Hyperglycemic emergencies in adults Diabetic Ketoacidosis Nonketotic Hyperglycemia



Hyperglycemic emergencies in adults Diabetic Ketoacidosis & Nonketotic Hyperglycemia Dr. Saeed Kalantari Professor of Endocrinology & Internal Medicine Razi Endocrine & metabolic department

Pathogenesis of DKA: § Absolute lack of insulin § Glucagon excess § Increased counter-regulatory hormones

Pathogenesis of NKH: § Relative insulin deficiency § Increased counter-regulatory hormones § Severe dehydration

Lipogenesis: § Glucose § Pyrovic acid § Acetyl Co. A Insulin activates Acetyl Co. A carboxylase § Malonyl Co. A § FA Glucagon inhibits

Ketogenesis: § FA + Co. A § Acetyl Co. A CPT 1 Carnitin § Carnitine Co. A CPT 2 § Acetyl Co. A B-oxydation § Keton body
Acetyl Co. A metabolism Pyrovic Acid Acetyl Co. A ATP FAT Gluconeogensis Ketons

Precipitating factors: § § § Infection Myocardial infarction Pregnancy Trauma Insulin under dose Drugs

Precipitating factors: § § § § SGLT 2 inhibitors Cocaine use Alcohol abuse Cushing Acromegaly Pancreatitis CVA

1 -Infection: The most common cause of DKA: § Urinary tract § Pneumonia § Acute abdomen

2 - Myocardial infarction: § Might be silent in elderly § Must be sought as a cause of DKA in elderly § Extreme epinephrine release

3 - Pregnancy: In the second half of pregnancy § HPL increased § Insulin resistancy

Pregnancy: § BHCG should be measured routinely in evaluating poor control or DKA in young diabetic women

4 - Drugs: § § § Glucocorticoids Diuretics Phenytoin Conventional & atypical antipsychotics OCP

Precipitating factors Patients with undiagnosed acromegaly may present with DKA as the primary manifestation of their disease

Clinical presentation: In DKA: § Symptoms of poor controlled DM for several days § But sign & symptoms of DKA evolve in <24 h

Clinical presentation: In NKH: § Symptoms evolves in several days to weeks

Clinical presentation: § § § § Polyuria Polydipsia Malaise Nausea Vomiting Ab. Pain* Ab. tenderness

Clinical presentation: § § § Kussmaul breathing Fruity breath Dehydration Hypotension Confusion Coma*

Clinical presentation: § Hypothermia (despite severe sepsis) § Dyspnea due to: acidosis myocardial infarction pneumonia
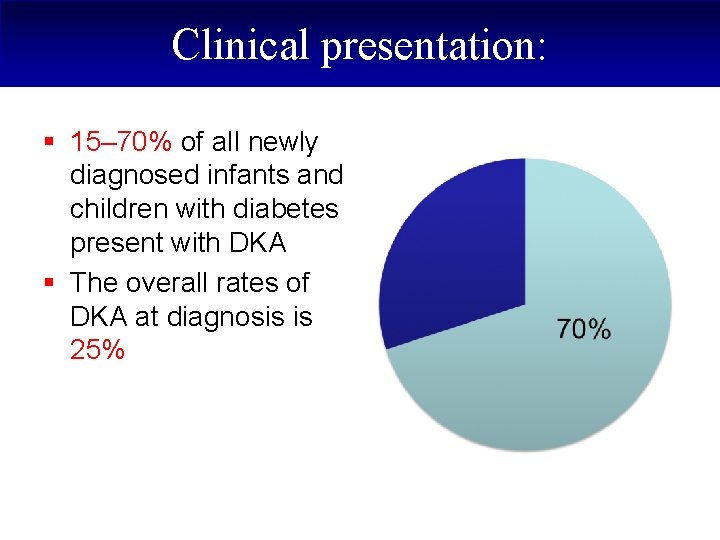
Clinical presentation: § 15– 70% of all newly diagnosed infants and children with diabetes present with DKA § The overall rates of DKA at diagnosis is 25%

