Hypertension Objectives Identify differential diagnosis of a case

Hypertension

Objectives: ü Identify differential diagnosis of a case presented with the symptoms of lower limb oedema. ü Differentiate between different etiologies of hypertension. ü Discuss briefly between stages of hypertension. ü Enumerate and discuss the importance signs& symptoms in patients with hypertension.

ü Investigate appropriately a patient with hypertension. ü Advice initial management plan for a patient with hypertension according to recent guidelines (NICE 127). ü Discuss non-drug management of hypertension. ü Identify long term complications of hypertension.

Case scenario • A 50 -year-old woman presents to your clinic for routine follow-up. She has a history of hypertension for ~ 15 years. She mentioned that she has noted fatigue and increased swelling in her lower extremities during the past several weeks. Medications: Amlodipine (CCB) 10 mg OD.

On Physical examination: • She appears to be in no apparent distress. Height: 153 cm Weight: 100 kg. Blood pressure: 165/98 mm. Hg, Pulse 85/minute RR: 20/minute. Cardiac exam was remarkable for an S 1, S 2 and S 4. Lungs were clear to auscultation and percussion. Abdomen was obese, non-tender and without masses or bruits. Lower extremities had good pulses with pitting edema. Other systemic examination was normal

Differential diagnosis of lower limp edema Ø Venous Insufficiency Ø Heart Failure Ø Pulmonary Hypertension Ø Drugs. E. g. (CCB & NSAIDS) Ø Idiopathic Edema Ø Lymphedema Ø Deep Vein Thrombosis Ø Obesity

What is hypertension? - A term used to describe high blood pressure. Blood pressure is a measurement of the force against the walls of the arteries as the heart pumps blood through the body. - The risk of morbidity and mortality increases progressively with increasing systolic and diastolic blood pressure. .
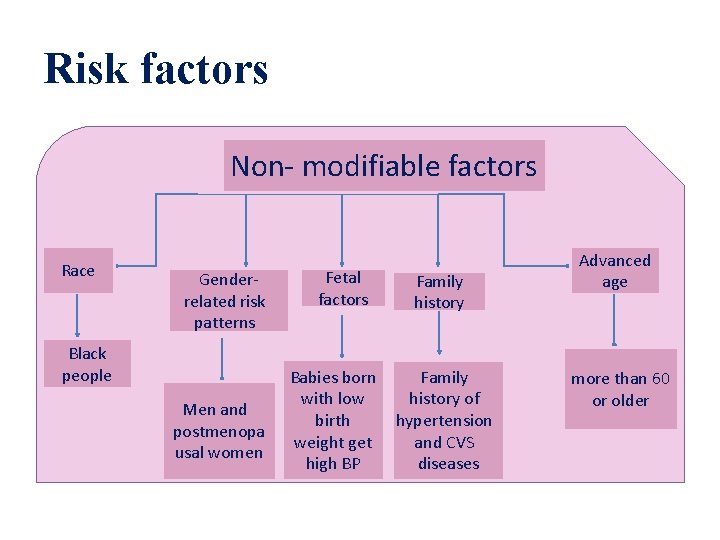
Risk factors Non- modifiable factors Race Genderrelated risk patterns Black people Men and postmenopa usal women Fetal factors Family history Babies born Family with low history of birth hypertension weight get and CVS high BP diseases Advanced age more than 60 or older
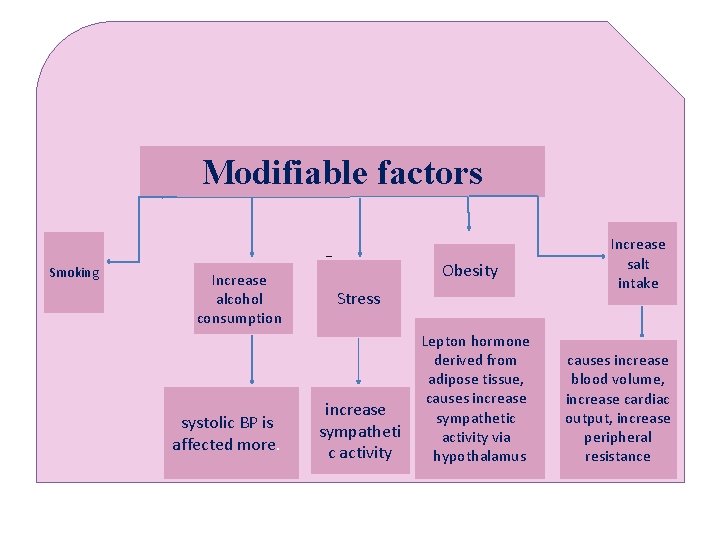
Modifiable factors Smoking Increase alcohol consumption systolic BP is affected more. Stress Obesity Stress increase sympatheti c activity Lepton hormone derived from adipose tissue, causes increase sympathetic activity via hypothalamus Increase salt intake causes increase blood volume, increase cardiac output, increase peripheral resistance

