ICU Standard Operating Procedures slide 2 ICU Structural




















- Slides: 31


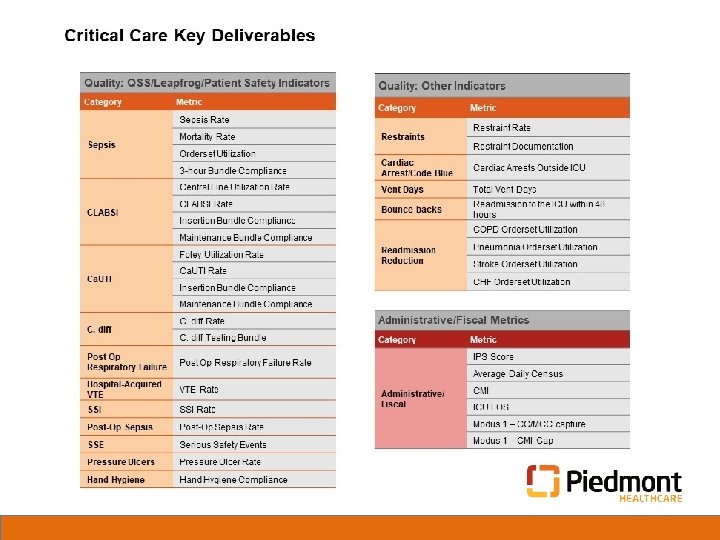
ICU Standard Operating Procedures slide 2 • ICU Structural Overview Bed Footprint, Stats & Staffing Model Level 2 ICU Management Structure • ICU Processes of Care Admission & Discharge Process Daily Rounding Standard Work Key ICU Deliverables Emergent Care Support Specialist Support Availability Common Procedural Questions • ICU Policies, Procedures & Ordersets Current State Future State • Key Stakeholder Walk Through

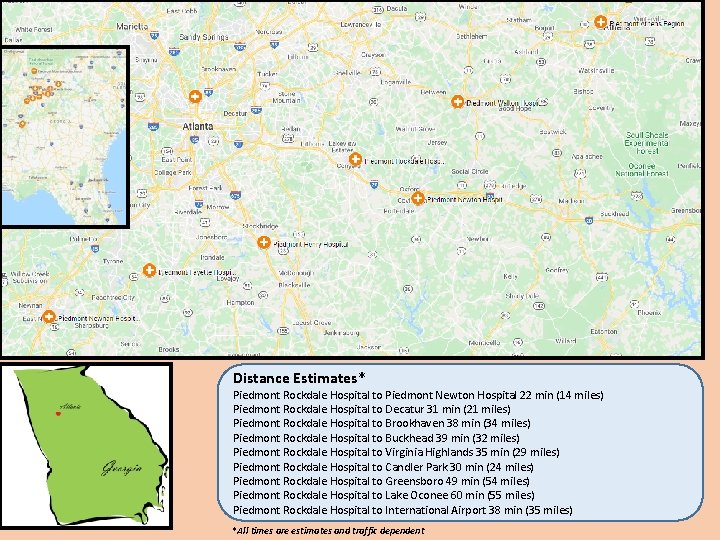
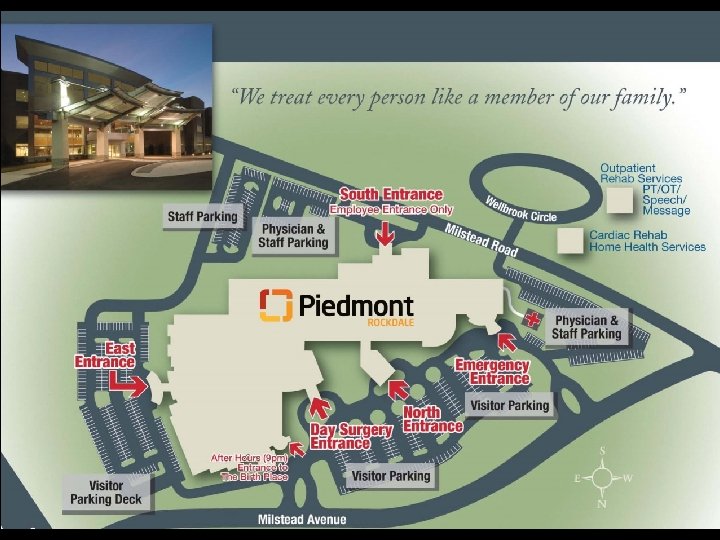
Piedmont Rockdale Hospital Campus slide 3

