Hypertension Definition Hypertension is that level of sustained
















- Slides: 24

Hypertension Definition: Hypertension is that level of sustained systemic arterial pressure which results over time in end-organ damage, most commonly in the eyes, the brain, the heart, the kidneys and the vasculature. Incidence in US: - among induvidualis over the age of 35 years : 20 -25% - over 60 years: 35 -40%

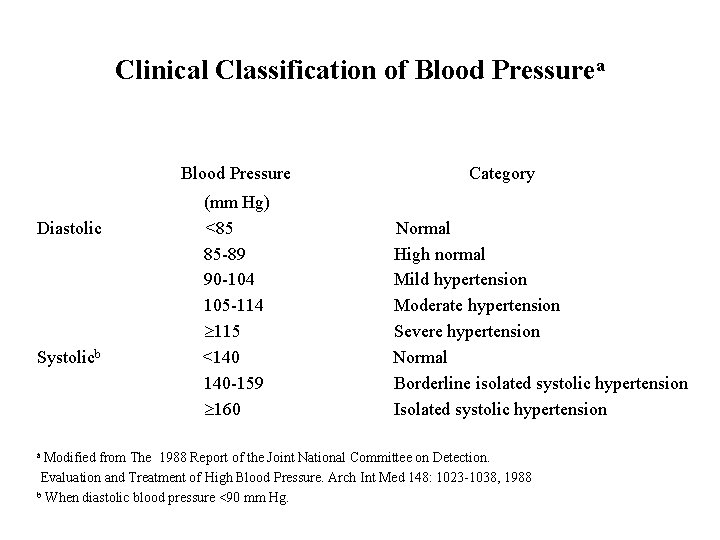
Clinical Classification of Blood Pressurea Blood Pressure Diastolic Systolicb a Modified (mm Hg) <85 85 -89 90 -104 105 -114 115 <140 140 -159 160 Category Normal High normal Mild hypertension Moderate hypertension Severe hypertension Normal Borderline isolated systolic hypertension Isolated systolic hypertension from The 1988 Report of the Joint National Committee on Detection. Evaluation and Treatment of High Blood Pressure. Arch Int Med 148: 1023 -1038, 1988 b When diastolic blood pressure <90 mm Hg.

Etiology 90 -95% cause: of hypertension in adults has no indentifiable primary or essential 5 -10% Secondary

Principal Causes of Hypertension I. 1. 2. Idiopathic (essential, primary) Renal A. Renovascular stenosis 1. Fibromuscular dysplasia 2. Atherosclerotic B. Renal parenchymal disease C. Obstructive nephropathy

Principal Causes of Hypertension II. Adrenal A. Medullary-pheochromocytoma B. Cortical 1. Primary aldosteronism a. Adrenal adenoma b. Bilateral adrenal hyperplasia 2. Cushing’s disease

Principal Causes of Hypertension III. Exogenous agents A. Oral contraceptives B. Sympathetic amines ( decongestants ) C. Nonsteroidal anti-infammatory drugs D. High dose corticosteroid administration E. Disorders simulating mineralocorticoid excess 1. Licorice 2. Chewing tobacco

Principal Causes of Hypertension IV. Miscellaneous A. Coarctation of aorta B. Acute stress

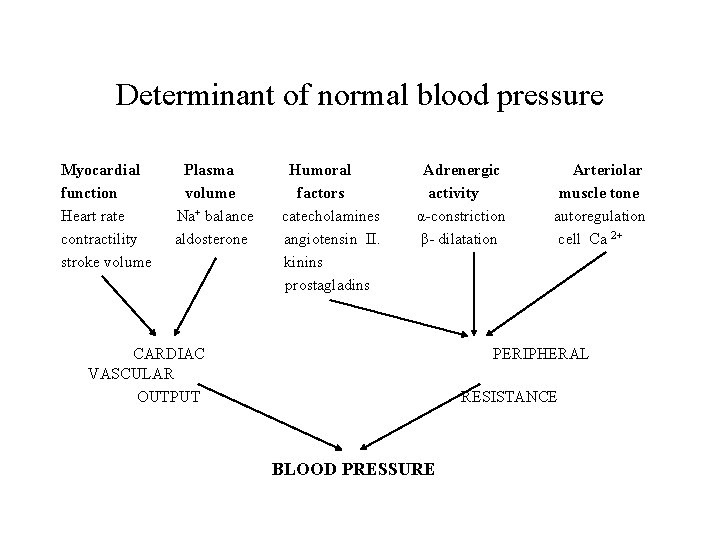
Determinant of normal blood pressure Myocardial function Heart rate contractility stroke volume Plasma volume Na+ balance aldosterone Humoral factors catecholamines angiotensin II. kinins prostagladins Adrenergic activity α-constriction β- dilatation CARDIAC VASCULAR OUTPUT Arteriolar muscle tone autoregulation cell Ca 2+ PERIPHERAL RESISTANCE BLOOD PRESSURE