Clinical presentation: § DKA at diagnosis is more common in younger children (<5 years of age)
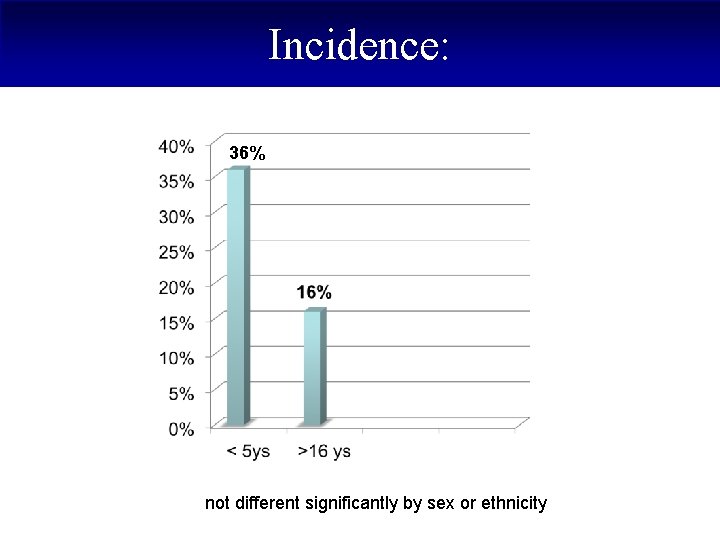
Incidence: 36% not different significantly by sex or ethnicity
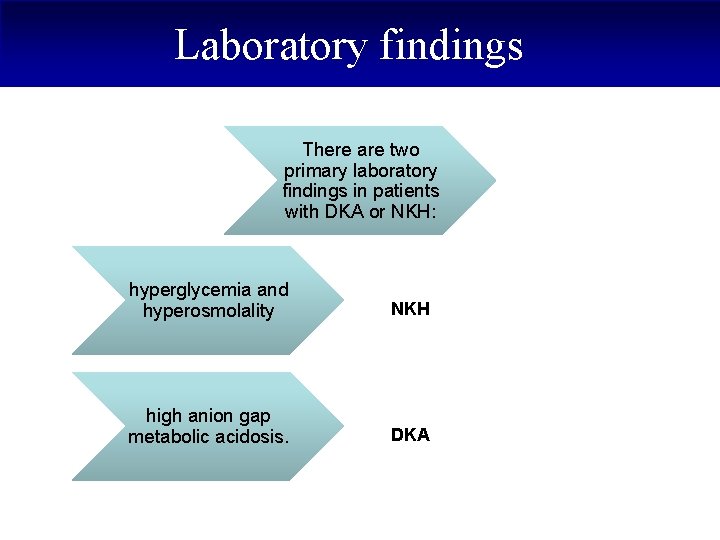
Laboratory findings There are two primary laboratory findings in patients with DKA or NKH: hyperglycemia and hyperosmolality NKH high anion gap metabolic acidosis. DKA
Plasma glucose

Plasma glucose At least two factors contribute to the lesser degree of hyperglycemia in DKA: § Patients with DKA often present early with symptoms of ketoacidosis rather than late with those of hyperosmolality.

Plasma glucose § Patients with DKA tend to be young, and to have a glomerular filtration rate that, in the first five years, may be as much as 50 percent above normal.

Plasma sodium § By raising the plasma osmolality, hyperglycemia results in osmotic water movement out of the cells, § thereby lowering the plasma sodium concentration by dilution.

Plasma sodium § The Na concentration will fall by approximately 2 m. Eq/L for each 100 mg/100 m. L (5. 5 mmol/L) increase in glucose concentration.

Plasma sodium § At glucose concentrations>400, there is a 4 meq/L reduction in plasma sodium per 100 mg/d. L further increase in plasma glucose.

Pseudohyponatremia § Some patients with uncontrolled diabetes have marked hyperlipidemia § In this setting, each liter of plasma contains less water and therefore less sodium.

Pseudohyponatremia § As a result, the measured plasma sodium concentration will fall, § though the physiologically important plasma water sodium concentration and plasma osmolality are not affected

Plasma potassium § Patients with DKA or NKH have, at presentation, a potassium deficit that averages 3 to 5 meq/kg

Plasma potassium Contributing factors: 1 - Increased urinary losses due to: § glucose osmotic diuresis § the excretion of potassium ketoacid anion 2 - Gastrointestinal losses

Plasma potassium § Despite these potassium losses, the plasma potassium concentration is usually normal or, in one-third of patients, elevated on admission.

Plasma potassium This paradoxical findings is due to: § The translocation of potassium out of the cells into the extracellular fluid.

Plasma potassium § Acidemia had been thought to play a major role in this response, § Although this transcellular exchange occurs in most forms of metabolic acidosis

Plasma potassium § it does not appear to be important in diabetic ketoacidosis. § As an example, hyperkalemia also occurs in nonketotic hyperglycemia despite the absence of ketoacidosis

Plasma potassium § Hyperosmolality and insulin deficiency are primarily responsible for the rise in the plasma potassium concentration.

