Hypothetical Relationship Between Early Reperfusion Mortality Reduction and
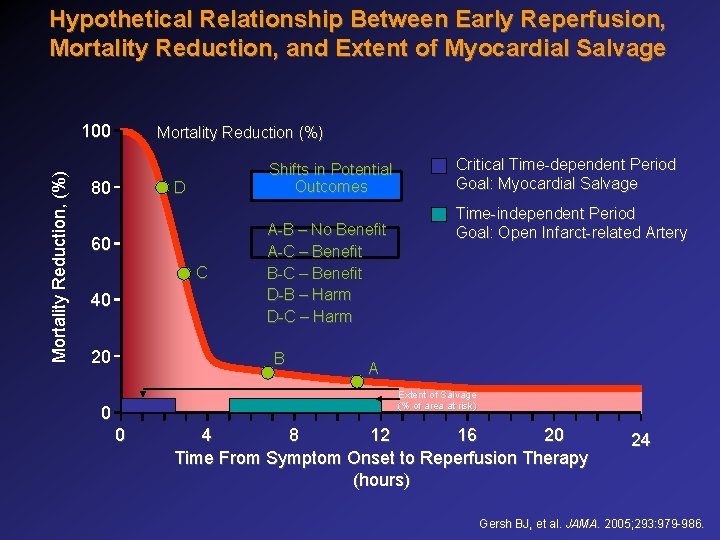
Hypothetical Relationship Between Early Reperfusion, Mortality Reduction, and Extent of Myocardial Salvage Mortality Reduction, (%) 100 Mortality Reduction (%) 80 Shifts in Potential Outcomes D 60 C 40 20 A-B – No Benefit A-C – Benefit B-C – Benefit D-B – Harm D-C – Harm B Critical Time-dependent Period Goal: Myocardial Salvage Time-independent Period Goal: Open Infarct-related Artery A Extent of Salvage (% of area at risk) 0 0 4 8 12 16 20 Time From Symptom Onset to Reperfusion Therapy (hours) 24 Gersh BJ, et al. JAMA. 2005; 293: 979 -986.

The 1 S and the 4 Ds: Symptoms Door Data Decision Drug or Device
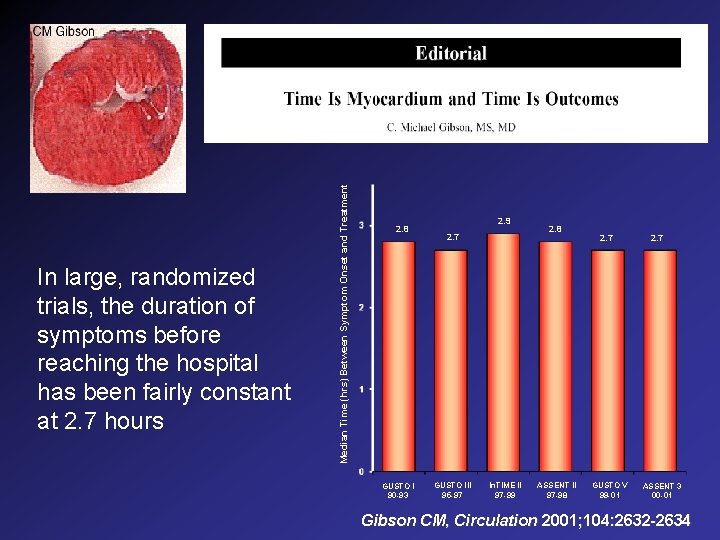
Median Time (hrs) Between Symptom Onset and Treatment In large, randomized trials, the duration of symptoms before reaching the hospital has been fairly constant at 2. 7 hours 2. 8 GUSTO I 90 -93 2. 9 2. 7 GUSTO III 95 -97 In. TIME II 97 -99 2. 8 ASSENT II 97 -98 2. 7 GUSTO V 99 -01 2. 7 ASSENT 3 00 -01 Gibson CM, Circulation 2001; 104: 2632 -2634

15 Years of National Registry of Myocardial Infarction 30 Minute Reduction in Door to Needle Time Reduces Mortality by 1% Gibson CM, AHJ 2008
