Hyperadrenocorticism in Dogs Hyperadrenocorticism HAC is caused by

Hyperadrenocorticism in Dogs

Hyperadrenocorticism (HAC) is caused by excess circulating coortisol or other steroid hormones. Pituitary-Dependent Hyperadrenocorticism (PDH) Adrenal Tumor (AT) Iatrogenic Hyperadrenocorticism

Pituitary-Dependent Hyperadrenocorticism (PDH) 80 -85% dogs with HAC Most have pituitary adenoma in pars distalis Most microadenomas (< 1 cm) 10 -20% macroadenomas (> 1 cm) Frequency and amplitude of ACTH “bursts” are chronically excessive excess cortisol secretion Adrenocortical hyperplasia Relatively ineffective feedback on pituitary adenoma Suppression of hypothalamic function and CRH Loss of hypothalamic control of ACTH and cortisol levels usually within reference ranges on single blood samples Chronic

Adrenal Tumor (AT) Adenoma or carcinoma (carcinomas larger) (50: 50 distribution) Cortisol secretion independent of pituitary control Suppression of CRH and ACTH Atrophy of contralateral adrenal and normal cells in affected adrenal Episodic random cortisol secretion can respond to ACTH

Iatrogenic Hyperadrenocorticism Excessive administration of glucocorticoids ◦ Allergic or immune-mediated disease ◦ Oral, eye, ear, or skin medications ◦ Suppression of endogenous ACTH ◦ Bilateral adrenocortical atrophy

Middle-aged and older dogs • PDH: 55 -60% female o 75%>9 yrs o Median 11. 4 yr • AT: 60 -65% female o 90%>9 yrs o Median 11. 6 yr Any breed can be affected PDH: Poodles, dachshund, terriers, beagles, German shepherd dogs 75%<20 kg AT: Poodles, GSD, dachshund, labs, terriers 50%>20 kg

Clinical Signs, History, Physical Examination Polyphagia (> 90%) Thin skin, bruising, striae PUPD (80 -85%) Seborrhea, pyoderma Abdominal enlargement (>80%) – “pot-bellied” Comedones o Hepatomegaly o Redistribution of fat o Abdominal muscle weakness Hyperpigmentation Anestrus Muscle weakness (75 -85%) Testicular atrophy Lethargy Facial paralysis Obesity Heat intolerance Alopecia o Truncal o Bilaterally symmetrical Calcinosis cutis Pseudomyotonia

CBC SERUM BIOCHEMISTRY “Stress leukogram” o Neutrophilia o Monocytosis o Lymphopenia o Eosinopenia Thrombocytosis n. RBCS Mild erythrocytosis (females - androgens) ALT (< 400) Mildly �fasting BG Normal to �BUN �cholesterol and triglycerides Mildly �bile acids Mild �Na Mild�K

Urinalysis ◦ SG < 1. 015, often < 1. 008 ◦ Mild increase in UP: C (less than 5) ◦ Urinary Tract Infection (UTI) in 40 -50% ◦ UTI often “silent” ◦ o Inactive sediment o No clinical signs o Low USG
Diagnostic Imaging Abdominal Radiographs ◦ Hepatomegaly ◦ Distended urinary bladder ◦ Urolithiasis ◦ Dystrophic calcification of soft tissues ◦ Osteoporosis of vertebrae ◦ Calcified adrenal gland o Rare o Consistent with adrenal adenoma or carcinoma Thoracic Radiographs Calcification of airways Osteoporosis of vertebrae Pulmonary metastases (Rare) Evidence of pulmonary thromboembolism
Abdominal Ultrasound Examination ◦ Adrenomegaly (PDH) ◦ Adrenal mass with small contralateral adrenal (AT) ◦ Calcified adrenal gland (A T) ◦ Tumor thrombus or metastasis ◦ Hepatomegaly ◦ Hyperechoic liver ◦ Distended urinary bladder ◦ Urolithiasis ◦ Dystrophic calcification of soft tissues Advanced Imaging ◦ Brain CT or MRI may reveal pituitary tumor o Recommended to confirm cause of neurological signs o Recommended if considering radiation therapy or surgery ◦ Abdominal CT recommended prior to adrenalectomy

Complications of Hyperadrenocorticism Hypertension (> 50%) Pancreatitis? ? ? Urinary tract infection (UTI) Diabetes mellitus o Pyelonephritis Poor wound healing o Cystitis (clinically silent) Recurrent infections Urolithiasis o Calcium-containing o Struvite, related to UTI Congestive heart failure Joint laxity Hypercoagulability ◦ Pulmonary thromboembolism ◦ Aortic thromboembolism