Plasma potassium § The rise in plasma osmolality leads to osmotic water movement out of the cells. § This can promote the parallel movement of potassium into the extracellular fluid

Plasma potassium § The rise in the plasma potassium concentration induced by acute hyperglycemia, can be as much as 1 meq/L for every 100 mg/d. L elevation in the plasma glucose concentration
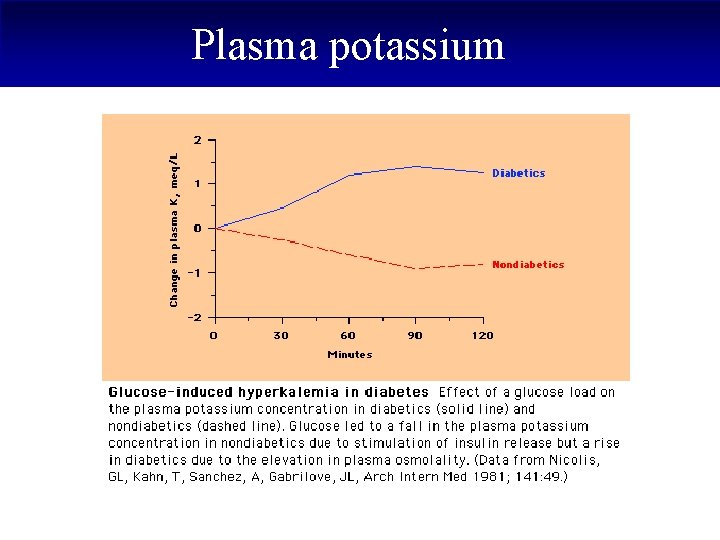
Plasma potassium

Plasma potassium § Volume depletion causes secondary hyperaldosteronism, which promotes urinary potassium excretion.

Plasma potassium § In patients with end-stage renal disease the translocation of potassium out of the cells is not counterbalanced by urinary losses disease. § Such patients can have marked hyperkalemia at presentation.

Plasma bicarbonate and anion gap § The plasma bicarbonate concentration in DKA is reduced to a variable degree, ranging from mild to severe.

Plasma bicarbonate and anion gap § In contrast, the plasma bicarbonate concentration is normal or only mildly reduced in NKH.

Plasma phosphate Negative phosphate balance because of: § decreased phosphate intake § phosphaturia caused by the glucosuriainduced osmotic diuresis.

Plasma phosphate § Despite the presence of phosphate depletion, the plasma phosphate concentration at presentation is usually normal or even high

Plasma phosphate § Because both insulin deficiency and, if present, metabolic acidosis cause a shift of phosphate out of the cells

Plasma phosphate § This transcellular shift is reversed and the true state of phosphate balance is unmasked after treatment with insulin.

Plasma amylase and lipase § Standard tests to diagnose acute pancreatitis, § but both are often elevated in patients with DKA who do not have pancreatitis.

Plasma amylase and lipase § An increase in either enzyme in DKA, even > threefold, does not make the diagnosis of acute pancreatitis in the absence of an abnormal abdominal CT scan

Plasma amylase and lipase Serum amylase can be: § pancreatic, § salivary, § or both

Diagnostic criteria for DKA A triad of: §Hyperglycemia (plasma glucose >250 mg/d. L), §High anion gap acidosis (p. H <7. 30) & Serum bicarbonate <15 -18 mmol/L §Ketonemia and ketonuria.

