IAEA Training Material on Radiation Protection in Radiotherapy















































- Slides: 73

IAEA Training Material on Radiation Protection in Radiotherapy Part 6 Brachytherapy Lecture 2: Brachytherapy Techniques

Brachytherapy • • Very flexible radiotherapy delivery Source position determines treatment success Depends on operator skill and experience In principle the ultimate ‘conformal’ radiotherapy • Highly individualized for each patient • Typically an inpatient procedure as opposed to external beam radiotherapy which is usually administered in an outpatient setting Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 2

Objectives • To be familiar with different implant techniques • To be aware of differences between permanent implants, low (LDR) and high dose rate (HDR) applications • To appreciate the potential for optimization in high dose rate brachytherapy • To be familiar with some special techniques used in modern brachytherapy (seed implants, endovascular brachytherapy) Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 3

Contents 1. Clinical brachytherapy applications 2. Implant techniques and applicators 3. Delivery modes and equipment 4. Special techniques • A. Prostate seed implants • B. Endovascular brachytherapy • C. Ophthalmic applicators Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 4

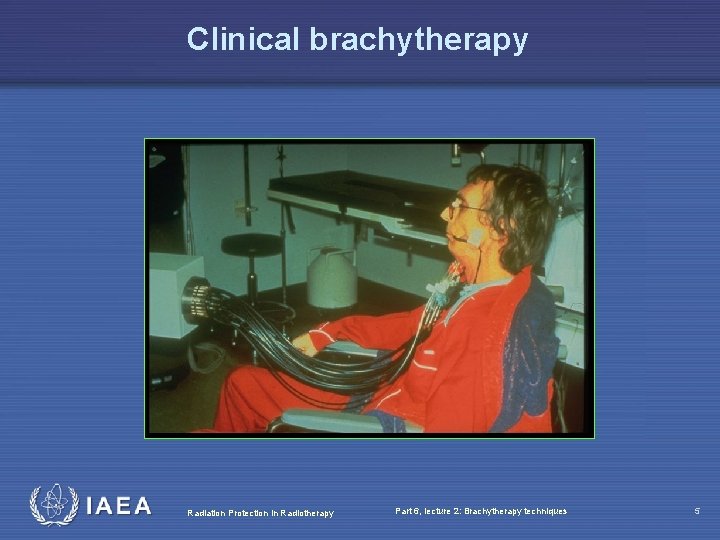
Clinical brachytherapy Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 5

History • Brachytherapy has been one of the earliest forms of radiotherapy • After discovery of radium by M Curie, radium was used for brachytherapy already late 19 th century • There is a wide range of applications - this versatility has been one of the most important features of brachytherapy Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 6

Today • Many different techniques and a large variety of equipment • Less than 10% of radiotherapy patients receive brachytherapy • Use depends very much on training and skill of clinicians and access to operating theatre Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 7

A brachytherapy patient • Typically localized cancer • Often relatively small tumour • Often good performance status (must tolerate the operation) • Sometimes pre-irradiated with external beam radiotherapy (EBT) • Often treated with combination brachytherapy and EBT Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 8

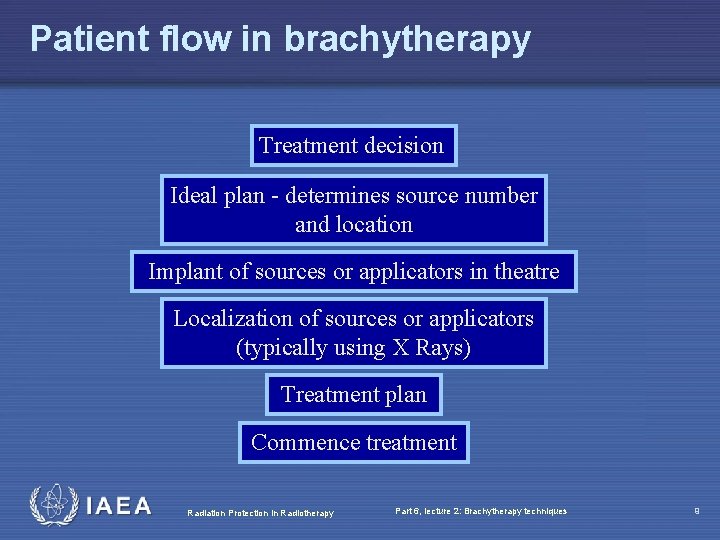
Patient flow in brachytherapy Treatment decision Ideal plan - determines source number and location Implant of sources or applicators in theatre Localization of sources or applicators (typically using X Rays) Treatment plan Commence treatment Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 9

1. Clinical brachytherapy applications A. Surface moulds B. Intracavitary (gynaecological, bronchus, . . ) C. Interstitial (Breast, Tongue, Sarcomas, …) not covered here: unsealed source radiotherapy (Thyroid, Bone metastasis, …) - this is dealt with in the IAEA training material on radiation protection in Nuclear Medicine Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 10

A. Surface moulds • Treatment of superficial lesions with radioactive sources in close contact with the skin Hand A mould for the back of a hand including shielding designed to protect the patient during treatment Radiation Protection in Radiotherapy Catheters for source transfer Part 6, lecture 2: Brachytherapy techniques 11

Historical example Surface applicator with irregular distribution of radium on the applicator surface (Murdoch, Brussels 1933) Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 12