Distance Estimates* Piedmont Rockdale Hospital to Piedmont Newton Hospital 22 min (14 miles) Piedmont Rockdale Hospital to Decatur 31 min (21 miles) Piedmont Rockdale Hospital to Brookhaven 38 min (34 miles) Piedmont Rockdale Hospital to Buckhead 39 min (32 miles) Piedmont Rockdale Hospital to Virginia Highlands 35 min (29 miles) Piedmont Rockdale Hospital to Candler Park 30 min (24 miles) Piedmont Rockdale Hospital to Greensboro 49 min (54 miles) Piedmont Rockdale Hospital to Lake Oconee 60 min (55 miles) Piedmont Rockdale Hospital to International Airport 38 min (35 miles) *All times are estimates and traffic dependent


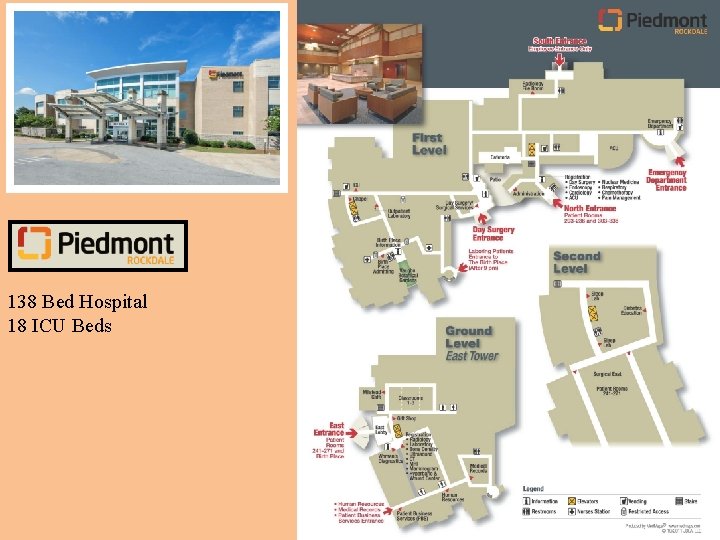
138 Bed Hospital 18 ICU Beds


ICU Structural Overview Bed Footprint, Stats and Staffing Model - 138 hospital bed campus - 18 bed medical surgical ICU - One intensivist team on campus (handling all critical care issues for the hospital) - No intermediate care unit at this time (discussions underway to build one out) - Staffing model: - Day Shift (6 am to 6 pm): 1 intensivist; 1 ICU APP - Night Shift (6 pm to 6 am): hospitalist program provides coverage; intensivist available by phone (with ability to respond in person if deemed necessary) - Open ICU: Intensivists not managing all patients within the ICU. Administration feels all patients that are critically ill are being managed by intensivist team when present. Planning move to closed ICU model. slide 8

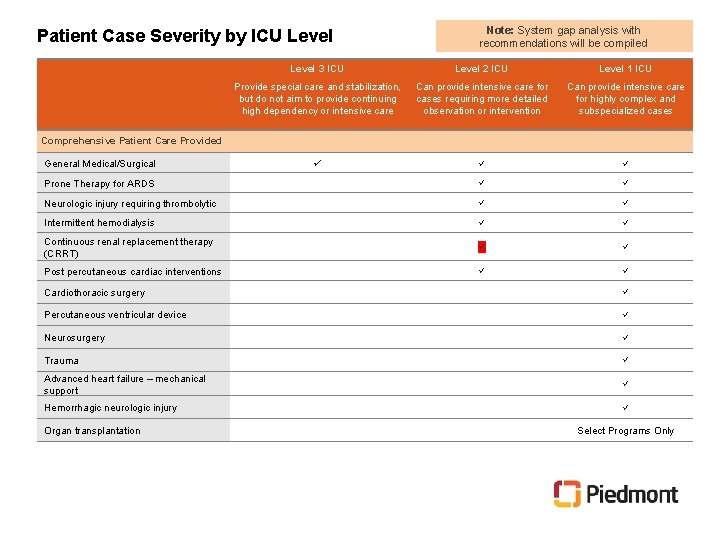
Patient Case Severity by ICU Level Note: System gap analysis with recommendations will be compiled Level 3 ICU Level 2 ICU Level 1 ICU Provide special care and stabilization, but do not aim to provide continuing high dependency or intensive care Can provide intensive care for cases requiring more detailed observation or intervention Can provide intensive care for highly complex and subspecialized cases Prone Therapy for ARDS Neurologic injury requiring thrombolytic Intermittent hemodialysis Continuous renal replacement therapy (CRRT) Post percutaneous cardiac interventions Comprehensive Patient Care Provided General Medical/Surgical Cardiothoracic surgery Percutaneous ventricular device Neurosurgery Trauma Advanced heart failure – mechanical support Hemorrhagic neurologic injury Organ transplantation Select Programs Only