Diagnostic criteria for NKH A pantad of: § Marked hyperglycemia (plasma glucose >600 mg/d. L) § Minimal acidosis (p. H >7. 30) & Serum bicarbonate >15 -18 mmol/L § Absent to mild ketonemia and small ketonuria, § Effective serum osmolality >320 m. Osm/L, § Altered consciousness
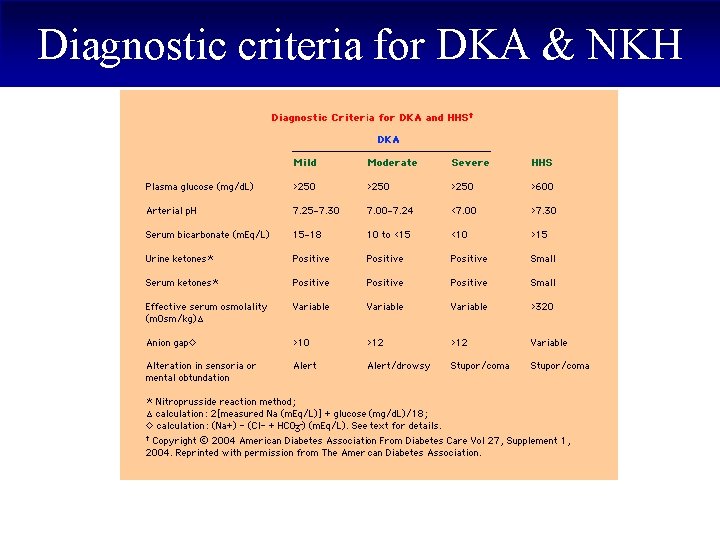
Diagnostic criteria for DKA & NKH
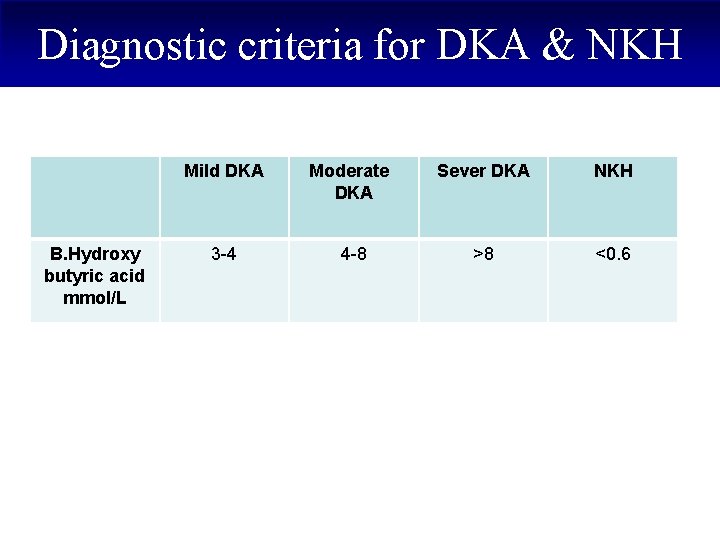
Diagnostic criteria for DKA & NKH B. Hydroxy butyric acid mmol/L Mild DKA Moderate DKA Sever DKA NKH 3 -4 4 -8 >8 <0. 6

Calculations: Correction of serum Na: § Corrected Na = measured Na + Calculation of the anion gap: § Na – (Cl + bicarbonate) § Normal AG* is 12 ± 2 Effective serum osmolality: § 2 Na + glucose (mg/dl) / 18 G / 42

Evaluation for pure metabolic acidosis: § Pco 2 = The last two numbers of the PH § Pco 2 = 1. 5 (serum HCO 3) + 8 ± 2 § A lower than predicted Pco 2 indicates respiratory alkalosis & may be a clue to sepsis.

Diagnosis 1 -Euglycemic DKA § § § Excellent hydration Increased GFR Insufficient insulin Pregnancy sodium-glucose co-transporter 2 (SGLT 2) inhibitors

Diagnosis 2 -Alklemic DKA § § Vomiting Diuretics Alkali ingestion Cushing syn.

Mixed acid-base abnormality Metabolic acidosis & metabolic alkalosis*: § PH is higher than predicted from Pco 2 = 1. 5 (serum HCO 3) + 8 ± 2 § Extreme elevation of anion gap AG = Na – (Cl + bicarbonate)

Mixed acid-base abnormality Respiratory alkalosis & metabolic acidosis: § A lower than predicted pco 2 indicated respiratory Alkalosis & sepsis Pco 2 = The last two numbers of the PH
Ketone bodies: Acetoacetic acid Acetone § chemically neutral B-OH butyric acid
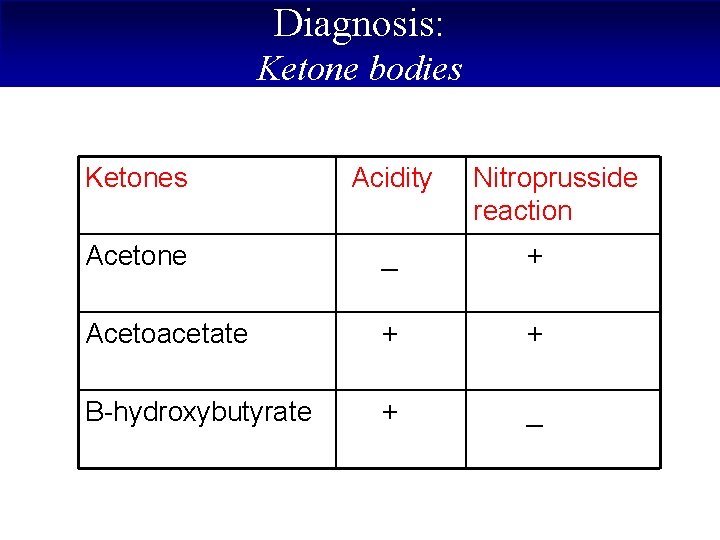
Diagnosis: Ketone bodies Ketones Acidity Nitroprusside reaction Acetone _ + Acetoacetate + + B-hydroxybutyrate + _

