I B D Extraintestinal Manifestations i ist r

I. B. D & Extraintestinal Manifestations i ist r o g o o l N. to r D ma u e h R
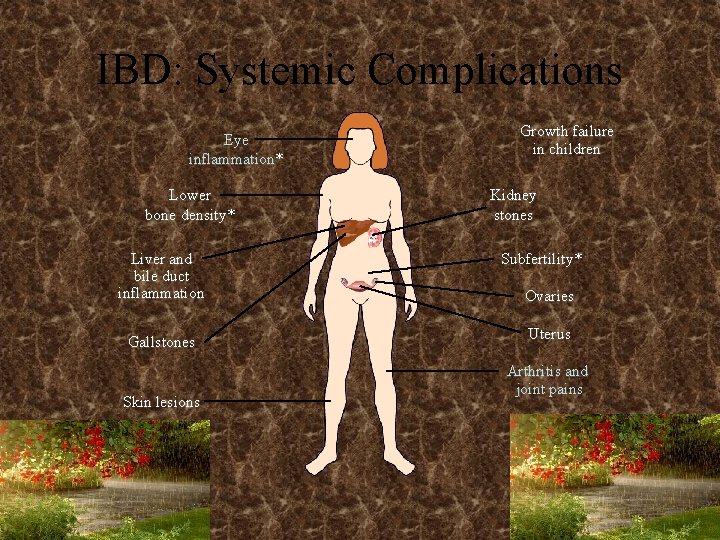
IBD: Systemic Complications Eye inflammation* Lower bone density* Liver and bile duct inflammation Gallstones Skin lesions *Higher incidence in women. Growth failure in children Kidney stones Subfertility* Ovaries Uterus Arthritis and joint pains
IBD: Extra-intestinal Manifestations Skin Eye Bones and Joints Kidney Liver/ Gall Bladder

Crohn's disease, those with colonic involvement are at higher risk of developing synovitis than those with isolated small bowel disease. Males and females are affected equally. Both children and adults are at risk for this complication of IBD.

Type I arthropathy — In type I arthropathy, the peripheral arthritis tends to be acute, is pauciarticular (affecting 4 or fewer joints), is often associated with flares of the bowel disease, occurs early in the course of the bowel disease, is selflimiting (90 percent under 6 months), and does not result in joint deformities. The knee is most commonly affected. Five percent of IBD patients develop type I arthropathy.

Type II arthropathy patients have polyarticular disease, with (MCP) joints being particularly involved. Other joints (knees, ankles, elbows, shoulders, wrists, (PIP), and (MTP) joints) are less often affect.

Approximately one half of the patients with IBD have migratory arthritis. Active synovitis may persist for months, and may recur repeatedly. Episodes of exacerbations and remissions may continue for years. Type II arthropathy affects 3 to 4 percent of patients with IBD. Articular involvement rarely precedes the diagnosis of IBD and joint symptoms typically do not parallel the activity of bowel disease.

Spinal arthropathy — Spondylitis occurs in 1 to 26 percent of patients with IBD. Males are more frequently affected than females. Patients typically complain of prolonged stiffness in the back and/or buttocks in the morning or after rest. Stiffness and associated pain are often relieved by exercise. Back symptoms are unrelated to those of the gastrointestinal disease

Axial arthropathy Less common than peripheral �� Spondylitis and Sacroilitis �� Presents as low back pain and morning stiffness �� Disease does not parallel bowel activity
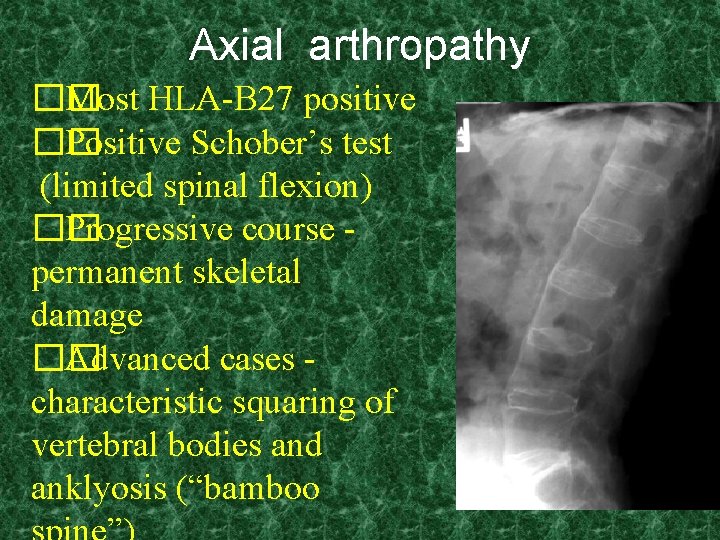
Axial arthropathy �� Most HLA-B 27 positive �� Positive Schober’s test (limited spinal flexion) �� Progressive course permanent skeletal damage �� Advanced cases characteristic squaring of vertebral bodies and anklyosis (“bamboo

