HYPOTHERMIA THERMOREGULATION Hypothermia Learning Outcomes 1 Describe the

HYPOTHERMIA THERMOREGULATION

Hypothermia Learning Outcomes 1. Describe the pathophysiology, etiology, clinical manifestations, and direct and indirect causes of hypothermia. 2. Identify risk factors associated with hypothermia. 3. Apply the nursing process in providing culturally competent care across the life span for individuals with hypothermia. 4. Discuss therapies used in the collaborative care of an individual with hypothermia. 5. Identify and employ evidence-based interventions for an individual with hypothermia.

Question One The nurse is assessing a three week old infant, and recognizes which finding as an early sign of hypothermia? 1. The infant is shivering. 2. Rectal temperature is 33° celsius. 3. Skin is cool to touch and pale. 4. Rapid and slightly labored respirations.

Question 2 What is a priority nursing intervention for a nurse caring for a premature infant born at 32 weeks gestation? 1. Provide a neutral thermal environment. 2. Promote bonding between infant and parents. 3. Teach parents regarding newborn care. 4. Administer immunizations to the newborn.

Question 3 While obtaining the admission history for an 80 -year-old client admitted to the medical unit, the nurse learns that the client keeps thermostat in the home at 64° in order to cut the cost of the monthly heating bill. What should the nurse include in the teaching plan for this client? 1. Importance of always keeping thermostat set on 74°F. 2. Referral to social services for assistance with resources. 3. Assessment for hypothermia. 4. Strategies to reduce the risk of hypothermia

Question 4 The nurse is teaching a client who will be undergoing heart open surgery about what to expect when waking up from anesthesia. The nurse explains the client will experience feeling cold, which is induced during surgery. The client asks the nurse why they induce cold. What is the best response by the nurse? 1. “Inducing a cold environment will make the surgery go faster. ” 2. “It will decrease the amount of bleeding during surgery. ” 3. “It will reduce the demand for tissue oxygenation. ” 4. “It will decrease symptoms related to anesthesia. ”

Hypothermia Overview Key Points Condition in which the core body temperature falls below 36° C Occurs when the heat the body produces is less than the heat lost Can be a life-threatening emergency, and can occur in any season and any geographic location

Hypothermia Pathophysiology and Etiology ¤ Induced Hypothermia − Deliberately lowering body temperature, reducing body’s need for oxygen ¤ Accidental − Result of immersion in cold water, exposure ¤ As body’s core temperature falls − Body tries to conserve core temperature at the expense of extremities

Hypothermia Pathophysiology and Etiology Routes of Heat Loss − Internal core to body surface − External surface to environment Core Temperature – usually higher than skin − Continuous transfer, conduction of heat − Greater the difference in temperature the more rapidly heat transfers − Transfer through increased O 2 consumption − Depletion of glycogen stores, brown fat

Hypothermia Pathophysiology and Etiology Induced Hypothermia − Reduced metabolic rates − Lower cellular demand for O 2 in tissues − Used to reduce neurological damage − Sequelae from post-cardiac arrest, lessen anoxia − Initiated with iced saline gastric lavage Goal client temperature of 33° Stop all potassium administration during rewarming Sedation, paralytic medications

Hypothermia Pathophysiology and Etiology Accidental Hypothermia − Exposure to cold environment − Immersion in cold water − Lack of adequate clothing, shelter, heat − Associated with near drowning − Other causes: Ingestion of alcohol, drugs, trauma Overwhelming sepsis

NEWBORN Large body surface area in relation to mass Limited insulating subcutaneous fat Loses 4 times more heat than adult Poor thermal stability Radiation and convection losses Thermal conduction − Marked difference between core and skin temperature − Cool environment peripheral vasodilation

NEWBORN, continued Thermogenisis − Increased metabolic rate − Muscular activity − Nonshivering thermogenisis (NST) Skin receptors Brown adipose tissue (BAT) – brown fat − NST from BAT primary source of heat Shivering – rare in newborn

NEWBORN, continued The distribution of brown adipose tissue (brown fat) in the newborn

