IHI Open School Chapter presentation Pierre M Barker

IHI Open School Chapter presentation Pierre M Barker MD Senior Vice President IHI Clinical Professor, Gillings School of Global Public Health, UNC

Our Mission To improve health and health care worldwide.
Our Mission To improve health and health care worldwide. Who We Are What We Will Improve Where We Work An Innovator Quality, Cost, and Value North America A Convener Patient Safety Latin America Europe Triple Aim for Populations A Partner A Driver of Results Middle East Person- and Family-Centered Care Africa Improvement Capability Asia Pacific QI + Joy in Work

P 4 How does IHI use QI to do its work?
Penicillin The Nobel Prize for Medicine was awarded in 1945 to: Sir Alexander Fleming Ernst B. Chain Sir Howard Florey

Penicillin 1928 From a single petri dish he had discarded, Alexander Fleming identified a mold and named it Penicillin. 1930 s Fleming tried with limited success to produce and test the effects of Penicillin as a surface antiseptic. 1939 Ernst Chain took an interest in Fleming’s work and with Howard Florey identified the active ingredient and produced it in larger quantities. Tested it by injecting Penicillin into two infected mice – who recovered.

Penicillin 1940 s With Norman Heatley, produced sufficient quantities to test penicillin in fifty mice. Tested it in three people who were dying from bacterial infections. Subsequent successful clinical trials led to funding to mass produce Penicillin. 1945 Sir Alexander Fleming, Ernst Chain & Sir Howard Florey awarded Nobel Prize for Medicine

Penicillin Sir Henry Harris said at the Florey Centenary lecture in 1998: "Without Fleming, no Chain; without Chain, no Florey; without Florey, no Heatley; without Heatley, no penicillin. “ Or: Without Fleming, no discovery; without Chain and Florey, no testing, without Heatley, no wide scale use of penicillin

After Fleming, Chain, Florey, Heatley Antibiotic Misuse For pediatric care, a study showed that doctors prescribe antibiotics 62% of the time if they perceive parents expect them and 7% of the time if they feel parents do not expect them. [1] Antibiotics were prescribed in 68% of acute respiratory tract visits – and of those, 80% were unnecessary according to CDC guidelines. [2] $1. 1 billion is spent annually on unnecessary adult upper respiratory infection antibiotic prescriptions. [5] http: //www. cdc. gov/getsmart/antibiotic-use/fast-facts. html 9

What is the Quality “Gap” “US adults receive 55% of scientifically indicated care (Acute: 53. 5%; Chronic: 56. 1%; Preventive: 54. 9%)” Beth Mc. Glynn , NEJM 2003 “ 4 million women, newborns and children in sub-Saharan Africa could be saved every year if well-established, currently available, affordable health care interventions could be implemented across the region” Joy Lawn, African Academies of Science , Accra, December 2009 10

What is the Quality problem? Basic science Proof of concept (efficacy) Large scale effectiveness Studies (RCTs) Reliable “real-life” implementation Scale-up
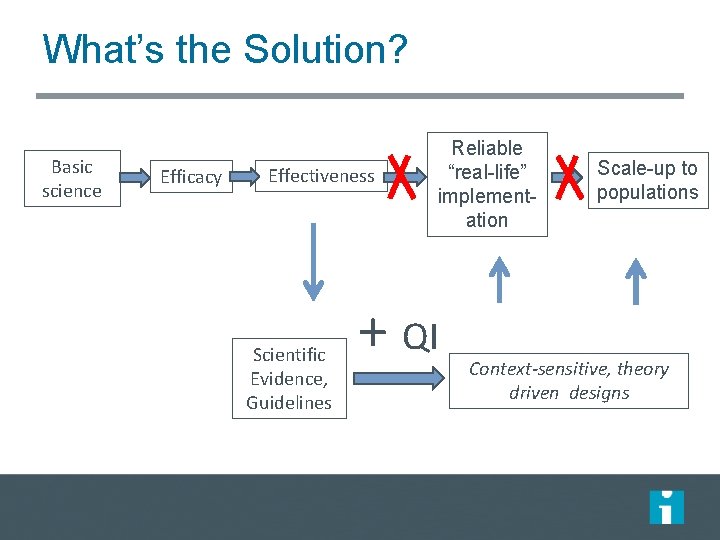
What’s the Solution? Basic science Efficacy Effectiveness Scientific Evidence, Guidelines Reliable “real-life” implementation + QI Scale-up to populations Context-sensitive, theory driven designs