Musculoskeletal Manifestations Less common is �� Septic joint (as a complication of psoas abscess extension) �� Amyloidos �� Pseudoarthritis due to withdrawal of steroids �� Aseptic necrosis of the hip due to steroids

Diagnosis — There is no pathognomonic finding to confirm the clinical suspicion of arthritis due to IBD. While the diagnosis may be suspected in the proper clinical setting, it remains largely one of exclusion

treatment Peripheral arthritis — Some agents, notably sulfasalazine, azathioprine, 6 -mercaptopurine, methotrexate, glucocorticoids, and tumor necrosis factor (TNF) inhibitors may be helpful for both bowel and joint inflammation. NSAIDs may relieve the arthritic symptoms, but may have an adverse effect on the IBD

— Osteoporosis is common in patients with inflammatory bowel diseases (IBD) such as Crohn's disease (CD) or ulcerative colitis (UC

a history and physical examination to elicit clinical risk factors for fracture. obtain a DXA in patients who are at higher risk for osteoporosis and fracture: (history of previous fragility fracture, postmenopausal, male >50 years, chronic corticosteroid therapy [>3 months], or hypogonadism)
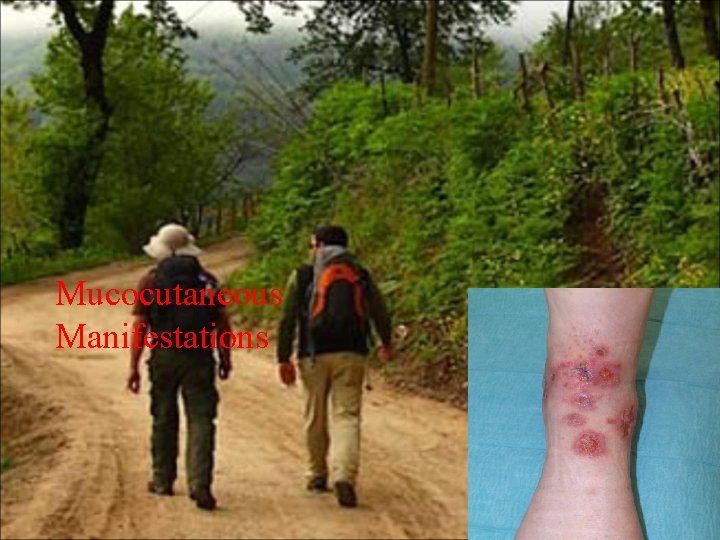
Mucocutaneous Manifestations
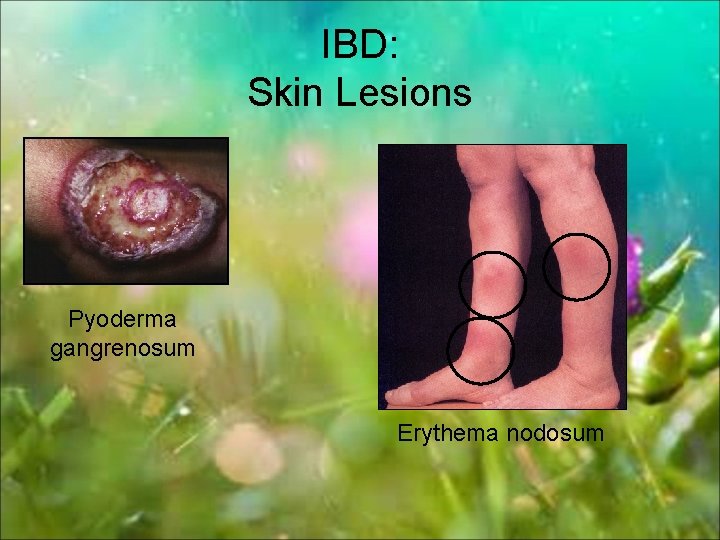
IBD: Skin Lesions Pyoderma gangrenosum Erythema nodosum

