IAS 2017 IASconference LOW HIV INCIDENCE BUT HIGH

#IAS 2017 | @IAS_conference LOW HIV INCIDENCE BUT HIGH HCV INCIDENCE AMONG PEOPLE WHO INJECT DRUGS IN HAIPHONG, VIETNAM: RESULTS OF THE ANRS 12299/NIDA P 30 DA 011041 DRIVE-IN STUDY M. K. Pham, J. P. Moles, H. Duong Thi, T. Nguyen Thi, G. Hoang Thi, T. T. Nham Thi, V. Vu Hai, H. O. Khuat Thi, R. Vallo, M. Peries, K. Arasteh, C. Quillet, J. Feelemyer, L. Michel, T. Hammett, N. Nagot, D. Des Jarlais, D. Laureillard, for DRIVE study group

#IAS 2017 | @IAS_conference Conflict of Interest “No Conflicts Of Interest To Declare”

#IAS 2017 | @IAS_conference Background • In Vietnam, HIV control programs targeting persons who inject drugs (PWID), including harm reduction and scaled-up antiretroviral therapy (ART) have been implemented for about 10 years. • National HIV prevalence declined from 30% in 2009 (66% in Hai Phong) to 10% in 2013 among PWID, with high geographical disparities. • No information on current HIV incidence rate, nor on HCV incidence.

#IAS 2017 | @IAS_conference Objectives • To estimate HIV and HCV prevalence and incidence among active PWID in Hai Phong, Vietnam • To identify the determinants of HCV seroconversion among this group

#IAS 2017 | @IAS_conference Methods • Community-based respondent driven sampling (RDS) survey among 'active PWID' in Haiphong, with HIV and HCV testing, implemented in October 2014 • Active PWID = positive urine test for heroin + injection marks • Longitudinal follow-up: HIV-negative participants and HCV-negative participants not on methadone maintenance therapy (MMT) were eligible for 1 year follow-up. • HIV/HCV testing, behavioural questionnaire at 6 and 12 months • Routine harm reduction activities and support to access MMT/HIV care by community-based organizations (CBO).
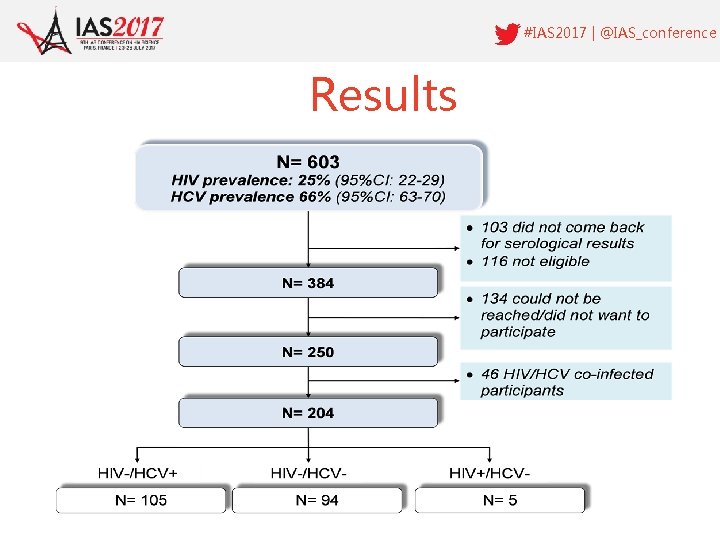
#IAS 2017 | @IAS_conference Results
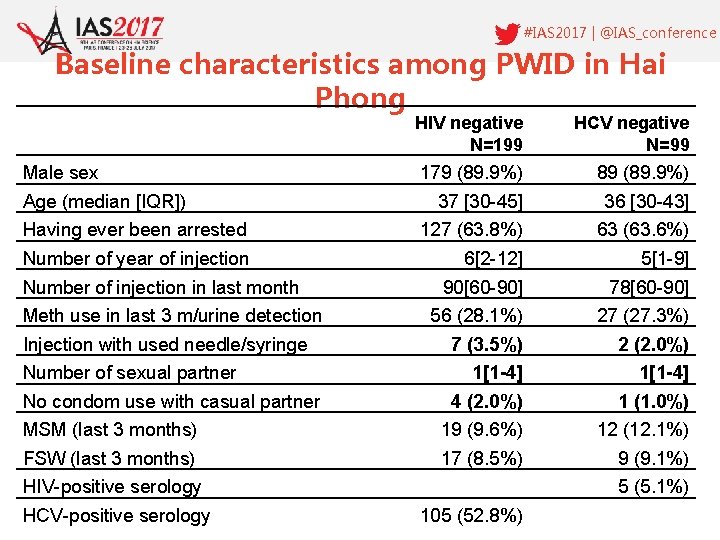
#IAS 2017 | @IAS_conference Baseline characteristics among PWID in Hai Phong HIV negative N=199 HCV negative N=99 179 (89. 9%) 89 (89. 9%) 37 [30 -45] 36 [30 -43] Having ever been arrested 127 (63. 8%) 63 (63. 6%) Number of year of injection 6[2 -12] 5[1 -9] 90[60 -90] 78[60 -90] 56 (28. 1%) 27 (27. 3%) 7 (3. 5%) 2 (2. 0%) 1[1 -4] 4 (2. 0%) 1 (1. 0%) MSM (last 3 months) 19 (9. 6%) 12 (12. 1%) FSW (last 3 months) 17 (8. 5%) 9 (9. 1%) Male sex Age (median [IQR]) Number of injection in last month Meth use in last 3 m/urine detection Injection with used needle/syringe Number of sexual partner No condom use with casual partner HIV-positive serology HCV-positive serology 5 (5. 1%) 105 (52. 8%)

