Illinois Institute of Technology Physics 561 Radiation Biophysics

Illinois Institute of Technology Physics 561 Radiation Biophysics Lecture 7: Radiation sensitivities of tumors and normal tissues Andrew Howard 24 June 2014 6/17/202 1 tumor and normal-tissue responses p. 1 of 102

Plans For This Class u u u In vivo assays of normal tissue Acute lethal response Teratogenesis ch 10 Nonstochastic effects (chapter 10) Late effects on normal tissue (chapter 11) 6/17/202 1 tumor and normal-tissue responses p. 2 of 102
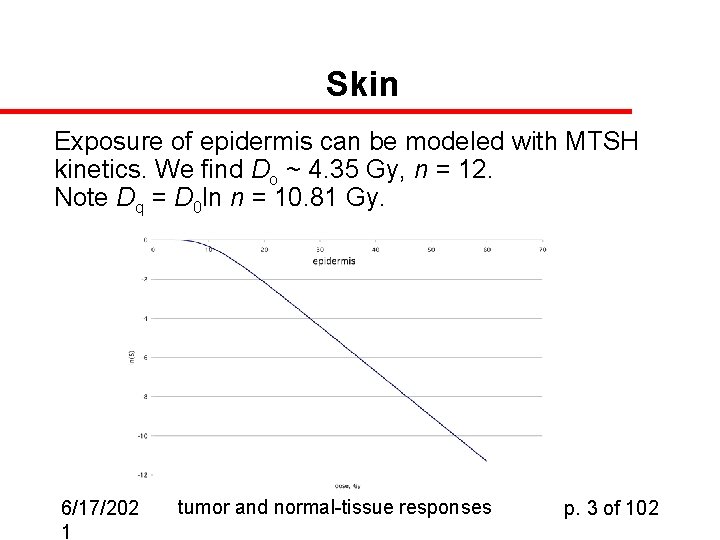
Skin Exposure of epidermis can be modeled with MTSH kinetics. We find Do ~ 4. 35 Gy, n = 12. Note Dq = D 0 ln n = 10. 81 Gy. 6/17/202 1 tumor and normal-tissue responses p. 3 of 102
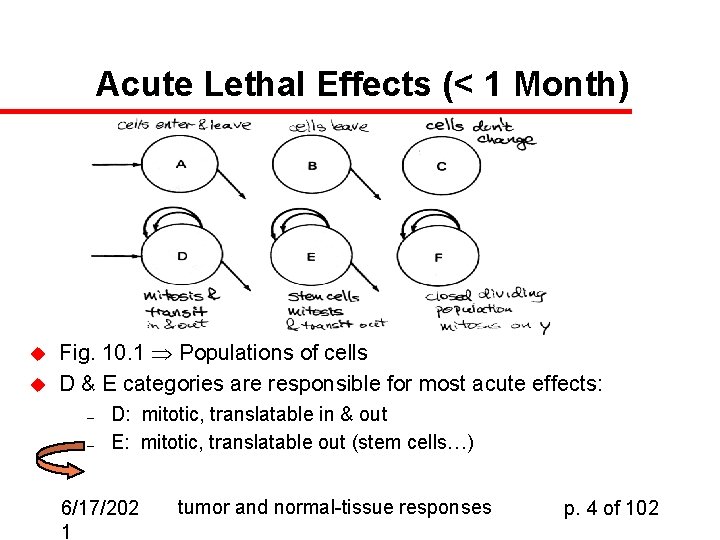
Acute Lethal Effects (< 1 Month) u u Fig. 10. 1 Populations of cells D & E categories are responsible for most acute effects: – – D: mitotic, translatable in & out E: mitotic, translatable out (stem cells…) 6/17/202 1 tumor and normal-tissue responses p. 4 of 102
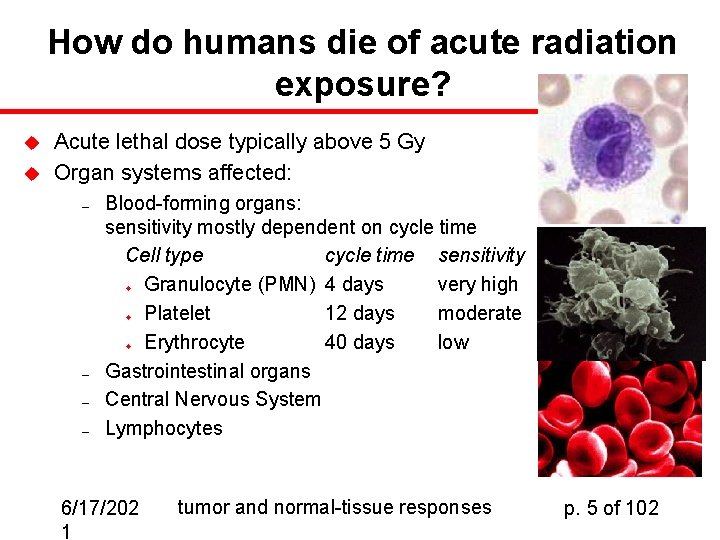
How do humans die of acute radiation exposure? u u Acute lethal dose typically above 5 Gy Organ systems affected: – Blood-forming organs: sensitivity mostly dependent on cycle time Cell type cycle time sensitivity Granulocyte (PMN) 4 days very high Platelet 12 days moderate Erythrocyte 40 days low Gastrointestinal organs Central Nervous System Lymphocytes u u u – – – 6/17/202 1 tumor and normal-tissue responses p. 5 of 102

Acute Lethal Effects (< 1 Month) u Blood-forming effects – – u u 3 weeks Not very repairable 1 - 2 - 5 Gy Lethality GI - If not fatal within 10 days, recovery likely Central Nervous Systems: resuts are dose-dependent – 1 Gy Vomiting Results from direct stimulation of neurons? 100 Gy Massive disorientation Death u u – u u 6/17/202 1 tumor and normal-tissue responses p. 6 of 102

Lymphocytes: a special case u u u Mature lymphocytes are fairly radiosensitive This is unusual for a nondividing, terminal cell type Some kind of “interphase death” 6/17/202 1 tumor and normal-tissue responses p. 7 of 102
A possible explanation u There’s a lot of p 53 gene product produced in lymphocytes: maybe they’re being stimulated into dying with moderate radiation exposure u http: //www. rcsb. org/pdb/static. do? p= education_discussion/molecule_of_t he_month/pdb 31_1. html 6/17/202 1 tumor and normal-tissue responses p 53 core domain PDB structure 2 BIN p. 8 of 102
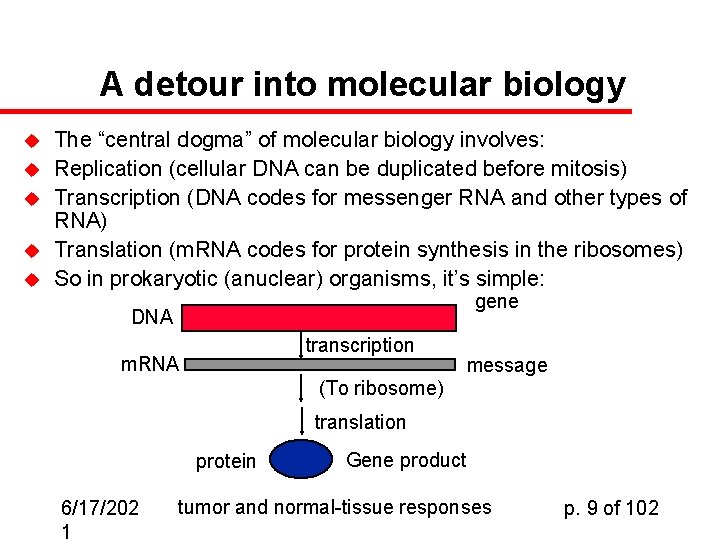
A detour into molecular biology u u u The “central dogma” of molecular biology involves: Replication (cellular DNA can be duplicated before mitosis) Transcription (DNA codes for messenger RNA and other types of RNA) Translation (m. RNA codes for protein synthesis in the ribosomes) So in prokaryotic (anuclear) organisms, it’s simple: gene DNA transcription m. RNA message (To ribosome) translation protein 6/17/202 1 Gene product tumor and normal-tissue responses p. 9 of 102
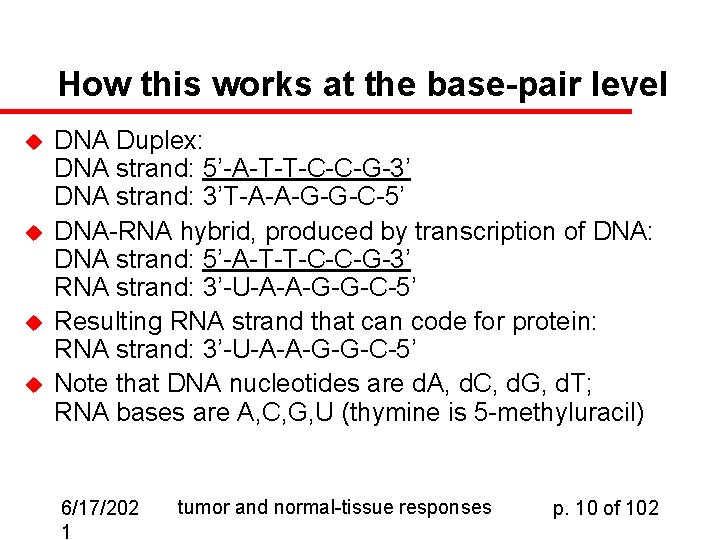
How this works at the base-pair level u u DNA Duplex: DNA strand: 5’-A-T-T-C-C-G-3’ DNA strand: 3’T-A-A-G-G-C-5’ DNA-RNA hybrid, produced by transcription of DNA: DNA strand: 5’-A-T-T-C-C-G-3’ RNA strand: 3’-U-A-A-G-G-C-5’ Resulting RNA strand that can code for protein: RNA strand: 3’-U-A-A-G-G-C-5’ Note that DNA nucleotides are d. A, d. C, d. G, d. T; RNA bases are A, C, G, U (thymine is 5 -methyluracil) 6/17/202 1 tumor and normal-tissue responses p. 10 of 102
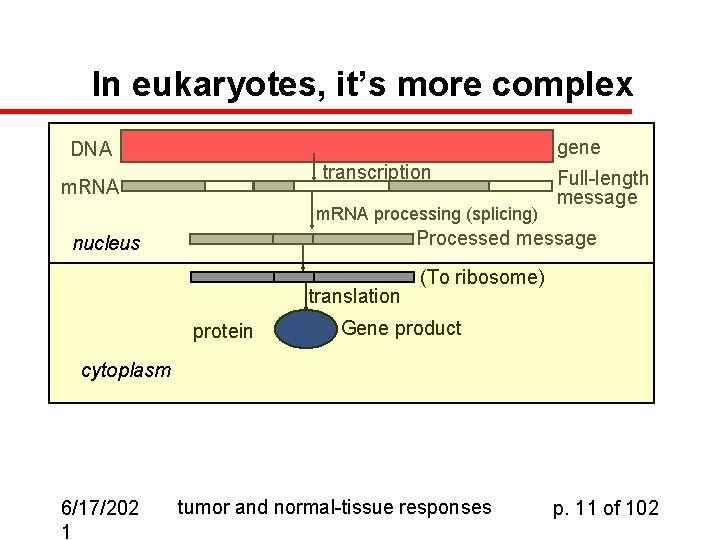
In eukaryotes, it’s more complex gene DNA transcription m. RNA processing (splicing) Full-length message Processed message nucleus translation protein (To ribosome) Gene product cytoplasm 6/17/202 1 tumor and normal-tissue responses p. 11 of 102