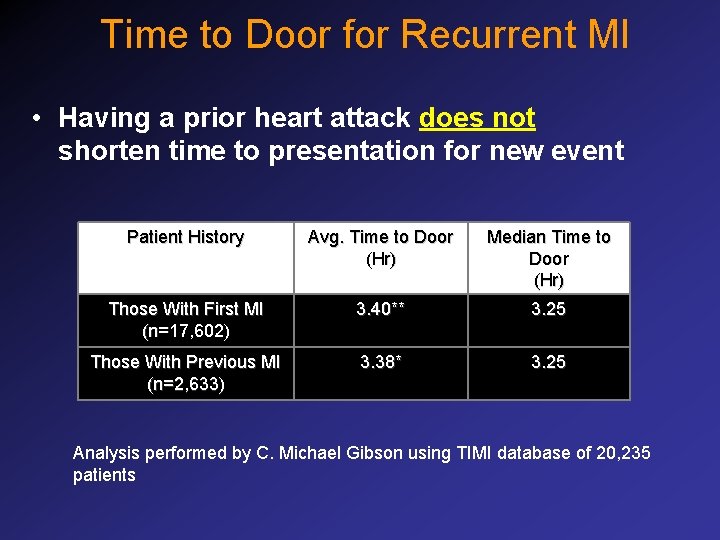

Time to Door for Recurrent MI • Having a prior heart attack does not shorten time to presentation for new event Patient History Avg. Time to Door (Hr) Median Time to Door (Hr) Those With First MI (n=17, 602) 3. 40** 3. 25 Those With Previous MI (n=2, 633) 3. 38* 3. 25 Analysis performed by C. Michael Gibson using TIMI database of 20, 235 patients

Atypical Pain or No Pain is Frequent Among Patients with MI n ~30% of AMIs are silent or without typical chest symptoms 1, 2 n There is a 7. 5% relative increase in mortality for every 30 minutes of delay 3 1. Kannel WB. "Silent myocardial ischemia and infarction: insights from the Framingham Study". Cardiol Clin 1986; 4 (4): 583– 91. 2. Davis TM, Fortun P, Mulder J, Davis WA, Bruce DG. "Silent myocardial infarction and its prognosis in a community-based cohort of Type 2 diabetic patients: the Fremantle Diabetes Study". Diabetologia 2004; 47 (3): 395– 9. 3. De Luca G, Suryapranata H, Ottervanger JP, Antman EM. Time delay to treatment and mortality in primary angioplasty for acute myocardial infarction: every minute of delay counts. Circulation 2004; 109(10): 1223 -5. Epub 2004 Mar 8.
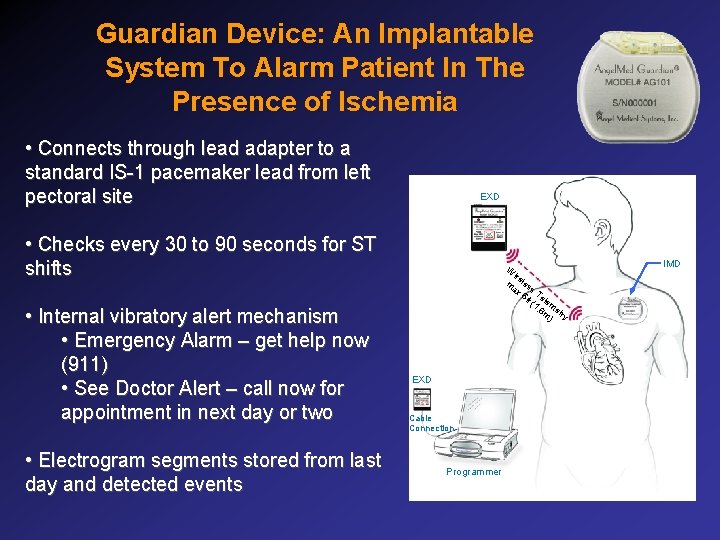
