HPN COMPLICATIONS Metabolic liver abnormalities Gallbladder sludge stones

HPN COMPLICATIONS Metabolic • liver abnormalities • Gallbladder sludge & stones • metabolic bone disease • trace element and /or vitamins deficiencies • manganese toxicity • renal function impairment B Messing. Approved centre for Intestinal failure. Paris 1 title, 6 sub titles, 25 materials + 4 additional

HPN-long term Complications • Renal function impairment * in SBS : avoid hyperoxaluria and oxalate-Ca renal stone Up to 25% of patients if steatorrhea and colon. Prevention : oral Ca and food with low oxalate content

Serious Renal Impairment Is Associated With Long-Term Parenteral Nutrition - 33 (13 M, 20 �W) adult 51 (21 -79) yr old - on Long-term HPN : 8. 3± 4. 4 yrs - Protein load : 1. 28± 0. 32 g. Kg. d - Nephrotoxic drug : 3. 4± 4. 0% of all HPN days - Bacteriemia/fungemia : 2. 3 (0. 5± 0. 5 / yr) episode - Cr clearance (Cr. Cl) decline was 3. 5± 6. 3% per year - age + 3 above factors : 50% change in Cr. Cl - age + infection factor : idem - excessive urinary phosphate excretion (? aciduria) - but no association with amino acid content of TPN - this decline in renal function is largely unexplained From L. -A. Buchman; A. Moukarzel, M. -E. Ament et al. JPEN 1993; 17: 438 -444