Numbers matter, too! u u u Suppose the original gene was 2000 base-pairs long. The full-length message will therefore be 2000 bases. The truncated (processed) m. RNA might be 720 bases. The resulting protein would be 720/3 = 240 amino acids long. Note that only 36% of the DNA is actually coding for protein in this case. 6/17/202 1 tumor and normal-tissue responses p. 12 of 102
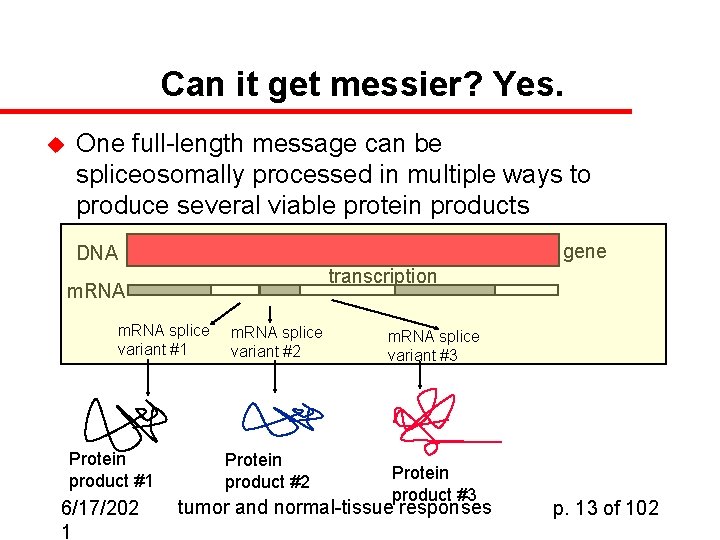
Can it get messier? Yes. u One full-length message can be spliceosomally processed in multiple ways to produce several viable protein products gene DNA transcription m. RNA splice variant #1 Protein product #1 6/17/202 1 m. RNA splice variant #2 Protein product #2 m. RNA splice variant #3 Protein product #3 tumor and normal-tissue responses p. 13 of 102

Bcl 3: an example u u Bcl 3 is an important gene in regulation of apoptosis and therefore in carcinogenesis and other developmentally-related pathologies. Exists in multiple splice variants, all derived from a single gene. Some variants stimulate apoptosis, others inhibit it! See Gil Ast, “The Alternative Genome, ” Scientific American, April 2005, pp. 58 -65. 6/17/202 1 tumor and normal-tissue responses p. 14 of 102

Why do we talk about this here? u u Alternative splicing may look like a topic that only a true molecular biologist would care about, but it isn’t. If a certain gene is being stimulated into producing more of its starting m. RNA, the protein-dependent outcome of that stimulation may be complex or even counter-intuitive, depending on this phenomenon If ionizing radiation were to turn on the BCL 3 gene, would that increase or decrease apoptosis? Unclear Even if we knew that, would we know whether that would be radioprotective? Not necessarily. 6/17/202 1 tumor and normal-tissue responses p. 15 of 102

Gestational Radiosensitivity u u Fig. 10 provides a long list of radiosensitivity data for various organs and organ systems In some cases the maximum sensitivities are early, in others much later 6/17/202 1 tumor and normal-tissue responses p. 16 of 102

Teratogenesis & Fetal Development u u u Teratogenesis - Embryological abnormality monster It’s traditional to argue that the fetus is highly radiosensitive, but it actually isn’t, compared to other rapidly dividing cell systems. We need to distinguish among: – – – 6/17/202 1 Damage to gametes before fertilization Somatic damage to growing organism Damage to mother that influences development tumor and normal-tissue responses p. 17 of 102

Measurement Problems associated with Teratogenesis u Confounding effects (how can one tell these phenomena apart? ) – – – u Genetic damage before fertilization Damage to embryo/fetus Damage to placental system High background – – High incidence of birth defects in unexposed subjects 5% of all births involve some significant abnormality 6/17/202 1 tumor and normal-tissue responses p. 18 of 102
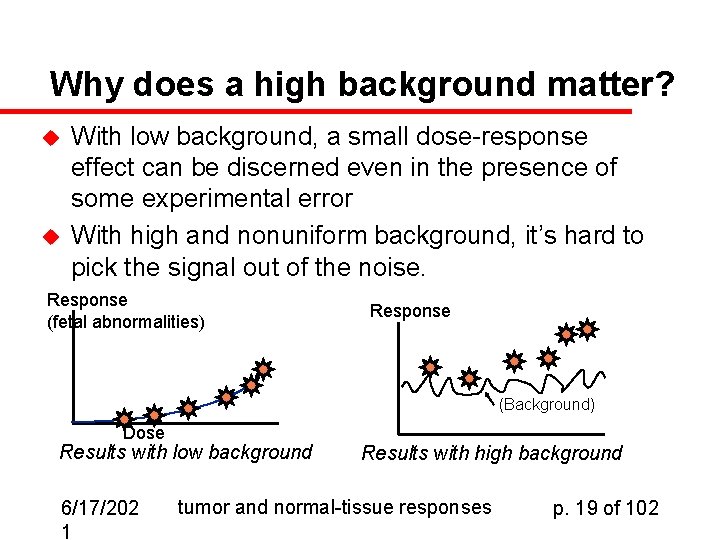
Why does a high background matter? u u With low background, a small dose-response effect can be discerned even in the presence of some experimental error With high and nonuniform background, it’s hard to pick the signal out of the noise. Response (fetal abnormalities) Response (Background) Dose Results with low background 6/17/202 1 Results with high background tumor and normal-tissue responses p. 19 of 102
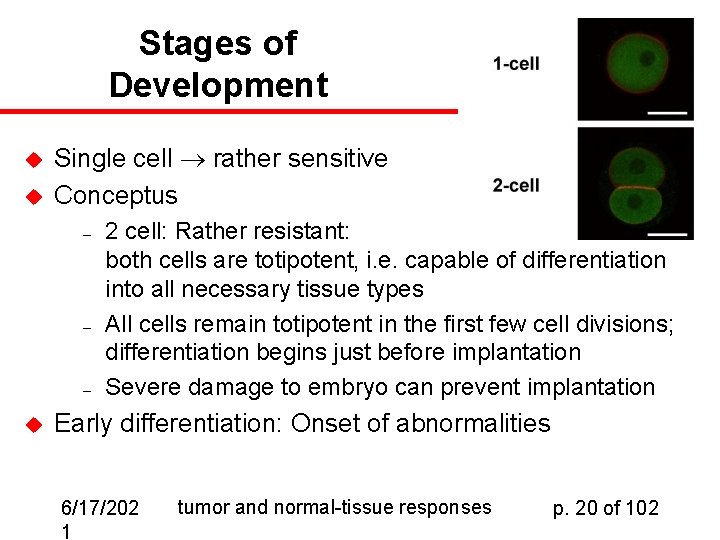
Stages of Development u u Single cell rather sensitive Conceptus – – – u 2 cell: Rather resistant: both cells are totipotent, i. e. capable of differentiation into all necessary tissue types All cells remain totipotent in the first few cell divisions; differentiation begins just before implantation Severe damage to embryo can prevent implantation Early differentiation: Onset of abnormalities 6/17/202 1 tumor and normal-tissue responses p. 20 of 102

Types of fetal damage u Severe mental retardation – – u Microcephaly – – u Occurs in 1 -5 Gy range? Is this really teratogenic or does it involve damage to mother at higher doses? Might occur even in 1 Gy range Data supporting that are disputable Other types of damage described in mouse studies 6/17/202 1 tumor and normal-tissue responses Microcephalic woman: in utero in Hiroshima when the bomb fell p. 21 of 102
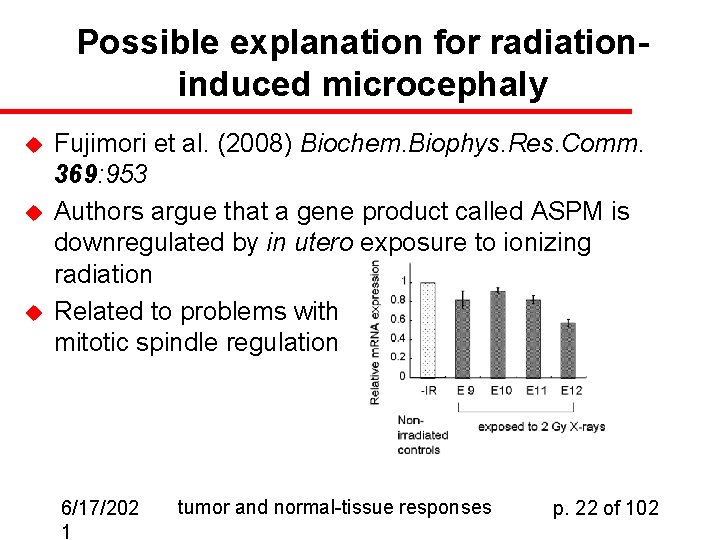
Possible explanation for radiationinduced microcephaly u u u Fujimori et al. (2008) Biochem. Biophys. Res. Comm. 369: 953 Authors argue that a gene product called ASPM is downregulated by in utero exposure to ionizing radiation Related to problems with mitotic spindle regulation 6/17/202 1 tumor and normal-tissue responses p. 22 of 102

