Hypothyroidism Hasan AYDIN MD Yeditepe University Medical Faculty

















































- Slides: 62

Hypothyroidism Hasan AYDIN, MD Yeditepe University Medical Faculty Endocrinology and Metabolism

Definition A deficiency of thyroid hormones, which in turn results in a generalized slowing down of metabolic processes.

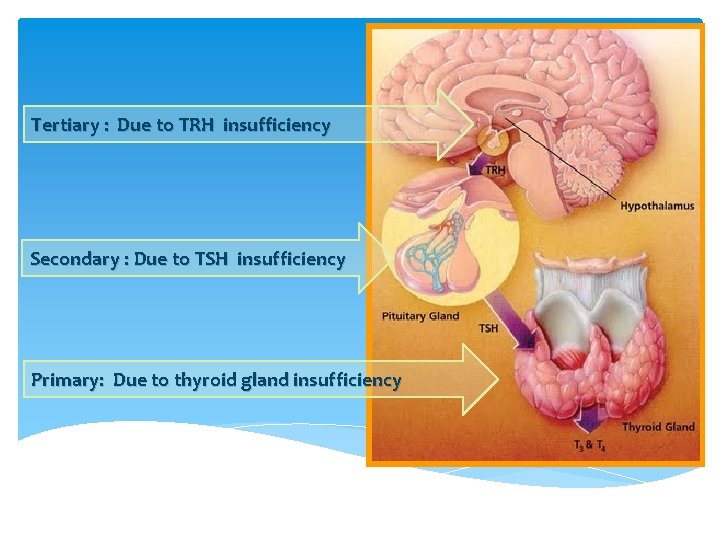
Tertiary : Due to TRH insufficiency Secondary : Due to TSH insufficiency Primary: Due to thyroid gland insufficiency

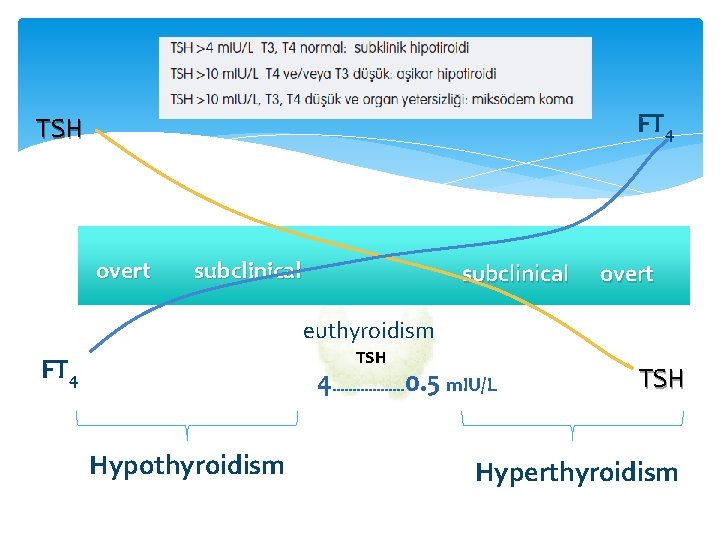
Hypothyroidism Diagnosis depend on laboratory Symptoms nonspecific s. TSH and Serbest T 4

FT 4 TSH overt subclinical overt euthyroidism TSH FT 4 4. . . . 0. 5 m. IU/L Hypothyroidism TSH Hyperthyroidism

TSH Normal Values Lower limit same for all ages 0. 5 m. IU/L Upper limit changes with age 4 m. IU/L 6 m. IU/L 7. 5 m. IU/L 2. 5 m. IU/L 3. 0 m. IU/L Healthy adult Age 70 -79 Age >80 pregnancy 1. trimester 2. -3. trimester

Hypothyroidism Epidemiology Most common endocrine disease Females > Males – 8 : 1 Presentation Often unsuspected and grossly under diagnosed 90 % of the cases are Primary Hypothyroidism Menstrual irregularities, miscarriages, growth retard. Vague pains, anaemia, lethargy, gain in weight In clear cut cases - typical signs and symptoms

