http www google comimgres Anatomy and Physiology Blood
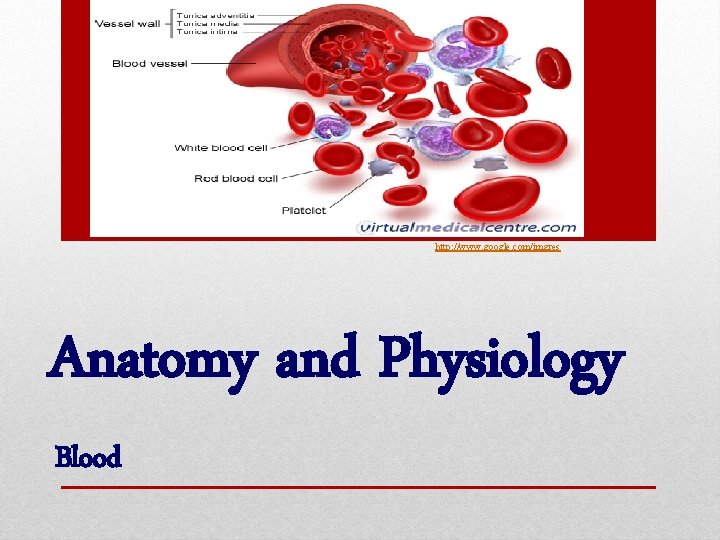
http: //www. google. com/imgres Anatomy and Physiology Blood

Blood has several functions, according to its components: red blood cells (rbc’s) carry oxygen, white blood cells (wbc’s) protect against/fight infection, and platelets promote clotting. • Blood within an adult human is ~5 liters. • Whole blood is heavier and more viscous than water. • A hematocrit (HCT) is the percentage of blood cell volume (generally 45%). • The majority of cells are rbc’s, then wbc’s, and platelets (considered fragments in the blood).
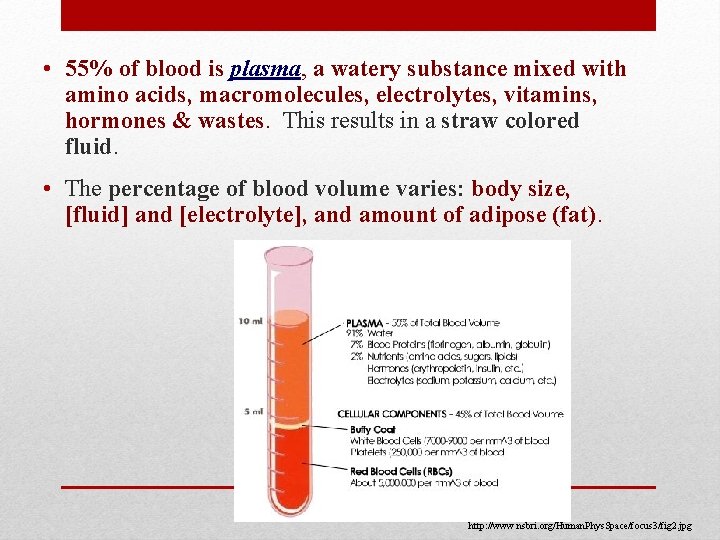
• 55% of blood is plasma, a watery substance mixed with amino acids, macromolecules, electrolytes, vitamins, hormones & wastes. This results in a straw colored fluid. • The percentage of blood volume varies: body size, [fluid] and [electrolyte], and amount of adipose (fat). http: //www. nsbri. org/Human. Phys. Space/focus 3/fig 2. jpg

• Blood components can be separated by centrifuging them: http: //www. google. com/imgres • plasma is the lightest (and rests atop the rest), the buffy coat is the middle layer of cells containing wbc’s and platelets while the bottommost layer contains the rbc’s.