Pathogenetic Mechanisms in Secondary Hypertension Disorder Mediators Pathophysiologic Mechanisms Pheochromocytoma Catecholamines Primary aldosteronism Renal artery stenosis Aldosterone Renin a Aldosterone GFR Renin a Cortisol Renin substrate Estrogen Renin Aldosterone Vasocontriction Cardiac output Na+ retention Vasoconstriction Na+ retention Vasoconstriction Na+ retention Renal insufficiency Cushing’s syndrome Oral contraceptives Aortic coarctation a A minority of cases.

Essential Hypertension ( EH ) Thirty years ago, Page coined the term hypertension „mosaic”; his notion regarding the heterogeneity of hypertension remains highly relevant today. Factors contributing to the development of EH: 1. Systemic hemodynamics 2. Plasma volume 3. Renin-angiotensin system 4. Sympathetic nervous system 5. Kidney 6. Dietary factors sodium, calcium, potassium, obesity, alcohol 7. Heredity 8. Race

Effect of volume expansion on mean arterial pressure, cardiac output, and systemic vascular resistance in an anephric 22 -year-old women From T. G. Coleman, H. J. Granger, and A. C. Guyton, Circ. Res. , 28 (suppl. 2): 76, 1971

Inverse relationship between plasma volume (in: milliliters per centimeter of height) and diastolic blood pressure in untreated men with essential hypertension From H. P. Dustan, R. C. Tarazi, E. L. Bravo, and R. A. Dart, Circ. Res. , 32 (suppl. 1): 73, 1973.

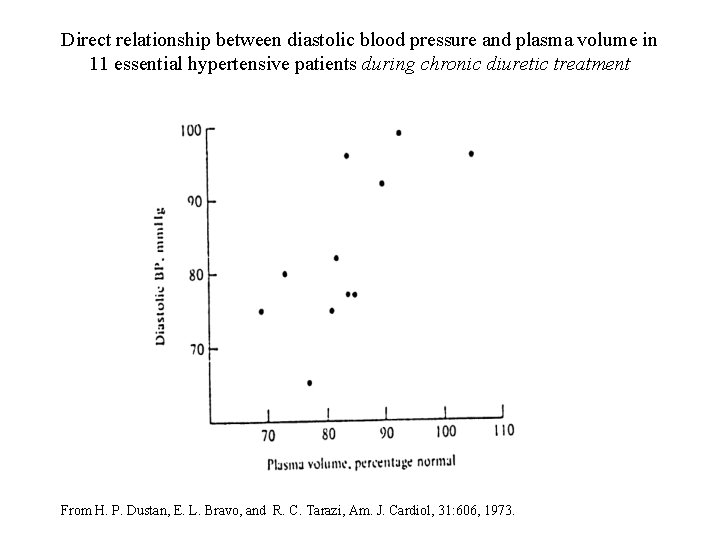
Direct relationship between diastolic blood pressure and plasma volume in 11 essential hypertensive patients during chronic diuretic treatment From H. P. Dustan, E. L. Bravo, and R. C. Tarazi, Am. J. Cardiol, 31: 606, 1973.