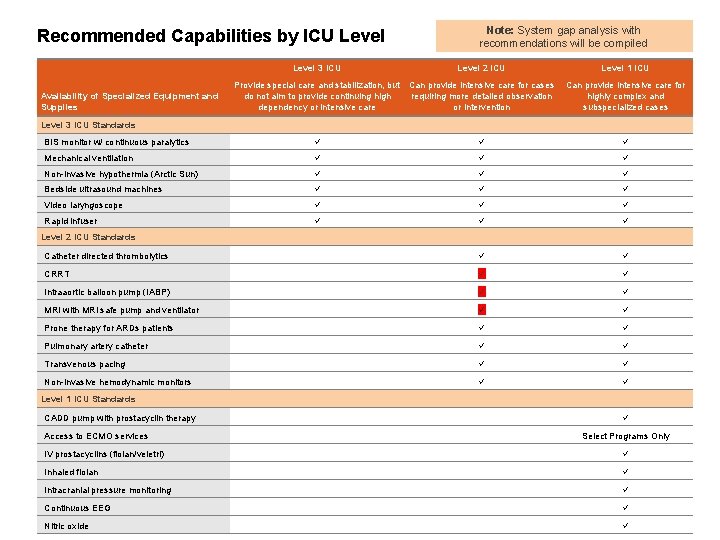
Recommended Capabilities by ICU Level 3 ICU Availability of Specialized Equipment and Supplies Note: System gap analysis with recommendations will be compiled Level 2 ICU Provide special care and stabilization, but Can provide intensive care for cases do not aim to provide continuing high requiring more detailed observation dependency or intensive care or intervention Level 1 ICU Can provide intensive care for highly complex and subspecialized cases Level 3 ICU Standards BIS monitor w/ continuous paralytics Mechanical ventilation Non-invasive hypothermia (Arctic Sun) Bedside ultrasound machines Video laryngoscope Rapid infuser Catheter directed thrombolytics CRRT Intraaortic balloon pump (IABP) MRI with MRI safe pump and ventilator Prone therapy for ARDs patients Pulmonary artery catheter Transvenous pacing Non-invasive hemodynamic monitors Level 2 ICU Standards Level 1 ICU Standards CADD pump with prostacyclin therapy Access to ECMO services Select Programs Only IV prostacyclins (flolan/veletri) Inhaled flolan Intracranial pressure monitoring Continuous EEG Nitric oxide