Causes of hypertension 1) Primary (essential) Hypertension: Has no known cause (idiopathic) ü Multi-factorial etiology : 2) Genetic Factors - Positive Family History 3). Environmental Factors -Obesity -Increased Sodium Intake -Stress - Increased Alcohol Intake -95% of hypertensive patient fall into this category.

Secondary Hypertension 2) Secondary Hypertension: Due to an underlying medical condition • Endocrine • Cardiovascular • Renal • Chronic alcohol abuse • Medications

Secondary Hypertension Renal: - Polycystic disease - Renal artery stenosis - Renin-producing tumors - Chronic renal disease - Renal vasculitis

Endocrine: - Adrenocortical hyperfunction (Cushing syndrome) - primary aldosteronism, congenital adrenal hyperplasia) - Exogenous hormones (glucocorticoids, estrogen) - Pheochromocytoma - Hypothyroidism - Hyperthyroidism - Pregnancy-induced

Cardiovascular: - Coarctation of aorta - Vasculitis - Increased intravascular volume

Medications: - Steroids - Oral contraceptives - Amphetamines and cocaine - Nonsteroidal anti-inflammatory - Psychiatric: carbamazepine, lithium and tricyclic, antidepressants
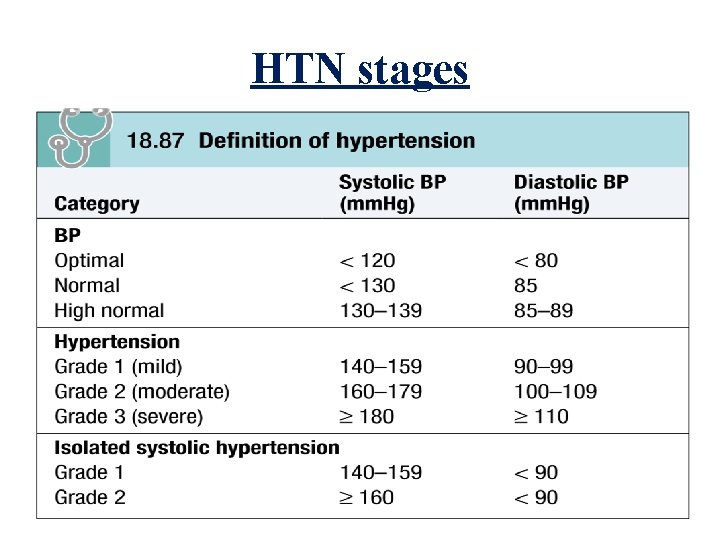
HTN stages

hypertensive crisis (BP >180/120 mm Hg) categorized as either - hypertensive emergency (extreme BP elevation with acute or progressing target organ damage) - hypertensive urgency (severe BP elevation without acute or progressing target organ injury). - Malignant hypertension when diastolic BP more than 130 mm. Hg. Unless treated, it may lead to death due to renal failure, heart failure or stroke.

