Hyperbilirubinemia in Infants Christine Piper RNC BSN pipercmalverno

Hyperbilirubinemia in Infants Christine Piper, RNC, BSN pipercm@alverno. edu Alverno College MSN 621 May 2006

Hyperbilirubinemia Pick a topic to get started! Introduction Pathophysiology Genetics Risk Factors & Symptoms Diagnosis Treatment Links References

How To Use This Tutorial • Each page will have action buttons that allow the user to “go back” or to “move forward” found in the lower right hand corner • There action buttons on the main page that allow the user to navigate to main topics, reference pages, and other internet links that might be of interest • To reach the main page after you are in a topic, there will be a home button located in the lower left hand corner that allows the user to go back to the main page

How To Use This Tutorial • Throughout this tutorial all italicized words are defined if you roll over the word with the mouse • Please note there are sound effects throughout the presentation

Purpose • The purpose of this tutorial is to provide information regarding the pathophysiology, risk factors, symptoms, diagnosis, and current treatment recommendations regarding hyperbilirubinemia in infants

Objectives • To understand the pathophysiology of hyperbilirubinemia • To identify risk factors for hyperbilirubinemia • To identify signs and symptoms of hyperbilirubinemia • To understand diagnosing of hyperbilirubinemia in infants • To understand current treatment recommendations

What Is Hyperbilirubinemia? • Hyperbilirubinemia (also known as jaundice) is an increased level of bilirubin in the blood • It may occur due to physiologic factors that are seen as “normal” in the newborn • It may be due to pathologic factors that alter the usual process in bilirubin metabolism (1)

What Is Hyperbilirubinemia? A. An increase in the amount of bilirubin in the blood B. A decrease in the amount of bilirubin in the blood C. There is no change in the amount of bilirubin in the blood

Correct Hyperbilirubinemia is an increase of bilirubin in the blood

Incorrect Try again If you break the word apart it helps you to define the word. For example hyper = high, excessive bilirubin = bilirubin emia = blood

Incorrect Try again If you break the word apart it helps you define the word. For example hyper = high, excessive bilirubin = bilirubin emia = blood

What Is Bilirubin? • Bilirubin is the by product of the breakdown of heme which is found in red blood cells (1) • Normal red blood cell destruction accounts for 80% of daily bilirubin produced in the newborn (10) • Infants produce twice as much bilirubin per day than as an adult (1) • There are two types of bilirubin - unconjugated (indirect) bilirubin and conjugated (direct) bilirubin

Unconjugated Bilirubin • Unconjugated (indirect) bilirubin – Fat-soluble – Not yet metabolized by the liver – Is not easily excreted – Is the biggest concern for newborn jaundice – If it is not converted it can be deposited into the skin which causes the yellowing of the skin or into the brain which can lead to kernicterus (1)

Conjugated Bilirubin • Conjugated (direct) bilirubin – Water soluble – It is metabolized by the liver – It is mostly excreted in stool and some in the urine

True or False Unconjugated (indirect) bilirubin is bilirubin that is broken down by the liver and is excreted through the urine and stool

Incorrect Unconjugated (indirect) bilirubin is bilirubin that has not yet been broken down by the liver