Diagnosis of Canine Hyperadrenocorticism Screening tests Differentiation tests Need to understand sensitivity and specificity o False positives and false negatives Can improve predictive value of tests by only testing the appropriate population o Consistent clinical signs o No concurrent illnesses

Screening Test: Basal Cortisol Just say NO for Cushing’s diagnosis ◦ Wide fluctuations throughout the day ◦ Normal dogs can be out of the reference range ◦ Basal levels higher with stress or other illnesses ◦ Cushing’s dogs usually in reference range ◦ Typical reference range: 1 -5 ug/dl NOTE: Can be used to RULE OUT hypoadrenocorticism

Screening Test: Urine Cortisol: Creatinine Ratio UCCR: screening test ◦ High sensitivity, But not 100% ◦ Few false negatives - but how few? o Depends on study: o one study: 75% sensitive o earlier study: 99% sensitive o May have 1/100 - 25/100 false negatives ◦ Low specificity o Many false positives o UCCR in 75 - 85% dogs with NON-adrenal disease ◦ Quick, easy, outpatient test

Screening Test: ACTH Stimulation Test Screening test – measures maximum secretory capacity of the adrenal cortex. How to do it: Obtain baseline cortisol sample • Inject Cortrosyn IV o 5 ug/kg(upto 250 ugmax) o 1 vial if >25 kg o 1/2 vialif<25 kg Obtain 1 -hour post ACTH cortisol sample

How to interpret it: �Pre-ACTH cortisol: normal: 0. 5 - 6. 0 μg/dl �Post-ACTH cortisol: o Normal: <18 μg/dl o Exaggerated: >22 μg/dl o Grey zone: 18 - 22 μg/dl �Hypoadrenocorticism: both values < 2 μg/dl �Usually < 0. 2 μg/dl

Pros and Cons of the ACTH Stimulation Test �More false negatives than LDDST o Lower sensitivity �Fewer false positives than LDDST o Higher specificity �Does not distinguish between PDH and AT �One hour test �Can combine with other procedures (e. g. ultrasound) �Useful in a referral setting �Only test for: o Iatrogenic Cushing’s o Hypoadrenocorticism o Monitoring mitotane or trilostane therapy

Screening Test: Low-Dose Dexamethasone Suppression Test (LDDST) �More sensitive (95%) than ACTH stimulation test �Less specific (more false positives) �CAN distinguish between PDH and A T �Not useful for iatrogenic Cushing’s or hypoadrenocorticism

How to do it �Blood sample at 0 (pre), 4, and 8 hours �Give 0. 01 mg/kg dexamethasone IV (0. 015? ) �Less expensive than ACTH stimulation test (at current price of Cortrosyn) �Takes 8 hours �Avoid stress, excitement, handling, other tests

How to interpret it LDDST Results Normal patient: ◦ � 0 hr: Cortisol=1 -5 mg/dl ◦ � 4 hr: Cortisol < 1. 4 mg/dl ◦ � 8 hr: Cortisol < 1. 4 mg/dl Cushing’s patient: � 8 hr: Cortisol > 1. 5 mg/dl

Discrimination Test: LDDST Discriminatory test in some cases o Cannot confirm AT “Decrease” occurs in 60 - 65% of dogs with PDH: o 4 hr: Cortisol < 1. 4 ug/dl, or o 4 hr or 8 hr: Cortisol < 50% baseline o Confirms PDH

Discrimination Test: High Dose Dexamethasone Suppression test (HDDST) How to do it ◦ �Give 0. 1 mg/kg dexamethasone iv ◦ �Blood sample at 0 (pre), 4, and 8 hours ◦ �AT: no suppression at 4 or 8 hours ◦ �PDH: v. Cortisol < 1. 4 mg/dl at 4 or 8 hours Cortisol < 50% baseline at 4 or 8 hours o 25% PDH cases do NOT suppress v 35 -40% do not suppress on LDDST v 25% do not suppress on HDDST v. If no suppression on LDDST, will only pick up another 10 -15% on the HDDST, so probably better to choose another test v. Can NEVER DIAGNOSE adrenal tumor on LDDST or HDDST

Treatment of Hyperadrenocorticism Before commencing treatment ◦ Be confident of the diagnosis ◦ Patient must have consistent clinical signs, clinicopathological findings, and positive diagnostic testing

What to do if HAC strongly suspected but tests do not confirm? Wait and retest Consider ACTH stimulation with sex hormone panel (controversial) What to do if tests confirm HAC but patient has minimal signs? Ensure that test results are not false positive Stress Concurrent non-adrenal illness No evidence that early treatment is beneficial Treat when o Signs affecting quality of life of dog, or Signs affecting quality of life of owner, or Signs concerning to veterinarian ◦ Monitor for occult complications of HAC �Hypertension �UTI�Proteinuria

Client Education Medical therapy is indicated for PDH and for adrenal tumors in which surgery is not an option. Medical therapy for HAC is life long, requires diligent monitoring and follow-up, and is potentially expensive. Serious side effects are possible with all forms of medical therapy.

