Ig E mediated hypersensitivity Allergens Most allergic Ig







- Slides: 12

Ig. E mediated hypersensitivity

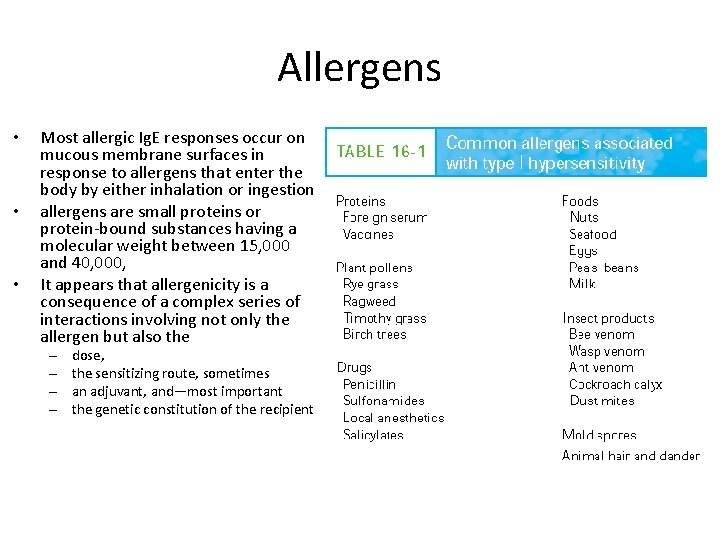
Allergens • • • Most allergic Ig. E responses occur on mucous membrane surfaces in response to allergens that enter the body by either inhalation or ingestion allergens are small proteins or protein-bound substances having a molecular weight between 15, 000 and 40, 000, It appears that allergenicity is a consequence of a complex series of interactions involving not only the allergen but also the – – dose, the sensitizing route, sometimes an adjuvant, and—most important the genetic constitution of the recipient

Effector mechanisms in lg. E-mediated allergic reactions • Mast-cell activation has different effects on different tissues • Mast cells line external mucosal surfaces and serve to alert the immune system to local infection • inflammatory reactions by secreting pharmacological mediators such as histamine stored in preformed granules and by synthesizing prostaglandins, leukotrienes, • Mast-cell activation has different and platelet -activating factor effects on different tissues from the plasma membrane

Ig. E- unique features • Unlike other antibodies, which are found mainly in body fluids, Ig. E is mostly found fixed on cells that carry this receptor-mast cells in tissues and basophils in the circulation • Serum Ig. E levels in normal individuals fall within the range of 0. 1– 0. 4 g/ml; even the most severely allergic individuals rarely have Ig. E levels greater than 1 g/ml • Ig. E is captured by the high-affinity Fce receptor (Fce. RI) in the absence of bound antigen • Ig. E was found to be composed of two heavy and two light chains with a combined molecular weight of 190, 000 • Mainly due to additional domain (CH 4) contributes to an altered conformation of the Fc portion of the molecule that enables it to bind to glycoprotein receptors on the surface of basophils and mast cells • Although the half-life of Ig. E in the serum is only 2– 3 days, once Ig. E has been bound to its receptor on mast cells and basophils, it is stable in that state for a number of weeks

Ig. E binding Fc receptors There are two types of Ig. E-binding Fe receptor • The first, Fce. RI, is a high affinity receptor of the immunoglobulin superfamily that binds Ig. E on mast cells and basophils • Between 40, 000 and 90, 000 Fce. RI molecules have been shown to be present on a human basophil The Fc. RI receptor contains four polypeptide chains: an and a chain and two identical disulfide-linked chains Fc. RI interact with the CH 3/CH 3 and CH 4/CH 4 domains of the Ig molecule via the two Ig-like domains of the chain Fc. RI Each chain of the high-affinity receptor contains an ITAM, a motif also present in the Ig-/Ig- heterodimer of the B-cell receptor and in the CD 3 complex of the T-cell receptor

