Human Biology BIOL 104 Talk Nine Reproductive Systems

Human Biology (BIOL 104) Talk Nine: Reproductive Systems Animal Reproduction and Development (Chapter 34)

A step sideways – global population • Earth is currently experiencing the most population increase in Human history. • 2. 5 billion in 1955 to 7. 4 billion in 2017 • At current rate, will double within 30 years! • Fastest growing nations have growth rates at or above 4% this will double the countries population every 17 years Graph courtesy of the Bixby Center on Population, Health & Sustainability (populationgrowth. org)
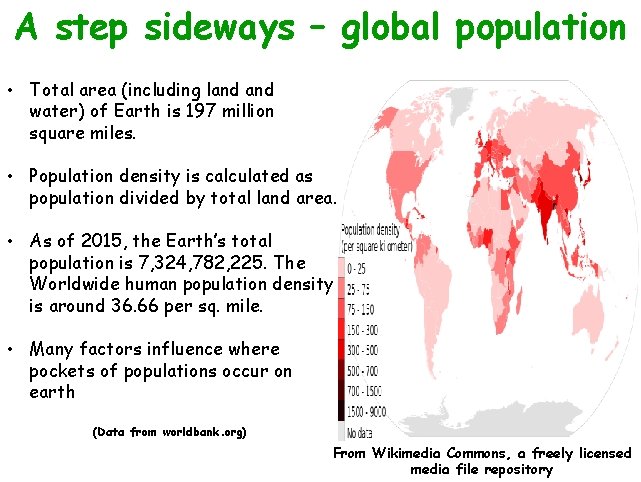
A step sideways – global population • Total area (including land water) of Earth is 197 million square miles. • Population density is calculated as population divided by total land area. • As of 2015, the Earth’s total population is 7, 324, 782, 225. The Worldwide human population density is around 36. 66 per sq. mile. • Many factors influence where pockets of populations occur on earth (Data from worldbank. org) From Wikimedia Commons, a freely licensed media file repository

