HYPERCALCEMIA APPROACH TO THE DIAGNOSIS Palak Choksi MD










































- Slides: 52

HYPERCALCEMIA: APPROACH TO THE DIAGNOSIS Palak Choksi, MD Assistant Professor of Medicine Metabolism, Endocrinology and Diabetes

Disclosures NONE

Intended Learning Outcomes –Review calcium metabolism –Describe symptoms of hypercalcemia –Review the etiology of hypercalcemia –Discuss the treatments for hypercalcemia –Conclusions

Intended Learning Outcomes –Review calcium metabolism –Describe symptoms of hypercalcemia –Review the etiology of hypercalcemia –Discuss the treatments for hypercalcemia –Conclusions

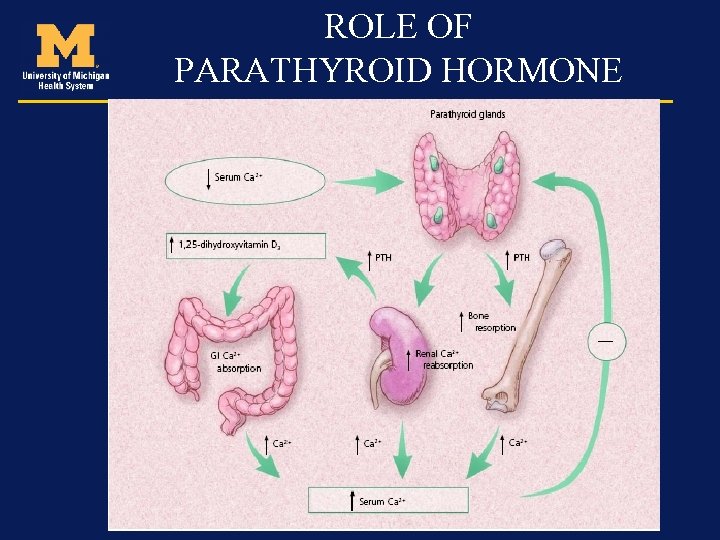
Calcium metabolism • Absorption from GI tract is by passive diffusion and active transport • Most of the calcium is reabsorbed by the kidney – net loss is about 2% • Calcium is controlled by both PTH and calcitonin

ROLE OF PARATHYROID HORMONE

Calcium • Total calcium - Free (ionized) calcium (50%) - Protein bound calcium (40%) - Calcium complexed with organic and inorganic molecules (10%)

Role of albumin High albumin states (volume depletion or multiple myeloma) may lead to pseudohypercalcemia. Low albumin states like malnutrition, total serum calcium may appear low while ionized calcium is again not very affected. Ca 2+= serum Ca 2+ + 0. 8 x [normal alb-patient alb]

Intended Learning Outcomes –Review calcium metabolism –Describe symptoms of hypercalcemia –Review the etiology of hypercalcemia –Discuss the treatments for hypercalcemia –Conclusions

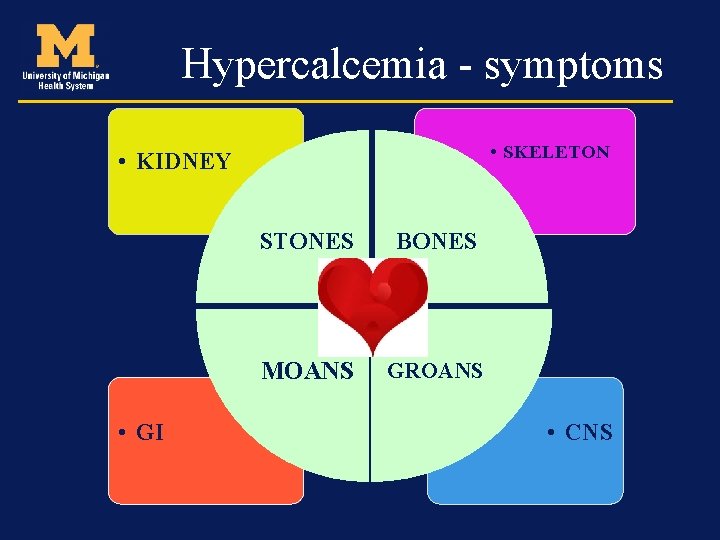
Hypercalcemia - symptoms • SKELETON • KIDNEY • GI STONES BONES MOANS GROANS • CNS