Guardian Device: An Implantable System To Alarm Patient In The Presence of Ischemia • Connects through lead adapter to a standard IS-1 pacemaker lead from left pectoral site EXD • Checks every 30 to 90 seconds for ST shifts • Internal vibratory alert mechanism • Emergency Alarm – get help now (911) • See Doctor Alert – call now for appointment in next day or two • Electrogram segments stored from last day and detected events W ire m les ax s 6 f Te t ( lem 1. 8 m etr ) y EXD Cable Connection Programmer IMD
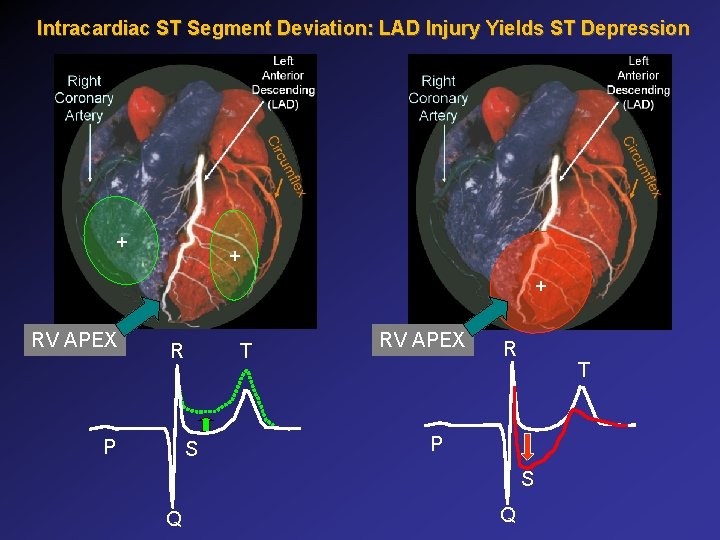
Intracardiac ST Segment Deviation: LAD Injury Yields ST Depression + + + RV APEX R P T S RV APEX R T P S Q Q
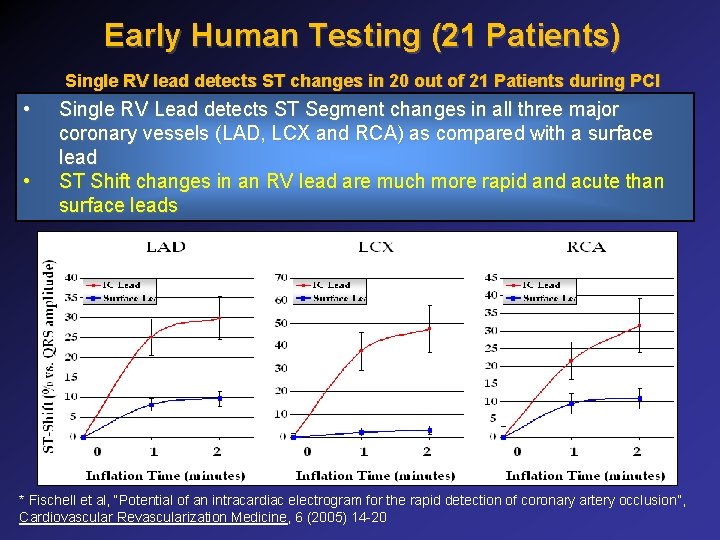
Early Human Testing (21 Patients) Single RV lead detects ST changes in 20 out of 21 Patients during PCI • • Single RV Lead detects ST Segment changes in all three major coronary vessels (LAD, LCX and RCA) as compared with a surface lead ST Shift changes in an RV lead are much more rapid and acute than surface leads * Fischell et al, “Potential of an intracardiac electrogram for the rapid detection of coronary artery occlusion”, Cardiovascular Revascularization Medicine, 6 (2005) 14 -20
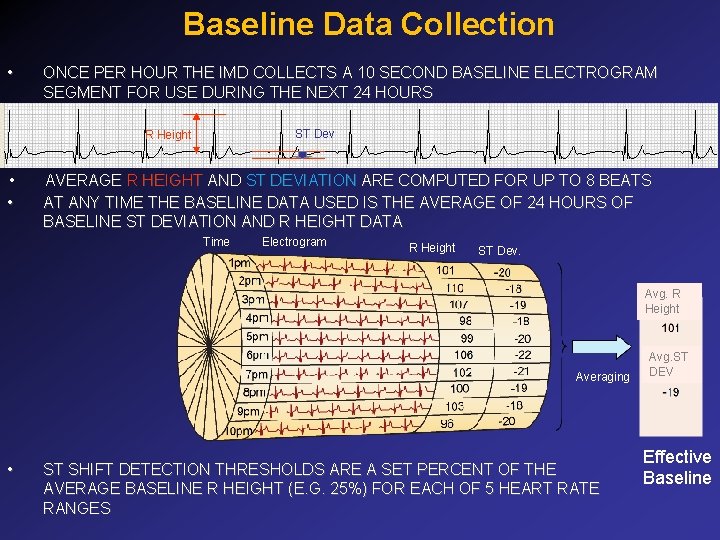