Blood Plasma: • clear, straw colored fluid • liquid portion of blood • contains ~90% water & a mix of dissolved chemicals (macromolecules, vitamins, electrolytes & wastes) http: //www. google. com/imgres • proteins are the most abundant of the dissolved substances in plasma

• There are 3 groups of proteins: albumins, globulins, and fibrinogen. • albumins: smallest but majority of the plasma proteins (by weight); regulate the movement of water controlling blood volume & controlling b. p. • globulins: transport lipids &fat soluble vitamins; 3 types: alpha, beta, gamma • fibrinogen: largest but least of plasma proteins; functions in blood coagulation (clumping)

Red Blood Cells: • Transports gases, like O 2 • a. k. a. erythrocytes • concave disks (look like • Mature rbc’s lack nuclei (no longer divide or donuts with no hole). produce proteins) http: //www. google. com/imgres http: //embryology. med. unsw. edu. au/Notes/images/rbc. jpg
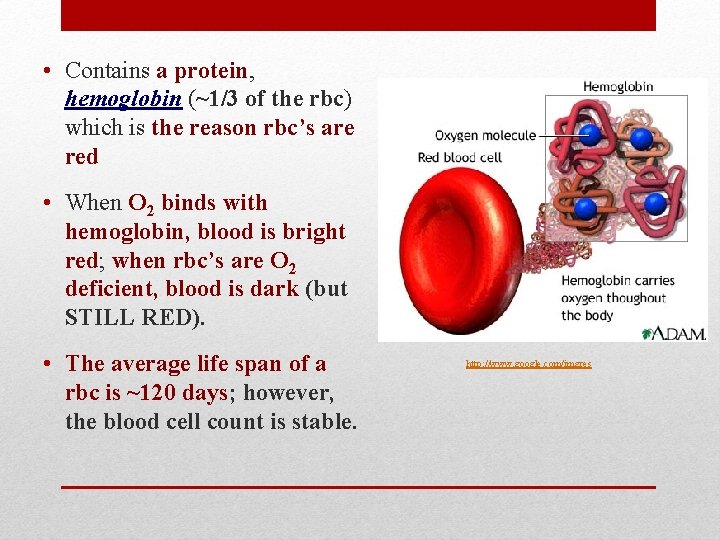
• Contains a protein, hemoglobin (~1/3 of the rbc) which is the reason rbc’s are red • When O 2 binds with hemoglobin, blood is bright red; when rbc’s are O 2 deficient, blood is dark (but STILL RED). • The average life span of a rbc is ~120 days; however, the blood cell count is stable. http: //www. google. com/imgres
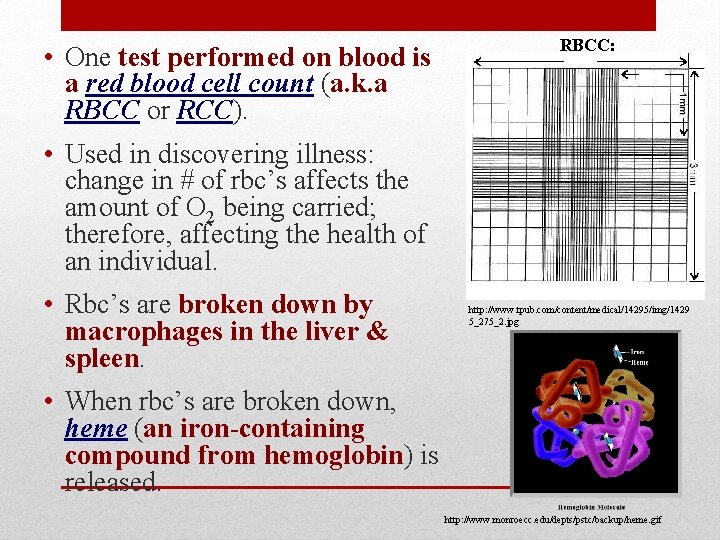
• One test performed on blood is a red blood cell count (a. k. a RBCC or RCC). RBCC: • Used in discovering illness: change in # of rbc’s affects the amount of O 2 being carried; therefore, affecting the health of an individual. • Rbc’s are broken down by macrophages in the liver & spleen. http: //www. tpub. com/content/medical/14295/img/1429 5_275_2. jpg • When rbc’s are broken down, heme (an iron-containing compound from hemoglobin) is released. http: //www. monroecc. edu/depts/pstc/backup/heme. gif