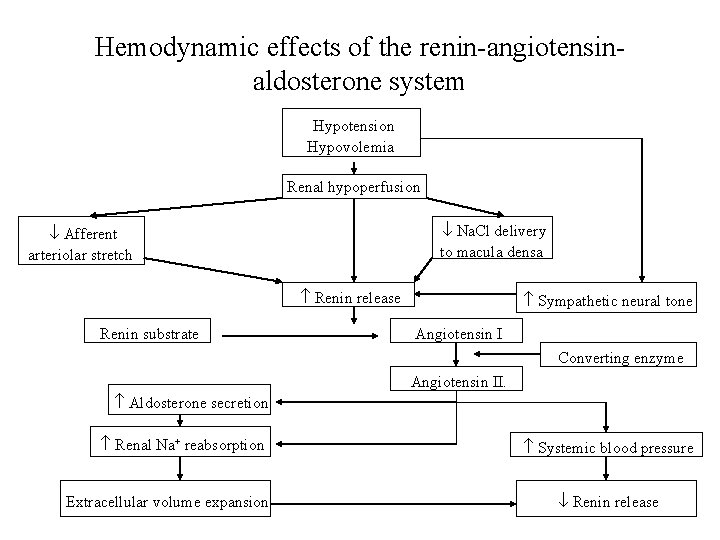
Hemodynamic effects of the renin-angiotensinaldosterone system Hypotension Hypovolemia Renal hypoperfusion Na. Cl delivery to macula densa Afferent arteriolar stretch Renin release Renin substrate Sympathetic neural tone Angiotensin I Converting enzyme Angiotensin II. Aldosterone secretion Renal Na+ reabsorption Extracellular volume expansion Systemic blood pressure Renin release

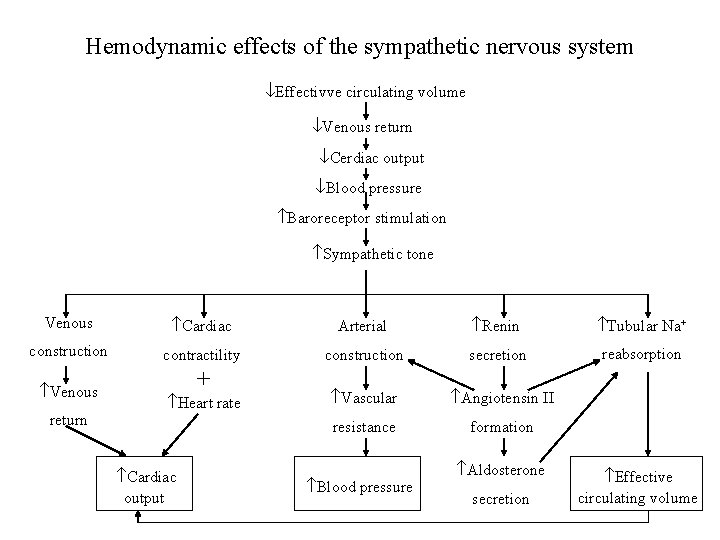
Hemodynamic effects of the sympathetic nervous system Effectivve circulating volume Venous return Cerdiac output Blood pressure Baroreceptor stimulation Sympathetic tone Venous Cardiac Arterial Renin Tubular Na+ construction contractility construction secretion reabsorption Vascular Angiotensin II resistance formation Venous return + Heart rate Cardiac output Blood pressure Aldosterone secretion Effective circulating volume

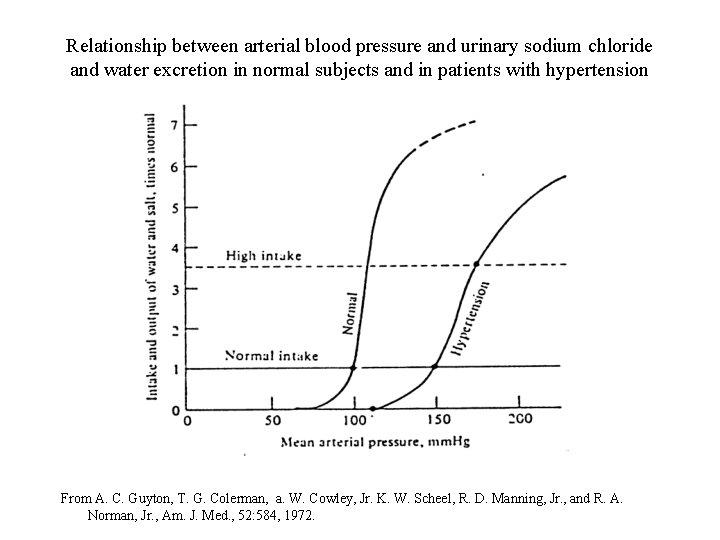
Relationship between arterial blood pressure and urinary sodium chloride and water excretion in normal subjects and in patients with hypertension From A. C. Guyton, T. G. Colerman, a. W. Cowley, Jr. K. W. Scheel, R. D. Manning, Jr. , and R. A. Norman, Jr. , Am. J. Med. , 52: 584, 1972.

