ICU Management of DKA HHS Alexandra Bandy AGACNP

ICU Management of DKA & HHS Alexandra Bandy AG-ACNP RN Cindy Gamboa FNP RN October 2018

Initial Evaluation O O O O O Blood glucose Venous bicarbonate (p. CO 2) Urine ketones or B-HBT Sodium (correct for hyperglycemia) Potassium (note if < or > 5) Creatinine (evaluate for AKI) Anion gap Serum osmolality Do not put too much weight on: lactate, WBCs but do complete an infectious workup as indicated

Overview O Definitions O Pearls / Things to Remember O Goals of Therapy O Management Techniques O LLEAP Orders O Healthcare Team Roles O Resources

Definitions Spectrum of hyperglycemia in the diabetic patient HONK/ HHS: Neurologic abnormalities common Glucose often exceeds 1000 DKA: Defined by metabolic acidosis Glucose usually below 800 (often 350500) **overlap occurs in > 1/3 of patients** Hyperosmolar Non-Ketotic State: serum osm >350 (2[Na + K] + glucose) venous bicarb >15 mmol/l mild or no ketonuria TYPE 2 TYPE 1 Diabetic Ketoacidosis: venous bicarb <15 mmol/L at least moderate ketonuria (or B-HBT >3) TYPE 1. 5

Pearls: O DKA and HHS are both defined by severe dehydration; adequately fluid replete! O DKA is a syndrome defined by acidemia, not hyperglycemia. Correct the p. H, then worry about the glucose. Give IVFs, stabilize K+, manage electrolyte losses via antiemeitics, then insulin. O Always consider what triggered the DKA… discharge will hinge upon fixing that issue (and often these are psycho-social so may take a few days to fix)
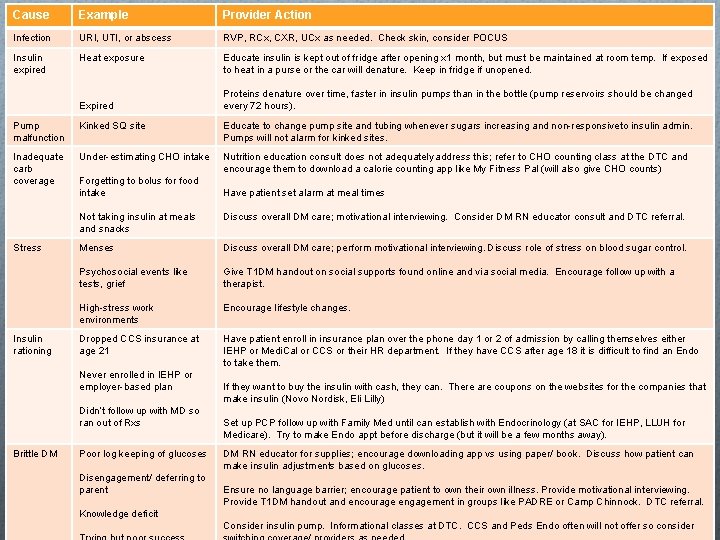
Cause Example Provider Action Infection URI, UTI, or abscess RVP, RCx, CXR, UCx as needed. Check skin, consider POCUS Insulin expired Heat exposure Educate insulin is kept out of fridge after opening x 1 month, but must be maintained at room temp. If exposed to heat in a purse or the car will denature. Keep in fridge if unopened. Expired Proteins denature over time, faster in insulin pumps than in the bottle (pump reservoirs should be changed every 72 hours). Pump malfunction Kinked SQ site Educate to change pump site and tubing whenever sugars increasing and non-responsive to insulin admin. Pumps will not alarm for kinked sites. Inadequate carb coverage Under-estimating CHO intake Nutrition education consult does not adequately address this; refer to CHO counting class at the DTC and encourage them to download a calorie counting app like My Fitness Pal (will also give CHO counts) Stress Insulin rationing Forgetting to bolus for food intake Not taking insulin at meals and snacks Discuss overall DM care; motivational interviewing. Consider DM RN educator consult and DTC referral. Menses Discuss overall DM care; perform motivational interviewing. Discuss role of stress on blood sugar control. Psychosocial events like tests, grief Give T 1 DM handout on social supports found online and via social media. Encourage follow up with a therapist. High-stress work environments Encourage lifestyle changes. Dropped CCS insurance at age 21 Have patient enroll in insurance plan over the phone day 1 or 2 of admission by calling themselves either IEHP or Medi. Cal or CCS or their HR department. If they have CCS after age 18 it is difficult to find an Endo to take them. Never enrolled in IEHP or employer-based plan Didn’t follow up with MD so ran out of Rxs Brittle DM Have patient set alarm at meal times Poor log keeping of glucoses Disengagement/ deferring to parent If they want to buy the insulin with cash, they can. There are coupons on the websites for the companies that make insulin (Novo Nordisk, Eli Lilly) Set up PCP follow up with Family Med until can establish with Endocrinology (at SAC for IEHP, LLUH for Medicare). Try to make Endo appt before discharge (but it will be a few months away). DM RN educator for supplies; encourage downloading app vs using paper/ book. Discuss how patient can make insulin adjustments based on glucoses. Ensure no language barrier; encourage patient to own their own illness. Provide motivational interviewing. Provide T 1 DM handout and encourage engagement in groups like PADRE or Camp Chinnock. DTC referral. Knowledge deficit Consider insulin pump. Informational classes at DTC. CCS and Peds Endo often will not offer so consider

