Hypertension HT High Blood Pressure HBP Renji Hospital

Hypertension (HT) High Blood Pressure (HBP) Renji Hospital Cardiology Department Li Hongbo slide 1

Introduction • Definition: Systemic arterial blood pressure elevated. • One of the most common disease in the world slide 2
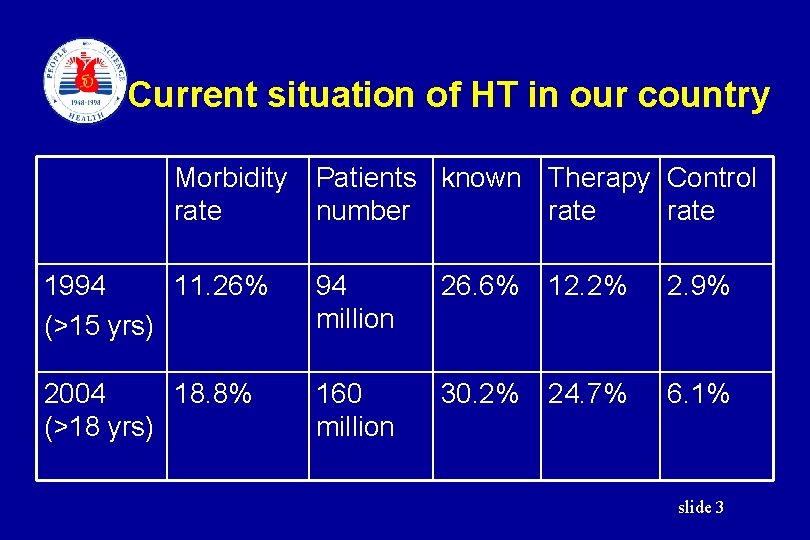
Current situation of HT in our country Morbidity Patients known Therapy Control rate number rate 1994 11. 26% (>15 yrs) 94 million 26. 6% 12. 2% 2. 9% 2004 18. 8% (>18 yrs) 160 million 30. 2% 24. 7% 6. 1% slide 3

Etiology • Genetic • Environment Dietary: Salt intake Alcohol intake Obesity Infant dysnutrition Psychological stress slide 4