Correct Conjugated (direct) bilirubin is bilirubin that is broken down by the liver and is excreted in urine or stool
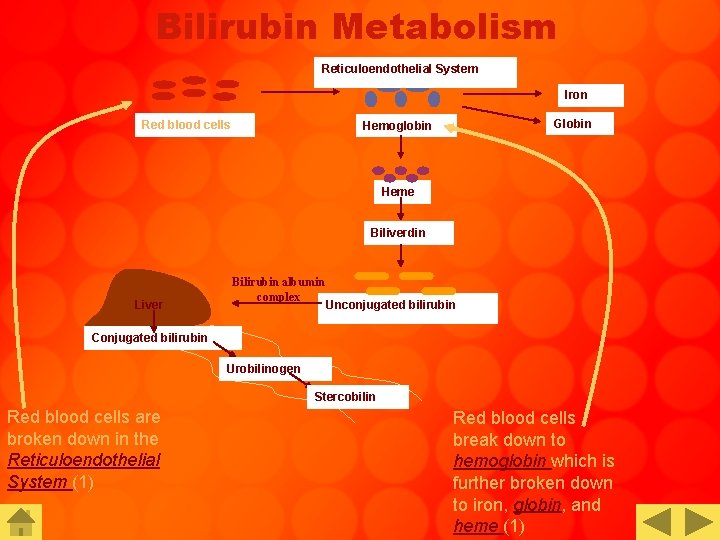
Bilirubin Metabolism Reticuloendothelial System Iron Red blood cells Globin Hemoglobin Heme Biliverdin Liver Bilirubin albumin complex Unconjugated bilirubin Conjugated bilirubin Urobilinogen Stercobilin Red blood cells are broken down in the Reticuloendothelial System (1) Red blood cells break down to hemoglobin which is further broken down to iron, globin, and heme (1)
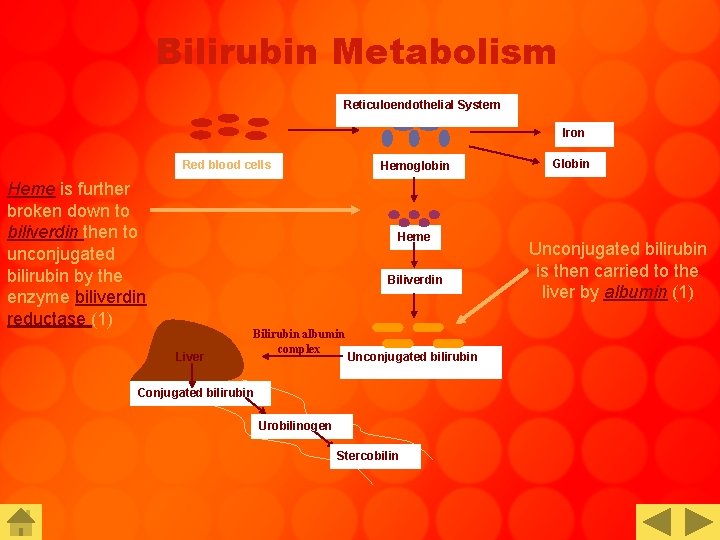
Bilirubin Metabolism Reticuloendothelial System Iron Red blood cells Heme is further broken down to biliverdin then to unconjugated bilirubin by the enzyme biliverdin reductase (1) Hemoglobin Heme Biliverdin Liver Bilirubin albumin complex Unconjugated bilirubin Conjugated bilirubin Urobilinogen Stercobilin Globin Unconjugated bilirubin is then carried to the liver by albumin (1)
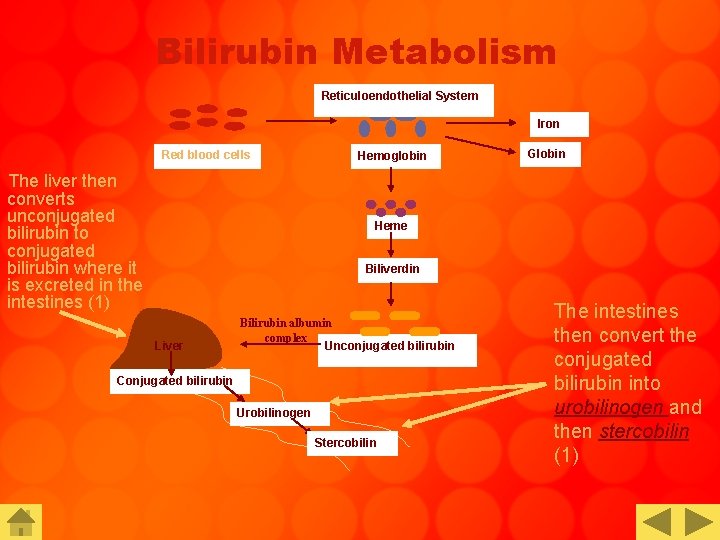
Bilirubin Metabolism Reticuloendothelial System Iron Red blood cells The liver then converts unconjugated bilirubin to conjugated bilirubin where it is excreted in the intestines (1) Hemoglobin Globin Heme Biliverdin Liver Bilirubin albumin complex Unconjugated bilirubin Conjugated bilirubin Urobilinogen Stercobilin The intestines then convert the conjugated bilirubin into urobilinogen and then stercobilin (1)
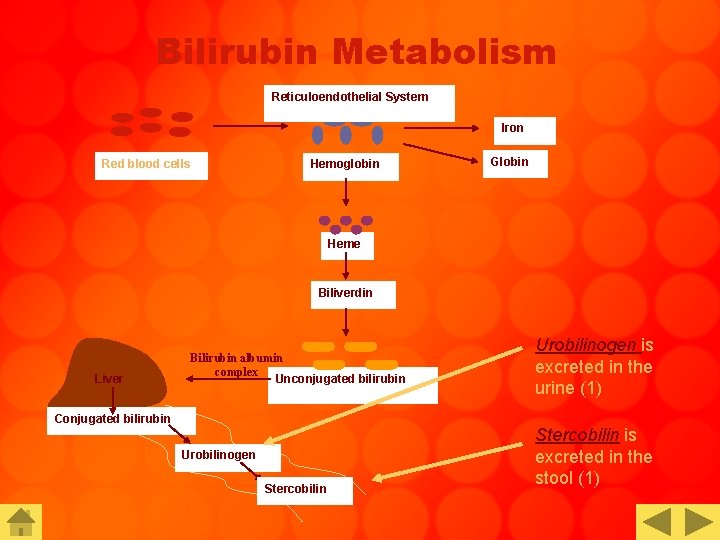
Bilirubin Metabolism Reticuloendothelial System Iron Red blood cells Hemoglobin Globin Heme Biliverdin Liver Bilirubin albumin complex Unconjugated bilirubin Conjugated bilirubin Urobilinogen Stercobilin Urobilinogen is excreted in the urine (1) Stercobilin is excreted in the stool (1)

Click On The Correct Response To Complete The Diagram Hemoglobin is further broken down to iron, globin, and heme Red blood cells are broken down to hemoglobin Liver converts unconjugated bilirubin to conjugated bilirubin where it is excreted in the intestines Unconjugated bilirubin is carried to the liver by albumin Stercobilin is excreted in the stool Intestines convert conjugated bilirubin into urobilinogen and stercobilin Heme is further broken down to bilverdin then to unconjugated bilirubin by the enzyme biliverdin reductase Urobilinogen is excreted in the urine

Click On The Correct Response To Complete The Diagram Red blood cells are broken down to hemoglobin Hemoglobin is further broken down to iron, globin, and heme Stercobilin is excreted in the stool Liver converts unconjugated bilirubin to conjugated bilirubin where it is excreted in the intestines Intestines convert conjugated bilirubin into urobilinogen and stercobilin Heme is further broken down to bilverdin then to unconjugated bilirubin by the enzyme biliverdin reductase Urobilinogen is excreted in the urine Unconjugated bilirubin is carried to the liver by albumin

Click On The Correct Response To Complete The Diagram Red blood cells are broken down to hemoglobin Hemoglobin is further broken down to iron, globin, and heme Heme is further broken down to bilverdin then to unconjugated bilirubin by the enzyme biliverdin reductase Stercobilin is excreted in the stool Liver converts unconjugated bilirubin to conjugated bilirubin where it is excreted in the intestines Intestines convert conjugated bilirubin into urobilinogen and stercobilin Urobilinogen is excreted in the urine Unconjugated bilirubin is carried to the liver by albumin

Click On The Correct Response To Complete The Diagram Red blood cells are broken down to hemoglobin Hemoglobin is further broken down to iron, globin, and heme Heme is further broken down to bilverdin then to unconjugated bilirubin by the enzyme biliverdin reductase Stercobilin is excreted in the stool Liver converts unconjugated bilirubin to conjugated bilirubin where it is excreted in the intestines Intestines convert conjugated bilirubin into urobilinogen and stercobilin Unconjugated bilirubin is carried to the liver by albumin Urobilinogen is excreted in the urine