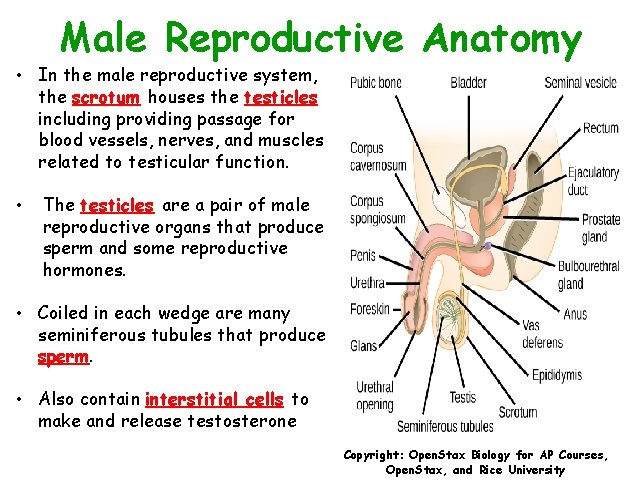
Male Reproductive Anatomy • In the male reproductive system, the scrotum houses the testicles including providing passage for blood vessels, nerves, and muscles related to testicular function. • The testicles are a pair of male reproductive organs that produce sperm and some reproductive hormones. • Coiled in each wedge are many seminiferous tubules that produce sperm. • Also contain interstitial cells to make and release testosterone Copyright: Open. Stax Biology for AP Courses, Open. Stax, and Rice University
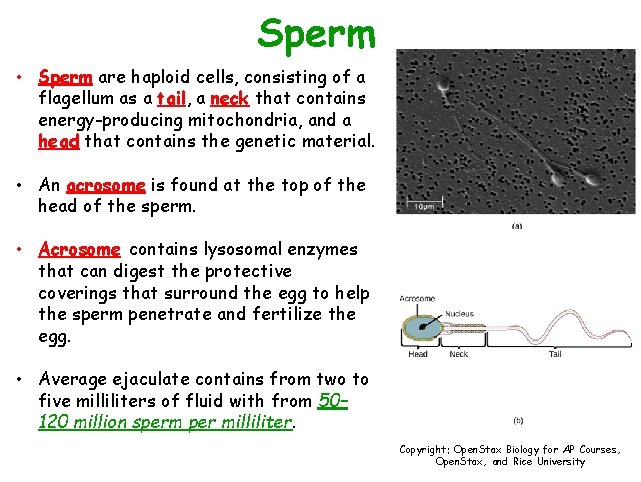
Sperm • Sperm are haploid cells, consisting of a flagellum as a tail, a neck that contains energy-producing mitochondria, and a head that contains the genetic material. • An acrosome is found at the top of the head of the sperm. • Acrosome contains lysosomal enzymes that can digest the protective coverings that surround the egg to help the sperm penetrate and fertilize the egg. • Average ejaculate contains from two to five milliliters of fluid with from 50– 120 million sperm per milliliter. Copyright: Open. Stax Biology for AP Courses, Open. Stax, and Rice University
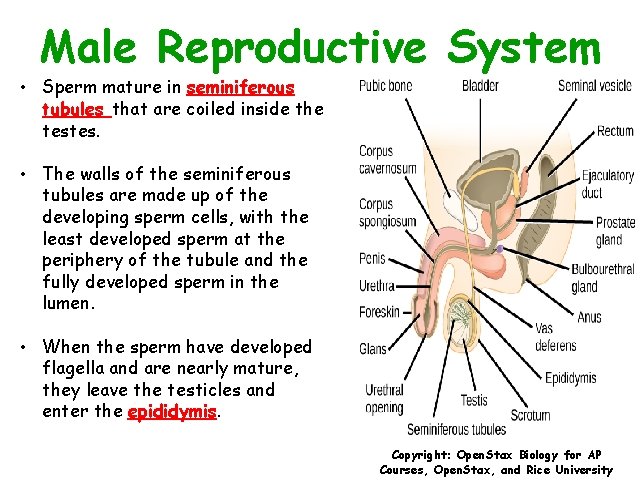
Male Reproductive System • Sperm mature in seminiferous tubules that are coiled inside the testes. • The walls of the seminiferous tubules are made up of the developing sperm cells, with the least developed sperm at the periphery of the tubule and the fully developed sperm in the lumen. • When the sperm have developed flagella and are nearly mature, they leave the testicles and enter the epididymis. Copyright: Open. Stax Biology for AP Courses, Open. Stax, and Rice University