Surgical Therapy Surgery is indicated for functional adrenocortical tumors o Adenoma – good prognosis o Carcinoma with no metastases Ultrasound CT Radiographs Recommend referral to specialists o Experienced surgeon o Good anesthetic support o Internist for management pre- and post-surgery Hypertension Hypercoagulability Post-operative hypoadrenocorticism Surgery for pituitary tumors o Hypophysectomy

Mitotane Safe, if used carefully �Normal dogs are relatively resistant o Reduced GI absorption in normal dogs compared to dogs with hyperadrenocorticism o Cortex is damaged but dogs not clinically affected o (HAC dogs more sensitive to loss of cortical function) �Some Cushing’s dogs appear “resistant” o Not getting drug o Drug not absorbed (give with food, crush or make suspension) o Bad batch of medication o Other medications interfering o Adrenal tumor o Resistant form of PDH (need a higher dose) o Incorrect diagnosis � 2 phases of therapy: o Loading/induction o Maintenance �Monitoring is key: o ACTH stimulation test Determine end-point of induction Confirm ongoing successful maintenance

Mitotane Induction Dose: 50 mg/kg o Divide daily dose o Give with food o Pick up subtle signs of induction o Reinforces importance of close monitoring �Stop therapy and do ACTH stimulation test when see: o Subtle decrease in appetite (usually happens first), or o Decrease in PUPD, or o Vomiting, anorexia, diarrhea, or �ACTH stimulation test at 7 days even if no change in signs �Concurrent prednisone: NO �Owner has prednisone on hand - call first �Successful induction is achieved when basal and post-ACTH cortisol: o both < 4 (5) mg/dl (40 ng/ml) and > 1 mg/dl �Most cases take 5 - 15 days

Mitotane Maintenance: �Give daily induction dose weekly (divided) �Example: o 10 kg dog required 250 mg BID for induction (7 days) o Maintenance dose would be 250 mg twice weekly o Divide dose (125 mg BID) �Continue to monitor with ACTH stimulation tests Mitotane Monitoring: ◦ �ACTH stimulation test: o At end of induction ◦ o 1 month later o 3 months later o every 6 months o 1 - 2 months after every dosage change o If problems arise ◦ �POST ACTH cortisol is the most important ◦ �CANNOT monitor with basal cortisol!
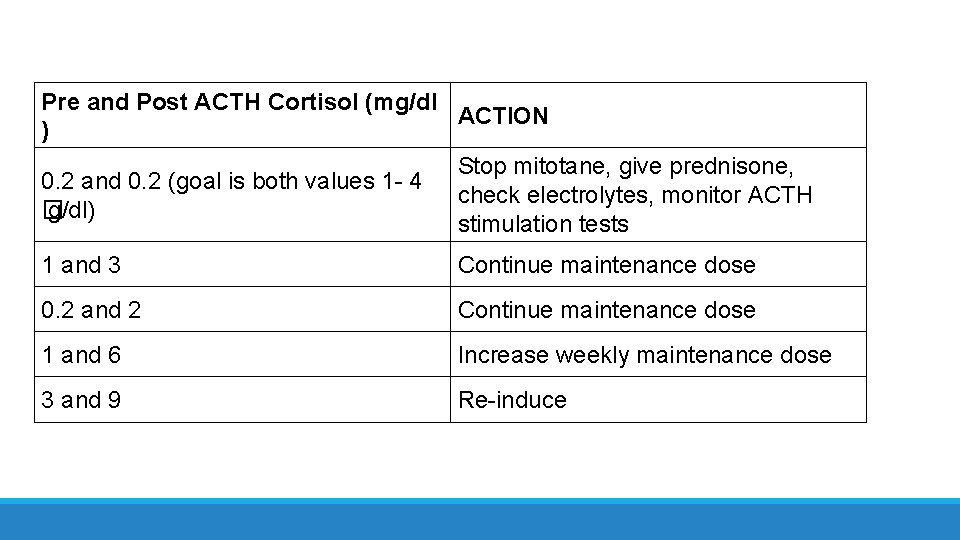
Pre and Post ACTH Cortisol (mg/dl ACTION ) Stop mitotane, give prednisone, 0. 2 and 0. 2 (goal is both values 1 - 4 check electrolytes, monitor ACTH � g/dl) stimulation tests 1 and 3 Continue maintenance dose 0. 2 and 2 Continue maintenance dose 1 and 6 Increase weekly maintenance dose 3 and 9 Re-induce