Erythema nodosum �� Female > Male �� Tender, red subcutaneous nodules �� Usually pretibial �� Strongly associated with arthropathy �� Occurs with flares of bowel symptoms
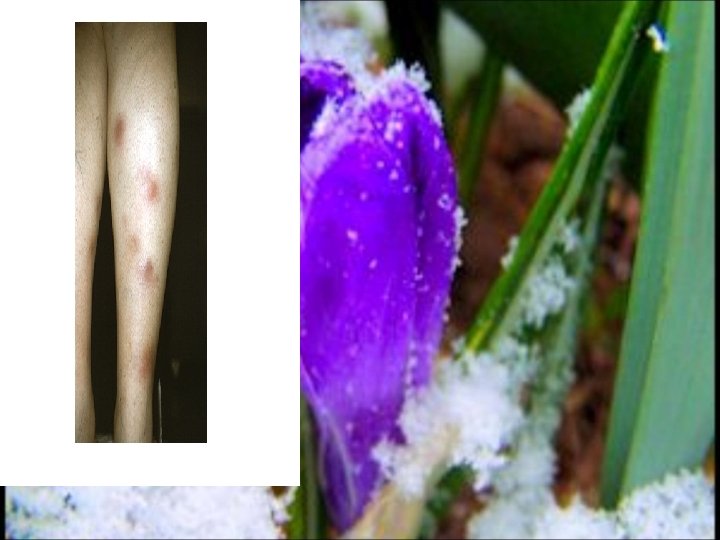

The appearance of erythema nodosum usually parallels intestinal disease activity, and treatment directed at the underlying bowel disease usually results in elimination of the lesions.

ERYTHEMA NODOSUM • • • Streptococcal infections- most common cause Sarcoidosis Idiopathic Tuberculosis IBD- More association in US than in developing countries Drugs- OCP, Erythromycin, sulfa, Other infections: histoplasmosis, Coccidiomycosis, Brucellosis, systemic Fungal infections, Leprosy, Mycoplasma, chlamidia, Gonococcemia Allergies Pregnancy of OCP Vasculitis- Behcets syndrom, SLE variants, Pancreatiits, Hodgkins T cell immunodeficincies

, therapy with prednisone may be required. The usual starting dose is 40 mg/day. A response is typically seen within one week; the prednisone can then be tapered over the ensuing three to four weeks
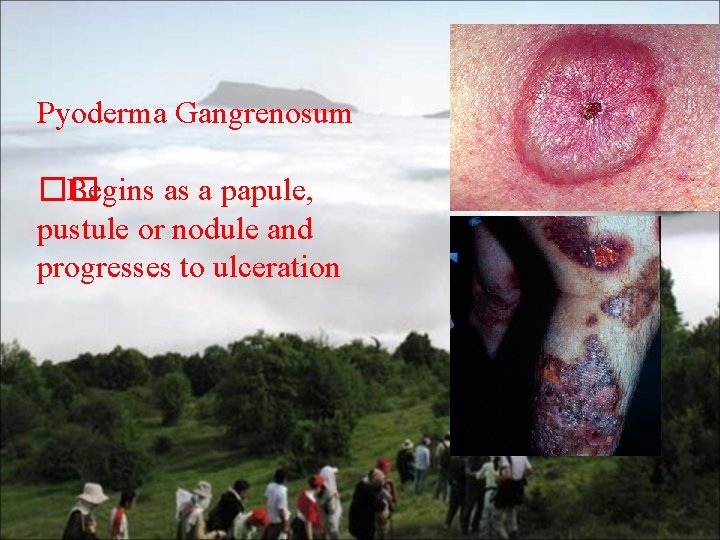
Pyoderma Gangrenosum �� Begins as a papule, pustule or nodule and progresses to ulceration

Subsequent necrosis of the dermis leads to the development of deep ulcerations that contain purulent material which is usually sterile on culture. Biopsy reveals nonspecific findings consistent with a sterile absces

PYODERMA GANGRENOSUM • Is an Inflammatory skin disease often associated with underlying systemic disorder such as IBD, Arthritis or Lymphoproliferative disorder • The eruptions begin as an isolated pustule or scattered lesions with rapid progression into large ulcers • Diagnosis is made after an infectious aetiology is excluded

