Hypoxic Ischemic Encephalopathy Electrolyte and Acidbase Disturbances Sodium
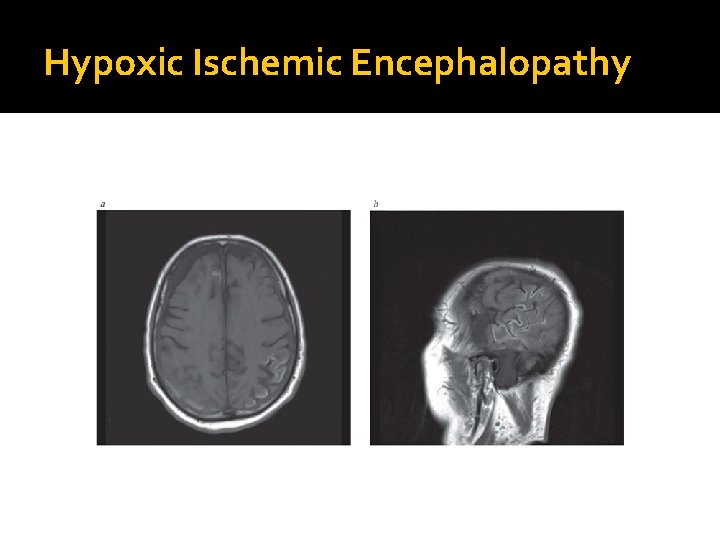
Hypoxic Ischemic Encephalopathy

Electrolyte and Acid-base Disturbances Sodium Hypernatremia and hyponatremia ▪ ▪ Impaired arousal and cognition Seizures Myoclonus Tremor Hyponatremia ▪ May have focal deficits ▪ Correct for hyperglycemia and pseudohyponatremia (high triglycerides) ▪ Rapid correction predisposes to osmotic demyelination syndrome (ODS) ▪ ▪ ▪ Obtundation Conjugate gaze palsy Corticospinal tract signs Pseudobulbar palsy Potentially fatal Hypernatremia ▪ Rapid correction may cause cerebral edema (idiogenic osmoles)
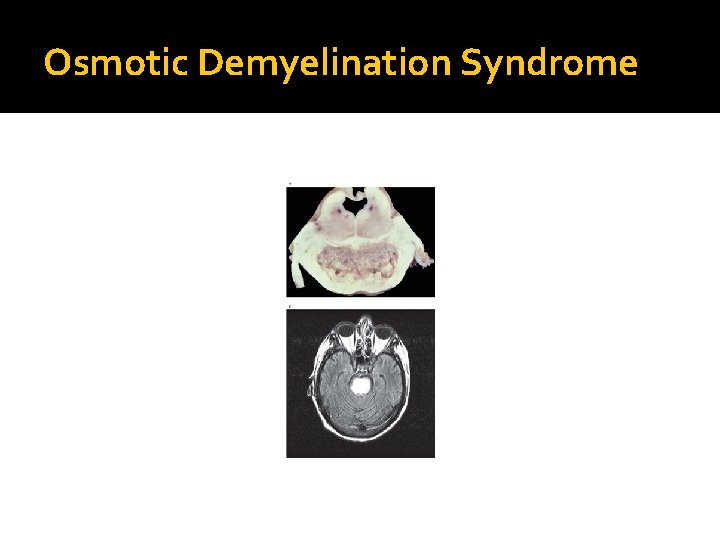
Osmotic Demyelination Syndrome

Electrolyte and Acid-base Disturbances (cont. ) Calcium disorders Impaired sensorium (agitation, delusions, hallucinations) Seizures (more common with hypocalcemia) Hypercalcemia ▪ ▪ ▪ Hyperparathyroidism (usual cause) Anorexia, vomiting, osmotic diuresis Impaired neuromuscular transmission (generalized weakness and hyporeflexia) Fluid resuscitation Furosemide, calcitonin, corticosteroids, bisphonates, plicamycin, and hemodialysis as adjunctive therapy Hypocalcemia ▪ Tetany and extrapyradamidal signs when severe Magnesium Calcium channel blockade Symptoms uncommon ▪ Hypermagnesemia (typically during IV infusion for eclampsia) ▪ Impaired arousal, hypotension, decreased neuromuscular transmission, respiratory depression ▪ Hypomagnesemia ▪ Coexists and similar to hypocalcemia Hypophosphatemia Rarely symptomatic (when severe—depressed consciousness and seizures)