Signs & symptoms 1) Severe headache 2) Fatigue or confusion 3) Vision problems 4) Chest pain 5) Difficulty breathing 6) Irregular heartbeat 7) Hematuria 8) Lower limb edema
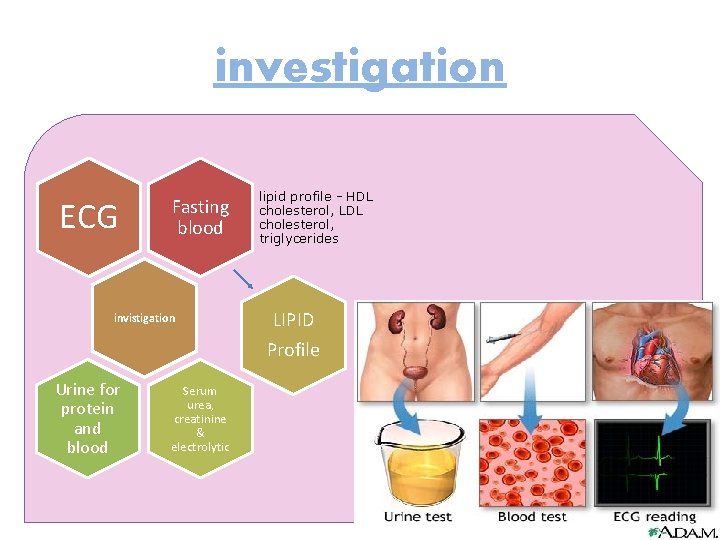
investigation ECG Fasting blood invistigation lipid profile - HDL cholesterol, LDL cholesterol, triglycerides LIPID Profile Urine for protein and blood Serum urea, creatinine & electrolytic

Optional laboratory tests Aortic Coarctation - Arm to leg systolic Blood Pressure difference (abnormal if >20 mm. Hg) - Chest X-Ray (notching of the lower rib borders) - Echocardiogram (Children) - MRI Chest (Adults) Cushing's Disease - 24 hour Urine Cortisol - Late night Salivary cortisol - Low dose Dexamethasone Suppression Test

Pheochromocytoma - 24 h Urine Metanephrine - Plasma free metanephrines • Note : - Patients with pheochromocytoma may have a history of paroxysmal headaches, sweating, tachycardia, palpitations, and orthostatic hypotension.
X-rays : - May show cardiomegaly X-RAY CHEST IN HEART FAILURE

Specialist investigations: ● Refer people to specialist care the same day if they have: − accelerated hypertension (BP > 180/110 mm. Hg ) with signs of papilloedema and/or retinal haemorrhage) − suspected phaeochromocytoma (labile or postural hypotension, headache, palpitations, pallor and diaphoresis). ● If needed, more investigations for secondary cause of hypertension could be performed.

How to measure BP? By sphygmomanometer

How to diagnose hypertension ? • Should be based on the average of two or more readings taken at each of two or more clinical encounters • The funduscopic examination. • Cardiopulmonary examination. • Peripheral vascular examination can detect evidence of atherosclerosis.

HTN Treatment HTN TREATMENT 1. Non-Pharmacological 2. Pharmacological

1 st life style modification 1) Weight reduction (BMI, 18. 5 to 24. 9 kg/m 2) 2) Adoption of the Dietary Approaches to Stop Diary Approach to Stop HTN (DASH) plan : - Low content of saturated fat, cholesterol, and total fat - Focuses on fruits, vegetables, and fat-free or low-fat dairy products - Rich in whole grains, fish, poultry, beans, seeds, and nuts - Contains fewer sweets, added sugars and sugary beverages, and red meats - Dietary sodium restriction ideally to 1. 5 g/day