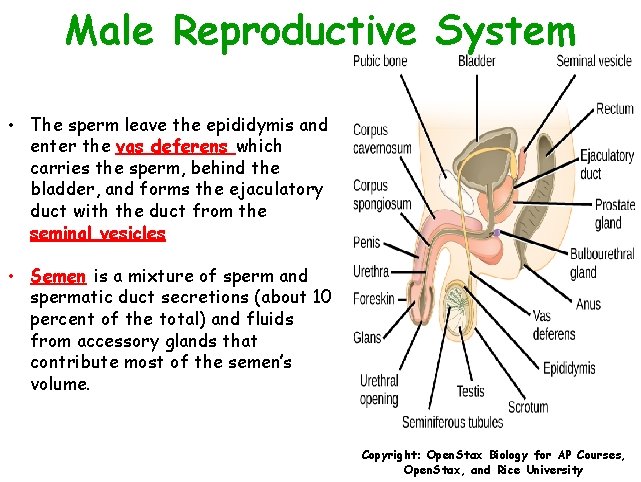
Male Reproductive System • The sperm leave the epididymis and enter the vas deferens which carries the sperm, behind the bladder, and forms the ejaculatory duct with the duct from the seminal vesicles • Semen is a mixture of sperm and spermatic duct secretions (about 10 percent of the total) and fluids from accessory glands that contribute most of the semen’s volume. Copyright: Open. Stax Biology for AP Courses, Open. Stax, and Rice University
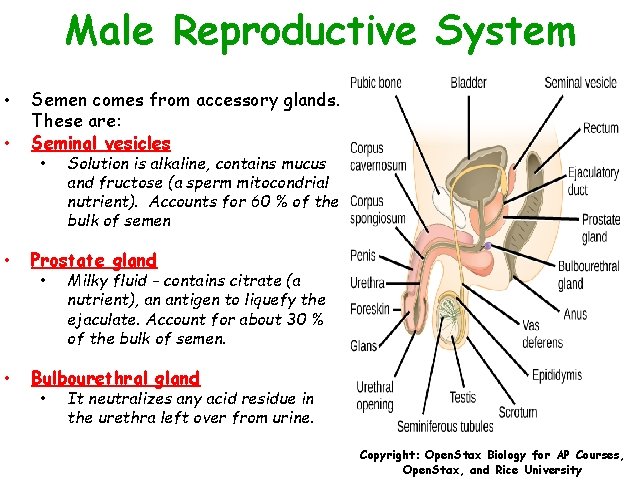
Male Reproductive System • • Semen comes from accessory glands. These are: Seminal vesicles • • Prostate gland • • Solution is alkaline, contains mucus and fructose (a sperm mitocondrial nutrient). Accounts for 60 % of the bulk of semen Milky fluid - contains citrate (a nutrient), an antigen to liquefy the ejaculate. Account for about 30 % of the bulk of semen. Bulbourethral gland • It neutralizes any acid residue in the urethra left over from urine. Copyright: Open. Stax Biology for AP Courses, Open. Stax, and Rice University
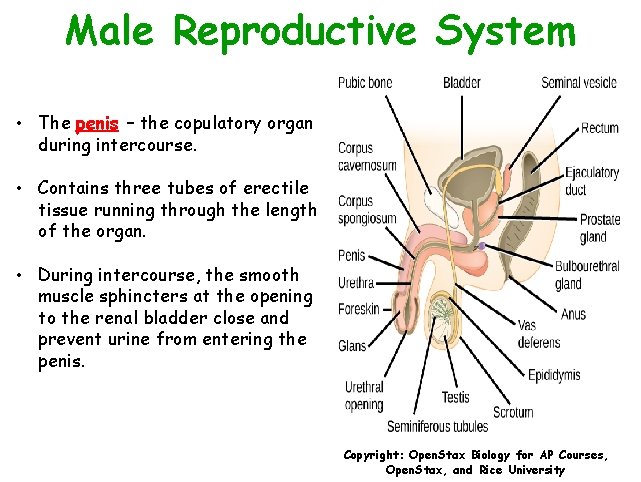
Male Reproductive System • The penis – the copulatory organ during intercourse. • Contains three tubes of erectile tissue running through the length of the organ. • During intercourse, the smooth muscle sphincters at the opening to the renal bladder close and prevent urine from entering the penis. Copyright: Open. Stax Biology for AP Courses, Open. Stax, and Rice University

