Human Reproduction Male reproductive system Functions of the























- Slides: 86

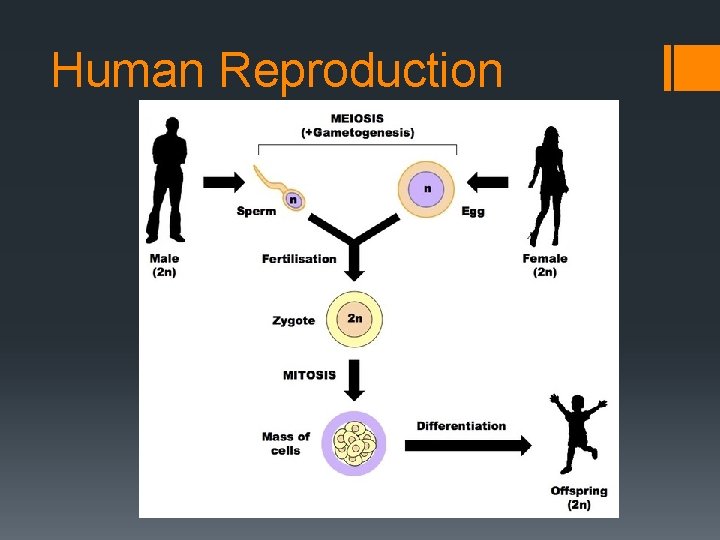
Human Reproduction

Male reproductive system

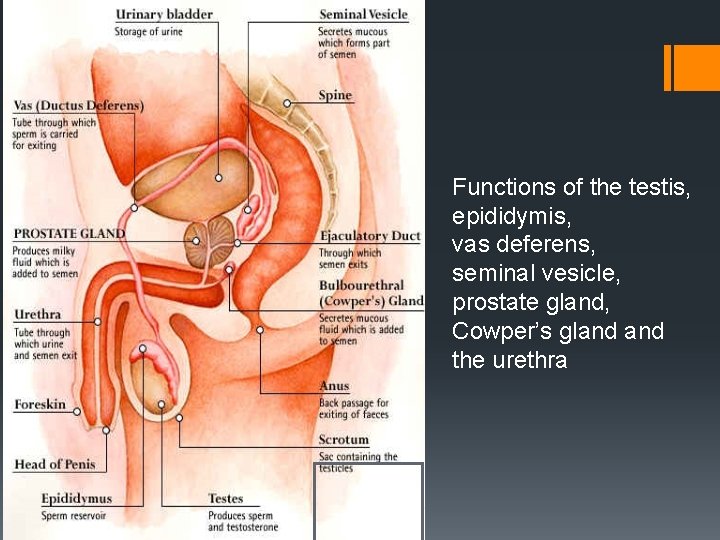
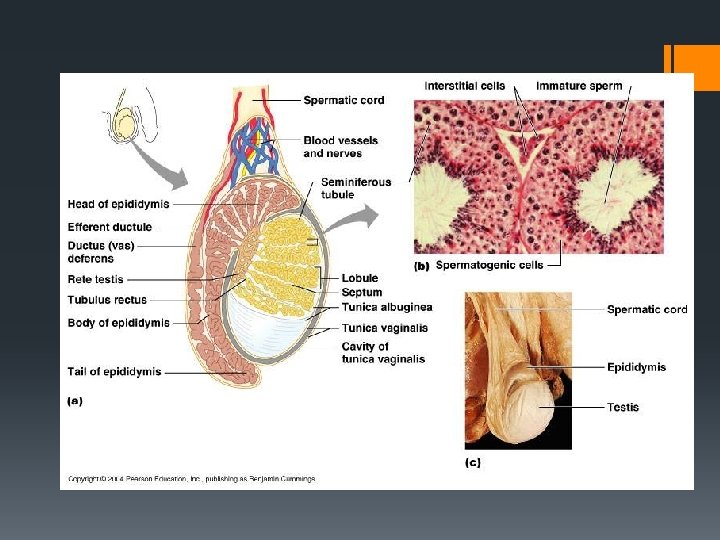
Functions of the testis, epididymis, vas deferens, seminal vesicle, prostate gland, Cowper’s gland the urethra

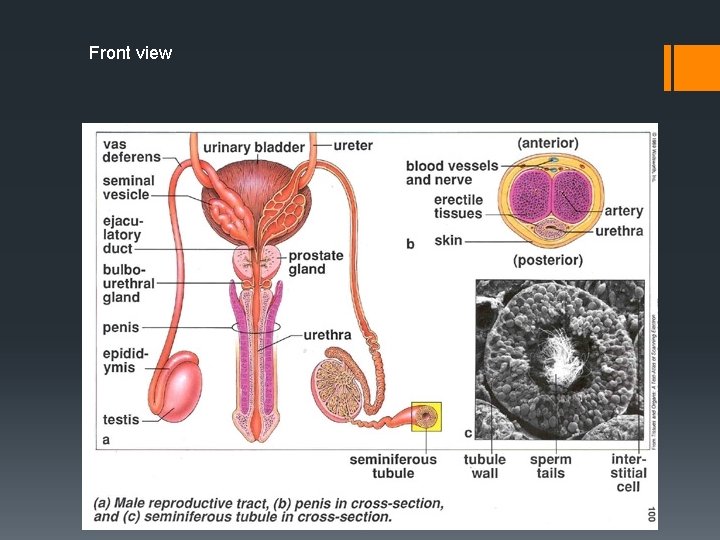
Front view

Three additional glands § Seminal vesicles: Provides carbohydrates to serve as an energy source for sperm § Prostate gland: Produces an alkaline fluid to neutralise the acidity of the vagina. § Cowper’s gland: provides mucus to help with sperm movement.


List the main changes that occur in male characteristics during puberty under the influence of testosterone.

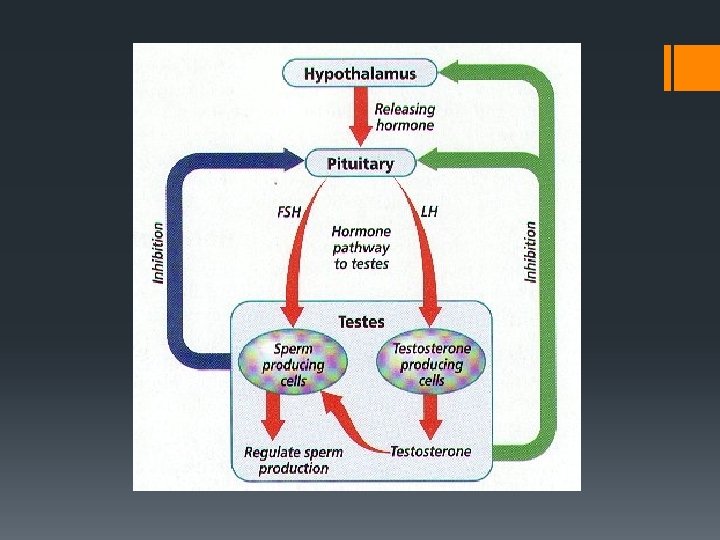
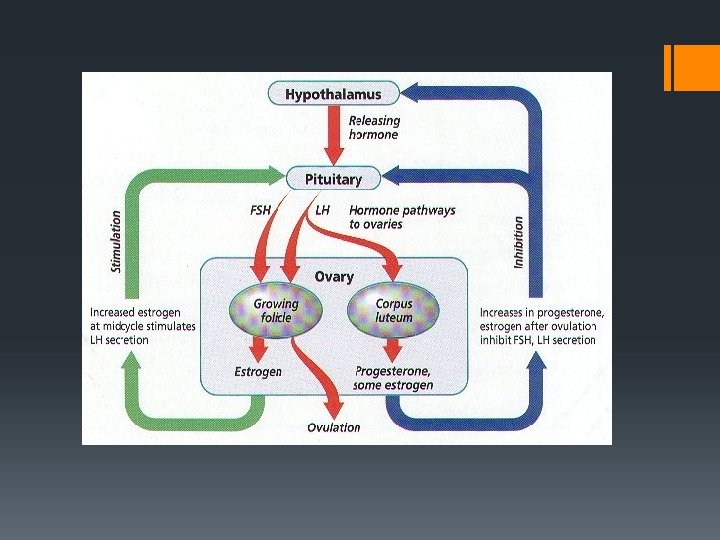
Male hormones § Testosterone: § produced by cells of Leydig in the testes § secondary sex characteristics at puberty § needed for sperm production § maintain reproductive organs § sex drive or libido § FSH: § Produced by hypophysis § Stimulates spermatogenesis § LH: § Produced by hypophysis § Stimulates the secretion of testosterone Don’t worry about these for now…