Diagnosis: 3 -nonketonemic. DKA Due to tissue hypoxia: § Sepsis § Hypotension § Shock

Diagnosis: nonketonemic. DKA § Acetoacetate / B – OH butyrate = 1/3 -1/5 § Increased NADH / NAD causes increased B-hydroxybutyrate production § The clue to diagnosis is increased AG

Diagnosis: nonketonemic. DKA* DKA+ weak nitroprusside test + AG : § Tissue hypoxia due to Sepsis Hypotension Shock § R/O lactic acidosis with serum lactate measurement

Diagnosis: ketonemi § A different problem in diagnosis arises with sulfhydryl drugs, particularly captopril (which also include penicillamine) § These drugs can interact with the nitroprusside reagent to produce a false positive ketone test.

Diagnosis: ketonemi In this setting, the diagnosis of DKA must be made on clinical grounds: § unexplained high anion gap metabolic acidosis in a patient with uncontrolled diabetes. Or by direct measurement of: § Beta-hydroxybutyrate.

Differential diagnosis: § 1 - Acute abdomen § 2 - Other causes of high-anion gap metabolic acidosis

Differential diagnosis: Causes of high-anion gap metabolic acidosis § § § Alcoholic ketoacidosis Starvation ketosis Uremia Lactic acidosis Intoxications: Ethylenglycol, methanol, aspirin, paraldehyde

Differential diagnosis: Alcoholic ketoacidosis & Starvation ketosis: § Clinical history § Plasma glucose mildly elevated ( rarely >200 mg/dl) or hypoglycemia

Differential diagnosis: Starvation ketosis: § Bicarbonate usually not <18 m. Eq/l

Differential diagnosis: Work up: § Hx of metformin use § Measurment of blood lactate, salicylate, methanol.

Treatment: fluid Severe dehydration: § 1 -2 L. NS in 1 st h Otherwise: § 500 -1000 cc NS /h for 4 h § 250 -500 cc ½ NS /h for 4 h § 125 -250 cc DW-5% or D 10% /h when BS < 200 in DKA & 300 mg/dl in NKH

Treatment: fluid § NS if corrected serum Na is low. § ½ NS if corrected serum Na is normal or increased.

Treatment: fluid § Should correct the deficits in 24 h in adults & 48 h in pediatrics § Changes is osmolality should not exceed 3 mosm / h (changes in Na should be<0. 5 meq /h).

Treatment: fluid D-5% or D 10% when BS <200 & <300 mg/dl until: § acidosis in DKA § mental changes & hyperosmalarity in NKH are resolved

Treatment insulin § Withhold until hypokalemia is excluded. § Insulin should be infused 1 h after k replacement ( when K < 3. 3 ).

Treatment insulin 3 ways to give insulin: § Insulin infusion, preferred (short half life, easy titration) § Frequent SQ insulin § Frequent IM insulin

Treatment insulin Mild DKA: Loading dose: § Reg 0. 3 -0. 6 U / kg, half IV & half IM or SC Maintenance: § Reg 0. 1 U /kg /h or 0. 2 units/kg /2 h § IM or SC is as effective as IV

Treatment insulin Regular insulin: § 0. 1 U / k iv push (not recommended in children) § 0. 1 U / k / h infusion in DKA, and in NKH Doubled each 1 -2 h if: § < 10% drop in BS /h, no improvement in AG & PH Halved: § When BS < 200 mg/d in DKA, <300 in NKH* Continue till the resolution of DKA or until patient is mentally alert.

Criteria for resolution of DKA: § PH & AG take 5 -10 h to resolve. § Ketonemia* takes 36 h to resolve due to acetone. § As a result, assessments of urinary or serum ketone levels by the nitroprusside method should not be used for monitoring resolution of DKA.