Medical Therapy: Trilostane Vetoryl® (Dechra) o Tested and licensed in Europe and USA for canine Cushing’s o Competitively inhibits steroid synthesis Inhibits 3 -�-hydroxysteroid dehydrogenase Converts pregnenolone to progesterone Converts 17 -OH pregnenolone to 17 -OH progesterone o Appears safe and effective o Monitor with ACTH stimulation tests o Adrenals keep getting bigger o Some reports of adrenal necrosis

Using Trilostane Start with lower dose o 1 mg/kg BID (or less) ACTH stimulation tests o Start 3 -4 hours post-pill o 10 -14 days Ensure not over-dosing o Monthly o Whenever clinical signs change o Aim for pre and post values between 2 and 6 ug/dl o ACTH response may decrease over time o Do not be too quick to increase dose

Canine Hypothyroidism

Hypothyroidism is an endocrinopathy caused by decreased production of thyroid hormone. Because most cells in the body are affected by thyroid hormone, hypothyroidism can affect most organs. Common signs are related to the dermatologic system and decreased metabolic rate. Approximately 1 in 200 dogs is affected.

Signalment Breed ◦ Golden retrievers, Doberman pinschers, and spaniels are predisposed. ◦ There may be regional differences. ◦ Multiple breeds are predisposed to lymphocytic thyroiditis and likely predisposed to hypothyroidism, 3 but any breed may develop hypothyroidism. Age & Range ◦ Mean age is 7 years (range, 0. 5– 15 years). ◦ Hypothyroidism secondary to lymphocytic thyroiditis appears to develop at a younger age than idiopathic thyroid atrophy. Sex ◦ Spayed and neutered dogs are at increased risk compared with intact dogs

Causes Primary hypothyroidism, the most common form, results from destruction of the thyroid glands. Secondary hypothyroidism, caused by decreased thyroid- stimulating hormone (TSH) release from the pituitary, has rarely been reported. Tertiary hypothyroidism, caused by hypothalamic dysfunction, has not been proven in dogs. Congenital hypothyroidism from thyroid peroxidase deficiency has been seen in rat terriers and toy fox terriers. Giant schnauzers also develop congenital hypothyroidism, probably from TSH or thyrotropinreleasing hormone (TRH) deficiency.

Pathophysiology Adult-onset hypothyroidism is typically caused by lymphocytic thyroiditis or idiopathic thyroid atrophy. Lymphocytic thyroiditis is characterized by infiltration of the thyroid gland by lymphocytes, plasma cells, and macrophages. ◦ Eventually, fibrous connective tissue replaces parenchyma Idiopathic thyroid atrophy is characterized by thyroid parenchyma being replaced by adipose tissue. ◦ Fibrosis and inflammation are minimal. ◦ Idiopathic thyroid atrophy may be the result of thyroiditis. Thyroid carcinoma is a rare cause of hypothyroidism, which does not develop until at least 75% of the thyroid has been destroyed.

Signs Common metabolic signs include weight gain, lethargy, and weakness; cold intolerance or heat-seeking behavior; and mental dullness. Dermatologic changes are common. Neurologic dysfunction is uncommon and resolves with levothyroxine supplementation. Peripheral neuropathy may result in exercise intolerance, ataxia, weakness, conscious deficits, and hyporeflexia proprioception Recent studies suggest that abnormalities in the limbs are more related to muscle than nerve. Cranial nerve dysfunction (V, VIII) and peripheral and central vestibular disease have been reported. Seizures are rare

Cardiac abnormalities (eg, weak apex beat, bradycardia) are uncommon. Reproductive abnormalities include periparturient mortality and lower birth weight in pups born to hypothyroid bitches, and inappropriate galactorrhea in females. Decreased fertility is not well documented in hypothyroid bitches. Decreased libido and fertility have been reported in males of other species; . Ocular changes may include corneal lipid deposits, lipemia retinalis, uveitis, secondary glaucoma, and keratoconjunctivitis sicca. Laryngeal paralysis and megaesophagus have been reported, but no causal relationship has been proven. Myxedema coma is very rare.

