Hyponatremia and Electrolyte Imbalances Exacerbated by Alcoholism and

Hyponatremia and Electrolyte Imbalances Exacerbated by Alcoholism and Poor Intakes Natalie Briggs, Dietetic Intern Andrews University April 11, 2018

Introduction ❖ ❖ ❖ 66 -year-old female Born March 21, 1951 December 4 -19, 2017 Hyponatremia, hypokalemia, hypomagnesemia COPD exacerbation Drinks 45 beers/week or 6 “light” beers daily + 3 large water bottles daily Extremely poor intake Lethargic, weak, nauseous 8# wt loss in 1 month prior 5’ 4” (162. 6 cm) and 129# (58. 6 kg) BMI 19. 6 Pulmonary, Nephrology, Neurology, Gastroenterology, Cardiology following

Purpose and Reasoning of Study ❖ ❖ ❖ Why does hyponatremia exist? Implications of imbalance Process of correcting electrolyte imbalances through nutrition Not often discussed in school 15 -day LOS Kind

Why Hyponatremia & Treatment ❖ ❖ ❖ ❖ Diuretic use Diarrhea Heart failure Liver disease Renal disease Alcoholism Excess fluid intake Inappropriate ADH secretion ❖ ❖ Restricting water intake Promoting water loss Replacing sodium deficit Correcting underlying disorders

Social History Lives in Middletown with retired husband (44 yrs) Enjoys gardening + watering plants around fireplace Husband grocery shops and does laundry Share ADLs Fully independent 3 -liter nasal cannula @ home One-story home with 2 steps to enter Has sister, brother, 2 kids FMH: HTN, heart disease, DM (father); osteoporosis, cancer (mother), COPD (sister), cancer (brother) ❖ 2 hospitalizations in past 6 month ❖ Financially sound ❖ ❖ ❖ ❖ ❖

Past Medical History ❖ ❖ ❖ HTN Unspecified disease of pancreas Tobacco use disorder Proteinuria Secondary polycythemia Unspecified pneumonia Abnormal glucose Lump in breast Enlargement of lymph nodes Hyposmolality Hyponatremia ❖ ❖ ❖ ❖ ❖ Thrombocythemia COPD exacerbation 17. 5 yr smoker (3 -4 cigarettes/day) Chronic airway obstruction Cervical spondylosis Arthritis Cardiac stress test (2014) Left wrist fracture (2015) Proximal humerus fracture (2016) Pacemaker (2017)

Medication List ❖ ❖ ❖ Feosol Theragran Zofran Protonix Phenergan Thiamine Solu-Medrol Lopressor Miralax/Dulcolax Culturelle Huma. Log

Medical Status and Treatment ❖ Shock + respiratory failure + seizure activity = intubation (O 2 in 40 s) ➢ Alcohol withdrawal with minor encephalopathy secondary to hyponatremia ❖ Endotracheal tube + OG ❖ Fi. O 2 50%, Levophed (10 mcg/min), Diprivan (13 ml/hr--340 kcal), Vancomycin (250 ml/hr), 3% sodium solution (25 cc/hr), NS @ 75 ml/hr ❖ Jevity 1. 2 @ 20 ml/hr suggested, but postponed d/t GIB ❖ GI scope found stomach blood clot from bleeding and impaired RBC from alcohol ❖ Ulcerative esophagitis ❖ High risk of refeeding syndrome ❖ Pressor support
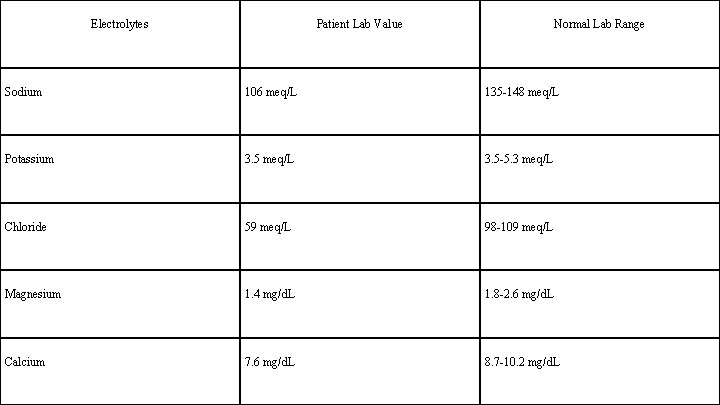
Electrolytes Patient Lab Value Normal Lab Range Sodium 106 meq/L 135 -148 meq/L Potassium 3. 5 meq/L 3. 5 -5. 3 meq/L Chloride 59 meq/L 98 -109 meq/L Magnesium 1. 4 mg/d. L 1. 8 -2. 6 mg/d. L Calcium 7. 6 mg/d. L 8. 7 -10. 2 mg/d. L