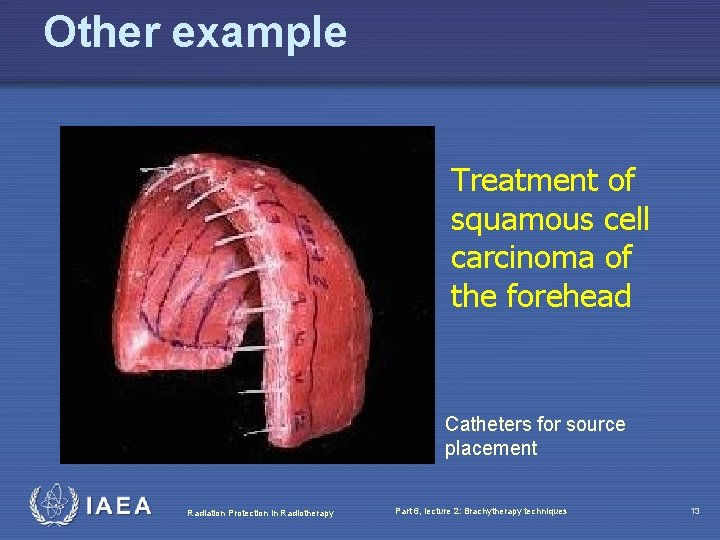
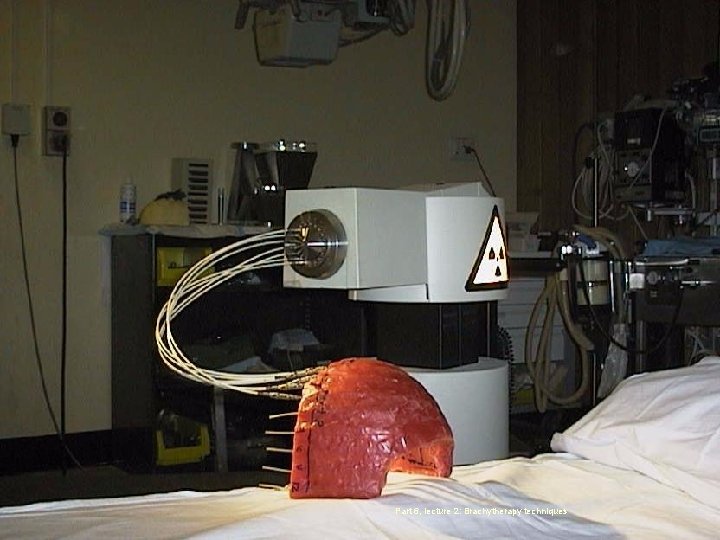
Other example Treatment of squamous cell carcinoma of the forehead Catheters for source placement Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 13

Source distance from the skin • Determines incident dose • Determines dose fall off in skin - the further the sources are from the skin the less influence has dose fall off due to inverse square law • Dose homogeneity - the further away the sources are the more homogenous the dose distribution is at the skin Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 14

Simulator films of forehead mould Dummy wires as markers for location Part 6, lecture 2: Brachytherapy techniques 15

Part 6, lecture 2: Brachytherapy techniques 16

Surface mould advantages • Fast dose fall off in tissues • Can conform the activity to any surface • Flaps available Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 17

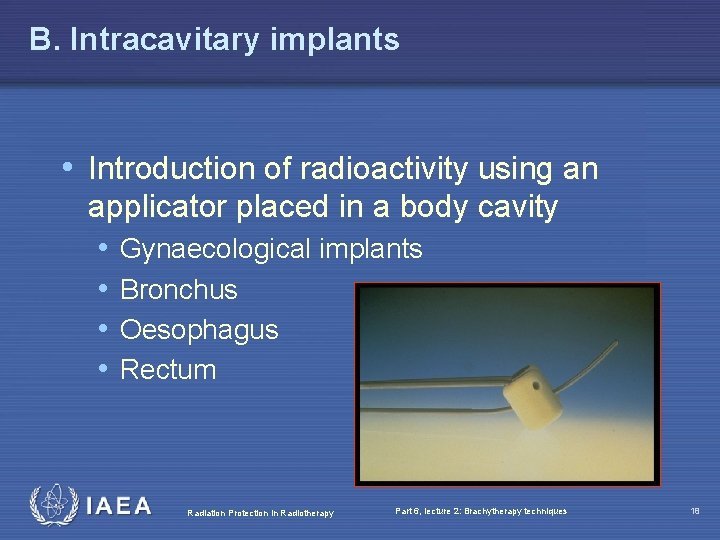
B. Intracavitary implants • Introduction of radioactivity using an applicator placed in a body cavity • Gynaecological implants • Bronchus • Oesophagus • Rectum Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 18

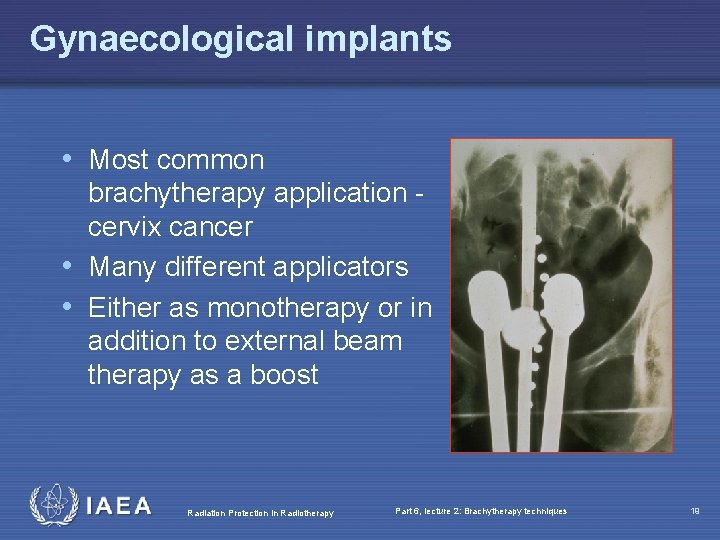
Gynaecological implants • Most common brachytherapy application cervix cancer • Many different applicators • Either as monotherapy or in addition to external beam therapy as a boost Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 19

