HPV TRANSMISSION DISINFECTION OVERVIEW Introduction to HPV related















- Slides: 21

HPV: TRANSMISSION & DISINFECTION

OVERVIEW Introduction to HPV & related diseases Transmission Tristel & HPV Recent advances in testing with HPV

& ME WHAT IS HPV? • Human papillomavirus • Small non-enveloped DNA virus • Physically stable and resistant with long durability • Most sexually transmitted disease worldwide • Over 200 different types identified • HPV classified into high-risk and low-risk types

& ME DISEASES & PREVALENCE HPV is associated with skin infections: • These result in non-cancerous skin growths (warts). • Infections in genital area are associated with genital or anal warts. • Mouth papillomas (benign epithelial tumours). Chronic infections of the cervix with HPV 16 and 18 causes cervical intraepithelial neoplasia (CIN) and leads to cancer. HPV is found in about 99% of cervical cancers. • More than 70% of these are caused by HPV types 16 and 18. HPV is also responsible for other anogenital cancers and oropharyngeal (throat) cancers. HPV type 16 is responsible for up to 60% of all HPV-associated cancers.

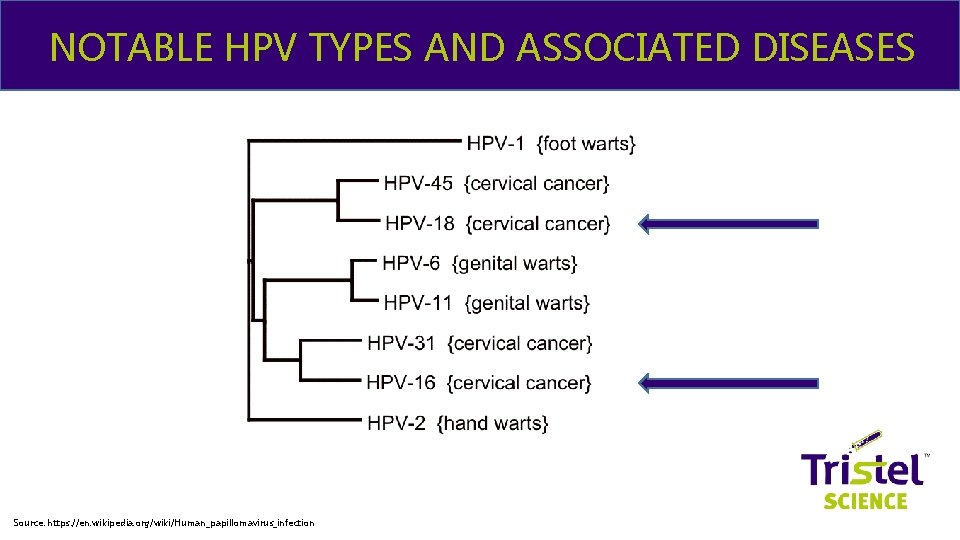
NOTABLE HPV TYPES AND ASSOCIATED DISEASES & ME Source: https: //en. wikipedia. org/wiki/Human_papillomavirus_infection

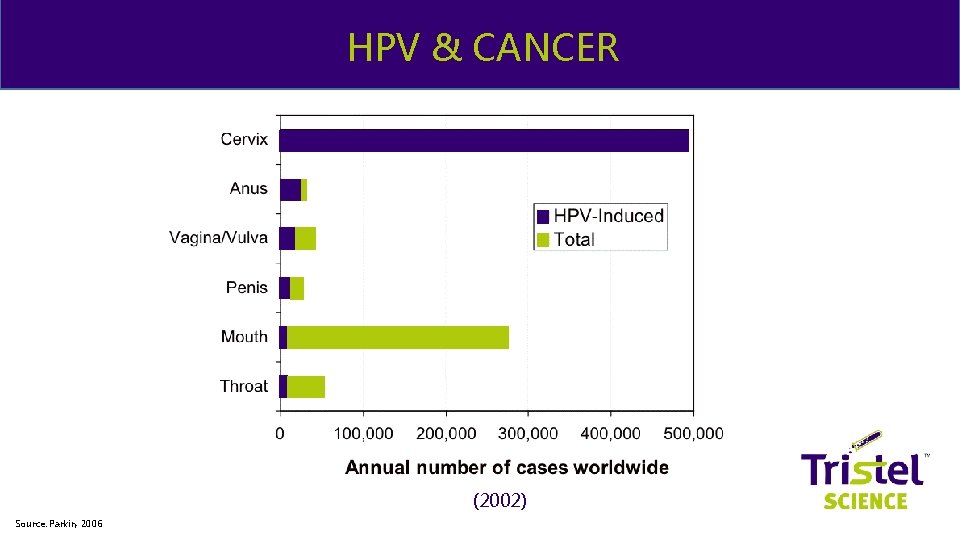
& ME HPV & CANCER (2002) Source: Parkin, 2006

& ME ROUTES OF TRANSMISSION HPV is spread predominantly through sexual intercourse. Other routes of transmission include: Vertical transmission: • From parent to offspring. • From mother to embryo, foetus or baby during pregnancy or childbirth. • At fertilisation via infected oocyte or spermatozoon. Horizontal transmission: • Via fomites. • Through kissing or hand-genital contact. • Through medical procedures such as colposcopy and transvaginal ultrasonography or ENT procedures. This presentation focuses on HPV transmission which can occur in medical facilities (nosocomial).