Electrolyte and Acid-base Disturbances (cont. ) Respiratory acidosis CO 2 narcosis Hypoxemia and hypotension Respiratory alkalosis Transient confusion and lightheadedness Perioral and acral paresthesias (decreased ionized calcium) Metabolic acid-base disorders Acute encephalopathy typically due to the underlying metabolic abnormality rather than the acid-base disturbance

End Organ Failure Hepatic encephalopathy Acetaminophen, viral hepatitis, and toxin-mediated injury can cause acute hepatic failure GI bleeding, high protein intake, meds, infections may trigger encephalopathy with chronic liver disease Clinical findings ▪ Depressed consciousness, agitation, asterixis, posturing, extensor plantar reflexes ▪ EEG shows triphasic waves ▪ Ammonia elevated in 90% Pathophysiology ▪ Decreased clearance of metabolic toxins and meds ▪ Blood-brain barrier permeability (cerebral edema) Treatment ▪ Lactulose, rifaximin, transplantation

End Organ Failure (cont. ) Uremic encephalopathy Clinical manifestations ▪ Confusion >> coma ▪ Myoclonus, asterixis ▪ EEG may show triphasic waves Pathophysiology ▪ Decreased clearance of neurotoxins Treatment ▪ Renal replacement therapy ▪ Dialysis dysequilibrium ▪ During or after dialysis in those recently started on dialysis ▪ Headache, seizures, lethargy, elevated intracranial pressure ▪ Treatment Stop/slow dialysis Osmotherapy may be required
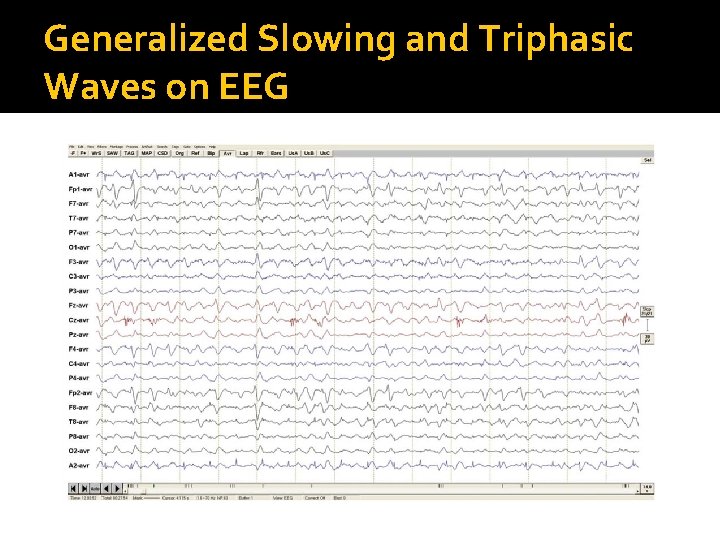
Generalized Slowing and Triphasic Waves on EEG

Nutritional Thiamine deficiency Wernicke encephalopathy ▪ ▪ Affects mammillary bodies, medial dorsal thalamus, and periaqueductal gray Triad (mental status changes, ataxia and opthalmoplegia) seldom all present Occasionally postural hypotension, cardiac failure, and GI symptoms Treatment ▪ IV thiamine Korsakoff syndrome ▪ ▪ ▪ Chronic disorder (often transition from Wernicke encephalopathy) Impaired memory and learning out of proportion to other cognitive domains Profound anterograde and retrograde amnesia Confabulation, anxiety, apathy Infrequent recovery

Nutritional (cont. ) Niacin deficiency Pellagra (pelle agra “rough skin”) ▪ Seen in ETOH use disorder, anorexia nervosa, INH use ▪ Irritability, insomnia, confusion, and cognitive impairment ▪ Startle myoclonus ▪ Photosensitive dermatitis, diarrhea ▪ Nicotinic acid metabolites in urine ▪ Treatment ▪ IV niacin 25 -250 mg 2 -3 times daily Lead toxicity Altered mental status, neuropathy (rare in isolation), dementia Intractable colic, weakness including wrist/foot drop, thin blue-gray line at gums (Burton line) Microcytic, hypochromic anemia with basophilic stippling or RBCs Painful neuropathy Hair and nail changes (Mees lines) Liver and renal dysfunction Color vision changes, neuropathy Pulmonary and renal dysfunction Apathy, ataxia, headaches, myoclonus, hallucinations and seizures Parkinsonism, gait abnormalities, tremor, and psychiatric disturbances Can occur with TPN containing trace elements Arsenic toxicity Mercury toxicity Bismuth toxicity Manganese toxicity