Developmental Toxicity u u u This is an attempt to get you to think about the collected information in fig. 10. Fig. 10 provides a long list of radiosensitivity data for various organs and organ systems In some cases the maximum sensitivities are early, in others much later Most effects on the eye (other than cataracts) occur relatively late Most functional disorders are very late Cephalic disorders occur all through gestation 6/17/202 1 tumor and normal-tissue responses p. 23 of 102

Stochastic Effects of Radiation u u One of two overarching categories of damage, particularly as it produces long-term effects: Percent of population affected by the exposure may be dose-dependent -BUT- u u u Severity of condition in an affected individual is independent of dose Cancer is traditionally regarded as stochastic, but that may be an oversimplification Nonstochastic damage is damage that does display dose-response relationships in an individual 6/17/202 1 tumor and normal-tissue responses p. 24 of 102
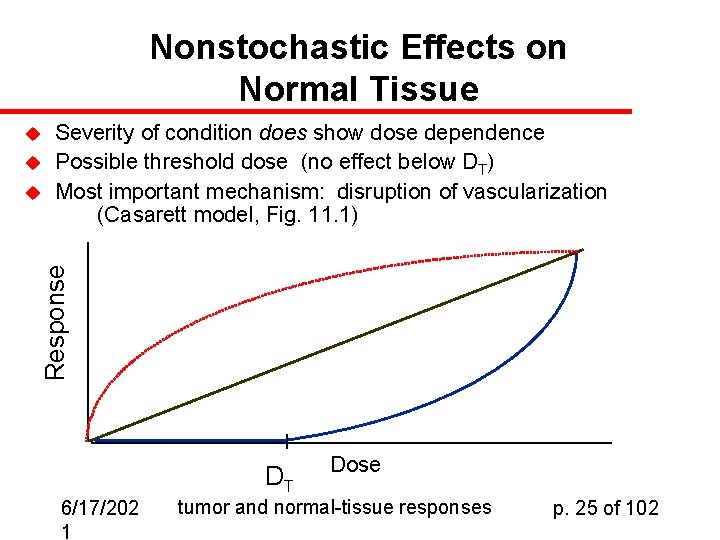
Nonstochastic Effects on Normal Tissue u u Response u Severity of condition does show dose dependence Possible threshold dose (no effect below DT) Most important mechanism: disruption of vascularization (Casarett model, Fig. 11. 1) DT 6/17/202 1 Dose tumor and normal-tissue responses p. 25 of 102

Casarett model for microvasculature u u u Sequence of events beginning with irradiation and ending with loss of function, susceptibility to disease, and death Shown in Fig. 11. 1 Note cyclic effect of fibrosis and secondary vascular regression 6/17/202 1 tumor and normal-tissue responses p. 26 of 102
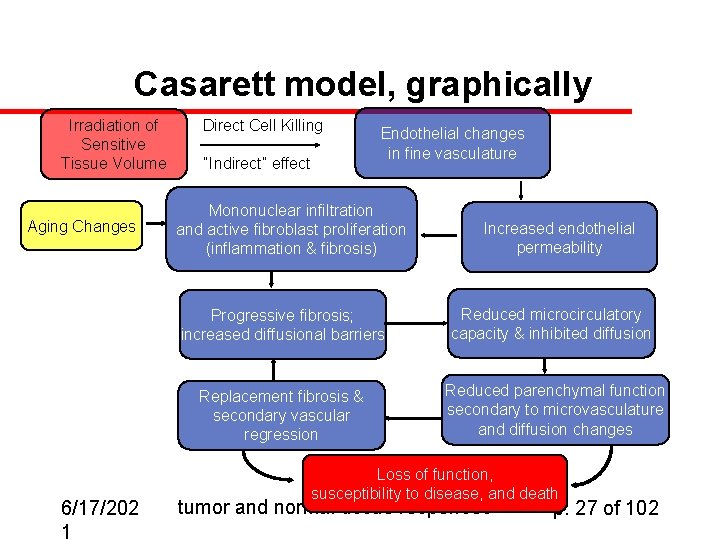
Casarett model, graphically Irradiation of Sensitive Tissue Volume Aging Changes 6/17/202 1 Direct Cell Killing “Indirect” effect Endothelial changes in fine vasculature Mononuclear infiltration and active fibroblast proliferation (inflammation & fibrosis) Increased endothelial permeability Progressive fibrosis; increased diffusional barriers Reduced microcirculatory capacity & inhibited diffusion Replacement fibrosis & secondary vascular regression Reduced parenchymal function secondary to microvasculature and diffusion changes Loss of function, susceptibility to disease, and death tumor and normal-tissue responses p. 27 of 102
Vascular endothelium as target u u Endothelial cells lining capillaries are a cellrenewal system, so damage there will hurt the organ that those capillaries supply with blood. Types of damage: – – 6/17/202 1 Direct: interphase death of cells in wall (DNA damage leading to apoptosis) Indirect: interference with cell renewal tumor and normal-tissue responses p. 28 of 102
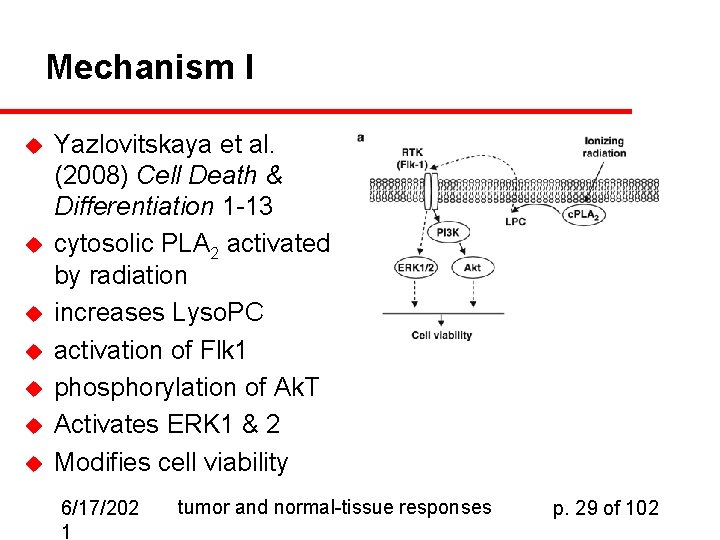
Mechanism I u u u u Yazlovitskaya et al. (2008) Cell Death & Differentiation 1 -13 cytosolic PLA 2 activated by radiation increases Lyso. PC activation of Flk 1 phosphorylation of Ak. T Activates ERK 1 & 2 Modifies cell viability 6/17/202 1 tumor and normal-tissue responses p. 29 of 102
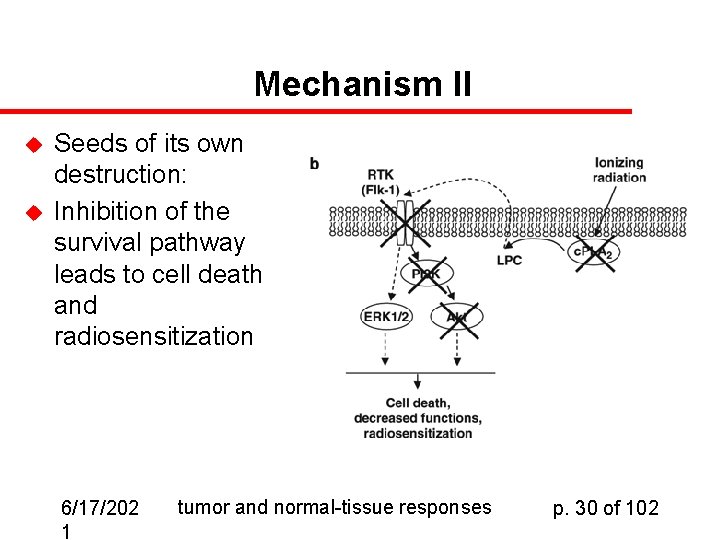
Mechanism II u u Seeds of its own destruction: Inhibition of the survival pathway leads to cell death and radiosensitization 6/17/202 1 tumor and normal-tissue responses p. 30 of 102

Gastrointestinal systems where this mechanism predominates u u 6/17/202 1 Esophagus Stomach Small & large intestine Rectum (not the only mechanism) tumor and normal-tissue responses p. 31 of 102

Other systems where this mechanism predominates u u u Skin (dermal layer) & other epidermal mucosal organs Liver (except for hepatitis) Kidneys (many other mechanisms) Lung (other mechanisms) Brain Spinal cord (low-dose effects are of this type) 6/17/202 1 tumor and normal-tissue responses p. 32 of 102

Functional Subunits u u Concept: The fate of an organ depends on individual functional subunits (FSUs). When all the stem cells that give rise to the functioning cells in a functional subunit die, then the functional subunit can’t continue to operate Examples: – In the kidney: the nephron – In the lung: the alveolus – In the pancreas: a single islet of Langerhans – In the small intestine: a gastrointestinal crypt Can we generalize this to all tissues? Maybe not. 6/17/202 1 tumor and normal-tissue responses p. 33 of 102