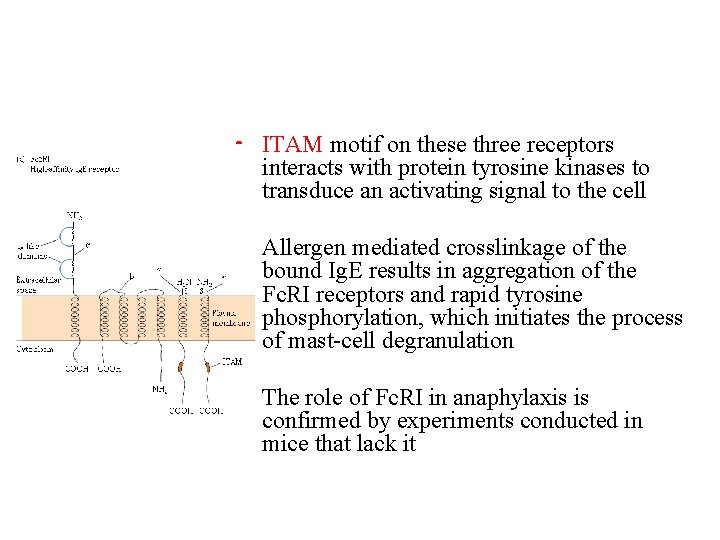
• ITAM motif on these three receptors interacts with protein tyrosine kinases to transduce an activating signal to the cell • Allergen mediated crosslinkage of the bound Ig. E results in aggregation of the Fc. RI receptors and rapid tyrosine phosphorylation, which initiates the process of mast-cell degranulation • The role of Fc. RI in anaphylaxis is confirmed by experiments conducted in mice that lack it

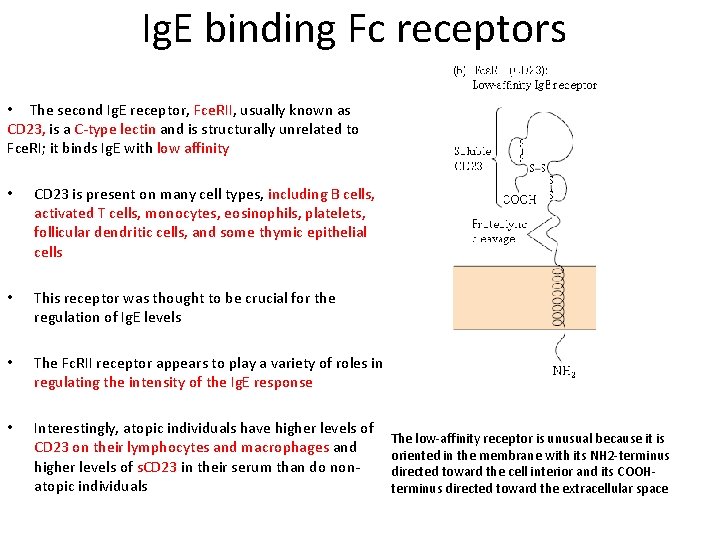
Ig. E binding Fc receptors • The second Ig. E receptor, Fce. RII, usually known as CD 23, is a C-type lectin and is structurally unrelated to Fce. RI; it binds Ig. E with low affinity • CD 23 is present on many cell types, including B cells, activated T cells, monocytes, eosinophils, platelets, follicular dendritic cells, and some thymic epithelial cells • This receptor was thought to be crucial for the regulation of Ig. E levels • The Fc. RII receptor appears to play a variety of roles in regulating the intensity of the Ig. E response • Interestingly, atopic individuals have higher levels of CD 23 on their lymphocytes and macrophages and higher levels of s. CD 23 in their serum than do nonatopic individuals The low-affinity receptor is unusual because it is oriented in the membrane with its NH 2 -terminus directed toward the cell interior and its COOHterminus directed toward the extracellular space

Mast cells • • • Mast cells were described by Ehrlich in the mesentery of rabbits and named Mastzellen ('fattened cells') Mast cells are derived from hematopoietic stem cells but mature locally often residing near surfaces exposed to pathogens and allergens, – such as mucosal tissues – connective tissues surrounding blood vessels Mast cell populations in different anatomic sites differ significantly in the types and amounts of allergic mediators they contain and in their sensitivity to activating stimuli and cytokines Mast cells also secrete a large variety of cytokines that affect a broad spectrum of physiologic, immunologic, and pathologic processes Human mast cells are classified on the basis of their protease content Mast cells of one class (MCT) predominantly express tryptase only, and these predominate in mucosal epithelia whereas those of another type (MCc. T) express tryptase, chymase, carboxypeptidase A, and cathepsin G and predominate in the submucosa and other connective tissues Granule released from mast cells may contents include the short-lived vasoactive amine histamine, serine esterases, and proteases such as chymase and tryptase

