HSC 4652 HEALTHCARE ETHICS Chapter 12 Patient Issues




















































- Slides: 55

HSC 4652 HEALTHCARE ETHICS Chapter 12 - Patient Issues & Physician-Patient Relationship Physician Ethics Survey

THINK ABOUT A RECENT PERSONAL HEALTHCARE EXPERIENCE. 1. How were you treated as a patient? 2. What ethical principles were honored? 3. What ethical principles were violated? 4. What did you notice, as a result of this class, about your experience?

PATERNALISM - A “parental” form of medical practice - The doctor always knows “best” - Seen heavily after WWI, when the medical profession became very powerful - Strengthened by a physician’s obligations - nonmaleficience (moral duty to avoid harm) - beneficience (create benefit) - Conflicts with patient autonomy

THE RISE OF CONSUMERISM - Integrated Medicine (IM) - Patient Centered; Emphasizes prevention, holistic healing and partnerships - Rise in use of technology - Internet usage and access to computer-based information - Increased number of insured patients - Payers begin determining treatment

PHYSICIAN-PATIENT MODELS 1. Paternal- physician has moral authority and decision making capacity 2. Partnership- patient and physician collaborate in the shared value of health; mutual participation 3. Friendship- patient and physician share a partnership with an added emotional component; patient puts trust/confidence in physician while physician responds with love/care and assumes patient’s interests 4. Rational Contractor- patient and physician related only through a series on contracts (goods and services exchange)

THE PATIENT EXPERIENCE - What makes you a patient? - Self-treatment vs. Entering the system - The Sick Role - Benefits and responsibilities - Patients enter the healthcare system with a diagnosis - System’s function is to label and treat your disease and get appropriate outcome - Personal system vs. closed system

MEASURING THE EXPERIENCE - Measurement and analysis of patient satisfaction - Surveys, questionnaires - Observation - Administrator rounds; mock patient experience; talk to patients in multiple departments; talk to staff (housekeeping) - Use measurement to determine ethical principle practice - Autonomy, beneficence, nonmaleficence, justice - Measurement is not management!

PATIENT-CENTERED CARE PLANETREE MODEL (HOLISTIC APPROACH) - Human interaction- centers on kindness, trust and concern for patient - Emphasis on information- open access to patient chart - Healing Partnership- family/loved ones included in healing process; unrestricted visitation - Food and nutrition- diet is tied to health outcomes; personalized menus - Power of the Spirit- prayer and spirituality emphasized; chaplains and counselors available; “patients are more than just bodies” - Integrative medicine- massage, aromatherapy, acupuncture - Healing arts- Beauty, from multiple sources, deemed necessary for healing; paintings and sculptures available from “art carts” - Environment- Less sterile; careful design choices; noise controls; natural light

ELMHURST MEMORIAL HOSPITAL

FOR EXECUTIVES…. Increasing Patient-centered care: - Increase your own empathy - It’s not just Finance and Forms; you exist for the patient - Communication - Educate personnel - Administrative Rounds - Visit patient rooms and address comfort, privacy, communication, treatment - Put your mission into action - More than words

SHARE A RECENT PERSONAL HEALTHCARE EXPERIENCE. 1. How were you treated as a patient? 2. What ethical principles were violated? 3. What ethical principles were honored? 4. What did you notice, as a result of this class, about your experience?


WOULD YOU EVER RECOMMEND OR GIVE LIFESUSTAINING THERAPY WHEN YOU JUDGED THAT IT WAS FUTILE?


WOULD YOU EVER CONSIDER HALTING LIFESUSTAINING THERAPY BECAUSE OF FAMILY DEMANDS, EVEN IF YOU FELT THAT IT WAS PREMATURE?


WOULD YOU EVER PRESCRIBE A TREATMENT THAT WAS A PLACEBO, SIMPLY BECAUSE THE PATIENT WANTED TREATMENT?


WOULD YOU EVER UNDERTREAT A PATIENT’S PAIN BECAUSE YOU WERE CONCERNED ABOUT REPERCUSSIONS OR BECAUSE YOU BELIEVE THAT A PATIENT – EVEN A TERMINAL PATIENT – MIGHT BECOME ADDICTED?


WOULD YOU EVER HIDE INFORMATION FROM A PATIENT ABOUT A TERMINAL OR PRE-TERMINAL DIAGNOSIS IN AN EFFORT TO BOLSTER THEIR SPIRIT OR ATTITUDE?


ARE THERE TIMES WHEN IT’S ACCEPTABLE TO COVER UP OR AVOID REVEALING A MISTAKE IF THAT MISTAKE WOULD NOT CAUSE HARM TO THE PATIENT?


ARE THERE TIMES WHEN IT’S ACCEPTABLE TO COVER UP OR AVOID REVEALING A MISTAKE IF THAT MISTAKE WOULD POTENTIALLY OR LIKELY HARM THE PATIENT?