Other types of late damage u u The assertion: If vascular damage were the whole story for the late effects of radiation, then the time of onset of late damage should be more or less the same for all organs. That’s false! Stromal and parenchymal damage – – 6/17/202 1 parenchymal cells are those involved in the actual function of an organ, e. g. the cells in the liver that actually filter out damaging chemicals Stromal cells are the support cells that undergird and provide morphological support for the parenchymal cells tumor and normal-tissue responses p. 34 of 102
Non-endothelial late effects u u u Rectum: thinning & perforation of rectum Epidermal layer of skin: desquamation Kidneys: complicated, multi-causal; tubular disfunction in glomerulus unrelated to vascular disorders Lung: killing of type 2 alveolar cells Spinal cord: fast paralysis involves damage to myelin sheath around cord Eye: improper differentiation of lens fiber cells leads to cataracts 6/17/202 1 tumor and normal-tissue responses p. 35 of 102

Summary of organ-specific effects See table in the html documents on Blackboard for full summary on nonstochastic effects 6/17/202 1 tumor and normal-tissue responses p. 36 of 102

And now for something mostly different u u u We’ll move away from nonstochastic late effects to a discussion of treatment modalities for tumors. Here we’re focusing on the fact that tumors are somewhat DNA repair-deficient and therefore respond differently to ionizing radiation than healthy tissues do We’ll look, in particular, at dose fractionation as a component of treatment planning for cancer 6/17/202 1 tumor and normal-tissue responses p. 37 of 102

Fractionation u u u Radiotherapy can’t wait for research: people need answers now Even in the 1930’s and 40’s it was recognized that there was an advantage in treating tumors to fractionate the dose, i. e. if the total dose you wanted to deliver was 5 Gy, you got a better therapeutic ratio if you delivered it in several small doses rather than all at once. We’ll now explore some quantitative models of the relationship between damage and fractionation 6/17/202 1 tumor and normal-tissue responses p. 38 of 102

Power Law and Timing u u Witte: measured dose D required to reach the threshold for skin erythema as a function of dose rate or number of fractions n: Power law: ln. D = a + blnn, i. e. b a+blnn a lnn D=e =e e D = Qnb, where Q = ea. 6/17/202 1 tumor and normal-tissue responses p. 39 of 102
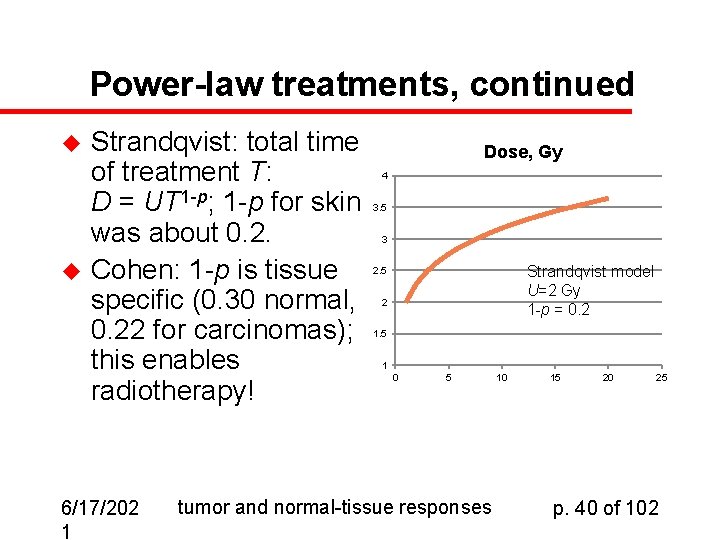
Power-law treatments, continued u u Strandqvist: total time of treatment T: D = UT 1 -p; 1 -p for skin was about 0. 2. Cohen: 1 -p is tissue specific (0. 30 normal, 0. 22 for carcinomas); this enables radiotherapy! 6/17/202 1 Dose, Gy 4 3. 5 3 Strandqvist model U=2 Gy 1 -p = 0. 2 2. 5 2 1. 5 1 0 5 tumor and normal-tissue responses 10 15 20 25 p. 40 of 102

Normalized Standard Dose u u u Ellis: tolerance dose D for normal tissue is related to the number of fractions N and the overall treatment time in days, T: D = r. T 0. 11 N 0. 24 The value of r is called the Normalized Standard Dose or NSD; it can be determined separately for each tissue and each treatment modality. 6/17/202 1 Tolerated Dose as function of # of treatments 9 8. 5 8 7. 5 7 6. 5 6 5. 5 5 4 # of treatments 0 tumor and normal-tissue responses 50 100 150 p. 41 of 102

What are we really doing here? u u u This is curve-fitting in its most unapologetic form. As far as I know there is no attempt to attach physical meanings to the exponent (1 -p) in the Strandqvist model. Nor is there a reason to think there’s anything physically significant about the 0. 11 and 0. 24 exponents in the Ellis formulation 6/17/202 1 tumor and normal-tissue responses p. 42 of 102

Time of treatment and number of fractions u u 6/17/202 1 Clearly time and number of fractions are (anti-)correlated variables BUT this approach can be helpful in treatment planning, at least within the range of conditions for which the formulas are valid. tumor and normal-tissue responses p. 43 of 102

Can we do better than this? u Explicit accounting for damage in terms of repairability: – – – u Sublethal Potentially lethal Nonrepairable Model suggests that the limiting slope of ln. S vs D as you fractionate a lot is determined by the single-hit (nonrepairable) mechanism 6/17/202 1 tumor and normal-tissue responses p. 44 of 102
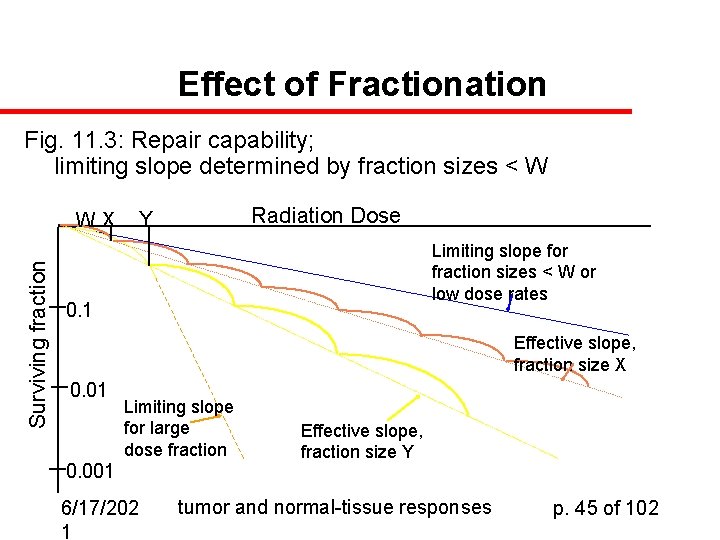
Effect of Fractionation Fig. 11. 3: Repair capability; limiting slope determined by fraction sizes < W Surviving fraction WX Radiation Dose Y Limiting slope for fraction sizes < W or low dose rates 0. 1 Effective slope, fraction size X 0. 01 Limiting slope for large dose fraction 0. 001 6/17/202 1 Effective slope, fraction size Y tumor and normal-tissue responses p. 45 of 102

Douglas & Fowler u u Used mouse-foot skin reaction to fractionated doses: ≤ 64 fractions , constant overall time For an isoeffect, the following equation held: n(a + b 2) = g where n = # of fractions, = dose per fraction note: I’m using where Alpen uses D, to reduce potential confusion with the overall dose. 6/17/202 1 tumor and normal-tissue responses p. 46 of 102

Douglas-Fowler Assumptions u u u Repair occurs after single doses Biological outcome depends on surviving fraction of critical clonogenic cells Every equal fraction will have same biological effect 6/17/202 1 tumor and normal-tissue responses p. 47 of 102

Survival fraction, Douglas&Fowler formulation u u u ln. S = n(Fe/a) Note that a is not a. For an appropriate choice of a, Fe = 1/(n ) Single-dose cell survival is S = exp[(Fe/a) ] So we do an isoeffect plot of Fe vs. : Fe = b + c 6/17/202 1 tumor and normal-tissue responses p. 48 of 102

Douglas & Fowler Survival Fraction, Continued u u u Thus ln. S = n(b /a + c 2/a) cf. Standard LQ model, assuming constant effect per fraction: ln. S = -n(a + b 2) Defining E = -ln. S, E/(n ) = a + b 1/(n ) = a/E + b /E plot vs Fe = 1/(n ) to get a/E, b/E. In practical situations we may not be able to measure E directly 6/17/202 1 tumor and normal-tissue responses p. 49 of 102
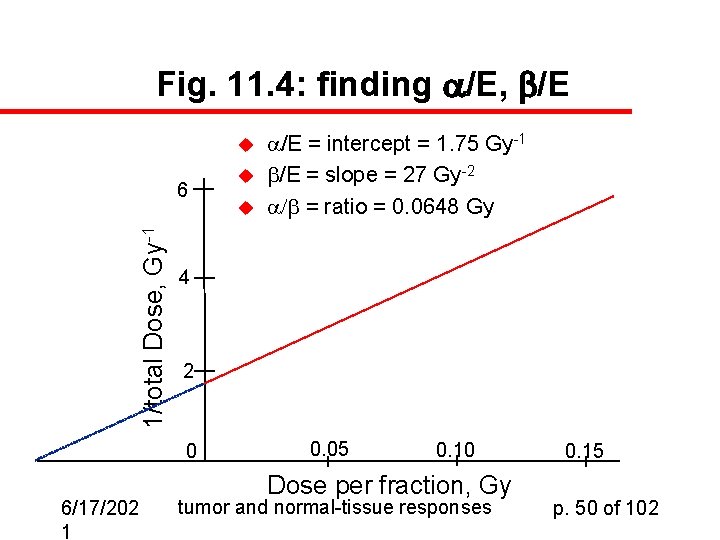
Fig. 11. 4: finding a/E, b/E u 1/total Dose, Gy-1 6 u 4 2 0 6/17/202 1 u /E = intercept = 1. 75 Gy-1 /E = slope = 27 Gy-2 / = ratio = 0. 0648 Gy 0. 05 0. 10 Dose per fraction, Gy tumor and normal-tissue responses 0. 15 p. 50 of 102

