HYPOTENSIVE ANESTHESIA By Khosrou Naghibi MD Isfahan University


HYPOTENSIVE ANESTHESIA By Khosrou Naghibi MD Isfahan University of Medical Sciences

Synonyms of DH • • Controlled hypotension Induced hypotension Circulatory control Hypotensive anesthesia

Purpose of DH: • This technique was deployed to: • Decrease Blood loss • Improve operative field • Decrease duration of Sx.

DELIBERATE HYPOTENSION To reduce bleeding • To reduce blood transfusions • Indicated: Oromaxillofacial surgery Endoscopic sinus microsurgery Middle ear microsurgery Spinal surgery Neuro surgery Major orthopaedic surgery Prostatectomy CV surgery Liver transplant surgery • • •

DH Cont. . Definition Ø Reduction in systolic blood pressure to 80 -90 mm. Hg Ø Decrease in MAP to 50 -65 mm. Hg in normotensive patients Ø Reduction in MAP by one-third of its baseline values

DELIBERATE HYPOTENSION DEFINITION: Reduction of the systolic blood pressure • to 80 -90 mm. Hg Reduction of mean arterial pressure • (MAP) to 50 -65 mm. Hg 30% reduction of baseline MAP • DRUG. 2007; 67 (7): 1053 -76

DH Cont. . Safe level of DH • Depends on the pt. • Healthy young pt. tolerate mean B. P. as low as 50 -60 mm. Hg. • Ch. hypertensive pts. tolerate a mean of B. P. no more than 25% lower than the base line. • Pts. with TIA may not tolerate any decrease in cerebral perfusion pressure.

• Extremes : • • Hypotension always avoided Hypotension produced for any desire of surgeon.
DH Cont. . Indication Ø Neurosurgery Ø Orthopedics: THR, spine fusion ØEar, Nose, Throat/Oral Surgery Ø Gynecologic/urologic: radical pelvic surgery, prostatectomy Ø Religious blood refusal, rare blood type, difficult cross matching

DH Cont. . Contraindications • Infants • Systemic disease compromising major organ function • Renal, cerebral, coronary artery diseases • Pt. with sickle cell anemia • Polycythemia (uncorrected)

DH Cont. . Significant reduction in O 2 delivery: • • • ANEMIA SEVER LUNG DISEASE LOW CARDIAC OUTPUT

DH Cont. . Absolute contraindications • Cerebrovascular disease • Inexperience of the anesthesiologist

DH Cont. . Complications • Underperfusion of major organ: • • Cerebral thrombosis Hemiplegia ATN Massive hepatic necrosis Blindness Retinal artery thrombosis Ischemic optic neuropathy • Surgical complications • Reactionary hemorrhage • Hematoma formation
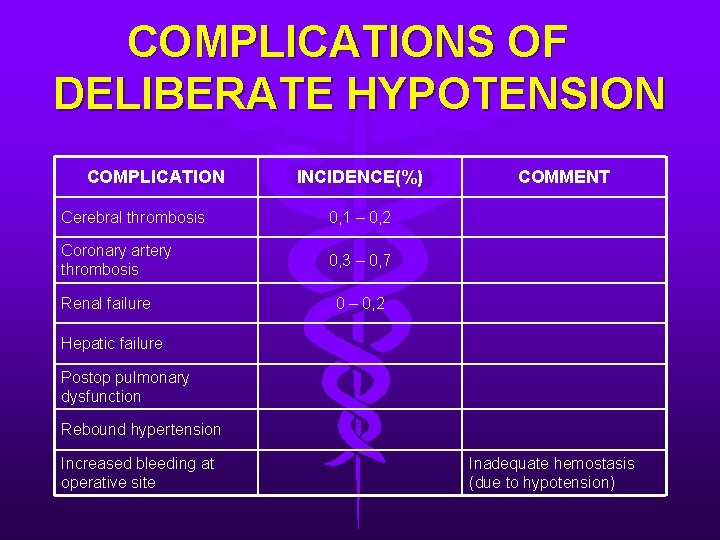

