Identifying and Responding to Sepsis BC Sepsis Inpatient

Identifying and Responding to Sepsis BC Sepsis Inpatient Pilot Project On CP 10 CD VGH Presentation Based on the work done by: §Dr. David Sweet and colleagues from: BC Patient Safety & Quality Council and §VGH Sepsis Working Team: Dr. Sweet, Doris Bohl, Leighanne Mac. Kenzie, Dr. Mackenzie-Feder, Jenifer Tabamo, Alison Beaty, Suzanne Miller, Dr. Yousefi
Sepsis pathophysiology • What is Sepsis? Recognize symptoms • Identify the signs of sepsis in typical acute care patients Apply BC Sepsis Guidelines • Identify the actions that you need to take to treat septic patients

• 6, 000 deaths a year in the Developed world • 50 lives lost each HOUR due to Sepsis • World Sepsis Declaration: reduce incidence by 20% by 2020 • Pledge to: increase awareness, implement best practice, track positive care and management of sepsis • CP 10 CD will be involved in Sepsis care by trialing 2 documents: The Sepsis Screening Tool and the Early Investigation and Treatment PPO

What is Sepsis? Abnormality in at least 2 out of 5 of the following: • Heart rate • Respiratory rate • White blood cell count • Temperature • Change in LOC
Causes of Infection • Bacteria • Virus • Fungus
Sources of Infection • • Skin wounds Abscesses Urinary tract infections Pneumonia Gastro-intestinial Vascular Contaminated medical devices ie: CVC lines and other invasive instruments
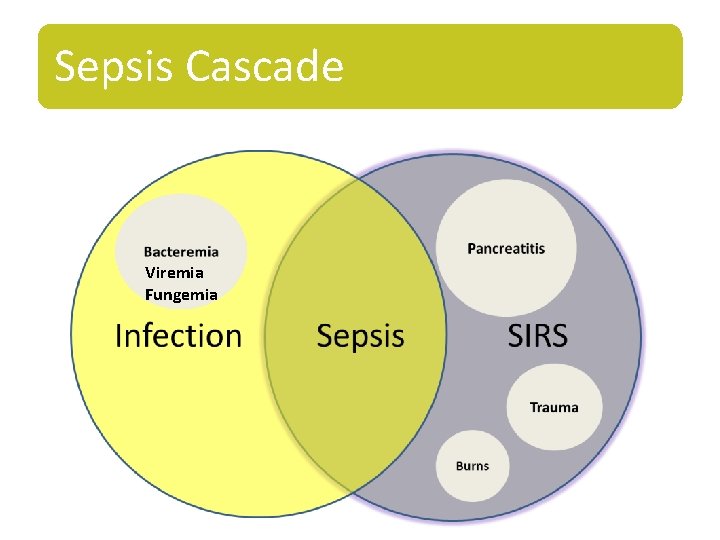
Sepsis Cascade Viremia Fungemia
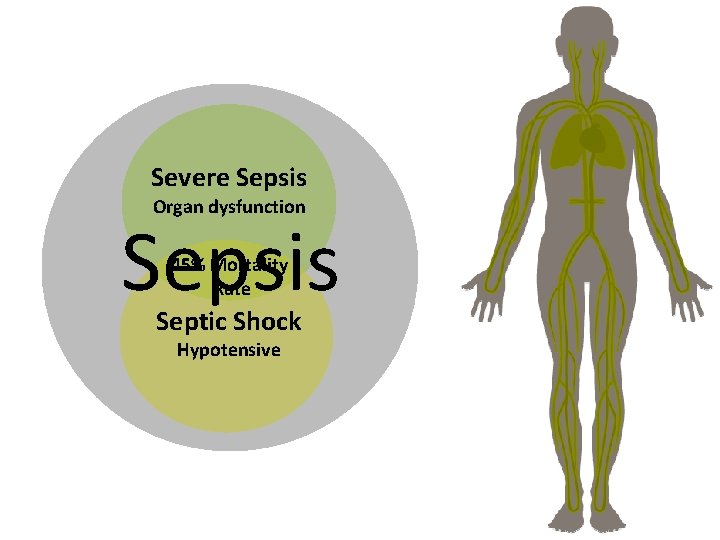
Severe Sepsis Organ dysfunction Sepsis 45% Mortality Rate Septic Shock Hypotensive
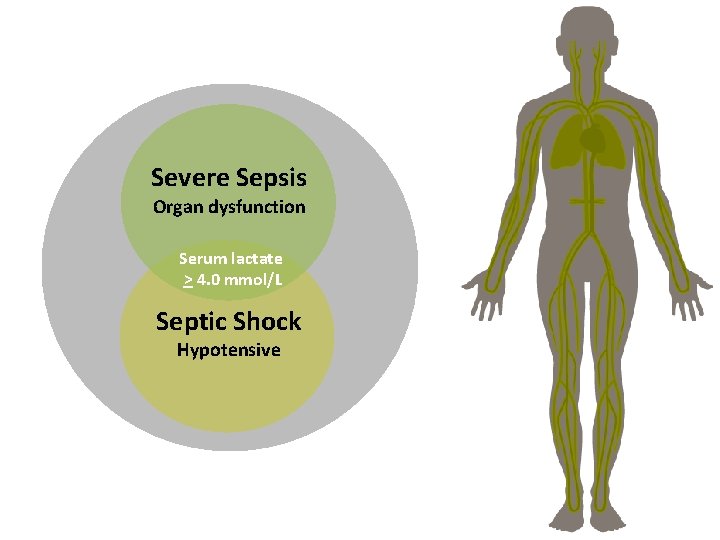
Severe Sepsis Organ dysfunction Serum lactate > 4. 0 mmol/L Septic Shock Hypotensive