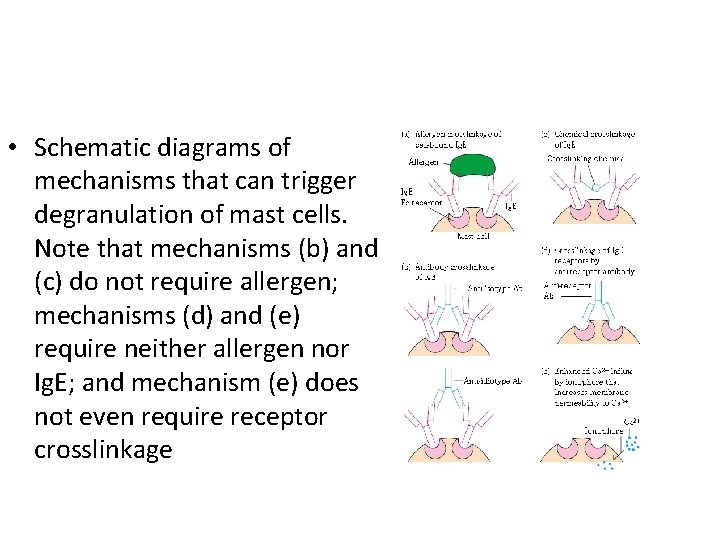
• Schematic diagrams of mechanisms that can trigger degranulation of mast cells. Note that mechanisms (b) and (c) do not require allergen; mechanisms (d) and (e) require neither allergen nor Ig. E; and mechanism (e) does not even require receptor crosslinkage


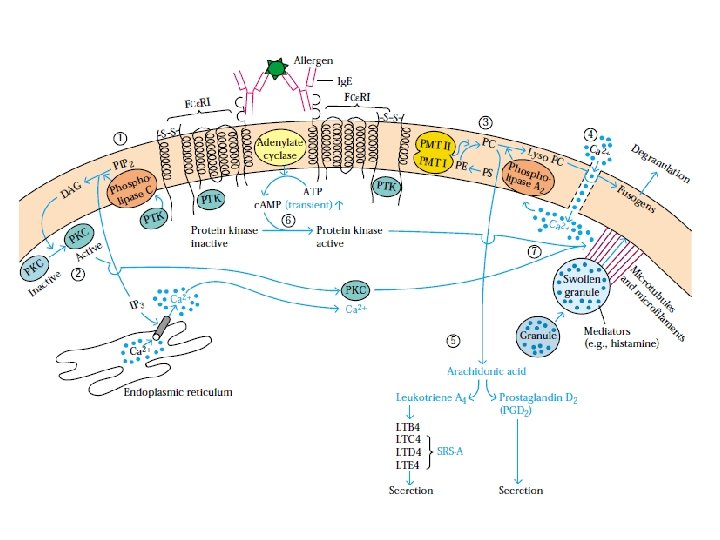
• Crosslinkage of the Fc. RI receptors activates PTKs, – resulting in the phosphorylation of tyrosines within the ITAMs of the subunit as well as – phosphorylation of residues on the subunit and on phospholipase C – second messengers • 15 s after crosslinkage of Fc. RI, methylation of various membrane phospholipids • increase in membrane fluidity and the formation of Ca 2+ channels • Increased Ca intake and release from intracellular stores • The Ca 2+ increase arachidonic acid, which is converted into two classes of potent mediators: prostaglandins and leukotrienes • the assembly of microtubules and the contraction of microfilaments helps in the release of granules

Several Pharmacologic Agents Mediate Type I Reactions • The mediators released during mast-cell or basophil degranulation determine the clinical manifestations • These mediators are pharmacologically active agents that act on – local tissues as well as on populations of secondary effector cells, including eosinophils, neutrophils, T lymphocytes, monocytes, and platelets