I Wanna PeeBut I Cant Renal Failure Dialysis

I Wanna Pee…But I Can’t!!! Renal Failure & Dialysis In the ED A. F. Chad, MD, CCFP Resident Rounds: July 25, 2002

Definitions: ARF • • • Deteriorating GFR over hours to days 50% decrease in GFR 50% decrease in Cr. Cl 50% increase in Scr Need dialysis Non-oliguric vs anuric
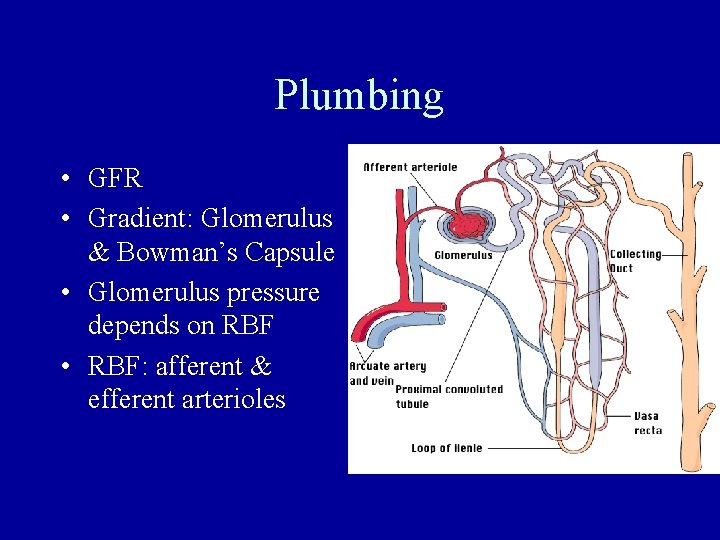
Plumbing • GFR • Gradient: Glomerulus & Bowman’s Capsule • Glomerulus pressure depends on RBF • RBF: afferent & efferent arterioles

When Kidney Pie Goes Wrong • • Acute Chronic Acute on Chronic Transplant

When Kidney Pie Goes Wrong • • Pre-renal Intrinsic Post-renal Evil Kidney Gnomes

Before Kidney Pie Goes Wrong • Most common cause • 40 -80% • Decreased renal perfusion

Before Kidney Pie Goes Wrong • • • Hypovolemia Sequestration Cardiac Renal artery Small Vessel

Inside Kidney Pie Goes Wrong • • 11 -45% of kids ATN 2 nd to ischemia 25% nephrotoxins

Inside Kidney Pie Goes Wrong • • Tubular Interstitial Glomerulonephritis Vasculitides

After Kidney Pie Goes Wrong • • • 2 -5% 20 -35% of Old Men Young Men - stones Young Women - CA Kids – M: postrior urethral valve – F: VCUR

After Kidney Pie Goes Wrong • Urethra and Bladder Outlet • Ureter • Intra Renal Failure

When It All Goes Down the Loo • • • GFR -> gradient b/t glomerulus & Bowman Pressure determined by aff & eff a. a. Prerenal: decreased RBF Intrinsic: release of vasoconstrictors Postrenal: increased tubular pressure

When It All Goes Down the Loo • Low RBF -> cell death -> slough ->block • Nephrons: ++ Filtration & hypertrophy • Too many damaged -> ++ hypertrophy -> sclerosis -> Decreased GFR -> CRF

This is NOT good for you!!! • Mortality 40 -90% • No change since Dialysis (other causes now) • OR for dying: 4. 9 for ARF • Worse for anuric / oliguric • 20 -60% will need dialysis • 25% of these long term

What 2 Ask? • FIFE • Sx of Hypovolemia (N&V&D, CVD, Hemorrhage, insensible) • Infxn, Hypo. TN, Meds, Xray, MSK, Allergy • Prostatism, OR, Gyne, Stones • Usuals (PMHx, All, ROS, FHx, SHx)