Disease Burden Overt hypothyroidism prevalance 0. 1 -2% Subclinical hypothyroidism prevalance 4 - 8. 5% > 60 y women %14 -20

Etiology

Causes of Hypothyroidism Primary Congenital Acquired Transient Secondary Pituitary Hypothalamic

Congenital Hypothyroidism Athyreosis Dyshormonogenesis Sodium/iodide symporter mutations TPO mutations Thyroglobulin gene mutations Deiodinase defects Thyroid hormone resistance TSH-receptor defect

Acquired Hypothyroidism Iodine deficiency Autoimmune thyroid disease Hashimoto’s , Graves disease Iatrogenic Post-thyroidectomy Radioactive iodine treatment Thyroid irradiation Medications/goitrogens

Hashimoto’s Disease Struma lymphomatosa : firm, enlarged thyroid Antibodies to thyroid antigens (TPO, Thyroglobulin, TSH receptor, T 4, T 3) Cellular abnormalities (increased CD 8+ T cells, aberrant HLA-DR expression, increased NK/K cells and cytokines) Slowly progressive disease (10 % hypothyroid) Associated with other autoimmune disease

Transient Hypothyroidism Subacute thyroiditis (de Quervain’s) Silent thyroiditis Post-partum thyroiditis (Hashimoto’s) Transient neonatal hypothyroidism

Secondary Hypothyroidism Pituitary Hypothalamic Tumor Infectious disease Infiltrating disease Vascular insufficiency TRH deficiency Empty sella syndrome Iatrogenic

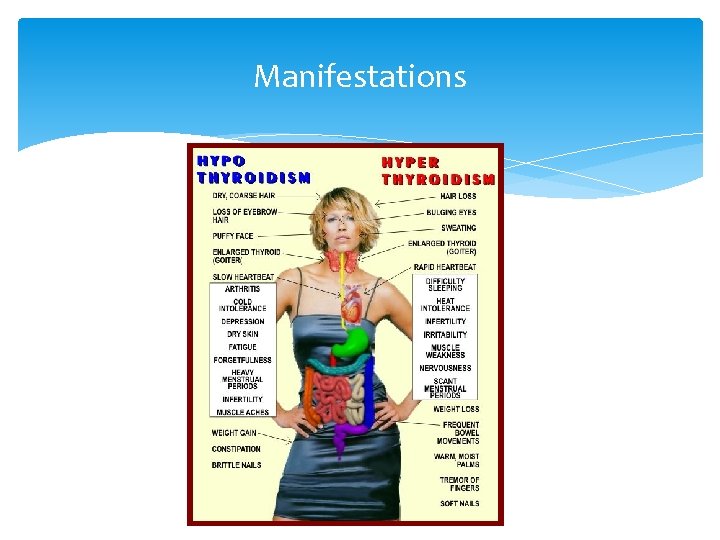
Manifestations

Manifestations

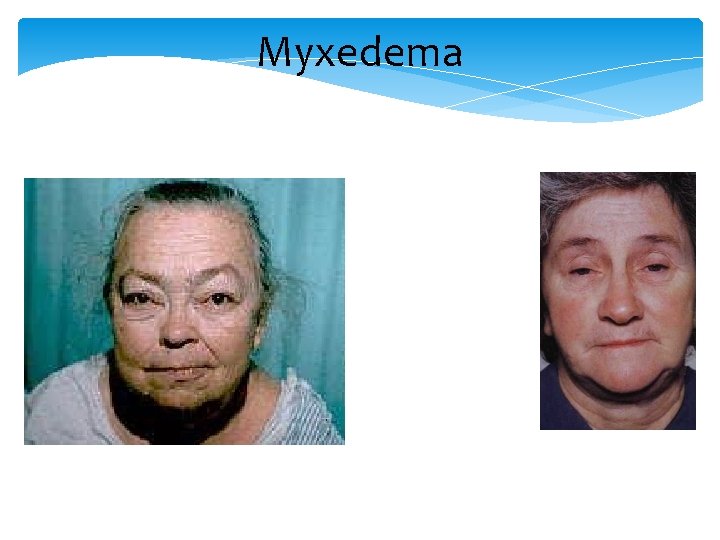
Skin and Appendages Myxedema (hyaluronic acid accumulation) Pale, cool and dry skin, hypercarotenemia Tongue is enlarged Thickened laryngeal/pharyngeal mucous membranes Slow wound healing, bruising Dry, brittle hair Temporal loss of eyebrows Brittle nails