Pathogenesis 1. High activity of the Sympathetic Nervous System 2. Renin-Angiotension Aldosterone System (RAAS) 3. Renal Sodium Handling 4. Vascular Remodelling 5. Endothelial Cell Dysfunction 6. Insulin Resistance slide 5
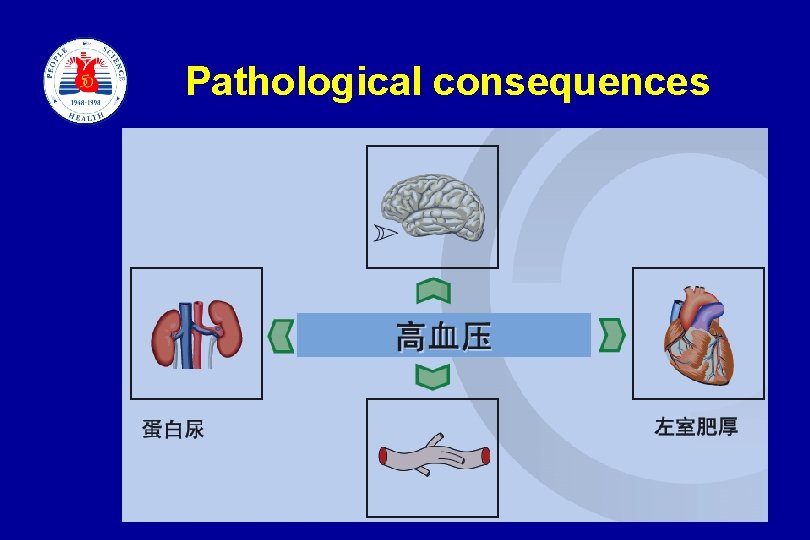
Pathological consequences slide 6
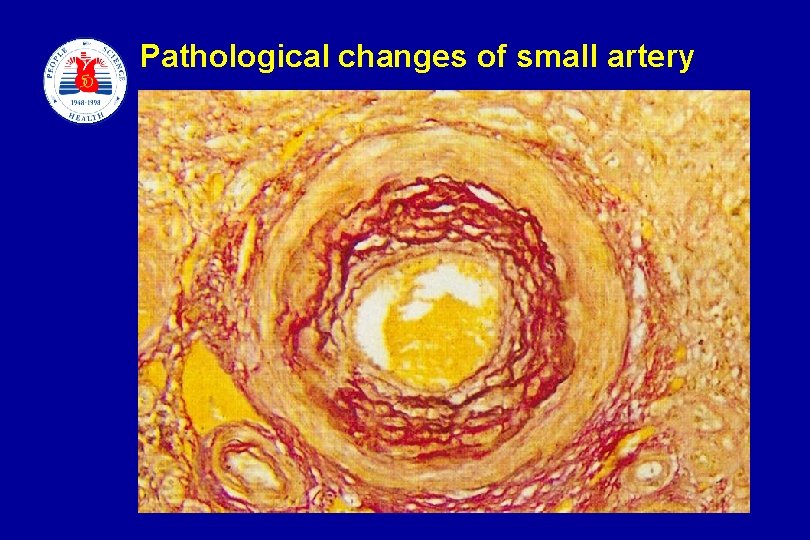
Pathological changes of small artery slide 8
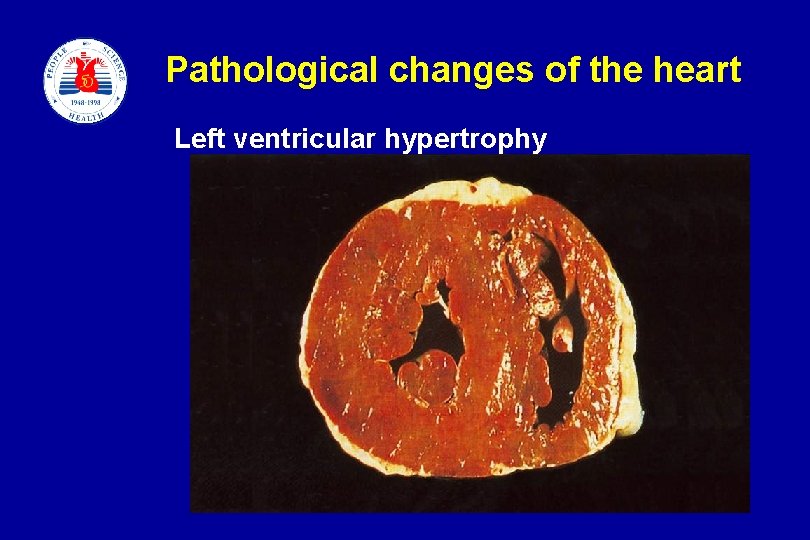
Pathological changes of the heart Left ventricular hypertrophy slide 9
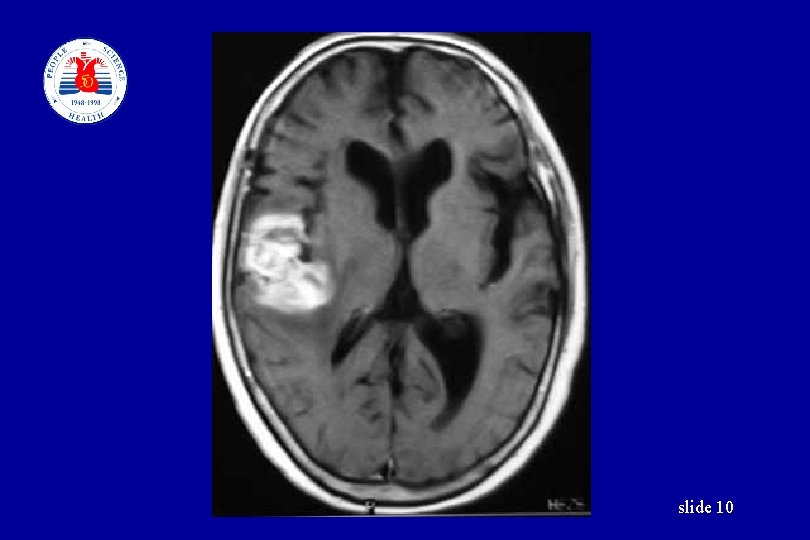
slide 10
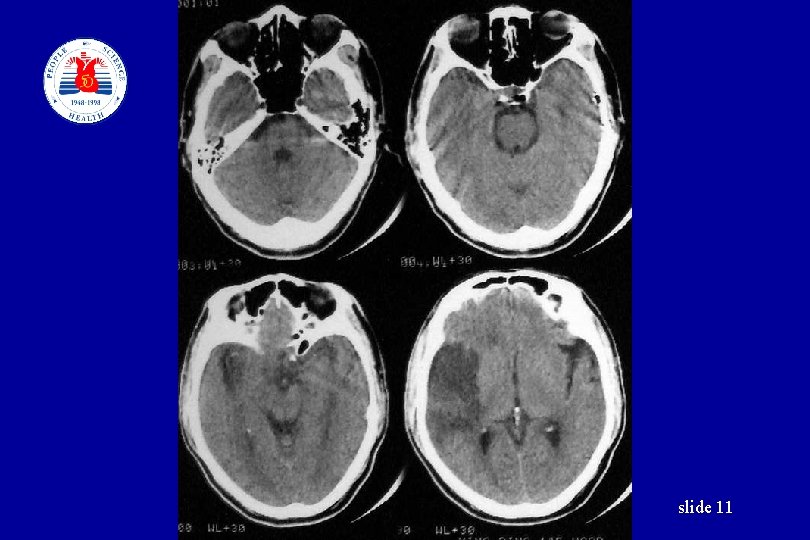
slide 11
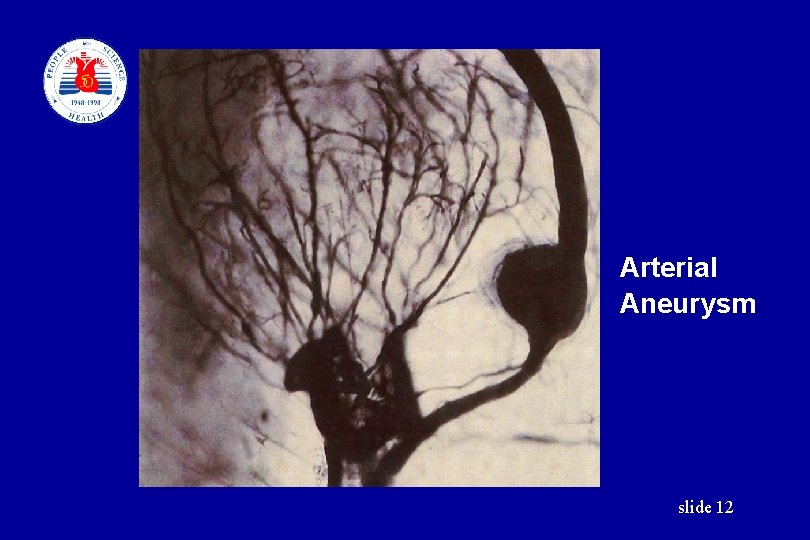
Arterial Aneurysm slide 12
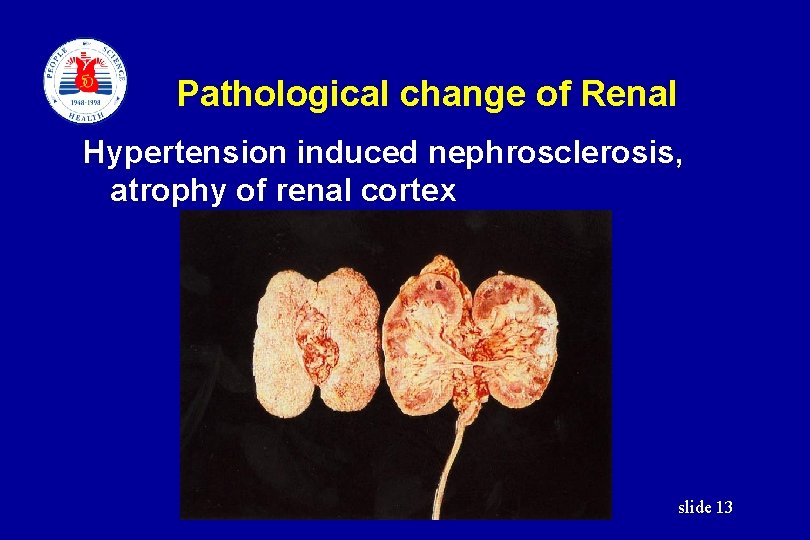
Pathological change of Renal Hypertension induced nephrosclerosis, atrophy of renal cortex slide 13

