Human Anatomy and Physiology Unit V GasExchange Absorption

Human Anatomy and Physiology Unit V Gas-Exchange, Absorption, and Excretion Part 1 The Respiratory System

Unit Topics Part 1 Respiratory System Part 2 Urinary System Part 3 Fluid, Electrolyte, and p. H Balance Part 4 Digestive System Part 5 Immunity Resources Your textbook – Chapter 23 Your lab manual – Exercise 32 and 33

Respiratory System Topics 1. 2. 3. 4. 5. 6. Anatomy of the Respiratory System Pulmonary Ventilation Lung Volumes and Capacities Oxygen and Carbon Dioxide Exchange Oxygen and Carbon Dioxide Transport Control of Respiration

Introduction 1. The respiratory system consists of the nose, pharynx, larynx, trachea, bronchi, and lungs • Otorhinolaryngology • (ENT) • Pulmonologist 2. The respiratory system has three main functions: • Gas exchange, p. H regulation, and Sound production

Introduction 3. The cardiovascular and respiratory systems cooperate to supply O 2 to and eliminate CO 2 from body tissues. 4. Respiration, the process of gas exchange in the body, has three basic steps: ventilation, external respiration, and internal respiration 5. The medulla oblongata and pons regulate ventilation

Respiratory System Topics 1. 2. 3. 4. 5. 6. Anatomy of the Respiratory System Pulmonary Ventilation Lung Volumes and Capacities Oxygen and Carbon Dioxide Exchange Oxygen and Carbon Dioxide Transport Control of Respiration
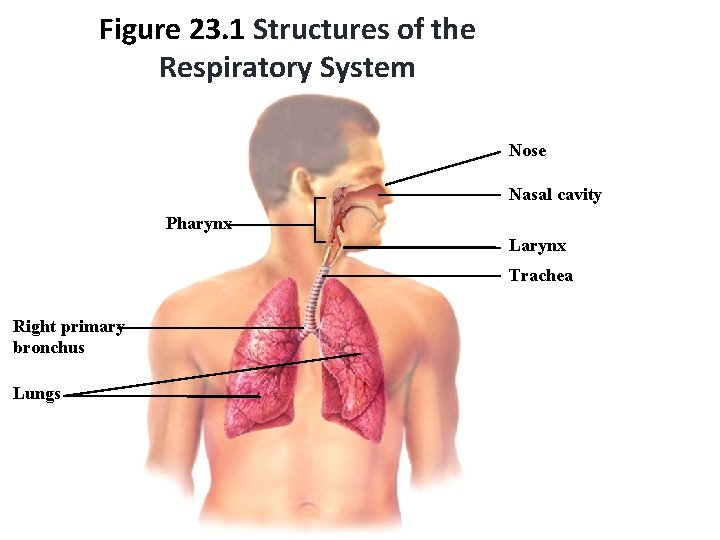
Figure 23. 1 Structures of the Respiratory System Nose Nasal cavity Pharynx Larynx Trachea Right primary bronchus Lungs
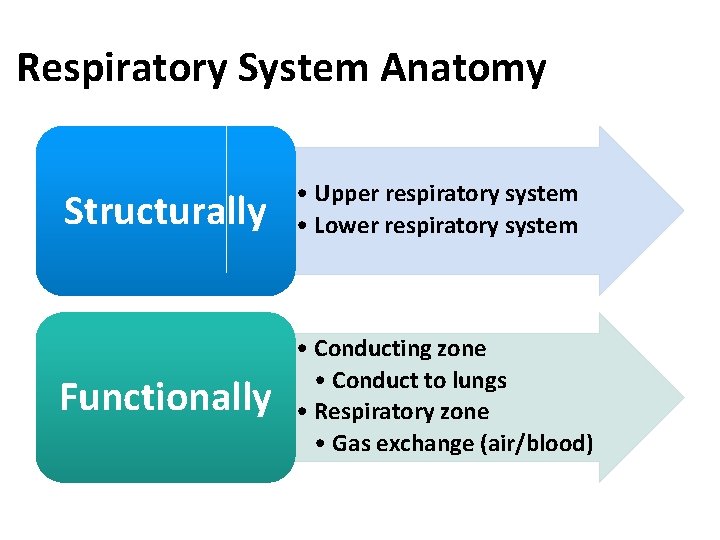
Respiratory System Anatomy Structurally • Upper respiratory system • Lower respiratory system Functionally • Conducting zone • Conduct to lungs • Respiratory zone • Gas exchange (air/blood)
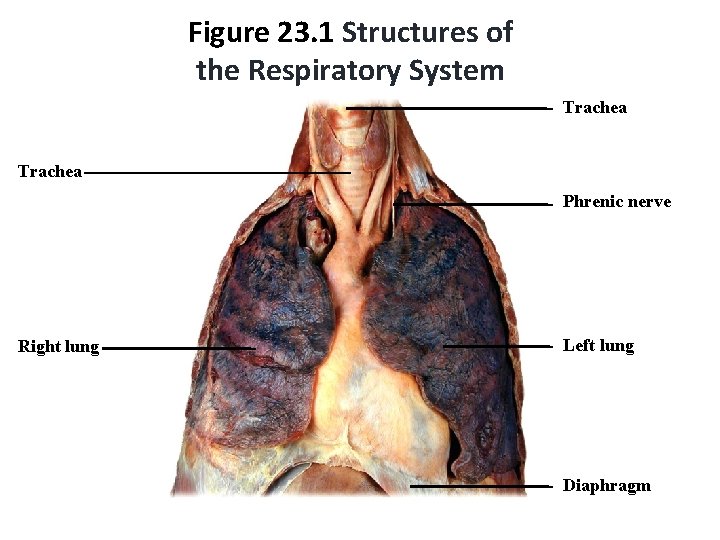
Figure 23. 1 Structures of the Respiratory System Trachea Phrenic nerve Right lung Left lung Diaphragm
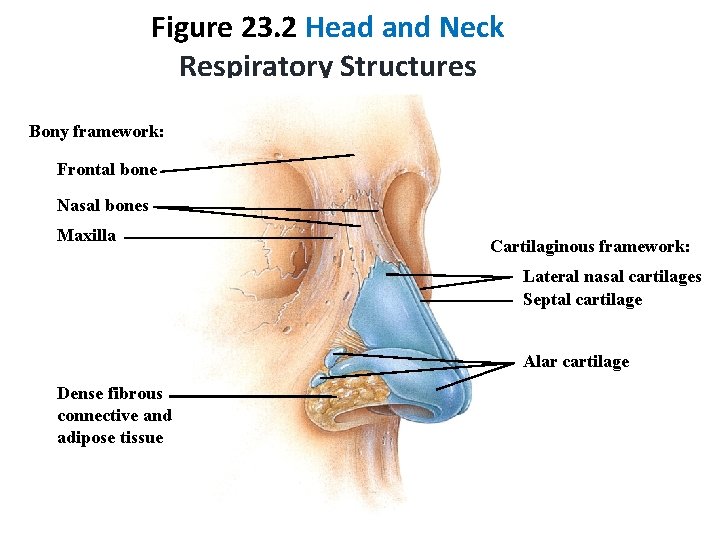
Figure 23. 2 Head and Neck Respiratory Structures Bony framework: Frontal bone Nasal bones Maxilla Cartilaginous framework: Lateral nasal cartilages Septal cartilage Alar cartilage Dense fibrous connective and adipose tissue
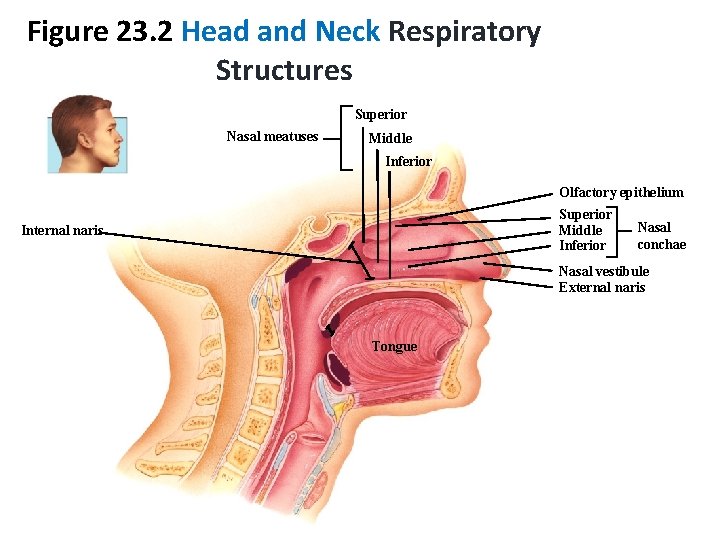
Figure 23. 2 Head and Neck Respiratory Structures Superior Nasal meatuses Middle Inferior Olfactory epithelium Superior Middle Inferior Internal naris Nasal conchae Nasal vestibule External naris Tongue
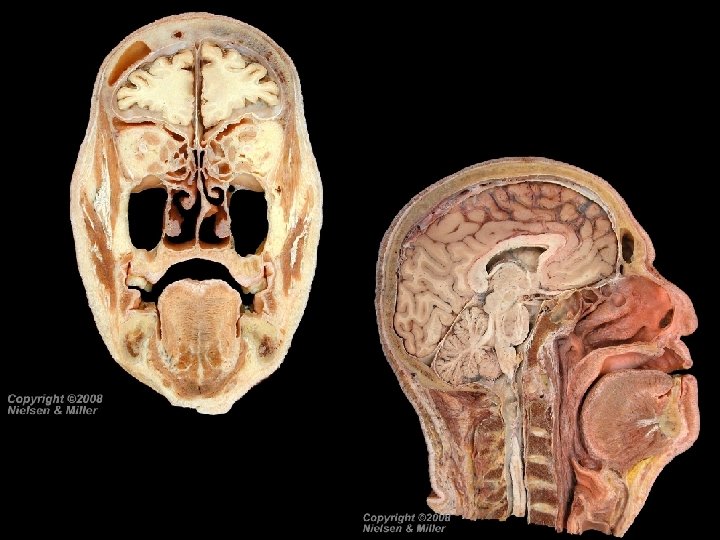

Nasal Cavity Function Warms, moistens, and filters air Receives olfactory stimuli Serves as a resonating chamber

Pharynx • Funnel-shaped tube • Connects nose and mouth with esophagus and trachea • Composed of skeletal muscle lined with mucous membrane