Applicability u u We don’t have to be using an LQ model to work with the Douglas-Fowler formulation; we just need a nonzero slope of ln. S vs. D at low dose. Thus MTSH doesn’t work: With MTSH, S= 1 - (1 - exp(-D/D 0))n For n > 1, d. S/d. D = -n(1 -exp(-D/D 0))n-1 at D = 0, d. S/d. D = -n(1 -e 0)n-1= -n(0)n-1 = 0. For n = 1, S = exp(-D/D 0) d. S/d. D = (-1/D 0)exp(-D/D 0) at D = 0, d. S/d. D = (-1/D 0)e-0 = -1/D 0 ≠ 0. 6/17/202 1 tumor and normal-tissue responses p. 51 of 102

Withers extension of Fe model u u Define flexure dose as the dose per fraction below which no further protection is provided by interfraction repair. It turns out the flexure dose is a multiple of / (units are correct: / is in Gy) 6/17/202 1 tumor and normal-tissue responses p. 52 of 102

Withers extension: results u u u Let’s pick a reference total dose Dref and a reference dose per fraction ref. Then -ln. Sref = Nref( ref + ref 2), where Nref is the reference number of doses (Dref= Nref ref) Then for a different total dose D and different dose per fraction , D = N , -ln. S= N ( + 2) 6/17/202 1 tumor and normal-tissue responses p. 53 of 102

Withers result u u u In order for the reference regimen to have the same effect as the test regimen, S = Sref, or -ln. S = -ln. Sref Therefore Nref( ref + ref 2) = N( + 2), i. e. Nref + Nref 2 = N + N 2 But Nref = Dref and N = D, so Nref 2 = Dref and N 2 = D Thus Dref( + ref) = D( + ) D/Dref = ( + ref)/ ( + ) = ( / + ref)/( / + ) 6/17/202 1 tumor and normal-tissue responses p. 54 of 102

Withers plot (fig. 11. 5) Comparison of three different Isoeffect curves, depending on / (with ref = 2 Gy): Yellow: α/β=10 Gy Red: α/β=3. 33 Gy Blue: α/β=1. 66 Gy 6/17/202 1 tumor and normal-tissue responses p. 55 of 102

Homework for later in July u u [This is a variation on problem 1 of chapter 11 in the book. I don't understand the wording of Alpen's problem, so I made up my own version] Suppose that the Ellis power law equation (11. 2) is valid in a particular tissue. A typical tumor dosing regimen consists of twenty treatments over four weeks using weekdays only, i. e. 26 days from the first Monday through the last Friday. Thus if the total dose delivered is 60 Gy, we deliver 3 Gy in each of the 20 treatments. 6/17/202 1 tumor and normal-tissue responses p. 56 of 102

Homework for later in July, continued u (a) Assuming NSD=17 Gy, calculate the tolerance dose associated with this regimen. Will we be able to deliver this treatment regimen without damage to the normal tissue? 6/17/202 1 tumor and normal-tissue responses p. 57 of 102

Homework, concluded u (b) If we wish to shorten the treatment time to three weeks (19 days from the first Monday to the last Friday) we will have to deliver larger doses per day, e. g. 60/19 = 3. 16 Gy/day if we include weekends. If we allow more than one dose delivery per day we can reduce the dose delivered in each treatment back to lower levels, though (1. 052 Gy/treatment). Calculate the number of doses we will have to deliver over the 19 -day period if we wish to ensure that the full 60 Gy will be tolerated. Determine the dose per treatment. 6/17/202 1 tumor and normal-tissue responses p. 58 of 102

Stochastic Effects u u These are defined as effects for which the percentage of the population affected by the exposure is dependent on dose BUT the severity of the [medical] condition in an individual is independent of dose. 6/17/202 1 tumor and normal-tissue responses p. 59 of 102

Does cancer really work that way? u u Not entirely Fry (1976): – – u Harderian gland tumors seldom invasive after low doses of low LET radiation More invasivity and metastasis after higher doses of low LET radiation Ullrich & Storer (1979): maybe there’s a threshold dose 6/17/202 1 tumor and normal-tissue responses p. 60 of 102
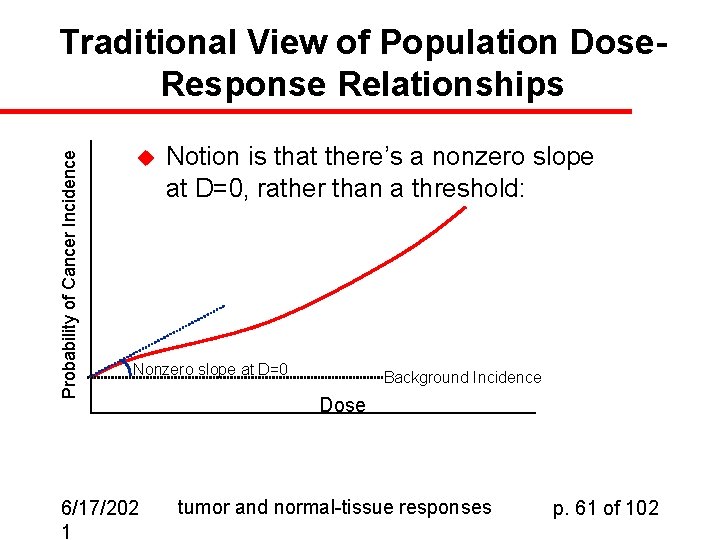
Probability of Cancer Incidence Traditional View of Population Dose. Response Relationships u Notion is that there’s a nonzero slope at D=0, rather than a threshold: Nonzero slope at D=0 6/17/202 1 Background Incidence Dose tumor and normal-tissue responses p. 61 of 102
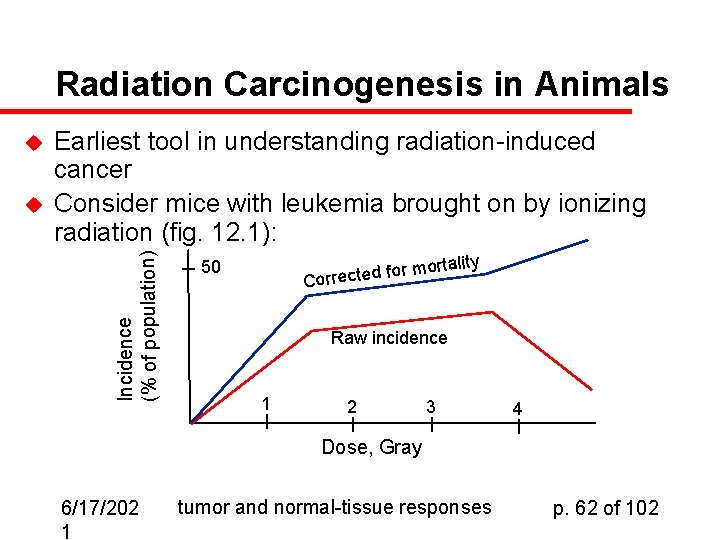
Radiation Carcinogenesis in Animals u Earliest tool in understanding radiation-induced cancer Consider mice with leukemia brought on by ionizing radiation (fig. 12. 1): Incidence (% of population) u rtality o m r o f d Correcte 50 Raw incidence 1 2 3 4 Dose, Gray 6/17/202 1 tumor and normal-tissue responses p. 62 of 102
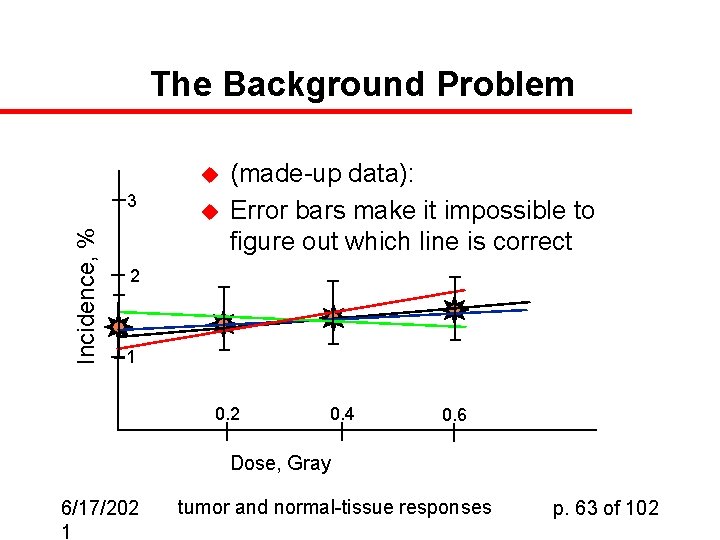
The Background Problem u Incidence, % 3 u (made-up data): Error bars make it impossible to figure out which line is correct 2 1 0. 2 0. 4 0. 6 Dose, Gray 6/17/202 1 tumor and normal-tissue responses p. 63 of 102
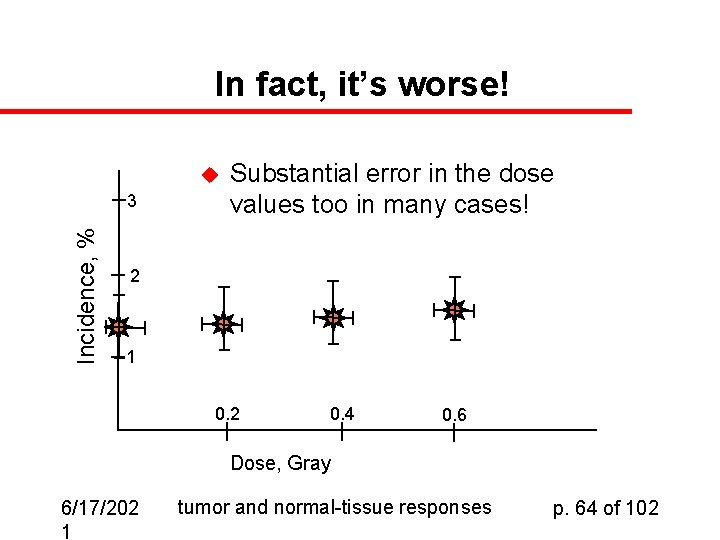
In fact, it’s worse! u Incidence, % 3 Substantial error in the dose values too in many cases! 2 1 0. 2 0. 4 0. 6 Dose, Gray 6/17/202 1 tumor and normal-tissue responses p. 64 of 102
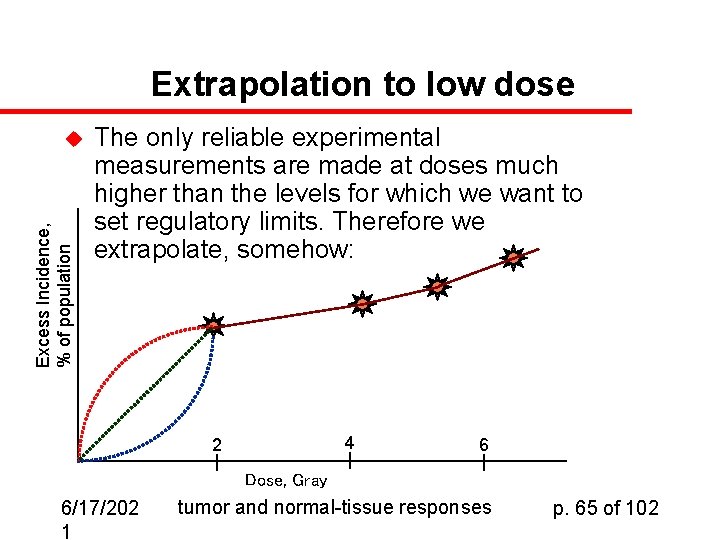
Extrapolation to low dose Excess Incidence, % of population u The only reliable experimental measurements are made at doses much higher than the levels for which we want to set regulatory limits. Therefore we extrapolate, somehow: 4 2 6 Dose, Gray 6/17/202 1 tumor and normal-tissue responses p. 65 of 102