& ME RISKS OF TRANSMISSION Nosocomial transmission via: • Medical devices which enter cavities such as transvaginal or transrectal probes or laryngoscopes. • Medical surfaces - HPV retains 30% of its infectivity even after dehydration for 7 days. Transvaginal probes are routinely protected by a condom, which acts as a physical barrier to contamination. Studies have shown that 0. 9% - 5% of the condoms get punctured during procedures. It has been shown that low-level disinfection does not remove all HPV DNA from infected probes. HPV DNA has also been found present on sterilised medical instruments used in patients with HPV genital tract infection.

& ME HPV & TRISTEL PRODUCTS DISINFECTION HAS NOT BEEN WORKING • 2012 study found that 7. 5% of transvaginal sonography probes (TVS) were HPV + in A&E. • 2011 study found of 198 samples, 7 (3. 5%) were HPV + in gynaecology department after endovaginal ultrasound procedure. • Same study also found that HPV was found in 6 out of 216 (2. 8%) samples before procedure. • Using a similar technique another 2012 study found 7. 5% of the samples were HPV positive. • 2014 study found HPV negative mothers had infants with HPV.

& ME HPV & TRISTEL PRODUCTS Study showed that HPV was identified on objects (fomites) commonly used in gynaecological care. Source: Human papillomavirus (HPV) contamination of gynaecological equipment, Switzerland, 2015

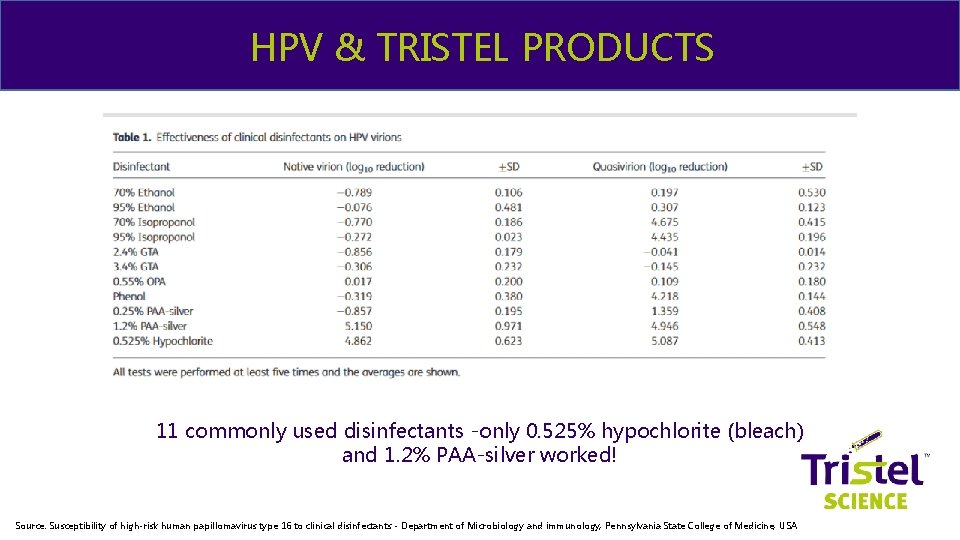
& ME HPV & TRISTEL PRODUCTS 11 commonly used disinfectants -only 0. 525% hypochlorite (bleach) and 1. 2% PAA-silver worked! Source: Susceptibility of high-risk human papillomavirus type 16 to clinical disinfectants - Department of Microbiology and immunology, Pennsylvania State College of Medicine, USA

& ME HPV & TRISTEL PRODUCTS WHY USE TRISTEL? • Commonly used clinical disinfectants, including those used as sterilants in medical and dental healthcare facilities have not been working. • This has been noticed by various health authorities and policy changes concerning disinfectant use has meant that the need for high-level disinfection has become more pronounced. • Tristel offers the level of disinfection needed to get the job done!