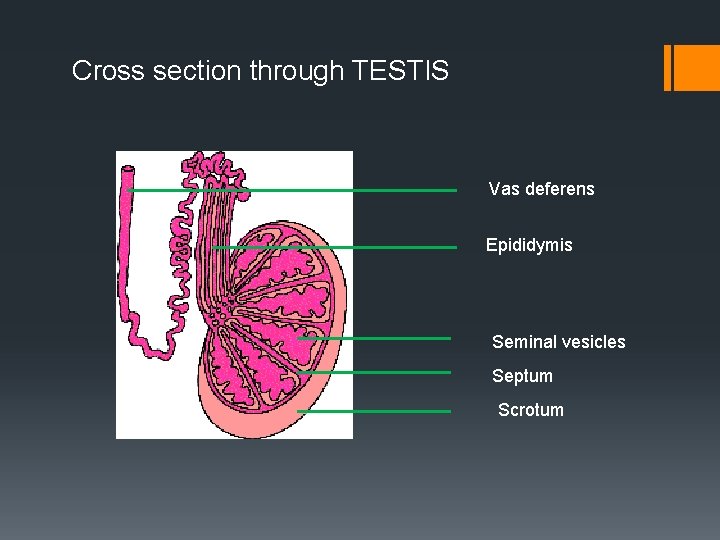
Cross section through TESTIS Vas deferens Epididymis Seminal vesicles Septum Scrotum


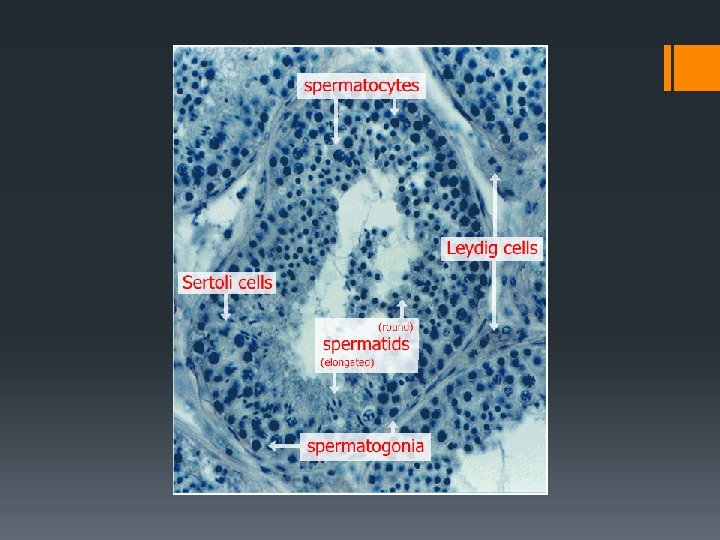
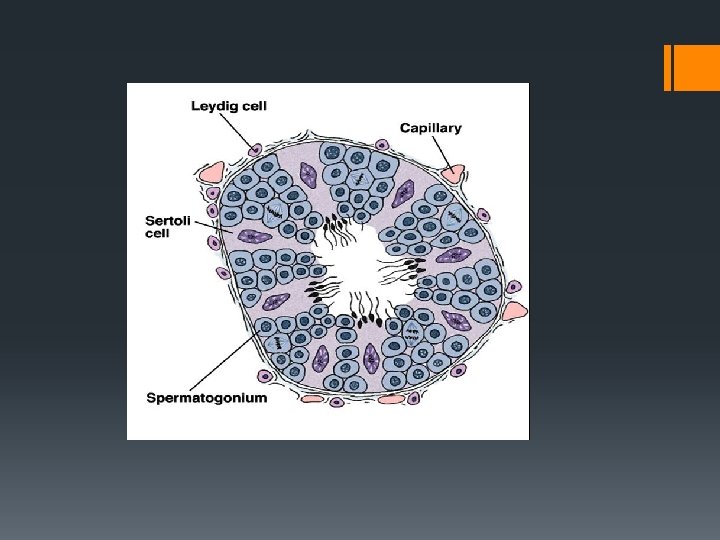
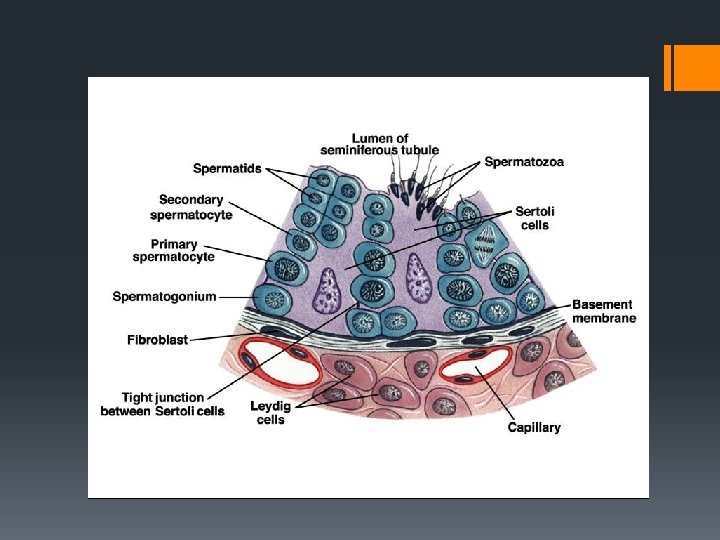
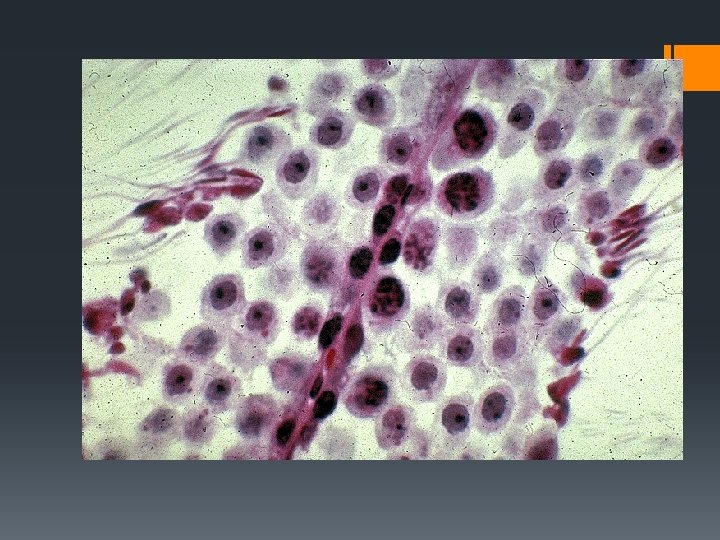
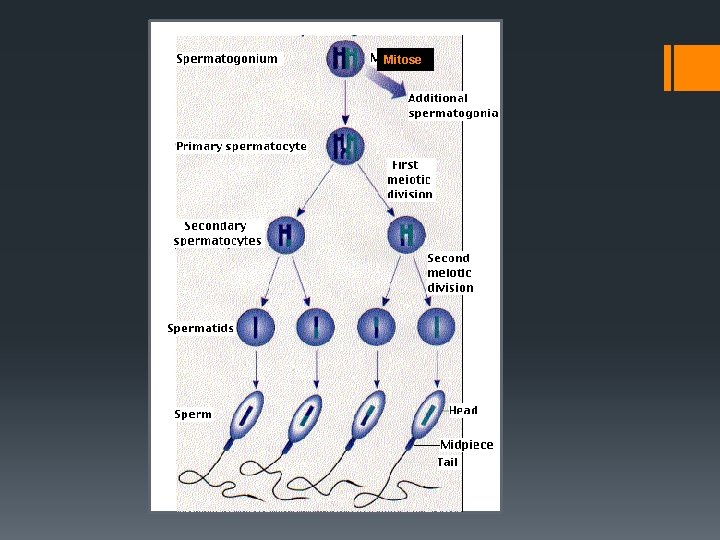
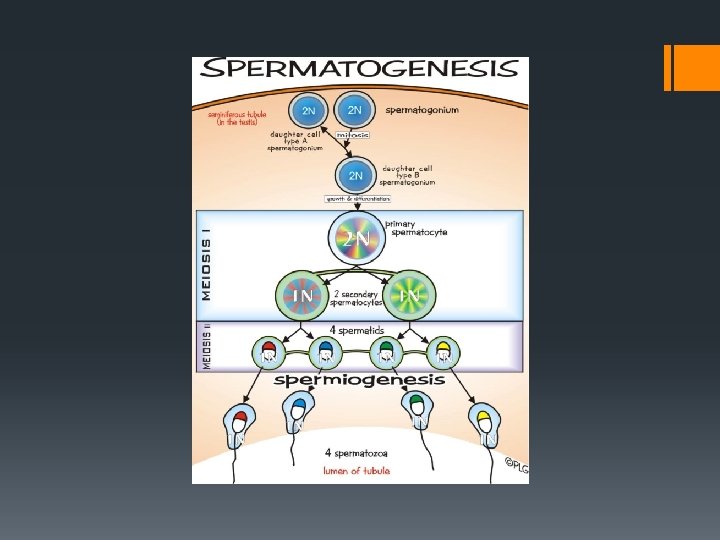
Gametogenesis Gamete Creation Spermatogenesis: Under the influence of testosterone, diploid cells in the seminiferous tubules of the testes undergo meiosis to form haploid sperm cells