Pharynx Nasopharynx • Posterior to nasal cavity; auditory tubes open into it • Contains pharyngeal tonsil • Lined with pseudostratified ciliated columnar epithelium (mucus memb. ) Oropharynx • Posterior to fauces; extends from soft palate to hyoid bone • Contains palatine and lingual tonsils • Lined by nonkeratinized stratified squamous epithelium (mucus memb. ) Laryngopharynx • Extends from hyoid bone to esophagus and larynx • Lined by nonkeratinized stratified squamous epithelium (mucus memb. )
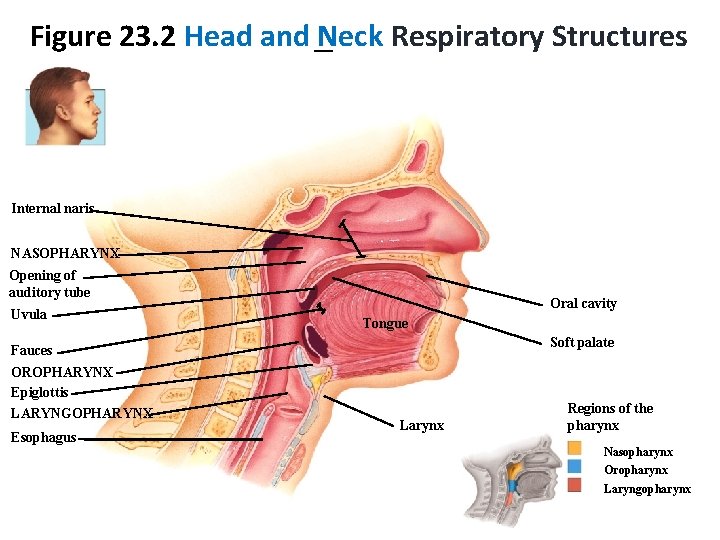
Figure 23. 2 Head and Neck Respiratory Structures Internal naris NASOPHARYNX Opening of auditory tube Uvula Oral cavity Tongue Soft palate Fauces OROPHARYNX Epiglottis LARYNGOPHARYNX Esophagus Larynx Regions of the pharynx Nasopharynx Oropharynx Laryngopharynx
Pharynx Functions Assists in deglutition Passageway for air and food Resonating chamber for speech sounds Houses tonsils
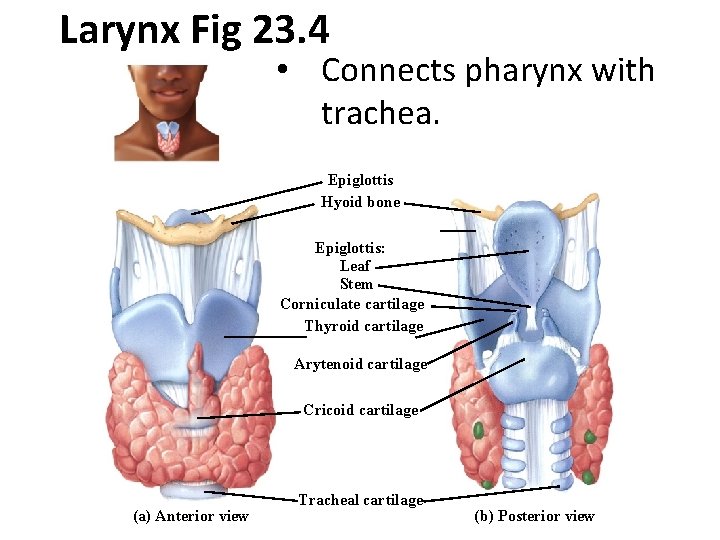
Larynx Fig 23. 4 • Connects pharynx with trachea. Epiglottis Hyoid bone Epiglottis: Leaf Stem Corniculate cartilage Thyroid cartilage Arytenoid cartilage Cricoid cartilage (a) Anterior view Tracheal cartilage (b) Posterior view

Larynx Cartilaginous Framework • Thyroid cartilage - forms anterior wall of larynx • Epiglottis - attached to anterior rim of thyroid cartilage • Cricoid cartilage - inferior to thyroid cartilage • Arytenoid cartilages - located behind above cricoid cartilage • Corniculate cartilages - located on top of arytenoid cartilages • Cuneiform cartilages - located above corniculate cartilages

Larynx Laryngeal Ligaments • Thyrohyoid membrane - connects thyroid cartilage to hyoid bone • Cricothyroid ligament - connects cricoid cartilage to thyroid cartilage • Cricotracheal ligament - connects cricoid cartilage to trachea

Larynx Glottis • The vocal cords + rima glottidis (space between them) • Affects voice modulation through expansion or contraction.
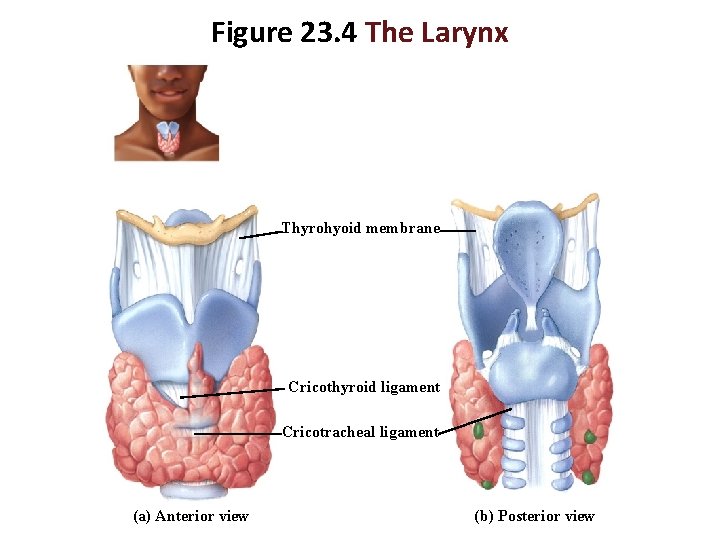
Figure 23. 4 The Larynx Thyrohyoid membrane Cricothyroid ligament Cricotracheal ligament (a) Anterior view (b) Posterior view
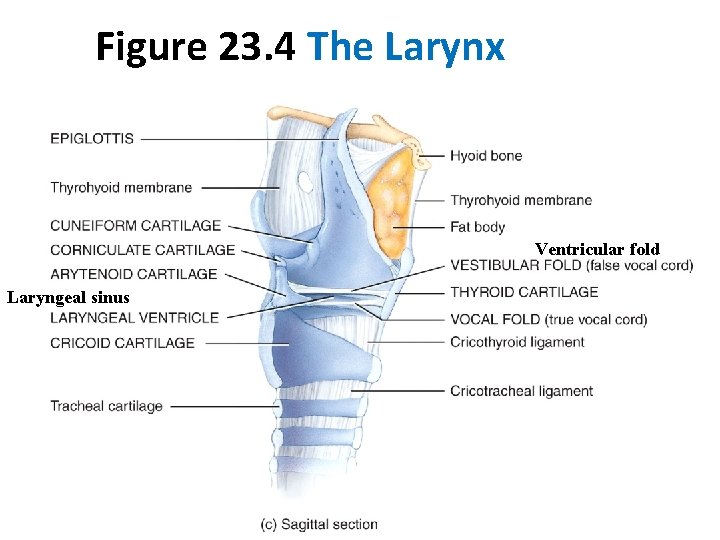
Figure 23. 4 The Larynx Ventricular fold Laryngeal sinus
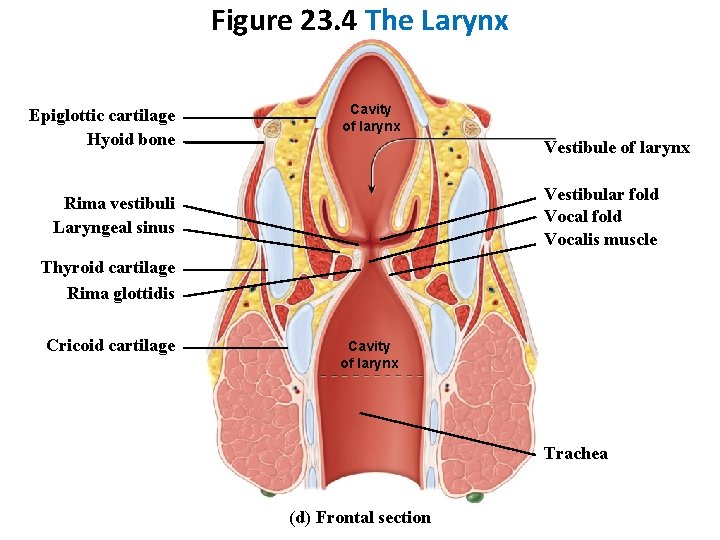
Figure 23. 4 The Larynx Epiglottic cartilage Hyoid bone Cavity of larynx Vestibule of larynx Vestibular fold Vocalis muscle Rima vestibuli Laryngeal sinus Thyroid cartilage Rima glottidis Cricoid cartilage Cavity of larynx Trachea (d) Frontal section
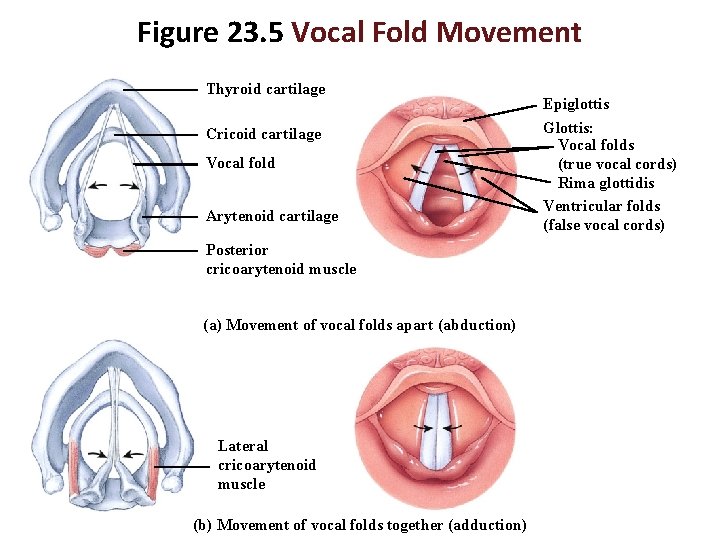
Figure 23. 5 Vocal Fold Movement Thyroid cartilage Cricoid cartilage Vocal fold Arytenoid cartilage Posterior cricoarytenoid muscle (a) Movement of vocal folds apart (abduction) Lateral cricoarytenoid muscle (b) Movement of vocal folds together (adduction) Epiglottis Glottis: Vocal folds (true vocal cords) Rima glottidis Ventricular folds (false vocal cords)
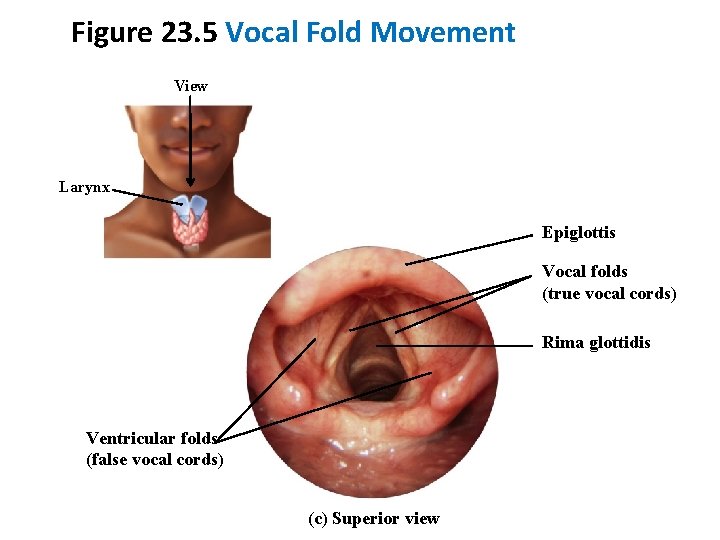
Figure 23. 5 Vocal Fold Movement View Larynx Epiglottis Vocal folds (true vocal cords) Rima glottidis Ventricular folds (false vocal cords) (c) Superior view

