Human SkinIntegumentary System Prepared by Mr Shoup Skin

Human Skin-Integumentary System Prepared by Mr. Shoup
Skin In the complex human body: 15% of body weight-8 -9 pounds • Largest organ of the body • 1 inch of skin-19 million skin cells and 300+ sweat glands 1 square inch of skin on the hand sprouts: • 30 hairs • Holds 9 feet of blood vessels • 134 yards of nerves • 9, 000 nerve endings • 700 pain, heat, and pressure sensors. • 30 million bacteria live on skin at least 14 species of fungi live in between your toes. • No hair on the soles of your feet, palms of your hands and on your lips. • Lose 30, 000 -40, 000+ skin cells per hour, 1 million skin cells per day=1. 6 lbs per year. 1. 6 trillion skin cells we have. • 50%-80% of house dust.

Function of the Skin • • • Temperature control Protection against the elements Water Proof Receive stimulus-touch-pressure, cold, hot, pleasure and pain Manufacture vitamin D 8 -9 pounds of skin on the average human body. 12 -20 square feet of skin Skin grows from bottom up to the top layer. Melanin-pigment that gives skin its color.
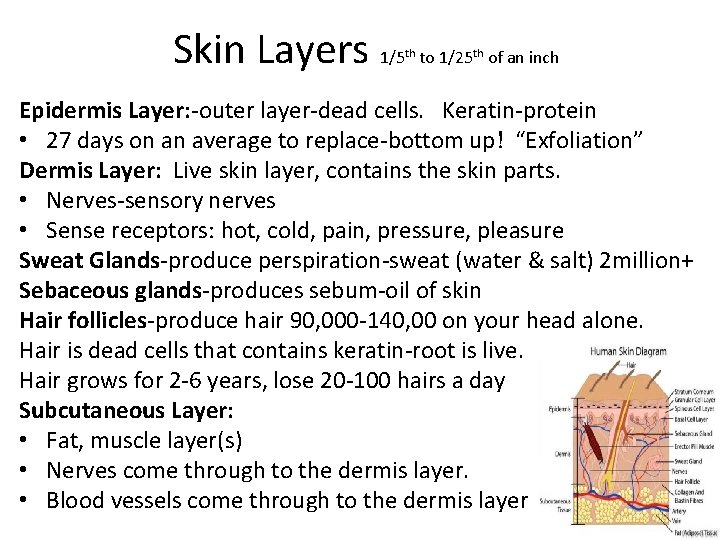
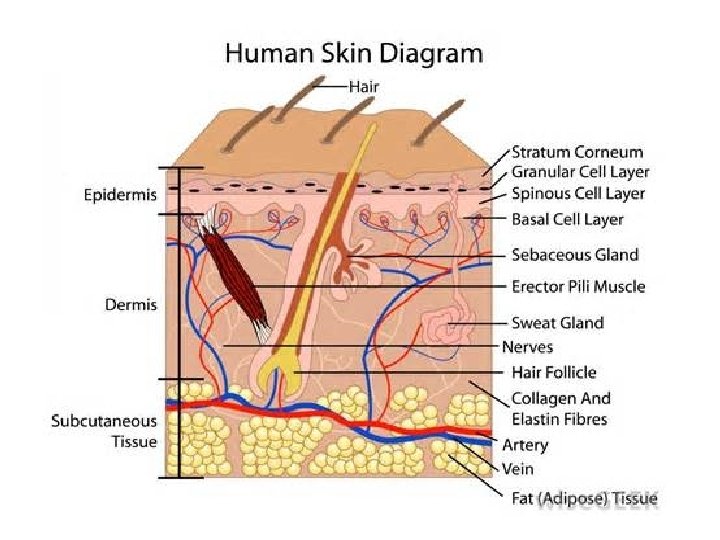
Skin Layers 1/5 th to 1/25 th of an inch Epidermis Layer: -outer layer-dead cells. Keratin-protein • 27 days on an average to replace-bottom up! “Exfoliation” Dermis Layer: Live skin layer, contains the skin parts. • Nerves-sensory nerves • Sense receptors: hot, cold, pain, pressure, pleasure Sweat Glands-produce perspiration-sweat (water & salt) 2 million+ Sebaceous glands-produces sebum-oil of skin Hair follicles-produce hair 90, 000 -140, 00 on your head alone. Hair is dead cells that contains keratin-root is live. Hair grows for 2 -6 years, lose 20 -100 hairs a day Subcutaneous Layer: • Fat, muscle layer(s) • Nerves come through to the dermis layer. • Blood vessels come through to the dermis layer