• Rbc production is controlled by a negative feedback mechanism: erythropoietin (a hormone) regulates rbc formation. • When O 2 is deficient, the kidneys & liver release erythropoietin to make rbc’s. • Rbc production requires: vitamin B 12, folic acid, and iron. • Anemia is a condition in which there are too few rbc’s or too little hemoglobin. This condition results in fatigue or lack of energy. Many women have this condition due to menstruation or pregnancy. • Look up anemia online or in text to see types.
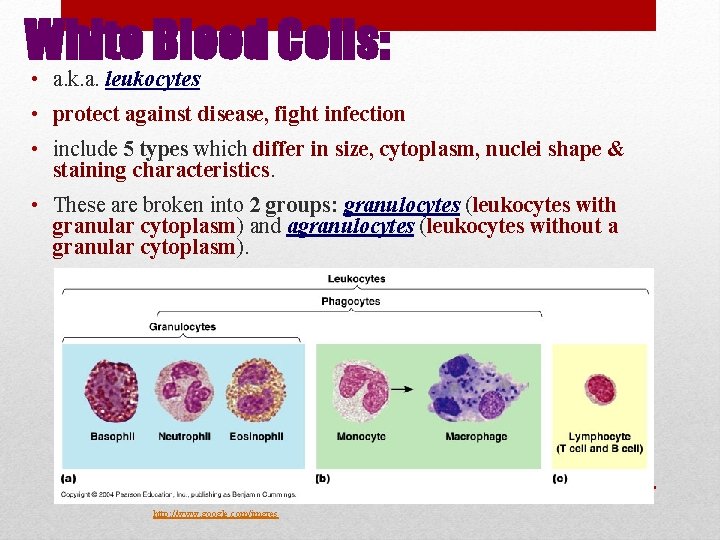
White Blood Cells: • a. k. a. leukocytes • protect against disease, fight infection • include 5 types which differ in size, cytoplasm, nuclei shape & staining characteristics. • These are broken into 2 groups: granulocytes (leukocytes with granular cytoplasm) and agranulocytes (leukocytes without a granular cytoplasm). http: //www. google. com/imgres
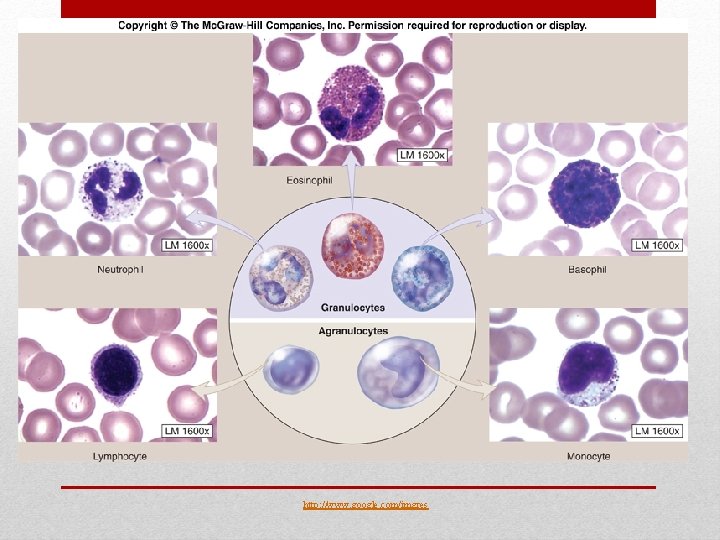
http: //www. google. com/imgres