Next slides are learned in lab
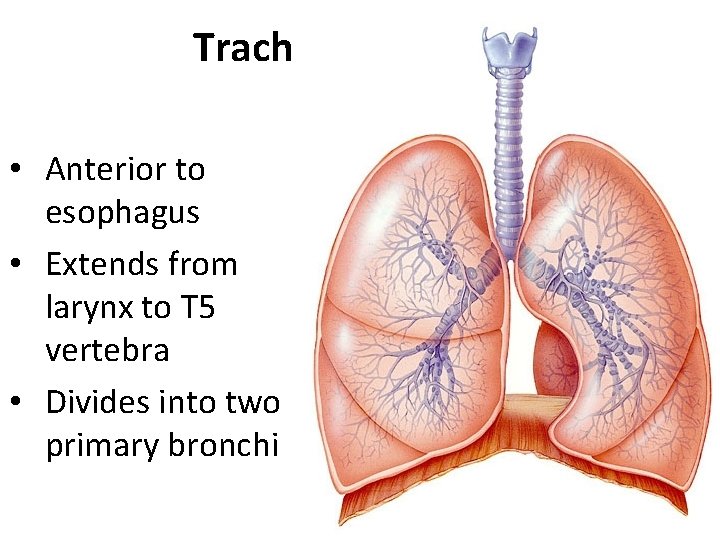
Trachea • Anterior to esophagus • Extends from larynx to T 5 vertebra • Divides into two primary bronchi
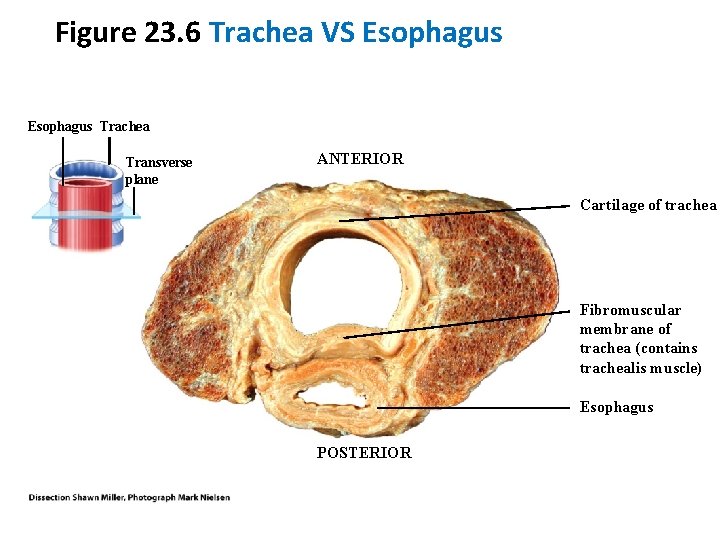
Figure 23. 6 Trachea VS Esophagus Trachea Transverse plane ANTERIOR Cartilage of trachea Fibromuscular membrane of trachea (contains trachealis muscle) Esophagus POSTERIOR
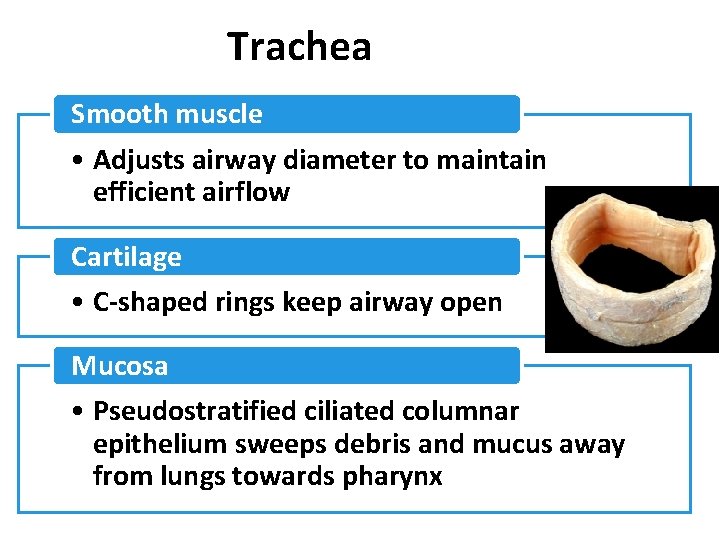
Trachea Smooth muscle • Adjusts airway diameter to maintain efficient airflow Cartilage • C-shaped rings keep airway open Mucosa • Pseudostratified ciliated columnar epithelium sweeps debris and mucus away from lungs towards pharynx

Bronchi • Bronchial tree begins at trachea and ends at terminal bronchioles • Carina divides into right and left primary bronchi • Right primary bronchus is more vertical and wider than the left primary bronchus
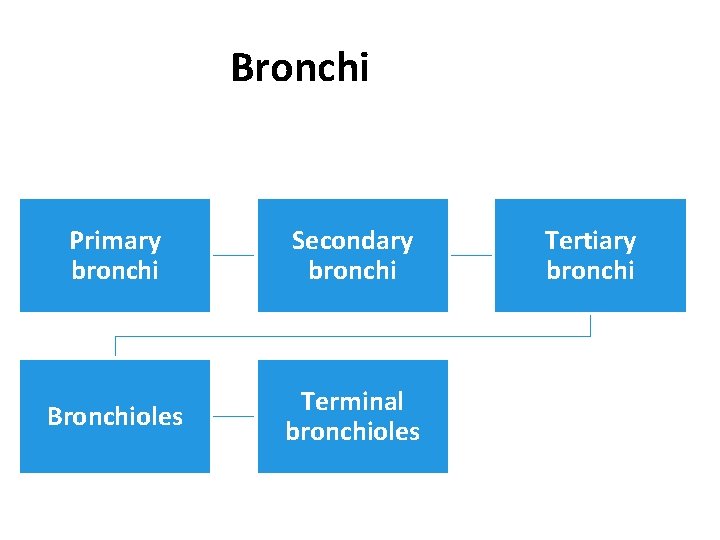
Bronchi Primary bronchi Secondary bronchi Bronchioles Terminal bronchioles Tertiary bronchi
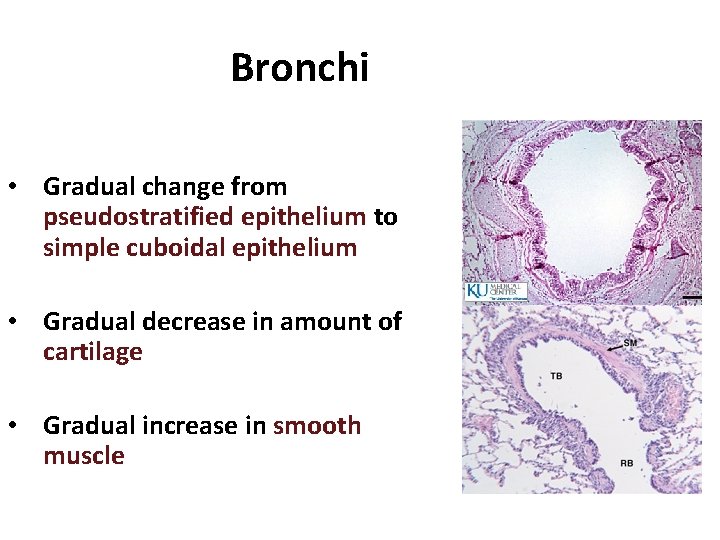
Bronchi • Gradual change from pseudostratified epithelium to simple cuboidal epithelium • Gradual decrease in amount of cartilage • Gradual increase in smooth muscle
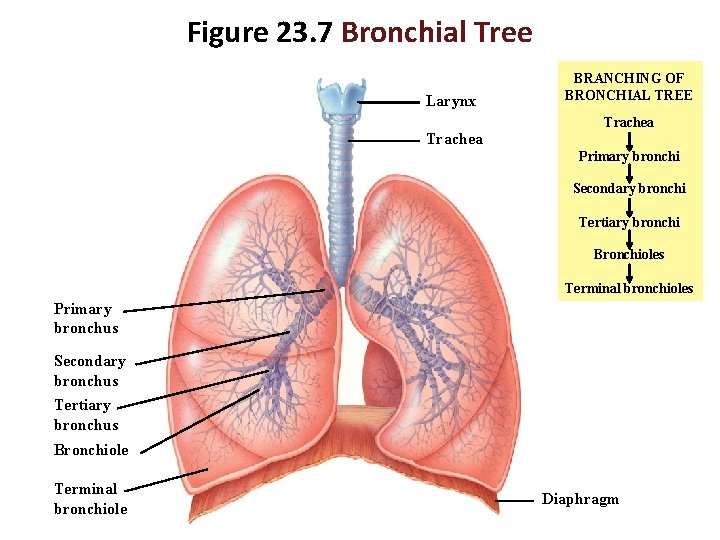
Figure 23. 7 Bronchial Tree Larynx BRANCHING OF BRONCHIAL TREE Trachea Primary bronchi Secondary bronchi Tertiary bronchi Bronchioles Terminal bronchioles Primary bronchus Secondary bronchus Tertiary bronchus Bronchiole Terminal bronchiole Diaphragm
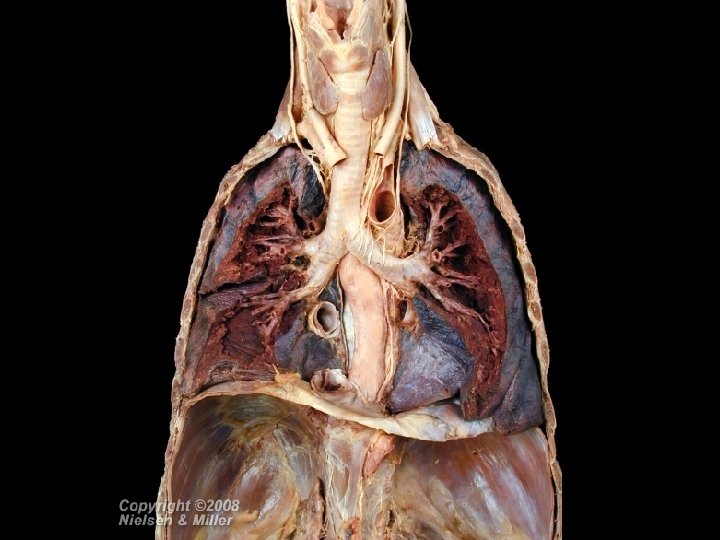
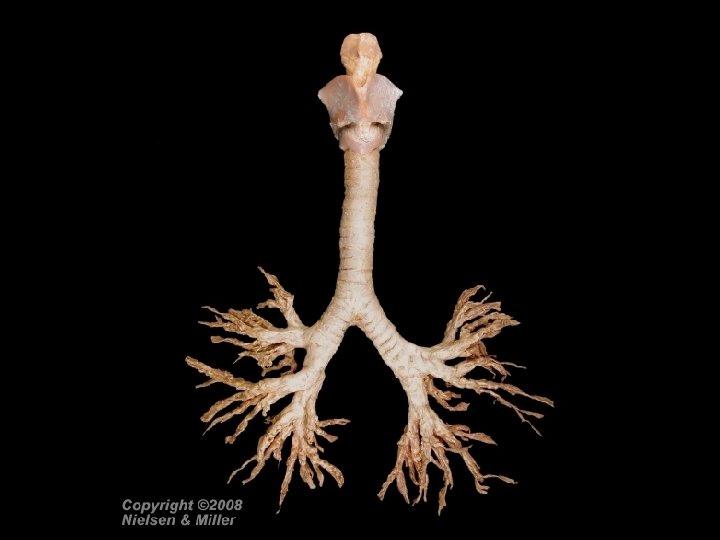