NEWBORN, continued BAT depleted metabolic response limited Keeping newborn warm − Promotes normal oxygen requirements − Chilling can cause respiratory distress signs and symptoms − Preterm infant may be unable to increase ventilation − Need extra protection from mild variations

Body Temperature Stability Newborn < children < adolescents, adults Elderly − More sensitive than middle-age adults − Decreased thermoregulatory control − Loss of subcutaneous fat − Environmental factors − Illness − CNS disorder

FROSTBITE Injury of skin resulting from freezing − If limited exposure skin, subcutaneous tissue involvement − Increased exposure deeper structures freeze − Skin freezes when temperature drops to 21°C-24°C − Occurs most commonly on exposed and peripheral areas
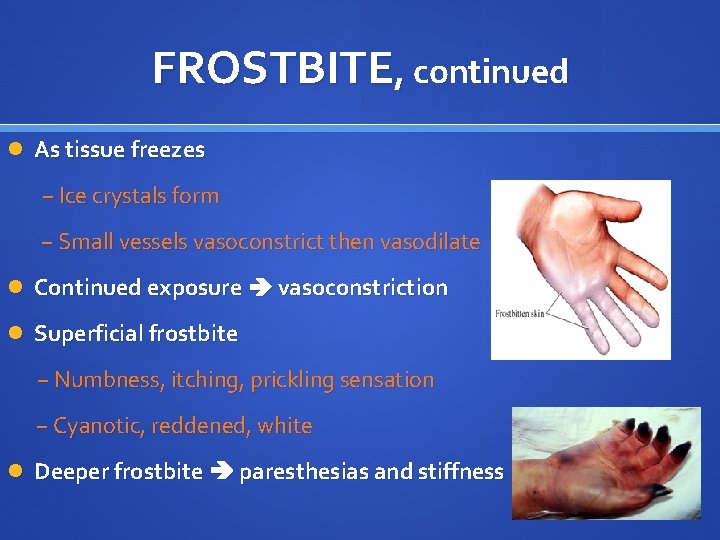
FROSTBITE, continued As tissue freezes − Ice crystals form − Small vessels vasoconstrict then vasodilate Continued exposure vasoconstriction Superficial frostbite − Numbness, itching, prickling sensation − Cyanotic, reddened, white Deeper frostbite paresthesias and stiffness

FROSTBITE, continued Thawing of tissues − Skin white or yellow − Loses elasticity − Burning pain − Edema, blisters − Necrosis, gangrene Rapid thawing may significantly decrease tissue necrosis

Risk Factors Older adult Infants, young children Adolescents Damage to hypothalamus Decreased ability to shiver Decreased basal metabolic rate Evaporation from skin in cool environments Exposure to cool environments

Risk Factors, continued Acute or chronic illness Inactivity Inadequate clothing Malnutrition Medications Trauma Hypothyroidism Immaturity of newborn

Clinical Manifestations Mild Hypothermia (34°-36°C ) �Fatigue �Slurred speech �Poor coordination and clumsiness �Confusion and poor judgment �Inappropriate behavior �Shivering �Tachycardia and tachypnea

Clinical Manifestations, continued Moderate Hypothermia (30°-34°C) �Depressed mental state �No shivering �Depressed respirations �Slow pulse or irregular heart rate �Hypotension �Pale or cyanotic skin �Hallucinations �Coma

Clinical Manifestations, continued Severe or Profound Hyperthermia (<30°C) �Absence of respirations and pulse �Ventricular fibrillation �Dilated and unresponsive pupils �Coma

Clinical Management Collaboration Primary Prevention * Reduce Risk Factors * Educate regarding avoidance to exposure and extreme temperatures * Provide adequate resources - Environmental control and shelter - Appropriate clothing

Clinical Management Collaboration Primary Prevention - Physical activity - Social services – assess parent’s ability to meet needs, financial constraints, homelessness - Free clinics - Manufacturing prescription programs - Schools

Clinical Management Collaboration, continued Secondary Prevention - Identify underlying cause - Provide comfort - Monitor vital signs closely - Cardiorespiratory monitor - Temperature regulation - Prevent complications