& ME HPV & TRISTEL PRODUCTS TRISTEL PRODUCT QUALITIES • Chemistry is safe to patient, staff and environment • Unblemished Health and Safety record of over 20 years • Effective against a wide range of microorganisms due to oxidation properties • Microorganisms are unable to build resistance against chlorine dioxide • Decontamination process is fast by industry standards (within minutes) • Excellent material compatibility • Compliance with local and international regulation • Simple, portable and affordable

& ME HPV & TRISTEL PRODUCTS Tristel Duo ULT Chemistry: Chlorine dioxide (Cl. O 2) Intended use: high-level disinfection of endocavity ultrasound probes, such as: • Transvaginal ultrasound probes • Transrectal ultrasound probes Other uses include high-level disinfection of non-invasive medical devices, such as: • Transabdominal probes • Bladder scanners • Blood pressure cuffs

& ME HPV & TRISTEL PRODUCTS Tristel Trio Wipe System Chemistry: Chlorine dioxide (Cl. O 2) Intended use: high-level disinfection of nonlumened invasive and non-invasive medical • devices, such as: Nasendoscopes • Transoesophageal echocardio probes (TOE/TEE) • Laryngoscope blades • Intubation endoscopes • Manometry catheters • Endocavity ultrasound probes • Laryngoscopes • Ophthalmic instruments

Tristel chemistry: Chlorine dioxide • Chlorine dioxide (Cl. O 2) is a powerful oxidant and eliminates microorganisms through oxidation. • Oxidants are substances which remove electrons from other atoms. • Chlorine dioxide ‘steals’ electrons from microorganisms disrupting the cells. This leads to cell death. • Chlorine dioxide inactivates viruses by inducing oxidative stress. • Cl. O 2 inactivates Poliovirus by reacting with the viral RNA and impairing RNA synthesis. • Cl. O 2 inactivates Influenza virus through specific oxidative modifications of specific amino acids residues on specific proteins.

& ME ADVANCES IN HPV TESTING THE IMPORTANCE OF REMAINING CURRENT • To maintain and potentially expand it’s share of the market Tristel must keep pace. • This includes testing new diseases or updating products with changes in regulatory testing method/standard. • It is better to survey, anticipate and prepare for changes than tackle them as they arrive. • Changes are anticipated for HPV…

& ME ADVANCES IN HPV TESTING LATEST DEVELOPMENTS • The ability of HPV to infect host can now be measured. • Two systems have been developed capable of producing high quantities of HPV virus.

& ME ADVANCES IN HPV TESTING • Testing has been performed with Duo ULT and Trio Wipes System against native HPV 16 and 18. • This testing has demonstrated that both of these disinfectants are effective. • Duo ULT and Trio Wipes System are based on chlorine dioxide chemistry which inactivate viruses by reacting with the viral RNA and impairing RNA synthesis. • We are moving forward to also include simulated use testing on devices to simulate real-life testing.

REFERENCES • Alvarez and O’Brien (1982) Mechanisms of inactivation of poliovirus by chlorine dioxide and iodine. Appl Environ Microbiol, 44(5): 1064 -71. • Casalegno et al. (2012) High risk HPV contamination of endocavity vaginal ultrasound probes: an underestimated route of nosocomioal infection? PLo. S One, 7(10): e 48137. • Ferenczy et al. (1989) HPV DNA in Fomites on Objects Used for the Management of Patients With Genital HPV Infections. Obstet Gynecol. 74(6): 950 -4. • Gallay et al. (2016) Human papillomavirus (HPV) contamination of gynaecological equipment. Sex Transm Infect. 92: 19 -23. • Khan et al. , (2005) High level disinfe. The elevated 10 -year risk of cervical precancer and cancer in women with human papillomavirus (HPV) type 16 or 18 and the possible utility of type-specific HPV testing in clinical practice. J Natl Cancer Inst. 97(14): 1072 -9. • Ma et al. (2012) Transvaginal ultrasound probe contamination by the human papillomavirus in the emergency department. Emerg Med J. 30(6): 472 -5. • Ma et al. (2012) High level disinfection reduces HPV contamination of transvaginal sonography probes in the emergency department. Published as a response to “ Transvaginal ultrasound probe contamination by the human papillomavirus in the emergency department. (Ma et al. , 2012)” • Meyers et al. (2014) Susceptibility of high-risk HPV type 16 to clinical disinfectants. J Antimicrob Chemother. 69(6): 1546 -50. • Miura and Shibata (2010) Antiviral Effect of Chlorine Dioxide against Influenza Virus and Its Application for Infection Control. The Open Antimicrobial Agents Journal. 2: 71 -8. • National Cervical Cancer Coalition. Cervical Cancer Overview. Available at: http: //www. nccc-online. org/hpvcervical-cancer/cervical-cancer-overview/. Accessed: 05/04/2018. • Tota et al. (2011) Epidemiology and burden of HPV infection and related diseases: implications for prevention strategies. Prev Med. 53 Suppl 1: S 12 -21. • Parkin (2006) The global health burden of infection-associated cancers in the year 2002. Int J Cancer. 118(12): 3030 -44. • Ryndock and Meyers (2014) A risk for non-sexual transmission of human papillomavirus? Expert Rev Anti Infect Ther. 12(10): 1165 -70. • Sabeena et al. (2017) Possible non-sexual modes of transmission of human papilloma virus. J Obstet Gynaecol Res. 43(3): 429 -35. • Syrjanen (2005) Human papillomavirus (HPV) in head and neck cancer. J Clin Virol. 32 Suppl 1: S 59 -66.