4) Regular aerobic physical activity. 5) Moderate alcohol consumption (2 or fewer drinks/day). 6) Smoking cessation 7) Do not offer calcium, magnesium or potassium supplements as a method of reducing blood pressure
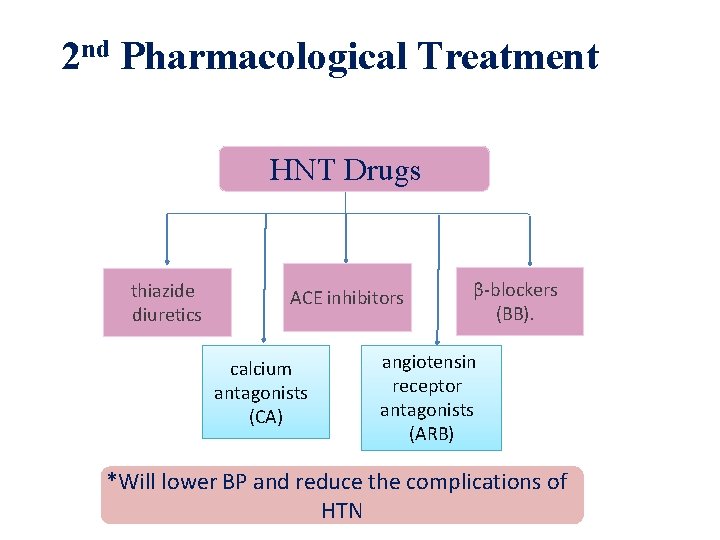
2 nd Pharmacological Treatment HNT Drugs thiazide diuretics ACE inhibitors calcium antagonists (CA) β-blockers (BB). angiotensin receptor antagonists (ARB) *Will lower BP and reduce the complications of HTN

2 nd Pharmacological Treatment 1) ACE Inhibitors ● Where to start? - Lisinopril 10 mg QD - Benazapril 10 mg QD - Enalapril 5 mg QD ● How much? - Up to 80 mg (only 40 mg for enalapril) ● Cost -- cheap! ● Side effects – dry cough , angioedema

2) CCBs ● Cost ? ● Where to start? - Amlodipine is generic - Amlodipine 5 mg QD - Diltiazem ER 120 mg QD - Diltiazem=cheap! - Nifedipine ER 30 mg QD - Nifedipine-less cheap ● How much ? ● Side effects ? - Amlodipine 10 mg QD - edema - Diltiazem ER 540 mg QD - constipation - Nifedipine ER 120 mg. QD

3) Thiazide diuretics ● Where to start? - Hydrochlorothiazide 12. 5 mg - Chlorthalidone 12. 5 mg ● How much ? - Up to 25 mg, unclear benefit beyond that ● Cost? Cheap! ● Side effects -- hypokalemia, glucose intolerance

4) Beta Blockers ● Do not start with beta blockers ● Why not? - Possible increase in stroke risk, particularly in elderly patients - first-line alternatives in patients who are 60 years and older, especially for stroke prevention.

Beta Blockers ● Where to start? - Metoprolol 25 mg BID - Atenolol 25 mg QD ● How much ? - Up to 100 mg ● Cost -- cheap! ● Side effects -- bradycardia, fatigue, depression

Even More Meds ● ARBs (losartan is generic but still pricey) ● Alpha blockers ● Aldosterone antagonists ACE inhibitors and ARBs not as effective in African-Americans

Indications & contraindications of medications
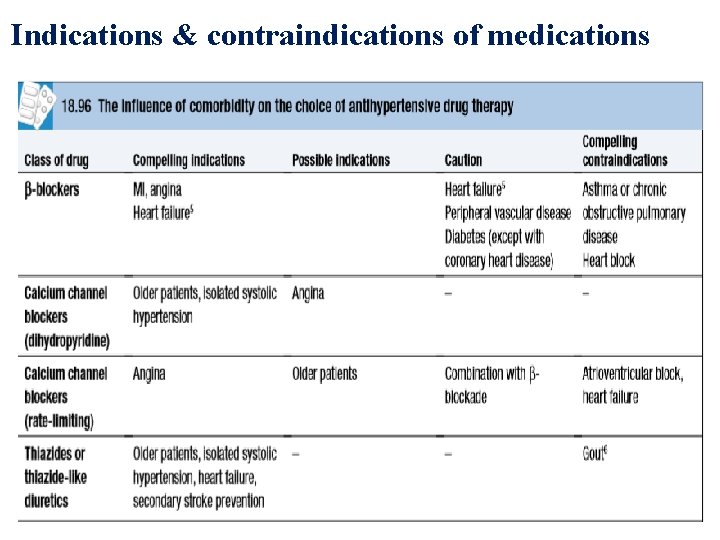
Indications & contraindications of medications
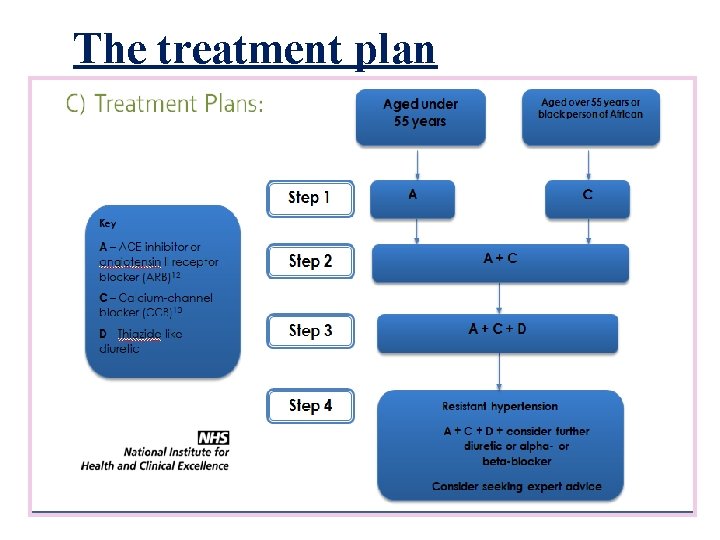
The treatment plan