. They occur most commonly on the legs, but can develop in any area of the body, including the abdominal wall adjacent to the stoma after colectomy as well as in other surgical scars or areas of trauma.
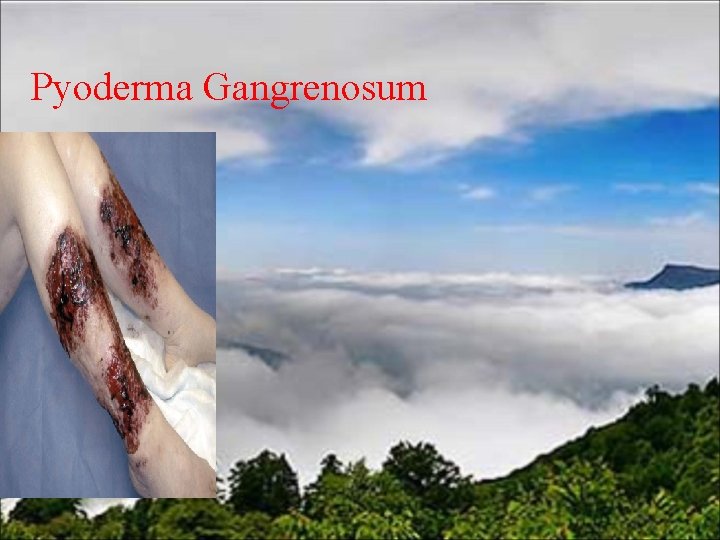
Pyoderma Gangrenosum

• Pyoderma gangrenosum — Despite its relatively infrequent occurrence, it often has more serious consequences than erythema nodosum such as persistence of the lesions and local discomfort even with appropriate therapy

Mucocutaneous Manifestations Less Common �� Apthous ulcerations in mouth �� Metastatic Crohn’s (granulomatous s inflammation of the skin) �� Leukocytoclastic vasculitis �� Sweet’s syndrome (neutrophilic s dermatosis) �� Increased rates of psoriasis

Lesions termed metastatic Crohn's disease consisting of ulcerating nodules that show noncaseating granulomas on biopsy. These lesions can occur anywhere on the body; they have been most frequently described on the anterior abdominal wall in the submammary area, and on the arms and legs ]. They respond well to systemic steroids.

Psoriasis occurs more commonly in patients with Crohn's disease than in the general population. ). Patients with psoriasis complicated by psoriatic arthritis commonly have microscopic inflammation in the colon even if they do not have bowel symptoms
Necrotizing cutaneous vasculitis is rarely associated with IBD. It is a serious complication which can progress to peripheral gangrene. Aggressive management with high dose steroids and possible colectomy is indicated.
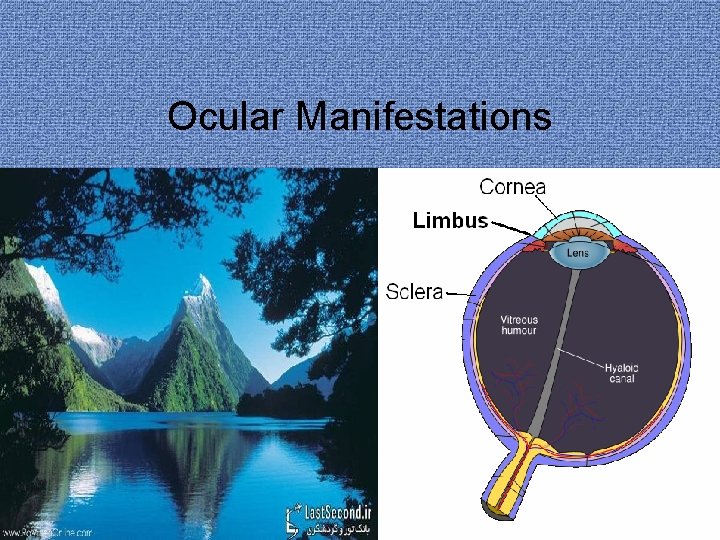
Ocular Manifestations

Ocular Manifestations �� < 10% with IBD will have ocular manifestations �� Can lead to permanent vision loss �� Important to know when to refer to ophtalmologist.