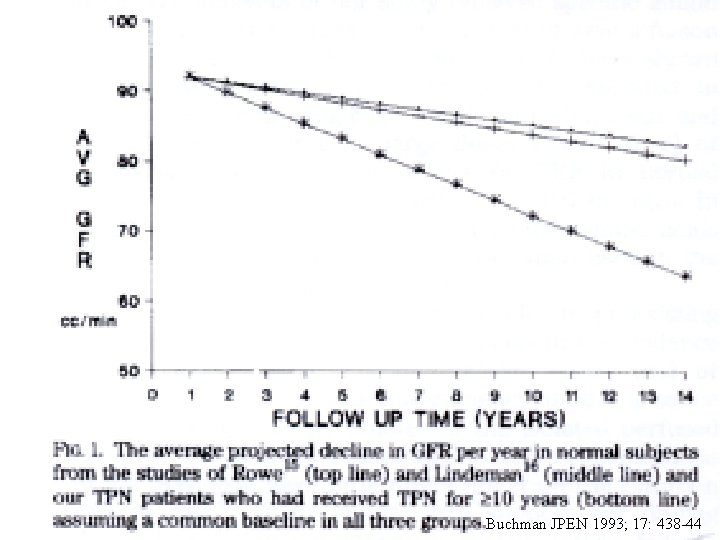
Buchman JPEN 1993; 17: 438 -44

HPN - Complications • deficiencies of trace elements • manganese toxicity • deficiencies of vitamins
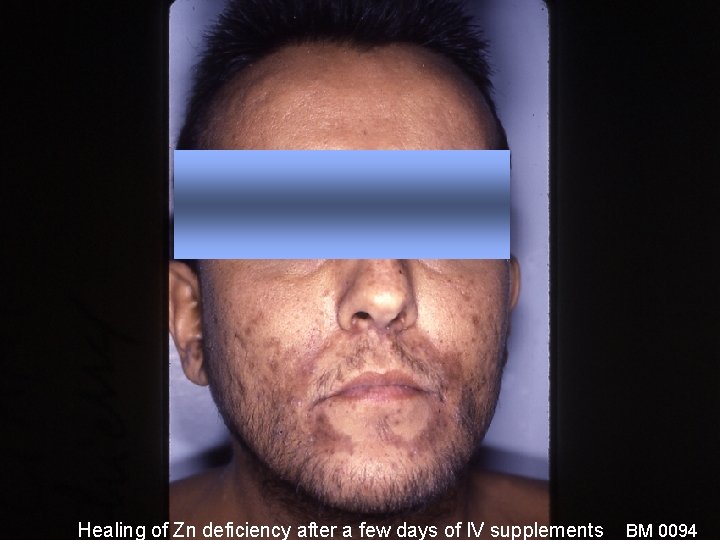
Healing of Zn deficiency after a few days of IV supplements BM 0094
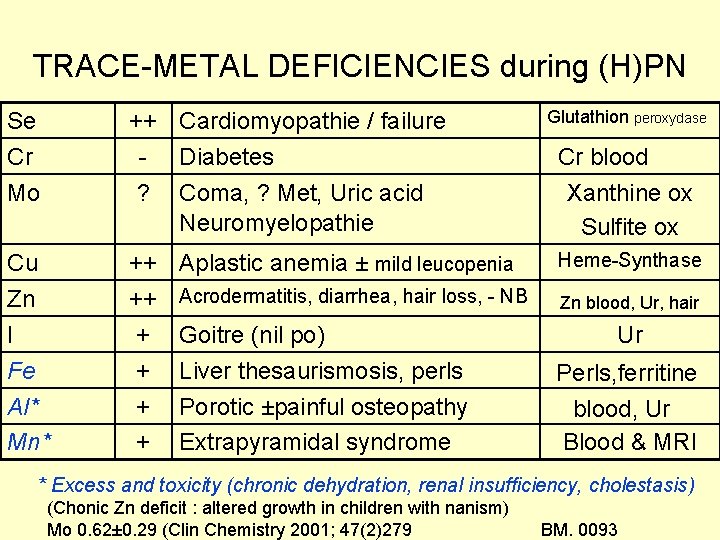
TRACE-METAL DEFICIENCIES during (H)PN Se Cr Mo ++ Cardiomyopathie / failure - Diabetes ? Coma, ? Met, Uric acid Neuromyelopathie Cu Zn I Fe Al* Mn* ++ ++ + + Glutathion peroxydase Cr blood Xanthine ox Sulfite ox Aplastic anemia ± mild leucopenia Heme-Synthase Acrodermatitis, diarrhea, hair loss, - NB Zn blood, Ur, hair Goitre (nil po) Ur Liver thesaurismosis, perls Perls, ferritine Porotic ±painful osteopathy blood, Ur Extrapyramidal syndrome Blood & MRI * Excess and toxicity (chronic dehydration, renal insufficiency, cholestasis) (Chonic Zn deficit : altered growth in children with nanism) Mo 0. 62± 0. 29 (Clin Chemistry 2001; 47(2)279 BM. 0093
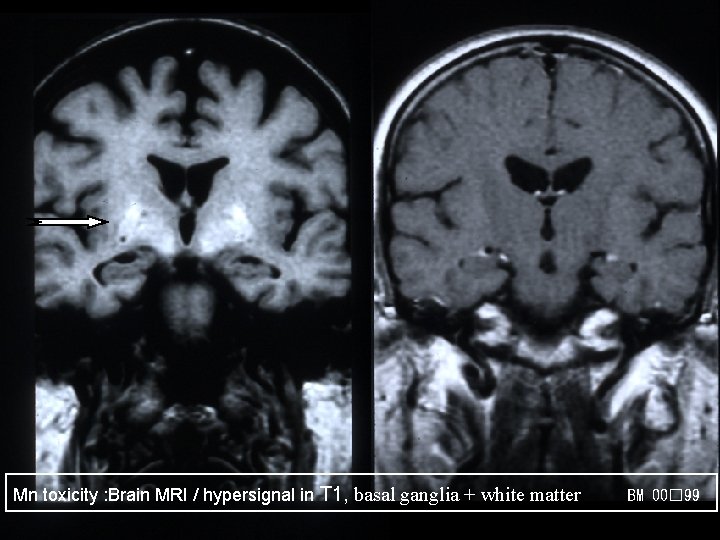
Mn toxicity : Brain MRI / hypersignal in T 1, basal ganglia + white matter BM 00� 99
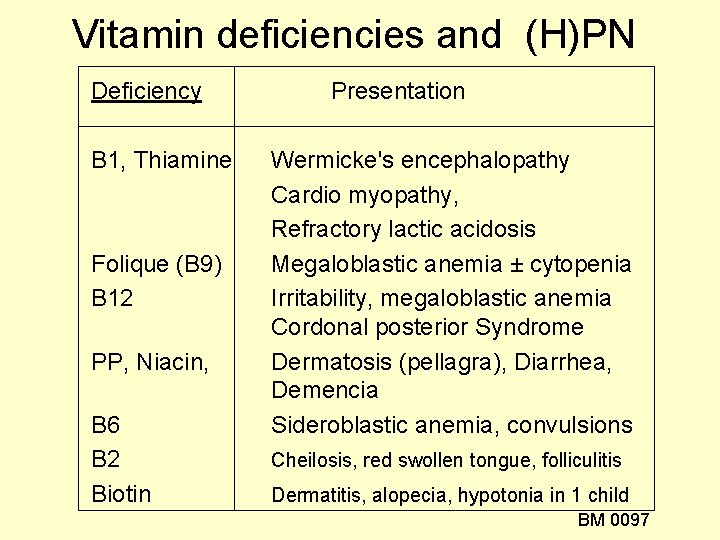