COMPLICATIONS OF DELIBERATE HYPOTENSION COMPLICATION INCIDENCE(%) Cerebral thrombosis 0, 1 – 0, 2 Coronary artery thrombosis 0, 3 – 0, 7 Renal failure COMMENT 0 – 0, 2 Hepatic failure Postop pulmonary dysfunction Rebound hypertension Increased bleeding at operative site Inadequate hemostasis (due to hypotension)

RELATIVE CONTRA INDICATIONS TO INDUCED HYPOTENSION Ischemic cerebrovascular desease Coronary artery desease Hypovolemia Anemia Severe hypertension Extremes of age • • •

Hemodynamic effects of Hypotensive drugs: TACHYPHYLAXIS: • Response despite repeated administration of the drug • More frequently seen in young adults • Has been reported with most drugs. TACHYCARDIA.

Control of heart rate: The key to preventing tachyphylaxia is control of heart rate: • Inhalational anesthesia • Avoiding fluid overload • Pre-Op. sedation + IV opioid.
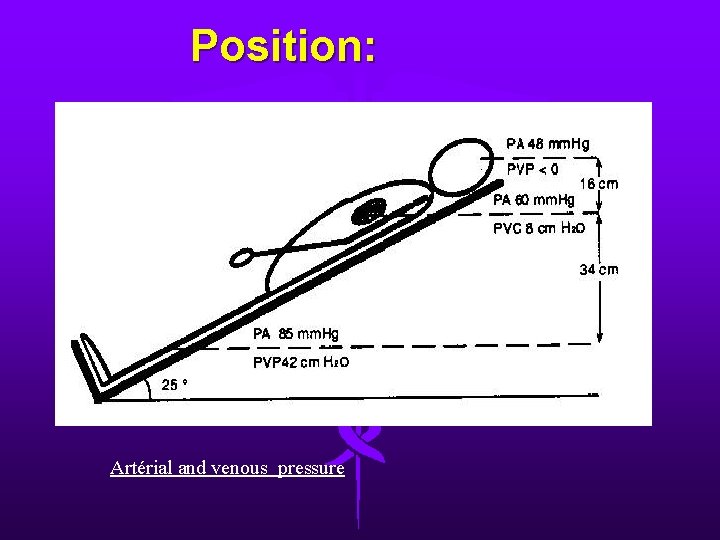
Position: Artérial and venous pressure
Reduction of bleeding : position 10 -15° head up tilt position Head position : head rest rotation - controlateral ear - jugular vein - bracchial plexus - carotid artery

DELIBERATE HYPOTENSION: NEW TECHNIQUES Use the natural hypotensive effects of • anaesthetic drugs with regard to the definition of the ideal hypotensive agent: Easy to administer Short onset time Disappears quickly when stopped Rapid elimination No toxic metabolites Negligible effect on vital organs Predictable effect Dose dependent effect • •

Remifentanil Key Concepts Remifentanil is an OPIOID l Pure m agonist l little binding at k, s, and d receptors¡ The effects of remifentanil are identical l with other commonly used opioids fentanyl¡ alfentanil¡ sufentanil¡

DELIBERATE HYPOTENSION: NEW TECHNIQUES Epidural anaesthesia • Remifentanil: - Propofol • Remifentanil: - Isoflurane • - Desflurane - Sevoflurane Epinephrine and inhalation anesthetics 5. 4 mcg/kg with isoflurane 10 mcg/kg with sevoflurane 10 mcg/kg with desflurane BJA 2008 Jan; 100(1): 50 -4 Rhinology 2007 mar; 45 (1): 72 -8 Eur J. Anaesthesiol 2007 may; 24 (5): 441 -6 AM J. Rhinol 2005 sept-oct; 19 (5): 514 -20 Laryngoscopie 2003 aug; 113 (8): 1369 -73

Monitoring during Controlled hypotension

DH Cont. . 1. Arterial blood pressure 2. ECG – myocardial perfusion Risk of: Tachycardia Bradycardia Arrhythmias St-sigment changes Ishcemia

3. Gas exchange: Capnography is essential: • • As a disconnection alarm Indicator of air embolism • ( Correlation between ETCO 2 & Pa. CO 2 is limited VD/VT) during DH • Helps avoid hyperventilation in DH Pulse oximetry 4. Temperature