Lungs • Paired organs in thoracic cavity • Extend from diaphragm to just slightly superior to the clavicles • Lie against ribs anteriorly and posteriorly • Enclosed and protected by double-layered pleural membrane • Parietal pleura - outer layer attached to thoracic wall • Visceral pleura - inner layer covering lungs • Pleural cavity between pleurae; contains serous lubricating fluid
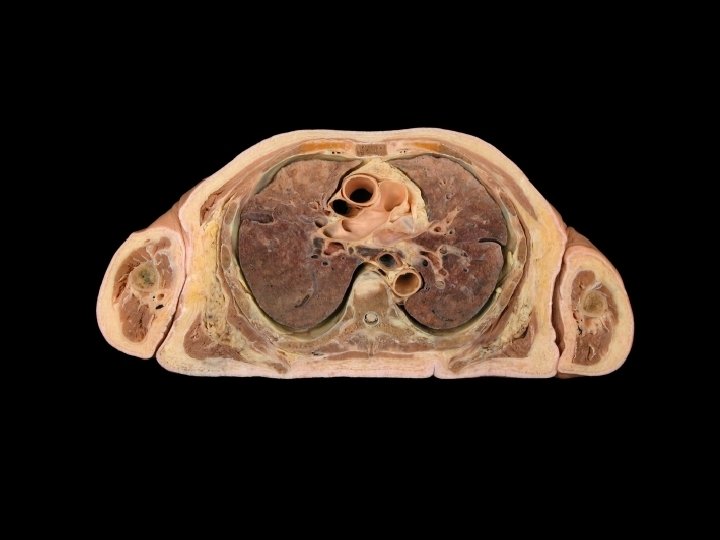
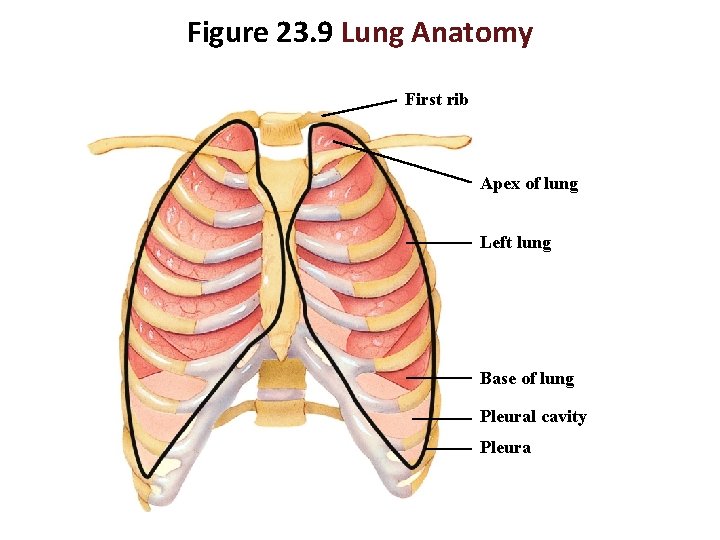
Figure 23. 9 Lung Anatomy First rib Apex of lung Left lung Base of lung Pleural cavity Pleura

Lobes, Fissures, and Lobules Left lung Right lung Superior and inferior lobes separated by oblique fissure. 8 bronchopulmonary segments Superior, middle and inferior lobes, separated by oblique and horizontal fissure 10 bronchopulmonary segments
Lobes, Fissures, and Lobules Left Lung Superior and inferior lobes separated by oblique fissure. 8 bronchopulmonary segments Right Lung Superior, middle and inferior lobes, separated by oblique and horizontal fissure 10 bronchopulmonary segments
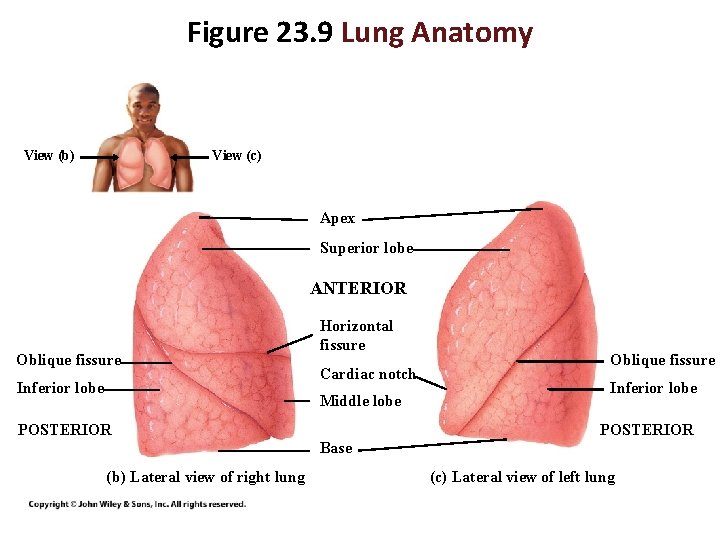
Figure 23. 9 Lung Anatomy View (b) View (c) Apex Superior lobe ANTERIOR Oblique fissure Inferior lobe Horizontal fissure Cardiac notch Middle lobe POSTERIOR Oblique fissure Inferior lobe POSTERIOR Base (b) Lateral view of right lung (c) Lateral view of left lung
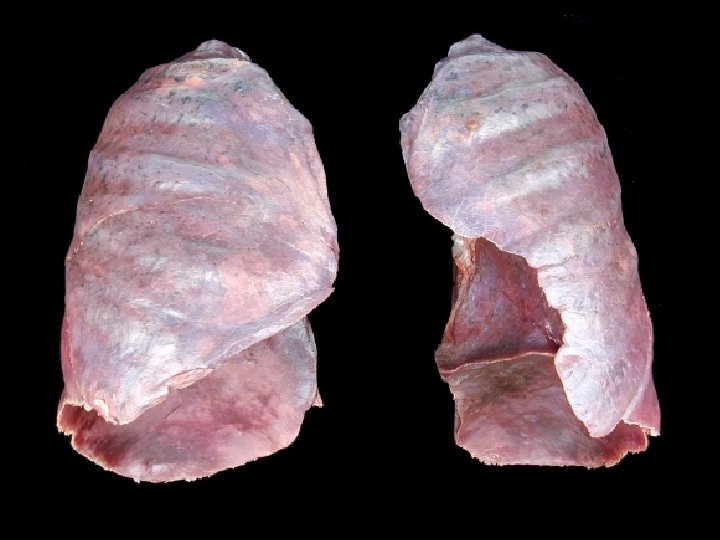
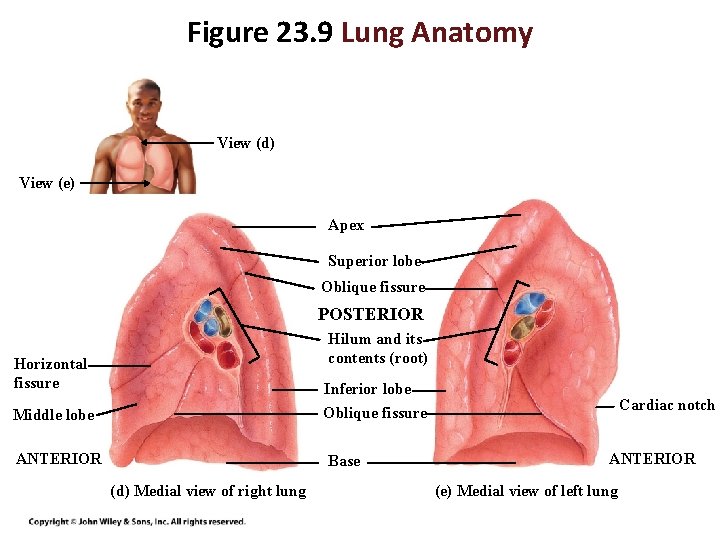
Figure 23. 9 Lung Anatomy View (d) View (e) Apex Superior lobe Oblique fissure POSTERIOR Hilum and its contents (root) Horizontal fissure Inferior lobe Oblique fissure Middle lobe ANTERIOR Base (d) Medial view of right lung Cardiac notch ANTERIOR (e) Medial view of left lung

Lobes, Fissures, and Lobules • Each bronchopulmonary segment is divided into many lobules • Each lobule is wrapped in elastic connective tissue and contains a lymphatic vessel, an arteriole, a venule, and a branch from a terminal bronchiole called a respiratory bronchiole. • Respiratory bronchioles open into alveolar ducts, each of which lead into 2 or more alveolar sacs.
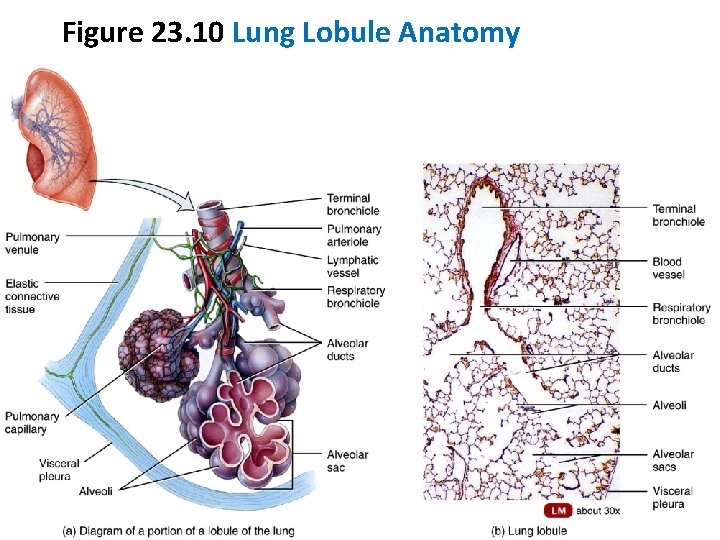
Figure 23. 10 Lung Lobule Anatomy