Cardiovascular System Decreased cardiac output (stroke volume + heart rate) Increased peripheral vascular resistance Narrow pulse pressure Pericardial effusion, dilated myocardium Coronary atherosclerosis (HT, HL) ECG changes (bradycardia, low amplitude QRS, prolonged PR, ST alterations)

Respiratory System Pleural effusions Decreased ventilatory drive (hypercapnia, hypoxemia) Involvement of respiratory muscles Obstructive sleep apnea

Gastrointestinal Delayed peristalsis, distension, constipation Ascitis (rare) Achlorhydria and pernicious anemia Reduced appetite

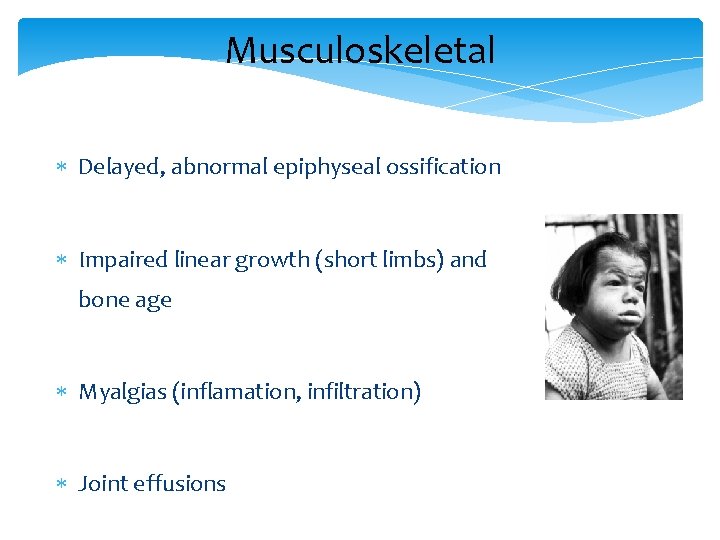
Musculoskeletal Delayed, abnormal epiphyseal ossification Impaired linear growth (short limbs) and bone age Myalgias (inflamation, infiltration) Joint effusions

Neuropsychiatric Decreased cerebral perfusion, myelination, and cortical developmentretardation Slow speech, lack of concentration and memory, depression, paranoia Delay in the relaxation phase of DTR Delayed nerve conduction, carpal tunnel syndrome Perceptive hearing loss (Pendred Synd. )

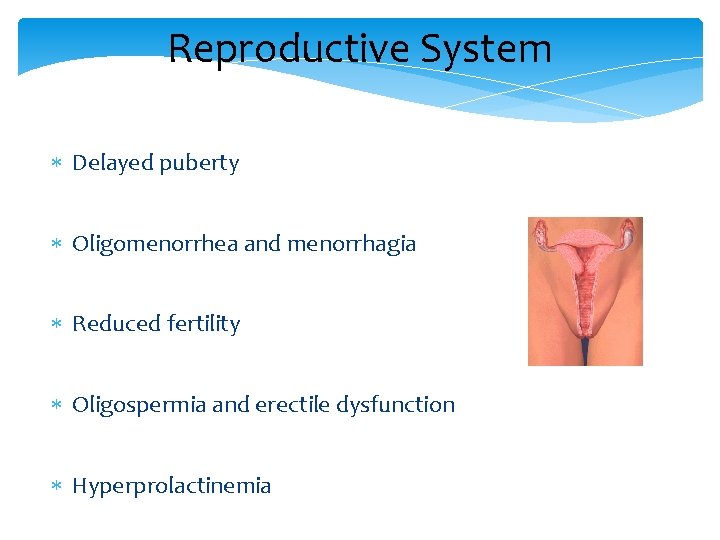
Reproductive System Delayed puberty Oligomenorrhea and menorrhagia Reduced fertility Oligospermia and erectile dysfunction Hyperprolactinemia