Endocrine Disorders Thyrotoxicosis (Graves’ disease or toxic multinodular goiter) Precipitating factors ▪ Trauma, obstetric labor, lithium, iodinated contrast, non-thyroid surgery Agitation, restlessness, emotional lability, confusion, psychosis, coma Tachycardia, fever Hypercoagulability (high index of suspicion for cerebral venous sinus thrombosis) Elevated thyroid levels, decreased TSH, high calcium, mild leukocytosis, hyperglycemia, elevated serum LDH and aminotransferase Treatment ▪ PTU or methimazole followed by iodine ▪ Supportive management with propranolol, antipyretics, and fluids 75% mortality with thyrotoxic storm Myxedema coma (rare, mortality 70%) Precipitating factors ▪ Infection, heart failure, trauma, cold exposure, anesthesia, and medication non-adherence superimposed on underlying hypothyroidism Cognitive dysfunction, depression, lethargy, somnolence, coma, hallucinations (“myxedema madness”), seizures Hypoventilation, bradycardia, cardiomegaly, decreased contractility Hyponatremia, decreased GFR Hypothermia Dry skin, sparse hair, macroglossia Periorbital, foot, and hand edema Decreased thyroid levels, elevated TSH (no correlation with severity), elevated CK, normocytic anemia, elevated CSF protein and opening pressure Treatment ▪ Thyroid hormone replacement and supportive