• are twice the size of a rbc • contain granular cytoplasm • are produced in the red bone marrow • life span is ~12 hours • include: Neutrophils, Basophils, and Eosinophils Granulocytes
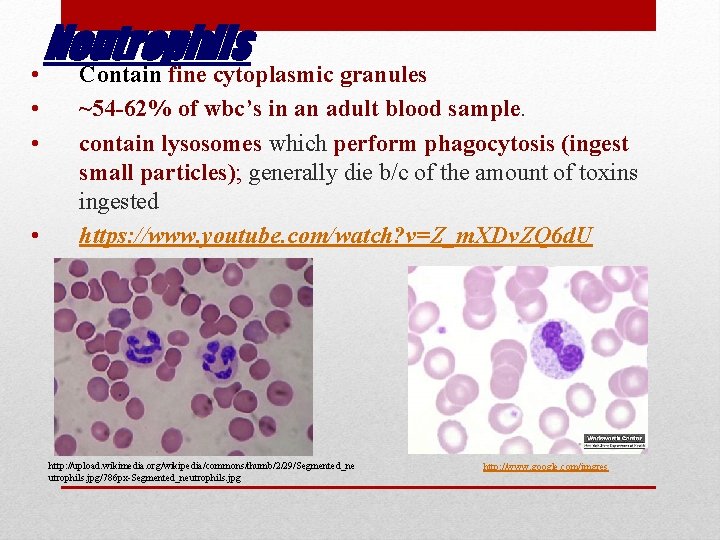
Neutrophils • Contain fine cytoplasmic granules • • • ~54 -62% of wbc’s in an adult blood sample. contain lysosomes which perform phagocytosis (ingest small particles); generally die b/c of the amount of toxins ingested https: //www. youtube. com/watch? v=Z_m. XDv. ZQ 6 d. U http: //upload. wikimedia. org/wikipedia/commons/thumb/2/29/Segmented_ne utrophils. jpg/786 px-Segmented_neutrophils. jpg http: //www. google. com/imgres

Eosinophils • uniformly sized cytoplasmic granules • ~1 -3% of wbc’s circulating. • kill specific parasites, control allergic reactions & inflammation & are weakly phagocytic http: //www. jameswpattersonmd. com/images/pages/churg_strauss_ eosinophils. jpg http: //www. google. com/imgres
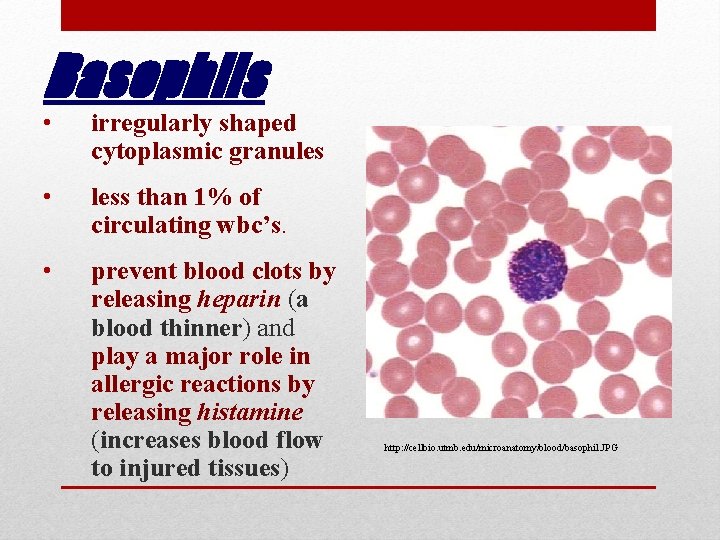
Basophils • irregularly shaped cytoplasmic granules • less than 1% of circulating wbc’s. • prevent blood clots by releasing heparin (a blood thinner) and play a major role in allergic reactions by releasing histamine (increases blood flow to injured tissues) http: //cellbio. utmb. edu/microanatomy/blood/basophil. JPG