Mitose



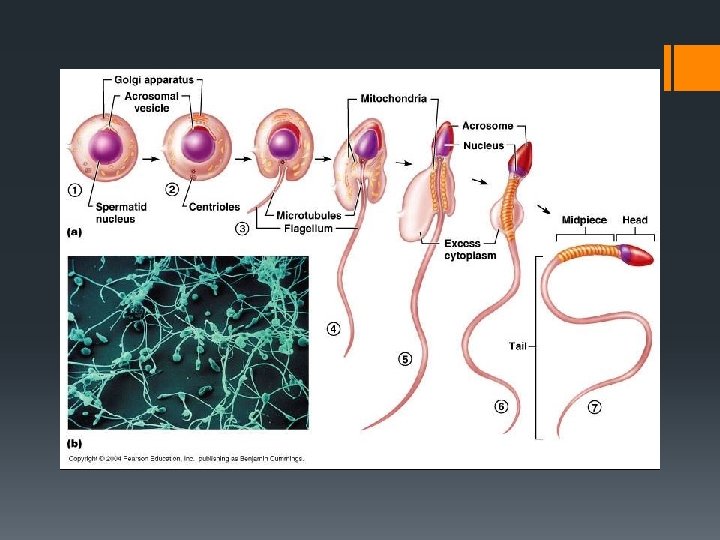
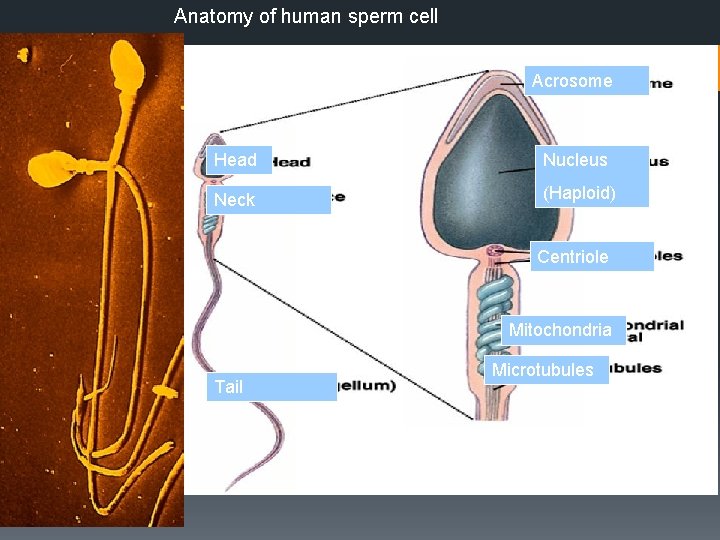
Anatomy of human sperm cell Acrosome Head Nucleus Neck (Haploid) Centriole Mitochondria Tail Microtubules

Female reproductive system

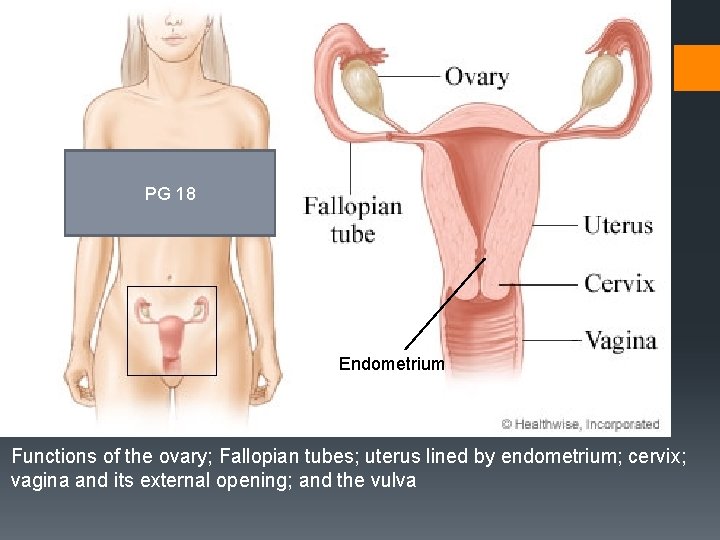
PG 18 Endometrium Functions of the ovary; Fallopian tubes; uterus lined by endometrium; cervix; vagina and its external opening; and the vulva

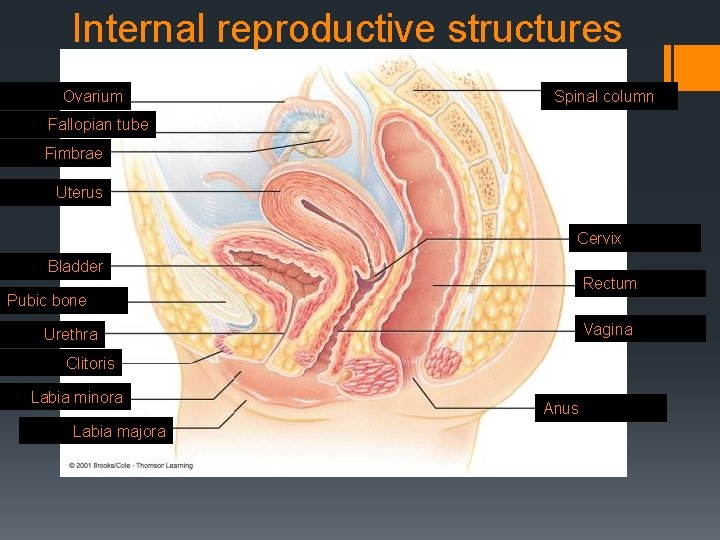
Internal reproductive structures Ovarium Werwelkolom Spinal column Fallopian tube Fimbrae Uterus Cervix Bladder Rectum Pubic bone Vagina Urethra Clitoris Labia minora Labia majora Anus

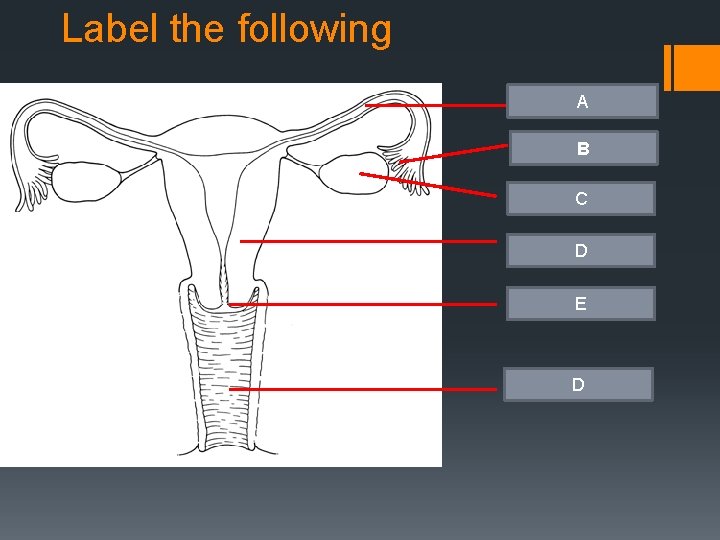
Label the following A tube Fallopian FALLOPIAN tubes Fimbrae. B Ovary C Uterus D Cervix E Vagina D


List the main changes that occur in female characteristics during puberty under the influence of oestrogen.