Differential Sensitivity u Some individuals within a population are more susceptible than others – – u To tumors To other conditions Why? – – 6/17/202 1 Defective DNA repair mechanisms Problems in cell signaling Lifestyle agents (smoking, drinking, lack of exercise) Genetic differences among individuals tumor and normal-tissue responses p. 66 of 102
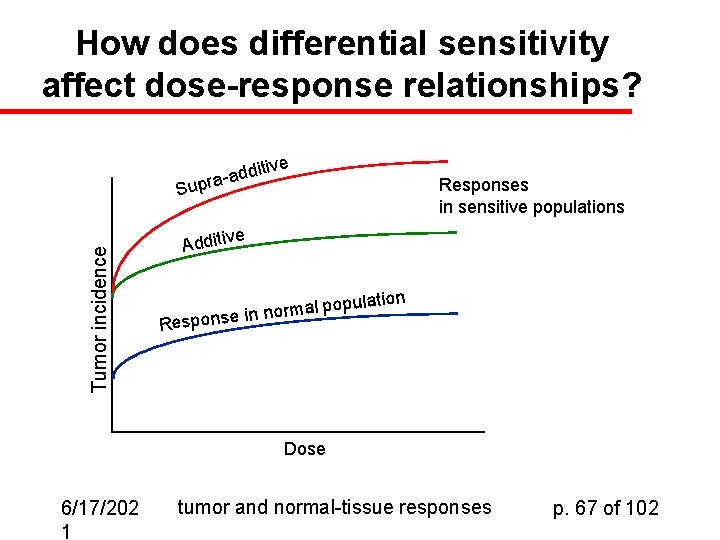
How does differential sensitivity affect dose-response relationships? ive dit d a a pr Tumor incidence Su Responses in sensitive populations e Additiv n opulatio p l a m r o n nse in Respo Dose 6/17/202 1 tumor and normal-tissue responses p. 67 of 102
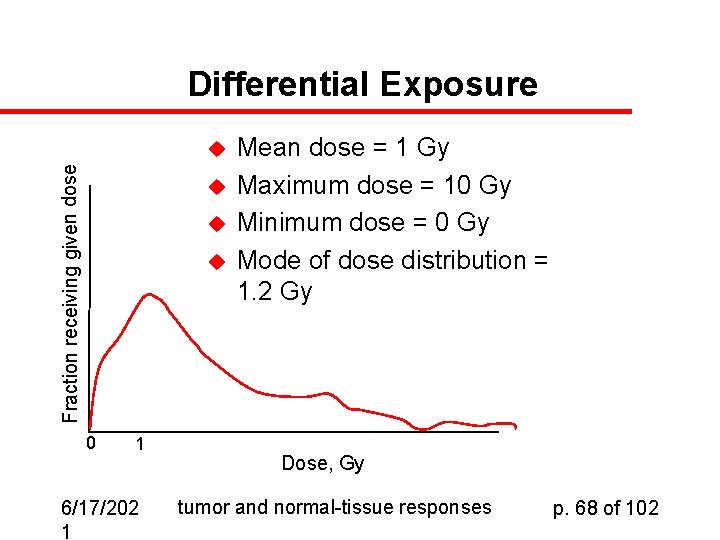
Differential Exposure Fraction receiving given dose u u 0 1 6/17/202 1 Mean dose = 1 Gy Maximum dose = 10 Gy Minimum dose = 0 Gy Mode of dose distribution = 1. 2 Gy Dose, Gy tumor and normal-tissue responses p. 68 of 102

Upton’s Summary of the Animal Data u u u Neoplasms of almost any type can be induced by irradiation of a suitable animal in a suitable way. Not every type of neoplasm is increased in frequency by irradiation of animals of one strain. Carcinogenic effects are interconnected through a variety of mechanisms. Some mechanisms involve direct effects on the tumor-forming cells; others don’t. High-LET radiation produces dose-dependent rather than dose-rate-dependent effects 6/17/202 1 tumor and normal-tissue responses p. 69 of 102

Upton, continued u u u Development of tumors is multicausal and multistage; effects of radiation may be modified by other agents. Low to intermediate doses produce no tumors unless promoted by other agents. At high doses the effect is suppressed by sterilization of potentially transformed cells; this causes saturation. Time distribution of appearance of tumors varies with type of tumor, genetics and age, conditions of irradiation. Dose-response curves vary significantly. 6/17/202 1 tumor and normal-tissue responses p. 70 of 102
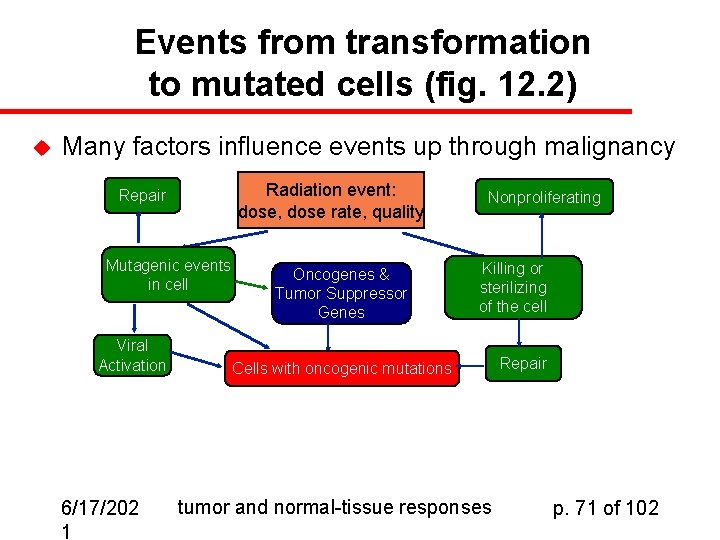
Events from transformation to mutated cells (fig. 12. 2) u Many factors influence events up through malignancy Radiation event: dose, dose rate, quality Repair Mutagenic events in cell Viral Activation 6/17/202 1 Oncogenes & Tumor Suppressor Genes Nonproliferating Killing or sterilizing of the cell Cells with oncogenic mutations tumor and normal-tissue responses Repair p. 71 of 102
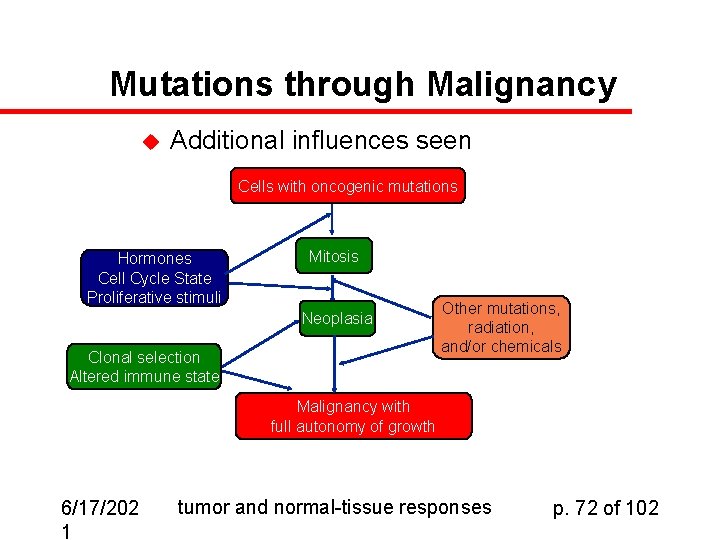
Mutations through Malignancy u Additional influences seen Cells with oncogenic mutations Hormones Cell Cycle State Proliferative stimuli Mitosis Neoplasia Clonal selection Altered immune state Other mutations, radiation, and/or chemicals Malignancy with full autonomy of growth 6/17/202 1 tumor and normal-tissue responses p. 72 of 102