What 2 look for? • • • ABC’s, VS (esp HR& BP - orthostatic) Fluid status Derm (skin, eyes) CV & Resp Abdo (MAGIC FINGER!!!) MSK
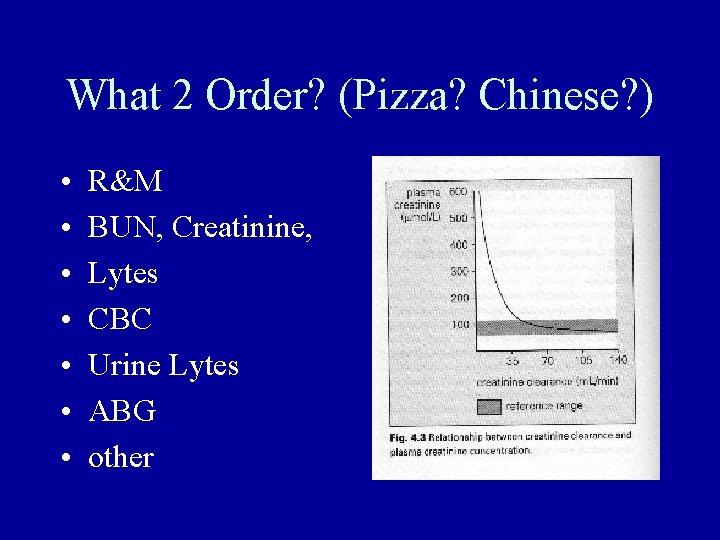
What 2 Order? (Pizza? Chinese? ) • • R&M BUN, Creatinine, Lytes CBC Urine Lytes ABG other

What 2 Calculate • Cockroft-Gault Equation (He taught me & does ice sculptures @ Xmas) – Cr. Cl=[(140 -age)x. Wt] / Scr – (x 0. 85 for F) – N~120 m. L/min • Fractional Excretion of Na – Fe. Na = (UNa/PNa) X (UCr/PCr) X 100 – <1% - Prerenal, >1% ATN
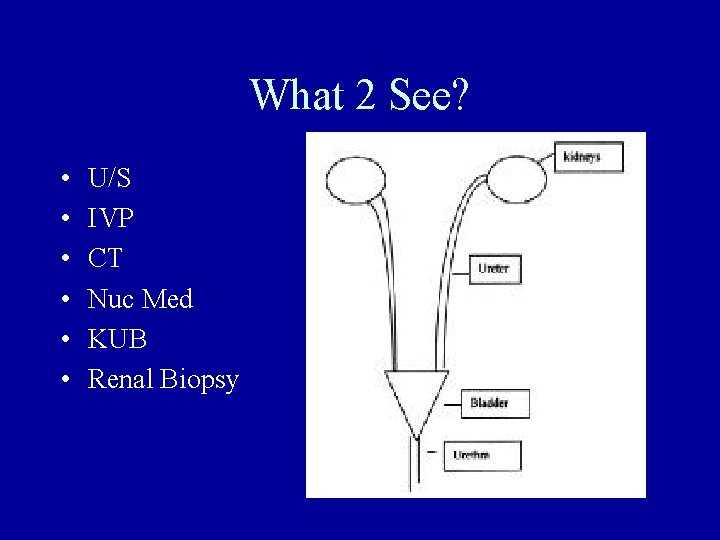
What 2 See? • • • U/S IVP CT Nuc Med KUB Renal Biopsy

Who Cares About This Crap! What Do I Do? !? ! • • ABCD Stop Toxins Rx post renal - Catheter Volume status Correct Lytes, Acid-Base Drugs? Dialyse

Diuretics? CRAP! 92 pts with ARF given diuretic or placebo NO change in recovery, need for HD, death Shilliday IR, Quinn KJ, Allison ME. Loop diuretics in the management of acute renal failure: a prospective, double-blind, placebocontrolled, randomized study. Nephrol Dial Transplant 1997 Dec; 12(12): 2592 -6

Dopamine? Not helpful in RCT of CVD OR pts Lassnigg A, Donner E, Grubhofer G, Presterl E, Druml W, Hiesmayr M. Lack of renoprotective effects of dopamine and furosemide during cardiac surgery. J Am Soc Nephrol 2000 Jan; 11(1): 97 -104 • Not Helpful in Anaesthesia either – Hladunewich M. Pathophysiology and management of renal insufficiency in the perioperative and critically ill patient. Anesthesiol Clin North America - 01 -Dec-2000; 18(4): 773 -89

CCB? • Not helpful 4 prevention radiocontrast tox Carraro M, Mancini W, Artero M, Stacul F, Grotto M, Cova M, Faccini L Dose effect of nitrendipine on urinary enzymes and microproteins following non-ionic radiocontrast administration. Nephrol Dial Transplant 1996 Mar; 11(3): 444 -8

Mannitol & HCO 3? • Good for Rhabdo within 6 hrs – Better OS, Rubenstein I: Management of shock and acute renal failure in casualties suffering from the crush syndrome. Ren Fail 19: 647 1997.