Endocrine Disorders (cont. ) Hashimoto encephalopathy (controversial) “Steroid responsive encephalopathy with autoimmune thyroiditis” (SREAT) and “non-vasculitic autoimmune meningoencephalitis” (NAIM) Common—Clouding of consciousnes with reduced wakefulness, attention, or cognitive function Reported—stroke-like episodes, coma, seizures, subacute cognitive decline, tremor, myoclonus, transient aphasia, sleep abnormalities, gait dysfunction, hallucinations High titers of antithyroid antibodies (ATG, TPO, antithyroid microsomal) MRI may show leukoencephalopathy Often prompt response to IVMP 1 gm daily 3 -5 days followed by prednisone 60 -100 mg daily up to 30 days Causes Acute adrenal insufficiency ▪ ▪ ▪ Manifestations ▪ ▪ Primary injury to adrenal gland Secondary—interference with ACTH release by the pituitary gland Tertiary—interference with corticotropin releasing hormone by the hypothalamus Iatrogenic—suppression of HPA axis due to chronic corticosteroid use Relative—inappropriately low cortisol production and adrenal suppression associated with sepsis (incidence 20 -60%) Confusion, lethargy, coma, convulsions Circulatory failure, abdominal pain, vomiting, fever, hypoglycemia, hyperkalemia, hyponatremia Treatment ▪ ▪ Circulatory support Stress-dose steroids
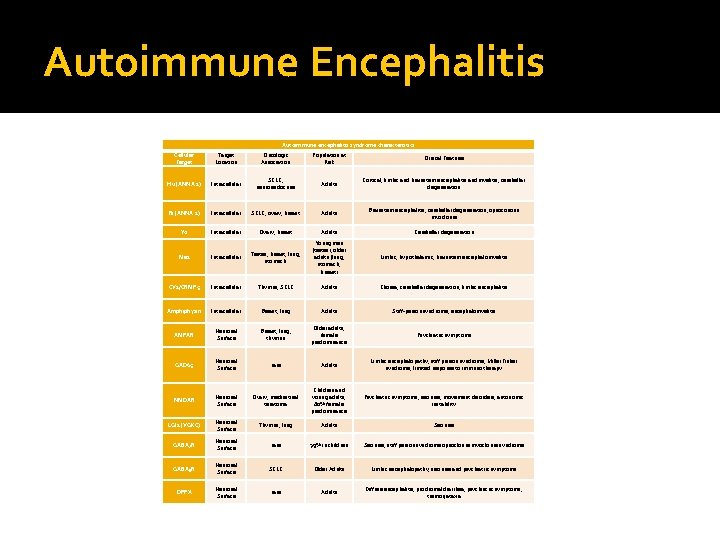
Autoimmune Encephalitis Autoimmune encephalitis syndrome characteristics Cellular Target Location Oncologic Association Population at Risk Clinical Features Hu (ANNA 1) Intracellular SCLC, neuroendocrine Adults Cortical, limbic and brainstem encephalitis and myelitis; cerebellar degeneration Ri (ANNA 2) Intracellular SCLC, ovary, breast Adults Brainstem encephalitis, cerebellar degeneration, opsoconous myoclonus Yo Intracellular Ovary, breast Adults Cerebellar degeneration Limbic, hypothalamic, brainstem encephalomyelitis Ma 2 Intracellular Testes, breast, lung, stomach Young men (testes), older adults (lung, stomach, breast) CV 2/CRMP 5 Intracellular Thymus, SCLC Adults Chorea, cerebellar degeneration, limbic encephalitis Amphiphysin Intracellular Breast, lung Adults Stiff-person syndrome, encephalomyelitis AMPAR Neuronal Surface Breast, lung, thymus Older adults, female predominance Psychiatric symptoms GAD 65 Neuronal Surface rare Adults Limbic encephalopathy, stiff person syndrome, Miller Fisher syndrome; limited response to immunotherapy NMDAR Neuronal Surface Ovary, mediastinal teratoma Children and young adults, 80% female predominance Psychiatric symptoms, seizures, movement disorders, autonomic instability LGI 1 (VGKC) Neuronal Surface Thymus, lung Adults Seizures GABAAR Neuronal Surface rare 39% in children Seizures, stiff person syndrome opsoclonus myoclonus syndrome GABABR Neuronal Surface SCLC Older Adults Limbic encephalopathy, seizures and psychiatric symptoms DPPX Neuronal Surface rare Adults Diffuse encephalitis, prodromal diarrhea, psychiatric symptoms, tremor/ataxia
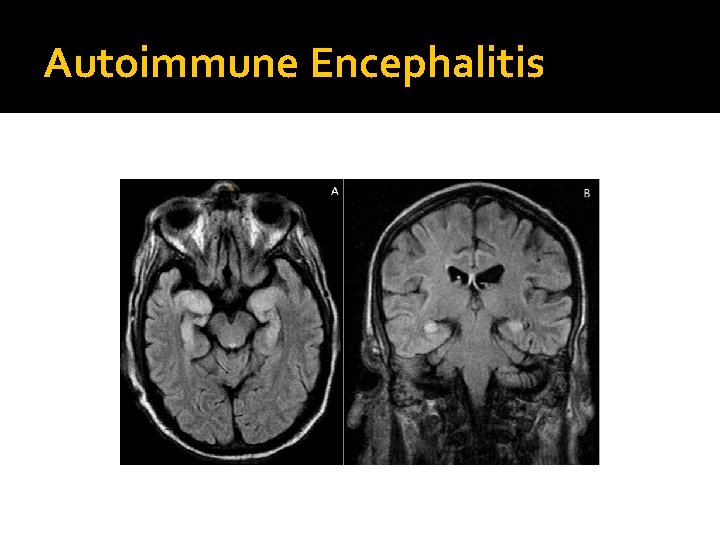
Autoimmune Encephalitis

Initial Management and Assessment ABCs Consider the following lab studies: Serum glucose and electrolytes Complete blood count, lactate, procalcitonin Liver and kidney function studies Urine toxicology screen Arterial blood gas Carboxyhemoglobin level (if carbon monoxide exposure suspected) For coma of acute onset and unknown cause administer: Dextrose, 25 g IV (to treat possible hypoglycemia) Thiamine, 100 mg IV (to prevent or treat Wernicke encephalopathy) Naloxone, 1 mg IV (to treat possible opiate overdose) Treat ongoing seizures Brain imaging (CT or MRI) if focal intracranial lesion is suspected CSF analysis if meningitis or SAH is suspected
- Slides: 15