Skin Disorders Boils: • A boil is a skin infection that starts in a hair follicle or oil gland. Also referred to as a skin abscess, it is a localized infection deep in the skin. • A boil generally starts as a reddened, tender area. Over time, the area becomes firm and hard. • Eventually, the center of the abscess softens and becomes filled with infectionfighting white blood cells that the body sends via the bloodstream to eradicate the infection. • This collection of white blood cells, bacteria, and proteins is known as pus. • Finally, the pus "forms a head, " which can be surgically opened or spontaneously drain out through the surface of the skin. http: //www. medicinenet. com/boils_pictures_slideshow/article. htm • Summary: • Bacterial infection-Staphylococcus Aureus • Red bump/green core develops-dead blood cells, dead cells, protein forming pus sac. • Treatment: • Lancing and drained out/warm packs • Antibiotics may be prescribed
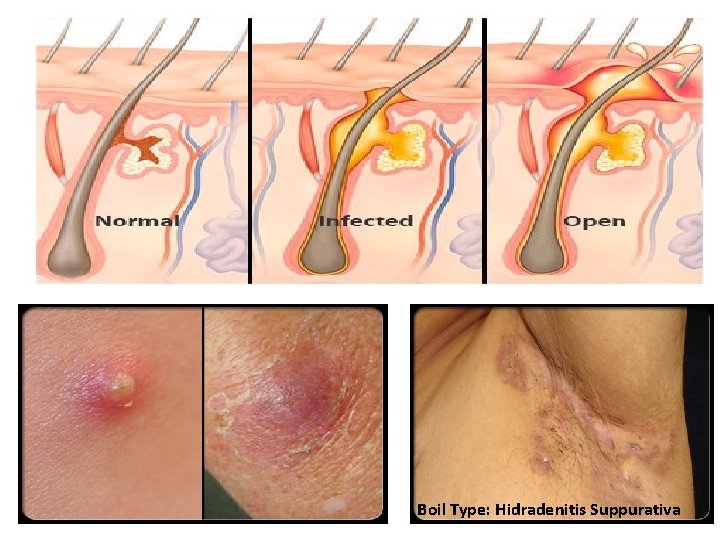
Boil Type: Hidradenitis Suppurativa
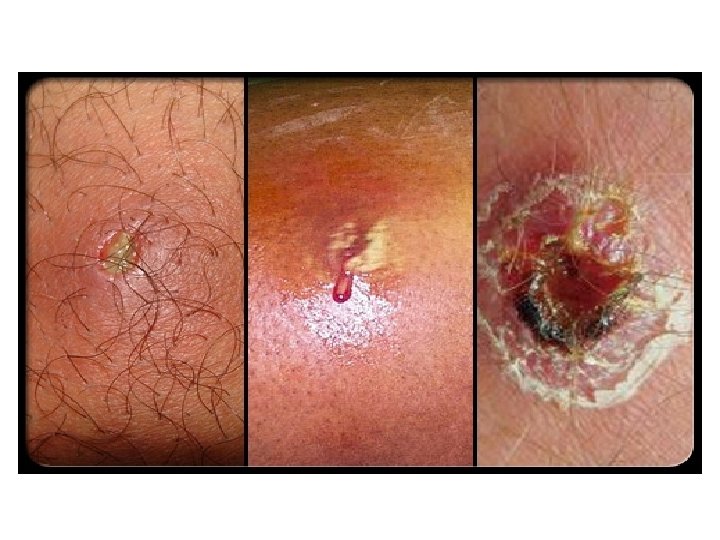

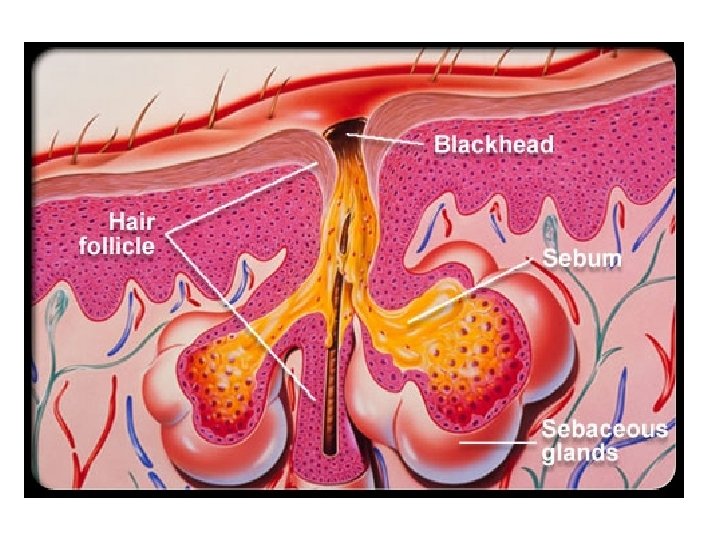
Acne begins with the development of a plug of hardened sebum that stops up the openings of the follicular pores on the face. These plugs seem to become darker with age, hence the term blackheads. When there is a layer of skin covering the follicular opening, the sebaceous plug usually does not darken and is called a "whitehead" by some. Once the follicle becomes clogged, it will enlarge as more skin and sebum is produced behind it. Bacterial contamination of this sebaceous mixture is common since bacteria normally inhabit the follicle. If stretched enough, the wall of the follicle ruptures. This enables this material access to the deeper tissues, which produces inflammation in the form of a pimple. http: //www. medicinenet. com/adult_acne_pictures_slideshow/article. htm
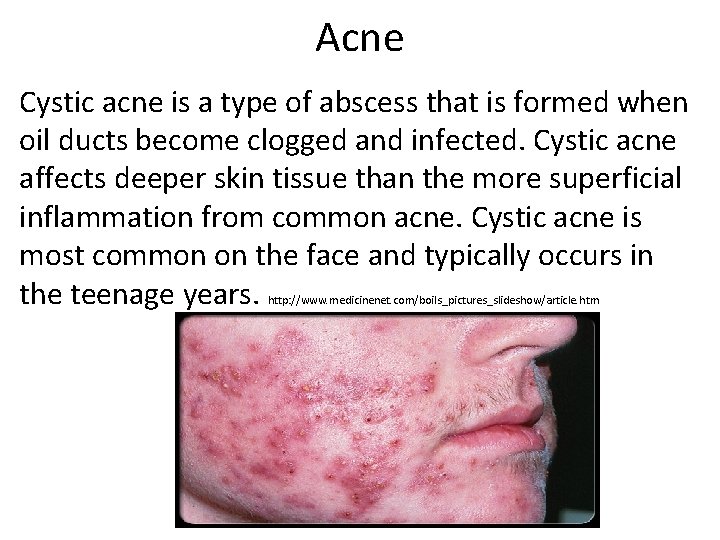
Acne Cystic acne is a type of abscess that is formed when oil ducts become clogged and infected. Cystic acne affects deeper skin tissue than the more superficial inflammation from common acne. Cystic acne is most common on the face and typically occurs in the teenage years. http: //www. medicinenet. com/boils_pictures_slideshow/article. htm