Baseline Data Collection • ONCE PER HOUR THE IMD COLLECTS A 10 SECOND BASELINE ELECTROGRAM SEGMENT FOR USE DURING THE NEXT 24 HOURS ST Dev R Height • • AVERAGE R HEIGHT AND ST DEVIATION ARE COMPUTED FOR UP TO 8 BEATS AT ANY TIME THE BASELINE DATA USED IS THE AVERAGE OF 24 HOURS OF BASELINE ST DEVIATION AND R HEIGHT DATA Time Electrogram R Height ST Dev. Avg. R Height Averaging • ST SHIFT DETECTION THRESHOLDS ARE A SET PERCENT OF THE AVERAGE BASELINE R HEIGHT (E. G. 25%) FOR EACH OF 5 HEART RATE RANGES Avg. ST DEV Effective Baseline
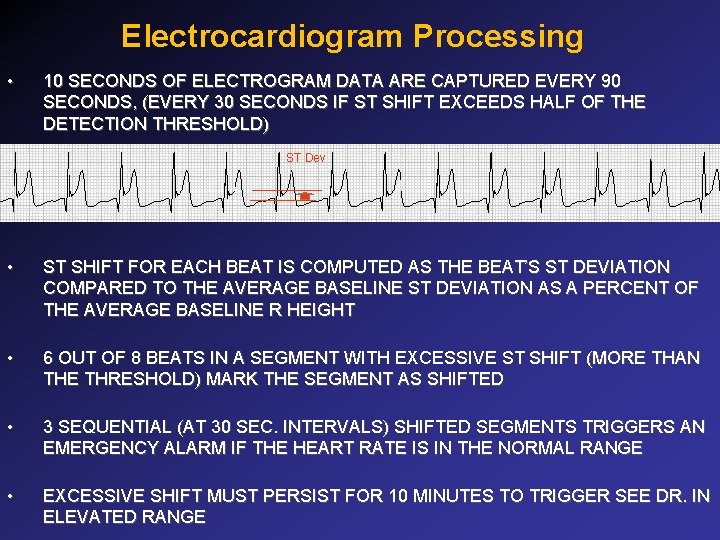
Electrocardiogram Processing • 10 SECONDS OF ELECTROGRAM DATA ARE CAPTURED EVERY 90 SECONDS, (EVERY 30 SECONDS IF ST SHIFT EXCEEDS HALF OF THE DETECTION THRESHOLD) ST Dev • ST SHIFT FOR EACH BEAT IS COMPUTED AS THE BEAT’S ST DEVIATION COMPARED TO THE AVERAGE BASELINE ST DEVIATION AS A PERCENT OF THE AVERAGE BASELINE R HEIGHT • 6 OUT OF 8 BEATS IN A SEGMENT WITH EXCESSIVE ST SHIFT (MORE THAN THE THRESHOLD) MARK THE SEGMENT AS SHIFTED • 3 SEQUENTIAL (AT 30 SEC. INTERVALS) SHIFTED SEGMENTS TRIGGERS AN EMERGENCY ALARM IF THE HEART RATE IS IN THE NORMAL RANGE • EXCESSIVE SHIFT MUST PERSIST FOR 10 MINUTES TO TRIGGER SEE DR. IN ELEVATED RANGE
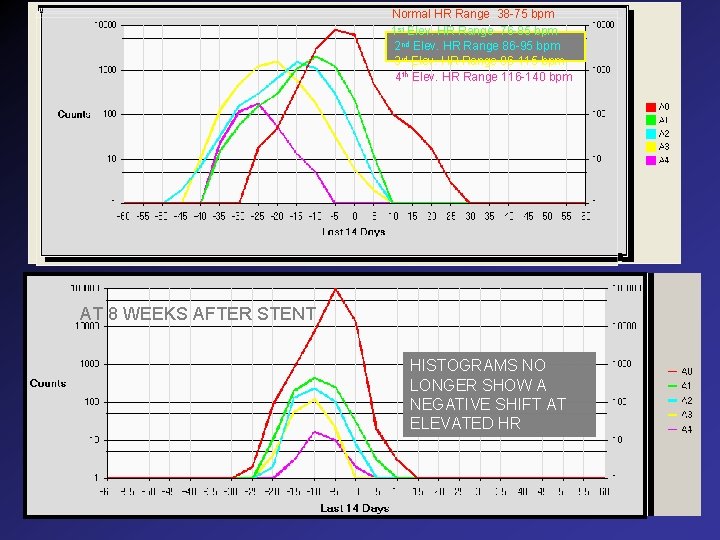