Psychosocial Support Handout

Things to Remember O O O O O Intravenous fluid replacement is FIRST LINE THERAPY for both DKA & HHS. Given patients may show signs of both, do not underestimate their fluid repletion needs. Adequate IVFs before insulin! Serum potassium monitoring is important! Patients present with normal or high K because of hyperosmolar state (dehydration), and as insulin is provided, their true state of potassium depletion is exacerbated by potassium being pulled into the cell through insulin-mediated K channels. For this reason, if K is low to normal (~4) on arrival, it must be replaced before insulin. The order set prompts this. Hourly glucose monitoring is required for appropriate insulin drip titration. Insulin gtt should not be titrated hourly. Low-dose insulin with drop of glucose 35 -70 mg/d. L per hour is appropriate. If these values aren’t achieved, then the RN or provider can increase or decrease from standard 0. 1 units/kg/hr. Consider type of DM when transitioning from insulin drip to SQ. In Type I, long-acting insulin (Lantus, NPH) must be given 1 -2 hours before stopping insulin drip. In Type 2, stopping of drip and initiating SQ can happen concurrently or consecutively. PO challenge has to be done before considering if the patient is ready for their long acting insulin Consider urinary catheter if incontinence (diabetic coma) or not voiding (given concerns for K build-up). Consider A-line placement for Q 4 H BMPs and trending acidosis (however, this can also be achieved from venous blood draws). Endocrinologists should see patients with A 1 Cs > 10, please refer upon discharge
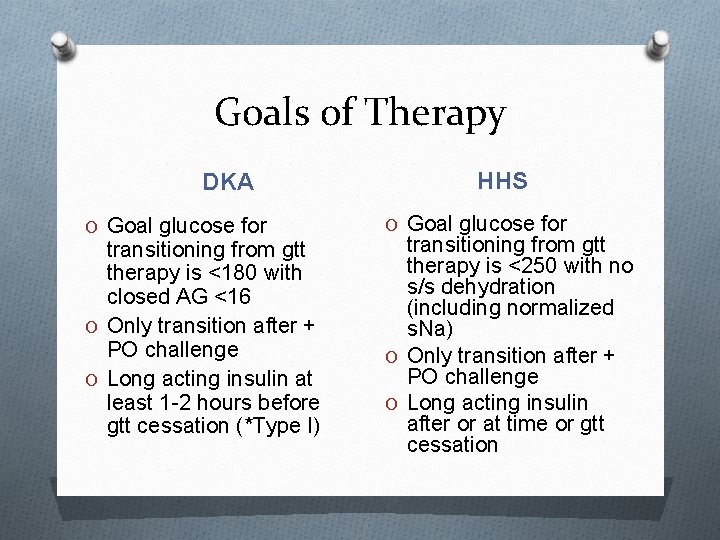
Goals of Therapy DKA O Goal glucose for transitioning from gtt therapy is <180 with closed AG <16 O Only transition after + PO challenge O Long acting insulin at least 1 -2 hours before gtt cessation (*Type I) HHS O Goal glucose for transitioning from gtt therapy is <250 with no s/s dehydration (including normalized s. Na) O Only transition after + PO challenge O Long acting insulin after or at time or gtt cessation

Management Techniques Order Sets Available O ADULT Diabetic Ketoacidosis (DKA) and HHS O PICU / Peds Diabetic Ketoacidosis IV Insulin Orders Do Not Use: Insulin Infusion (Insulin Drip) Orders