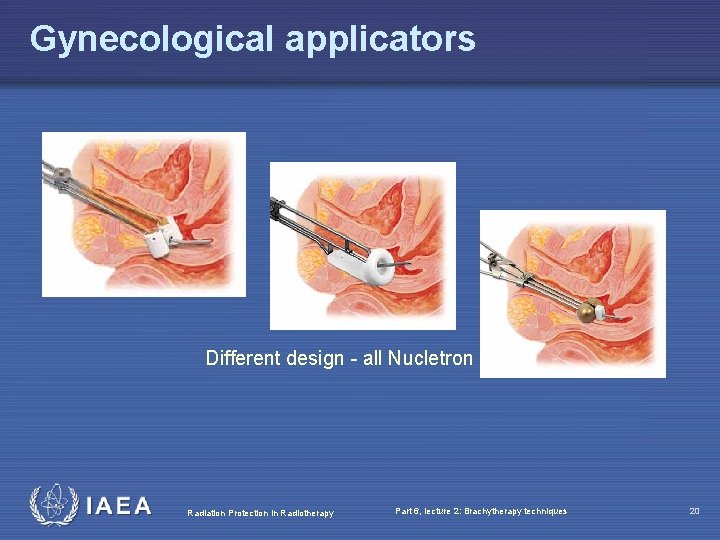
Gynecological applicators Different design - all Nucletron Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 20

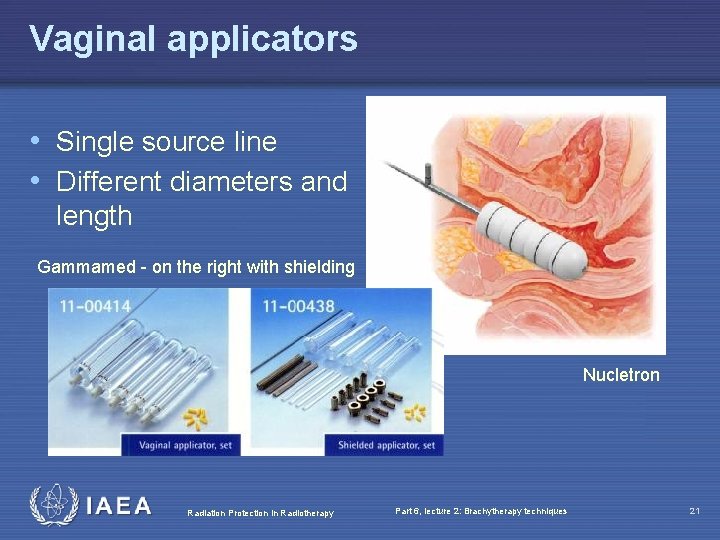
Vaginal applicators • Single source line • Different diameters and length Gammamed - on the right with shielding Nucletron Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 21

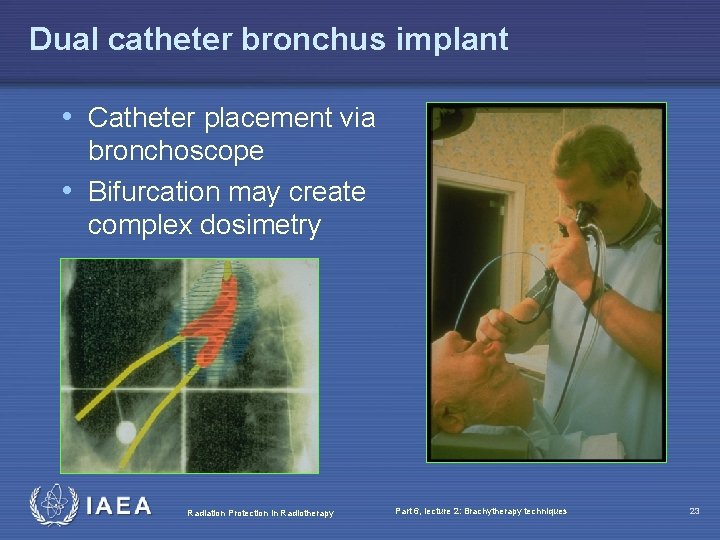
Bronchus implants • Often palliative to open air ways • Usually HDR brachytherapy • Most often single catheter, however also dual catheter possible Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 22

Dual catheter bronchus implant • Catheter placement via bronchoscope • Bifurcation may create complex dosimetry Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 23

C. Interstitial implants • Implant of needles or flexible catheters directly in the target area • Breast • Head and Neck • Sarcomas • Requires surgery - often major Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 24

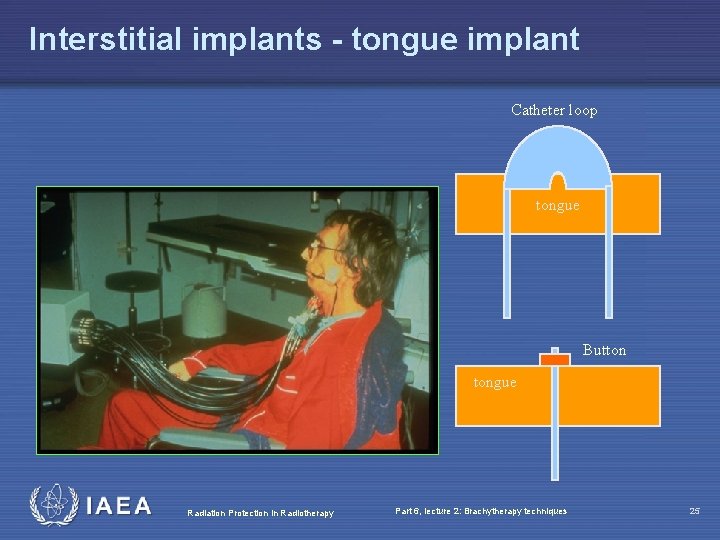
Interstitial implants - tongue implant Catheter loop tongue Button tongue Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 25