Tumors: Definitions u Tumor: abnormal, de-differentiated cellular proliferation – – u u Benign: small mass reaches a certain size and then stops growing Malignant: those capable of uncontrolled growth & metastasis Cancer: a malignant tumor Carcinogen: a chemical or physical agent that increases the likelihood of cancer 6/17/202 1 tumor and normal-tissue responses p. 73 of 102

Cancer: Prevalence and Significance u u 550, 000 cancer deaths per year in the US 20 -40% caused by environmental and workplace agents Others caused by smoking, diet, and natural causes Teasing apart these statistics is tricky: – – Probability of any individual getting cancer under a particular set of circumstances is small Multistage model makes multiple causes likely 6/17/202 1 tumor and normal-tissue responses p. 74 of 102
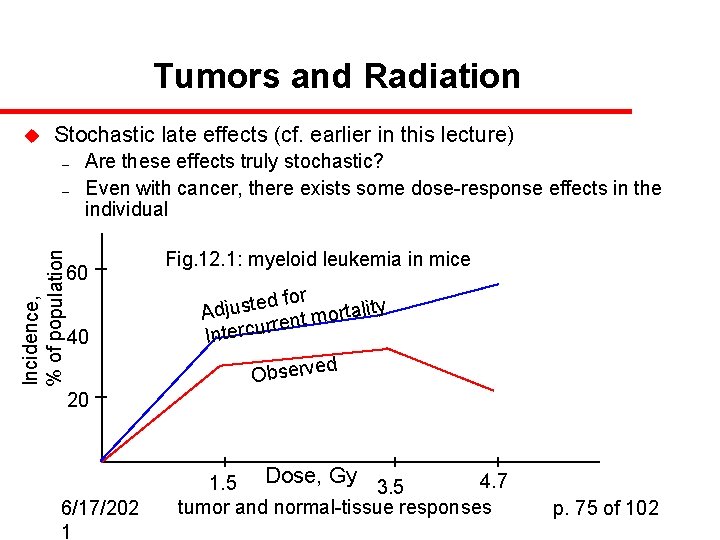
Tumors and Radiation u Stochastic late effects (cf. earlier in this lecture) – Incidence, % of population – Are these effects truly stochastic? Even with cancer, there exists some dose-response effects in the individual 60 40 Fig. 12. 1: myeloid leukemia in mice for d e t s u j ality t r Ad o m t rren Intercu d Observe 20 6/17/202 1 4. 7 1. 5 Dose, Gy 3. 5 tumor and normal-tissue responses p. 75 of 102
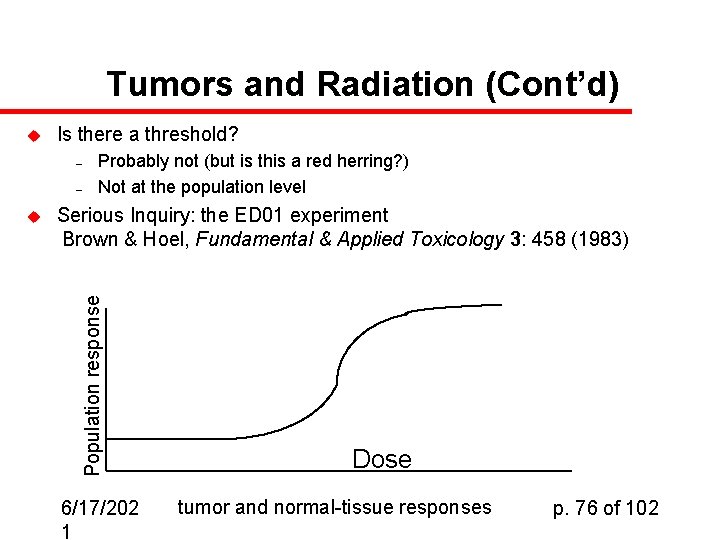
Tumors and Radiation (Cont’d) u Is there a threshold? – – Serious Inquiry: the ED 01 experiment Brown & Hoel, Fundamental & Applied Toxicology 3: 458 (1983) Population response u Probably not (but is this a red herring? ) Not at the population level 6/17/202 1 Dose tumor and normal-tissue responses p. 76 of 102

Upton’s rules (remember? ) u u u u Irradiation can produce almost any kind of neoplasm if we do it right Not every type of neoplasm has its incidence increased by irradiation of animals of any one species or strain Carcinogenic effects depend on a variety of mechanisms Some effects are direct, some are indirect Incidence rises more steeply with dose for high-LET radiation than for low-LET radiation Irradiation interacts with other causative agents Promotion may depend on other agents 6/17/202 1 tumor and normal-tissue responses p. 77 of 102

How do Cancers Begin? : The Clonal Theory u u u In general, mutational events in a single cell are sufficient to begin the process of tumorigenesis Often several mutations must arise in order for cancer to be a likely outcome Generally the mutation must be in one of the 50 or so genes that control cell replication and differentiation The mutagenic events are never enough to guarantee development of cancer (but that still leaves open the possibility that radiation could cause cancer all by itself, if it can act as a promoter too …) Mutations must be followed by promotional events, which stimulate uncontrolled cell division 6/17/202 1 tumor and normal-tissue responses p. 78 of 102
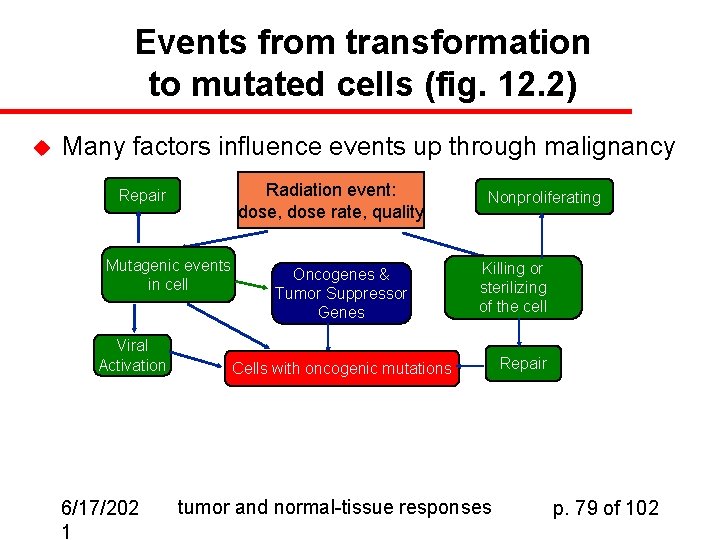
Events from transformation to mutated cells (fig. 12. 2) u Many factors influence events up through malignancy Radiation event: dose, dose rate, quality Repair Mutagenic events in cell Viral Activation 6/17/202 1 Oncogenes & Tumor Suppressor Genes Nonproliferating Killing or sterilizing of the cell Cells with oncogenic mutations tumor and normal-tissue responses Repair p. 79 of 102
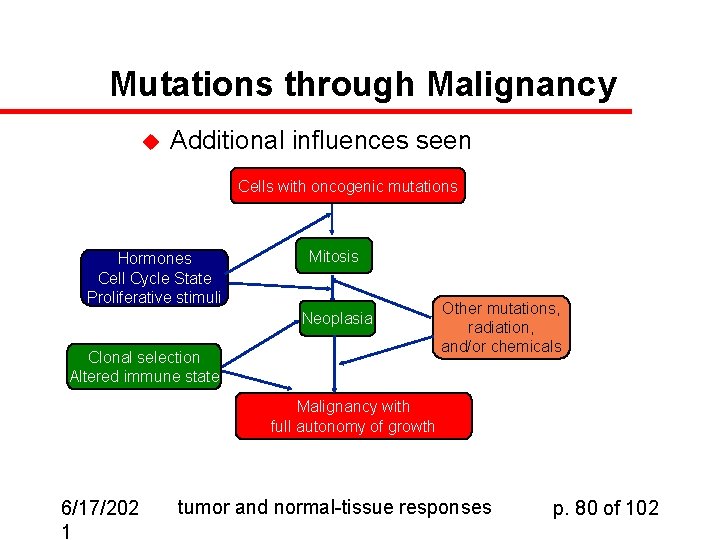
Mutations through Malignancy u Additional influences seen Cells with oncogenic mutations Hormones Cell Cycle State Proliferative stimuli Mitosis Neoplasia Clonal selection Altered immune state Other mutations, radiation, and/or chemicals Malignancy with full autonomy of growth 6/17/202 1 tumor and normal-tissue responses p. 80 of 102
Modifying Factors 6/17/202 1 u Immune system u Hormonal effects u Oncogenes u Oncogenic viruses u Environmental factors tumor and normal-tissue responses p. 81 of 102

How Cancers Develop: The Multistage Theory u Initiation – – u Promotion – – – u DNA damage e. g. Intercalators Generally not mutational Involves changes in control systems, e. g. arachidonic acid cascade Tumors are present and capable of metastasis but haven’t necessarily metastisized Progression – Development of metastatic tumors 6/17/202 1 tumor and normal-tissue responses p. 82 of 102
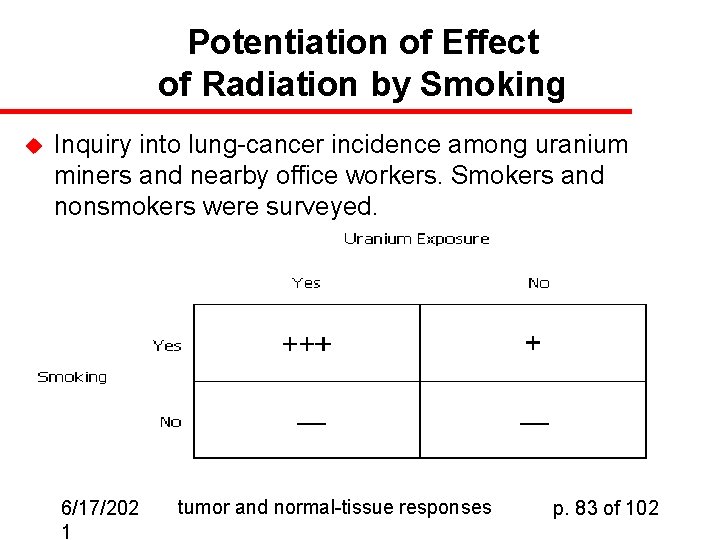
Potentiation of Effect of Radiation by Smoking u Inquiry into lung-cancer incidence among uranium miners and nearby office workers. Smokers and nonsmokers were surveyed. 6/17/202 1 tumor and normal-tissue responses p. 83 of 102