What Is Deep-Cyst Acne? • Cystic acne is common acne in its most severe form. • This form of acne is likely to result in permanent scarring. • It is quite rare in adults. • Most patients with cystic acne require aggressive medical therapy to prevent blemishes.
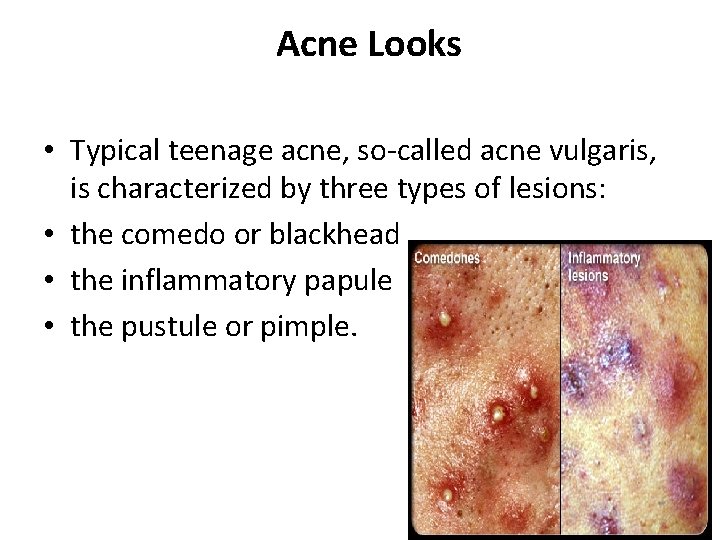
Acne Looks • Typical teenage acne, so-called acne vulgaris, is characterized by three types of lesions: • the comedo or blackhead • the inflammatory papule • the pustule or pimple.

Acne Treatment • Some over-the-counter and prescription acne creams help by unplugging the follicles. • Others - such as antibiotics - kill the bacteria that move into the follicles. • The oral retinoid Accutane works differently by reducing the amount of oil secreted by glands in the skin. • http: //www. medicinenet. com/image-collection/acne_picture/picture. htm • Keep hands off face • Wash with water and soap • Keep hair off forehead
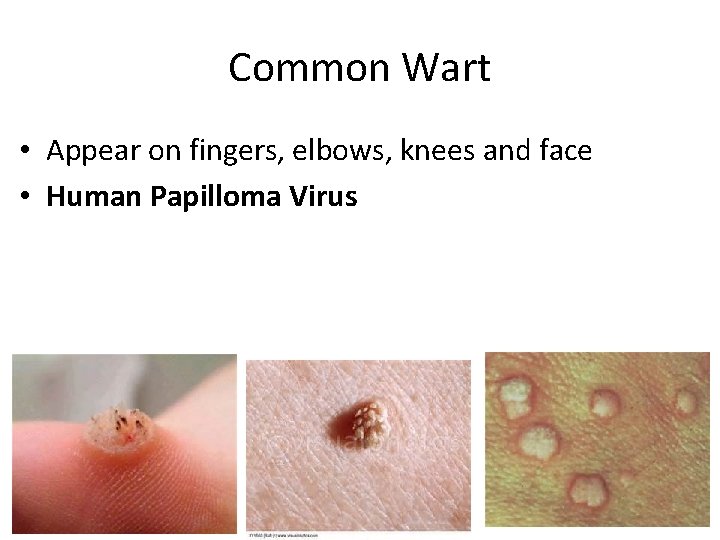
Common Wart • Appear on fingers, elbows, knees and face • Human Papilloma Virus

