Hypertension Karen Ruffin RN MSN Ed Blood Pressure

Hypertension Karen Ruffin RN, MSN Ed.
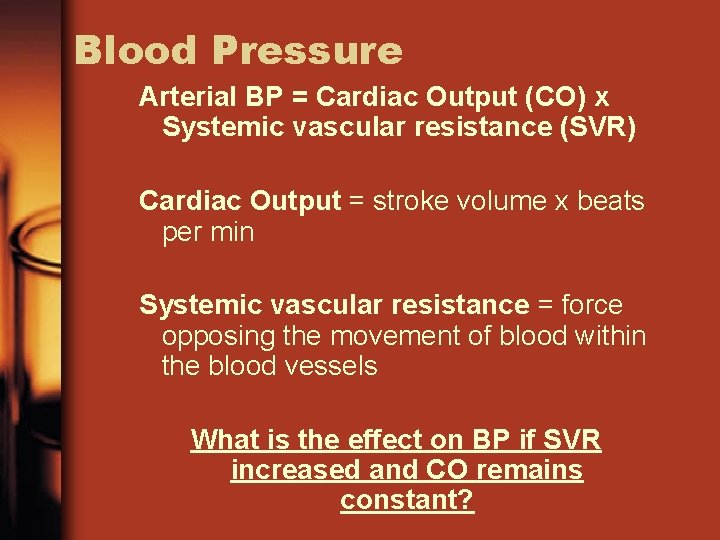
Blood Pressure Arterial BP = Cardiac Output (CO) x Systemic vascular resistance (SVR) Cardiac Output = stroke volume x beats per min Systemic vascular resistance = force opposing the movement of blood within the blood vessels What is the effect on BP if SVR increased and CO remains constant?
Blood Pressure Ø Definition: the force exerted by the blood against the walls of the blood vessels ØAdequate to maintain tissue perfusion during activity and rest ØArterial blood pressure: primary function of cardiac output and systemic vascular resistance

Mechanisms that Regulate Blood Pressure Ø Sympathetic Nervous System Ø Vascular Endothelium Ø Renal System Ø Endocrine System
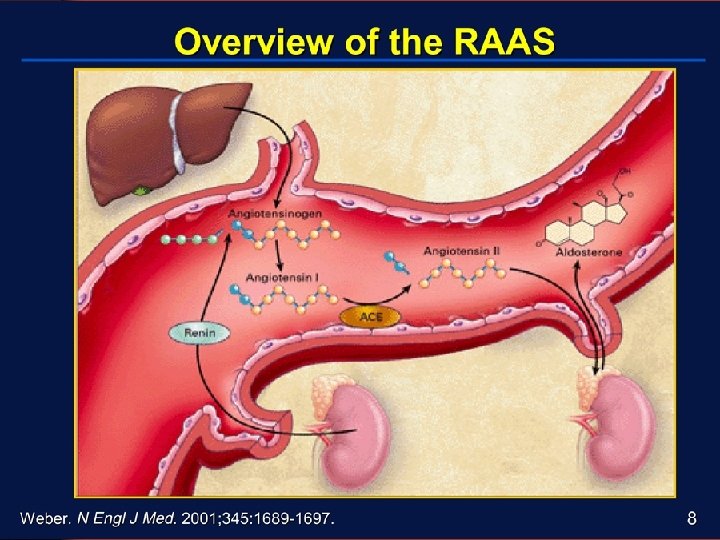
Hypertension Aldosterone Mechanism • Increased Aldosterone = • Increases sodium reabsorption = • Increases water reabsorption = • Increases blood volume = • Increases cardiac output
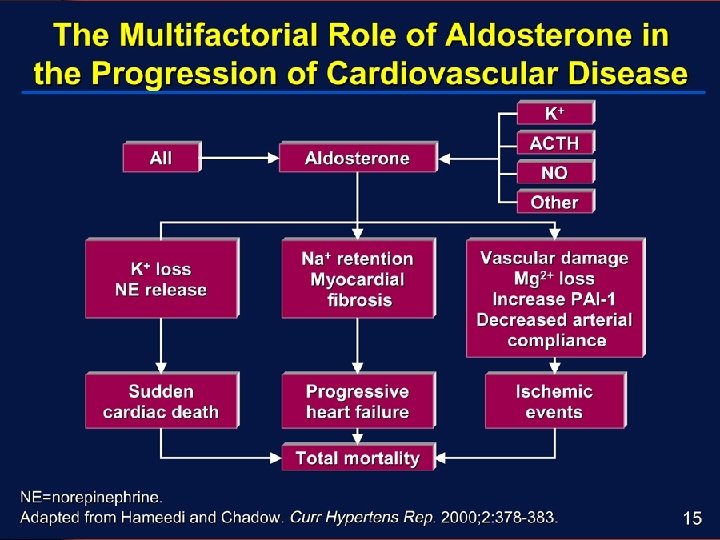
Hypertension Ø Regulatory mechanisms in the health person function in response to the demands on the body Ø When Hypertension develops, one or more of these mechanisms are defective ØSympathetic Nervous System ØVascular Endothelium ØRenal System ØEndocrine System