Click On The Correct Response To Complete The Diagram Red blood cells are broken down to hemoglobin Stercobilin is excreted in the stool Hemoglobin is further broken down to iron, globin, and heme Heme is further broken down to bilverdin then to unconjugated bilirubin by the enzyme biliverdin reductase Unconjugated bilirubin is carried to the liver by albumin Intestines convert conjugated bilirubin into urobilinogen and stercobilin Urobilinogen is excreted in the urine Liver converts unconjugated bilirubin to conjugated bilirubin where it is excreted in the intestines
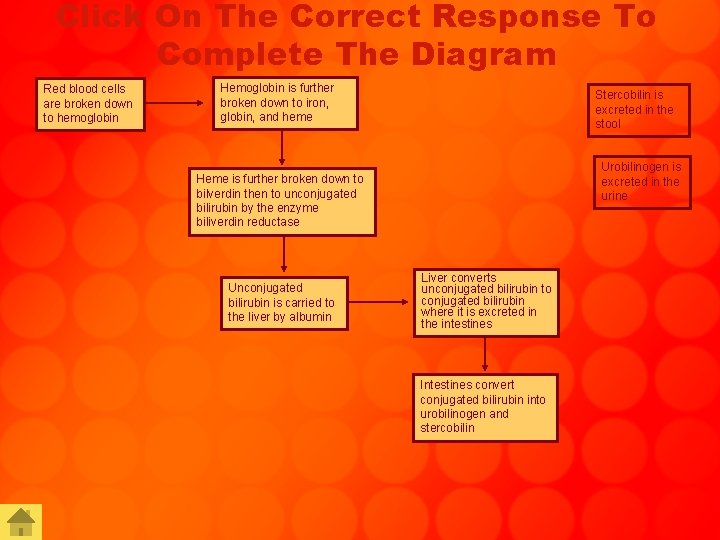
Click On The Correct Response To Complete The Diagram Red blood cells are broken down to hemoglobin Hemoglobin is further broken down to iron, globin, and heme Stercobilin is excreted in the stool Urobilinogen is excreted in the urine Heme is further broken down to bilverdin then to unconjugated bilirubin by the enzyme biliverdin reductase Unconjugated bilirubin is carried to the liver by albumin Liver converts unconjugated bilirubin to conjugated bilirubin where it is excreted in the intestines Intestines convert conjugated bilirubin into urobilinogen and stercobilin

Click On The Correct Response To Complete The Diagram Red blood cells are broken down to hemoglobin Hemoglobin is further broken down to iron, globin, and heme Stercobilin is excreted in the stool Heme is further broken down to bilverdin then to unconjugated bilirubin by the enzyme biliverdin reductase Unconjugated bilirubin is carried to the liver by albumin Liver converts unconjugated bilirubin to conjugated bilirubin where it is excreted in the intestines Intestines convert conjugated bilirubin into urobilinogen and stercobilin Urobilinogen is excreted in the urine
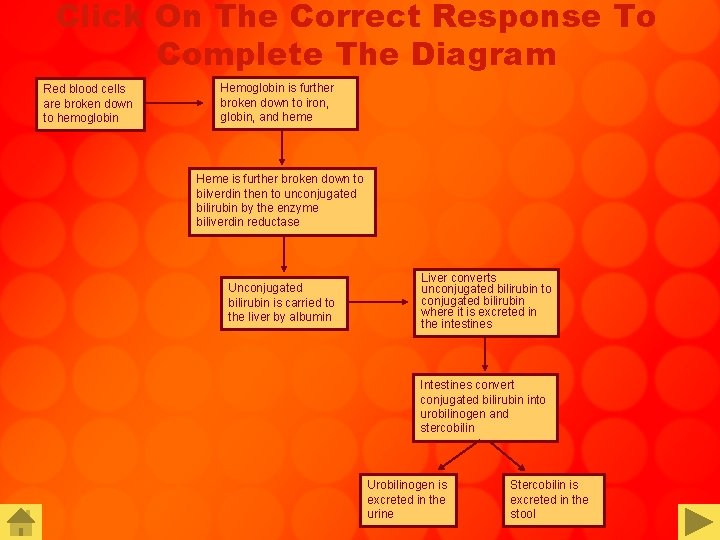
Click On The Correct Response To Complete The Diagram Red blood cells are broken down to hemoglobin Hemoglobin is further broken down to iron, globin, and heme Heme is further broken down to bilverdin then to unconjugated bilirubin by the enzyme biliverdin reductase Unconjugated bilirubin is carried to the liver by albumin Liver converts unconjugated bilirubin to conjugated bilirubin where it is excreted in the intestines Intestines convert conjugated bilirubin into urobilinogen and stercobilin Urobilinogen is excreted in the urine Stercobilin is excreted in the stool

What Is Physiologic Jaundice? • Physiologic jaundice is an exaggerated normal process seen in 60% of term infants, and 80% of premature infants (1) • It normally occurs during the first week of life • It is normally benign and self-limiting • Associated with a bilirubin level greater than 5 -7 mg/d. L (1)