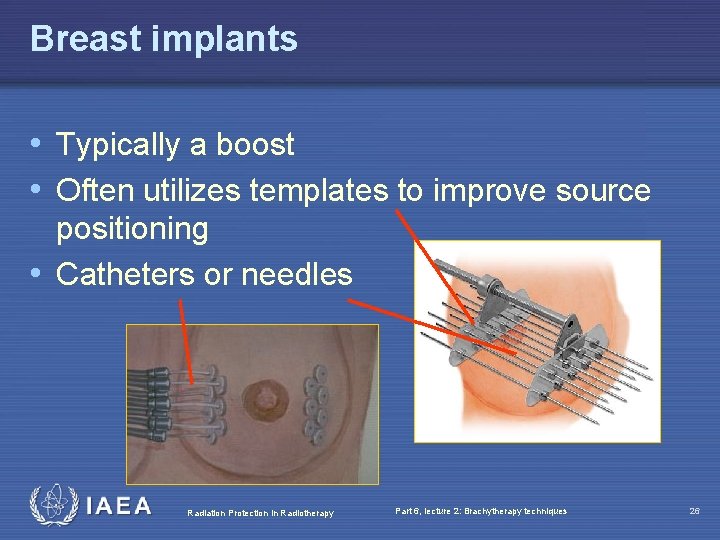
Breast implants • Typically a boost • Often utilizes templates to improve source positioning • Catheters or needles Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 26

2. Implant techniques and applicators • Permanent implants • patient discharged with implant in place • Temporary implants • implant removed before patient is discharged from hospital Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 27

Permanent implants • Implantation of sealed sources (typically seeds) into the target organ of the patient • Sources are NOT removed and patient is discharged with activity in situ (compare part 16 of the course) Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 28

Radiation protection issues • Patients are discharged with radioactive sources in place: • lost sources • exposure of others • issues with accidents to the patient, other medical procedures, death, autopsies and cremation Discussed in more detail in parts 9 (Medical Exposure), 16 (Discharge of patients) and 17 (Public exposure) Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 29

Source requirement for permanent implants • Low energy gammas or betas to minimize radiation levels outside of the patient (125 -I is a good isotope) • May be short-lived to reduce dose with time (198 -Au is a good isotope) • More details on most common 125 -I prostate implants in section 4 A of the lecture Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 30

Temporary implants • Implant of activity in theatre • Manual afterloading • Remote afterloading Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 31

Implant of activity in theatre • (Common for permanent implants) • For temporary implants common practice 40 years ago when radium was commonly used • for example gynecological implants of radium or 137 -Cs needles • Today only very rarely used for temporary implants - one of few examples are 192 Ir hairpins for tongue implants Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 32

Problems with handling activity in the operating theatre • Potential of lost sources • The time to place the sources in the best possible locations is typically limited • Radiation protection of staff may require awkward operation Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 33

Afterloading • Implant only empty applicator or needles/catheters in theatre • Once patient has recovered, dummy sources are introduced to verify the location of the applicators (typically using diagnostic X Rays) • The treatment is planned • The sources are introduced into the applicator or needle/catheter Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 34

Afterloading • Manual • Remote • The sources are placed • The sources are driven manually usually by a physicist • The sources are removed only at the end of treatment Radiation Protection in Radiotherapy from an intermediate safe into the implant using a machine (“afterloader”) • The sources are withdrawn every time someone enters the room Part 6, lecture 2: Brachytherapy techniques 36

Afterloading advantages • No rush to place the sources in theatre more time to optimize the implant • Treatment is verified and planned prior to delivery • Significant advantage in terms of radiation safety (in particular if a remote afterloader is used) Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 37

Quick question: Why is afterloading the method of choice from a radiation safety perspective?

Some radiation safety aspects of afterloading • No exposure in theatre • Optimization of medical exposure possible • No transport of a radioactive patient necessary ‘Live’ implants should be avoided for temporary implants Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 39

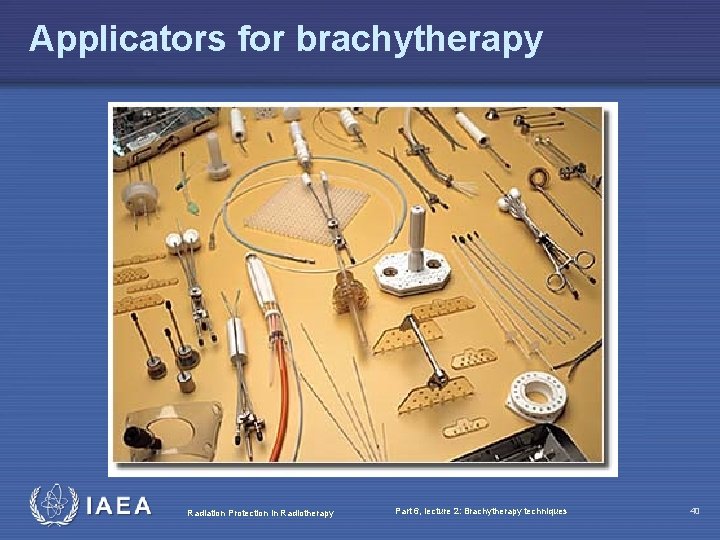
Applicators for brachytherapy Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 40

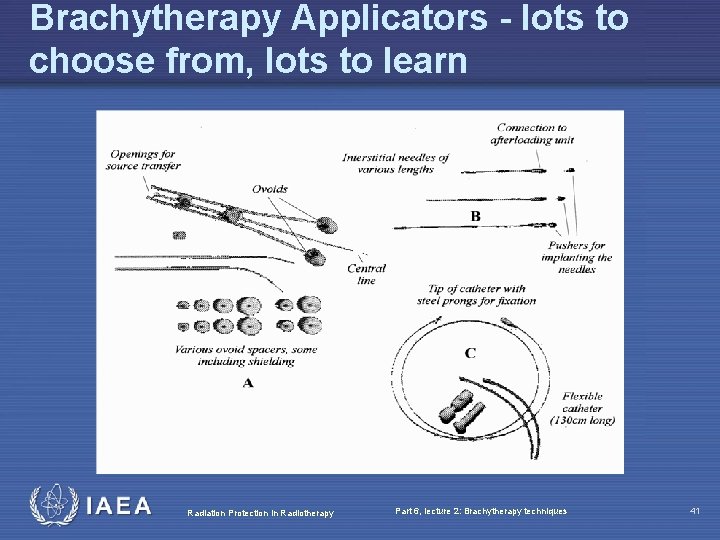
Brachytherapy Applicators - lots to choose from, lots to learn Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 41