• no cytoplasmic granules • include 2 types of wbc’s: Monocytes & Lymphocytes https: //www. youtube. com/watch? v=BDr 44 v. LNn. PY https: //www. youtube. com/watch? v=qv. GVoxdy-y. M&spfreload=1 Agranulocytes
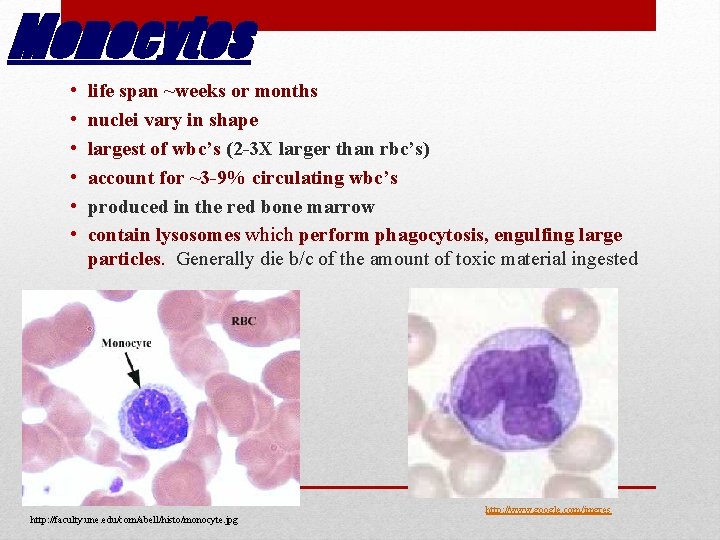
Monocytes • • • life span ~weeks or months nuclei vary in shape largest of wbc’s (2 -3 X larger than rbc’s) account for ~3 -9% circulating wbc’s produced in the red bone marrow contain lysosomes which perform phagocytosis, engulfing large particles. Generally die b/c of the amount of toxic material ingested http: //faculty. une. edu/com/abell/histo/monocyte. jpg http: //www. google. com/imgres

Lymphocytes • life span ~years • nuclei is large & round • slightly larger than rbc’s http: //www. google. com/imgres • ~25 -33% of circulating wbc’s • produced in the red bone marrow & lymphatic system organs • produce antibodies providing immunity. http: //www. unis. org/UNIScience. Net/RBCs+Lymphocytes. jpg

• There are 5 types of White Blood cells in circulation. • From the majority of cells to the least amount of cells in circulation: Neutrophils (N) Lymphocytes (L) Monocytes (M) Eosinophils (E) Basophils (B) • An acronym: Never Let My Eggs Break! Brief Summary

White Blood Cells: • A white blood cell count (WBCC) is a diagnostic test that measures the amount of wbc’s in a sample of blood. • Generally, a differential WBCC (DIFF) is performed. This is a test that provides the %ages of wbc’s (types of leukocytes in a sample of blood). • Wbc’s are able to leave the blood & move by amboid motion (self-propulsion)
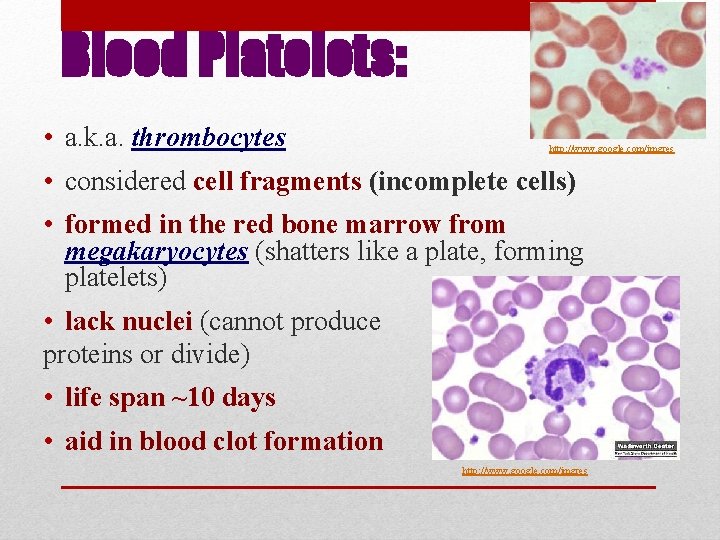
Blood Platelets: • a. k. a. thrombocytes http: //www. google. com/imgres • considered cell fragments (incomplete cells) • formed in the red bone marrow from megakaryocytes (shatters like a plate, forming platelets) • lack nuclei (cannot produce proteins or divide) • life span ~10 days • aid in blood clot formation http: //www. google. com/imgres