Clinical Management Collaboration, continued Tertiary Prevention - Remove from cold - Provide warm environment – dry clothes - Warming blankets - Administer warm oral fluids - Keep limbs close to body

Clinical Management Collaboration, continued Tertiary Prevention - Cover scalp with blanket or cap - Apply warming pads to axillae, groin, forehead, and nape of neck - Supply warm oral or intravenous fluids - Warm fluid gastric lavage

Clinical Management Collaboration, continued Tertiary Prevention, continued - Rapidly rewarm affected areas in circulating warm water, 104°-105° F (40 -40. 5°C) for 20 to 30 minutes - Following rewarming, keep on bedrest with affected areas elevated - Avoid rubbing or massaging affected areas - Heated humidified oxygen - Administer analgesics and anti-inflammatory agents

Clinical Management Collaboration, continued Tertiary Prevention, continued - Debride blisters - Whirlpool therapy to clean skin and debride necrotic tissue - Support respiratory and cardiac function - Reduce handling to decrease risk of cardiac fibrillation - Hemodialysis and/or peritoneal dialysis

Nursing Process ASSESSMENT Body Temperature – below normal range Cool skin Cyanotic nail beds, slow capillary refill Blood pressure Pallor Piloerection and shivering Tachycardia

Nursing Process DIAGNOSIS Imbalanced Body Temperature, Risk for Ineffective Thermoregulation Hypothermia Impaired Skin Integrity, Risk for

Nursing Process PLANNING Prevention is a primary nursing goal: - Thermoregulation: Balance among heat production, heat gain, and heat loss - Thermoregulation in Neonate: Balance among heat production, heat gain, and heat loss during the first 28 days of life - Vital Signs: Temperature is within normal range

Nursing Process IMPLEMENTATION All Clients - Remove from cold, rewarming - Mild hypothermia → warm with blankets - Severe hypothermia → Hypothermic blanket - Warm IV fluids - Dry clothing - Monitor vital signs, urine output - Assess for cold-related injuries

Nursing Process IMLEMENTATION: NEWBORN Newborns - Transfer to NICU - Critical in very-low-birth-weight infants - Polyethylene wrapping - Head coverings - Swaddling, nesting - Observe for signs of cold stress

Nursing Process IMLEMENTATION: NEWBORN, continued Newborns, continued ■ Signs of cold stress - Increased movement, respirations - Decreased skin temperature, peripheral perfusion - Development of hypoglycemia • Result of metabolic effects of cold stress • Glucometer values

Nursing Process IMLEMENTATION: NEWBORN, continued Newborns, continued ■ Hypothermia in newborn - Maintain neutral thermal environment - Warm newborn slowly - Increase air temperature 1°C/hour until stable - Monitor skin temperature every 15 -30 minutes - Remove plastic wrap caps, while rewarming - Warm IV fluids before infusing - Block heat loss

Nursing Process IMLEMENTATION: CHILDREN Teach Parents - Layer children’s clothing, hats in cold climates - Recognizing signs of hypothermia - Decrease time of exposure to cold temperatures - Know how to treat mild hypothermia Teach School-age, Adolescents - Recognize and manage hypothermia in self, others - Prevention techniques

Nursing Process IMLEMENTATION: CHILDREN, continued First Aid - Move to dry area - Remove wet clothing - Protect from further environmental exposure - Wrap in dry clothing - Encourage to drink warm high calorie liquid

Nursing Process IMPLEMENTATION: OLDER ADULTS The older adult is less able to maintain internal temperature Similar to treatment at any age Assess for other risk factors: - Nutritional status - Home environment - Financial concerns - Self-care deficits

Nursing Process EVALUATION No piloerection or shivering Maintain core temperature within normal ranges Report thermal comfort Describe adaptive measures - Minimize fluctuations in body temperatures - Report early signs and symptoms

Learning Activity Break up into small groups (2 to 4 students). Develop a plan of care for preventing hypothermia for one of the following clients: • A premature newborn • A term newborn • An elderly man • A homeless woman living in a city with a cold climate
- Slides: 43