How do we study radiation-induced carcinogenesis? u u u Induction and progress of cancer in experimental animals Transformation of cells grown in tissue culture Human epidemiological studies – – – Accidental exposures: Radium-dial workers, Chernobyl victims, foot fluoroscopes Medicinal exposures Atomic bomb victims 6/17/202 1 tumor and normal-tissue responses p. 84 of 102

What Constitutes a Cancer? u u u 6/17/202 1 Morphological change Cell immortality (escape from apoptosis) Tumorigenicity, i. e. spread of undifferentiated cells tumor and normal-tissue responses p. 85 of 102

Oncogenes u u Genes that are activated or show enhanced expression in tumors Limited data showing connection between human radiation-induced tumors and activation of oncogenes 6/17/202 1 tumor and normal-tissue responses p. 86 of 102

ED 01 study u u We mentioned this a bit earlier Study run by scientists at the National Institute of Environmental Health Sciences in Research Triangle Park, North Carolina BALB-C mice analyzed for liver tumors Test compound was 2 -acetylaminofluorene, a known carcinogen in rodents: 6/17/202 1 tumor and normal-tissue responses p. 87 of 102

ED 01 study, continued u u 24000 mice in various exposure groups Endpoints and elements of study: – – u Sophisticated statistical analyses: – – u Time to tumor incidence Dose “fractionation” (but this is a chemical) Initial analyses around 1981 Re-analysis a few years later Compared various dose-response models 6/17/202 1 tumor and normal-tissue responses p. 88 of 102

ED 01 quantitation u u u Analyze tumor incidence according to P(t, d) = 1 - exp(-F(t, d)), where t = time and d = dose. P, the tumor incidence fraction, behaves like 1 -S in our survival curve studies Some analyses suggest that 2 -AAF is primarily a promotor, not an initiator – – So it isn’t a great model for what radiation does… But it still illustrates the importance of careful statistics! 6/17/202 1 tumor and normal-tissue responses p. 89 of 102

Experimental Systems for Studying Rad-induced Tumors u u We need these because we can’t deliberately do high-dose experiments on humans! CHO cells – – u Chinese Hamster Ovary Good for looking at early effects--Initiation Difficult to model the promotional events. Transformation results in loss of contact inhibition Mouse embryo fibroblasts – – Immortalized Still display contact inhibition 6/17/202 1 tumor and normal-tissue responses p. 90 of 102
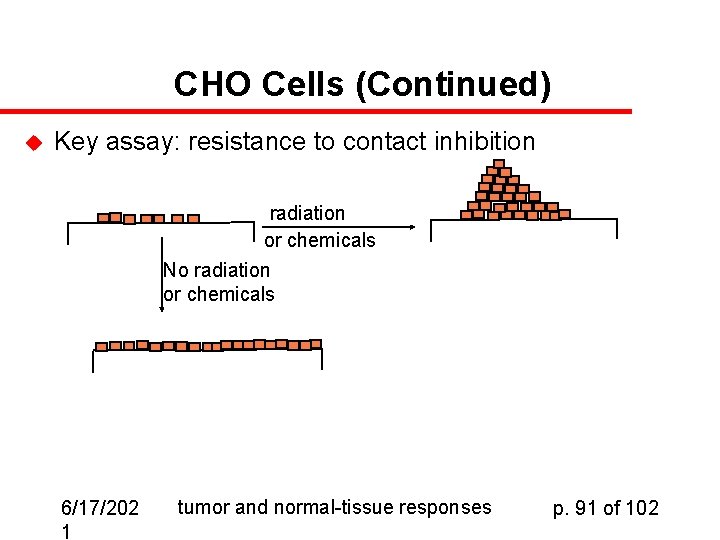
CHO Cells (Continued) u Key assay: resistance to contact inhibition radiation or chemicals No radiation or chemicals 6/17/202 1 tumor and normal-tissue responses p. 91 of 102

Mouse Embryo Cells: u Experiment: growing total confluence Lose contact inhibition? Can induce tumors in syngeneic animals u Limitation in both systems: u u – – Fibroblasts (mesenchymals) Most human tumors are epithelial 6/17/202 1 tumor and normal-tissue responses p. 92 of 102

Mutagenesis u u u Many chemicals, as well as radiation, can be shown to cause mutations. It is therefore logical to test for mutagenicity as a first-stage inquiry into the likelihood that a compound or a radiation treatment might be carcinogenic Standard mutagenic test: The Ames test (developed by Bruce Ames), in which Salmonella cells are exposed to a chemical and mutation rates in the cells are measured. 6/17/202 1 tumor and normal-tissue responses p. 93 of 102

Is an Ames Test a Good Substitute for These Complex Systems? u u No! 1, 8 -dinitropyrene is the most mutagenic substance known in the Ames test; yet it is only weakly tumorigenic in rats. NO 2 6/17/202 1 tumor and normal-tissue responses p. 94 of 102

Why might we care about dinitropyrene? u u u Most mutagenic substance known in Salmonella strain TA 98: 72900 revertants/nanomole Nitroarenes like this one were found to be present in used toner, i. e. , combustion waste from Xerox toner When this appeared, Xerox chemists reformulated their toner to drastically reduce the nitroarene content in the used toner. Mermelstein (1981) Mutation Research 89: 187 -196. Löfroth et al(1980) Science 209: 1037 -1039 and Mermelstein et al (1980) Science 209: 1039 -1043. So: all’s well that ends well! 6/17/202 1 tumor and normal-tissue responses p. 95 of 102

This is also a story about enzyme induction u u u Nitroarenes like dinitropyrene and other polynuclear aromatic hydrocarbons, (e. g. benzo(a)pyrene) are known to be inducers of enzyme activities Some of these enzyme activities actually activate toxicants rather than detoxifying them Most of the activity of these enzymes will detoxify; But if 1% makes things worse, we want to understand that 1% activation So we found that pretreatment with these compounds could induce subsequent binding of other compounds to mouse DNA: Howard et al (1986), Biochem. Pharm. 35: 2129 -2134. 6/17/202 1 tumor and normal-tissue responses p. 96 of 102

Animal Cell-Line Cancer Studies u u How similar are these rodent cell systems (CHO, mouse) to human cells? Answer: Human cells: – – – 6/17/202 1 Are more resistant to spontaneous immortalization Tend to give more nearly linear responses to dose Radical scavengers and cold don’t protect as much: That suggests that direct mechanisms prevail in humans and indirect mechanisms are more important in rodents tumor and normal-tissue responses p. 97 of 102

More on humans vs. rodents u u u 6/17/202 1 High-LET studies indicate that repair is less effective in humans than in humans Is the timescale a factor in that? Humans live a lot longer than rodents. Promotion can be studied in animal cells, along with initiation tumor and normal-tissue responses p. 98 of 102

Radiation Carcinogenesis in Human Populations u u Occupational: radiologists, miners, dial painters Medical exposures: – – – u u Ankylosing spondylitis Nonmalignant disease in pelvis and breast Multiple fluoroscopies in to chest (e. g. in TB patients) Infants & children with enlarged thymus and ringworm Children exposed in utero to diagnostic X-rays Nuclear accidents and weapon detonations Environmental background (see last chapter) 6/17/202 1 tumor and normal-tissue responses p. 99 of 102

Dose-Incidence in Cancer Studies u u u We seek a relationship relating post-exposure incidence ID to dose D and normal incidence In Model might be: Linear: ID = In + 1 D Quadratic: ID = In + 2 D 2 LQ: ID = In + 1 D + 2 D 2 Corrected for loss of clonogenic potential: ID = (In + 1 D + 2 D 2)exp(- 1 D+ 2 D 2) 6/17/202 1 tumor and normal-tissue responses p. 100 of 102
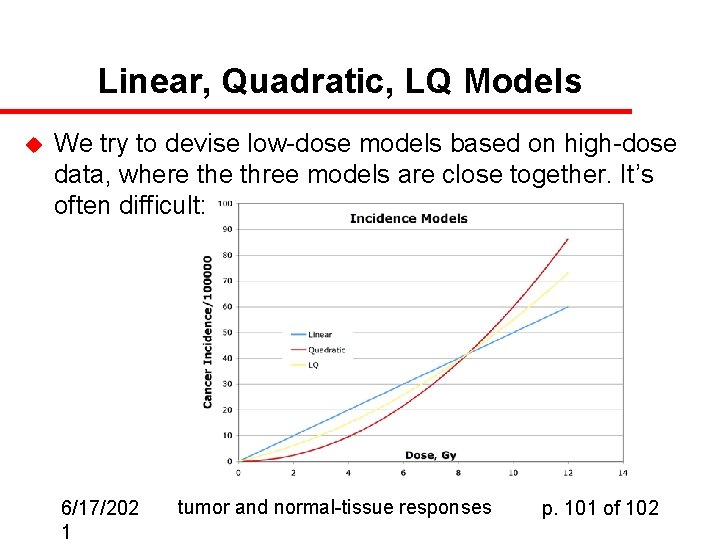
Linear, Quadratic, LQ Models u We try to devise low-dose models based on high-dose data, where three models are close together. It’s often difficult: 6/17/202 1 tumor and normal-tissue responses p. 101 of 102

Latency u u Definition (in the cancer context): Time between the mutational events that began cellular transformation and the appearance of a medically observable malignancy How long in humans? – – A few years (blood or lymphatic cancers) 15 -30 years for solid tumors Animals: scale these numbers to animal’s lifespan These numbers are minima: leukemia can take > 15 yrs 6/17/202 1 tumor and normal-tissue responses p. 102 of 102
- Slides: 102