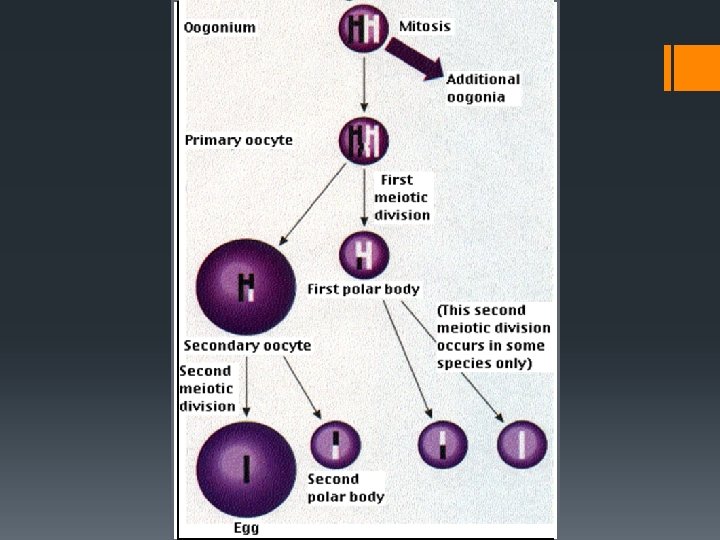
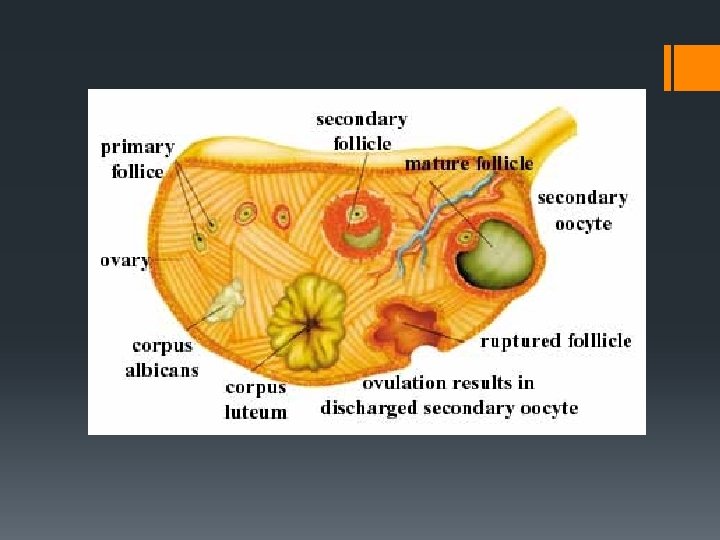
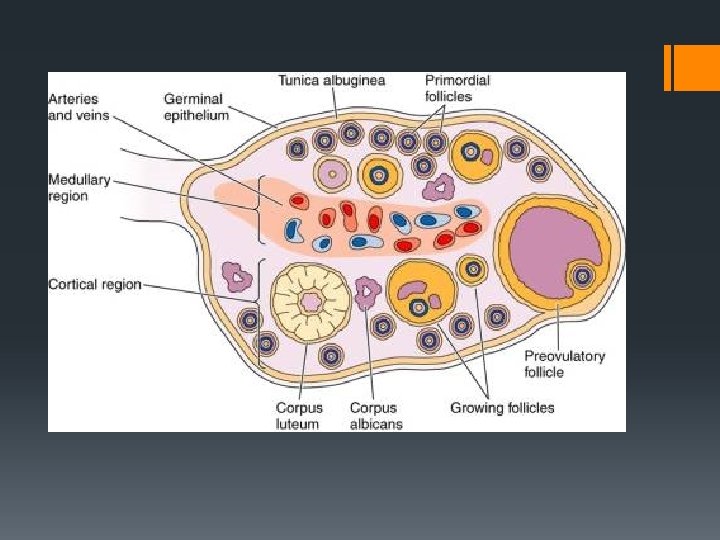
oogenesis Egg Creation Oogenesis: Under the influence of FSH diploid cells in the ovary undergo mitosis to form numerous follicles. One cell inside a follicle enlarges and undergoes meiosis. Of the four cells that are produced, only one survives to form a mature, haploid ovum.


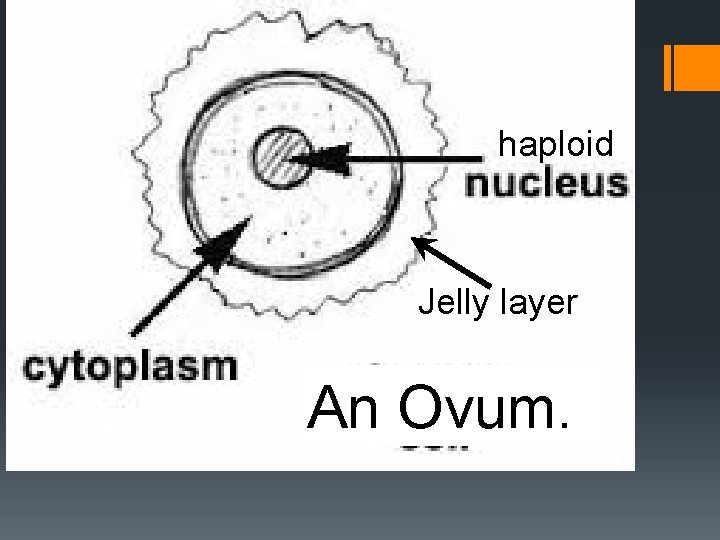
haploid Jelly layer An Ovum.

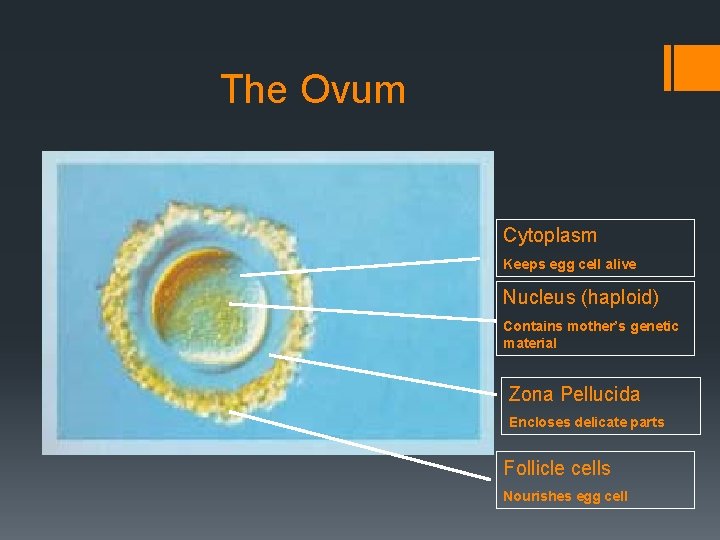
The Ovum Cytoplasm Keeps egg cell alive Nucleus (haploid) Contains mother’s genetic material Zona Pellucida Encloses delicate parts Follicle cells Nourishes egg cell

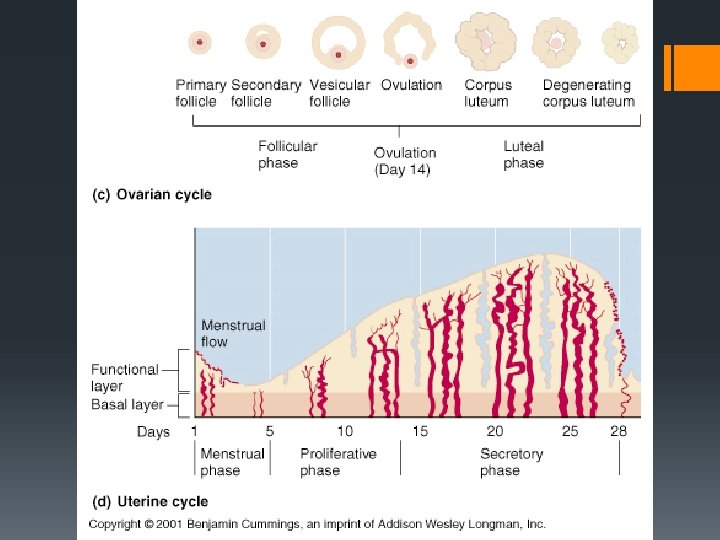
Menstrual cycle Includes uterine (uterus lining) and ovarian (ovary) cycles

Hormonal control of the menstrual cycle Copy and complete the table below. Gland Hormone F O L P Function

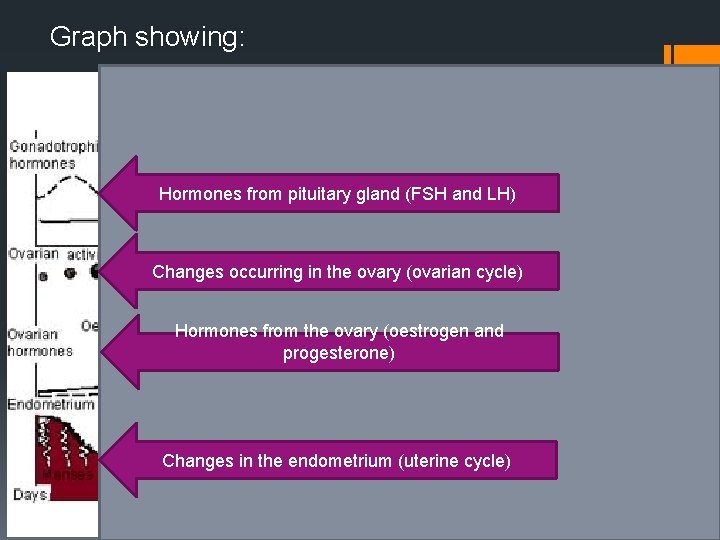
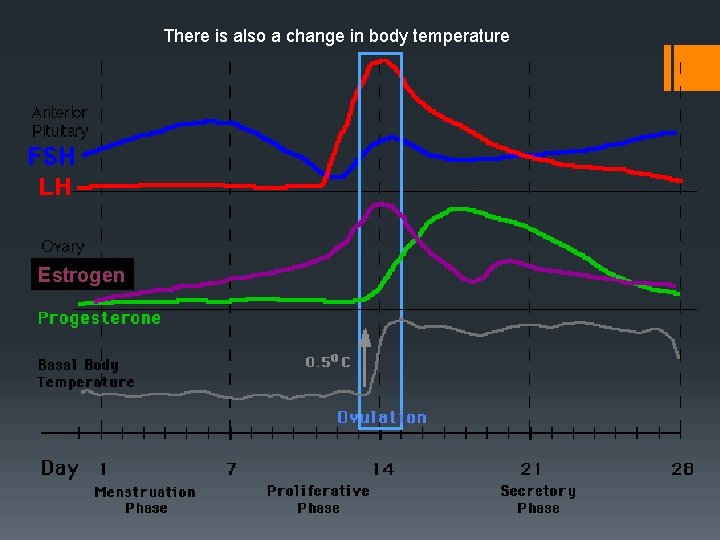
Graph showing: Hormones from pituitary gland (FSH and LH) Changes occurring in the ovary (ovarian cycle) Hormones from the ovary (oestrogen and progesterone) Changes in the endometrium (uterine cycle)