Alveoli • About 300 million alveolar sacs in a normal lung • Gas exchange occurs across alveolar-capillary respiratory membrane • Type I alveolar cells - squamous epithelial cells; tight junctions prevent fluid leakage into alveolar air spaces • Type II alveolar cells - secrete alveolar fluid; keeps alveolar cells moist and contains surfactant; Surfactant lowers alveolar fluid surface tension • Alveolar macrophages - remove fine dust particles and debris from alveolus
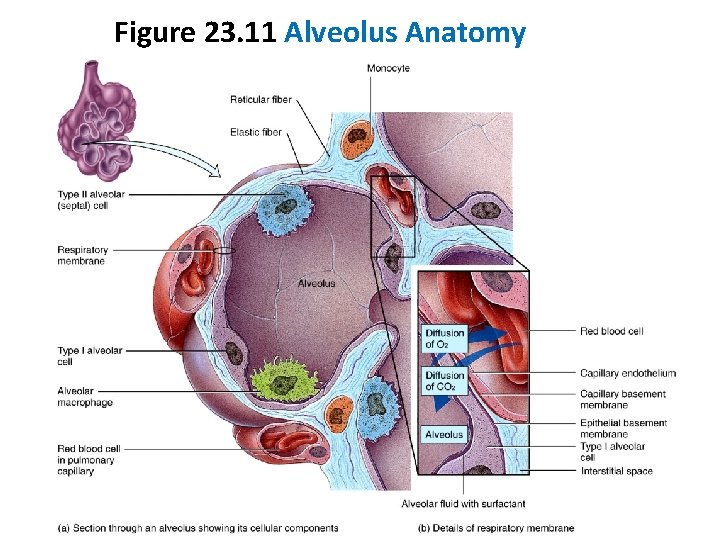
Figure 23. 11 Alveolus Anatomy
Blood Supply to the lungs • Lungs have a double blood supply • Blood enters lungs via pulmonary arteries (pulmonary circulation) and bronchial arteries (systemic circulation) • Most blood leaves by pulmonary veins; some drains into bronchial veins • Ventilation-perfusion coupling - vasoconstriction in response to hypoxia diverts pulmonary blood from poorly ventilated areas to well ventilated areas

Respiratory System Topics 1. 2. 3. 4. 5. 6. Anatomy of the Respiratory System Pulmonary Ventilation Lung Volumes and Capacities Oxygen and Carbon Dioxide Exchange Oxygen and Carbon Dioxide Transport Control of Respiration

Respiration • Reminder The process of gas exchange in the body, has three basic steps: • Ventilation • External respiration • Internal respiration

PULMONARY VENTILATION • Pulmonary ventilation – • Inhalation and exhalation • Exchange between atmosphere and lung alveoli • Air exchange is due to pressure change created by respiratory muscle contraction and relaxation • Air exchange also influenced by alveolar fluid surface tension, lung compliance, and airway resistance

Pressure Changes during Pulmonary Ventilation • Air flows down a pressure gradient: • Into lungs when alveolar pressure < atmospheric pressure • Out of lungs when alveolar pressure > atmospheric pressure • Boyle’s Law – For a fixed amount of an ideal gas kept at a fixed temperature in a closed space, pressure and volume are inversely proportional. • The volume of a gas varies inversely with its pressure • Changes in lung volume cause changes in alveolar pressure
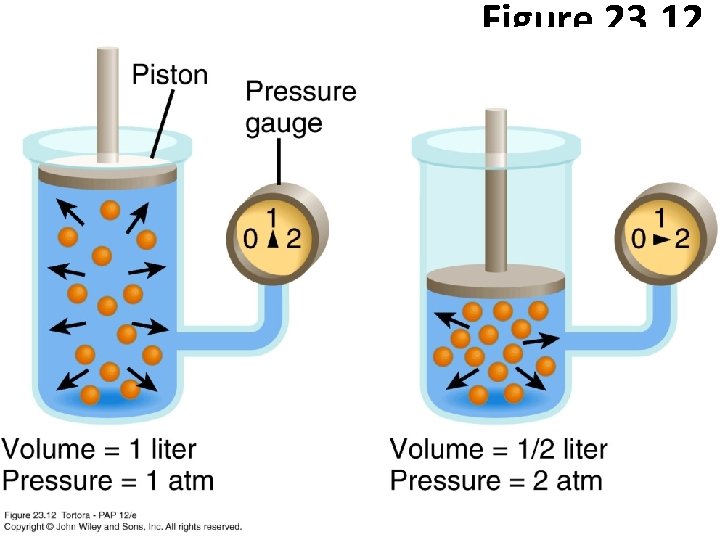
Figure 23. 12 Boyle’s law

Inhalation • Inhalation - the process of bringing air into the lungs • Inhalation occurs when alveolar pressure falls below atmospheric pressure
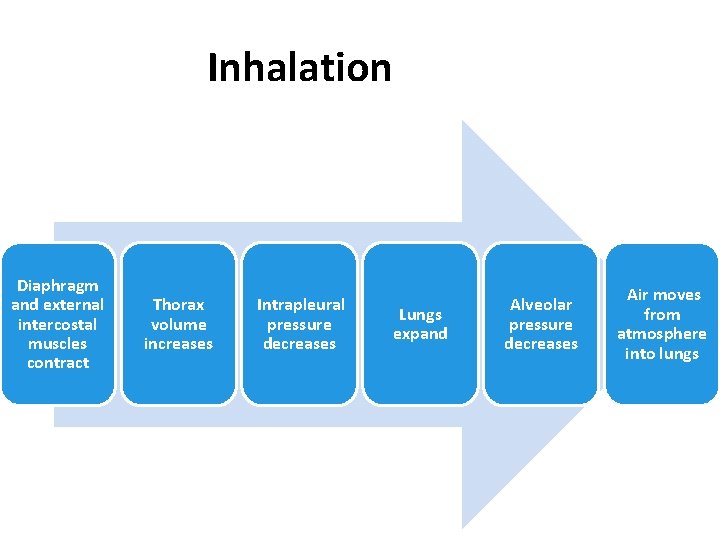
Inhalation Diaphragm and external intercostal muscles contract Thorax volume increases Intrapleural pressure decreases Lungs expand Alveolar pressure decreases Air moves from atmosphere into lungs
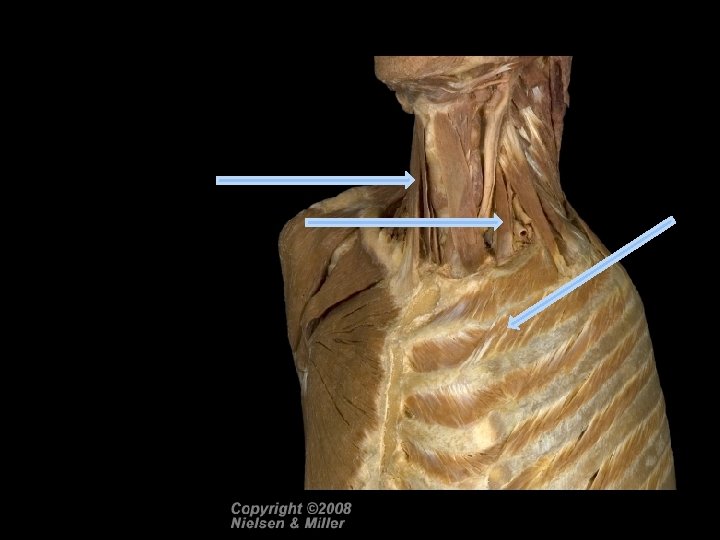
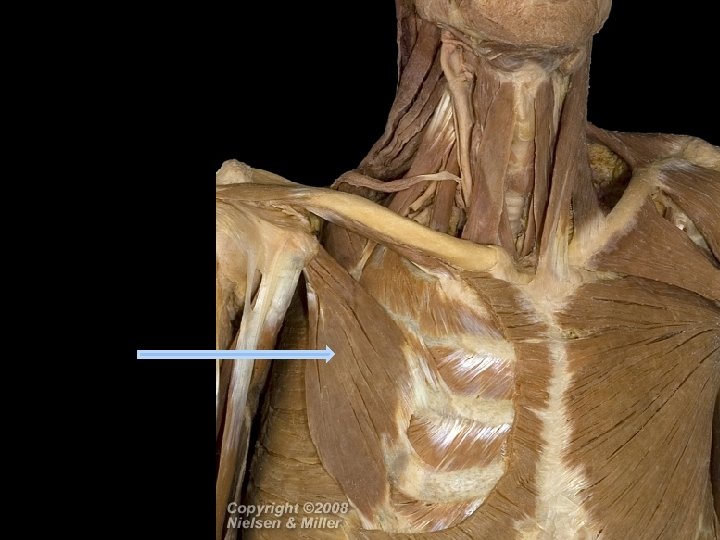
Inhalation • Accessory muscles of inspiration are used during forced inhalation: • Sternocleidomastoids • Scalenes • Pectoralis minor
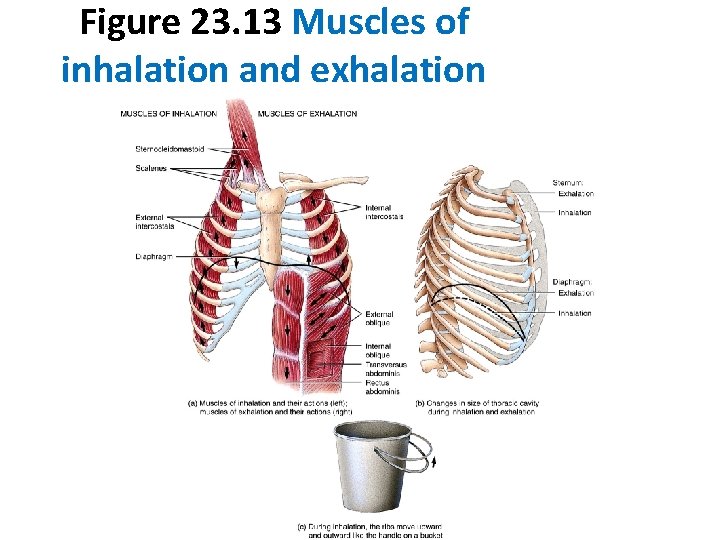
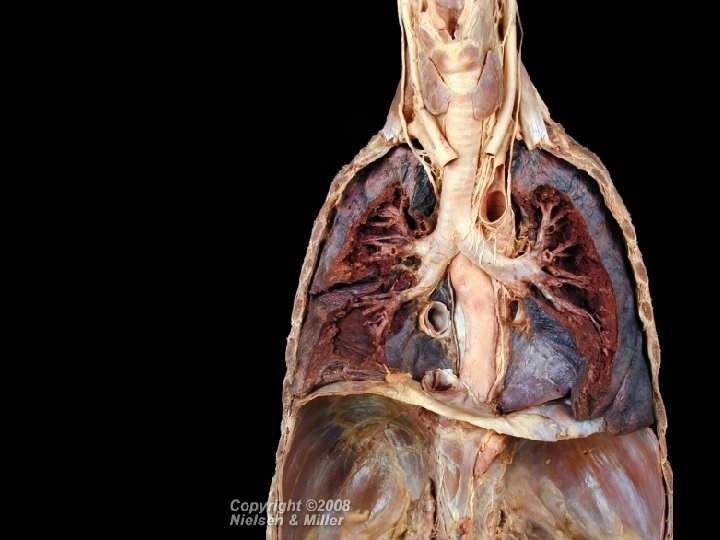
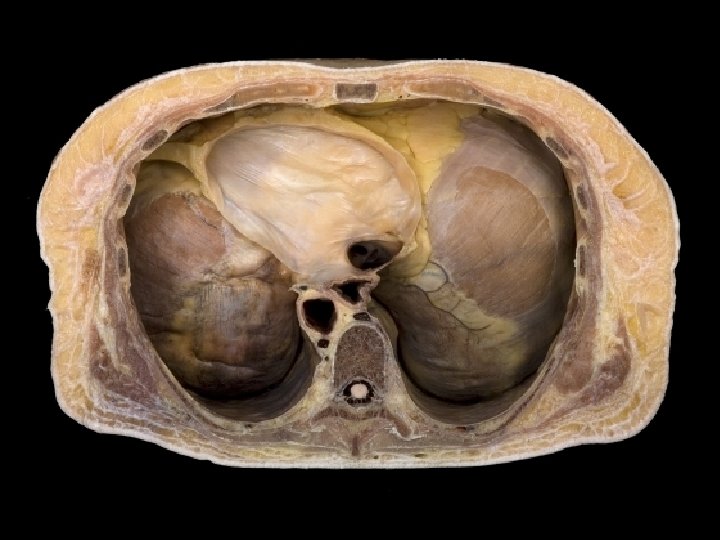
Figure 23. 13 Muscles of inhalation and exhalation
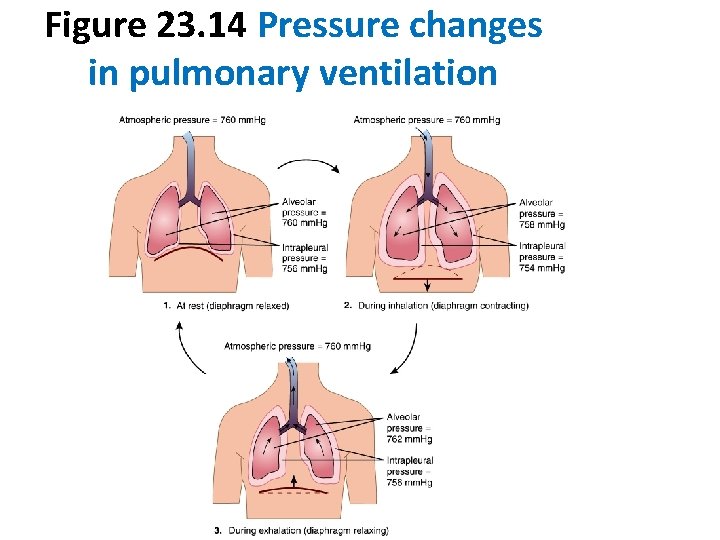
Figure 23. 14 Pressure changes in pulmonary ventilation