Hypertension Pathophysiology Ø Primary (Essential) Hypertension: ØElevated BP without an identified cause ØAccounts for 95% of all cases of hypertension ØCause – unknown ØContributing Factors: Increased SNS activity, overproduction of Na+ retaining hormones & vasoconstrictors, increased Na+ intake ØRisk Factors: Modifiable & Non-modifiable

Primary Hypertension Pathophysiology Ø Heredity – interaction of genetic, environmental, and demographic factors Ø Water & Sodium Retention – 20% of pts with high Na+ diet develop HTN Ø Altered Renin-Angiotensin Mechanism – found in 20% of patients Ø Stress & Increased SNS Activity Ø Insulin Resistance & Hyperinsulinemia Ø Endothelial Cell Dysfunction

Diagnosis of Hypertension Dx is made after multiple readings over several weeks NIH/Joint Committee Definition: Category Optimal Normal High Normal Systolic <110 <120 130 -139 and or Stage 1 Stage 2 Stage 3 140 -159 160 -179 =>180 or or or Diastolic < 80 <85 85 -89 90 -99 100 -109 => 110

Secondary Hypertension Pathophysiology Ø Specific cause of hypertension can be identified Ø Affects >5% of adults with hypertension ØWhat conditions can lead to or cause hypertension?

Primary Hypertension Risk Factors Ø Ø Ø Age Alcohol Cigarette Smoking Diabetes Mellitus Elevated serum lipids Ø Excess Na+ in diet Ø Gender Ø Family History Ø Obesity Ø Ethnicity Ø Sedentary Lifestyle Ø Socioeconomic Ø Stress Which risk factors are modifiable or non modifiable?

Primary Hypertension Clinical Manifestations Ø Organs that are affected by Hypertension: Ø Myocardium – angina / left ventricular hypertrophy Ø Brain – TIA / CVA Ø Peripheral vascular – Peripheral pulse change Ø Kidney – renal failure Creatinine / Proteinuria Ø Eyes – Hemorrhages with or without papilledema

Primary Hypertension Clinical Manifestations Ø “Silent Killer” – asymptomatic and insidious Ø Severe HTN – fatigue, reduced activity tolerance, dyspnea, dizziness, palpitations, angina

Hypertension Medical Diagnosis Ø History and Physical Examination Ø Renal Function ØSerum Creatinine & Urine Creatinine Clearance Ø Electrolytes – especially K+ Ø Blood Glucose Ø Serum Lipids/EKG Ø Ambulatory BP Monitoring

Primary Hypertension Medical Management Ø Risk Stratification ØLevel of BP ØPresence of Target Organ Disease ØOther Risk Factors

Primary Hypertension Medical Management Ø Lifestyle modification Ø Nutritional therapy Ø Alcohol consumption Ø Physical activity Ø Tobacco avoidance Ø Stress management Ø Drug Therapy

Stepped Approach to Manage Hypertension Lifestyle modification Not at Goal BP Drug Therapy Not at Goal BP Substitute med / add a 2 nd med/ increase dose Not at Goal BP Continue adding / changing meds until control