Other Decreased erythropoetin (anemia) Decreased Factor 8 and 9 Low basal metabolic rate Increased cholesterol, TG, LDL and decreased HDL

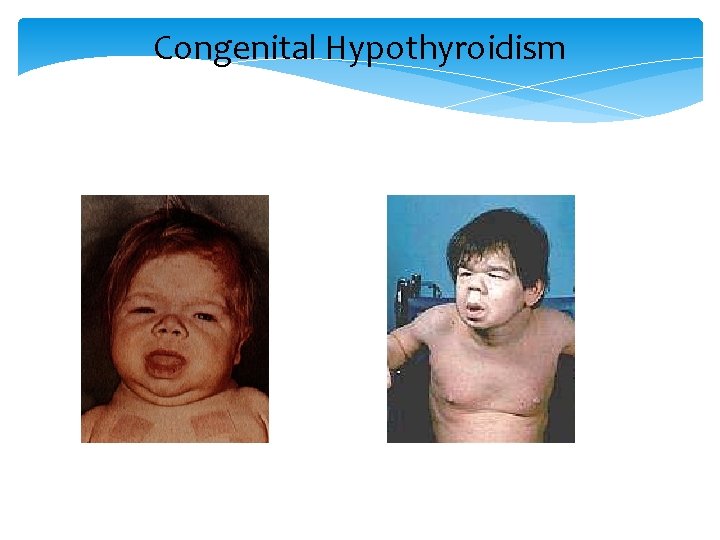
Infantile Hypothyroidism (Cretinism) Retardation of mental development and growth Protuberant abdomen, umblical hernia, dry skin, poor hair and nail growth, delayed teeth eruption, waddling gait Epiphysial dysgenesis

Congenital Hypothyroidism

Myxedema Coma Severe myxedema, bradycardia, hypotension, subnormal temperature, seizures Alveolar hypoventilation, dilutional hyponatremia are common Exposure to cold, infection, trauma, central nervous system depressants trigger coma

Myxedema

Myxedema

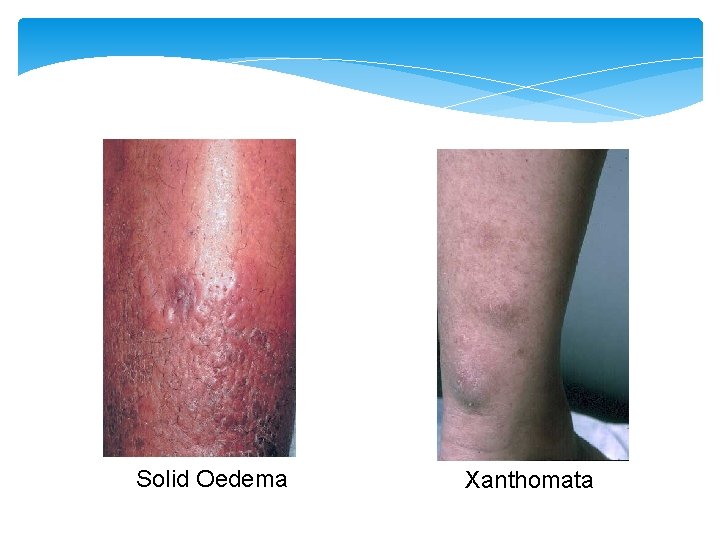
Solid Oedema Xanthomata

Diagnosis

Laboratory Tests TSH T 3 and T 4 Thyroid antibodies RAIU Serum lipids CK, SGOT, LDH Hemogram

Diagnosis of Primary hypothyroidism Overt hypothyroidism TSH >4. 0 m. IU/L, s T 4 low Subclinical hypothyroidism TSH >4. 0 m. IU/L, s T 4 Normal Euthyroid TSH 0. 5 -4. 0 m. IU/L, s. T 4 Normal 0 4 10. . . . TSH, m. IU/L