Method • Physiologic technique • Pharmacologic technique

DELIBERATE HYPOTENSION AGENTS USED ALONE: • Inhalation anaesthetics Sodium nitroprusside Nitroglycerin Trimethaphan Prostaglandine E 1 Adenosine Remifentanil Agents for spinal anaesthesia • • ALONE OR COMBINED: • Calcium channel antagonists • Beta-Blockers • Fenoldopam • COMBINED: • ACE inhibitors • Clonidine •

Physiologic technique § Body positioning § Hemodynamic effects of mechanical ventilation § Changes in heart rate & circulatory volume

Pharmacologic technique • Ideal agent - Ease of administration - Predictable & dose-dependent effect - Rapid onset/offset - Quick elimination without the production of toxic metabolites - Minimal effects on blood flow to vital organs

1)Inhalational anesthetics – negative inotropic effect vasodilation • • Advantage Provides surgical anesthesia Rapid onset/offset Easy to titrate Cerebral protection Disadvantage • Decreases CO • Cerebral vasodilation

3)Sodium nitroprusside Direct vasodilator (nitric oxide release) • • Disadvantage Cyanide/thiocyanate toxicity Increased ICP Increased pulm. shunt Sympathetic stimulation Rebound hypertension Coronary steal Tachycardia • • • Advantage Rapid onset/offset East to titrate Increases CO

4)Nitroglycerin Direct vasodilator • • (nitric oxide release) Advantage Rapid onset/offset East to titrate Limited increase in heart rate No coronary steal • • • Disadvantage Lack of efficacydepending on anesthetic technique Increased ICP Increased pulm. shunt Methemoglobinemia Inhibition of plt. aggregation

5)Beta adrenergic antagonist Beta adrenergic blockade myocardial contractility) • • Advantage Rapid onset/offset Decreased myocardial O 2 consumption No increase in ICP No increase in pulm. shunt (decreased Disadvantage • • Decreased CO Heart block Bronchospasm Limited efficacy when used alone
6)Calcium channel blocker - vasodilation • • • Advantage Disadvantage Rapid onset Limited increase in HR • Prolonged duration of action Increase CO No effect on • Increased ICP airway reactivity • Increased pulm. Increased shunt GFR/urine output

Intravenous drugs

7)Remifentanil • Remifentanil is an OPIOID • Pure m agonist • little binding at k, s, and d receptors § Rapid onset/offset § Decreases blood pressure & heart rate § No need for additional use of a potent hypotensive or adjunct agents

Remifentanil Key Concepts • Remifentanil is an ESTER. Metabolized by nonspecific esterases in blood and tissue • Anesthesia maintained with high-dose remifentanil will be associated with rapid recovery. l Within 5 -10 minutes of turning off an infusion there is virtually no residual remifentanil drug effect

Remifentanil Potential Benefits • Changes in remifentanil drug effect rapidly follow changes in the remifentanil infusion rate. • The analgesic effects are evanescent. • Post-operative analgesic needs must be anticipated.

Remifentanil Metabolism • • Extremely rapid Not influenced by: • • • Hepatic disease Renal disease Pseudocholinesterase deficiency Administration of neostigmine Very young age Modest decrease in elderly patients

Anesthesia Technique • • • Monitoring Induction Position head up 450 BP drop range 20% - 40% of baseline HR range 50 – 60 beat/min

Observation, cont’d • PONV: • • Nausea & Vomiting. prophylactic anti-emetics are given perioperatively.
DH… • Ear Sx. • Produce bloodless surgical field for microscopy • Stapedectomy : • <0. 75 ml of blood loss condition • >1. 5 ml of blood loss good op. bad op. condition • In middle ear Sx. Even slight hemorrhage fibrosis so B. P. Improves the results.

Deliberate Hypotension In FESS § Moderate DH (systolic pressure 80 80 mm. Hg) • Reduces the capillary bleeding § Bloodless operative field provides good sinuses surgical conditions

CONCLUSION • Proper initiation of DH depends on the anesthesiologist. • Desired level of blood pressure can be achieved by skillful use of gravity, ventilation & drugs helped by proper monitoring and adequate Post Op. care. • Teamwork with cooperation between anesthesiologist and surgeon is of great importance in the care of pts. who undergo deliberate hypotension.

THANK YOU
- Slides: 46