Vitamin deficiencies and (H)PN Deficiency B 1, Thiamine Folique (B 9) B 12 PP, Niacin, B 6 B 2 Biotin Presentation Wermicke's encephalopathy Cardio myopathy, Refractory lactic acidosis Megaloblastic anemia ± cytopenia Irritability, megaloblastic anemia Cordonal posterior Syndrome Dermatosis (pellagra), Diarrhea, Demencia Sideroblastic anemia, convulsions Cheilosis, red swollen tongue, folliculitis Dermatitis, alopecia, hypotonia in 1 child BM 0097
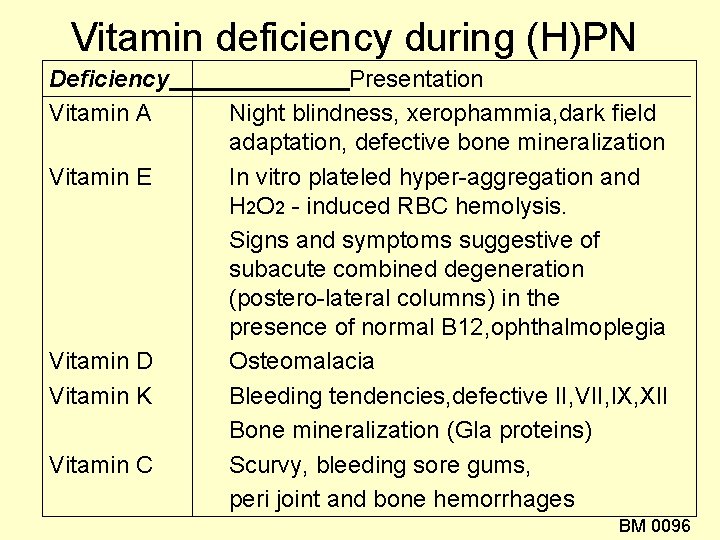

Vitamin deficiency during (H)PN Deficiency Vitamin A Vitamin E Vitamin D Vitamin K Vitamin C Presentation Night blindness, xerophammia, dark field adaptation, defective bone mineralization In vitro plateled hyper-aggregation and H 2 O 2 - induced RBC hemolysis. Signs and symptoms suggestive of subacute combined degeneration (postero-lateral columns) in the presence of normal B 12, ophthalmoplegia Osteomalacia Bleeding tendencies, defective II, VII, IX, XII Bone mineralization (Gla proteins) Scurvy, bleeding sore gums, peri joint and bone hemorrhages BM 0096
HPN-LD Complications • Multifactorial metabolic bone disease
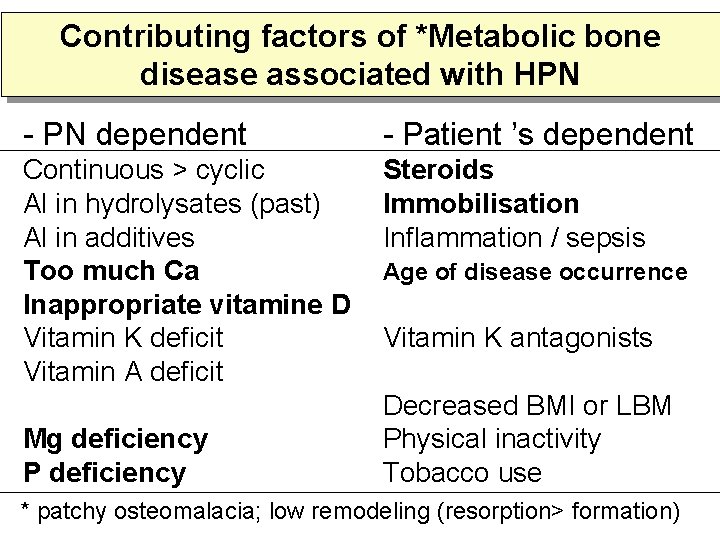