Renal (stones) • Polyuria • Renal insufficiency (rarely seen in mild disease, although in severe cases may cause a reversible drop in GFR) • Nephrolithiasis • Nephrogenic DI

Skeleton (Bones) • Bone pains • Arthritis • Osteoporosis • Osteitis fibrosa cystica

Neuro-psychiatric (Groans) • Depression • Anxiety • Cognitive dysfunction • Lethargy, confusion, stupor, and coma may occur in patients with severe hypercalcemia • More likely to occur in the elderly and in those with rapidly rising calcium concentrations

Gastro-intestinal (Moans) • Constipation • Anorexia • Nausea • Pancreatitis • Peptic Ulcers

Cardiovascular • Increases myocardial contractility and irritability • Shortened QT interval • Prolonged PR • Wide QRS complexes • Calcium deposition in coronary arteries and myocardial fibers • Hypertension

Intended Learning Outcomes –Review calcium metabolism –Describe symptoms of hypercalcemia –Review the etiology of hypercalcemia –Discuss the treatments for hypercalcemia –Conclusions

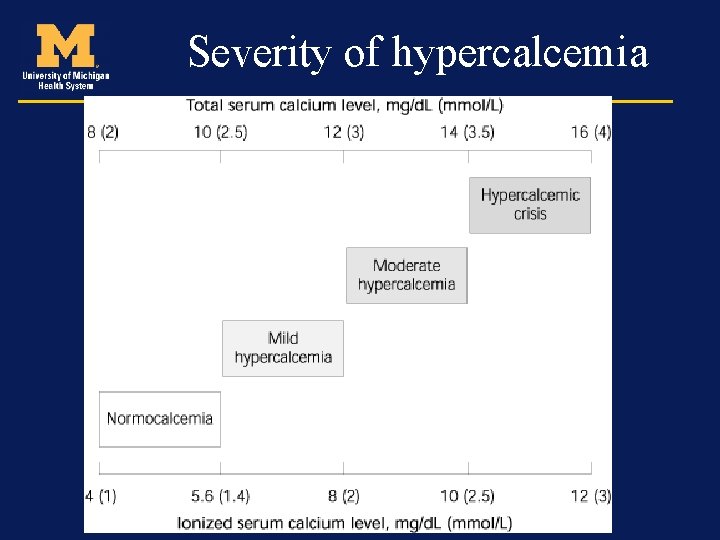
Severity of hypercalcemia

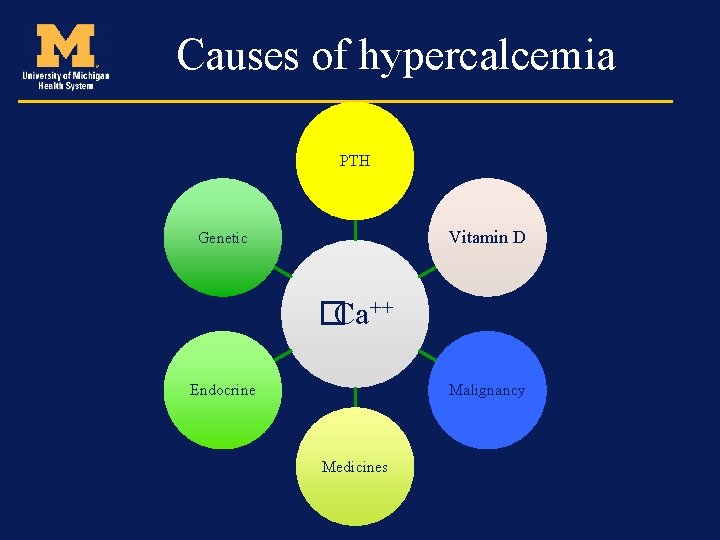
Causes of hypercalcemia PTH Vitamin D Genetic �Ca++ Endocrine Malignancy Medicines

Endocrine causes • Thyrotoxicosis • Adrenal failure • Pheochromocytoma • Drugs: Thiazides, Estrogen, Tamoxifen, Lithium, Vitamin A • Milk-Alkali Syndrome • Immobilization