Circumcision • Cuts or otherwise removes some or all of the foreskin (prepuce) from the penis. • Circumcision predates recorded human history, with depictions found in stone-age cave drawings and Ancient Egyptian tombs. The origins of the practice are lost in antiquity. • Theories include that circumcision is a form of ritual sacrifice or offering, a sign of submission to a deity, a rite of passage to adulthood, a mark of defeat or slavery, or an attempt to alter aesthetics or sexuality. • Circumcision of males is a religious requirement of the Islamic and Jewish faiths

Circumcision • The American Medical Association states that medical associations in the US, Australia, and Canada do not recommend routine “nontherapeutic” circumcision, which it defines as the non-religious, non-ritualistic, not medically necessary, elective circumcision of male newborns. • Why? • What about HIV ?

• Religion: Circumcision • Circumcision is fundamental to Judaism. It is an essential component of Jewish practice and is a commandment obligatory under Jewish law for all Jewish males on the eighth day after birth unless health reasons force a delay. • In Islam, the timing of Muslim circumcision varies. • While circumcision may be performed at all ages from newborn period to adulthood, the medical profession has encouraged medical circumcisions in the first week after birth to reduce complications.

Circumcision • Cultural: • Circumcision can be part of an initiation rite in some African, Pacific Islander, and certain isolated Australian aboriginal traditions. • Among the Urhobo people of southern Nigeria it is symbolic of a boy entering into manhood. The ritual expression, Omo te Oshare ("the boy is now man"), constitutes a rite of passage from one age set to another.

Circumcision • HIV: • The most recent data indicate that circumcision is correlated with significantly reduced risks of HIV transfer during heterosexual intercourse. • Between 48% and 53% reduction, although the topic remains the subject of ongoing research and debate in the medical community. • There also fears that some may mistakenly believe they will be protected against HIV through circumcision and see circumcision as a safe alternative to other forms of protection, such as condoms.