Medical Status and Treatment ❖ ❖ ❖ LLE/RLE non-pitting edema CT scan: acute/subacute infarcts Bronchoscopy: mucus, LLL worst Extubation attempted; pt became SOB, tachycardic and hypertensive Troponin elevated: NSTEMI during intubation 5. 5 days without nutrition = 4# wt loss (GIB) On 6 th day, D. R. successfully extubated to 6 -liter nasal cannula No neurological deficit Impaired mobility--hypotension, dyspnea, tachycardia prevented OT/PT Prognosis good Did not like s/p intubation diet Unjury and Ensure Plus acceptance

Nutrition ❖ Intubated nutrition needs: ➢ 1580 -1690 kcal and fluids initially ➢ 63 -79 grams PRO ❖ S/p intubation (12/9/17) and seen by SLP: ➢ ➢ Pureed diet with nectar-thick liquids and 1, 000 ml fluid restriction 1, 400 -1, 500 kcal 51 -61 grams PRO 50 -75% ❖ 12/13/17 seen by SLP: ➢ Regular diet with thin liquids (plus later 1, 200 ml fluid restriction and 1, 500 ml @ DC) ➢ Could tolerate grilled cheese, peanut butter, crackers, fruit and thin water ➢ 100%

24 -Hour Recall and Typical Diet ❖ ❖ One meal/day @ dinnertime Dinner: fish, chicken, beef, vegetables, breads Snacks throughout day: crackers, cheese, apples Drinks her calories: beer

Medical Status and Treatment 8 days no bowel movement (poor intake + limited mobility) Miralax + Dulcolax C/o gas, cramping, tender abdomen, nausea Several bowel movements occurred that night Poor po intake @ 20% with nausea and thick phlegm NS @ 50 ml/hr (lowered d/t continued hyponatremia) Positive for UTI and put on steroids 12/15/17 transferred to rehab, ate dinner independently then respiratory failure ❖ 3 -liter to 8 -liter NC and sent to CTU/ 12 -liter high-flow NC overnight ❖ NPO for thoracentesis and advanced later on that day ❖ Ate better on regular diet ❖ ❖ ❖ ❖

Medical Status and Treatment Ate breakfast the next day: eggs, yogurt, fruit and a lunch Ate applesauce with meds Refused supplementation Encouraged po intake as close to 100% as possible Smoking and alcohol cessation discussed per MD 12/12/17 to 12/18/17 125# to 114# or 9% wt loss 12% wt loss throughout 15 -day stay + 8# wt loss in month prior = 17% wt loss ❖ While on pureed diet, nectar-thick, she admitted to not intaking much plus while intubated, no nutrition was ever started ❖ Hypotension (65/35) + fluctuating respiratory status = sent to CV ICU ❖ Easily fluid overloaded, constipated ❖ ❖ ❖ ❖

Final Result ❖ Sent to LTAC for Rocephin for UTI, IV steroids for COPD exacerbation and mucus plugging, high-flow NC Vapotherm @ 20 L/60% ❖ Overwhelmed with whole recovery period, but encouraged to take it one day at a time ❖ Emphasized eating 3 meals/day in LTAC and at home ❖ Encouraged supplementation ❖ Counseled on healthy eating and its importance ❖ More willing to change habits--Ensure @ house ❖ High to moderate nutrition risk throughout stay ➢ ICU, vent, TF ➢ Respiratory failure, poor appetite and poor po intake ❖ Left on regular diet, thin liquids and 1, 500 ml fluid restriction