Algorithmic Approach Normal calcium ? Suspect Calcium � Serum Calcium Hypocalcemia 8. 5 to 10. 3 > 10. 3 mg % < 8. 0 mg %

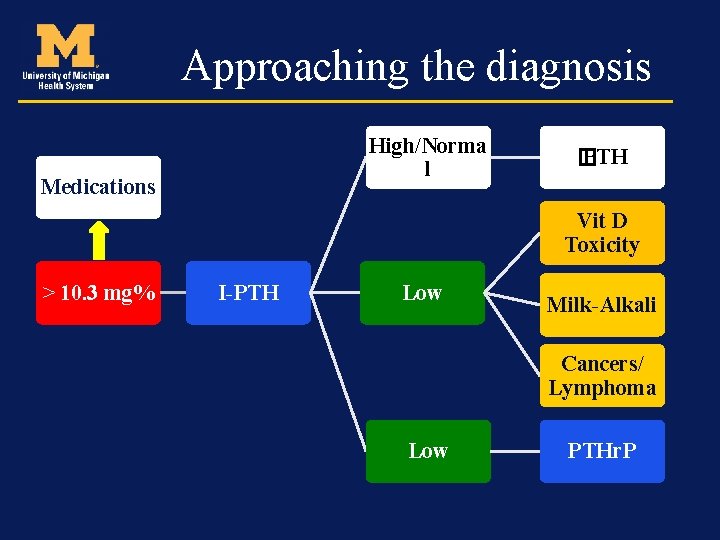
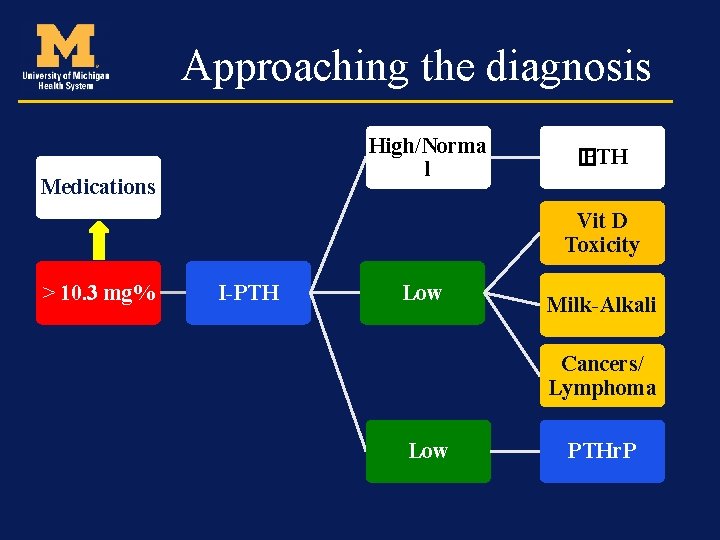
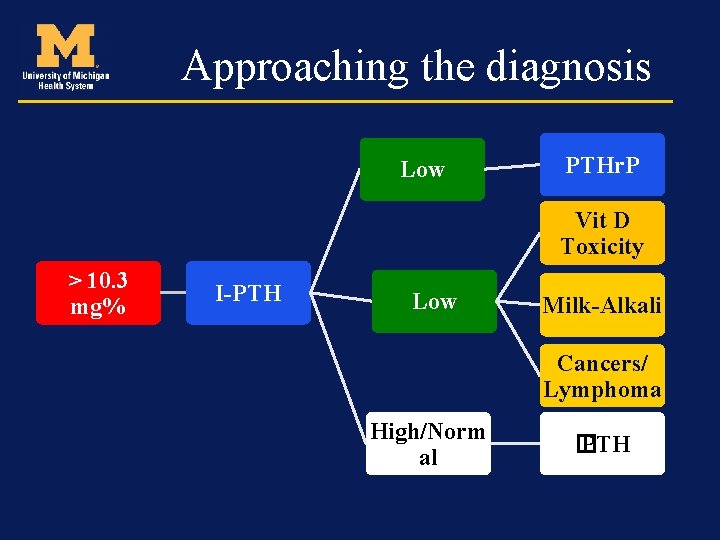
Approaching the diagnosis High/Norma l Medications � PTH Vit D Toxicity > 10. 3 mg% I-PTH Low Milk-Alkali Cancers/ Lymphoma Low PTHr. P

Case • 40/ W noted to have mild elevations in serum calcium on routine testing. Calcium at the last two visits is 10. 410. 6 mg/d. L. • She is relatively asymptomatic. • You obtain labs: • PTH: • 120


Case • 40/ W asymptomatic hypercalcemia • You obtain labs: • PTH: 120 • Phos: 2. 0 • Vitamin D (25 OHD): 40 • Creatinine: 1. 0 • Albumin: 4. 0 • Likely diagnosis: ?