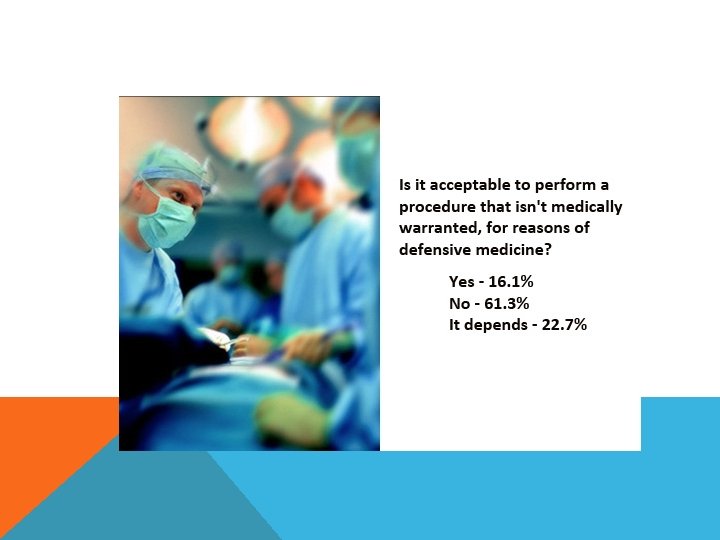
IS IT ACCEPTABLE TO PERFORM A PROCEDURE THAT ISN’T MEDICALLY WARRANTED, FOR REASONS OF DEFENSIVE MEDICINE?


SHOULD PHYSICIAN-ASSISTED SUICIDE BE ALLOWED IN SOME SITUATIONS?


IF A PHYSICIAN FRIEND OR COLLEAGUE WERE IMPAIRED (ALCOHOL, DRUGS, OR ILLNESS) OR WAS NO LONGER COMPETENT, AND HE OR SHE IGNORED YOUR WARNINGS TO GET HELP, WOULD YOU REPORT THAT PERSON TO A SUPERIOR OR TO THE STATE MEDICAL BOARD?


WOULD YOU REFER A PATIENT TO A PHYSICIAN SIMPLY TO RETURN A FAVOR TO THE DOCTOR, WHEN YOU DIDN’T THINK THAT PERSON WAS THE BEST QUALIFIED?


WOULD YOU FEEL CONFLICTED ABOUT DROPPING INSURERS THAT DON’T PAY WELL, EVEN THOUGH SOME LONGTIME PATIENTS WOULD PROBABLY STOP SEEING YOU?


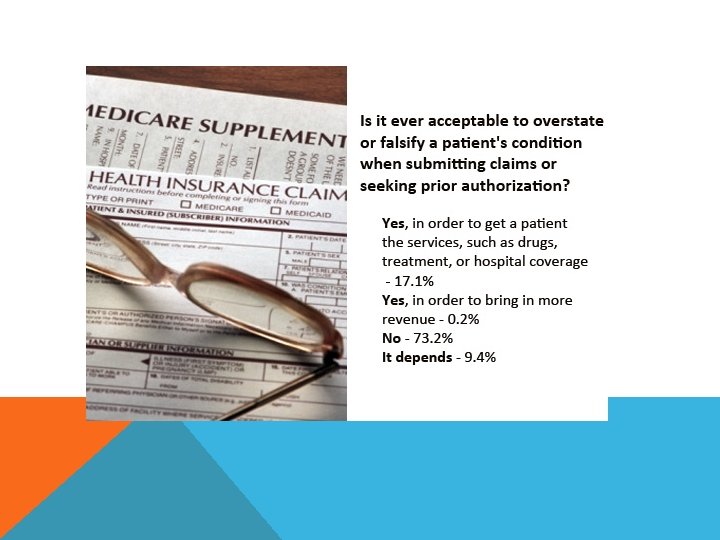
IS IT EVER ACCEPTABLE TO OVERSTATE OR FALSIFY A PATIENT’S CONDITION WHEN SUBMITTING CLAIMS OR SEEKING PRIOR AUTHORIZATION?


WOULD YOU EVER “FIRE” A “NON-COMPLIANT” PATIENT SO THAT YOU COULD IMPROVE YOUR PAYFOR-PERFORMANCE SCORES OR TO STOP DEALING WITH PATIENTS WHO “OVERUSE” RESOURCES ON THEIR CAPITATION PLANS?


WOULD YOU EVER DISCUSS PATIENT INFORMATION IN SITUATIONS THAT DID NOT FULLY PROTECT THEIR PRIVACY (E. G. , SOCIALLY OR WHILE TALKING ABOUT SUBJECTS NOT RELATED TO THE PATIENT)?


IS IT EVER ACCEPTABLE TO BREAK PATIENT CONFIDENTIALITY IF YOU KNOW THE PATIENT’S HEALTH STATUS MAY BE HARMING OTHERS?


WOULD YOU AGREE THAT YOU SHOULD REFUSE GIFTS OR PERKS FROM PHARMACEUTICAL COMPANIES BECAUSE THEY MAY INFLUENCE YOUR MEDICAL JUDGMENT?


COULD YOU BECOME INVOLVED IN A ROMANTIC OR SEXUAL RELATIONSHIP WITH A PATIENT?


SHOULD IT BE LEGAL FOR PEOPLE TO BUY ORGANS FOR TRANSPLANT, IF THEY WOULD NOT BE ABLE TO RECEIVE AN ORGAN BY WAITING THEIR TURN THROUGH THE NATIONAL DATABASE?


WOULD YOU PERFORM AN ABORTION IN CERTAIN SITUATIONS, EVEN IF IT WERE AGAINST YOUR OWN BELIEFS?


WHAT DO YOU THINK IS A PHYSICIAN’S BIGGEST ETHICAL DILEMMA?