Eye Findings in IBD �� Tearing �� Burning �� Itching �� Ocular Pain �� Photophobia �� Conjunctival/Scleral Hyperemia �� Blurred Vision

Episcleritis �� Ocular exam – focal or diffuse patches of redness within which white patches of sclera can be seen between the dilated episcleral vessels �� Symptoms usually improve with treatment of underlying IBD
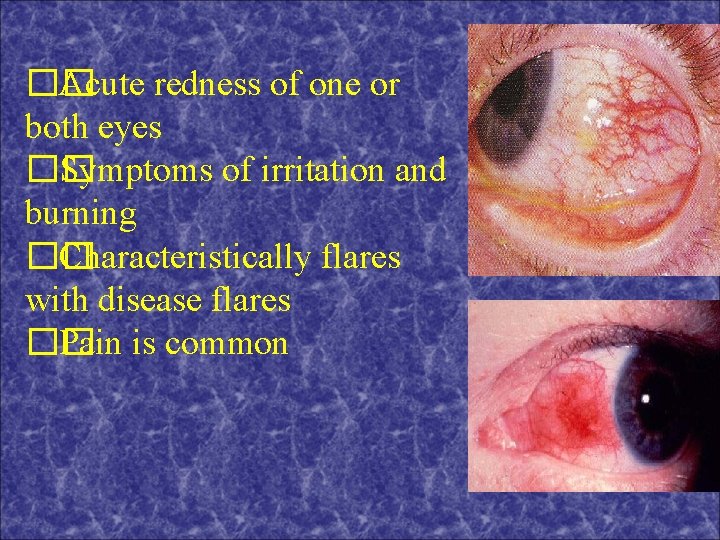
�� Acute redness of one or both eyes �� Symptoms of irritation and burning �� Characteristically flares with disease flares �� Pain is common
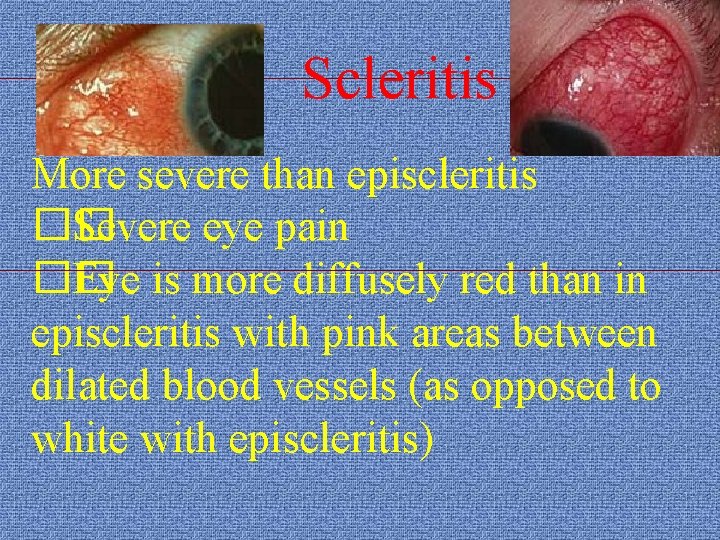
Scleritis More severe than episcleritis �� Severe eye pain �� Eye is more diffusely red than in episcleritis with pink areas between dilated blood vessels (as opposed to white with episcleritis)

Scleritis �� Can lead to vision impairment �� Can lead to retinal detachment or optic nerve swelling �� Must be treated with systemic steroids, or immunosuppressants to prevent vision loss �� Requires urgent referral to ophtalmologist.

Ocular Manifestations Key Points �� If the patient present with a red eye + pain or visual changes, REFER to ophtho (scleritis/uveitis can lead to permanent visual loss) �� All IBD patients should have routine eye exams

Genitourinary Manifestations

Nephrolithiasis -7 -10% patients with IBD �� Uric acid and calcium oxalate most common types

Nephrolithiasis Uric acid stones Due to volume depletion (diarrhea/ileostomy output) and hypermetabolic state Kidneys respond to fluid loss by forming concentrated acidic urine which favors uric acid crystal precipitation Patients with ileostomy are at highest risk - -

IBD and Fertility

IBD and Fertility females with Crohn’s have somewhat impaired fertility – Mechanisms vary – (dyspareunia, perineal disease, impaired ovulation, etc) �� Males with Crohn’s may have reversible s infertility due to sulfasalazine �� No difference in fertility in UC patients

Pregnancy and IBD �� Patients in remission are likely to remain in remission throughout the pregnancy �� Patients with active disease at the time of conception have poorer outcomes

Hepatobiliary Manifestations

Gallstones -17 -34% of patients with CD �� Does not appear to be an increased risk in UC �� CD of the colon does not increase the risk for gallstone formation

PSC Most common hepatobiliary complication of IBD �� 70 -80% PSC patients have concomitant IBD �� 1. 4 -7. 5% IBD patients will develop PSC

Pancreatitis �� Increased risk of both acute and chronic pancreatitis in IBD

Secondary Systemic Amyloidosis �� Very rare ––CD > UC (0. 9% vs. 0. 07%)�� Often affects the kidney�� Proteinuria Nephrotic Syndrome Fat pad biopsy most sensitive test for diagnosis.