Clinical Features • The blood pressure varies widely over time, depending on many variables, including SNS activity, posture, state of hydration, and skeletal muscle tone. • Symptoms: Always asymptomatic Symptoms often attributed to hypertension: headache, tinnitus, dizziness, fainting slide 14

Clinical Features • Complications of Hypertension Heart: LVH, CAD, HF Brain: TIA, Stroke Renal: Microalbuminuria, renal dysfunction Ratinopathy slide 15

Laboratory Examination • Blood pressure measurement: Clinic Blood Pressure Home Blood Pressure Ambulatory monitoring slide 16

Ambulatory Measurement • Ambulatory monitoring can provide: – readings throughout day during usual activities – readings during sleep to assess nocturnal changes – measures of SBP and DBP load – Exclude white coat or office hypertension • Ambulatory readings are usually lower than in clinic (hypertension is defined as > 135/85 mm Hg) slide 17

Laboratory Examination • • • Urinalysis Blood examination Chest X Ray EKG UCG (Ultrasound cardiography) Retina examination slide 18
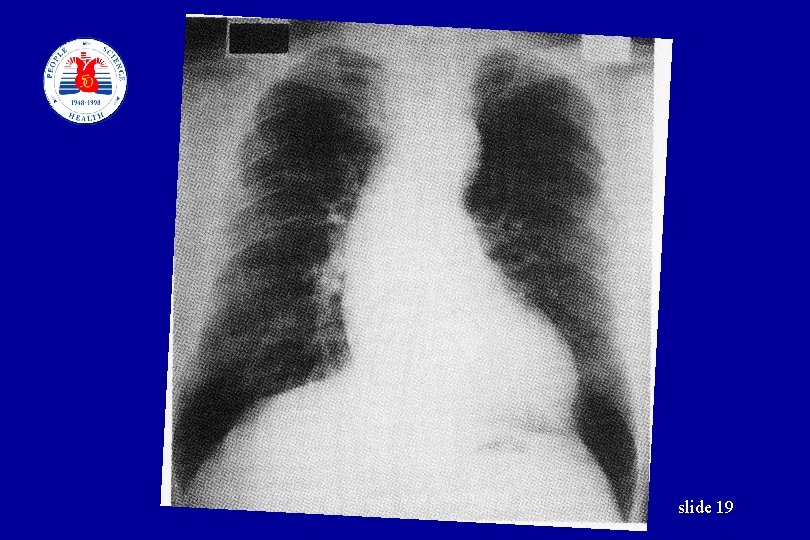
slide 19
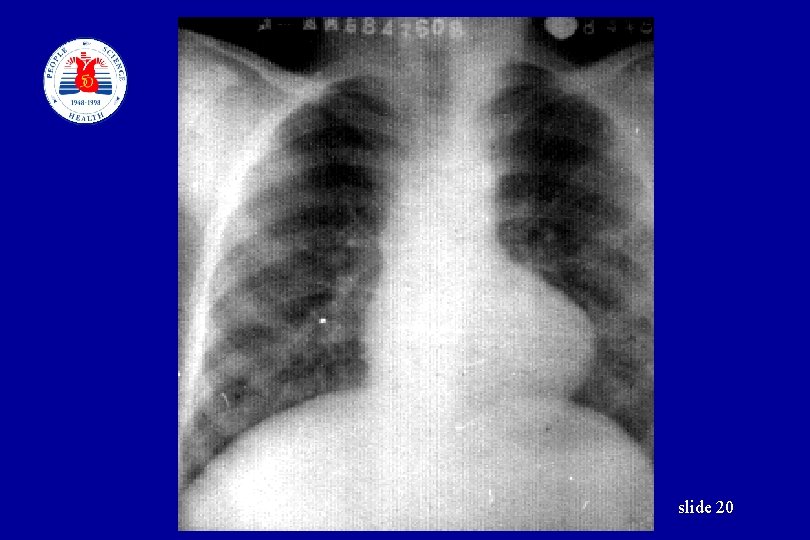
slide 20
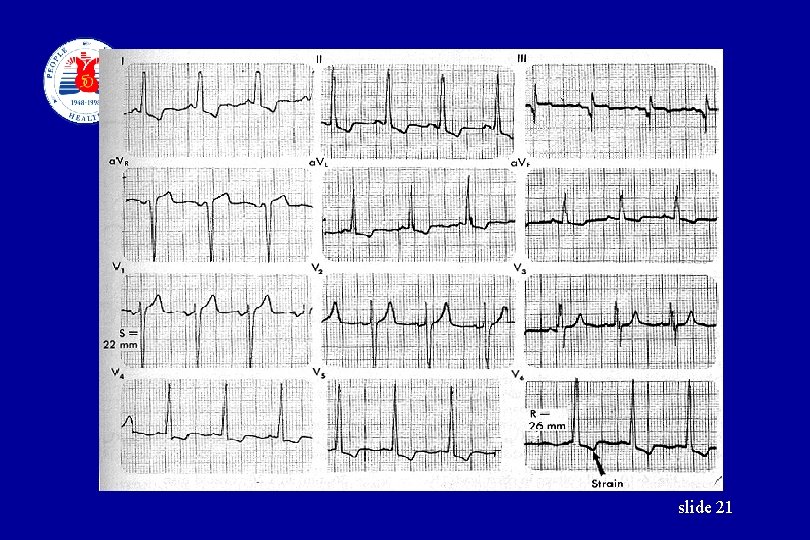
slide 21
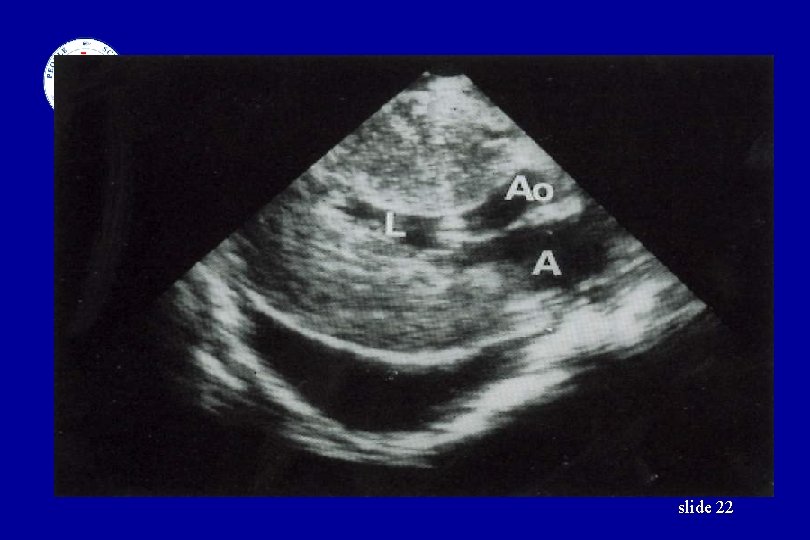
slide 22