Circumcision • In the USA: • WHY? • WHEN? • WHAT DO YOU THINK?
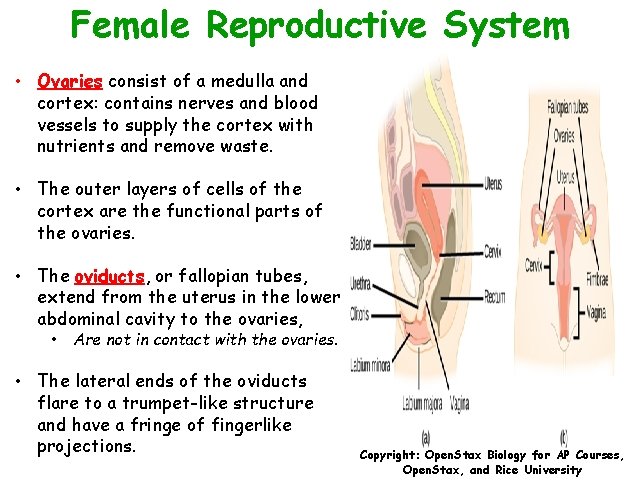
Female Reproductive System • Ovaries consist of a medulla and cortex: contains nerves and blood vessels to supply the cortex with nutrients and remove waste. • The outer layers of cells of the cortex are the functional parts of the ovaries. • The oviducts, or fallopian tubes, extend from the uterus in the lower abdominal cavity to the ovaries, • Are not in contact with the ovaries. • The lateral ends of the oviducts flare to a trumpet-like structure and have a fringe of fingerlike projections. Copyright: Open. Stax Biology for AP Courses, Open. Stax, and Rice University
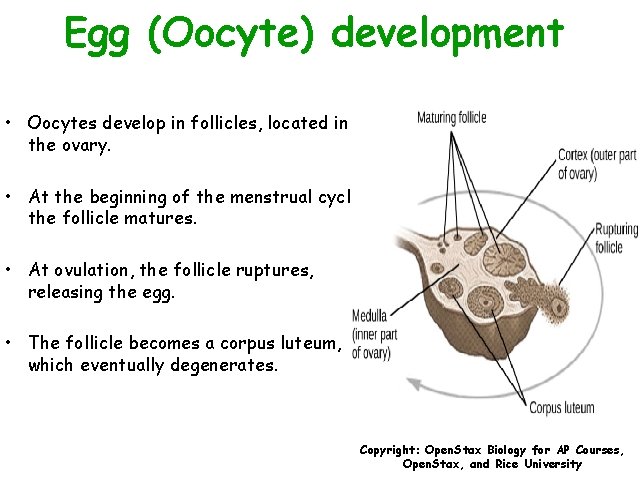
Egg (Oocyte) development • Oocytes develop in follicles, located in the ovary. • At the beginning of the menstrual cycle, the follicle matures. • At ovulation, the follicle ruptures, releasing the egg. • The follicle becomes a corpus luteum, which eventually degenerates. Copyright: Open. Stax Biology for AP Courses, Open. Stax, and Rice University
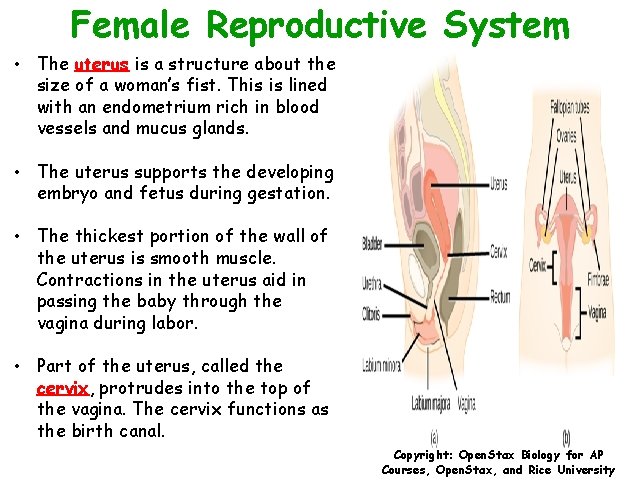
Female Reproductive System • The uterus is a structure about the size of a woman’s fist. This is lined with an endometrium rich in blood vessels and mucus glands. • The uterus supports the developing embryo and fetus during gestation. • The thickest portion of the wall of the uterus is smooth muscle. Contractions in the uterus aid in passing the baby through the vagina during labor. • Part of the uterus, called the cervix, protrudes into the top of the vagina. The cervix functions as the birth canal. Copyright: Open. Stax Biology for AP Courses, Open. Stax, and Rice University
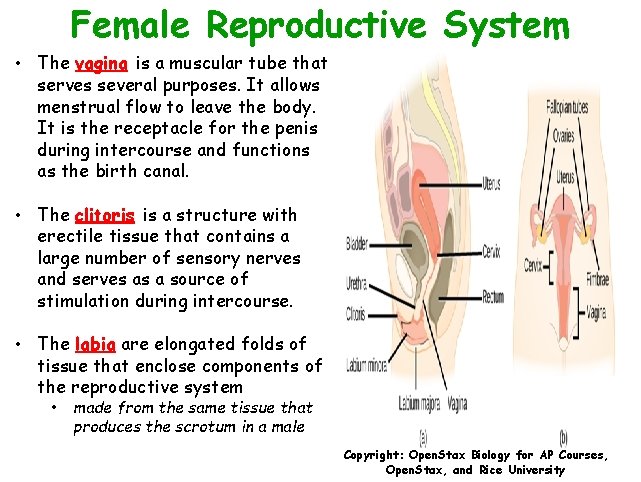