Hematologic Manifestations

Anemia Multifactorial GI Blood loss B 12 malabsorption in CD patient with ileal inflammation or resection Iron malabsorption with CD of the duodenum Folate malabsorption with inflammation in the jejunum Bacterial overgrowth due to strictures or resection (low B 12, nml/high folate ) – – –

LAB FINDINGS • In mild cases Lab findings are NORMAL • Anemia is a common finding from Iron deficiency of Blood loss or B 12/ Folate malabsorption in CD • Hypoalbuminemia, metabolic bone disease from malabsorption are common in CD • Hypokalemia , Metabolic acidosis from severe diarrhea • Acute Phase reactants- ESR, CRP • UC p ANCA +/ ASCA - • CD p ANCA -/ ASCA +

General Recommendations for Patients with IBD �� Annual eye exams if significant history of steroid use (increased cataract formation) and early referral for visual symptoms �� Baseline DEXA, calcium and vitamin D supplementation ’

The erythema nodosum and episcleritis parallel disease activity while pyoderma gangrenosum and uveitis may not.

PRIMARY RESPIRATORY INVOLVEMENT — Pulmonary complications of IBD include inflammation of small and large airways, pulmonary parenchymal disease, serositis, and pulmonary embolism
![bronchitis or bronchiectasis: cough and variable amounts of mucopurulent sputum production]. symptoms unresponsive to bronchitis or bronchiectasis: cough and variable amounts of mucopurulent sputum production]. symptoms unresponsive to](http://slidetodoc.com/presentation_image/79b6db08cf27fe5471a0d9173446ea65/image-58.jpg)
bronchitis or bronchiectasis: cough and variable amounts of mucopurulent sputum production]. symptoms unresponsive to antibiotics. Chest radiographyare: frequently normal or show nonspecific changes resulting from bronchial wall thickening or bronchiectasis

Enteric-pulmonary fistulas, such as colobronchial, ileo-bronchial, and esophagobronchial, have been described in patients with Crohn’s disease.

The clinical presentation of ILD is generally characterized by a subacute onset of dyspnea, crackles on chest examination, and radiographic findings of diffuse ground glass or reticular opacities, most prominent at the lung bases. Patients may have a stable course or manifest progressive respiratory insufficiency.

Sarcoidosis — Several cases of sarcoidosis coexisting with ulcerative colitis or Crohn’s disease have been reported.

TREATMENT — The treatment of the various pulmonary complications of IBD depends on the site, severity, and type of involvement. The activity of the underlying IBD does not always correlate with the activity of lung involvement, so lung involvement is often treated independently.

Thromboembolism Both UC and Crohn’s disease are prothrombotic �� Venous thromboembolism > arterial �� In > 50% with thrombosis, no precipitating factor found �� Associated factors include - thrombocytosis; increased levels of fibrinogen, fibrinopeptide A, factor V, and factor VIII; antithrombin III deficiency; and free protein S deficiency - All are related to active bowel inflammation.

Pulmonary thromboembolism — In patients with IBD, the choice of treatment of acute pulmonary thromboembolism depends on the expected risk of gastrointestinal bleeding. For patients with active IBD, especially with significant bleeding, an inferior vena cava filter is usually inserted anticoagulation deferred until the IBD is under control. If the patient is not deemed to be at increased risk for gastrointestinal bleeding, the usual guidelines for anticoagulation with heparin and then warfarin are followed.

ITP and IBD • Not a frequent association • Usually associated with Ulcerative Colitis • Decrease in platelet counts observed during flares • Various treatment modalities used to induce remission

ITP and IBD • Treatment – Short course of steroids – IVIG – Splenectomy may be required to maintain platelet count • + colectomy if active colitis – Colectomy should be considered if colitis remains active despite medical therapy

- Slides: 67