Diagnosis Differentials Dermatologic abnormalities could be caused by hyperadrenocorticism and alopecia X. Metabolic signs could be caused by many other disease processes. Laboratory Findings CBC, serum biochemistry profile, and urinalysis are indicated to rule out other diseases before thyroid-specific tests are conducted. Mild nonregenerative anemia is common. Most hypothyroid dogs have fasting hypercholesterolemia and hyper- triglyceridemia. Alkaline phosphatase (ALP) and alanine aminotransferase (ALT) may be slightly elevated.

Thyroid-Specific Diagnostics Total T 4 (TT 4) concentration is a sensitive but nonspecific screening test; values are low in most patients. Additional testing (free T 4 [f. T 4 ], TSH) is recommended before diagnosing hypothyroidism. Euthyroid dogs may have low TT 4 levels because of individual varia- tion, nonthyroid illness, or drug administration. Euthyroid sight hounds and sled dogs often have levels below the reference range, leading to inaccurate diagnosis. Measurement of f. T 4 by equilibrium dialysis is a more accurate indicator of thyroid function than TT 4, as f. T 4 (not bound to proteins) is the active form. ◦ It is also less affected by nonthyroid illness when compared with TT 4. ◦ Measurement of f. T 4 without an equilibrium dialysis step offers no diagnostic benefit over TT 4. Because of decreased negative feed- back, TSH concentrations are often elevated in hypothyroid dogs. Increased TSH in conjunction with decreased TT 4 or f. T 4 is specific for hypothyroidism; hypothyroid dogs have nor- mal TSH concentrations. however, up to 33% of

Measurement of T 3 concentrations is less accurate than measurements of TT 4 and f. T 4. The TSH stimulation test evaluates thyroid reserve. ◦ Lack of increase in T 4 concentration 4– 6 hours after TSH adminis- tration is standard for diagnosis of hypothyroidism, but the expense of human recombinant TSH limits the test’s clinical usefulness The TRH stimulation test is less straightforward, less reliable, and more difficult to obtain than the TSH stimulation test. Of dogs with hypothyroidism, antithyroglobulin antibodies (ATAs) are found in ~35%, anti-T 3 antibodies in 34%, and anti-T 4 antibodies in 15% Antibody presence is not diagnostic of hypothyroidism; <20% of euthy- roid dogs with ATAs develop hypothyroidism signs within 1 year.

In patients with consistent signs, CBC results, and serum biochemistry findings, begin by measuring TT 4 concentration. If value is low, f. T 4 and TSH concentrations are measured. A low f. T 4 concentration with an increased TSH concentration is approximately 86% accurate for diagnosis. ◦ As some hypothyroid patients will have TSH concentrations within reference range, therapeutic trial is recommended in patients with low f. T 4 and strong clinical suspicion. While owners may avoid additional diagnostics beyond decreased TT 4 concentration, treatment without appropriate diagnostics should be avoided. Cost of treatment is expensive over time, and inappropriate diagnosis may lead to delayed diagnosis of another disease

Drug Interference with Thyroid Testing Several medications can affect thyroid hormone concentrations; these drugs (except sulfonamides) rarely cause clinical hypothyroidism but can interfere with test results. ◦ Glucocorticoids decrease TT 4, f. T 4, and sometimes TSH in a dose- dependent manner. ◦ Such testing should be avoided when steroids are administered Phenobarbital can cause decreased TT 4 and f. T 4 and slightly increased TSH but does not cause clinical hypothyroidism. Sulfonamides block T 3 and T 4 synthesis and long-term administration cause clinical hypo- thyroidism with increased TSH. Aspirin decreases TT 4 and f. T 4 concentrations. Carprofen, meloxicam, and deracoxib do not appear to significantly affect thyroid function.

Medications Oral levothyroxine supplementation is initiated at 0. 02 mg/kg q 12 h. Dose may be based on surface area for larger dogs (0. 5 mg/m 2). Patients that respond to therapy and have appropriate TT 4 concen-trations can be switched to q 24 h therapy but may require q 12 h dose if response is not maintained. Precautions Because thyroxine increases cardiac oxygen demand, initial dose should be decreased by 25%– 50% in patients with cardiomyopathy.

Patient Monitoring Concentrations of TT 4 should be assessed 4 weeks (sooner in patients with clinical signs of hyperthyroidism) after initiation of levothyroxine ther- apy or dose adjustment. Adjustments should be made based on both TT 4 concentrations and clinical response to therapy. Once an appropriate treatment is established, TT 4 concentrations should be measured q 6 mo.
- Slides: 47