Normal HR Range 38 -75 bpm 1 st Elev. HR Range 76 -85 bpm 2 nd Elev. HR Range 86 -95 bpm 3 rd Elev. HR Range 96 -115 bpm 4 th Elev. HR Range 116 -140 bpm Week Before LCX Stent – HR Related ST Depression Histograms AT 8 WEEKSAFTERLCX STENT MORNING STENT HISTOGRAMS NO LONGER SHOW A NEGATIVE SHIFT AT ELEVATED HR
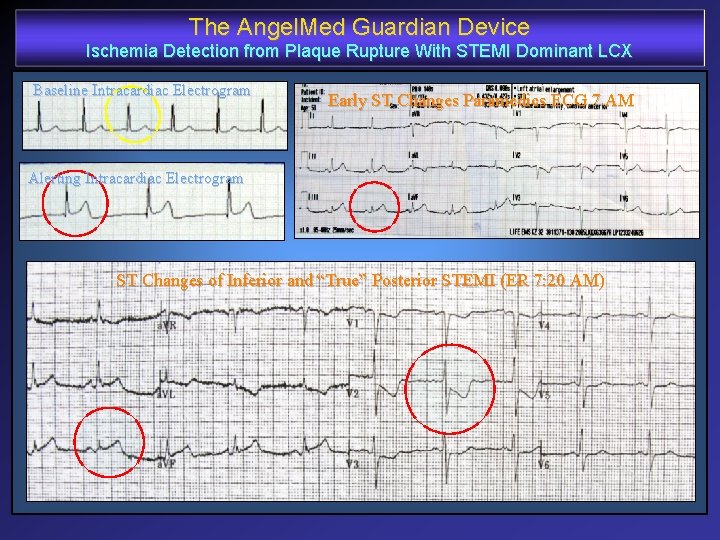
The Angel. Med Guardian Device Ischemia Detection from Plaque Rupture With STEMI Dominant LCX Baseline Intracardiac Electrogram Early ST Changes Paramedics ECG 7 AM Alerting Intracardiac Electrogram ST Changes of Inferior and “True” Posterior STEMI (ER 7: 20 AM)
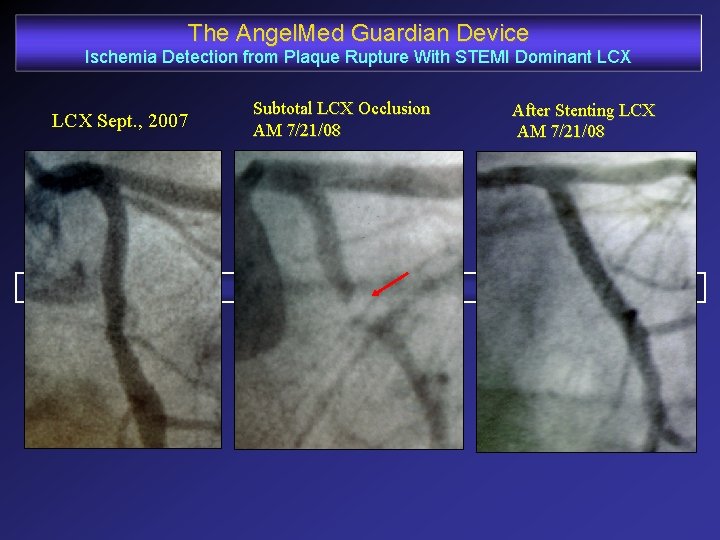
The Angel. Med Guardian Device Ischemia Detection from Plaque Rupture With STEMI Dominant LCX Sept. , 2007 Subtotal LCX Occlusion AM 7/21/08 After Stenting LCX AM 7/21/08

Patient 03 Ruptured Plaque Event Patient put on Heparin, Aspirin & Clopidigrel Second event clears due to Drugs
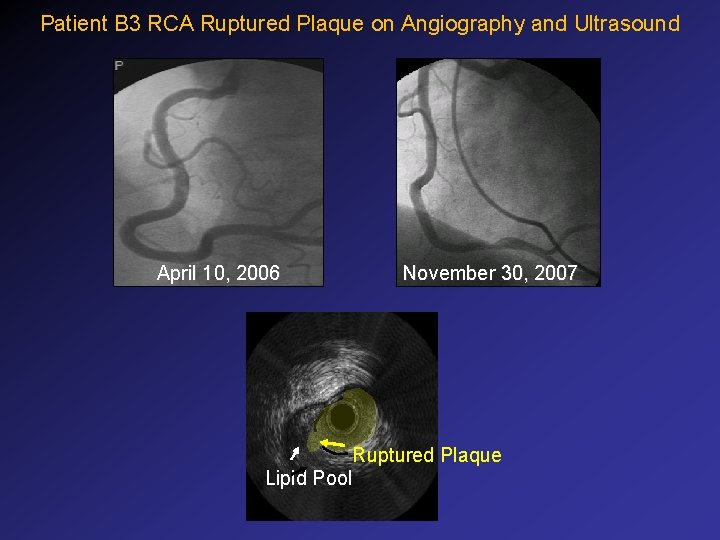
Patient B 3 RCA Ruptured Plaque on Angiography and Ultrasound April 10, 2006 November 30, 2007 Ruptured Plaque Lipid Pool

Completed Studies • DETECT: US Feasibility study completed 5/08, 2 plaque ruptures detected • Cardio. Saver: Brazilin study completed in Oct. 2007, 2 plaque ruptures detected and no STEMI false positives/negatives with current algorithm. Median symptom to door time only 19. 5 minutes in these two studies.

ALERT AMI PI: CM Gibson Co-PI: D Holmes 3, 000 acute coronary syndrome patients with either: Diabetes (Type I or Type II), compromised renal function (Cr > 1. 2 mg/dl or creatinine clearance less than 50), or TIMI Risk Score > 3 Implant At 14 days ETT performed to max heart rate to train device re anticipated ST deviation at different heart rate bins 7 -14 Day Follow-Up Alerts turned ON Randomization at 7 -14 Day visit 7 -14 Day Follow-Up Alerts turned OFF 1 Month Follow-Up Alerts remain ON 1 Month Follow-Up Alerts remain OFF 3 Month Follow-Up Alerts remain ON 3 Month Follow-Up Alerts remain OFF 6 Month Follow-Up Alerts remain ON 6 Month Follow-Up Alerts turned ON Primary Endpoint: Cardiac or unexplained death, new Q-wave MI, time to door > 2 hours for a thrombotic coronary occlusion event

Conclusions • Time is muscle • Greatest improvements in salvage are when improvements in delivery of care made during the earliest phase of symptoms • Improvements in door to data, and decision to drug/device times have improved outcomes • Symptom to door and data to decision times are two targets for further improvements in the timely delivery of STEMI care
- Slides: 19