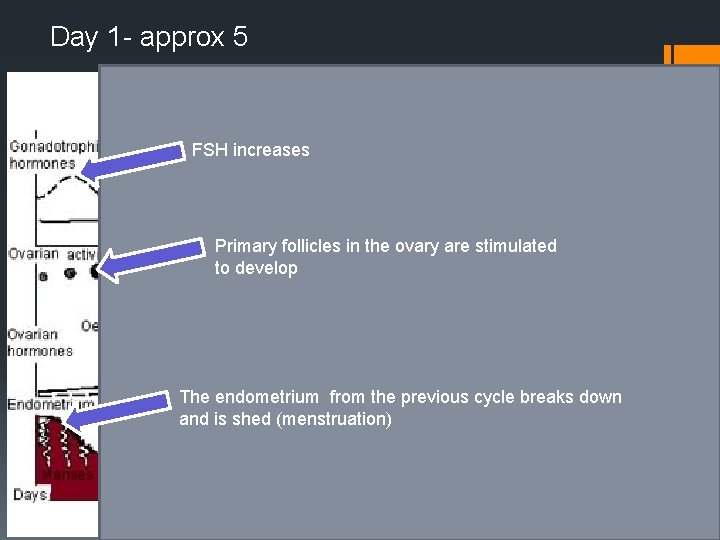
Day 1 - approx 5 FSH increases Primary follicles in the ovary are stimulated to develop The endometrium from the previous cycle breaks down and is shed (menstruation)

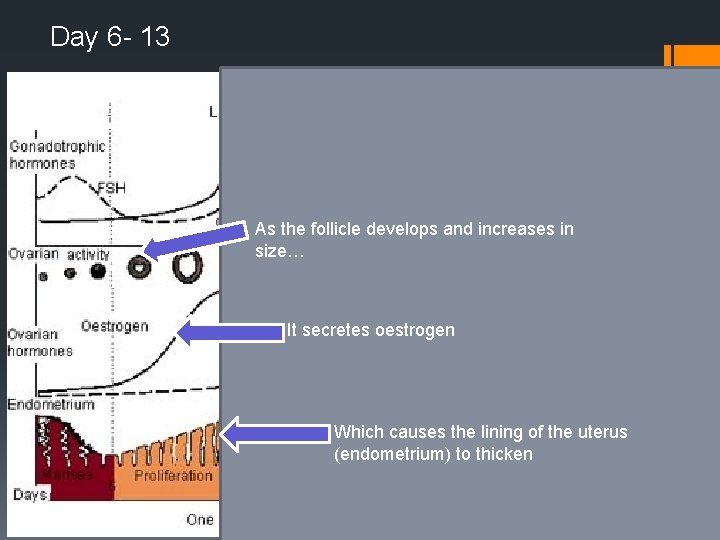
Day 6 - 13 As the follicle develops and increases in size… It secretes oestrogen Which causes the lining of the uterus (endometrium) to thicken

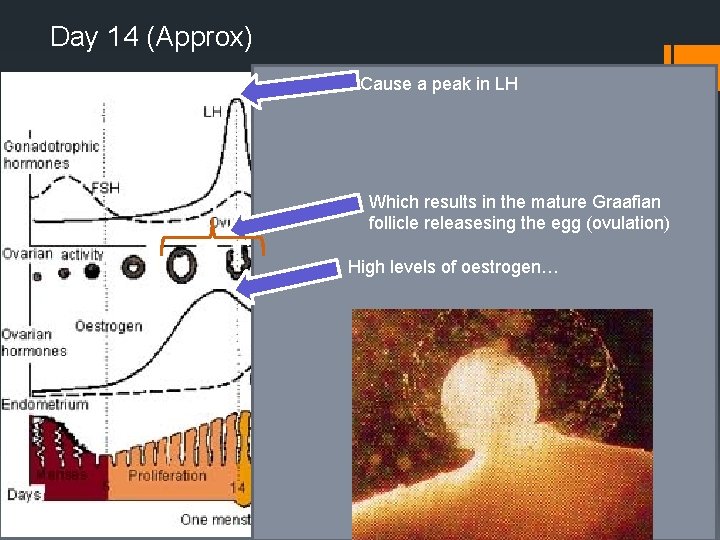
Day 14 (Approx) Cause a peak in LH Which results in the mature Graafian follicle releasesing the egg (ovulation) High levels of oestrogen…

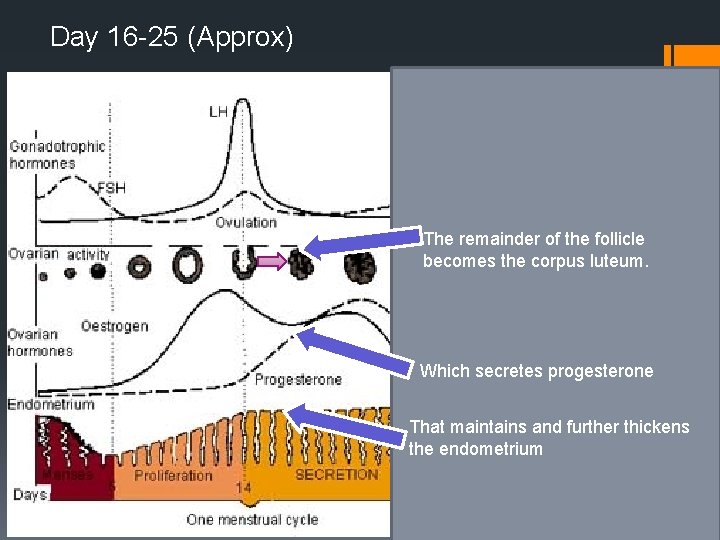
Day 16 -25 (Approx) The remainder of the follicle becomes the corpus luteum. Which secretes progesterone That maintains and further thickens the endometrium

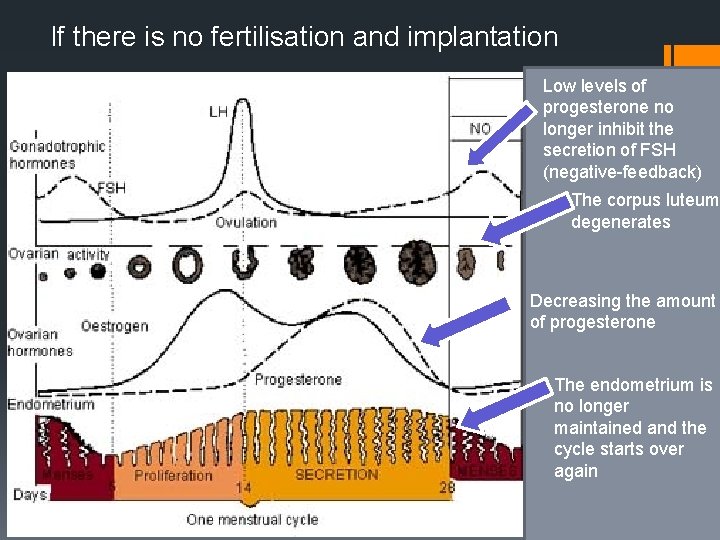
If there is no fertilisation and implantation Low levels of progesterone no longer inhibit the secretion of FSH (negative-feedback) The corpus luteum degenerates Decreasing the amount of progesterone The endometrium is no longer maintained and the cycle starts over again

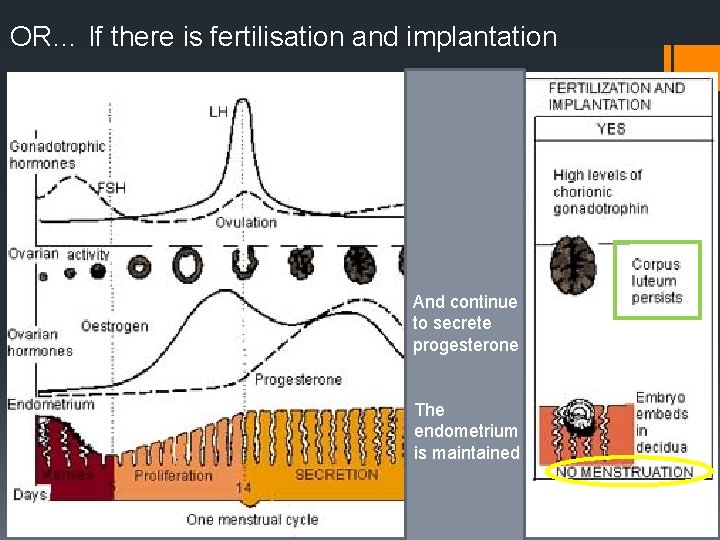
OR… If there is fertilisation and implantation And continue to secrete progesterone The endometrium is maintained