The Keith-Wagner Criteria (change in retina) KW I: Minimal arteriolar narrowing, irregularity of the lumen, and increased light reflex KW II: More marked narrowing and irregularity with arteriovenous nicking (crossing defects) KW III: Flame-shaped hemorrhages and exudates in addition to above arteriolar changes KW IV: Any of the above with addition of papilledema slide 23
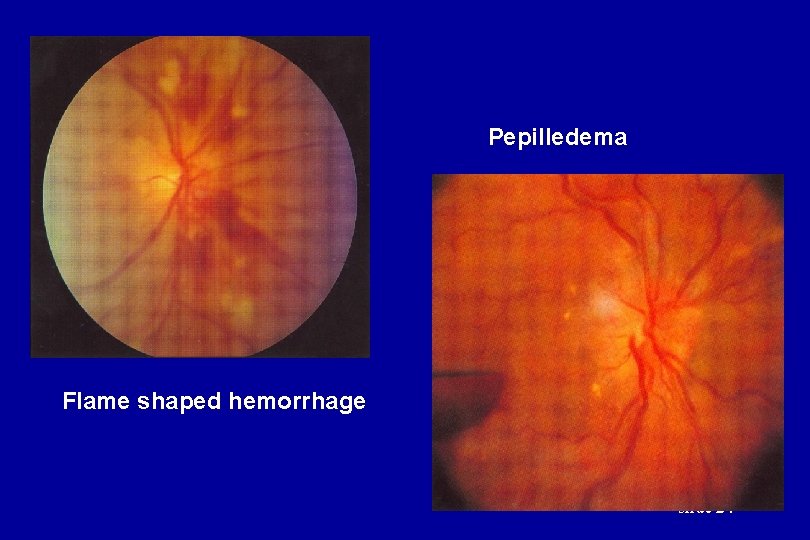
Pepilledema Flame shaped hemorrhage slide 24

Diagnosis & Differential Diagnosis slide 25
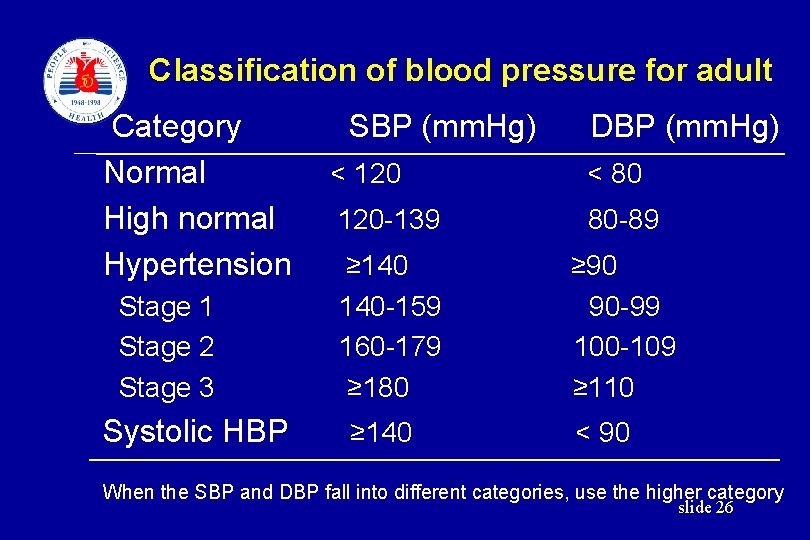
Classification of blood pressure for adult Category SBP (mm. Hg) DBP (mm. Hg) Normal < 120 < 80 High normal 120 -139 80 -89 Hypertension ≥ 140 ≥ 90 Stage 1 140 -159 90 -99 Stage 2 160 -179 100 -109 Stage 3 ≥ 180 ≥ 110 Systolic HBP ≥ 140 < 90 When the SBP and DBP fall into different categories, use the higher category slide 26
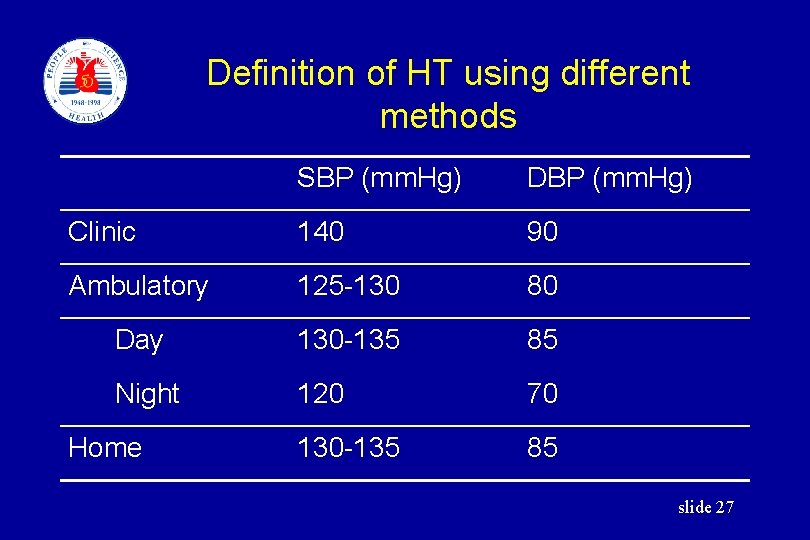
Definition of HT using different methods SBP (mm. Hg) DBP (mm. Hg) Clinic 140 90 Ambulatory 125 -130 80 Day 130 -135 85 Night 120 70 Home 130 -135 85 slide 27
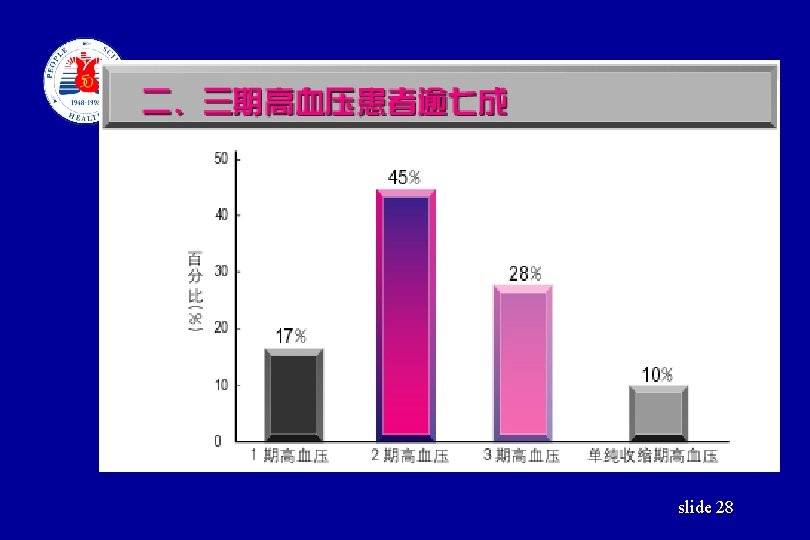
slide 28