Factors That Contribute To Physiologic Jaundice • Prematurity • Polycythemia

Prematurity & Hyperbilirubinemia • Premature infants are more susceptible to hyperbilirubinemia due to: • Immature hepatic system • Delayed enteral feedings • Decrease in serum albumin levels
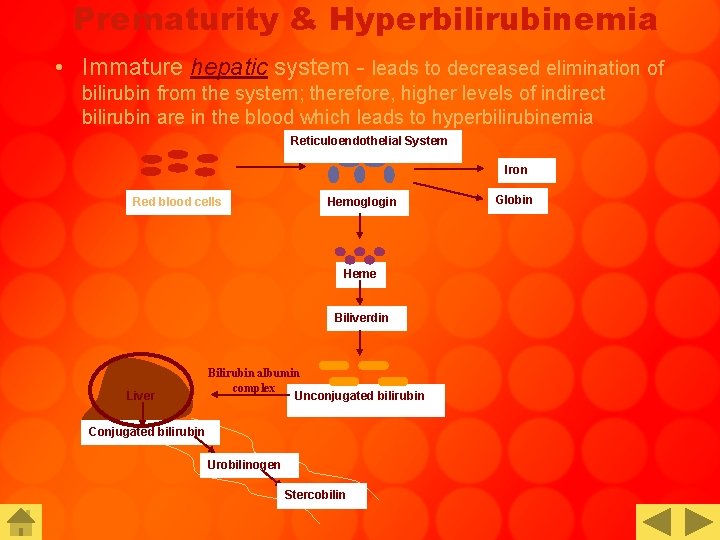
Prematurity & Hyperbilirubinemia • Immature hepatic system - leads to decreased elimination of bilirubin from the system; therefore, higher levels of indirect bilirubin are in the blood which leads to hyperbilirubinemia Reticuloendothelial System Iron Red blood cells Hemoglogin Heme Biliverdin Liver Bilirubin albumin complex Unconjugated bilirubin Conjugated bilirubin Urobilinogen Stercobilin Globin
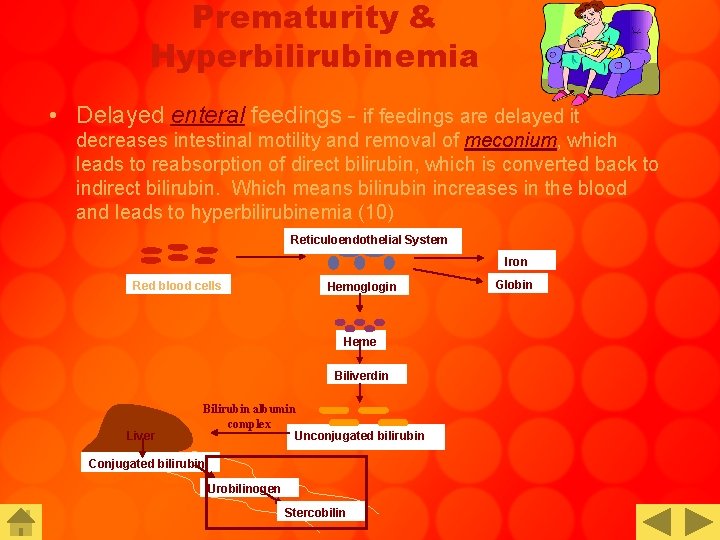
Prematurity & Hyperbilirubinemia • Delayed enteral feedings - if feedings are delayed it decreases intestinal motility and removal of meconium, which leads to reabsorption of direct bilirubin, which is converted back to indirect bilirubin. Which means bilirubin increases in the blood and leads to hyperbilirubinemia (10) Reticuloendothelial System Iron Red blood cells Hemoglogin Heme Biliverdin Liver Bilirubin albumin complex Unconjugated bilirubin Conjugated bilirubin Urobilinogen Stercobilin Globin
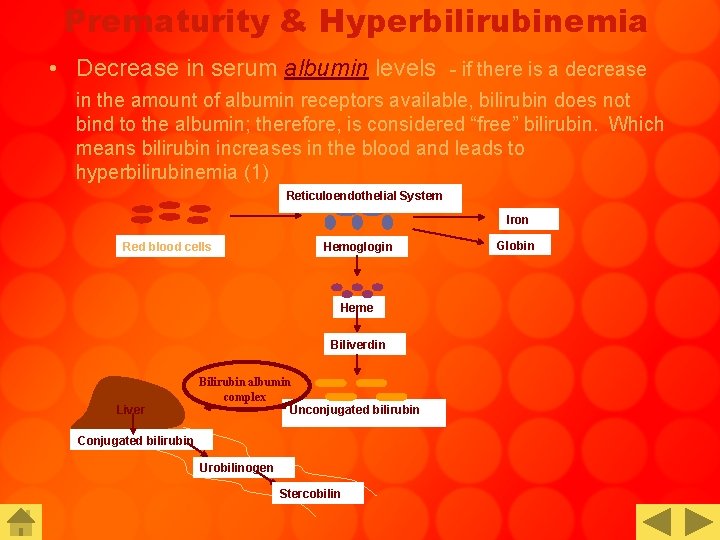
Prematurity & Hyperbilirubinemia • Decrease in serum albumin levels - if there is a decrease in the amount of albumin receptors available, bilirubin does not bind to the albumin; therefore, is considered “free” bilirubin. Which means bilirubin increases in the blood and leads to hyperbilirubinemia (1) Reticuloendothelial System Iron Red blood cells Hemoglogin Heme Biliverdin Liver Bilirubin albumin complex Unconjugated bilirubin Conjugated bilirubin Urobilinogen Stercobilin Globin

Polycythemia & Hyperbilirubinemia • Polycythemia is an increased level of red blood cells (RBCs) in the circulatory system • A infant has more RBCs than an adult, and the lifespan of an RBC is shorter in neonates (1) • Increased RBCs and a shorter lifespan leads to increased destruction of RBCs, which leads to more bilirubin in the blood, which leads to hyperbilirubinemia
What percent of term infants have jaundice? A. 80% B. 50% C. 60%
Incorrect Please try again
Incorrect Please try again

Correct 60% of term infants have physiologic jaundice

What Is Pathologic Jaundice? • Pathologic jaundice is due to factors that alter the process of bilirubin metabolism • It usually appears within 24 hours of life • Associated with a bilirubin level increase of 0. 5 mg/d. L/ hour or 5 mg/d. L per day (10) • Persists for longer than 7 to 10 days (10)

Factors That Contribute To Pathologic Jaundice • Hemolytic anemia • Rh incompatibility • ABO incompatibility • G 6 PD (glucose-6 -phosphate deficiency) deficiency