How to treat hypertensive patients who have DM ? The BP goal in diabetes is less than 130/80 mm Hg. should be treated with ACE inhibitor or an ARB. Both classes provide nephroprotection andreduced CV risk. A thiazide-type diuretic is recommended as the second agent to lower BPand provide additional CV risk reduction. • CCBs are useful add-on agents for BP control in hypertensive patients withdiabetes

Follow up Labs: Potassium and Creatinine, maybe sodium ● at initiation of treatment ● 2 -4 weeks after starting ● Again after every dose adjustment ● Annually

Long term complications & end organs damages with HTN
Complications of HTN Heart Blood vessels Kidney Organs affected brain eyes
Complications of HTN 1)Atherosclerosis: formation of fibro fatty lesions in the intimal lining of the large and medium sized arteries such as aorta and its branches, coronary arteries and cerebral arteries 2)Stroke or Heart Attack: If an atherosclerotic plaque breaks off inside the artery, or the blood vessel ruptures, a blood clot can form within the artery. If this blocks blood flow to the brain it can lead to a stroke. If it blocks blood flow to the heart it can result in a heart attack.
Complications of HTN 3)Aneurysm: The blood vessels have been weakened to such an extent that part of the blood vessel wall ‘balloons’ or bulges. 4)Vascular dementia: High blood pressure can cause the blood vessels that supply your brain with blood to narrow or become damaged.

Complications of HTN 5) Hypertensive retinopathy :
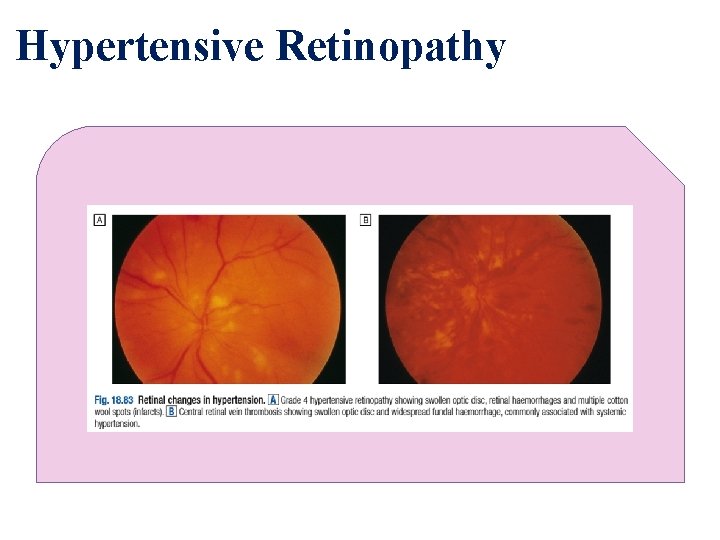
Hypertensive Retinopathy

References 1. NICE clinical guideline 127. 2. (JNC 8). JAMA. 2014 Feb 5; 311(5): 507 -20

Thank You
- Slides: 48