Evaluation Components • Medical history • Physical examination • Routine laboratory tests slide 29

Physical Examination • Blood pressure readings (2 or more) • Height, weight, and waist circumference • Examination of the neck, heart, lungs, abdomen, and extremities • Neurological assessment slide 30

Laboratory Tests Recommended Before Initiating Therapy • Urinalysis • Complete blood count • Blood biochemistry (potassium, sodium, calcium, creatinine, and fasting glucose) • Lipid profile (total cholesterol and HDL cholesterol) • 12 -lead electrocardiogram • Chest X Ray slide 31

Evaluation Objectives • To identify cardiovascular risk factors • To assess presence or absence of target organ damage • To identify associated clinical condition • To identify other causes of hypertension These evaluation may used in stratification of the hypertension patients slide 32

Cardiovascular Risk Factors • • Blood pressure Age Gender Dyslipidemia Abdomen Obesity Family History of cardiovascular disease CRP ≥ 1 mg/dl slide 33

Target Organ Damage • • Left ventricular hypertrophy Echo shows IMT of carotid artery Plasma creatinine slight elevation Microalbuminuria slide 34

Associated Clinical Condition • Cerebrovascular diseases: Stroke, TIA • Heart diseases: MI, AP, CHF, Coronary artery revasculation • Kidney diseases: DN, Dysfunction of the kidney, Proteinuria, CRF • Diabetes • Peripheral artery disease • Retinopathy slide 35

Stratification of Individual Risk slide 36

Stratification of Risk to Quantity Prognosis • Risk stratification (typical 10 years risk of stroke or myocardial infarction ) Low risk = less than 15% Medium risk = about 15 -20% High risk = about 20 -30% Very high risk = 30% or more slide 37
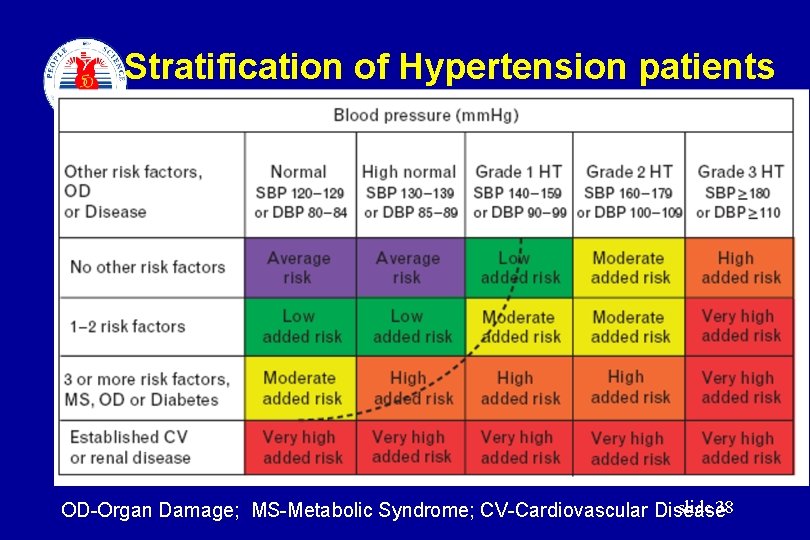
Stratification of Hypertension patients slide 38 OD-Organ Damage; MS-Metabolic Syndrome; CV-Cardiovascular Disease

Differential Diagnosis Should exclude Secondary Hypertension slide 39

Secondary Hypertension Common Causes • Renal Dysfunction Glomerulonephritis Pyelonephritis Obstructive nephropathy Collagen diseases, Congenital diseases Diabetes nephropathy Renal tumor---- renin secreting tumor • Phenochromocytoma • Primary aldosteronism slide 40

Phenochromocytoma • • • Ganglion-neurotomas and neuroblastomas Excretion of large amounts of catecholamines 90% arise in the adrenal medulla 10% are malignant. Paroxymal or persist HT Clinic features: Headache, sweating, palpitations, nervousness, weight loss, hypermetabolism, orthostatic hypotension, severe presser response slide 41

Primary Aldosteronism • • • Mild or moderate hypertension Hypokalemia, muscle weakness, paralysis Polyuria, nocturia and polydipsia, Hypochloremic alkalosis Urine aldosterone elevation Plasma renin active decrease slide 42

Secondary Hypertension Other Causes • • • Sleep Obstructive Apnea Syndrome Renal artery stenosis Cushing’s syndrome Coarctation of the aorta Drug-induced: NSAIDs; Sympathomimetic medications; Epogen Monoamine oxidase inhibitors; Mineralocorticoids; Immuno-inhibitors; slide 43

Therapy slide 44

Goal of Hypertension Management • < 140/90 mm Hg • With Diabetes or kidney dysfunction: <130/80 mm. Hg – To reduce morbidity and mortality of cerebral and cardiovascular complications. slide 45