13 What is the Science behind QI and how can we use it to design better programs?

Quality Improvement: Bringing Together Two Types of Knowledge Evidence Based Subject Matter Knowledge Protocols/Guidelines, Physical resources, Clinical Training the “what” the “how” Implementation Knowledge Motivation/Leadership Efficient Systems Accurate Reflective Data Context-sensitive learning
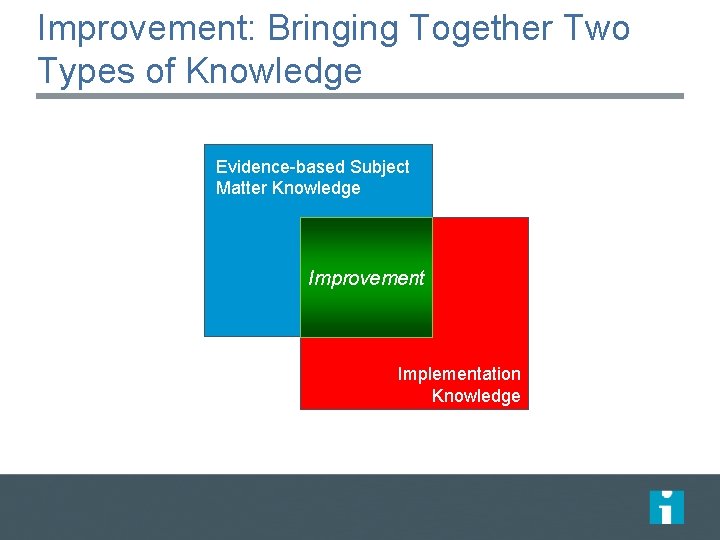
Improvement: Bringing Together Two Types of Knowledge Evidence-based Subject Matter Knowledge Improvement Implementation Knowledge
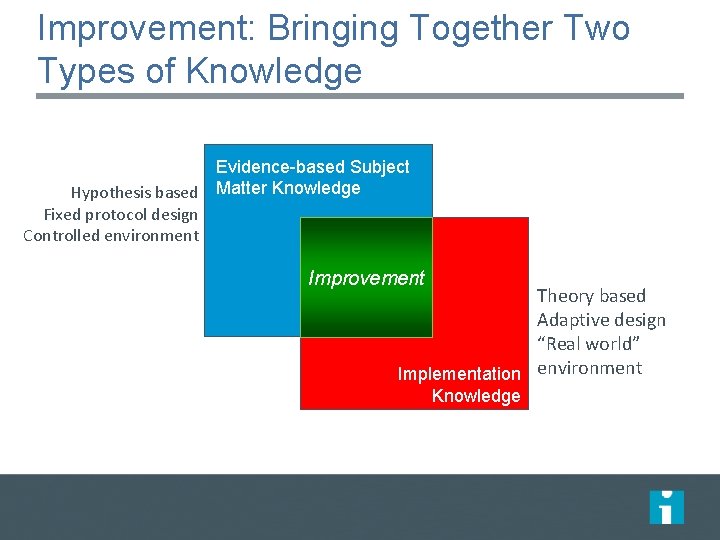
Improvement: Bringing Together Two Types of Knowledge Evidence-based Subject Hypothesis based Matter Knowledge Fixed protocol design Controlled environment Improvement Theory based Adaptive design “Real world” Implementation environment Knowledge
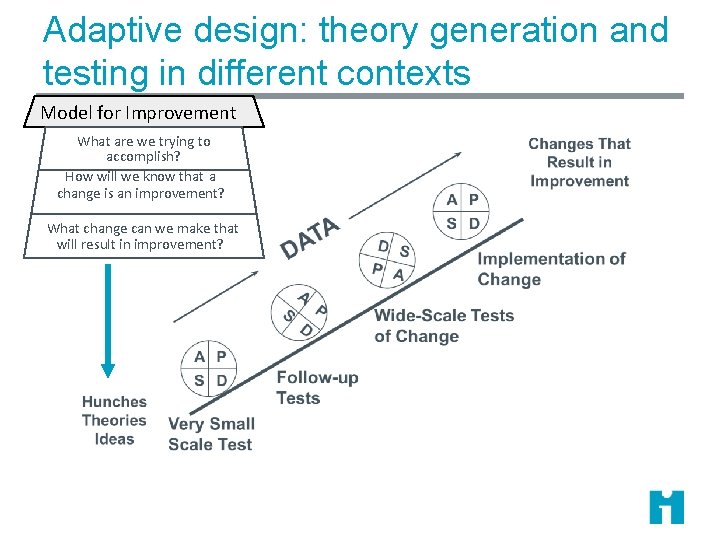
Adaptive design: theory generation and testing in different contexts Model for Improvement What are we trying to accomplish? How will we know that a change is an improvement? What change can we make that will result in improvement?