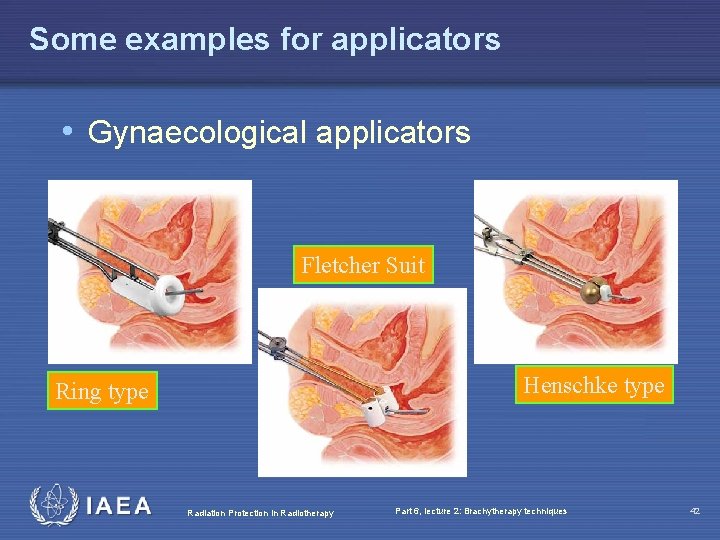
Some examples for applicators • Gynaecological applicators Fletcher Suit Henschke type Ring type Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 42

Rotterdam Applicator • A choice of sizes allows customized treatment of each patient Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 43

Close-up view Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 44

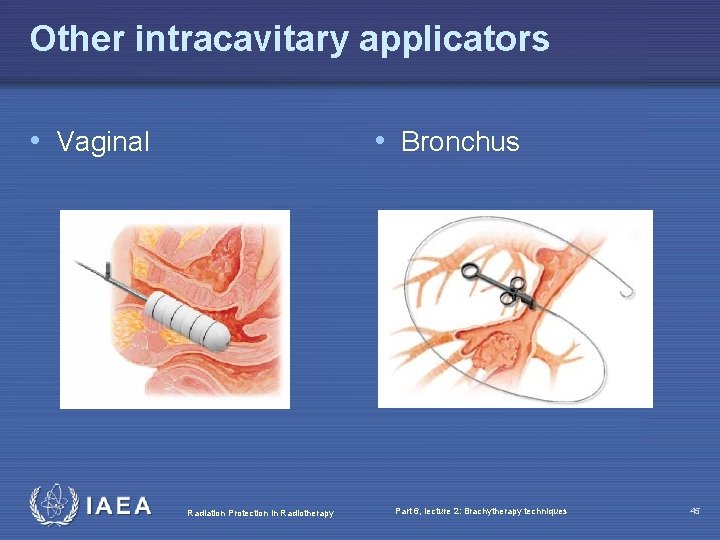
Other intracavitary applicators • Vaginal • Bronchus Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 45

Interstitial applicators • Needles • hollow and rigid • may use templates for placement • usually have pusher during implantation in tissue Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 46

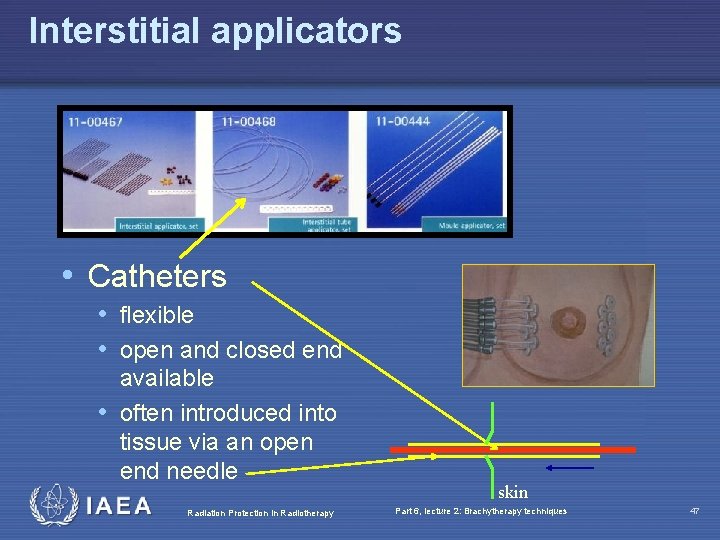
Interstitial applicators • Catheters • flexible • open and closed end available • often introduced into tissue via an open end needle Radiation Protection in Radiotherapy skin Part 6, lecture 2: Brachytherapy techniques 47

3. Delivery modes and equipment • • Low Dose Rate (LDR) Medium Dose Rate (MDR) High Dose Rate (HDR) Pulsed Dose Rate (PDR) Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 48

Delivery modes - different classifications are in use • Low Dose Rate • Medium Dose Rate • High Dose Rate • Pulsed Dose Rate Radiation Protection in Radiotherapy • • • < 1 Gy/hour around 0. 5 Gy/hour > 1 Gy/hour not often used >10 Gy/hour pulses of around 1 Gy/hour Part 6, lecture 2: Brachytherapy techniques 49