Algorithm for Treatment of Hypertension patient Lifestyle Modifications Not at Goal Blood Pressure Initial Drug Choices slide 46
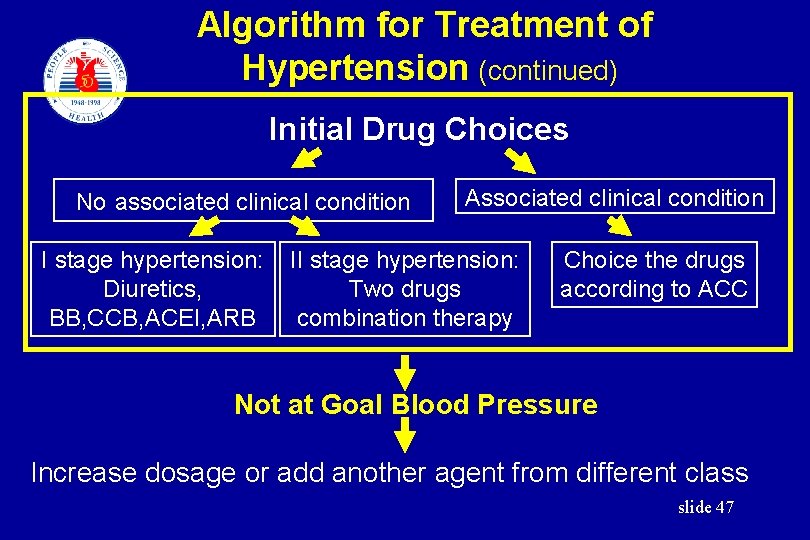
Algorithm for Treatment of Hypertension (continued) Initial Drug Choices No associated clinical condition Associated clinical condition I stage hypertension: II stage hypertension: Diuretics, Two drugs BB, CCB, ACEI, ARB combination therapy Choice the drugs according to ACC Not at Goal Blood Pressure Increase dosage or add another agent from different class slide 47
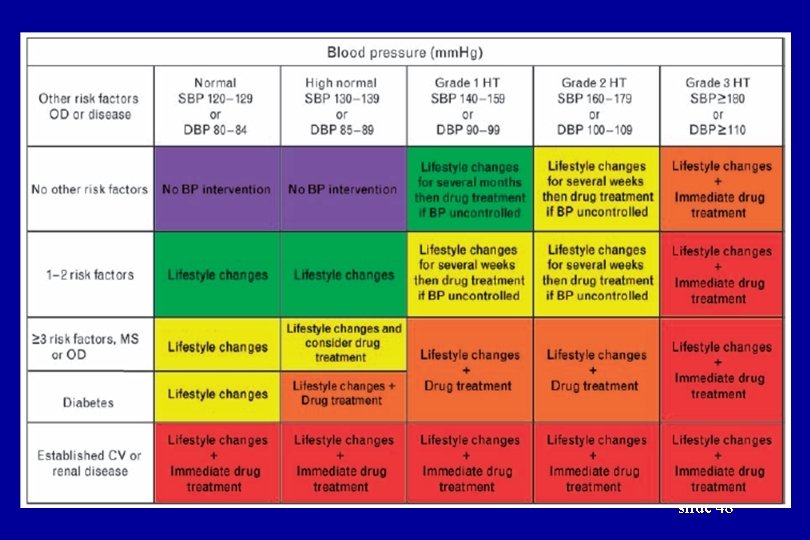
slide 48

Lifestyle Modifications • • • Stop smoking Limit alcohol intake Lose weight and keep fit Suitable diet Increase aerobic physical activity Decrease psychological stress slide 49

Principle of Drug Therapy • Drug therapy should be individually • A low dose of initial drug therapy • Combination therapies may provide additional efficacy with fewer adverse effects. • Optimal formulation should provide 24 -hour efficacy with once-daily dose. slide 50

Antihypertensive Drugs • Diuretics • • ß-Adrenergic receptor blockers (BB) Calcium channel blockers (CCB) ACE inhibitors (ACEI) Angiotensin II receptor blockers (ARB) slide 51

Diuretics Adverse effect • • • Hypokalemia Hyperurecemia Hyperlipidemia Hyperglycemia and insulin resistance Should be used in renal dysfunction patient with caution slide 52

ß-Adrenergic Receptor Blockers • • Reduce heart rate, decreased cardiac output. Inhibited renin released Can be used in all degrees hypertension Reduce the mortality of cardiovascular accident • May reverse left ventricular hypertrophy • May improve clinical outcomes in patients with congestive heart failure slide 53

Adverse Effects of ß -Adrenergic Receptor Blockers • Fatigue, limbs cold • Should not be used in patient with asthma , COPD, decompensated CHF, heart block and sick sinus syndrome, peripheral artery disease. • Should be used with caution in insulindependent diabetes • May influence glucose and lipid metabolism slide 54

Calcium Channel Blocker (CCB) • • Primarily arteriolar dilators CCB uniformly reduce vascular resistance Similarly effective and safe Mono-therapy response rates from 55% to 84% in all age ranges • Without altering glucose tolerance or lipid levels. slide 55

Adverse effect of CCB The side effects related to vasodilation: • Headache • Flushing in face • Ankle edema slide 56

ACEI Side effects • • • A dry cough seen in as many as 20% of patients Hypotension Hyperkalemia Functional renal insufficiency Angioneurotic edema Should not be used in renal artery stenosis, severe renal failure, severe aortic valve stenosis, HISS patients slide 57

Angiotensin II Receptor Blockers (ARB) • Selectively block the AT 1 receptors • The efficacy is similar to ACEI • Side effect is very slight slide 58

ACEI & ARB Should be used in patient with: • • Left ventricular hypertrophy Myocardiac infarction Heart failure Early stage of Renal dysfunction slide 59
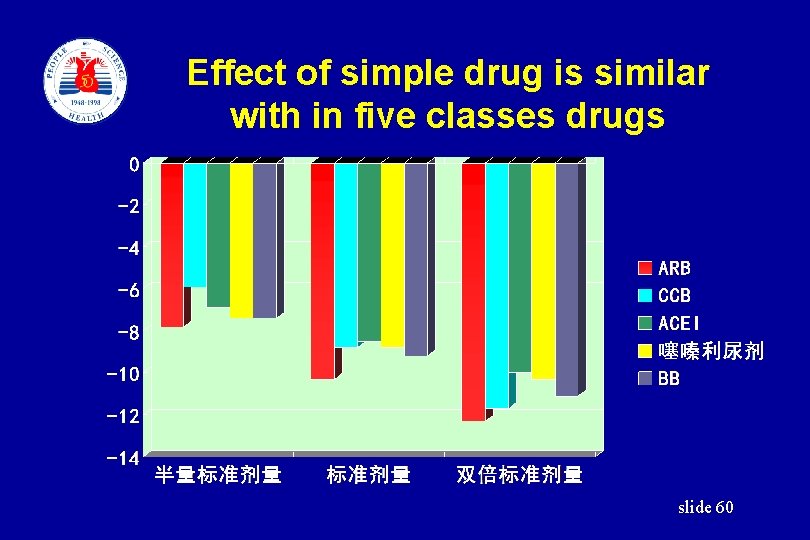
Effect of simple drug is similar with in five classes drugs slide 60