Plantar Warts • Plantar warts are different from most other warts. • They tend to be flat and cause the buildup of the top layer of the skin (that has to be peeled away before the plantar wart itself can be seen. • They can be quite painful. • Plantar warts are caused by human papillomavirus (HPV) type 1, 2, 4 and 63 and tend to affect teenagers. http: //www. medicinenet. com/image- collection/plantar_warts_picture/picture. htm
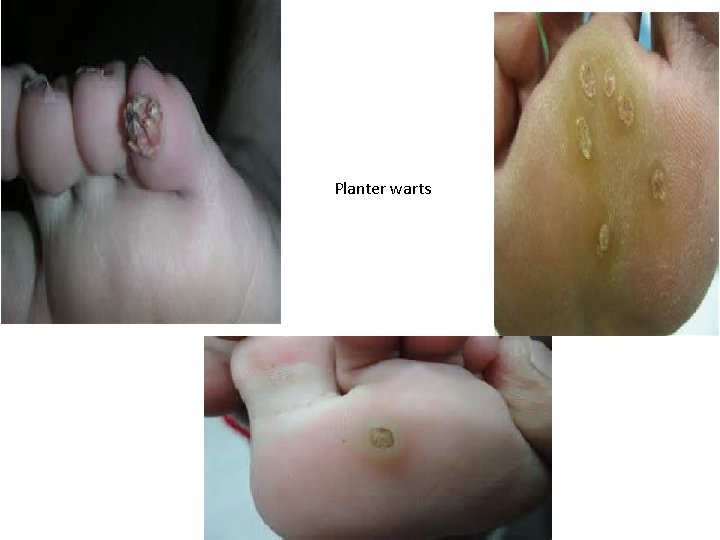
Planter warts

Wart Treatments • Over-the-counter treatments for warts include salicylic-acid preparations and freezing kits. • Salicylic-latin word from the willow tree • Duct Tape Therapy-causes immune system to attack wart • Raw garlic cloves-may have antiviral affects • Chemical-podophyllin • Freezing-cryosurgery • Burning-electro cautery • Surgical/Laser Treatments

Genital Warts • Genital warts (technically known as condylomata acuminatum) are most commonly associated with two human papilloma virus types, HPV-6 and HPV-11. • Sexually transmitted, high-risk human papilloma viruses include types 16, 18, 31, 33, 35, 39, 45, 51, 52, 56, 58, 59, 68, 69, and possibly a few others. These high-risk types of human papilloma viruses cause growths that are usually flat and nearly invisible, as compared with the warts caused by types HPV-6 and HPV-11. • These can be spread also by close skin to skin contact, but mostly by sexual behavior.
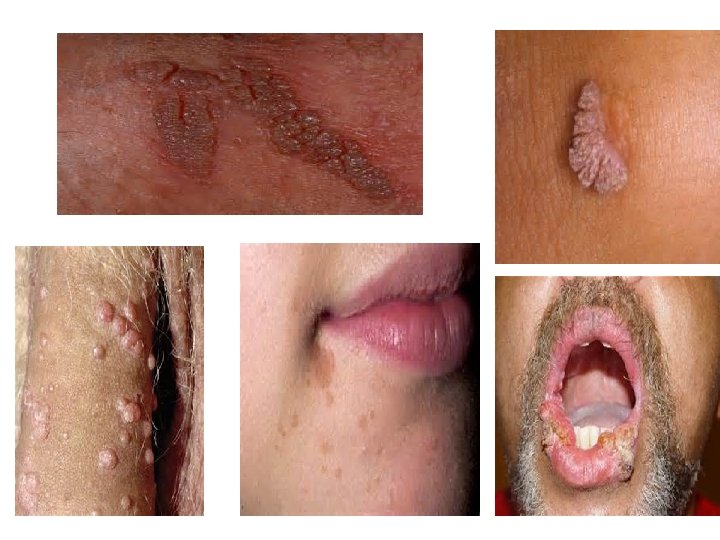
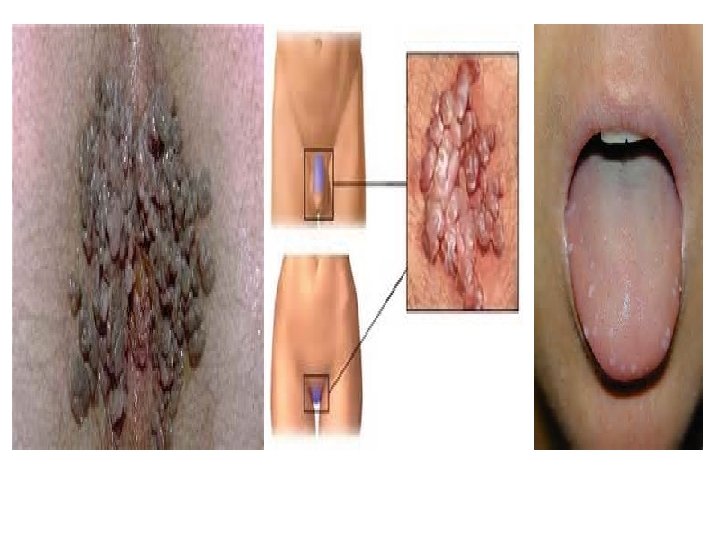

Genital Warts A treatment that can be administered by the patient is a 0. 5% solution or gel of podofilox (Condylox). The medication is applied to the warts twice per day for 3 days followed by 4 days without treatment. Treatment should be continued up to 3 to 4 weeks or until the lesions are gone. Podofilox may also be applied every other day for a total of three weeks

Genital Warts Alternatively, a 5% cream of imiquimod (Aldara, a substance that stimulates the body's production of cytokines, chemicals that direct and strengthen the immune response) is likewise applied by the patient three times a week at bedtime, and then washed off with mild soap and water 6 to 10 hours later. The applications are repeated for up to 16 weeks or until the lesions are gone.