Medical Management – Drug Therapy Ø Diuretics Ø Thiazide Ø Loop Ø K+ Sparing Ø Adrenergic Blockers/ Inhibitors Ø B-Adrenergic Blockers Ø Central Acting Adrenergic Antagonists Ø Peripheral Acting Adrenergic Antagonists Ø A-Adrenergic Blockers Ø Vasodilators Ø Angiotensin Inhibitors Ø Calcium Channel Blockers
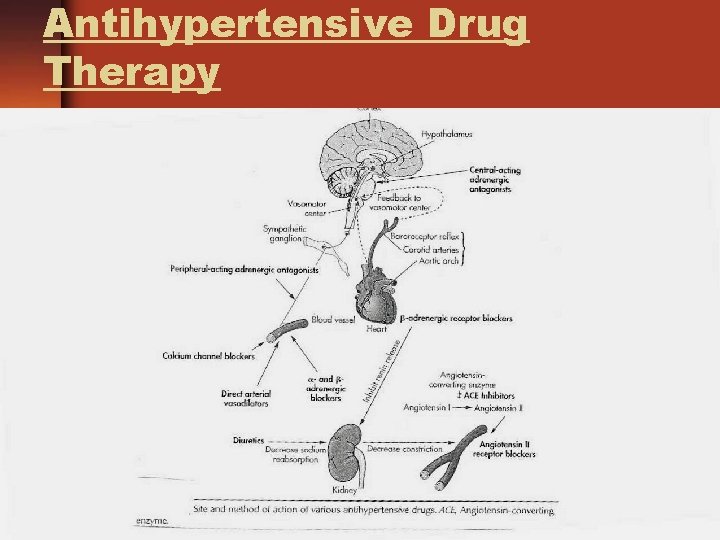
Antihypertensive Drug Therapy

Lack of Responsiveness to Therapy Ø Nonadherence to Therapy Ø Drug-Related Causes Ø Associated conditions Ø Secondary Hypertension Ø Volume overload

Nursing Care for the Patient with Hypertension • What will you assess? ? • What are some potential nursing diagnosis? ? ? • What are your goals for those diagnosis? ? • What are your interventions? ? ? • How will you evaluate your goals? ? ?

Basic Human Needs • What Basic Human Need is being affected? • What other Basic Human Needs are effected by hypertension?

Nursing Care for the Patient with Hypertension
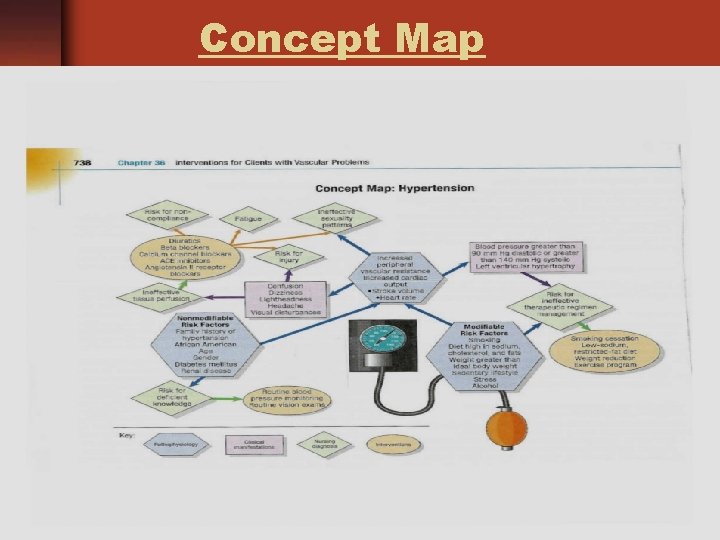
Concept Map

• The patient with essential hypertension is prescribes the beta blocker metoprolol (Lopressor). Which assessment data would make the nurse question administering the medication? • • A. The patients blood pressure is 112/90. B. The patients apical pulse is 56. C. The patients ha an occipital headache. D. The patient is complaining of a yellow haze.

• The nurse is preparing to administer the following medications. Which medications would the nurse question administering? • A. Vasodilator hydralazine(Apresoline) to the patient with blood pressure of 168/94. • B. Beta Blocker Lopressor(metoprolol) to a patient with a serum sodium level of 137. • C. Calcium Channel blocker diltiazem(Cardizem) to a patient with a glucose level of 280. • D. Loop Diuretic(Lasix) to a patient with a K+ of 3. 1.

Primary Hypertension Case Study
- Slides: 27