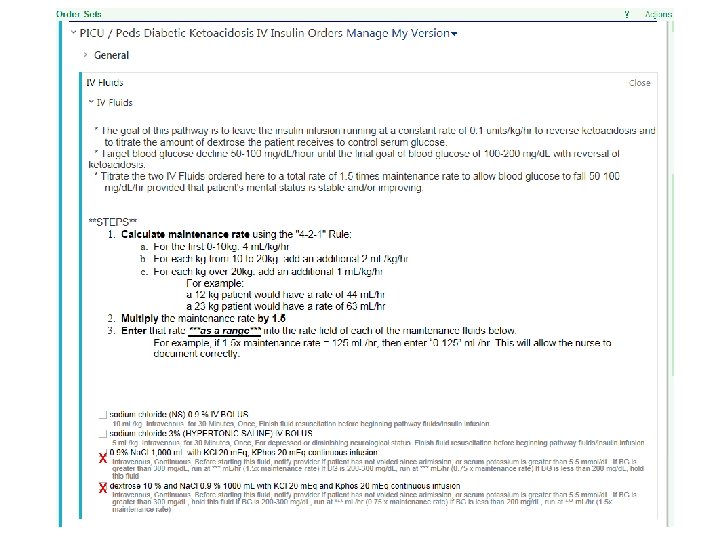
DO NOT USE INSULIN DRIP ORDER SET! If you see orders to manipulate the insulin gtt based on dextrose administration, this is incorrect! Please delete these administration orders. We only ever titrate based on glucose They are from the “Insulin Infusion (Insulin Drip)” order set, not the appropriate DKA/HHS order sets.

PICU / Peds Diabetic Ketoacidosis IV Insulin Orders O AKA original “ 2 -bag system”: RN will titrate 2 solutions (either D 10 or NS) that contain electrolyte replacements (20 m. Eq KCl and 20 m. Eq Kphos) at various weight-based rates depending on glucose level O Cannot adjust electrolytes O Not ideal for ESRD given fixed electrolytes. Can be tricky in CHF as fluid volume can be large given cc/kg dosing. O RN reviews POCT glucose to adjust rates
x x
x

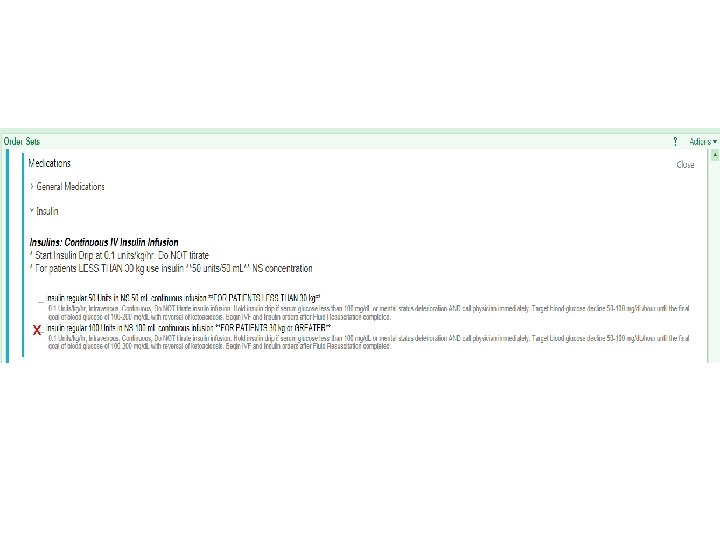
ADULT DKA and HHS O Also uses 2 IVF bags concurrently O MD can choose from 4 different 2 -bag systems for DKA O O depending on underlying metabolic disarray MD can also choose from 4 different 2 -bag systems for HHS For the most part, this is the superior set for our population at ECICU because it uses 1/2 NS or LR not NS, it includes a more specific K replacement, and it allows for a higher fluid repletion rate The nurses are used to the insulin titration now and will appropriately de-escalate the gtt rate if the patients' sugars go low overnight if this is written into the admin instructions. The float nurses from the floor however sometimes miss these instructions and just keep giving D 50. If the patient’s insulin rate has been downtitrated due to falling glucoses and a few hours later their glucoses are high, the MD needs to take over the order set and adjust the rate themselves
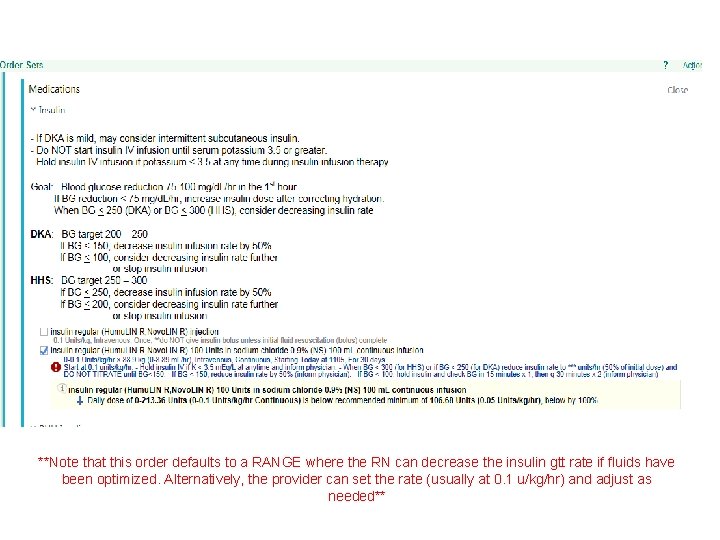
**Note that this order defaults to a RANGE where the RN can decrease the insulin gtt rate if fluids have been optimized. Alternatively, the provider can set the rate (usually at 0. 1 u/kg/hr) and adjust as needed**
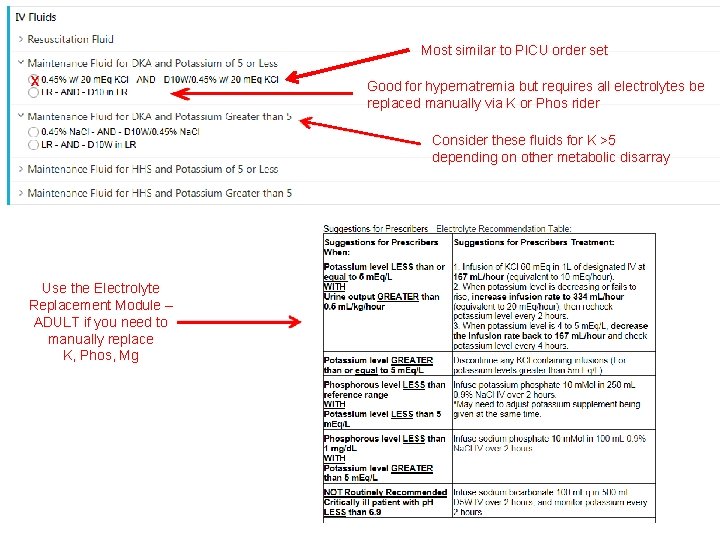