There is also a change in body temperature Estrogen

The events in the ovarian cycle: § Development of the Graafian follicle § Ovulation § Formation of the corpus luteum The events in the uterine cycle: § Changes that take place in the thickness of the endometrium § Menstruation


Females hormones 1 § FSH (Follicle stimulating hormone): § stimulates oogenesis § development of follicle § LH (Luteinizing hormone): § triggers ovulation § development and maturation of corpus luteum

Female hormones 2 § Estrogen: § released by the follicles later by corpus luteum and placenta during pregnancy § secondary sex characteristics at puberty. § maintain reproductive organs § causes the lining of the uterus, the endometrium, to grow and thicken in preparation of implantation of a fertilized egg. § prepare breasts for lactation (milk production) § build-up of estrogen inhibits FSH production § build-up of estrogen stimulates LH production

Female hormones 3 § Progesterone: § released by corpus luteum and released from placenta, if pregnant § causes the lining of the uterus, the endometrium, to grow and thicken in preparation of implantation of a fertilized egg. § During pregnancy: § maintains placenta § stops uterus from contracting (abortion) § Prepare breasts for lactation (milk production)


Menstruation


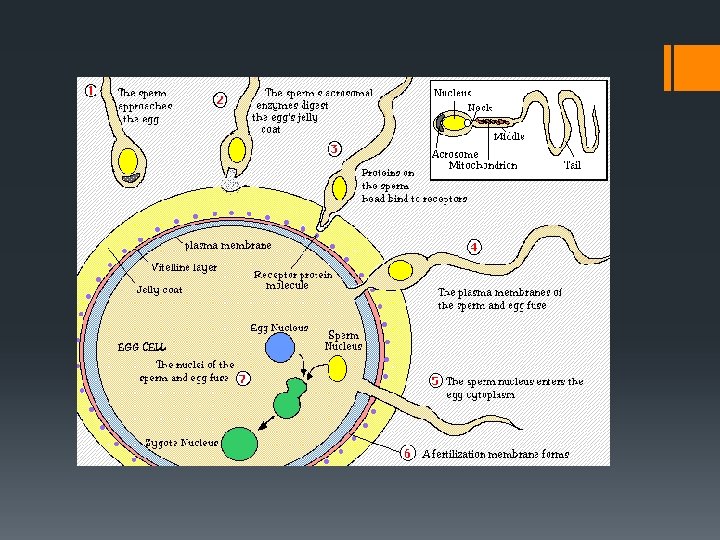
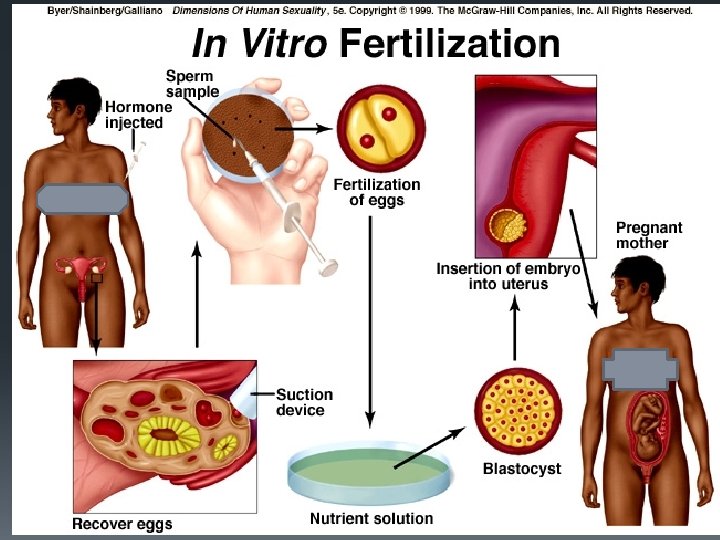
COPULATION: Union of sex organs (penis is inserted into the vagina). FERTILISATION: Fusion of the sperm and ovum nuclei to form a (diploid) Zygote (in the fallopian tube).

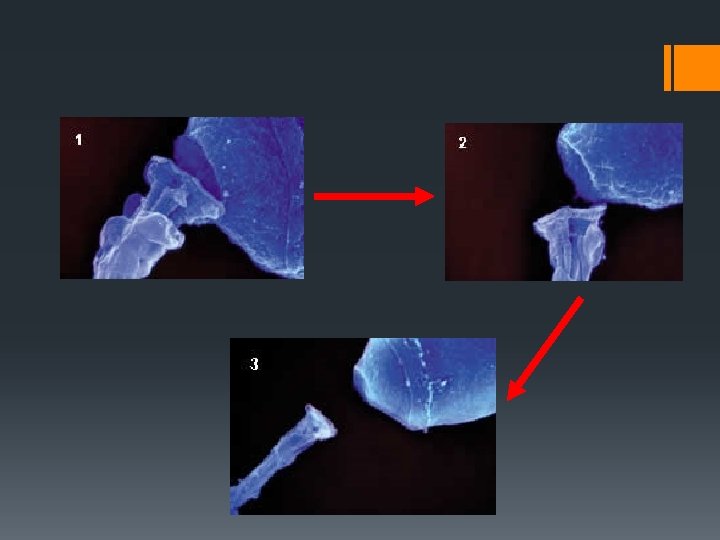
Fertilization


Ovum Sperm

He (God) has created both sexes, male and female, from a drop of semen which has been ejected. (Qur'an, 53: 45 -46 )