• This is a. k. a. blood cell formation • Occurs in red bone marrow • Erythropoietin (hormone) controls rbc production. • Thrombopoietin (hormone) controls thrombocyte production. • Interleukins & colony stimulating factors (CSFs) control wbc production. Hematopoiesis:

• This is the stoppage of bleeding. • When a blood vessel (bv) is cut, blood flows. Almost immediately, a bv spasm, a. k. a. a vasospasm, occurs. This is the constriction of a bv by the smooth muscles contracting, slowing blood flow. • This occurs in 3 steps: vascular spasm, platelet plug formation, and coagulation. Hemostasis
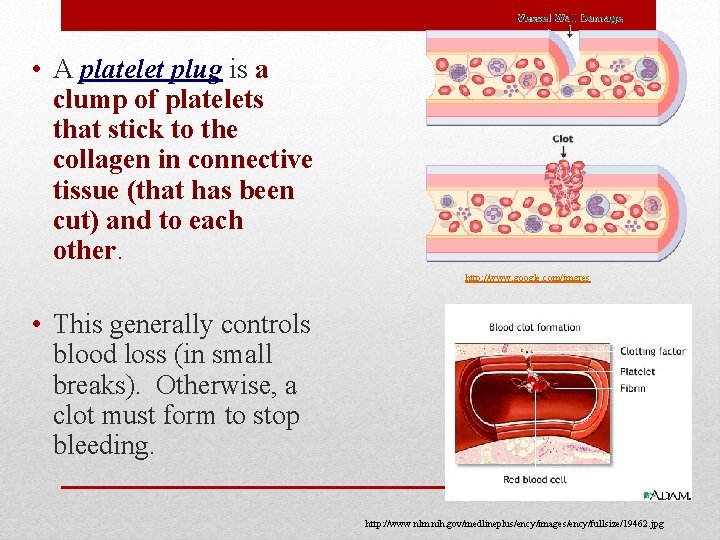
• A platelet plug is a clump of platelets that stick to the collagen in connective tissue (that has been cut) and to each other. http: //www. google. com/imgres • This generally controls blood loss (in small breaks). Otherwise, a clot must form to stop bleeding. http: //www. nlm. nih. gov/medlineplus/ency/images/ency/fullsize/19462. jpg

Blood Coagulation • This causes a blood clot and is the result of clotting factors (biochemicals that help or inhibit the formation of a clot). • In normal bodies, anticoagulants do not allow blood to clot. • However, when a clot forms (called formation), fibrinogen forms fibrin (insoluble threads of protein). • A blood clot forms from a series of events: prothrombin (a normal component of plasma produced in the liver) is converted to thrombin in the presence of Ca++. • Thrombin then triggers a series of reactions that convert fibrinogen into fibrin, causing a blood clot.