Exhalation • Exhalation - process of moving air out of lungs • Exhalation occurs when alveolar pressure is higher than atmospheric pressure
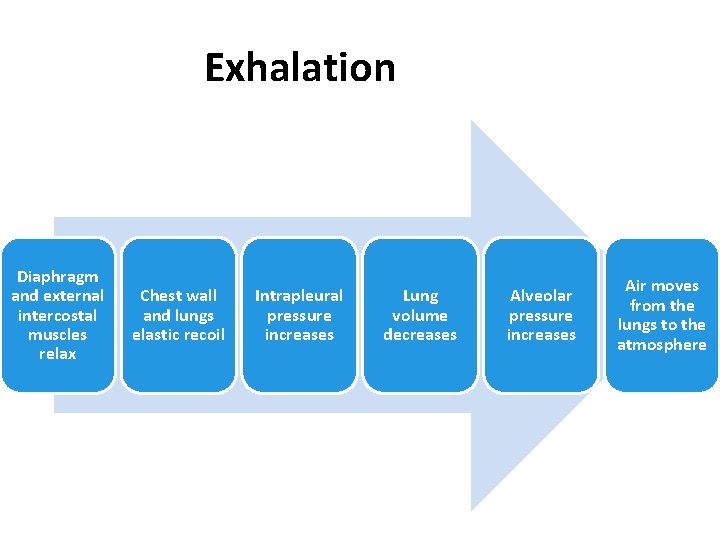
Exhalation Diaphragm and external intercostal muscles relax Chest wall and lungs elastic recoil Intrapleural pressure increases Lung volume decreases Alveolar pressure increases Air moves from the lungs to the atmosphere

Exhalation • Exhalation becomes active during labored breathing • Accessory muscles of expiration are used during forced exhalation: • Internal intercostals • Abdominal muscles
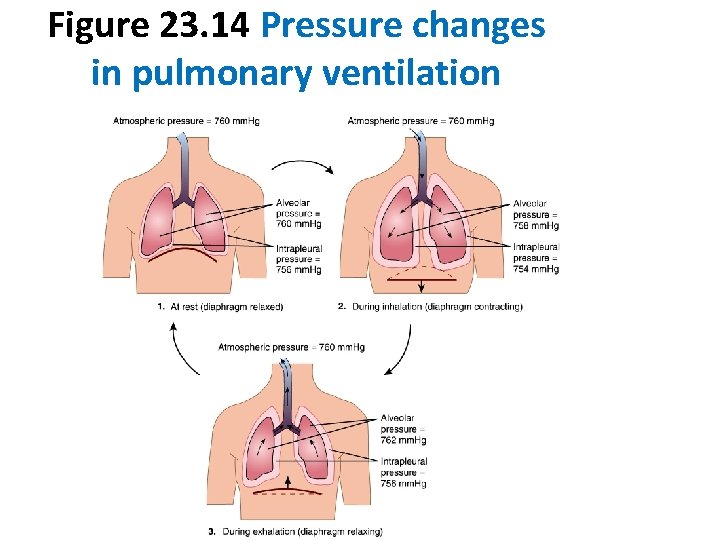
Figure 23. 14 Pressure changes in pulmonary ventilation
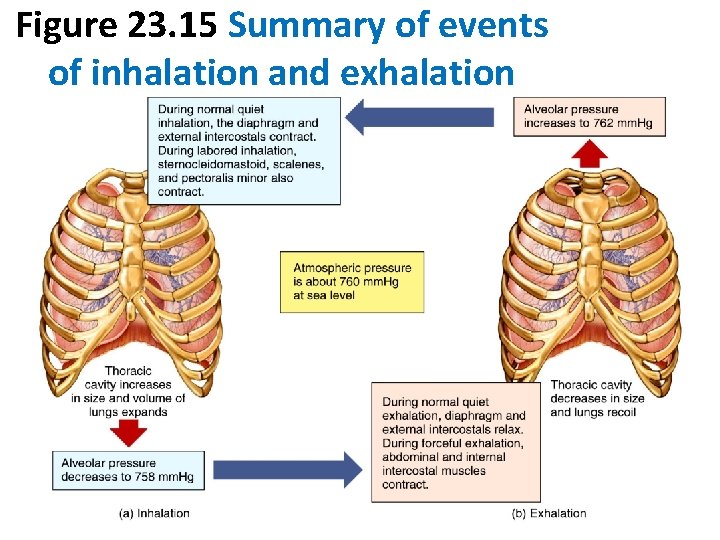
Figure 23. 15 Summary of events of inhalation and exhalation

Other Factors Affecting Pulmonary Ventilation Assigned Reading pages 860 -861 • • • Alveolar fluid surface tension Lung compliance Airway resistance Reminder – table 23. 1 page 857 is a very good summary of the tissue types of the respiratory system anatomy. Important!! Table 23. 2 – summary of modified breathing movements. Easy to make test questions from this…

Respiratory System Topics 1. 2. 3. 4. 5. 6. Anatomy of the Respiratory System Pulmonary Ventilation Lung Volumes and Capacities Oxygen and Carbon Dioxide Exchange Oxygen and Carbon Dioxide Transport Control of Respiration
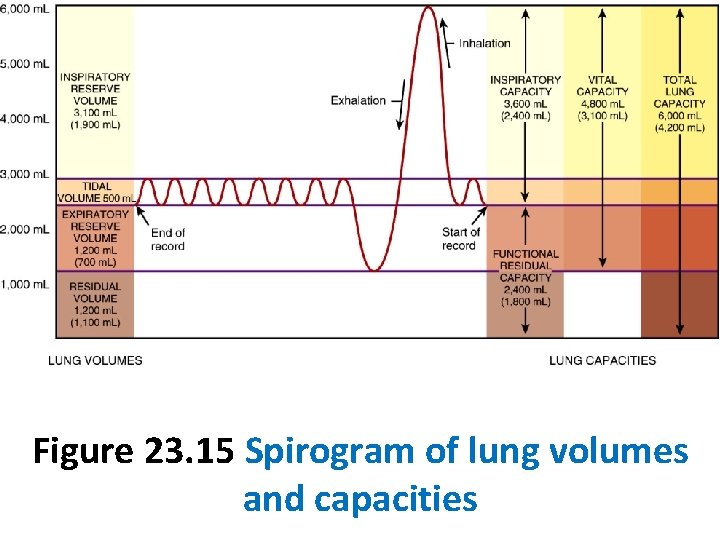
Figure 23. 15 Spirogram of lung volumes and capacities

Respiratory System Topics 1. 2. 3. 4. 5. 6. Anatomy of the Respiratory System Pulmonary Ventilation Lung Volumes and Capacities Oxygen and Carbon Dioxide Exchange Oxygen and Carbon Dioxide Transport Control of Respiration

Gas Exchange • The point of pulmonary ventilation = exchange of 2 gases. • Level of lungs (external) • Level of tissues (internal)

EXCHANGE OF OXYGEN AND CARBON DIOXIDE Dalton’s law • Explains how gases diffuse down a pressure gradient Henry’s law • Explains how gas solubility (how much gas can a liquid actually carry) affects diffusion
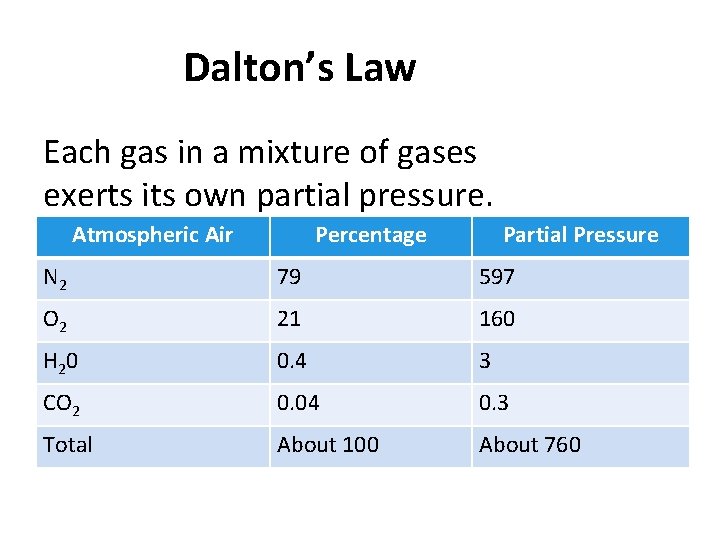
Dalton’s Law Each gas in a mixture of gases exerts its own partial pressure. Atmospheric Air Percentage Partial Pressure N 2 79 597 O 2 21 160 H 2 0 0. 4 3 CO 2 0. 04 0. 3 Total About 100 About 760