Genital Warts http: //www. medicinenet. com/script/main/art. asp? articlekey=3813 Only an experienced physician can perform some of the treatments for genital warts. These include, for example, placing a small amount of a 10% to 25% solution of podophyllin resin on the lesions, and then, after a period of hours, washing off the podophyllin. The treatments are repeated weekly until the genital warts are gone.

Genital Warts http: //www. medicinenet. com/script/main/art. asp? articlekey=3813 An 80% to 90% solution of trichloroacetic acid (TCA) or bichloracetic acid (BCA) can also be applied weekly by a physician to the lesions. Injection of 5 -flurouracil epinephrine gel into the lesions has also been shown to be effective in treating genital warts. Interferon alpha, a substance that stimulates the body's immune response, has also been used in the treatment of genital warts. Treatment regimens involve injections of interferon into the lesion every other day over a period of 8 to 12 weeks. Alternative methods include cryotherapy (freezing the genital warts with liquid nitrogen) every 1 to 2 weeks, surgical removal of the lesions, or laser surgery. Laser surgery and surgical excision both require a local or general anesthetic, depending upon the extent of the lesions
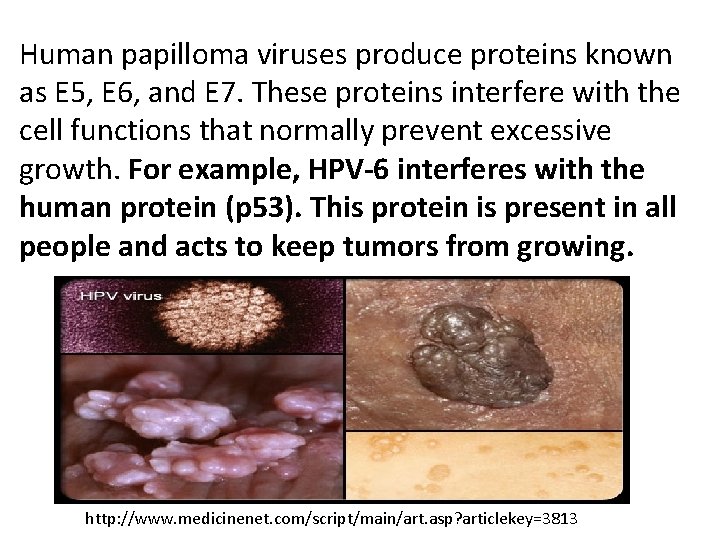
Human papilloma viruses produce proteins known as E 5, E 6, and E 7. These proteins interfere with the cell functions that normally prevent excessive growth. For example, HPV-6 interferes with the human protein (p 53). This protein is present in all people and acts to keep tumors from growing. http: //www. medicinenet. com/script/main/art. asp? articlekey=3813

Prevention of Genital Warts A vaccine is available against common HPV types associated with the development of genital warts and cervical and an genital carcinomas. This vaccine (Gardasil 9) has received FDA approval for use in females between 9 and 26 years of age and in males aged 9 to 15. It confers immunity against 9 HPV types: 6, 11, 16, 18, 31, 33, 45, 52, and 58. An earlier version of this vaccine (Gardasil) is directed at 4 common HPV types (6, 11, 16, 18). Another vaccine directed at HPV types 16 and 18, known as Cervarix, has been approved for use in females aged 10 to 15. http: //www. medicinenet. com/script/main/art. asp? articlekey=3813 Abstinence Condom Use

Impetigo • A bacterial skin infection caused by the staphylococcus or, more rarely, streptococcus bacteria. • The first sign of impetigo is a patch of red, itchy skin. • Pustules develop on this area, soon forming crusty, yellow-brown sores that can spread to cover entire areas of the face, arms, and other body parts. • Honey-colored crust that forms after the pustules burst. • Most patients are children. • Treatment is by antibiotics.