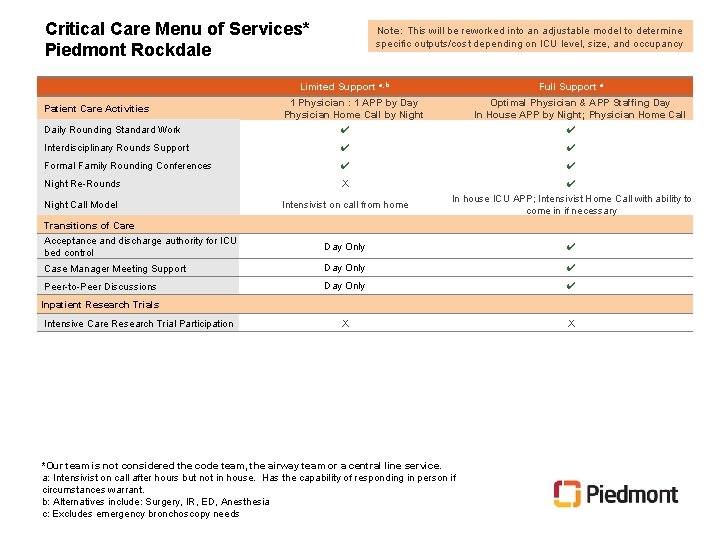
Critical Care Menu of Services* Piedmont Rockdale Note: This will be reworked into an adjustable model to determine specific outputs/cost depending on ICU level, size, and occupancy Limited Support a, b Patient Care Activities Daily Rounding Standard Work Full Support a 1 Physician : 1 APP by Day Physician Home Call by Night ✔ Optimal Physician & APP Staffing Day In House APP by Night; Physician Home Call ✔ Interdisciplinary Rounds Support ✔ ✔ Formal Family Rounding Conferences ✔ ✔ Night Re-Rounds X Night Call Model Intensivist on call from home ✔ In house ICU APP; Intensivist Home Call with ability to come in if necessary Transitions of Care Acceptance and discharge authority for ICU bed control Day Only ✔ Case Manager Meeting Support Day Only ✔ Peer-to-Peer Discussions Day Only ✔ X X Inpatient Research Trials Intensive Care Research Trial Participation *Our team is not considered the code team, the airway team or a central line service. a: Intensivist on call after hours but not in house. Has the capability of responding in person if circumstances warrant. b: Alternatives include: Surgery, IR, ED, Anesthesia c: Excludes emergency bronchoscopy needs

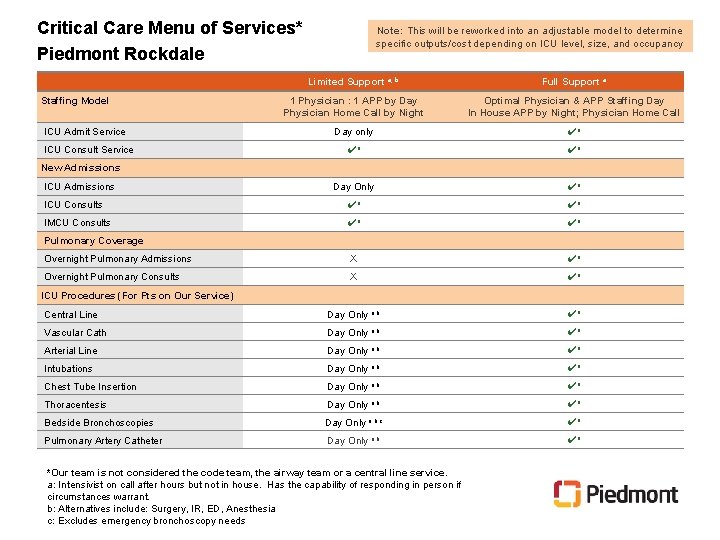
Critical Care Menu of Services* Piedmont Rockdale Note: This will be reworked into an adjustable model to determine specific outputs/cost depending on ICU level, size, and occupancy Limited Support a, b Full Support a 1 Physician : 1 APP by Day Physician Home Call by Night Optimal Physician & APP Staffing Day In House APP by Night; Physician Home Call Day only ✔a ✔a ✔a Day Only ✔a ICU Consults ✔a ✔a IMCU Consults ✔a ✔a Overnight Pulmonary Admissions X ✔a Overnight Pulmonary Consults X ✔a Central Line Day Only a, b ✔a Vascular Cath Day Only a, b ✔a Arterial Line Day Only a, b ✔a Intubations Day Only a, b ✔a Chest Tube Insertion Day Only a, b ✔a Thoracentesis Day Only a, b ✔a Bedside Bronchoscopies Day Only a, b, c ✔a Pulmonary Artery Catheter Day Only a, b ✔a Staffing Model ICU Admit Service ICU Consult Service New Admissions ICU Admissions Pulmonary Coverage ICU Procedures (For Pts on Our Service) *Our team is not considered the code team, the airway team or a central line service. a: Intensivist on call after hours but not in house. Has the capability of responding in person if circumstances warrant. b: Alternatives include: Surgery, IR, ED, Anesthesia c: Excludes emergency bronchoscopy needs