Most similar to PICU order set x Good for hypernatremia but requires all electrolytes be replaced manually via K or Phos rider Consider these fluids for K >5 depending on other metabolic disarray Use the Electrolyte Replacement Module – ADULT if you need to manually replace K, Phos, Mg

RN-MD Roles Nurses O Release recurring labs (ABGs, BMPs) and draw or call lab to facilitate O Notify MD when blood glucose <200 or with significant change O Communicate results of PO challenge to provider ASAP O Monitor fluid/ volume status Providers O Order & review serial electrolytes / AG/ p. H (Q 4 H recommended) O Make patient NPO except if hypoglycemic and juice given O Consider infectious precipitators; full workup O Re-evaluate patient at regular intervals

Transitioning to SQ Insulin Dosing Long Acting O O O O Find out home regimen and if patient was taking it, compare with A 1 C Use the Lantus weight based order to approximate what dose should be Based on above, decide on a dose and decrease it by a few units (no more than 50%) as most patients have poor PO intake in the hospital It’s easiest to transition the patient at the same time as they usually take their Lantus (either AM or PM) Consider using the standard insulin gtt for hyperglycemia and d/c the dextrose-containing IVFs if the gap is closed/ bicarb normal and patient is eating but it’s going to be a few hours till their normal Lantus dose The next day, review glucoses. The total daily dose of short acting should be equal in units to long acting (about 50/50) and the fasting glucose first thing in AM should be at goal. If ratio trends towards short acting and FBG is high, then increase Lantus. Feel free to consult Endo with questions. Adjusting Short Acting O O O Find out home regimen: the majority should have a sliding scale or correction factor (1 unit per x over 100) as well as a carbohydrate ratio (1 unit per x carbs). If they are taking in carb-containing POs (even if not off 2 -bag with insulin gtt) you should give them a carb ratio or a fixed mealtime bolus of short acting insulin to prevent worsening hyperglycemia If the patient isn’t eating a full tray of food religiously, order the correction factor be given before meals and the carb ratio or mealtime bolus be given within 15 minutes of completing meal as long as >25% meal eaten. If they are scarfing everything down, then they can have both shortacting shots combined. All type 1 s should have carb coverage of some sort. If they aren’t counting carbs, refer them to the DTC for education and come up with a way for them to improve their knowledge (calorie count apps are the best way). If they are unwilling, then a flat mealtime bolus is fine. Adjust sliding scale throughout the day as needed. Consider 0200 checks or post-prandials as needed to verify mealtime boluses appropriate.

Resources MC 8100 > NMCCS_ECHSH > ECICU Resident Reading List: ABCD Guidelines on DKA and HHS Up. To. Date DKA Management Online: http: //emedicine. medscape. com/article/118361 overview#showall (DKA) http: //emedicine. medscape. com/article/1914705 overview (HHS)
- Slides: 20