Diagnosis of Secondary or Tertiary Hypothyroidism • TSH low or normal • s. T 4 low

Differential Diagnosis Elderly patients Chronic renal failure Nephrotic states Pernicious anemia Euthyroid Sick Syndrome Down Syndrome

Screening for Hypothyroidism High risk population: • • • Women age > 60 Family history Personal history of thyroid diseases Symptoms or signs atributed to hypothyroidism Presence of goiter Hyperlipidemia Tip 1 diabetes mellitus Hyperprolactinemia CPK elevation Otoimmün disase history Consensus group : ATA, AACE, & ES

Co-morbidity Hypercholesterolemia Depression Infertility – Menstrual Irregularities Diabetes mellitus

Hypothyroidism and Hypercholesterolemia 14% of patients with elevated cholesterol have hypothyroidism Approximately 90% of patients with overt hypothyroidism have increased cholesterol and / or triglycerides

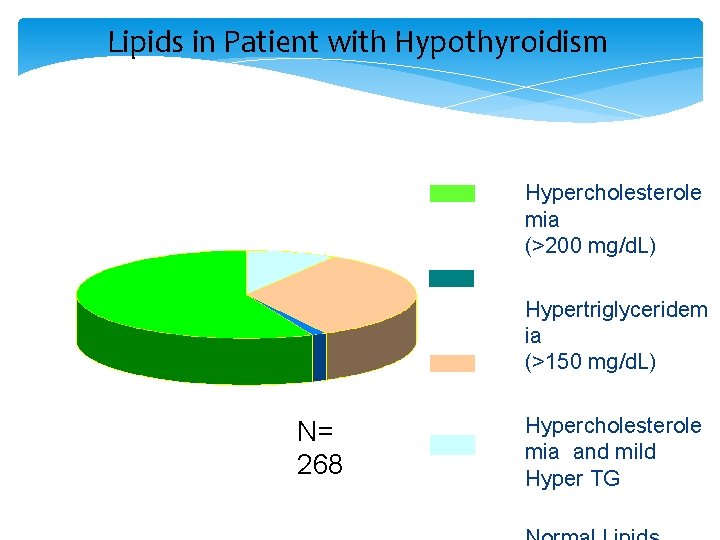
Lipids in Patient with Hypothyroidism Hypercholesterole mia (>200 mg/d. L) Hypertriglyceridem ia (>150 mg/d. L) N= 268 Hypercholesterole mia and mild Hyper TG

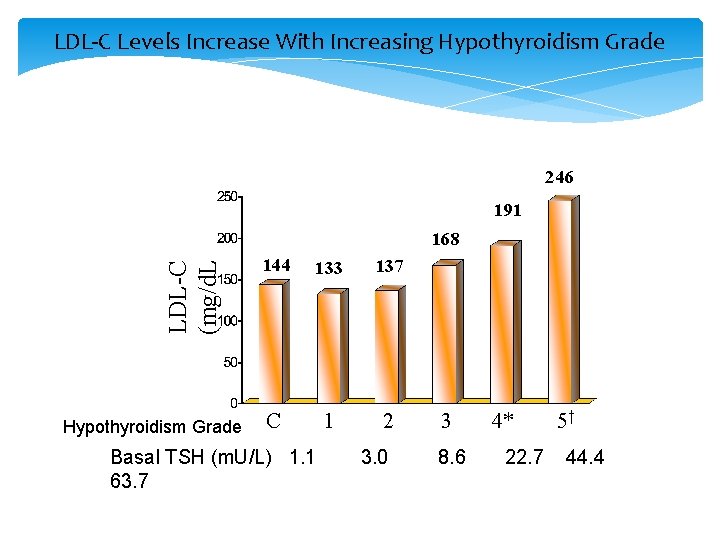
LDL-C Levels Increase With Increasing Hypothyroidism Grade 246 191 LDL-C (mg/d. L 168 Hypothyroidism Grade 144 133 137 C 1 2 Basal TSH (m. U/L) 1. 1 63. 7 3. 0 3 8. 6 4* 22. 7 5† 44. 4