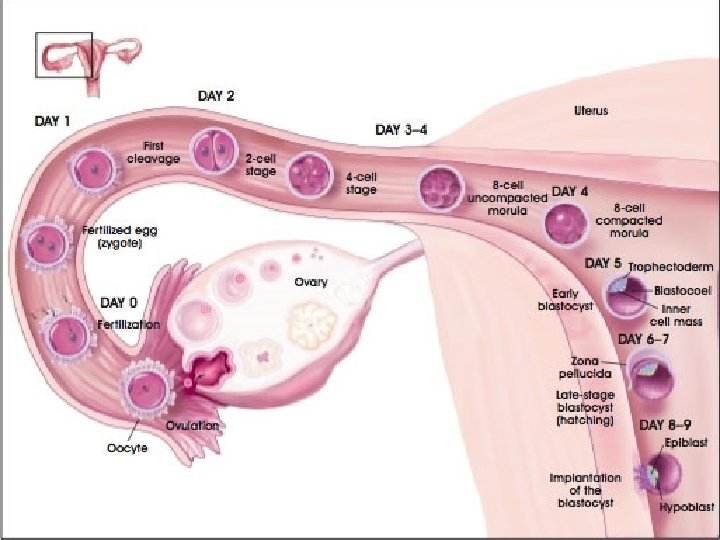
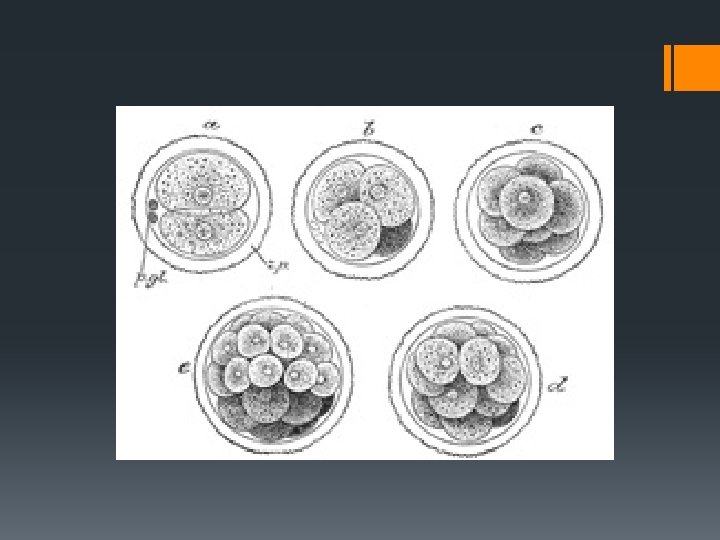
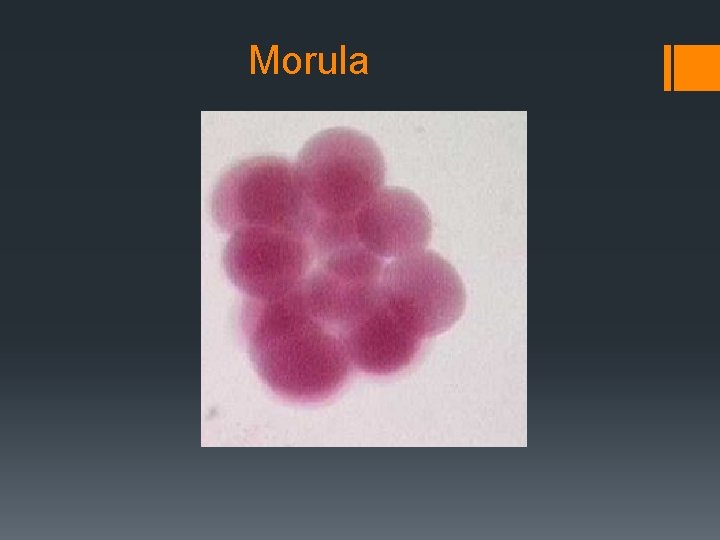
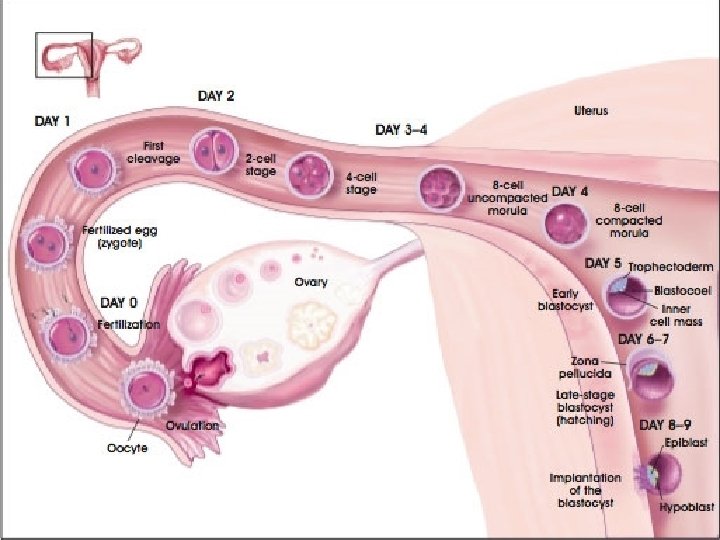
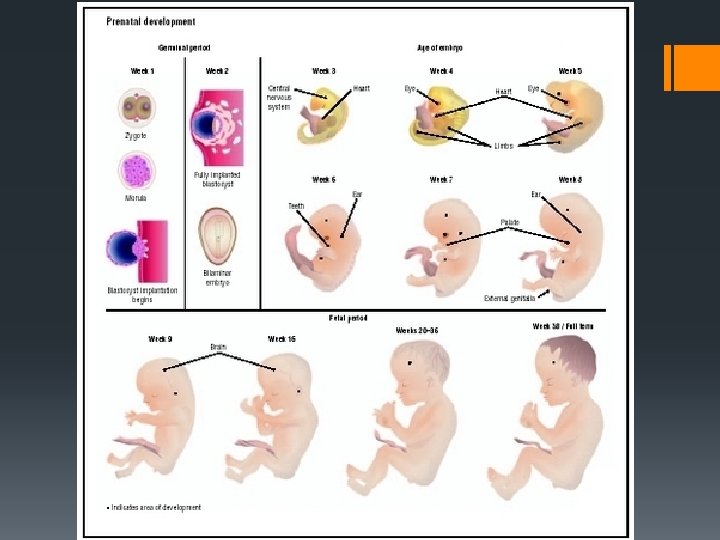
Embryonic development Diploid Zygote Morula (8/many cell stage) Blastocyst (Hollow ball of cells) Embryo Foetus (after approx 3 months)


Morula


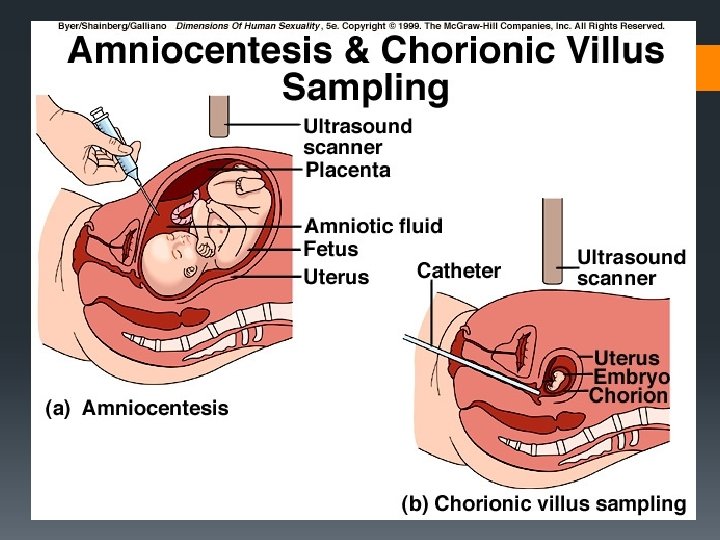
Embryonic membranes § 1. Chorion Villi of placenta § 2. Amnion Fluid-filled space § 3. Yolk sac Part of umbilical cord § 4. Allantois Umbilical blood vessels

Gestation (pregnancy) From implantation till birth.

Implantation § The blastocyst embeds itself in the endometrium

Pg 101 Ex 8 no 3, 4 and 6


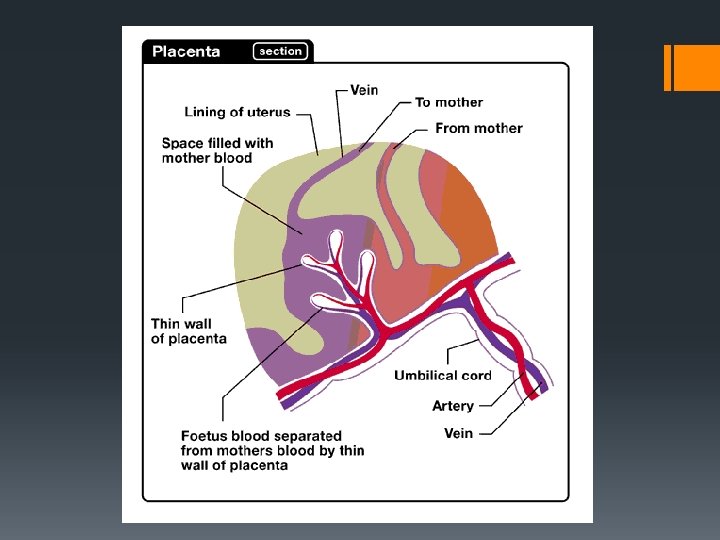
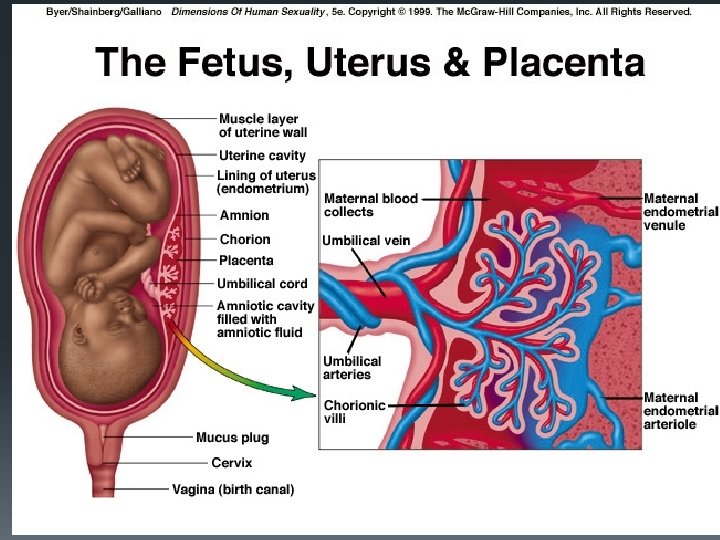
Identify and state the functions of the following parts of the developing embryo/foetus: § Chorion and chorionic villi § Amnion, amniotic cavity and amniotic fluid § Umbilical cord (including umbilical artery and umbilical vein) § Placenta


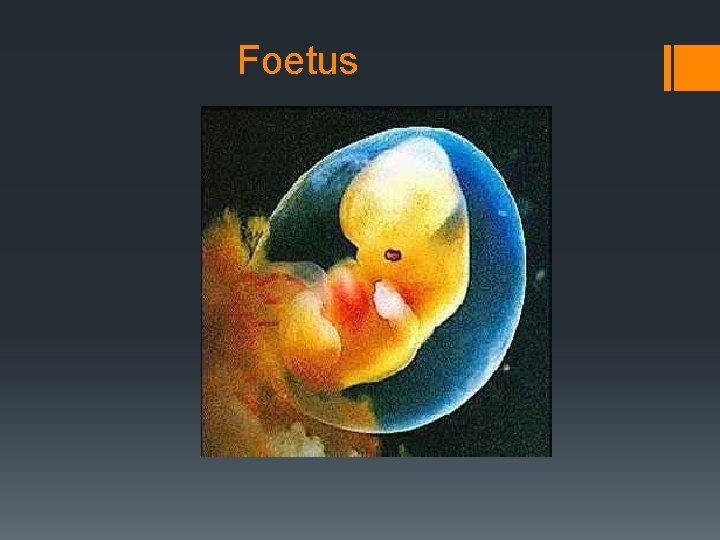
Foetus


Placental functions § 1. Gaseous exchange § 2. Nutrition § 3. Excretion

Hormones § 1. FSH – Hypophysis § 2. LH – Hypophysis d n n a i a e t n n i o a r e m y t s c n e g a g o n o r P str reg e p O § 3. Oestrogen – Graafian follicle + corpus luteum + placenta § 4. Progesterone - corpus luteum + placenta § 5. Relaxin § 6. Prolactin § § 7. HCG § 8. Oxytocin These are not prescribed