Contributing factors of *Metabolic bone disease associated with HPN - PN dependent - Patient ’s dependent Continuous > cyclic Al in hydrolysates (past) Al in additives Too much Ca Inappropriate vitamine D Vitamin K deficit Vitamin A deficit Steroids Immobilisation Inflammation / sepsis Mg deficiency P deficiency Age of disease occurrence Vitamin K antagonists Decreased BMI or LBM Physical inactivity Tobacco use * patchy osteomalacia; low remodeling (resorption> formation)
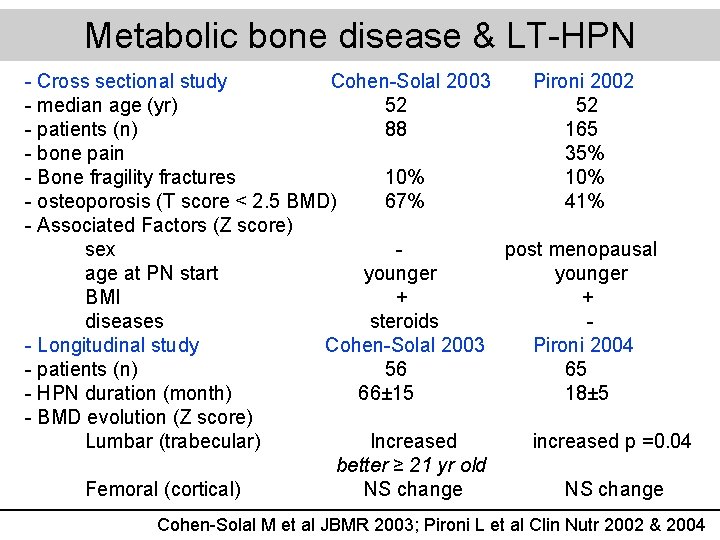
Metabolic bone disease & LT-HPN - Cross sectional study Cohen-Solal 2003 - median age (yr) 52 - patients (n) 88 - bone pain - Bone fragility fractures 10% - osteoporosis (T score < 2. 5 BMD) 67% - Associated Factors (Z score) sex - age at PN start younger BMI + diseases steroids - Longitudinal study Cohen-Solal 2003 - patients (n) 56 - HPN duration (month) 66± 15 - BMD evolution (Z score) Lumbar (trabecular) Increased better ≥ 21 yr old Femoral (cortical) NS change Pironi 2002 52 165 35% 10% 41% post menopausal younger + Pironi 2004 65 18± 5 increased p =0. 04 NS change Cohen-Solal M et al JBMR 2003; Pironi L et al Clin Nutr 2002 & 2004
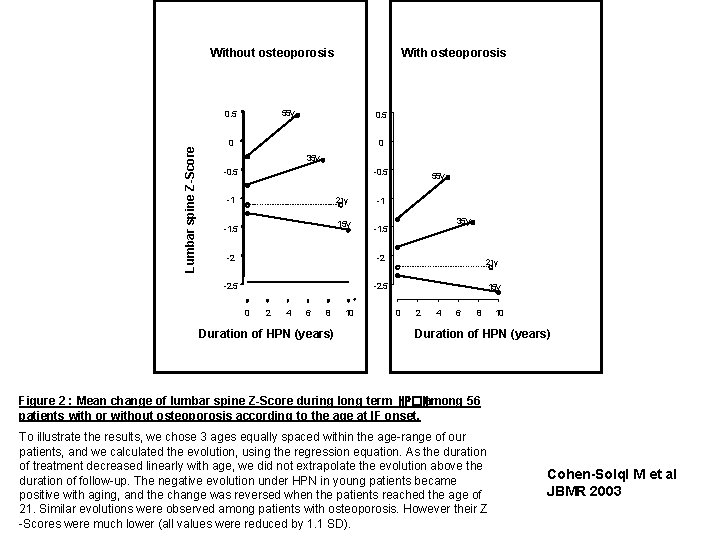