Female Reproductive System • The vagina is a muscular tube that serves several purposes. It allows menstrual flow to leave the body. It is the receptacle for the penis during intercourse and functions as the birth canal. • The clitoris is a structure with erectile tissue that contains a large number of sensory nerves and serves as a source of stimulation during intercourse. • The labia are elongated folds of tissue that enclose components of the reproductive system • made from the same tissue that produces the scrotum in a male Copyright: Open. Stax Biology for AP Courses, Open. Stax, and Rice University
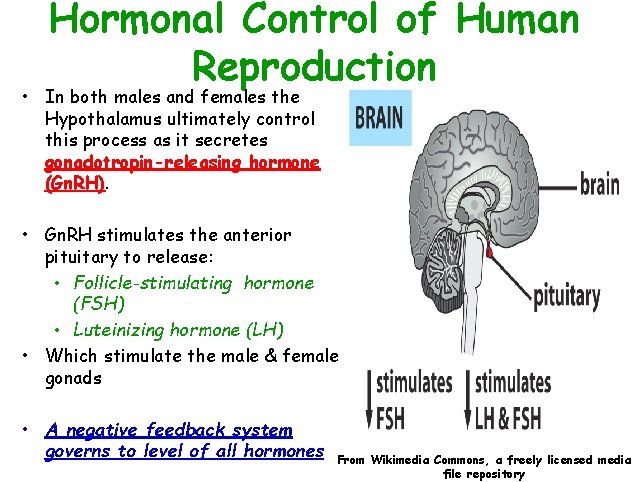
Hormonal Control of Human Reproduction • In both males and females the Hypothalamus ultimately control this process as it secretes gonadotropin-releasing hormone (Gn. RH). • Gn. RH stimulates the anterior pituitary to release: • Follicle-stimulating hormone (FSH) • Luteinizing hormone (LH) • Which stimulate the male & female gonads • A negative feedback system governs to level of all hormones From Wikimedia Commons, a freely licensed media file repository
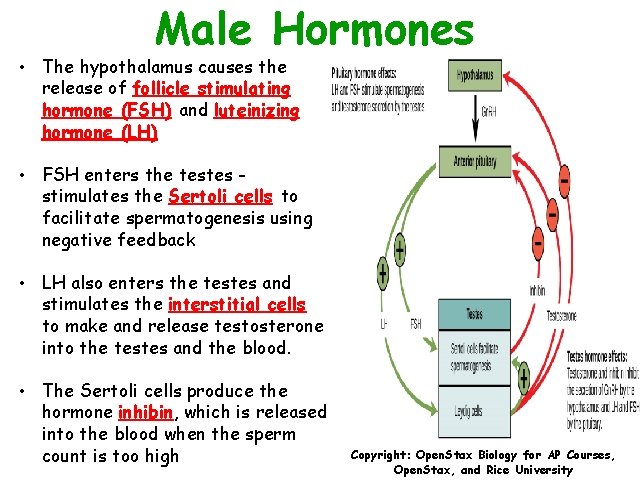
Male Hormones • The hypothalamus causes the release of follicle stimulating hormone (FSH) and luteinizing hormone (LH) • FSH enters the testes stimulates the Sertoli cells to facilitate spermatogenesis using negative feedback • LH also enters the testes and stimulates the interstitial cells to make and release testosterone into the testes and the blood. • The Sertoli cells produce the hormone inhibin, which is released into the blood when the sperm count is too high Copyright: Open. Stax Biology for AP Courses, Open. Stax, and Rice University