Combination Therapies • May provide additional efficacy with fewer adverse effects. • In our country, Diuretics and CCB was used as the basement drug in combination therapy. • Others: Three drugs combination slide 61
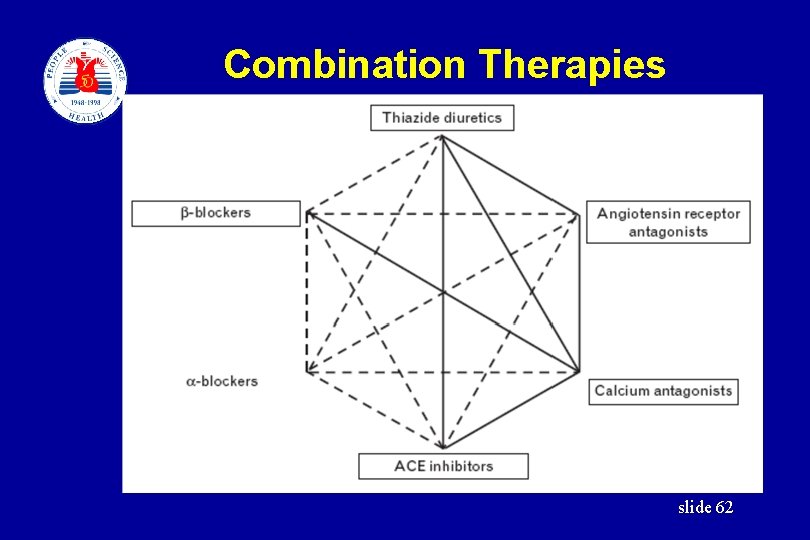
Combination Therapies slide 62
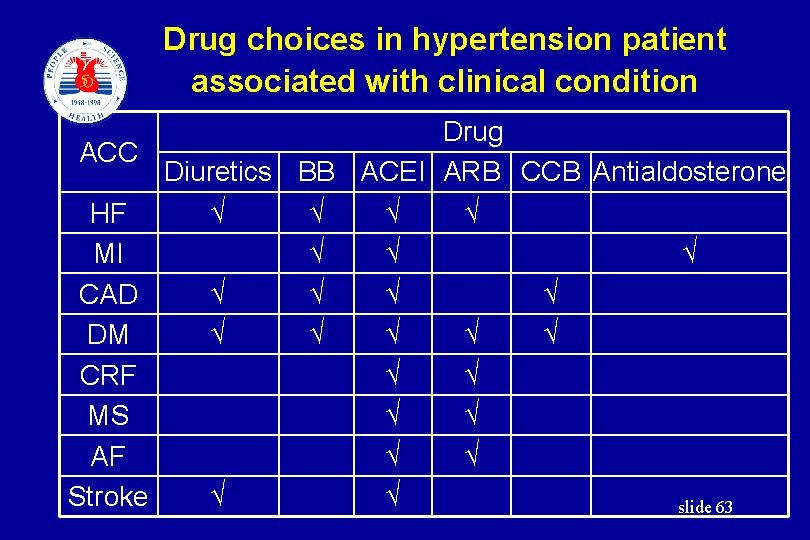
Drug choices in hypertension patient associated with clinical condition Drug ACC Diuretics BB ACEI ARB CCB Antialdosterone √ √ HF √ √ √ MI √ √ CAD √ √ √ DM √ √ CRF √ √ MS √ √ AF √ √ Stroke slide 63

Causes for Inadequate Response to Drug Therapy • Incorrect measurement of the BP • Volume overload or Pseudo-resistance • Drug-related causes • Associated conditions slide 64

Hypertensive crisis • Hypertensive Emergencies and Urgencies • Emergencies: The blood pressure is elevated severely and associated with target organ damage, such as hypertensive encephalopathy, AMI, pulmonary edema, require immediate blood pressure reduction. • Urgencies: The blood pressure is elevated severely but no target organ damage has acute target organ damage. • Fast-acting drugs are available. slide 65

Drugs Available for Hypertensive Crisis Vasodilators Adrenergic Inhibitors • Nitroprusside • Labetalol • Nicardipine • Esmolol • Nitroglycerin • Phentolamine slide 66

Case 1 Male, 40 yrs Found BP elevated (135/95 mm. Hg) during physical examination three days ago. What shill we do? slide 67

Medical history; Family history Physical examination: measure BP, heart sound, etc. Laboratory test: exclude secondary HT Finishing evaluation of the patient Does the patient need drug therapy? slide 68

Case 2 Male, 65 yrs, Have acute myocardiac infarction for one week. Have diagnosed with HT for 10 yrs, therapy with CCB, and now the BP was 150/80 mm. Hg. How to treat his HT? slide 69

Evaluated the heart function and combining disease such as DM, renal function etc. Choose ACEI, ARB or BB slide 70

Case 3 Male 29 years old Blood pressure elevated for two years With paroxysmal dizziness, blurred vision, sweating and palpitation BP: 160 -180/90 -100 mm. Hg HR: 100 -120 bpm When the patient with symptoms, the BP would elevate to 240 -260/120 -130 mm. Hg, and HR increase to 130 -150 bpm. slide 71

Physical examination: BP: 165/100 mm. Hg HR: 112 bpm No positive sign in chest examination Can find a mass at right abdomen, if press on it the BP of the patient elevated to 250/120 mm. Hg, and the HR increased to 145 bpm. slide 72

Laboratory test: Blood routine, Urinalysis, Blood biochemistry are normal Plasma renine activation: 0. 93 ng/ml. h (0. 93 -6. 56) AT II: 51. 5 pg/ml ↓ (55. 3 -115. 3) Aldosterone: 129. 4 pd/ml (63 -239. 6) NE: 33. 40 pmol/ml ↑↑ (0. 51 -3. 26) 12 -lead electrocardiogram: High voltage of LV Chest X ray: Normal slide 73
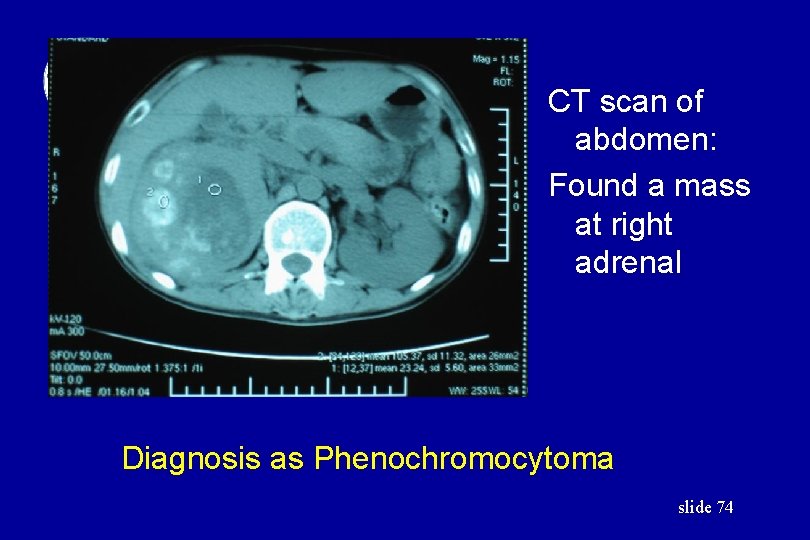
CT scan of abdomen: Found a mass at right adrenal Diagnosis as Phenochromocytoma slide 74