Goals ❖ Improve electrolyte balance ❖ Body health, strength and healing ❖ Stop continual weight loss ❖ ❖ 3 meals/day, 100% Choose healthy options One Ensure daily Decrease alcohol intake to 0 -1 drinks/day
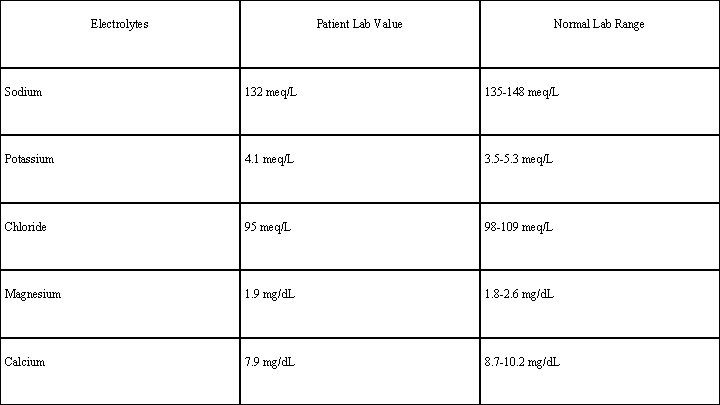
Electrolytes Patient Lab Value Normal Lab Range Sodium 132 meq/L 135 -148 meq/L Potassium 4. 1 meq/L 3. 5 -5. 3 meq/L Chloride 95 meq/L 98 -109 meq/L Magnesium 1. 9 mg/d. L 1. 8 -2. 6 mg/d. L Calcium 7. 9 mg/d. L 8. 7 -10. 2 mg/d. L
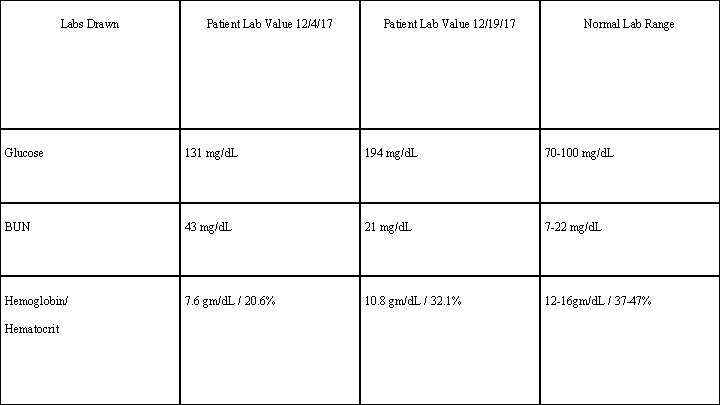

Labs Drawn Patient Lab Value 12/4/17 Patient Lab Value 12/19/17 Normal Lab Range Glucose 131 mg/d. L 194 mg/d. L 70 -100 mg/d. L BUN 43 mg/d. L 21 mg/d. L 7 -22 mg/d. L Hemoglobin/ 7. 6 gm/d. L / 20. 6% 10. 8 gm/d. L / 32. 1% 12 -16 gm/d. L / 37 -47% Hematocrit

Conclusion ❖ ❖ ❖ ❖ Hyponatremia is a serious complication that is life-threatening Can occur easily. . . drinking too many fluids Problem to be aware of for individuals struggling with alcoholism Being aware of GIB and gastrointestinal issues Importance of minimal to no alcohol consumption Adequate food intake for survival and to thrive Open-minded, kind couple Positive reinforcement

Bibliography Queensland Ambulance Service (2016). Orogastric tube insertion. Retrieved from https: //www. ambulance. qld. gov. au/docs/clinical/cpp/CPP_Orogastric%20 tube%20 inserti on. pdf. Lewis, James L. III (2018). Hyponatremia. Retrieved from https: //www. merckmanuals. com/professional/endocrine-and-metabolic-disorders/electrol yte-disorders/hyponatremia. Mayo Clinic (2018). Hyponatremia. Retrieved from https: //www. mayoclinic. org/diseases-conditions/hyponatremia/symptoms-causes/syc-203 73711. Davis, C (2018). Electrolytes. Retrieved from http: //grfx. cstv. com/photos/schools/stjo/genrel/auto_pdf/2011 -12/misc_non_event/Electr olytes. pdf. NIH (2016). Magnesium. Retrieved from https: //ods. od. nih. gov/factsheets/Magnesium-Consumer/. NIH (2017). Upper GI endoscopy. Retrieved from https: //www. niddk. nih. gov/health-information/diagnostic-tests/upper-gi-endoscopy. Healthline (2017). Everything you should know about refeeding syndrome. Retrieved from https: //www. healthline. com/health/refeeding-syndrome. Schrier, Stanley, MD (2017). Hematologic complications of alcohol use. Retrieved from https: //www. uptodate. com/contents/hematologic-complications-of-alcohol-use.

Bibliography Continued. . . Collins, William (2017). Bronchial washing procedures. Retrieved from https: //www. livestrong. com/article/161434 -bronchial-washing-procedures/. Healthline (2017). SIADH. Retrieved from https: //www. healthline. com/health/syndrome-of-inappropriate-antidiuretic-hormone. Mc. Cleary, EJ and Tajchman, S (2016). Parenteral nutrition and infection risk in the intensive care unit: a practical guide for the bedside clinician. 4. 476 -89. Retrieved from https: //www. ncbi. nlm. nih. gov/pubmed/27317614. NIH (2017). Atelectasis. Retrieved from https: //www. nhlbi. nih. gov/health-topics/atelectasis. ASLHA (2017). Long-term acute care hospitals. Retrieved from https: //www. asha. org/slp/healthcare/LTAC/. Boulder Medical Center (2017). Nutrition recommendations for those who consume alcohol. Retrieved from https: //www. bouldermedicalcenter. com/nutrition-recommendations-consume-alcohol/. AHA (2018). 5 Reasons to eat more color. Retrieved from https: //healthyforgood. heart. org/add-color/infographics/5 -reasons-to-eat-more-color.
- Slides: 21