#IAS 2017 | @IAS_conference Results • 45/204 (22%) participants did not reach 12 months f-up: 3 withdrew, 4 died, 22 were arrested and 16 moved out • No HIV seroconversion during the 206 pers-yrs of follow-up (HIV incidence 95%CI: 0 -1. 8/100 persyrs). • 18 participants seroconverted for HCV incidence of 19. 4/100 pers-yrs [95%CI; 11. 5 -30. 7]. • 13/18 HCV seroconversion happened during the first 8 months HCV incidence of : – 26. 7/100 pers-yrs (14. 2 -45. 6) w 0 - w 32 – 13. 2/100 pers-yrs (4. 3; 30. 8) w 32 - w 64
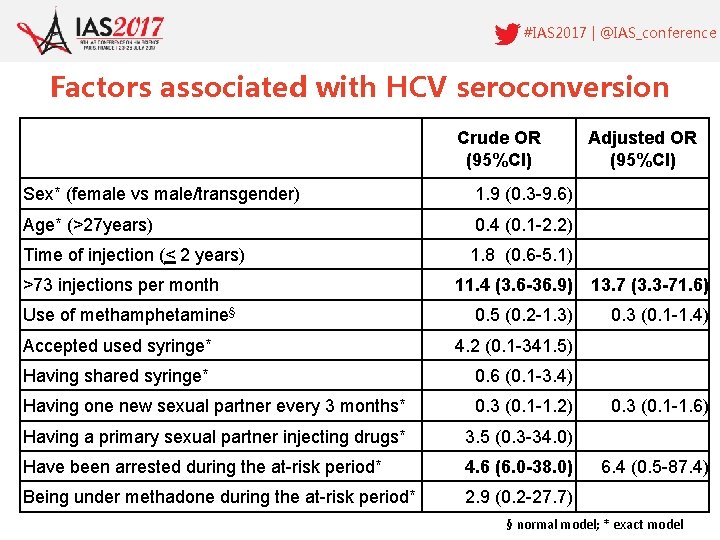

#IAS 2017 | @IAS_conference Factors associated with HCV seroconversion Crude OR (95%CI) Sex* (female vs male/transgender) 1. 9 (0. 3 -9. 6) Age* (>27 years) 0. 4 (0. 1 -2. 2) Time of injection (< 2 years) 1. 8 (0. 6 -5. 1) >73 injections per month Use of methamphetamine§ Adjusted OR (95%CI) 11. 4 (3. 6 -36. 9) 13. 7 (3. 3 -71. 6) 0. 5 (0. 2 -1. 3) 0. 3 (0. 1 -1. 4) Accepted used syringe* 4. 2 (0. 1 -341. 5) Having shared syringe* 0. 6 (0. 1 -3. 4) Having one new sexual partner every 3 months* 0. 3 (0. 1 -1. 2) Having a primary sexual partner injecting drugs* 3. 5 (0. 3 -34. 0) Have been arrested during the at-risk period* 4. 6 (6. 0 -38. 0) Being under methadone during the at-risk period* 2. 9 (0. 2 -27. 7) 0. 3 (0. 1 -1. 6) 6. 4 (0. 5 -87. 4) § normal model; * exact model

#IAS 2017 | @IAS_conference Conclusions • Low HIV incidence among active PWID in Haiphong • Larger data are required to confirm HIV is close to elimination among active PWID • In contrast, the HCV incidence is unacceptably high. More investigations is required to understand the routes of HCV transmission. • However, as in other settings, it is unlikely that harm reduction activities alone, even if adapted to HCV infection, will be able to control HCV in this group. • Therefore, large access to HCV treatment is now a priority given the efficacy and safety of the DAA • Further implementation studies are required to define an appropriate model of HCV testing and cure among PWID in Vietnam.

#IAS 2017 | @IAS_conference Acknowledgments • Funding agencies: Agence Nationale de Recherches sur le SIDA et les hépatites virales (ANRS) and the US National Institute of Drug Abuse (NIDA) • Haiphong Provincial Health authorities, Viet Tiep Hospital, Haiphong • Dr. Vu Van Cong, Pr. Truong Thi Xuan Lien, Pr. F. BarréSinoussi • The DRIVE scientific advisory board, and particularly Laurence Weiss and Jean-Pierre Daulouède • All the participants enrolled in the study
- Slides: 11