Case example: Antenatal Corticosteroids (ACS) for improving preterm survival 21 studies, 3885 women, 4269 infants • Treatment with ACS reduced neonatal death from prematurity by ~30% , RDS by ~44% • ACS not increase risk to the mother of death or sepsis. “ACS effective in women with premature rupture of membranes and pregnancy related hypertension syndromes. ”

Translating evidence to context
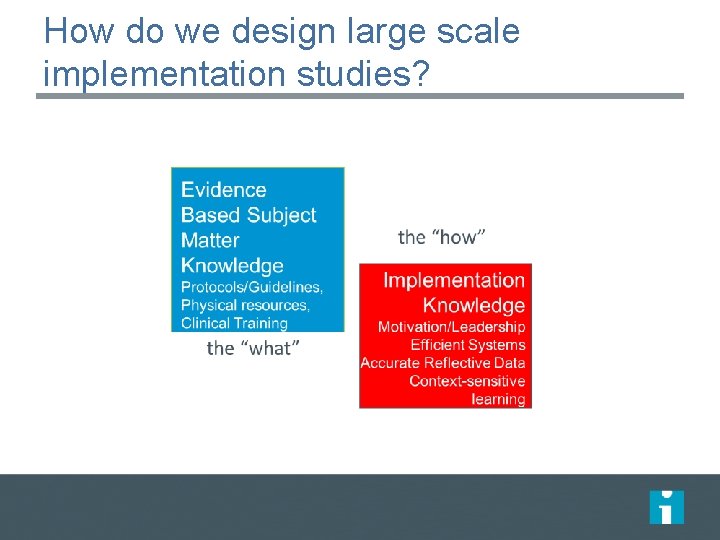
How do we design large scale implementation studies?
A different Approach to ACS: Malawi • 15. 9 million people • Neonatal mortality of 31/1000 live births (US 4/1000) • Major causes: Prematurity (45%), Neonatal sepsis and Asphyxia • Highest rate of prematurity worldwide (17%) • 75% women deliver in hospital Nkhoma Mission Hospital ≈ 5, 000 deliveries/yr no previous QI experience
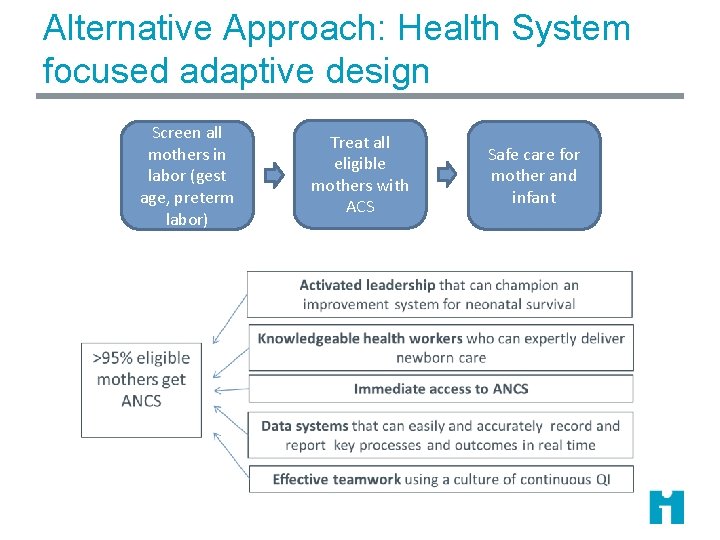
Alternative Approach: Health System focused adaptive design Screen all mothers in labor (gest age, preterm labor) Treat all eligible mothers with ACS Safe care for mother and infant