Low dose rate brachytherapy • The only type of brachytherapy possible with manual afterloading • Most clinical experience available for LDR brachytherapy • Performed with remote afterloaders using 137 -Cs or 192 -Ir Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 50

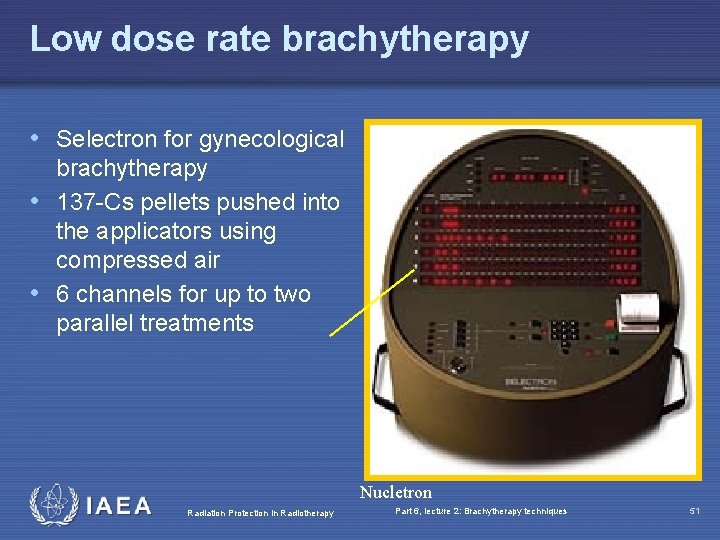
Low dose rate brachytherapy • Selectron for gynecological brachytherapy • 137 -Cs pellets pushed into the applicators using compressed air • 6 channels for up to two parallel treatments Nucletron Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 51

Simple design • No computer required • Two independent timers • Optical indication of source locations • Permanent record through printout • Key to avoid unauthorized use Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 52

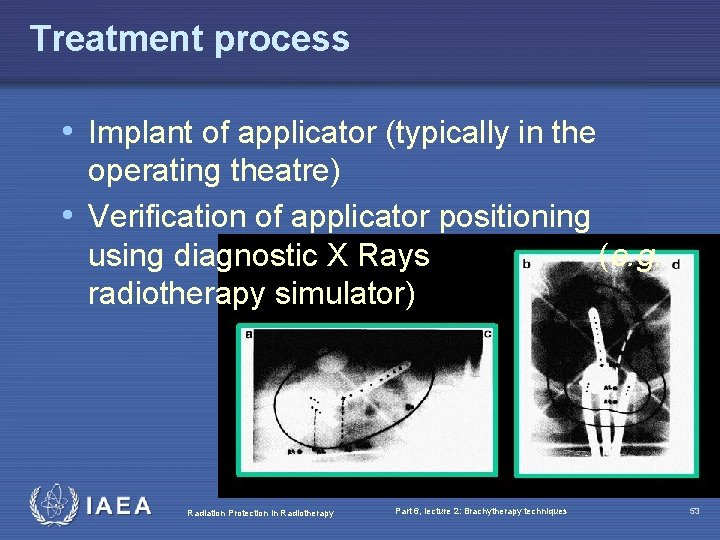
Treatment process • Implant of applicator (typically in the operating theatre) • Verification of applicator positioning using diagnostic X Rays (e. g. radiotherapy simulator) Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 53

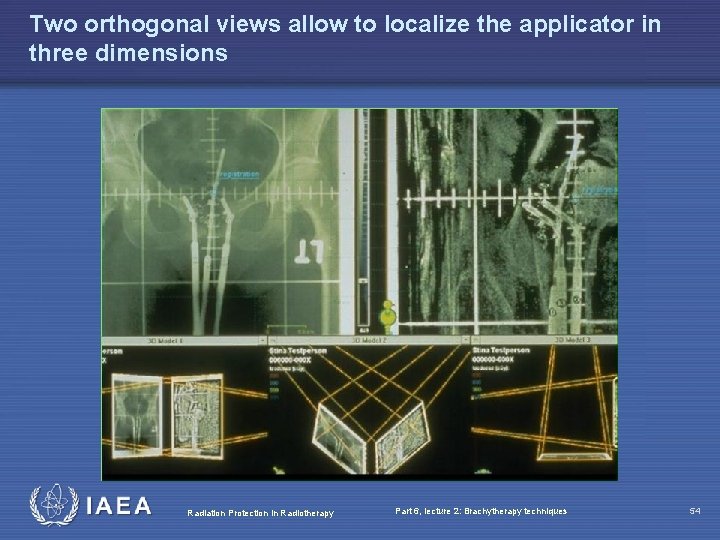
Two orthogonal views allow to localize the applicator in three dimensions Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 54

Treatment planning • Most commercial treatment planning systems have a module suitable for brachytherapy planning: • Choosing best source configuration • Calculate dose distribution • Determine time required to give desired dose at prescription points • Record dose to critical structures Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 55

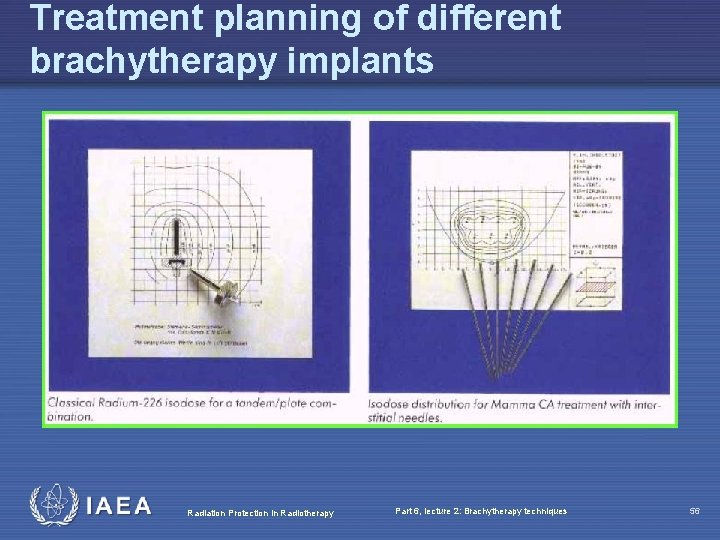
Treatment planning of different brachytherapy implants Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 56