Hemolytic Anemia & Hyperbilirubinemia • Hemolytic anemia is an incompatibility between the blood of the mother and her fetus • This can occur due to Rh incompatibility or ABO blood incompatibility

Rh Incompatibility • Rh incompatibility is when the mother lacks the Rh factor on the surface of her red blood cells and her baby is born with the Rh factor on his or her red blood cells (13) • This occurs in about 15% of the Caucasian population and 7% of the African American population (13) • It does not occur with the first born child
Rh Incompatability • In Rh incompatibility there is potential for the infant’s blood to enter the mother’s system (13) • If this happens the mother will develop antibodies against the fetal blood cells which may cross the placenta and destroy the infant’s red blood cells (13) • Increased destruction of red blood cells leads to increased bilirubin in the blood; therefore, leading to hyperbilirubinemia

Treatment for Rh Incompatibility • There is an injection called Rh immune globulin (also known as Rhogam) which is given to pregnant women at 28 weeks of pregnancy and within 72 hours of delivering their first infant who is born Rh positive (13) • This injection prevents the mother’s body from forming antibodies against the Rh factor found on fetal red blood cells (13) • If the mother is already sensitized, meaning her body has already made antibodies against the Rh factor, the injection will be ineffective (13) • This injection prevents sensitization in more than 95% of Rh negative women (13)

ABO Blood Incompatibility • ABO incompatibility occurs if the mother has type O blood and the infant has blood type A, B, or AB

ABO Blood Incompatibility • Fetal cells cross the placenta and enter the mother’s bloodstream (6) • When this occurs the mother’s body forms antibodies against the fetal cells (6) • Those antibodies are then small enough to cross back through the placenta into the baby’s circulation and cause destruction of red blood cells (6) • Increased destruction of red blood cells leads to increased bilirubin in the blood; therefore, leading to hyperbilirubinemia

Glucose-6 -Phosphate Dehydrogenase G 6 PD • The function of G 6 PD enzyme is to initiate an oxidation/reduction reaction (3) • An oxidation/reduction reaction is transferring electrons from one molecule to the next (3) • Oxidation is the loss of electrons and reduction is the gain of electrons (3)

G 6 PD Pentose Phosphate Pathway Retrieved from http: //www. malariasite. com/malaria/g 6 pd. htm Used with permission (11) The G 6 PD enzyme is responsible for reducing NADP+ (nicotinamide adenine dinucleotide phosphate) to NADPH (reduced nicotinamide adenine dinucleotide phosphate) (3)

G 6 PD • Without adequate levels of NADPH, red blood cells are more prone to stress and oxidation, which leads to hemolysis of red blood cells (3) • If there is a G 6 PD deficiency there will not be adequate levels of NADPH; therefore, leading to increased hemolysis of red blood cells • Increased hemolysis of red blood cells leads to increased levels of bilirubin, which then leads to hyperbilirubinemia

Physiologic Jaundice versus Pathologic Jaundice Physiologic Occurs 24 hours after birth Prematurity Polycythemia Pathologic Occurs less than 24 hours after birth Hemolytic anemia G 6 PD deficiency

Identify The Causes Of Pathologic Jaundice Hemolytic anemia ABO incompatibility Increased fluid intake G 6 PD deficiency Prematurity Polycythemia Rh incompatibility Headache

Kernicterus • Kernicterus is a rare, irreversible complication of hyperbilirubinemia • If bilirubin levels become markedly elevated, the unconjugated bilirubin may cross into the blood brain barrier and stain the brain tissues (1) • If staining of the brain tissues occurs there is permanent injury sustained to areas of the brain which leads to neurological damage (10)

Kernicterus • “Kernicterus is used to describe the yellow staining of the brain nuclei as seen on autopsy (kern means nuclear region of the brain; icterus means jaundice)” (Juretschke, 2005, p. 10)
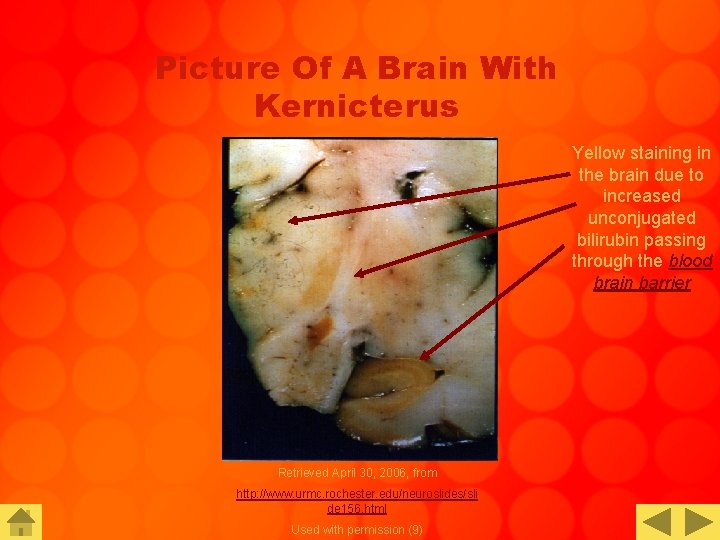
Picture Of A Brain With Kernicterus Yellow staining in the brain due to increased unconjugated bilirubin passing through the blood brain barrier Retrieved April 30, 2006, from http: //www. urmc. rochester. edu/neuroslides/sli de 156. html Used with permission (9)

Kernicterus • Early signs of kernicterus are: lethargy, poor feeding, temperature instability, and hypotonia (1) • Symptoms then progress to: hypertonia, opisthotonos and arching, fever, seizures, and high pitched cry (10) • Long term effects are: choreoathetoid cerebral palsy, tremerousness, mental retardation, sensorineural hearing loss, dental dysplasia, and upward gaze paresis (10)

True or False Genetics play a part in hyperbilirubinemia

Correct There are studies that link genetic mutations in enzymes to increased risk for hyperbilirubinemia

Incorrect There are studies that link genetic mutations in enzymes to increased risk for hyperbilirubinemia