Dalton’s Law • The composition of alveolar air differs from atmospheric air because: • O 2 is constantly diffusing out of alveolar air • CO 2 is constantly diffusing into alveolar air • Humidification increases water’s partial pressure, which decreases partial pressures of other gases
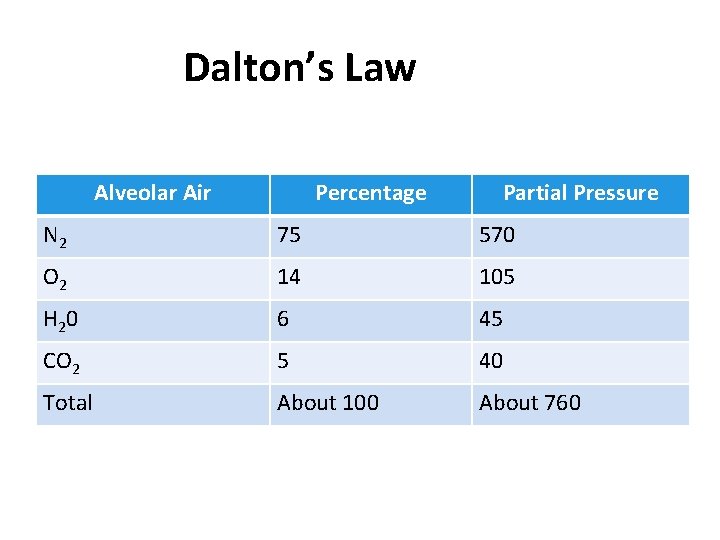
Dalton’s Law Alveolar Air Percentage Partial Pressure N 2 75 570 O 2 14 105 H 2 0 6 45 CO 2 5 40 Total About 100 About 760

Henry’s Law • The quantity of a gas that will dissolve in a liquid is proportional to the partial pressure of the gas and its solubility • • At atmospheric pressure, N 2 is relatively insoluble in blood At atmospheric pressure, CO 2 is more soluble than oxygen

External and Internal Respiration • O 2 and CO 2 diffuse from areas of high partial pressure to areas of low partial pressure.
External Respiration External respiration • Gas exchange between air in the lungs and blood • Converts deoxygenated blood into oxygenated blood

External Respiration During external respiration, O 2 and CO 2 diffuse down their partial pressure gradients. Gas Alveolar Air Venous Blood O 2 105 40 CO 2 40 45
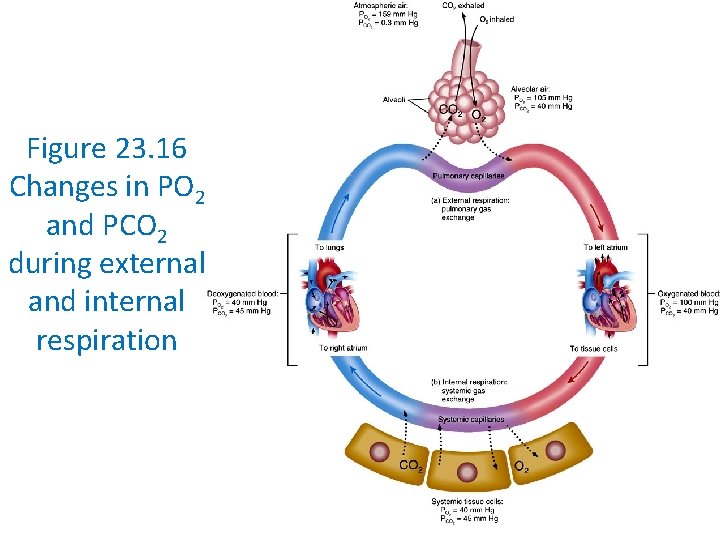
Figure 23. 16 Changes in PO 2 and PCO 2 during external and internal respiration
Internal Respiration Internal respiration • Gas exchange between blood and tissue cells • Converts oxygenated blood into deoxygenated blood
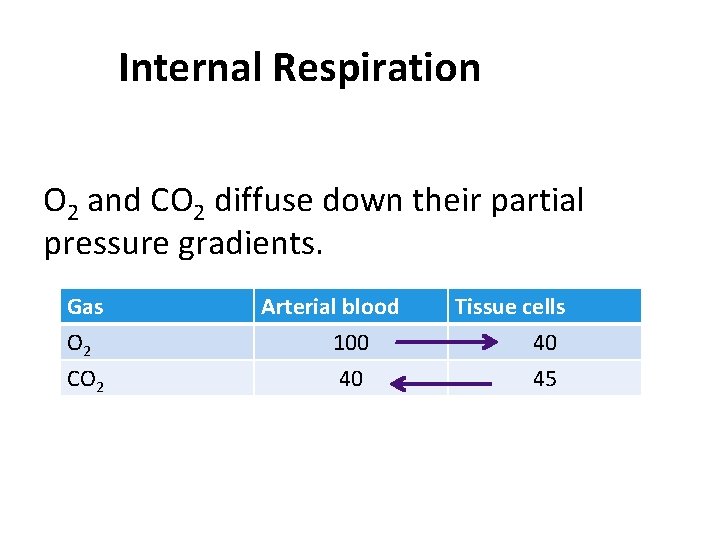
Internal Respiration O 2 and CO 2 diffuse down their partial pressure gradients. Gas O 2 CO 2 Arterial blood 100 40 Tissue cells 40 45
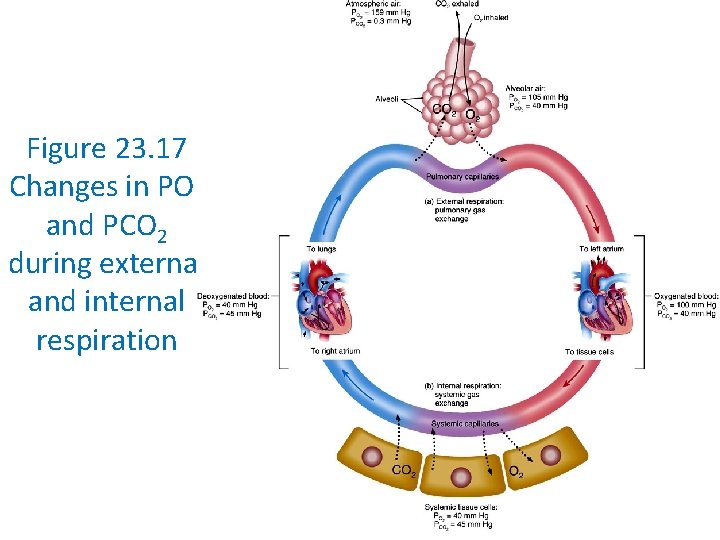
Figure 23. 17 Changes in PO 2 and PCO 2 during external and internal respiration

Factors that Affect the Rate of Oxygen and Carbon Dioxide Exchange Partial pressure differences of the gases • greater partial pressure differences faster diffusion rates Surface area available for gas exchange • more surface area faster diffusion rate Diffusion distance • thinner membrane faster diffusion Molecular weight and gas solubility • lighter more soluble molecules faster diffusion

Respiratory System Topics 1. 2. 3. 4. 5. 6. Anatomy of the Respiratory System Pulmonary Ventilation Lung Volumes and Capacities Oxygen and Carbon Dioxide Exchange Oxygen and Carbon Dioxide Transport Control of Respiration
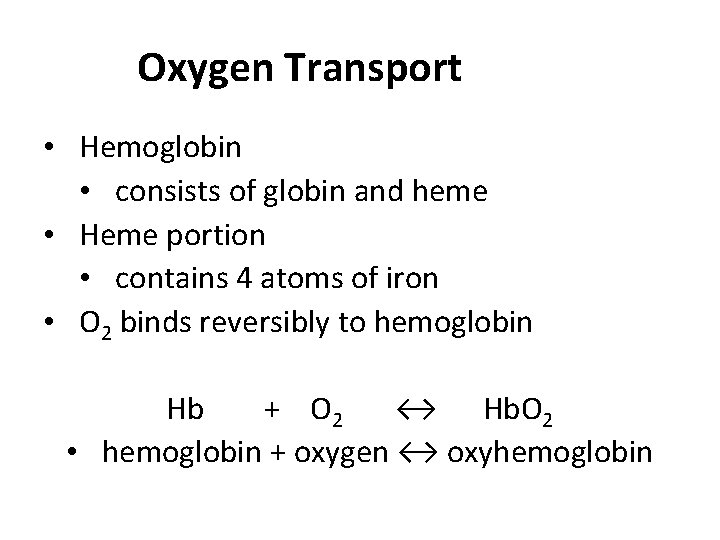
Oxygen Transport • Hemoglobin • consists of globin and heme • Heme portion • contains 4 atoms of iron • O 2 binds reversibly to hemoglobin Hb + O 2 ↔ Hb. O 2 • hemoglobin + oxygen ↔ oxyhemoglobin

The relationship between Hemoglobin and Oxygen Partial Pressure • The most important factor that determines how much oxygen combines with hemoglobin is oxygen’s partial pressure (PO 2). • As PO 2 increases, more O 2 combines with hemoglobin.

The relationship between Hemoglobin and Oxygen Partial Pressure • In pulmonary capillaries, where PO 2 is high, hemoglobin is very “sticky” and a lot of O 2 binds to it. • In systemic capillaries, where PO 2 is low, hemoglobin is not as “sticky” for O 2 and the dissolved O 2 is unloaded via diffusion into tissue cells.
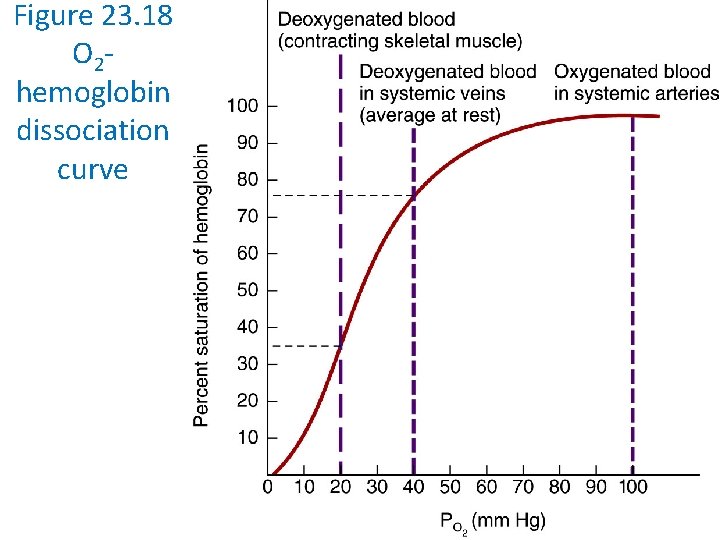
Figure 23. 18 O 2 hemoglobin dissociation curve