Methods: Moving research into hands of front line providers
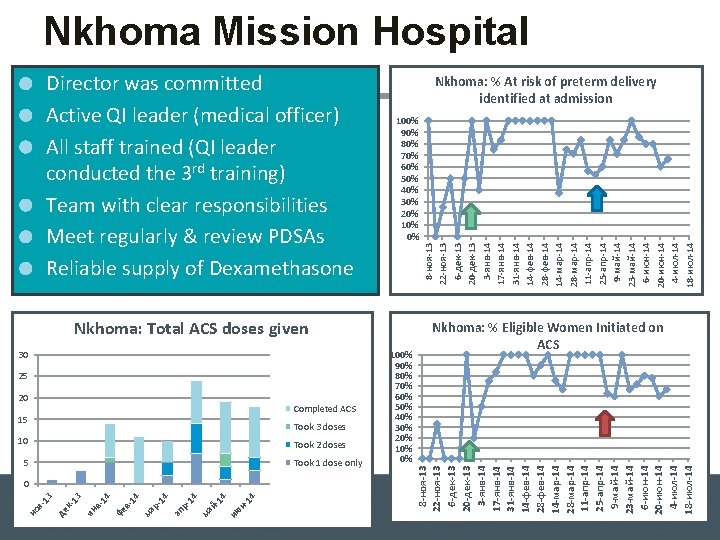
Nkhoma Mission Hospital Nkhoma: % At risk of preterm delivery identified at admission 8 -ноя-13 22 -ноя-13 6 -дек-13 20 -дек-13 3 -янв-14 17 -янв-14 31 -янв-14 14 -фев-14 28 -фев-14 14 -мар-14 28 -мар-14 11 -апр-14 25 -апр-14 9 -май-14 23 -май-14 6 -июн-14 20 -июн-14 4 -июл-14 18 -июл-14 100% 90% 80% 70% 60% 50% 40% 30% 20% 10% 0% Nkhoma: Total ACS doses given 30 25 20 Completed ACS 15 Took 3 doses 10 Took 2 doses 5 Took 1 dose only 14 4 ию н- -1 ма й 4 р14 ап р1 14 ма фе в- в 14 ян 13 кде но я- 13 0 100% 90% 80% 70% 60% 50% 40% 30% 20% 10% 0% Nkhoma: % Eligible Women Initiated on ACS 8 -ноя-13 22 -ноя-13 6 -дек-13 20 -дек-13 3 -янв-14 17 -янв-14 31 -янв-14 14 -фев-14 28 -фев-14 14 -мар-14 28 -мар-14 11 -апр-14 25 -апр-14 9 -май-14 23 -май-14 6 -июн-14 20 -июн-14 4 -июл-14 18 -июл-14 Director was committed Active QI leader (medical officer) All staff trained (QI leader conducted the 3 rd training) Team with clear responsibilities Meet regularly & review PDSAs Reliable supply of Dexamethasone