Genetics & Hyperbilirubinemia • A study done from 2001 to 2003 looked at three enzymes with possible genetic defects that were linked to increased rates of hyperbilirubinemia in the Asian population (7)

Genetics & Hyperbilirubinemia • The study was conducted in Taiwan • The reason for this is because the Asian population has twice the incidence of hyperbilirubinemia than the Caucasian population (7) • They were looking to identify potential genetic defects that contribute to the higher incidence of hyperbilirubinemia

Genetics & Hyperbilirubinemia The three enzymes are: • G 6 PD - glucose-6 -phosphate dehydrogenase • OTAP 2 - organic anion transporter 2 • UGT 1 A 1 - UDPglucuronsyltransferase 1 A 1

G 6 PD Pentose Phosphate Pathway Retrieved from http: //www. malariasite. com/malaria/g 6 pd. htm Used with permission (11) The G 6 PD enzyme is responsible for reducing NADP+ (nicotinamide adenine dinucleotide phosphate) to NADPH (reduced nicotinamide adenine dinucleotide phosphate) (3)

Glucose-6 -Phosphate Dehydrogenase G 6 PD • The function of G 6 PD enzyme is to initiate an oxidation/reduction reaction (3) • An oxidation/reduction is transferring electrons from one molecule to the next (3) • Oxidation is the loss of electrons and reduction is the gain of electrons (3)

G 6 PD • G 6 PD is also responsible for maintaining adequate levels of NADPH inside the cells (3) • If there is a G 6 PD deficiency there will not be adequate levels of NADPH • Without adequate levels on NADPH, red blood cells are more prone to stress and oxidation, which leads to hemolysis of red blood cells (3) • If there is increased hemolysis of red blood cells, there will be increased levels of bilirubin, which then leads to hyperbilirubinemia
G 6 PD enzyme Retrieved April 8, 2006, from http: //www. rcsb. org/pdb/explore. do? structure. Id=1 QKI Used with permission
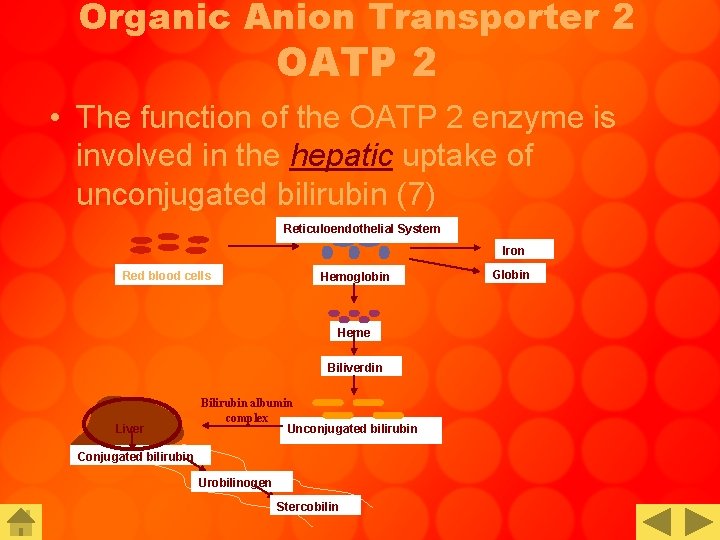
Organic Anion Transporter 2 OATP 2 • The function of the OATP 2 enzyme is involved in the hepatic uptake of unconjugated bilirubin (7) Reticuloendothelial System Iron Red blood cells Hemoglobin Heme Biliverdin Liver Bilirubin albumin complex Unconjugated bilirubin Conjugated bilirubin Urobilinogen Stercobilin Globin

Organic Anion Transporter 2 OATP 2 • In the study done, the authors identified polymorphisms in the OATP 2 enzyme, which led to increased risk for hyperbilirubinemia in the Asian population (7) • If the enzyme activity is delayed there will be increased levels of unconjugated bilirubin in the blood, therefore leading to hyperbilirubinemia

UDP - Glucuronsyltransferase 1 A 1 UGT 1 A 1 • The function of UGT 1 A 1 is to convert unconjugated or indirect bilirubin to conjugated or direct bilirubin (7) Reticuloendothelial System Iron Red blood cells Hemoglobin Heme Biliverdin Liver Bilirubin albumin complex Unconjugated bilirubin Conjugated bilirubin Urobilinogen Stercobilin Globin

UDP - Glucuronsyltransferase 1 A 1 UGT 1 A 1 • In the study done, the authors identified polymorphisms in the UGT 1 A 1 enzyme which, led to increased risk for hyperbilirubinemia in the Asian population (7) • If the enzyme activity is delayed there will be increased bilirubin in the blood, therefore leading to hyperbilirubinemia

What enzyme is responsible for converting unconjugated (indirect) bilirubin to conjugated (direct) bilirubin? A. G 6 PD B. UGT 1 A 1 C. OATP 2

Correct The UGT 1 A 1 is responsible for converting unconjugated (indirect) bilirubin to conjugated (direct) bilirubin

Incorrect Please try again! The G 6 PD enzyme is responsible for maintaining adequate levels of NADPH in the red blood cells which helps prevent hemolysis of red blood cells

Incorrect Please try again! The OATP 2 enzyme is involved in the hepatic uptake of unconjugated bilirubin

What enzyme is responsible for maintaining adequate levels of NADPH in the red blood cells which helps prevent hemolysis of red blood cells? A. G 6 PD B. OATP 2 C. UGT 1 A 1

Correct The G 6 PD enzyme is responsible for maintaining adequate levels of NADPH in the red blood cells which helps prevent hemolysis of red blood cells

Incorrect Please try again! The OATP 2 enzyme is involved in the hepatic uptake of unconjugated bilirubin

Incorrect Please try again! The UGT 1 A 1 is responsible for converting unconjugated (indirect) bilirubin to conjugated (direct) bilirubin

What enzyme is involved in the hepatic uptake of unconjugated bilirubin? A. G 6 PD B. OATP 2 C. UGT 1 A 1

Correct The OATP 2 enzyme is involved in the hepatic uptake of unconjugated bilirubin