Approaching the diagnosis High/Norma l Medications � PTH Vit D Toxicity > 10. 3 mg% I-PTH Low Milk-Alkali Cancers/ Lymphoma Low PTHr. P

Case • 40/ W noted to have mild elevations in serum calcium on routine testing. Calcium at the last two visits is 10. 4 -10. 6 mg/d. L. She is relatively asymptomatic. You obtain labs: PTH: 120 Phos: 2. 0 Vitamin D (25 OHD): 40 Creatinine: 1. 0 Albumin: 4. 0 • Likely diagnosis: Primary hyperparathyroidism • •

Primary Hyperparathyroidism • Most common cause in the outpatient setting • Renal calculi seen in 15 -20% • Classic bone disease (brown tumors, osteitis fibrosa cystica, subperiosteal resorption) is rarely seen • Increased risk for vertebral fractures

Familial Hypocalciuric Hypercalcemia (FHH) • Rare, autosomal dominant condition • caused by an inactivating disorder of calcium-sensing receptors (Ca. SR) • PTH normal to mildly elevated, mild hypercalcemia • Fractional excretion of calcium is lower than 1%, despite hypercalcemia. • Genetic testing is not often required • Cl. Ca/Cl. Cr= (Uca X SCr) X (Sca X UCr) • A ratio of 0. 01 or less is typically with FHH

Case 70/M with history of renal cell carcinoma. Calcium levels are noted to be recently elevated at 13. 0 mg/d. L. • You obtain labs: - PTH: 23 - Phos: 2. 1 - Vitamin D: 40 - Creatinine: 1. 0 - Albumin 3. 6 - PTH-r. P: 1. 0 (High) •

Approaching the diagnosis Low PTHr. P Vit D Toxicity > 10. 3 mg% I-PTH Low Milk-Alkali Cancers/ Lymphoma High/Norm al � PTH

Case • 70/M with history of renal cell carcinoma. Calcium levels are noted to be recently elevated at 13. 0 mg/d. L. • You obtain labs: - PTH: 23 - Phos: 2. 1 - Vitamin D: 40 - Creatinine: 1. 0 - Albumin 3. 6 - PTH-rp: 1. 0 (High) - Likely diagnosis: Hypercalcemia of malignancy

Humoral Hypercalcemia of Malignancy • Usually have obvious malignant disease • Most common cause for inpatient hypercalcemia • PTH is low, PTH-r. P is elevated • Associated with localized bone destruction

Case • 51/M presents with fatigue and trouble concentrating with a 5 -lb weight loss. Calcium levels are noted to be recently elevated at 13. 0 mg/d. L. • You obtain labs: - PTH: 17 - Phos: 3. 0 - CXR: Hilar lymphadenopathy 24 hour urine calcium is elevated - Vitamin D: 27, Creatinine is normal - DHVD: 110 - Likely diagnosis: Hypercalcemia due to granulomatous disease

Hypercalcemia associated with granulomatous diseases • Sarcoidosis is most commonly associated although can occur in any granulomatous disease • Increased activation of 1α hydroxylase that converts 25 OHD to 1, 25(OH)2 D

Intended Learning Outcomes –Review calcium metabolism –Describe symptoms of hypercalcemia –Review the etiology of hypercalcemia –Discuss the treatments for hypercalcemia –Conclusions

Treatment • Asymptomatic or mildly symptomatic patients do not require immediate treatment • Chronic hypercalcemia with no symptoms 12 -14 mg/dl can be monitored as well • > 14 mg/dl needs treatment even if asymptomatic

Treatment • Correction of dehydration/volume depletion • Correction of any electrolyte abnormalities • Discontinuation of medications that may cause calcium elevation • Reduction of dietary calcium in states of intestinal hyperabsorption (vitamin D intoxication and milk alkali) • Weight bearing or mobilization