• Symptoms usually began 1 -3 days after infection. • Sores (lesions) begin as small red spots, usually on the face (especially around the nose and mouth), but can appear anywhere on the body. • The sores are often itchy, but usually not painful. • The sores develop into blisters that break open and ooze fluid -- this fluid contains infectious bacteria that can infect others if they have contact with it. • After a few days, the ruptured blisters form a flat, thick, honey-colored (yellowish-brown) crust that eventually disappears, leaving red marks that heal without scarring. • There may be swollen glands (enlarged lymph nodes), but usually no fever. NYS Health Department
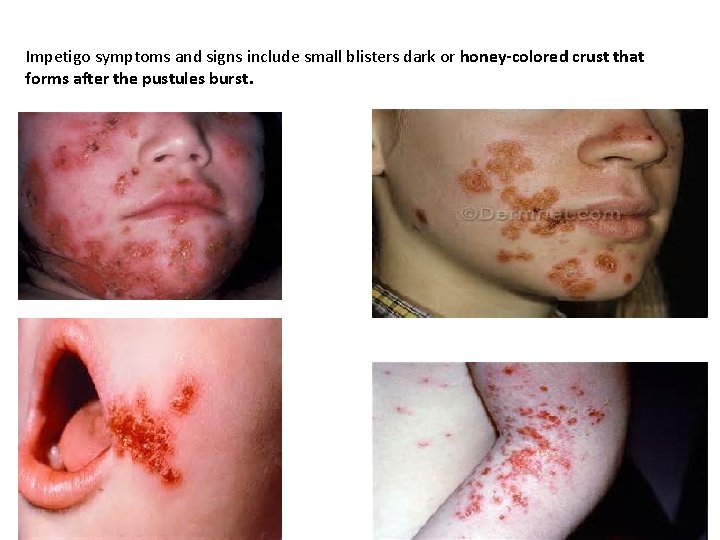
Impetigo symptoms and signs include small blisters dark or honey-colored crust that forms after the pustules burst.

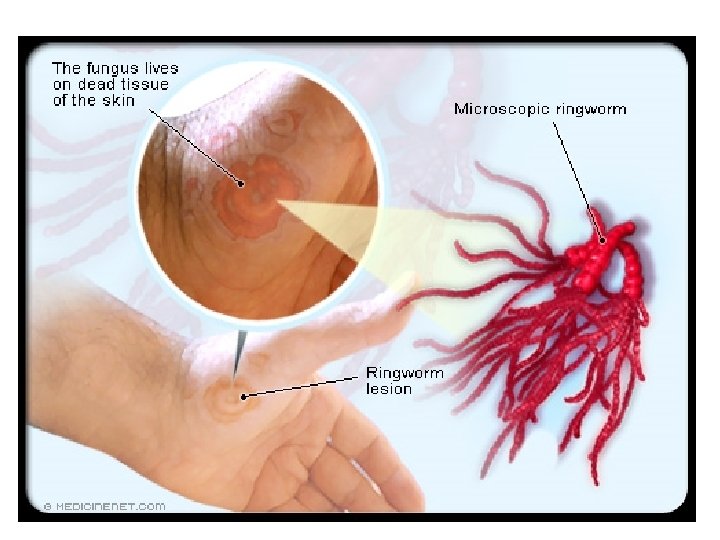
Ringworm • Ringworm is a common skin disorder otherwise known as tinea. (Latin-Growing worm) • While there are multiple forms of ringworm, the most common affect the: • Fungus infections: • Skin on the body (tinea corporis), • The scalp (tinea capitis), • The feet (tinea pedis, or "athlete's foot"), or • The groin (tinea cruris, or "jock itch").

How to get Ringworm? • Fungus infection • Ringworm is highly contagious and can be spread multiple ways. • You can get it from an infected person • Infected Animal • From an object • From the soil • Heat and moisture help fungi grow and thrive, which makes them more common in areas of frequent sweating as well as skin folds such as those in the groin or between the toes. • This also accounts for their reputation as being caught from contaminated items such as toilet articles, clothing, pool surfaces, showers, and locker rooms.