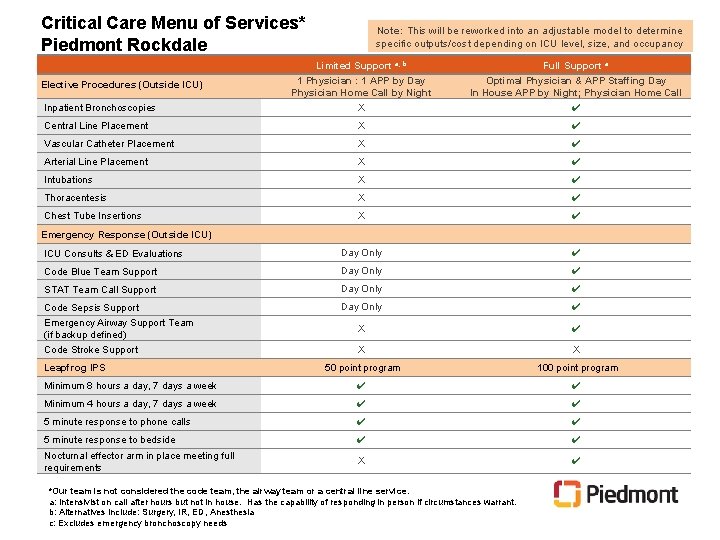
Critical Care Menu of Services* Piedmont Rockdale Note: This will be reworked into an adjustable model to determine specific outputs/cost depending on ICU level, size, and occupancy Limited Support a, b Full Support a 1 Physician : 1 APP by Day Physician Home Call by Night X Optimal Physician & APP Staffing Day In House APP by Night; Physician Home Call ✔ Central Line Placement X ✔ Vascular Catheter Placement X ✔ Arterial Line Placement X ✔ Intubations X ✔ Thoracentesis X ✔ Chest Tube Insertions X ✔ ICU Consults & ED Evaluations Day Only ✔ Code Blue Team Support Day Only ✔ STAT Team Call Support Day Only ✔ Code Sepsis Support Day Only ✔ Emergency Airway Support Team (if backup defined) X ✔ Code Stroke Support X X 50 point program 100 point program Minimum 8 hours a day, 7 days a week ✔ ✔ Minimum 4 hours a day, 7 days a week ✔ ✔ 5 minute response to phone calls ✔ ✔ 5 minute response to bedside ✔ ✔ Nocturnal effector arm in place meeting full requirements X ✔ Elective Procedures (Outside ICU) Inpatient Bronchoscopies Emergency Response (Outside ICU) Leapfrog IPS *Our team is not considered the code team, the airway team or a central line service. a: Intensivist on call after hours but not in house. Has the capability of responding in person if circumstances warrant. b: Alternatives include: Surgery, IR, ED, Anesthesia c: Excludes emergency bronchoscopy needs

ICU Admission and Discharge Process Admission to ICU - Admissions generally occur from the ER, acute care floor, PACU, OR or other procedural areas (ICU admission acceptance can be intensivist or intensivist designee – APP or hospitalist) - Admissions from outside facilities require physician to physician communication (APPs should not accept outside facility transfers or call for transferring out of the facility) - Ideally, no ICU bed should be released without acceptance by the ICU physician team (or designee) and handoff. - Acceptance of a patient to the ICU by telephone (ie the intensivist or designee is not required to evaluate the patient in person if they feel the presentation clearly outlines the need for ICU care therefore not delaying ICU bed assignment). - Bed requests go through the nursing house supervisor (if we accept a patient to the ICU please ensure that is communicated to the house supervisor) slide 14 Detailing of program currently underway. Some items may be inaccurate.

ICU Admission and Discharge Process Admission to ICU - We believe in Right Care, Right Now Care models. As such, upon point of contact handoff our intensivist team engages the care of the patient. When possible, we attempt to be at bedside as quickly as is feasible to assess the patients stability and urgent/emergent care needs. We go to the ER, the acute care floors, the PACU, etc. We do not wait for the patient to come to the ICU prior to seeing. - Our intensivists and ICU APPs communicate frequently to triage the most pressing needs/tasks for our patients. slide 15 Detailing of program currently underway. Some items may be inaccurate.

ICU Admission and Discharge Process Transfer out of ICU Process - Discharge from the ICU is at the discretion of the intensivist team. Having said that, high performing intensivist teams seek to have the trust and confidence of their colleagues. - Target time for discharge out of ICU orders to be done is by 10 am. - Handoff to the receiving team should be completed prior to transfer orders being placed. Document in the daily ICU note the name of the physician (or designee) to whom handoff was provided. - Attending status is not changed on the patient until the patient leaves the ICU. If the patient remains in the ICU due to no acute care floor beds available we will remain engaged and driving the care of the ICU patient. slide 16 Detailing of program currently underway. Some items may be inaccurate.