• Fibrin causes a meshwork of threads that trap platelets & blood cells, forming a mass that stops blood flow. • Fibrin threads are eventually dissolved and the injury is healed. • This is how bruises (hematomas) are healed. Hematomas are caused by blood leaks within a damaged tissue. http: //cache. eb. com/eb/image? id=98328&rend. Type. Id=4
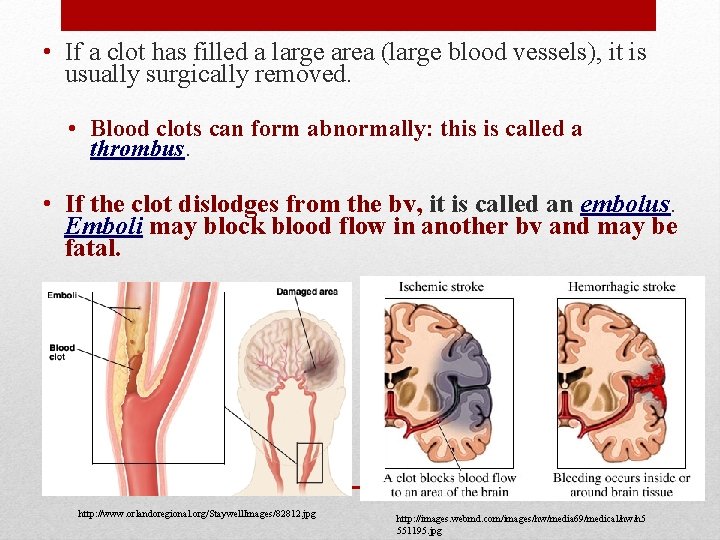
• If a clot has filled a large area (large blood vessels), it is usually surgically removed. • Blood clots can form abnormally: this is called a thrombus. • If the clot dislodges from the bv, it is called an embolus. Emboli may block blood flow in another bv and may be fatal. http: //www. orlandoregional. org/Staywell. Images/82812. jpg http: //images. webmd. com/images/hw/media 69/medical/hw/h 5 551195. jpg
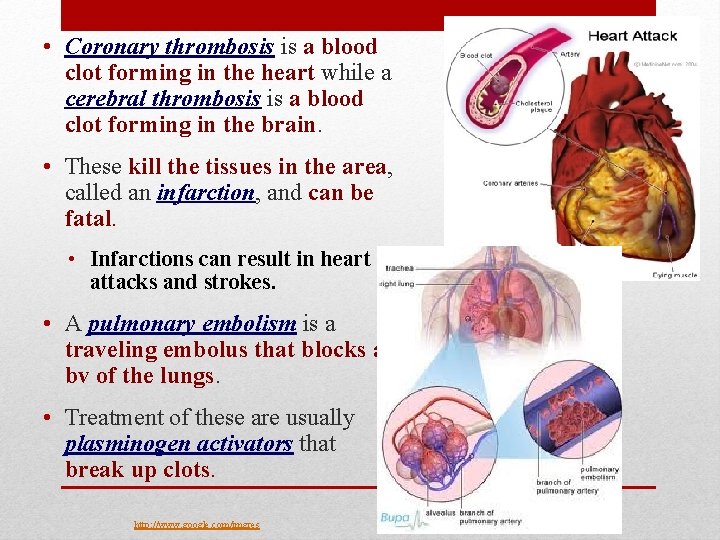
• Coronary thrombosis is a blood clot forming in the heart while a cerebral thrombosis is a blood clot forming in the brain. • These kill the tissues in the area, called an infarction, and can be fatal. • Infarctions can result in heart attacks and strokes. • A pulmonary embolism is a traveling embolus that blocks a bv of the lungs. • Treatment of these are usually plasminogen activators that break up clots. http: //www. google. com/imgres
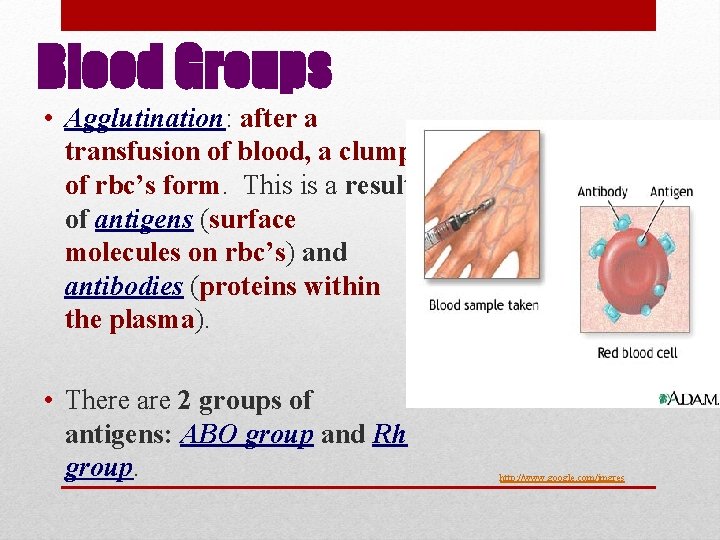
Blood Groups • Agglutination: after a transfusion of blood, a clump of rbc’s form. This is a result of antigens (surface molecules on rbc’s) and antibodies (proteins within the plasma). • There are 2 groups of antigens: ABO group and Rh group. http: //www. google. com/imgres

ABO group • This is the presence or absence of antigens on the surface of rbc’s. • These antigens are A, B, or A and B. • These are a direct result of the person’s blood type, which is inherited. • If a person has antigen A, then he has type A blood; if a person has antigen B, then he has type B blood; if a person has both antigens A and B, then that person has type AB blood; if a person lacks antigens, then the person has type O blood.