Female Hormones • The control of reproduction in females is more complex. • As with the male, the anterior pituitary hormones cause the release of the hormones FSH and LH. • In addition, estrogens and progesterone are released from the developing follicles. • Estrogen is the reproductive hormone in females that assists in endometrial regrowth, ovulation, and calcium absorption • Progesterone assists in endometrial re-growth and inhibition of FSH and LH release.

Female Hormones • FSH stimulates development of egg cells, called ova, which develop in structures called follicles. • Follicle cells produce the hormone inhibin, which inhibits FSH production. • LH also plays a role in the development of ova, induction of ovulation, and stimulation of estradiol and progesterone production by the ovaries. • Estradiol and progesterone are steroid hormones that prepare the body for pregnancy. • Estradiol produces secondary sex characteristics in females, while both estradiol and progesterone regulate the menstrual cycle.
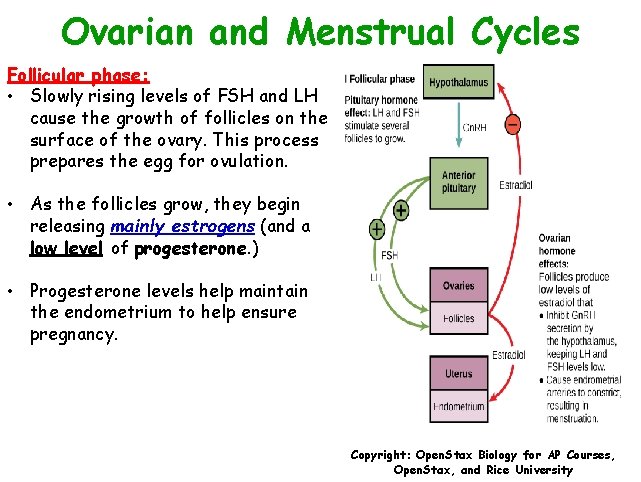
Ovarian and Menstrual Cycles Follicular phase: • Slowly rising levels of FSH and LH cause the growth of follicles on the surface of the ovary. This process prepares the egg for ovulation. • As the follicles grow, they begin releasing mainly estrogens (and a low level of progesterone. ) • Progesterone levels help maintain the endometrium to help ensure pregnancy. Copyright: Open. Stax Biology for AP Courses, Open. Stax, and Rice University
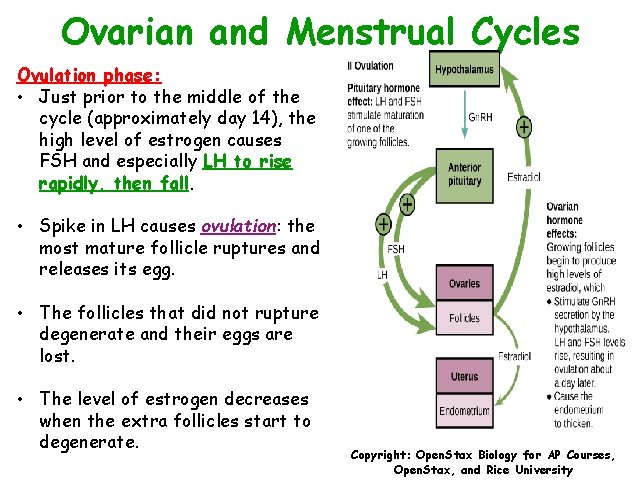
Ovarian and Menstrual Cycles Ovulation phase: • Just prior to the middle of the cycle (approximately day 14), the high level of estrogen causes FSH and especially LH to rise rapidly, then fall. • Spike in LH causes ovulation: the most mature follicle ruptures and releases its egg. • The follicles that did not rupture degenerate and their eggs are lost. • The level of estrogen decreases when the extra follicles start to degenerate. Copyright: Open. Stax Biology for AP Courses, Open. Stax, and Rice University
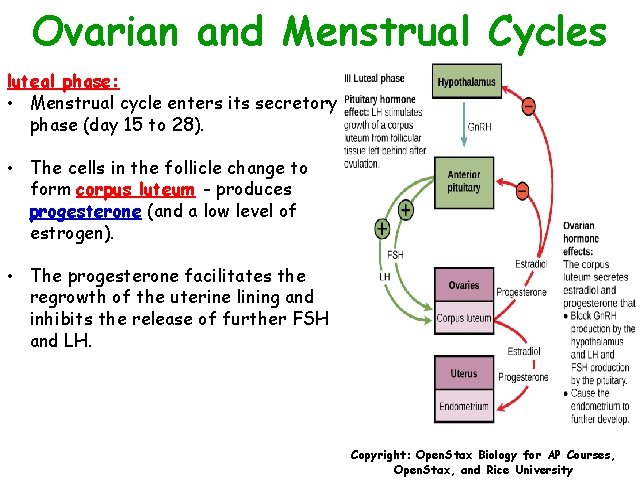
Ovarian and Menstrual Cycles luteal phase: • Menstrual cycle enters its secretory phase (day 15 to 28). • The cells in the follicle change to form corpus luteum - produces progesterone (and a low level of estrogen). • The progesterone facilitates the regrowth of the uterine lining and inhibits the release of further FSH and LH. Copyright: Open. Stax Biology for AP Courses, Open. Stax, and Rice University
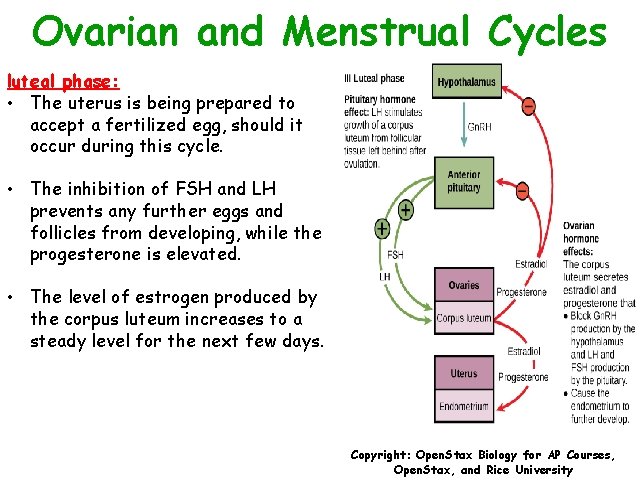
Ovarian and Menstrual Cycles luteal phase: • The uterus is being prepared to accept a fertilized egg, should it occur during this cycle. • The inhibition of FSH and LH prevents any further eggs and follicles from developing, while the progesterone is elevated. • The level of estrogen produced by the corpus luteum increases to a steady level for the next few days. Copyright: Open. Stax Biology for AP Courses, Open. Stax, and Rice University
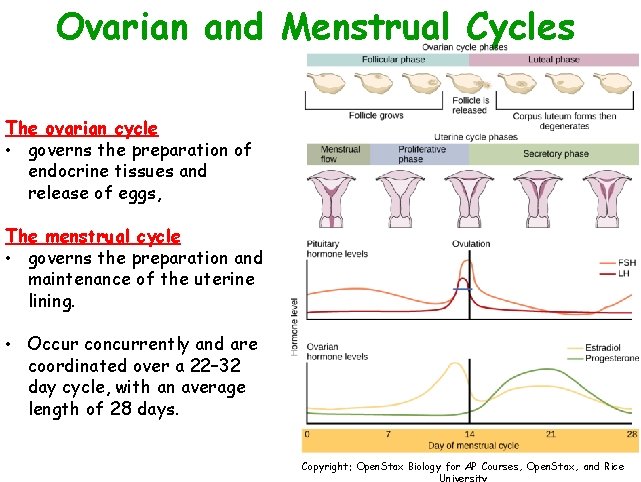
Ovarian and Menstrual Cycles The ovarian cycle • governs the preparation of endocrine tissues and release of eggs, The menstrual cycle • governs the preparation and maintenance of the uterine lining. • Occur concurrently and are coordinated over a 22– 32 day cycle, with an average length of 28 days. Copyright: Open. Stax Biology for AP Courses, Open. Stax, and Rice University

