovery Strategies • • Introduces the concept of “recovery” Encourages people to develop own definition Tone of hope and optimism to move forward Helps consumers establish personally meaningful goals • Identifies and puts into practice strategies toward personal recovery goals (Kim and Francis)


Topic 3: Stress-Vulnerability Model • Discussion of the origin and course of MI • How to then prevent a worsening course • What important ideas for consumers are contained in this Model?

Topic 4: Building Social Support • Understand the importance of social support in one’s own life to one’s recovery • Skills to meet new people • Skills to get closer to people you already know (Video, Susan and Mark)

Building Social Support Exercise: Starting a casual conversation • Explain and identify “icebreakers” • You model using an icebreaker to start a conversation • Role-play the consumer doing the same • Give positive feedback. • Make 1 corrective suggestion • Same role-play using the corrective action

Topic 5: Using Medication Effectively • Consumers are encouraged to make their own choices about medication taking – Explore role of medication in managing symptoms – Benefits of my medication/Side effects my medication – Informed decision making about medications • Strategies for getting the most out of medication are described – Medication regimen matches life demands – Building routine into medication taking, Simplify! – Keep the benefits in mind

Topic 6: Drug and Alcohol Use Part I: Psycho-education about D&A use. *Commonly used substances and their effects *Why do people use drugs and alcohol? *Unique relationship between D&A and MI. *Problems related to D&A use. Part II: Making a decision about D&A use. *Weighing the pros and cons of using/sobriety *Deciding to cut down or stop using

Drug and Alcohol Use Part III: Actions to cut down or stop using *Dealing with high risk situations. *Finding new ways of getting needs met. *Making a personal sobriety plan.

Topic 7: Reducing Relapses: Four areas of focus • • Identify early warning signs of relapse Identify precipitants (triggers) to relapse Plan ways to respond to first signs of relapse Involve others to support efforts to monitor and respond to signs of relapse so they don’t become full-blown relapse (Video: Susan and Tracy)

Doing IMR in a Group • • • 6 -10 consumers 2 Co-leaders Meet weekly or 2 x a week 40 -50 sessions Use IMR Educational Handouts Use “Group Guidelines”

Advantages to Doing IMR in a Group Format • • Some agencies have strong group tradition Easier to stay focused on the skills Peer helping peer Role playing is more effective (generalizing) • Problem-solving is richer • Can be more cost effective

IMR Group Supervision Purpose: *Support and affirmation for practitioners to do their job *Generate fresh ideas *Learn, learn Focus: *Clients only! (Present 1 -3 client situations per supervision) Tools: *Strength assessment, client’s IMR goals, *Problem solving model Outcomes: *A plan: 1 -3 ideas to try with helping the client *Fist steps to carrying out those ideas *Recognition of success and achievements

Ongoing Supervision/Training (Outline of a sample session done every 1 -2 weeks) • Go-round of Current Problems/Issues doing IMR (15 minutes) • Review last meeting’s practice assignment (5 minutes) • Introduce a Skill (10 minutes) • Model Skill (5 minutes) • Role-Play Skill (10 minutes) • Develop Practice Assignment (5 minutes)

5 Step Problem Solving Method • • 1. Define: What is the Problem? 2. Brainstorm Possible Solutions 3. List Pluses and Minuses of Solutions 4. Choose the best Solution or combination of Solutions • 5. Plan the steps to carry out the Best Solution: Action Plan

Monitoring the Practice • Internal monitoring *Referrals *Follow-up to referrals *Faithfulness to the model (Fidelity Scales) *Consumer outcomes

What Factors Helped? • A strong program leader • Senior Administrative support • Regular supervision and training • Practitioners given credit for time spent • Toolkits • Consultation and Training • Compensation for lost productivity

What Factors Hurt? • Administrative indifference • Staff turnover • No hospital integration • Program leader apathy • “We already do this” • No rewards • Lack of monitoring

Closing Thoughts “Having strategies for coping with mental illness is extremely important. It is hard to enjoy your life if you are constantly sick with mental illness. . However, believing in yourself, having hope that things will continue to get better and looking forward to your future also vital in overcoming mental illness. Our hopes and dreams are not delusions. Our hopes and dreams are what makes us human. ” David Kime, artist, writer, floral designer, person in recovery from bipolar disorder

THAT”S ALL FOLKS! What Questions Do You Have? cunningh@mhcgm. org
- Slides: 72