• If the person has type A blood, they have anti-B; this means that the have antibodies against antigen B. What is the significance of this? A person with type A blood cannot receive type AB or type B blood receive type A or type O blood. Blood Type A B AB O Antigen A B A&B none Antibody anti-B anti-A none anti-A &B Transfuse A; O B; O A; B; AB; O O
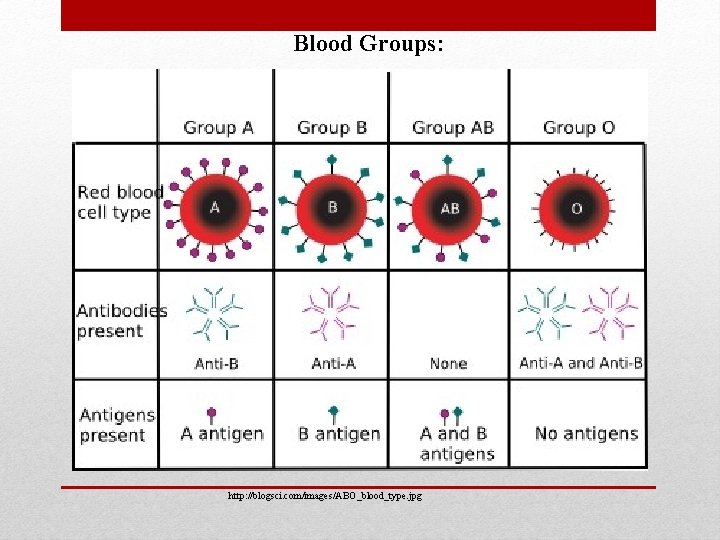
Blood Groups: http: //blogsci. com/images/ABO_blood_type. jpg

• This was named after the Rhesus monkey. These are antigens (factors) in human blood (as well as monkey blood). • These antigens are inherited as well. • When blood types are said to be Rh negative (Rh-), there are no Rh antigens while if the blood type is said to be Rh positive (Rh+), there is at least 1 type of Rh antigen. Rh Blood Group
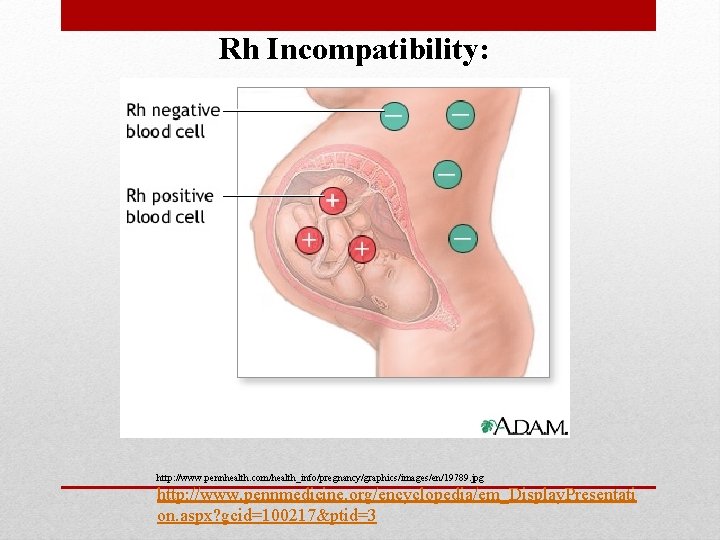
Rh Incompatibility: http: //www. pennhealth. com/health_info/pregnancy/graphics/images/en/19789. jpg http: //www. pennmedicine. org/encyclopedia/em_Display. Presentati on. aspx? gcid=100217&ptid=3

THE END!

• This slide show was developed by Dana Halloran, • Cardinal Mooney High School, Sarasota, FL. • Used with her personal permission, • adapted and amended by Rosa Whiting, • Manatee School for the Arts, Palmetto, FL.
- Slides: 37