High Dose Rate Brachytherapy • Most modern brachytherapy is delivered using HDR • Reasons? • Outpatient procedure • Optimization possible Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 57

HDR brachytherapy • In the past possible using 60 -Co pellets • Today, virtually all HDR brachytherapy is delivered using a 192 -Ir stepping source Source moves step by step through the applicator - the dwell times in different locations determine the dose distribution Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 58

HDR 192 -Ir source Source length 5 mm, diameter 0. 6 mm Activity: around 10 Ci Radiation Protection in Radiotherapy From presentation by Pia et al. Part 6, lecture 2: Brachytherapy techniques 59

Optimization of dose distribution adjusting the dwell times of the source in an applicator Nucletron Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 60

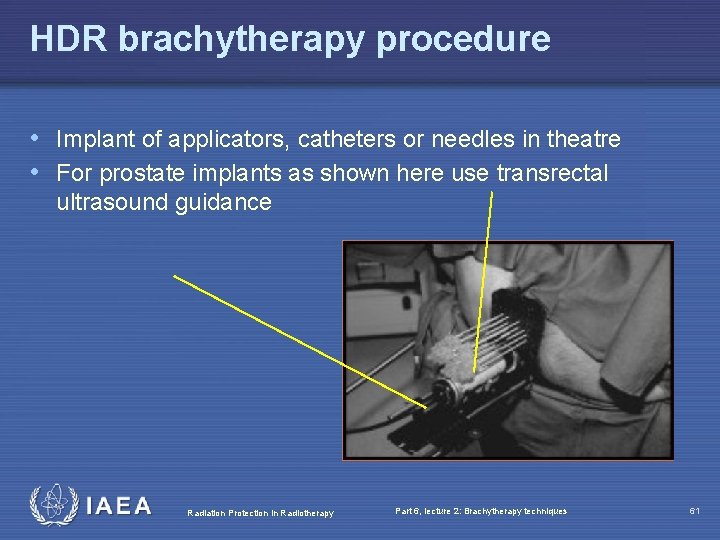
HDR brachytherapy procedure • Implant of applicators, catheters or needles in theatre • For prostate implants as shown here use transrectal ultrasound guidance Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 61

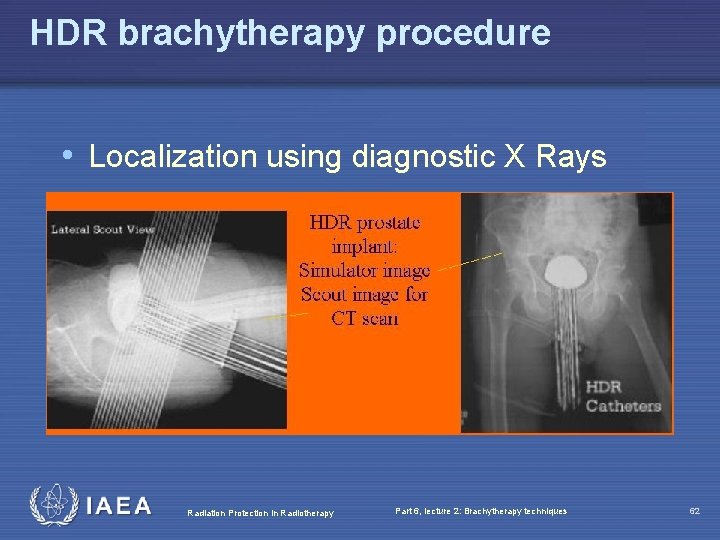
HDR brachytherapy procedure • Localization using diagnostic X Rays Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 62

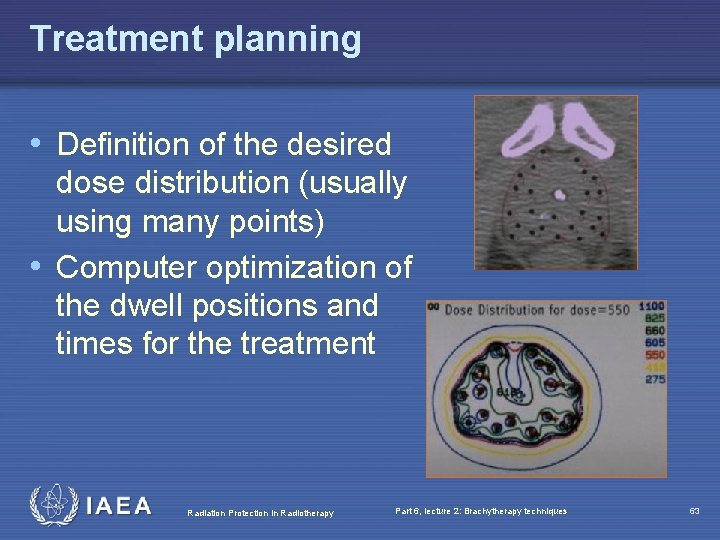
Treatment planning • Definition of the desired dose distribution (usually using many points) • Computer optimization of the dwell positions and times for the treatment Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 63