Trial Documents
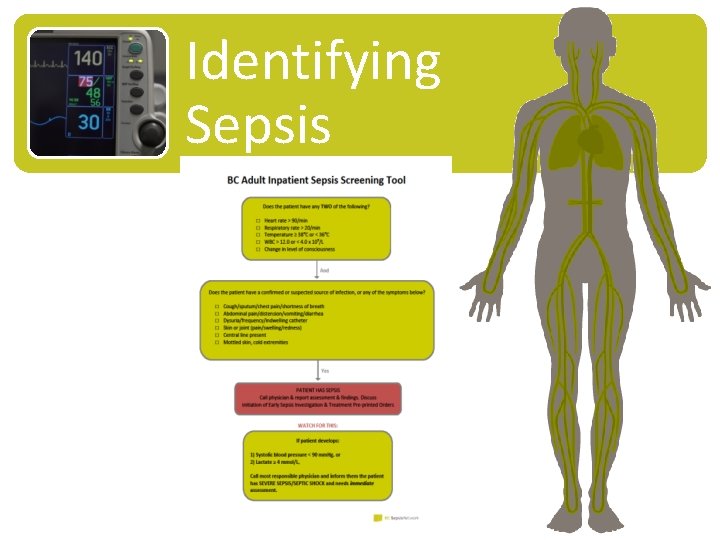
Identifying Sepsis

SIRS + Infection = Sepsis Does the patient have any TWO of the following? • Heart rate > 90/min • Respiratory rate > 20/min • Temperature ≥ 38 o. C or < 36 o. C • WBC > 12. 0 or < 4. 0 x 109/L • Change in level of consciousness

Sepsis + Risk Factors = Severe Sepsis or Septic Shock Does the patient have a confirmed or suspected source of infection, or any of the symptoms below? • Cough/sputum/chest pain/shortness of breath • Abdominal pain/distension/vomiting/diarrhea • Dysuria/frequency/indwelling catheter • Skin or joint (pain/swelling/redness) • Central line present • Mottled skin, cold extremities

Sepsis + Risk Factors = Severe Sepsis or Septic Shock If the patient has SEPSIS: CALL THE PHYSICIAN Report Findings & Discuss initiating the Early Sepsis Investigation And Treatment Pr-Printed Orders

Taking Action

INITIAL INTRAVENOUS AND HYDRATION • Ensure at least #20 Gauge IV access is in place □ Initiate IV bolus of: □ Normal Saline, □ Ringer’s Lactate or □ Plasmalyte _____m. L (max 2 L) and give over ____ minutes (physician to assess post-bolus)

LABORATORY AND DIAGNOSTIC INVESTIGATIONS: All investigations are STAT • Lactate (Venous Plasma). Notify physician immediately if lactate greater than 2 mmol/L • CBC and differential, INR, PTT, electrolytes, BUN, creatinine, glucose, liver function tests, lipase, troponin • Blood cultures X 2 sets BEFORE antibiotics (include culture from central line, if present) □ Urinalysis and urine C&S (as per VCH guidelines) □ Sputum for C&S □ 12 lead ECG □ Repeat lactate 2 hours after the first lactate is drawn. Notify physician of results □ Chest X-ray □ Other____________

Administer Antibiotics Administer antibiotic as order by Physician

MONITORING □ NPO • Vital Signs and Oxygen saturation Q 1 H X 6 H • Glasgow Coma Score (GCS) Q 1 H X 6 H • Supplemental O 2 to maintain oxygen saturation greater than 92%. Page RT if requiring high flow oxygen • Monitor urine output if able

URGENT CONSIDERATIONS • If hypotension (SBP less than 90 mm. Hg) despite initial fluid bolus, or lactate greater than 4 mmol/L, notify physician that SEVERE SEPSIS/SEPTIC SHOCK is present and call Critical Care Outreach Team (CCOT) • Physician to consider ICU consultation • If drainable focus of infection identified, organize early source control/drainage • Physician to determine further management and disposition of patient

IN-PATIENT WARD EARLY SEPSIS INVESTIGATION AND TREATEMENT PAGE 2 NURSING GUIDELINES: • May insert a second IV access and Foley catheter depending on the hemodynamic status and clinical needs of the patient • Ensure IV fluid start and stop times and IV fluid bolus amounts are documented in the 24 Hour Fluid Flowsheet • Monitor vital signs with oxygen saturation and perform respiratory assessment and documentation prior to and after completion of each fluid bolus to determine ongoing changes. • Contact MD for deterioration in vitals signs or clinical status using SBAR. • Ensure thorough documentation and accurate nursing handover with shift changes
Source. Control

Prevention

Performance Measurement

Audit Forms

The Basic Steps of Sepsis Response 1. Know Early Warning Signs from Sepsis Screening Tool 2. Understand basic sepsis pathophysiology 3. Contact Hospitalist/Physician 4. Discuss with physician to initiate Early Sepsis Investigation And Treatment Tool 4. Ensure IV Access and Initiate IV as ordered 5. Blood Work a) Notify physician if Lactate > 2 mmo/L b) Blood Cultures before Antibiotic 6. Close Nursing Monitoring 7. Accurate documentation and Nursing handover

For more information… • Doris Bohl, Clinical Educator • Janet Boates, Brenda Briggs, Roselin Jhinku, PCCs • Melinda David, PSM • Leighanne Mac. Kenzie, Operations Director Medicine • Dr. David Sweet, Clinical Lead – Sepsis BCPSQC

QUESTIONS? ?
- Slides: 29