ICU Processes of Care Daily Rounding Standard Work - Our ICU team works to maintain a daily EPIC sticky note census that is concise and enables efficient, effective handoffs shift to shift. - Upon arrival to the hospital our Intensivists/ICU APPs huddle up to run the patient list, divide up patient care responsibilities. Another huddle up post IDRs and at around 4 pm should occur to ensure task loop closures are occurring/progressing. - Our Intensivist/ICU APP should check in regularly with the ICU charge nurse and ICU respiratory therapist during their shift to ensure high quality communication occurs. - We should communicate daily with the bedside nurse caring for our patients. - Interdisciplinary rounds should be supported Monday-Friday (and Saturday/Sunday when feasible). These should be able to be completed in under 60 min for an 18 bed ICU. slide 17 Detailing of program currently underway. Some items may be inaccurate.

slide 18

Interdisciplinary Rounds 19 • ICU medical directors (or designee) required to lead/oversee interdisciplinary rounds • Rounds to be completed on all patients in unit on a daily basis • Rounds include all members of the critical care team, as appropriate

ICU Processes of Care Daily Rounding Standard Work - We should communicate daily with the patients and their next of kin. - For complex patient care scenarios formal family conferences are encouraged linking several members of the critical care team (subspecialty support as indicated) and the patients medical decision making support members (at discretion of patient or NOK). - Intensivists and ICU APPs should communicate professionally, directly and clearly with regards to balancing the work to be completed for the day. Attention must be paid to power gradients, level of experience and competing time demands. slide 20 Detailing of program currently underway. Some items may be inaccurate.

ICU Processes of Care Emergent Care Support (inside and outside of ICU) - CODE BLUE Response Team: Hospitalist team responds. If our intensivist team is present and available we will respond to CODE BLUE alerts. - STAT Team Overhead Alerts: Stat team nurse responds (out of staffing STAT team nurse). If contacted by STAT team nurse we will respond as indicated. - CODE SEPSIS: Hospitalist team responds. Future state, intensivist team to respond when present to CODE SEPSIS Red Alerts. - CODE Stroke: Hospitalist team responds. Hospitalist will contact intensivist team if patient is in ICU or needs ICU level of care for handoff discussions. - CODE STEMI: Cardiology team responds. Cardiologist will contact intensivist team if patient is in ICU or needs ICU level of care for handoff discussions. slide 21 Detailing of program currently underway. Some items may be inaccurate.

ICU Processes of Care Specialist Support Teams - Emergency Department - Hospitalist Program - General Surgery Program - General and Interventional Cardiology Program - Interventional Radiology with Support for GI bleeds - Nephrology (not doing CRRT at this time; plans to initiate program) - Neurology Program - No Palliative Care Presence - No Thoracic Surgery* Presence - No Cardiothoracic Surgery* Presence - No Neurosurgery* Presence *Typically not present in - No Endocrinology* Presence Level 2 ICU programs - No ENT* Presence Detailing of program currently underway. Some items may be inaccurate. slide 22

ICU Processes of Care Common Procedural Questions - Who does tracheostomies? General surgery in the OR. There are discussions underway for surgery to do perc trachs at bedside when feasible. - Is there a PICC team? No. PICC lines placed by IR. - Is there an IV team? No. - Who does central lines for Non-ICU patients (or ICU patients when intensivist team not present)? IR when available. Otherwise, ED or general surgery. - Who supports intubations? By day, intensivist team (with Anesthesia backup when felt to be needed). Afterhours, RT with Hospitalist assist (ED vs Anesthesia for backup when felt to be needed). - Who supports chest tubes? By day, intensivist team (with surgery backup if needed). By night, ED. slide 23 Detailing of program currently underway. Some items may be inaccurate.

ICU Processes of Care Common Procedural Questions - Is there a central line cart? Under development - Is there an ultrasound machine available? Yes, housed in the ICU. - Is there a difficult airway bag available? Under development - Is there a video laryngoscope avialable? Yes, glidescope housed in the ICU. - Is there capability for bedside bronchoscopy? Yes slide 24 Detailing of program currently underway. Some items may be inaccurate.