Hypothyroidism and Depression Depressive symptoms are common in hypothyroidism Many hypothyroid patients fulfill DSM-IV criteria for a depressive disorder Depressed patients may be more likely than normal individuals to be hypothyroid All depressed patients should be evaluated for thyroid dysfunction

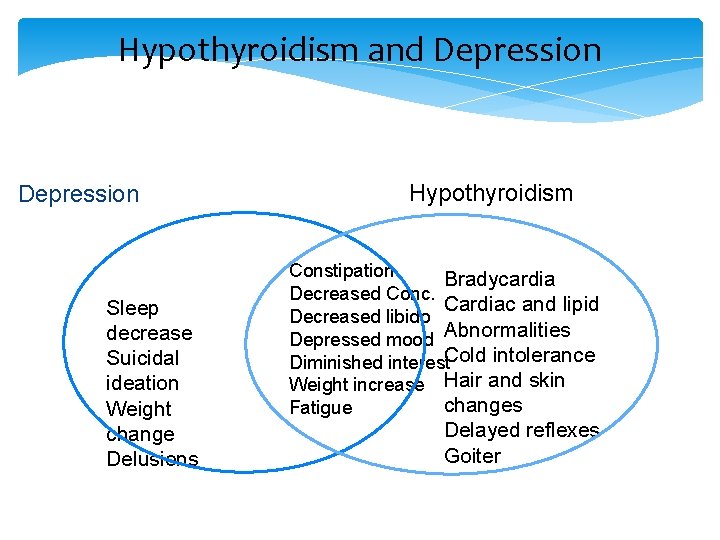
Hypothyroidism and Depression Sleep decrease Suicidal ideation Weight change Delusions Hypothyroidism Constipation Bradycardia Decreased Conc. Cardiac and lipid Decreased libido Depressed mood Abnormalities Diminished interest. Cold intolerance Weight increase Hair and skin changes Fatigue Delayed reflexes Goiter

Hypothyroidism and Infertility 1. Hypothyroidism associated with infertility, miscarriage, stillbirth 2. Infertility : Evaluate thyroid function, treat hypothyroidism 3. Equivocal results: Begin therapy; discontinue if no pregnancy for several months.

Hypothyroidism and Diabetes 1. Approximately 10% of patients with type 1 diabetes mellitus develop sub-clinical hypothyroidism 2. In diabetic patients - examine for goitre 3. TSH measurement at regular intervals

Hormone Replacement

Who should be treated? TSH > 10 m. IU/L TSH >4 m. IU/L, T 4 ↓ TSH 4 - 10 m. IU/L and T 4 normal but Symptomatic Thyroid otoantibody pozitivity (Anti TPo, Anti TG) Pregnant women 1 st trimesterde TSH > 2. 5 m. IU/L 2 nd or 3 rd trimester TSH > 3 m. IU/L

Many Causes, One Treatment Goal : Normalize TSH level regardless of cause of hypothyroidism Treatment : Once daily dosing with Levothyroxine sodium (1. 6 µg/kg/day) Monitor TSH levels at 6 to 8 weeks, after initiation of therapy or dosage change

Many Causes, One Treatment of choice is levothyroxin Branded thyroxine recommended Brand consistency recommended No divided doses - illogical Not recommended for use : l Desiccated thyroid extract l Combination of thyroid hormones l T 3 replacement except in Myxedema coma

Dosage Adjustments Age (in elderly start with half dose) Severity and duration of hypothyroidism (↑ dose) Weight (0. 5µg/kg/day ↑ upto 3. 0µg/kg/day) Malabsorption (requires ↑ dose) Concomitant drug therapy (only on empty stomach) Pregnancy ( 25% ↑ in dose), safe in lactating mother Presence of cardiac disease (start alt. day Rx)