Pee for Them: Hemodialysis • • • Acidosis Lytes (esp K+) Fluid (too much) Uremia (pericarditis, encephalopathy) Drugs Evil Humours

Disposition: Bring ‘em in!!!

Definitions: CRF • Progressive decline in GFR over months to years • Irreversible • Chronic insufficiency: GFR=30 -70 m. L/min • CRF: GFR<30 m. L/min • ESRD: GFR<10 m. L/min

CRF: problems • • Lytes Pericardium IHD Hypo. TN Dysequilibrium Infection Vascular

ESRD • Kidneys don’t work -> Uremia • 96 - USA- 300, 000 Rx (75, 000 new) • DM (33%), HTN (25%), Glomerular (18%), Evil Kidney Gnomes (0. 371%) • Either get New Kidney(s) or Dialysis • 30% 5 year survival rate (with Rx!) • CVD (50%), Infxn (25%), Withdrawal

ESRD: Beware the Gnomes!

UREMIA: This is Mucho Bad!!! • CLINICAL Dx!!!

UREMIA: Neuro • • Uremic Encephalopathy Dialysis Dementia SDH Peripheral

UREMIA: CV • HTN • CHF • Pericarditis

UREMIA: Heme • Anemia • Bleeding • Immunocompromise

UREMIA: GI • • GIB Ascites N&V Diverticular Dx

UREMIA: Bone • • Metastatic Calcification #’s Cysts CTS
I Will Be Your Kidney: Dialysis

How Does HD Work? • • • Pt’s blood into HD machine Filter instead of glomerulus Gradient determines fluid & solute removal Lytes (Na, K, Cl, HCO 3, Ca, Mg), Glucose Not proteins

How Does PD Work? • Uses peritoneum as filter • Diasylate: varied osmotic pressures • Fluid left in for a while, then drained

I Will Be Your Kidney: Dialysis • Chart review 50 CRF pts in Camden, NJ: 68% went home post HD in ED ERSacchetti A. ED hemodialysis for treatment of renal failure emergencie. s Am J Emerg Med - 01 May-1999; 17(3): 305 -7 • Chart review 288 HD pts presenting to ER in Albany, NY: 68% admitted Mc. Erlean M et al. The Emergency Department Care of Hemodialysis Patients. Acad Emerg Med - 1999; 6(5): 538.

Complications During HD • • • Vascular Hypotension Dysequilibrium Air Embolism Lytes

What 2 Ask HD? • • • Cause ESRD? Dialysis schedgy (missed appt? ) Baseline Weight, Labs Weight gain b/t HD Sx Uremia
What 2 Look 4 HD? • • VS Vascular Access CV Neuro

What 2 Ask PD? • • Cause ESRD? Recent PD complications Baseline weight, labs Sx Uremia
What 2 Look 4 PD? • VS • Abdomen • Peritoneal catheter

I can PEE …Again!!!! Transplant Specific Issues • • • Rejection Infection ARF CVD Liver Dx The BIG C

Pee 4 You: What 2 Ask? • • FIFE Temp? Date of Transplant Graft Source? Rejection Hx Chronic Infxn Baseline (creatinine, wt, VS) PMHx, Meds, All, SHx

Special 4 Borrowed Kidneys: ARF • AFR in Transplanted: 20% change in Scr • Causes: – Surgical complications – Rejection – Immunosuppressive Nephrotoxicity

Special 4 Borrowed Kidneys: Infections ONE mos post Surg • UTI (E. Coli) • IV’s (S. aureus, S. viridans) • Pneumonias (streptococcus)

Special 4 Borrowed Kidneys: Infections SIX mos post Surg • Viremia (CMV, EBV) • Meningitis (Listeria) • Sepsis (Aspegillosis)

Special 4 Borrowed Kidneys: Infections Later on • Like you & I (with min immunosupression) • Chronic (EBV, CMV, Hep’s) • Opportunistic (with max immunosupression)

THE END • QUESTIONS will be answered on a fee for service basis.
- Slides: 52