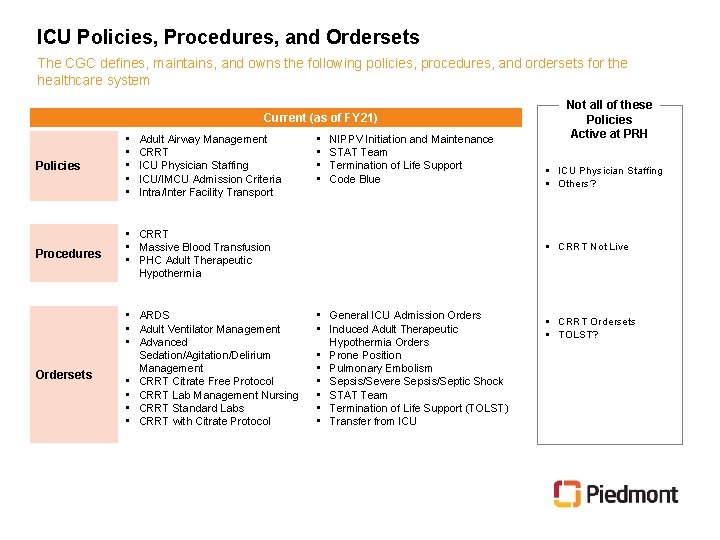
ICU Policies, Procedures, and Ordersets The CGC defines, maintains, and owns the following policies, procedures, and ordersets for the healthcare system Current (as of FY 21) Policies • • • Procedures • CRRT • Massive Blood Transfusion • PHC Adult Therapeutic Hypothermia Ordersets Adult Airway Management CRRT ICU Physician Staffing ICU/IMCU Admission Criteria Intra/Inter Facility Transport • ARDS • Adult Ventilator Management • Advanced Sedation/Agitation/Delirium Management • CRRT Citrate Free Protocol • CRRT Lab Management Nursing • CRRT Standard Labs • CRRT with Citrate Protocol • • NIPPV Initiation and Maintenance STAT Team Termination of Life Support Code Blue Not all of these Policies Active at PRH § ICU Physician Staffing § Others? § CRRT Not Live • General ICU Admission Orders • Induced Adult Therapeutic Hypothermia Orders • Prone Position • Pulmonary Embolism • Sepsis/Severe Sepsis/Septic Shock • STAT Team • Termination of Life Support (TOLST) • Transfer from ICU § CRRT Ordersets § TOLST?

ICU Processes of Care: How to Orderset www. pulmcast. com/locums slide 26

Who is the team? Who is the customer? Key Stakeholders: Our Patients Family Members Our Division Leadership Our Physicians Our APPs Our ICU Team Physicians APPs ICU Nurses Stat Team Nurses ICU Respiratory Therapists Pharmacists Nutritionists Rehab Service Members Care Managers slide 27 Service Excellence Key Stakeholders: Hospital C-Suite Med Exec Leaders ER Physicians Hospitalist Physicians Always Available One Call That’s All Thank you may I have another How can I help What matters most? Key Stakeholders: Nephrology Physicians Cardiology Physicians Infectious Disease Physicians General Surgery Physicians Anesthesiology Physicians Depends on the team… Depends on the team member…

Executive Team Meghan Kirkland, PA APP Director Chief of Pulmonary, Critical Care, Sleep Coy Lassiter, MD Senior Director of Clinical Care Martha Carr, MBA, MHA, CCRN, MSN Chief of Quality Piedmont Clinical Governance Council Chair Jermaine Jackson, MD Chief of Critical Care Services Director of Physician Recruitment Medical Director Professional Development Chad Case, MD

Piedmont Rockdale Hospital Executive Team Richard Tanzella Piedmont Rockdale Chief Executive Officer Leigha Fallis, RN Piedmont Rockdale Chief Nursing Officer slide 29 Geoffrey Cole, M. D. Piedmont Rockdale Chief Medical Officer Marty Wynn Piedmont Rockdale Chief Financial Officer

Piedmont Rockdale Hospital Key Team Members Cynthia Palmer Piedmont Rockdale ICU Nurse Manager Seth Duncan Piedmont Rockdale ED Admin Director slide 30 Rick Rodriquez Piedmont Rockdale Respiratory Therapy Director