Ovarian and Menstrual Cycles • If pregnancy does not occur: • The corpus luteum degenerates and the levels of estrogen and progesterone decrease. • The endometrium begins to degenerate as the progesterone levels drop, initiating the next menstrual cycle. • The decrease in progesterone also allows the hypothalamus to send Gn. RH to the anterior pituitary, releasing FSH and LH and starting the cycles again. • The endometrium begins to regrow, replacing the blood vessels and glands that deteriorated during the end of the last cycle.

Menopause • As women approach their mid-40 s to mid-50 s, their ovaries begin to lose their sensitivity to FSH and LH. Menstrual periods become less frequent and finally cease. • There are still eggs and potential follicles on the ovaries, but without the stimulation of FSH and LH, they will not produce a viable egg to be released. • The side effects of menopause include: • • • hot flashes and heavy sweating (especially at night) headaches, some hair loss muscle pain vaginal dryness Insomnia Depression weight gain mood swings.

Menopause • Estrogen is involved in calcium metabolism, without it, blood levels of calcium decrease. To replenish the blood, calcium is lost from bone which may decrease the bone density and lead to osteoporosis. • Hormone replacement therapy (HRT) can prevent bone loss, but therapy can have negative side effects -increased risk of: • stroke or heart attack • blood clots • breast cancer • ovarian cancer • endometrial cancer • gall bladder disease • dementia

The end! Any Questions?
- Slides: 33