Incorrect Please try again! The G 6 PD enzyme is responsible for maintaining adequate levels of NADPH in the red blood cells which helps prevent hemolysis of red blood cells

Incorrect Please try again! The UGT 1 A 1 is responsible for converting unconjugated (indirect) bilirubin to conjugated (direct) bilirubin

Major Risk Factors for Hyperbilirubinemia in Full-Term Newborns • Jaundice within first 24 hours after birth • A sibling who was jaundiced as a neonate • Unrecognized hemolysis such as ABO blood type incompatibility or Rh incompatibility • Nonoptimal sucking/nursing • Deficiency in glucose-6 -phosphate dehydrogenase, a genetic disorder • Infection • Cephalohematomas /bruising • East Asian or Mediterranean descent Retrieved April 18, 2006, from http: //www. cdc. gov/mmwr/preview/mmwrhtml/mm 5023 a 4. htm Used with permission (2)

Signs & Symptoms • • • Poor feeding Increased sleepiness Increased yellowing of the skin or sclera Increased bilirubin level Hypotonia

Diagnosis • Check bilirubin level • Check complete blood count • Check reticulocyte count • Coombs test • Blood groups & types • G 6 PD level • Albumin level • Visual assessment (least reliable)

Bilirubin Level • This test is to measure the amount of bilirubin in the blood • Increased bilirubin = hyperbilirubinemia • In term infants a normal bilirubin level is between 1. 0 - 10. 0 mg/d. L (4) • There is NO safe bilirubin level identified

Complete Blood Count • This test will determine if the infant has increased red blood cells in the circulatory system (polycythemia) • If an infant has a hematocrit greater than 65% this places that infant at risk for hyperbilirubinemia (16)

Reticulocyte Count • This test measures young non-nucleated red blood cells (4) • If the reticulocyte count is greater than 5% in the first week of life, this identifies the infant as trying to replace destroyed red blood cells (16)

Blood Groups & Types • ABO grouping and Rh types are confirmed by examining RBCs for presence of blood group antigens and RBCs and antibodies against these antigens (4)

Direct Coombs Test Retreived April 18, 2006, from http: //en. wikipedia. org/wiki/Image: Coombs_test_schematic. png Used with Permission (15) • “The direct coombs test is a direct measure of the amount of maternal antibody coating the infant’s red blood cell” (Blackburn, 1995, p. 21) • If the antibody is present, the test is positive

Indirect Coombs Test Retreived April 18, 2006, from http: //en. wikipedia. org/wiki/Image: Coombs_test_schematic. png Used with Permission (15) • “The indirect coombs test measures the effect of a sample of the infant’s serum (which is thought to contain maternal antibodies) on unrelated adult RBCs” (Blackburn, 1995, p. 21) • “If the infant’s serum contains antibodies, they will interact with and coat these adult RBCs (positive test)” (Blackburn, 1995, p. 21)

G 6 PD Level • The G 6 PD level is done to identify neonates at risk for G 6 PD deficiency • “The Beutler fluorescent spot test is a rapid and inexpensive test that visually identifies NADPH produced by G 6 PD under ultraviolet light. When the blood spot does not fluoresce, the test is positive; it can be false-positive in patients who are actively hemolysing. It can therefore only be done several weeks after a hemolytic episode” (Glucose-6 -phosphatedehydrogenase deficiency, n. d. , ¶ 16)

Albumin Level • This test indicates the reserve amount of serum albumin available for binding indirect bilirubin (16) • A normal albumin level in a term infant is between 2. 6 - 3. 6 g/d. L (4)

Visual Assessment • “Visual assessment of jaundice is most accurate when the infant’s skin is blanched with light digital pressure in a well-lit room” (Juretschke, 2005, p. 11) • “As bilirubin levels rise, the accuracy of visual assessment decreases” (Juretschke, 2005, p. 11)
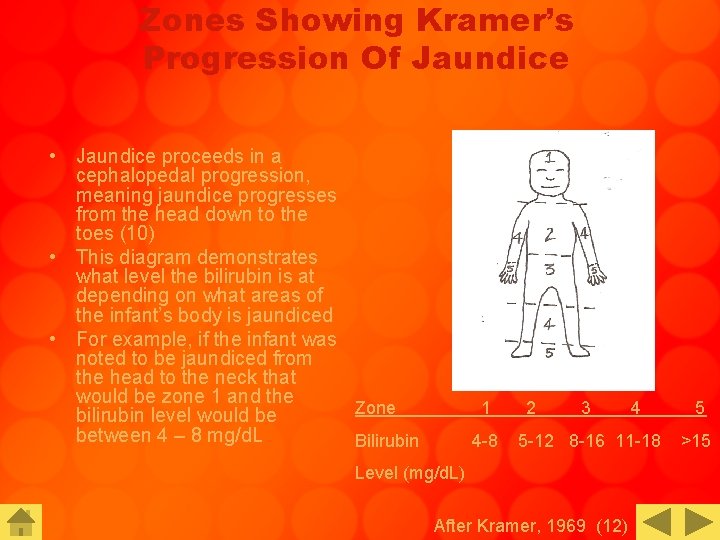
Zones Showing Kramer’s Progression Of Jaundice • Jaundice proceeds in a cephalopedal progression, meaning jaundice progresses from the head down to the toes (10) • This diagram demonstrates what level the bilirubin is at depending on what areas of the infant’s body is jaundiced • For example, if the infant was noted to be jaundiced from the head to the neck that would be zone 1 and the Zone bilirubin level would be between 4 – 8 mg/d. L Bilirubin 1 4 -8 2 3 4 5 -12 8 -16 11 -18 Level (mg/d. L) After Kramer, 1969 (12) 5 >15

Treatment • • • Phototherapy is treatment of choice Encourage frequent feedings Intravenous hydration Intravenous immune globulin Exchange transfusion