Case 4 Male, 56 yrs, Severe chest pain for five hours, sweating, Physical examination: BP 165/110 mm. Hg, HR 78 bpm EKG: normal slide 75
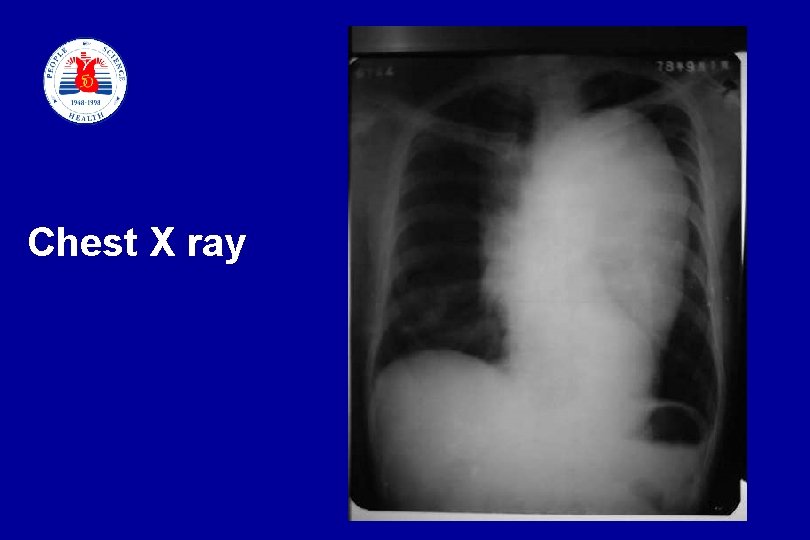
Chest X ray slide 76
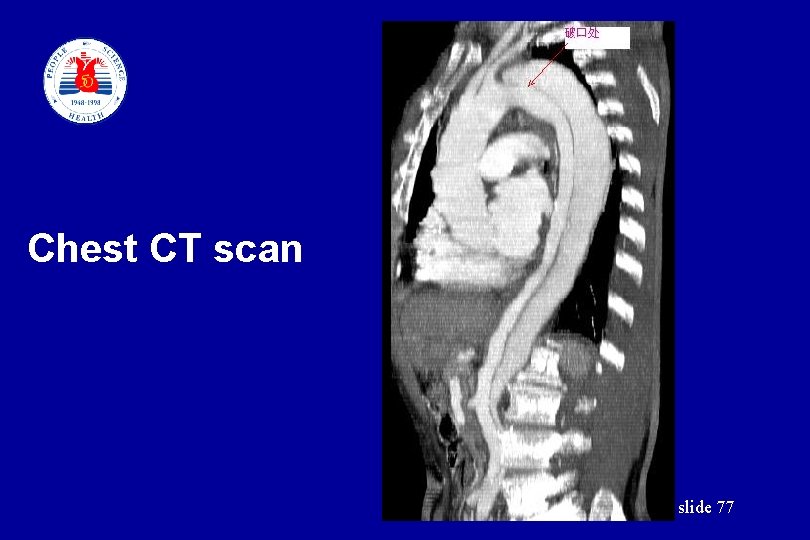
Chest CT scan slide 77
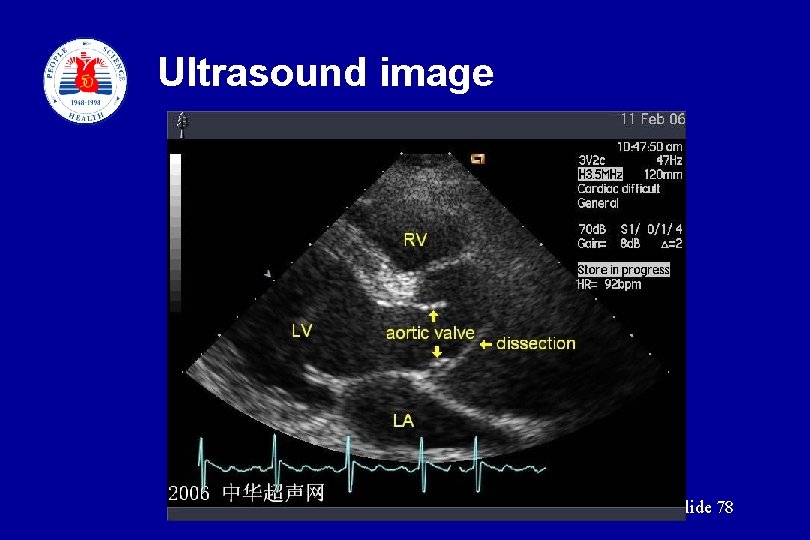
Ultrasound image slide 78

Therapy: control the BP between 100 -120/70 mm. Hg, the lower the better slide 79
Case 5 Male, 68 years old Hypertension history for 30 years Headache, blurred vision, vomiting for 2 hours Paralysis of left side body BP: 220/130 mm. Hg HR: 106 bpm CT scan of the head: Normal slide 80

Diagnosis: Hypertensive crisis Therapy: Controlled the BP, using fast-acting drug,such as Nitroprusside, Labetalol The reduction of BP should less than 25% in 24 hours BP ≥ 160/100 mm. Hg in 48 hours slide 81

Summary 1 • Definition and stratification of HT • Pathological changes of HT (brain, heart, kidney, arteries) • Specific therapy for patients with LVH, CAD, and HF. ACEI can be used for all type patients. • In older persons, diuretics and CCB are preferred. • Many patients need combination therapy. slide 82

Summary 2 • Goal of Hypertension therapy: <140/90 mm. Hg • Goal of the patients with renal insufficiency with proteinuria (>1 g/day): <125/75 mm. Hg; (< 1 g/day): <130/80 mm. Hg. • Goal of the patients with diabetes: <130/80 mm Hg. slide 83
- Slides: 82