IHI Global Work
Transition to IHI Global

Regional structure and Leadership 27
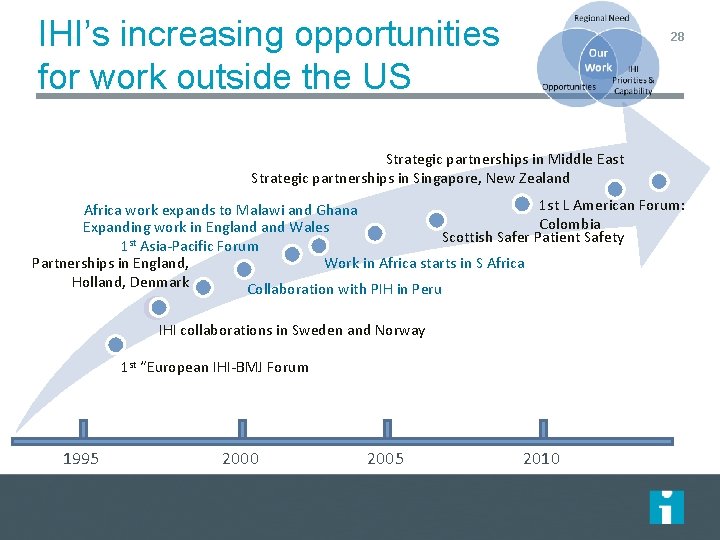
IHI’s increasing opportunities for work outside the US 28 Strategic partnerships in Middle East Strategic partnerships in Singapore, New Zealand 1 st L American Forum: Africa work expands to Malawi and Ghana Colombia Expanding work in England Wales Scottish Safer Patient Safety 1 st Asia-Pacific Forum Partnerships in England, Work in Africa starts in S Africa Holland, Denmark Collaboration with PIH in Peru IHI collaborations in Sweden and Norway 1 st “European IHI-BMJ Forum 1995 2000 2005 2010
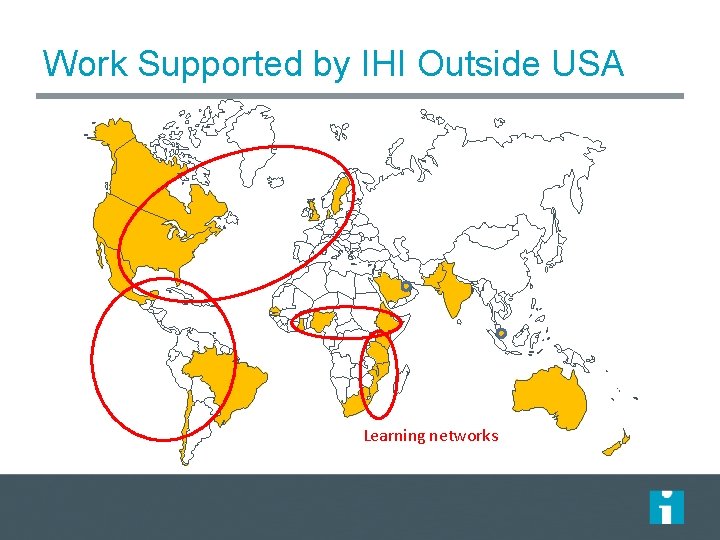
Work Supported by IHI Outside USA Learning networks
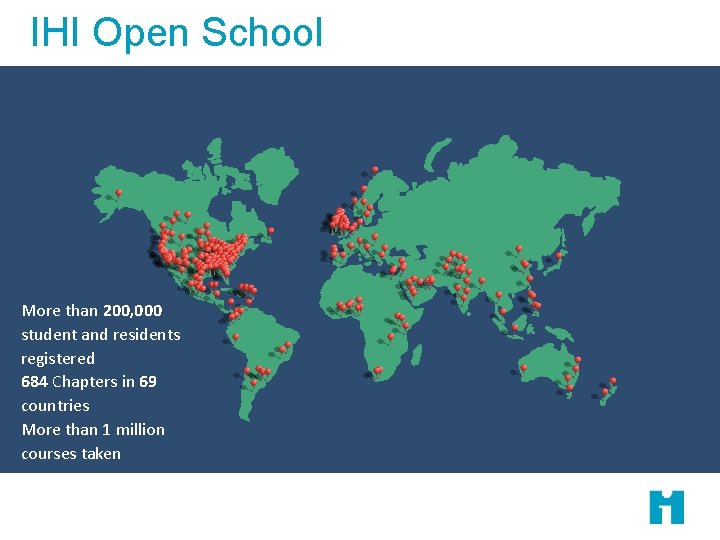
IHI Open School More than 200, 000 student and residents registered 684 Chapters in 69 countries More than 1 million courses taken

P 31 Thank you!
- Slides: 31