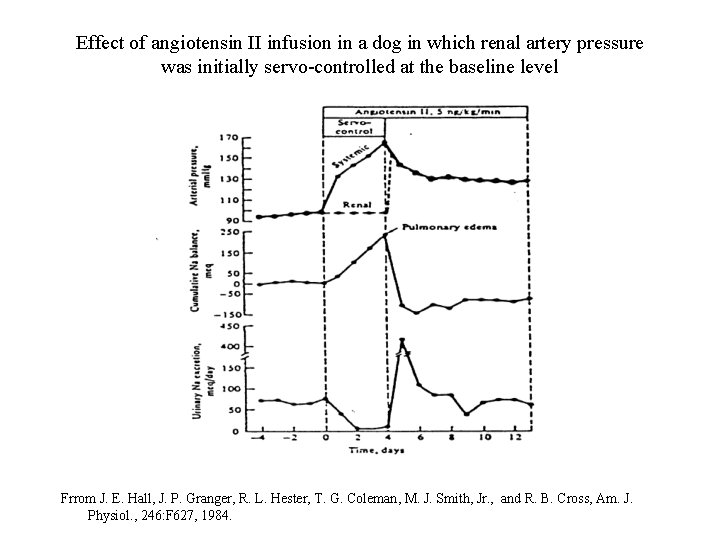
Effect of angiotensin II infusion in a dog in which renal artery pressure was initially servo-controlled at the baseline level Frrom J. E. Hall, J. P. Granger, R. L. Hester, T. G. Coleman, M. J. Smith, Jr. , and R. B. Cross, Am. J. Physiol. , 246: F 627, 1984.

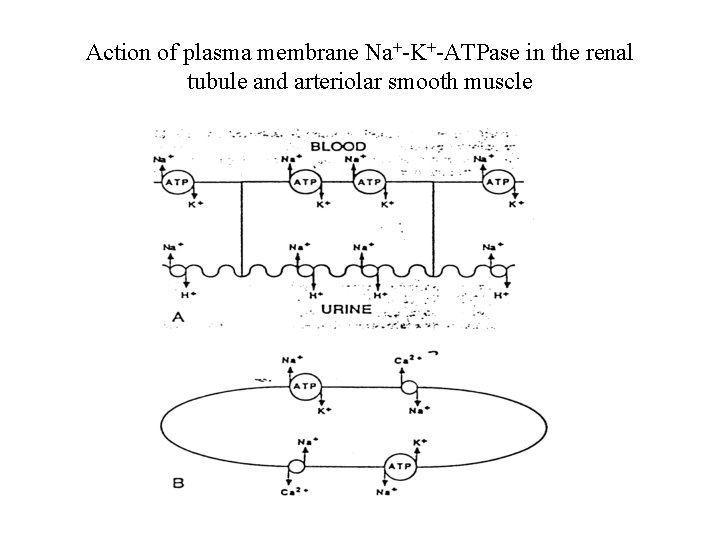
Action of plasma membrane Na+-K+-ATPase in the renal tubule and arteriolar smooth muscle

Correlation between mean arterial pressure and intracellular free calcium concentration in platelets From P. Erne, P. Bolli, E. Burgisser, and F. R. Buhler, N. Engl. J. Med. , 310: 1084, 1984.

Calcium The prevalence of EH appears to inversaly relates to dietary calcium intake with the risk rising two to three times as daily Ca intake falls from 1200 to less than 300 mg. There is, however, a direct correlation between mean arterial pressure and intracellular free calcium. Mechanism (? ): Contradiction: extracellular Ca++ intracellular Ca++ Hypocalcemia could promote intracellular Ca cummulation (? )

Potasium In humans with EH K supplementation has been shown to produce a moderate fall in BP averaging 5 to 6 mm. Hg. Mechanism(? ): - it acts mainly in Na sensitive patients - it may act in part by enhancing urinary sodium excretion

Obesity The incidence of hypertension is increased in obese patients - increase in plasma volume - sympathetic activity enhanced - SVR higher - insulin resistance increased Na retention ( insulin increase Na-K-ATP ase activity, increased insulin resistance and secretion Na-KATP ase )

Alcohol 1 or 2 drink a day 1. 5 to 2 times as likely to become hypertensive Mechanism: plasma volume ; NE ; renin ; Na-excretion

Others Smoking, coffeine (? ) Heredity and Race 70 -80 % of patients with EH have a positive family history Correlation's within families between parents and children's medium, identical twins, (high) adopted children (low)