Other Factors Affecting Hemoglobin Affinity for Oxygen Blood p. H • As p. H decreases, hemoglobin’s affinity for O 2 declines PCO 2 • As PCO 2 increases, hemoglobin’s affinity for O 2 declines Temperature • As temperature increases, hemoglobin’s affinity for O 2 declines BPG • As BPG increases, hemoglobin’s affinity for O 2 declines
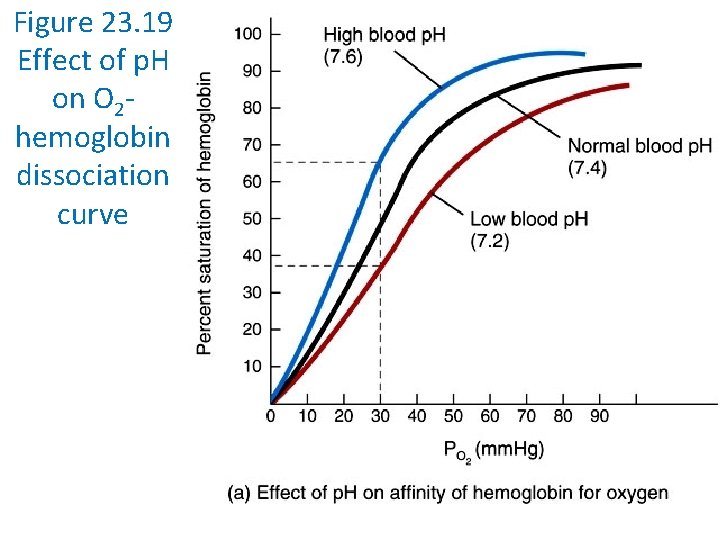
Figure 23. 19 Effect of p. H on O 2 hemoglobin dissociation curve
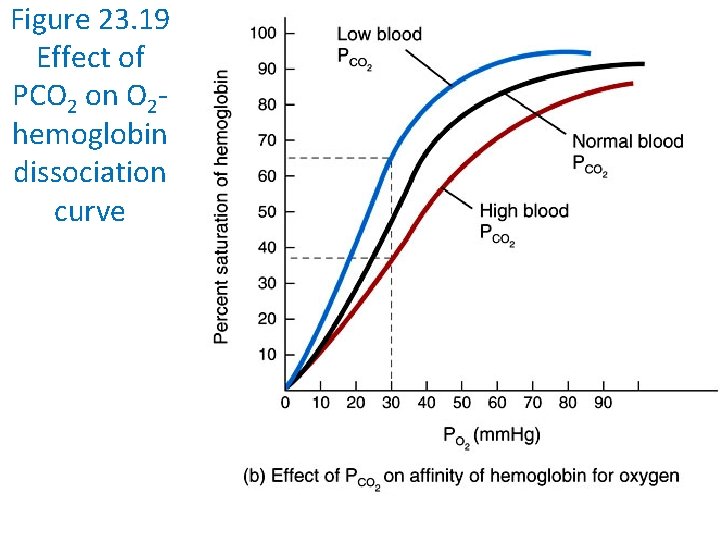
Figure 23. 19 Effect of PCO 2 on O 2 hemoglobin dissociation curve
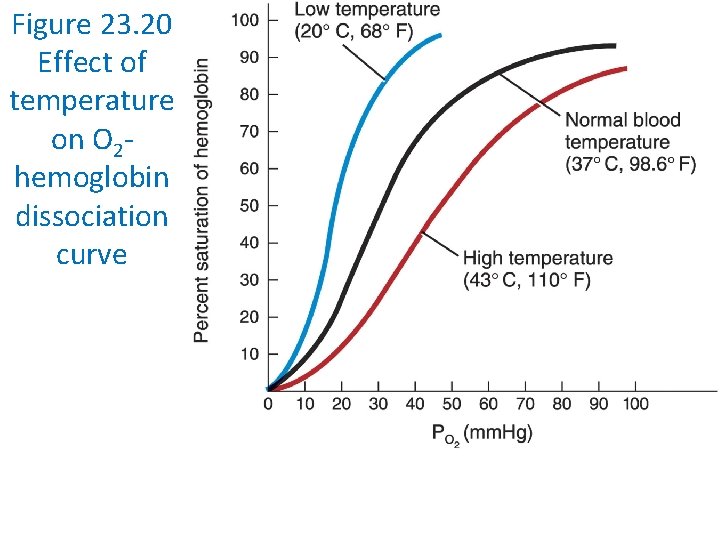
Figure 23. 20 Effect of temperature on O 2 hemoglobin dissociation curve

Oxygen Affinity of Fetal and Adult Hemoglobin • Fetal hemoglobin has a higher affinity for oxygen than does adult hemoglobin • Fetal hemoglobin binds BPG less strongly and can carry more oxygen to offset the low oxygen saturation in maternal blood in the placenta
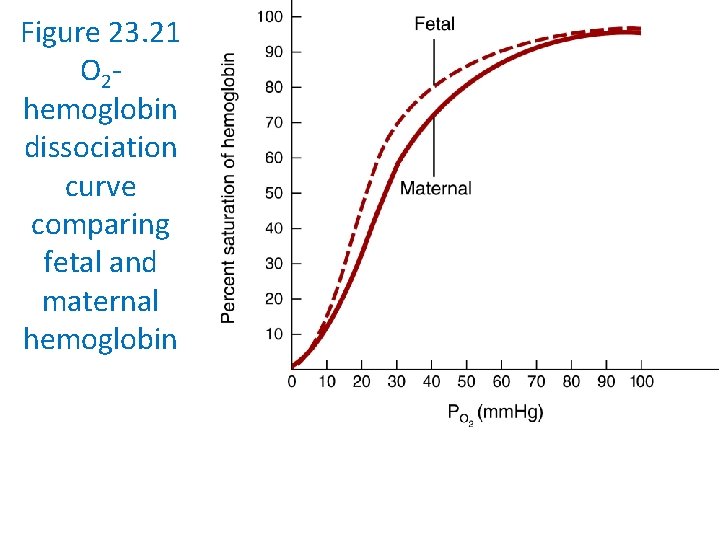
Figure 23. 21 O 2 hemoglobin dissociation curve comparing fetal and maternal hemoglobin

Carbon Dioxide Transport • CO 2 is carried in blood in the form of: 1. Dissolved CO 2 (7%) 2. Carbaminohemoglobin (23%) 3. Bicarbonate ions (70%) • CO 2 + H 20 ↔ H 2 CO 3 ↔ H+ + HCO 3 -

Carbon Dioxide Transport • As CO 2 enters RBCs it is converted into bicarbonates (builds up within RBCs). • Bicarbonate ions diffuse out of the cell plasma (down its [ gradient ] ). • In exchange, Cl- diffuses into RBCs • The conversion of CO 2 to bicarbonate ions and the related chloride shift maintains the ionic balance between plasma and RBCs.
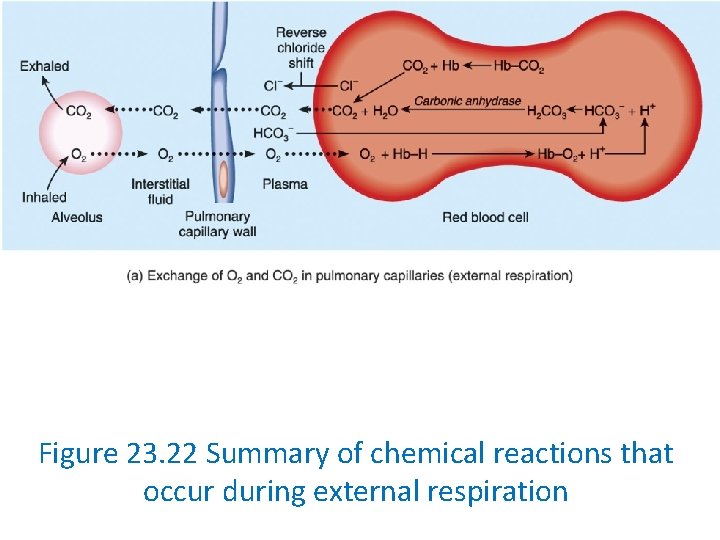
Figure 23. 22 Summary of chemical reactions that occur during external respiration
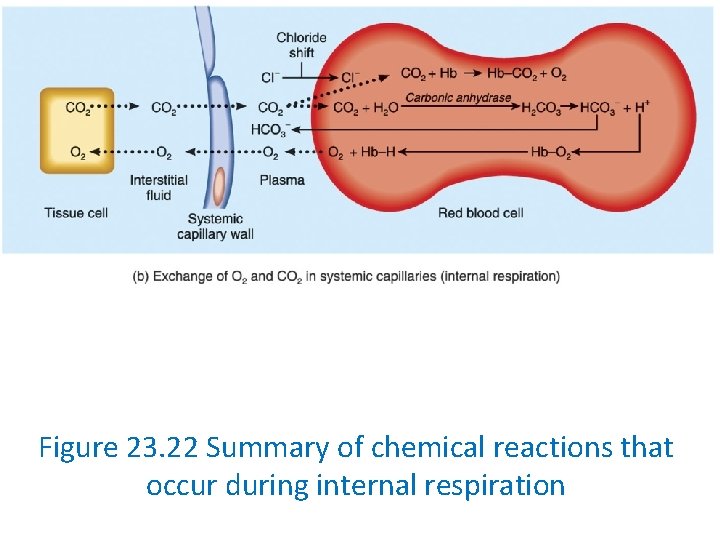
Figure 23. 22 Summary of chemical reactions that occur during internal respiration

Respiratory System Topics 1. 2. 3. 4. 5. 6. Anatomy of the Respiratory System Pulmonary Ventilation Lung Volumes and Capacities Oxygen and Carbon Dioxide Exchange Oxygen and Carbon Dioxide Transport Control of Respiration

Respiratory Center • The respiratory center is composed of neurons in: • Medullary rhythmicity area in the medulla oblongata • Pneumotaxic area in the pons • Apneustic areas in the pons
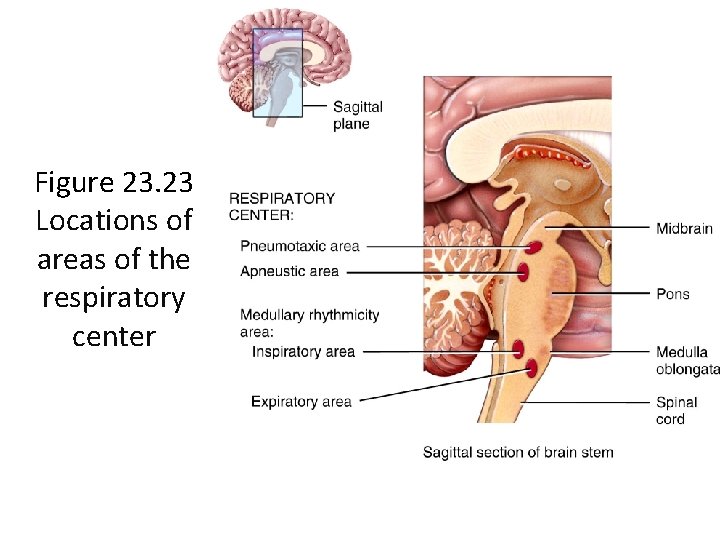
Figure 23. 23 Locations of areas of the respiratory center
- Slides: 106