Phototherapy • “In the mid-1950 s, Sister Jean at Rochford General Hospital in England noted that infants exposed to sunlight were less jaundiced in the uncovered skin areas than their nonexposed counterparts” (17) • Phototherapy works by converting indirect bilirubin to lumirubin, a water-soluble compound that is a more excretable form of bilirubin (10)
Phototherapy • “Only certain wavelengths (colors) of light are absorbed by bilirubin; as bilirubin is a yellow pigment, blue is absorbed more effectively, however, green light is more deeply absorbed into the skin” (17) An infant undergoing phototherapy Retrieved April 24, 2006, from http: //en. wikipedia. org/wiki/Image: Infant_jaundice_treatment. jpg Used with permission

Frequent Feedings • Encouraging frequent feedings at least eight times per day helps to stimulate intestinal motility and removal of meconium, thus reducing reabsorption of direct bilirubin into the system (1)

Intravenous Hydration • Intravenous hydration of infants with hyperbilirubinemia was thought to decrease bilirubin levels, however, unless an infant is dehydrated intravenous hydration is not indicated (17)

Intravenous Immune Globulin • Intravenous immune globulin (IVIG) has been used to decrease bilirubin levels due to hemolytic anemia • It is thought that IVIG interferes with receptors in the reticulendothelium that are necessary for hemolysis to occur (10)

Exchange Transfusion • An exchange transfusion is used only in extreme cases when phototherapy has failed • The process for an exchange transfusion involves small amounts of blood being removed from the infant and then replaced with the same amount of donor RBCs and plasma (1) • The process continues until twice the circulating volume has been replaced (1) • The exchange replaces ~ 87% of the circulating blood volume and decreases the bilirubin level by ~ 55% (1)

Links • For information on kernicterus there is a website entitled Parents of Infants and children with Kernicterus. Their website is http: //www. pickonline. org/ • A Sentinel Alert was issued in April 2001 by the Joint Commission on Accreditation of Healthcare Organizations on Kernicterus. The website address is http: //www. jointcommission. org/Sentinel. E vents/Sentinel. Event. Alert/sea_18. htm

References 1. Blackburn, S. (1995). Hyperbilirubinemia and neonatal jaundice. Neonatal Network, 14(7), 15 -29. 2. Center for Disease Control and Prevention. (2001). Kernicterus in fullterm infants-United States, 1994 -1998. Morbidity and Mortality Weekly Report, 50(23), p. 494. Retrieved April 18, 2006, from http: //www. cdc. gov/mmwr/preview/mmwrhtml/mm 5023 a 4. htm 3. Ethnasios, R. (2003). Physiology of G 6 PD. Retrieved March 2, 2006, from http: //www. rialto. com/g 6 pd/physiolo. htm 4. Fischbach, F. Nurses’ quick reference to common laboratory and diagnostic tests (2 nd ed. ). Philadelphia: Lippincott-Raven. 5. Glucose-6 -phosphate dehydrogenase deficiency. (n. d. ). Wikipedia. Retrieved May 1, 2006, from Answers. com Web site: http: //www. answers. com/topic/glucose-6 -phosphate-dehydrogenasedeficiency 6. Hull, J. (2006). ABO incompatibility. Retrieved March 31, 2006, from http: //www. drhull. com/Ency. Master/A/ABO_incompatibility. html

References 7. Huang, M. , Kua, K. , Teng, H. , Tang, K. , Weng, H. , & Huang, C. (2004). Risk factors for severe hyperbilirubinemia in neonates. Pediatric Research, 56(5), 682 -89. 8. Infant undergoing home phototherapy for jaundice. (2005). Retrieved April 25, 2006, from http: //en. wikipedia. org/wiki/Image: Infant_jaundice_treatment. jpg 9. Józefowicz, R. , Miller, J. , & Powers, J. (2000). Neuropathy and neuroimaging laboratory: Mind, brain, and behavior course. University of Rochester School of Medicine and Dentistry. Retrieved April 30, 2006 from http: //www. urmc. rochester. edu/neuroslides/slide 156. html 10. Juretschke, L. (2005). Kernicterus: Still a concern. Neonatal Network, 24(2), 7 -19. 11. Kakkilaya, B. , M. D. (2005). Glucose 6 phosphate dehydrogenase deficiency. Retrieved March 18, 2006, from http: //www. malariasite. com/malaria/g 6 pd. htm 12. Kramer, L. (1969). Advancement of dermal icterus in the jaundiced newborn. American Journal of Diseases of Children, 118(3), 454 -458. Copyright © (1969), American Medical Association, All Rights Reserved.

13. References March of Dimes Birth Defects Foundation. (2001). Quick reference and fact sheets: Rh disease. Retrieved February 28, 2006, from http: //www. marchofdimes. com/printable. Articles/681_1220. asp? printabl e=true 14. PDB ID: 1 QKI (Identification of the enzyme in the database) Au, S. W. N. , Gover, S. , Lam, V. M. S. , & Adams, M. J. Human Glucose-6 -Phosphate Dehydrogenase: The Crystal Structure Reveals a Structural Nadp+ Molecule and Provides Insights Into Enzyme Deficiency. Stucture v 8 pp. 293 (2000). Retrieved April 8, 2006, from http: //www. rcsb. org/pdb/explore. do? structure. Id=1 QKI 15. Rad, A. (2006). Coombs test. Retrieved May 1, 2006, from http: //en. wikipedia. org/wiki/Coombs_test 16. Schwobel, A. & Sakraida, S. (1997). Hyperbilirubinemia: new approaches to an old problem. Journal of Perinatal & Neonatal Nursing, 11(3), 78 -98. 17. Steffensrud, S. (2004). Hyperbilirubinemia in term and near term infants: Kernicterus on the rise? Newborn and Infant Nursing Reviews, 4(4), 191 -200.

References 18. Venes, D. (Ed. ). (2005). Taber’s cyclopedic medical dictionary (20 th ed. ), Philadelphia: F. A. Davis Company.

The End! • Thank you for taking the time to complete this tutorial on neonatal jaundice • If there any questions, please contact me at pipercm@alverno. edu
- Slides: 109