Ringworm Cause and Symptoms Cause by: Fungal infection Symptoms: • Itchy, red raised, scaly patches that may blister and ooze • The patches often have sharply defined edges • Often red ring on the out side with normal skin tone in the center. This creates the appearance of the ring.
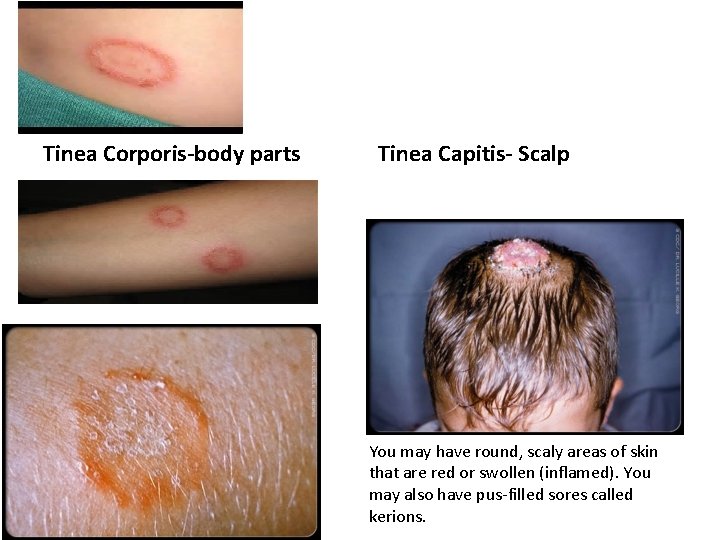
Tinea Corporis-body parts Tinea Capitis- Scalp You may have round, scaly areas of skin that are red or swollen (inflamed). You may also have pus-filled sores called kerions.
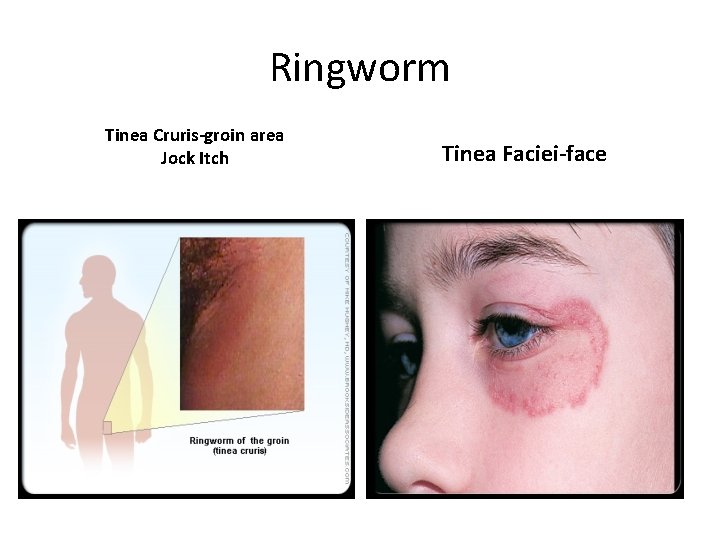
Ringworm Tinea Cruris-groin area Jock Itch Tinea Faciei-face
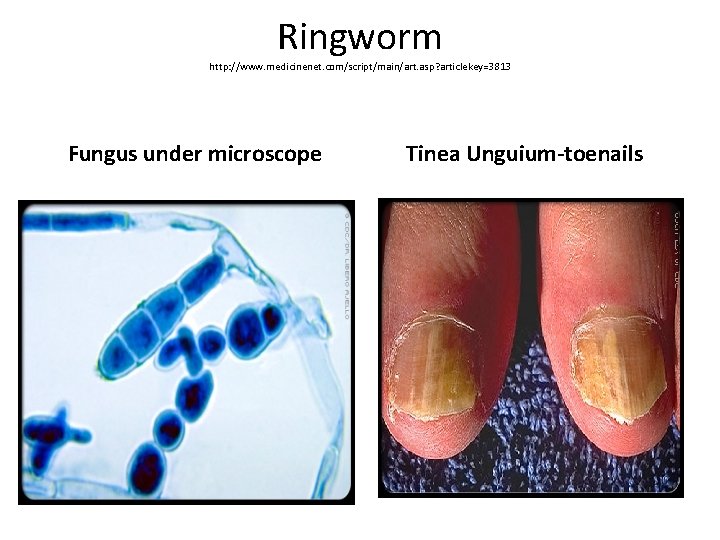
Ringworm http: //www. medicinenet. com/script/main/art. asp? articlekey=3813 Fungus under microscope Tinea Unguium-toenails

Treatments • The health care provider may swab the area and send it for a culture. • Wood's lamp examination is a test that uses ultraviolet (UV) light to look at the skin closely. Different creams and solutions: • • Clotrimazole-OTC Cruex, Desenex, Lotrimin creams, lotions, and solutions. Miconazole-Monistat Derm cream Ketoconazole-Nizoral cream Tebinafine-Lamisil cream and solution-OTC Itaconazole-Sporanox Fluconazole-Diflucan http: //www. medicinenet. com/script/main/art. asp? articlekey=3813

Psoriasis • Psoriasis is an autoimmune disorder where rapid skin cell reproduction results in raised, red, dry, and scaly patches of skin. • It is not contagious. • It most commonly affects the skin on the elbows, knees, and scalp, though it can appear anywhere on the body. • Anyone can have psoriasis. About 7. 5 million people in the U. S. are affected, and it occurs equally in men and women. • Psoriasis can occur at any age but is most often diagnosed between the ages of 15 to 25. • It is more frequent in Caucasians. • The cause of psoriasis is unknown
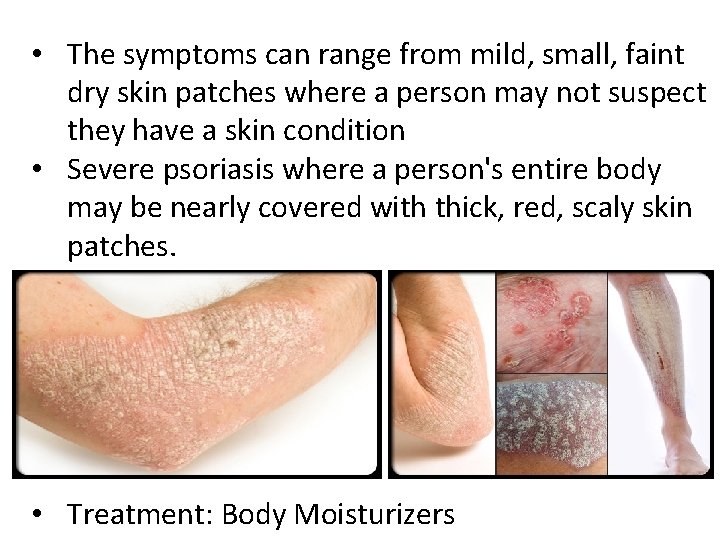
• The symptoms can range from mild, small, faint dry skin patches where a person may not suspect they have a skin condition • Severe psoriasis where a person's entire body may be nearly covered with thick, red, scaly skin patches. • Treatment: Body Moisturizers

MRSA-Methicillin-Resistant Staphylococcus Aureus • MRSA is a staph bacterium that certain antibiotics in the penicillin family should be able to treat, but cannot. • When the infection is resistant to the medication, it is called resistance. • However, other non-penicillin antibiotics can effectively treat most MRSA infections.