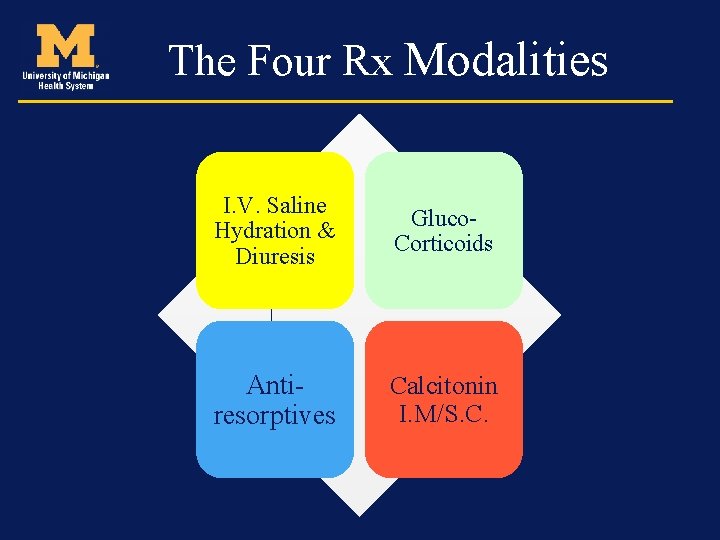
The Four Rx Modalities I. V. Saline Hydration & Diuresis Gluco. Corticoids Antiresorptives Calcitonin I. M/S. C.

Treatment • Agents that decrease the release of calcium from bone or increase the uptake of calcium into bone • Agents that increased urinary excretion of calcium • Agents that reduce intestinal absorption of calcium

Treatment • IV fluids Depending on clinical status 200 -300 ml/hour to maintain UO of 100 -150 ml/hour Dehydration can make hypercalcemia worse by impairing the renal excretion of calcium

Salmon Calcitonin • IM or SQ injections at dose of 4 IU/kg • At 6 -12 hour intervals • Modest reductions and low toxicity profile • Vitamin D intoxication and immobilization • Acts quickly • Escape phenomenon may develop in 48 hours

Bisphonates • Inhibit release of calcium by interfering with osteoclast mediated bone resorption • More potent than saline and calcitonin • Can be used for hypercalcemia of any cause • Max effect seen in 2 -4 days • Also used to prevent hypercalcemia and skeletal events in malignancy

Bisphonates • Pamidronate 60 or 90 mg IV over 2 -4 hours • Zoledronic acid (ZA) 4 mg over 15 minutes • ZA preferred due to quicker infusion time • Side effects (low grade fever, myalgias, osteonecrosis of the jaw, atypical fractures)

NEWER THERAPIES • DENOSUMAB monoclonal antibody • RANKL inhibitor • Humoral hypercalcemia of malignancy • Bisphonate refractory hypercalcemia

Treatment • Agents that decrease the release of calcium from bone or increase the uptake of calcium into bone • Agents that increased urinary excretion of calcium • Agents that reduce intestinal absorption of calcium

Loop diuretics • WITH SALINE • Correct volume depletion first! • 80 -120 mg every 2 -6 hours • Monitor lytes, large losses of K and Mg • Fallen out of favor: 1) Better drugs 2) Frequent monitoring of lytes

Dialysis • Renal insufficiency • Congestive heart failure • Life threatening hypercalcemia

Treatment • Agents that decrease the release of calcium from bone or increase the uptake of calcium into bone • Agents that increased urinary excretion of calcium • Agents that reduce intestinal absorption of calcium

Glucocorticoids • Vitamin D intoxication or endogenous production of calcitriol (sarcoidosis, TB) • Prednisone 20 -40 mg • Lowers calcium in 2 -5 days

Intended Learning Outcomes –Review calcium metabolism –Describe symptoms of hypercalcemia –Review the etiology of hypercalcemia –Discuss the treatments for hypercalcemia –Conclusions

Conclusion • Most common cause of hypercalcemia in the outpatient setting is primary hyperparathyroidism • Most common cause of hypercalcemia in the inpatient setting is malignancy • Establishing the cause is important for treatment decisions

palak@med. umich. edu