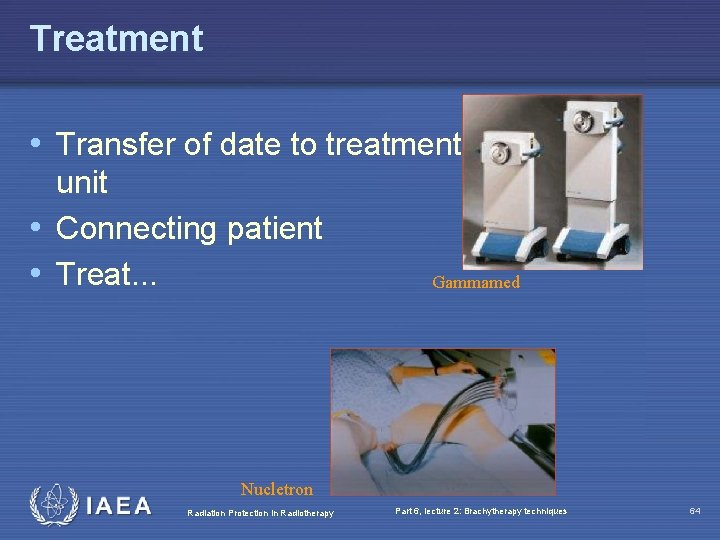
Treatment • Transfer of date to treatment unit • Connecting patient • Treat. . . Gammamed Nucletron Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 64

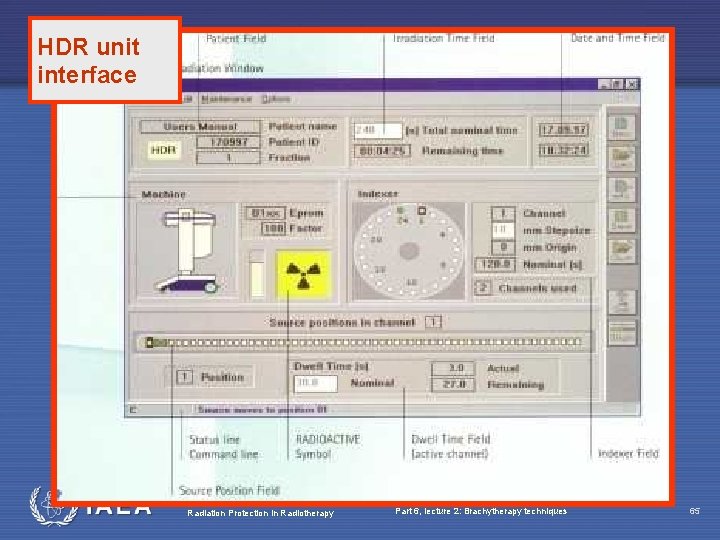
HDR unit interface Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 65

HDR brachytherapy • Usually fractionated (e. g. 6 fractions of 6 Gy) • Either patient has new implant each time or stays in hospital for bi-daily treatments • Time between treatments should be >6 hours to allow normal tissue to repair all damage Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 66

HDR units: different designs available Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 67

Catheters are indexed to avoid mixing them up Transfer catheters are locked into place during treatment - green light indicates the catheters in use Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 68

HDR systems • Can be moved between different facilities or into theatre for intra-operative work Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 69

Pulsed dose rate • Unit has a similar design as HDR, however the • • activity is smaller (around 1 Ci instead of 10 Ci) Stepping source operation - same optimization possible as in HDR Treatment over same time as LDR treatment to mimic favorable radiobiology In-patient treatment: hospitalization required Source steps out for about 10 minutes per hour and then retracts. Repeats this every hour to deliver minifractions (‘pulses’) of about 1 Gy Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 70

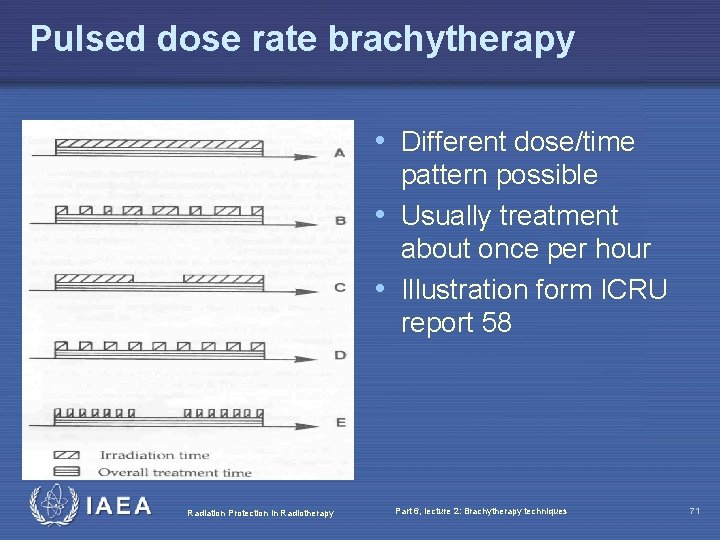
Pulsed dose rate brachytherapy • Different dose/time pattern possible • Usually treatment about once per hour • Illustration form ICRU report 58 Radiation Protection in Radiotherapy Part 6, lecture 2: Brachytherapy techniques 71

Features of PDR: • Advantages • Disadvantages 9 Emulates LDR 9 Optimized dose distribution 9 Visitors and nursing staff can use the time between pulses while the activity is in the safe Radiation Protection in Radiotherapy - Potential radiation safety hazard of a source stuck in the patient: H In LDR - low activity, no severe problem H In HDR - physicist is present during treatment H In PDR - will someone with sufficient training be there within 10 minutes? Even at midnight? ? ? Part 6, lecture 2: Brachytherapy techniques 72

Question: Please list advantages and disadvantages of High Dose Rate Brachytherapy as compared to Low Dose Rate brachytherapy. Assume both approaches are performed using remote afterloading equipment.

The answer should include: • Advantages 9 Out patient procedure 9 Optimization of dose distribution using stepping source 9 Possibly better geometry as patient anesthetized 9 No exposure of nursing staff during procedure 9 No source preparation Radiation Protection in Radiotherapy • Disadvantages $Potential radiobiological disadvantage $Fractionation required $More shielding required $There is no time to intervene if machine failure occurs $More sophisticated (and expensive) Part 6, lecture 2: Brachytherapy techniques 74