ADA criteria for resolution of DKA: § Blood glucose <200 mg/d. L and at least two of the following goals are met: § Bicarbonate ≥ 15 § PH > 7. 3 § AG < 12 m. Eq/L

Treatment insulin* If NPO, continue insulin infusion : § & supplement with sc Reg QID as needed: § In adults: 5 U 50 mg BS > 150 mg/dl up to 20 U for BS >=300 as correction insulin.

Treatment insulin If can eat: § Combination of NPH +Reg (basal & bolus) § Continue infusion for 1 -2 h

Treatment insulin § Insulin dose for newly diagnosed DM after resolution of DKA: § Prepubertal = 0. 75 -1. 0 U/kg § Pubertal = 1. 0 – 1. 2 U/kg § Adults = 0. 5 - 0. 8 U/kg

Treatment potasium Start K when: § The patient is not in renal failure § Adequate urine flow (50 cc/h) is established § EKG dose not show evidence of hyperkalemia beyond peak T waves

Treatment potasium § If immediate serum K measurements are unavailable, an EKG may help to determine whether the patient has hyperor hypokalemia

Treatment potasium § § K deficit = 3 - 5 meq / k K < 3 meq / l 40 meq / h K < 4 meq / l 30 meq / h K < 5 meq / l 20 meq / h

Treatment: bicarbonate Indications: § PH ≤ 6. 9 § Severe hyperkalemia § Lactic acidosis § Bicarbonate < 5 mmol/l § Acidosis induced respiratory or cardiac failure § Stop when PH ≥ 7

Treatment: bicarbonate § 50 -100 meq (1 -2 amp) added to 200 – 400 cc isotonic serum or ½ NS & infused at 200 cc / h § Treatment repeated every 2 h if necessary § In pediatric patients 1 -2 meq / k over the course of 1 h

Treatment phosphate § Like K, total body stores are depleted § Serum P normal or high at presentation § Serum P decreases with insulin therapy

Treatment Hypophosphatemia § § Rhabdomyolysis Hemolytic anemia Hypoxia Cardiac & skeletal muscle and respiratory depression

Treatment phosphate § Most patients are asymptomatic § Prophylactic P administration is more harmful than beneficial. § Replacement does not affect outcome.

Treatment phosphate Indications: § Cardiac dysfunction, anemia, respiratory depression § Serum P < 1 mg/ dl § 20 - 30 meq / L (up to 40 - 60 meq totally) potasium phosphate added to replacement fluids § In children severe hypocalcemia & tetany reported

Monitoring: § General measurments: § The serum glucose, every hour until stable, § Serum electrolytes, BUN, creatinine, and venous p. H (for DKA) every two to four hours, depending upon disease severity and the clinical response

Monitoring: § Monitoring with arterial blood gases is unnecessary during the treatment of DKA; § venous p. H, which is approximately 0. 03 units lower than arterial p. H, is adequate to assess the response to therapy.

Monitoring: An alternative to monitoring venous p. H is: §monitor the serum bicarbonate (to assess correction of the metabolic acidosis) §and the serum anion gap (to assess correction of the ketoacidemia)

Monitoring: § Where available, bedside ketone meters that measure capillary blood beta hydroxybutyrate are an alternative to the measurement of anion gap.

Complications of DKA: cerebral edema § Cerebral edema occurs in 0. 5 to 1 % of cases of DKA in children, § and is the leading cause of mortality. § The clinician should be vigilant for early signs of cerebral edema § and should treat promptly if cerebral edema is suspected

Complications of DKA: cerebral edema § Most common in children with newly diagnosed DM § Occurs within 24 h after treatment

Complications of DKA: § Hypertriglyceridemia (serum amylase & Na are falsely low, Chloride is falsely high, masking AG) § Pancreatitis § Myocardial infarction ( CPK & transaminases may increase nonspecifically)

Complications of DKA: § Pulmonary edema due to a reduction in colloid osomotic pressure of serum. § Pulmonary rales on phy. examination higher risk for pulmonary edema

Complications of DKA: § § § § Hypokalemia Hyperkalemia Hypoglycemia Infection Gastric dilation Vascular thrombosis Mucormycosis

Follow up: § Normal AG hyperchloremic acidosis should be expected & is of no clinical concern if AG gradually normalizes during therapy

Hypercholoremic acidosis Normal AG acidosis Mechanisms: § 1 - Loss of large quantities of ketoanions so, regeneration of bicarbonate is reduced. § 2 - adminsitration of iv fluids containing Cl

Prognostic: Poor prognosis in DKA & NKH if: § Hypothermia § Hypotension § Coma § Extremes of age

- Slides: 111