Birth process (aka parturation) Three stages of the natural birth process § Labour (contractions of uterus and dilation of cervix, breaking of the “water”) § expulsion of baby § release of the afterbirth (placenta)

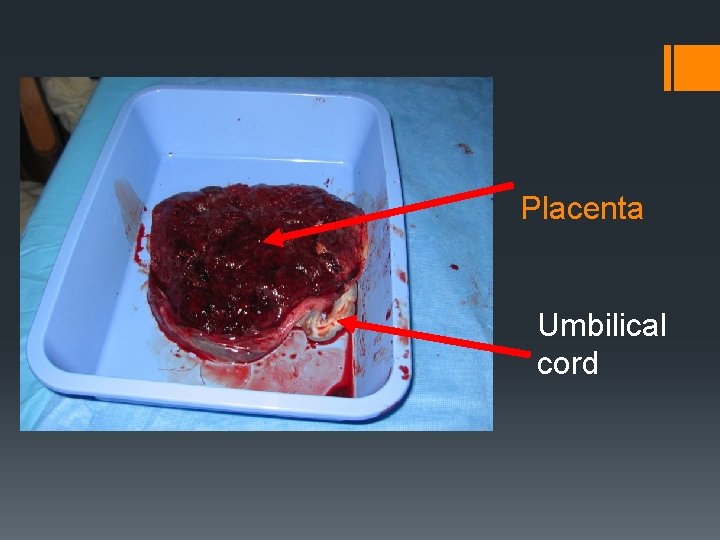
Placenta Umbilical cord

Contraception (preventing pregnancy) Not assessed


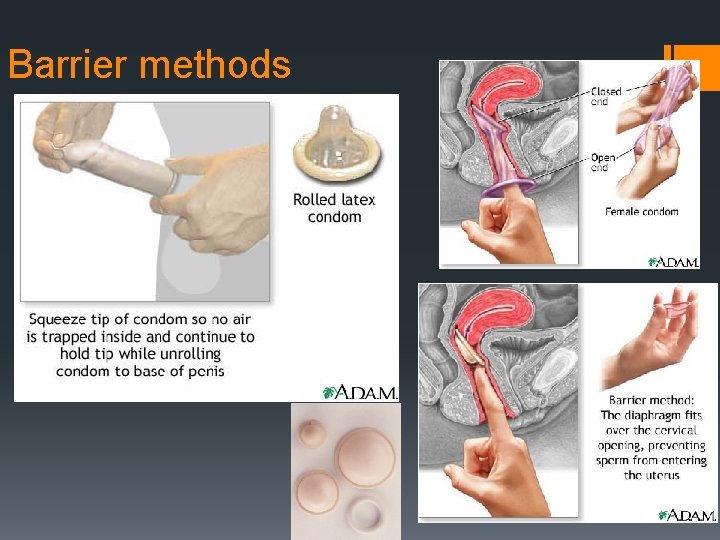
Barrier methods

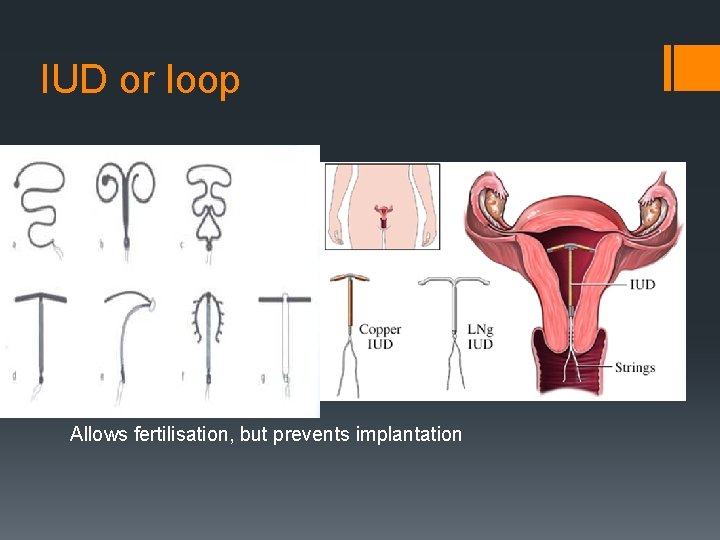
IUD or loop Allows fertilisation, but prevents implantation

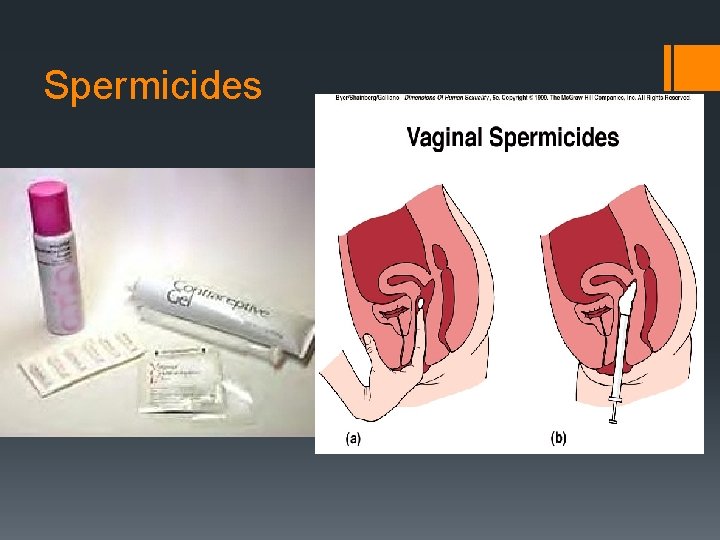
Spermicides Diaphragm

Other chemical methods § “The pill” (daily) § Injections (2 -3 months) § Implants (3 -5 years)




Ultra-sound scans




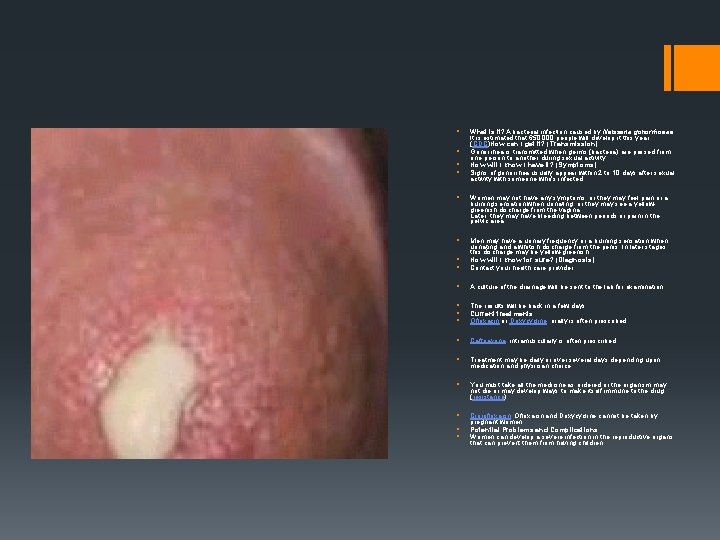
§ § Gonorrrhoea § § What is it? A bacterial infection caused by Neisseria gonorrhoeae. It is estimated that 650, 000 people will develop it this year. (CDC)How can I get it? (Transmission) Gonorrhea is transmitted when germs (bacteria) are passed from one person to another during sexual activity How will I know I have it? (Symptoms) Signs of gonorrhea usually appear within 2 to 10 days after sexual activity with someone who's infected § Women may not have any symptoms, or they may feel pain or a burning sensation when urinating, or they may see a yellowgreenish discharge from the vagina. Later, they may have bleeding between periods or pain in the pelvic area. § § § Men may have a urinary frequency or a burning sensation when urinating and a whitish discharge from the penis. In later stages, this discharge may be yellow-greenish How will I know for sure? (Diagnosis) Contact your health care provider § A culture of the drainage will be sent to the lab for examination § § § The results will be back in a few days Current treatments Ofloxacin or Doxycycline, orally is often prescribed § Ceftriaxone, intramuscularly is often prescribed § Treatment may be daily or over several days depending upon medication and physician choice § You must take all the medicine as ordered or the organism may not die or may develop ways to make itself immune to the drug (resistance) § Ciprofloxacin, Ofloxacin and Doxycycline cannot be taken by pregnant women Potential Problems and Complications Women can develop a severe infection in the reproductive organs that can prevent them from having children. § §