Start Low and Go Slow Starting dose for healthy patients < 50 years at 1. 6 µg/kg/day Starting dose for healthy patients > 50 years should be < 0, 50 µg/day. Dose ↑ by 25 µg, if needed, at 6 to 8 weeks intervals. Starting dose for patients with heart disease should be 12. 5 to 25 µg/day and increase by 12. 5 to 25 µg/day, if needed, at 6 to 8 weeks intervals

How the Patient Improves l Feels better in 2 – 3 weeks l Reduction in weight is the first improvement l Facial puffiness then starts coming down l Skin changes, hair changes take long time to regress l TSH starts showing decrements from the high values l TSH returns to normal eventually

Drug Interactions Reduced Absorption Drugs that affect metabolism l Cholestyramine resin l Rifampin l Sucralfate l Carbamazepine l Phenytoin l Phenobarbitol l Amiodarone l Ferrous sulfate l Soybean formula l Aluminum hydroxide l Colestipol hydrochloride

Inappropriate Dosage Over-replacement risks Reduced bone density / osteoporosis Tachycardia, arrhythmia. atrial fibrillation In elderly or patients with heart disease, angina, arrhythmia, or myocardial infarction Under-replacement risks Continued hypothyroid state Long-term end-organ effects of hypothyroidism Increased risk of hyperlipidemia

Special Situations

Sub-clinical Hypothyroidism Chronic autoimmune thyroiditis Graves’ hyperthyroidism with radioiodine, surgery Inadequate replacement therapy for hypothyroidism Lithium carbonate therapy (for depressive illness)

Subclinical Hypothyroidism High TSH with normal Free T 4 Commonest cause is chronic autoimmune thyroiditis (Hashimoto’s disease) Associated with increased titer of antithyroid antibodies: - Anti thyroglobulin autobodies - Antimicrosomal (Antiperoxidase) antibodies Suspected with thyroid enlargement but may be associated with atrophy

Prognosis May stay sub clinical May progress to clinical 5% per year with positive antibodies In elderly risk is 20%/ year

Post-Partum Thyroiditis Definition Occurrence of hyperthyroidism and / or hypothyroidism during the postpartum period in women who were euthryroid during pregnancy At Highest Risk Patients with type 1 diabetes, previous history of PPT or other autoimmune disease such as Hashimoto’s disease and Graves’ disease

Sick Euthyroid Syndrome l Total T 3 reduced l FT 3 reduced l Total T 4 reduced l FT 4 Normal l TSH Normal l Clinically Euthyroid

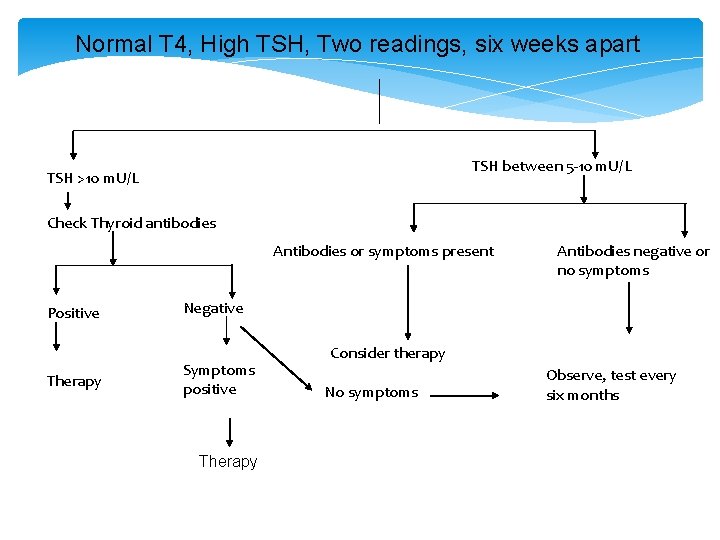
Normal T 4, High TSH, Two readings, six weeks apart TSH between 5 -10 m. U/L TSH >10 m. U/L Check Thyroid antibodies Antibodies or symptoms present Positive Therapy Antibodies negative or no symptoms Negative Symptoms positive Therapy Consider therapy No symptoms Observe, test every six months

Thank You