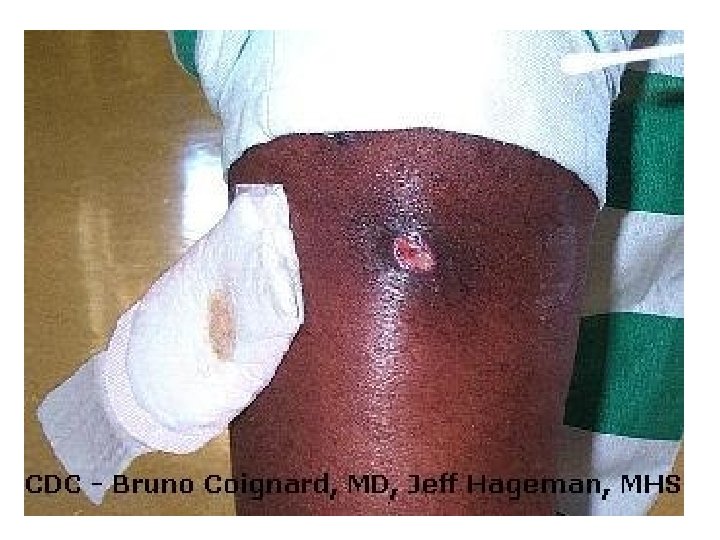
Facts About MRSA • MRSA infections commonly occur where there is a break in the skin (for example, a cut or wound), especially in areas covered by hair (for example, the beard area, back of the neck, armpit, groin, legs, or buttocks) • MRSA may look like a bump on the skin that may be red, swollen, warm to the touch, painful, filled with pus, or draining. The pus or drainage contains the infectious bacteria that can be spread to others. People with MRSA may have a fever. • MRSA can be very serious and even cause death. • MRSA can cause pneumonia or severe infections of the blood, bones, surgical wounds, heart valves, and lungs. • MRSA can be fatal if not identified and treated with effective antibiotics. • Most often, MRSA is transmitted by direct skin-to-skin contact with someone who has the infection. • MRSA can be spread by indirect contact too (for example contact with a mat that has infected drainage on it or by sharing a towel or cell phone with someone who has MRSA). Because of this, never share personal hygiene and health items.

Sun Care to the Skin Two types of ultraviolet radiation that reach the Earth: 1. Overexposure to ultraviolet (UVA) light 2. Overexposure to (UVB) light-sunburn • Never use a tanning bed, booth or sun lamp. • Wear a wide brimmed hat, long-sleeved shirts and long pants whenever possible. • Wear sunglasses that block both type of UV rays (UVA and UVB). Sunglasses will protect the tender skin around the eyes and reduce the risk of cataracts. • Use a sunscreen labeled "broad-spectrum" with a sun protection factor (SPF) rating of 15 or higher. SPF 15 blocks out 93% of UV rays, while an SPF 30 blocks out 97% of UV rays. • Apply the sunscreen to dry skin 15 -30 minutes before going outdoors and again after swimming or perspiring. • One ounce of sunscreen, enough to fill a shot glass, is considered the amount needed to completely cover the exposed areas of the body. • Avoid direct sun at midday, between 10 a. m. and 4 p. m. , when the sun's rays are strongest. • Follow these tips on cloudy days too! Clouds do not block most UV rays. NYS Health Department

Melanoma-Skin Cancer Begins usually before the age of 18 -Why? ? ? • Three types of skin cancer: 1. Squamous-thin, flat cells at the top of epidermis layer-Lip, ears, fingers, neck, head areas 2. Basal-round cells at the middle of the epidermis layer. Face, neck, Arms/Legs areas 3. Melanoma-the bottom layer of the epidermis layer. Usually begins in a mole • New York State: • Melanoma is the eighth most common type of cancer among both men and women in NYS. • More than 3, 700 NYS residents are diagnosed with melanoma annually. • Each year about 500 New Yorkers die from melanoma. • For adults age 20 to 34 years, melanoma ranks among the top five cancers. • • • United States: Skin cancer (all types combined) is the most commonly occurring cancer with over two million cases a year. The number of new cases of melanoma in the US is on the rise. An estimated 9, 000 people die annually of melanoma in the U. S. Melanoma is the most common cancer in young women aged 25 -29. NY State Health Department

Cancer signs for Moles • What’s a mole? When cells in the skin grow in a cluster instead of being spread throughout the skin-melanocytes. • Normal to have 10 -40 moles by adulthood • ABCD Rules: • A=Asymmetry-one half of mole does not match the other half. • B=Border-The edges are uneven, notched or blurred • C=Color-The color is not consistent throughout the mole • D=Diameter-The diameter is greater than ¼ inch or has been growing. • E=Evolution
- Slides: 46