Without osteoporosis 55 y 0. 5 Lumbar spine Z-Score With osteoporosis 0. 5 0 0 35 y -0. 5 -1 21 y 15 y -1. 5 -1 -2 -2. 5 2 4 6 8 Duration of HPN (years) 10 35 y -1. 5 -2 0 55 y 21 y 15 y 0 2 4 6 8 10 Duration of HPN (years) Figure 2 : Mean change of lumbar spine Z-Score during long term HP�Namong 56 patients with or without osteoporosis according to the age at IF onset. To illustrate the results, we chose 3 ages equally spaced within the age-range of our patients, and we calculated the evolution, using the regression equation. As the duration of treatment decreased linearly with age, we did not extrapolate the evolution above the duration of follow-up. The negative evolution under HPN in young patients became positive with aging, and the change was reversed when the patients reached the age of 21. Similar evolutions were observed among patients with osteoporosis. However their Z -Scores were much lower (all values were reduced by 1. 1 SD). Cohen-Solql M et al JBMR 2003
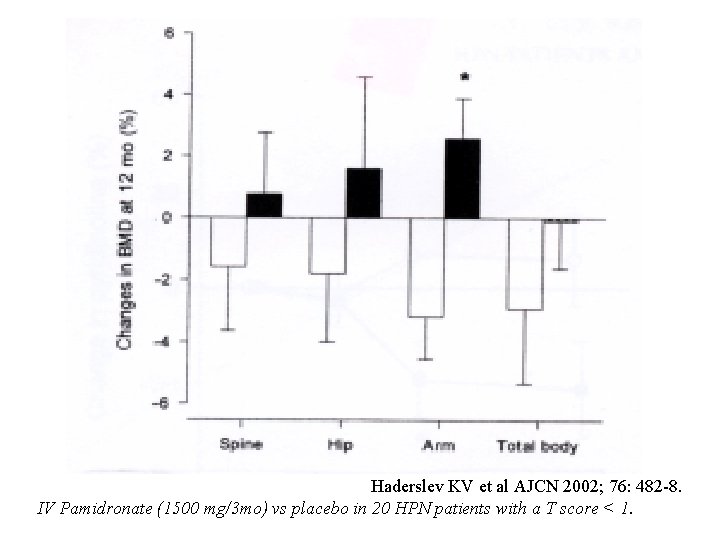
Haderslev KV et al AJCN 2002; 76: 482 -8. IV Pamidronate (1500 mg/3 mo) vs placebo in 20 HPN patients with a T score < 1.

Metabolic bone disease & LT-HPN • Osteomalacia : - Check vit D metabolites & Ca, P and Mg balances • Low remodeling bone : - ibid & reinforces Ca, Mg, Vit D metabolites orally - Avoid too much N & Ca IV (calciuria & lower PTH) - Check Al in Blood & in All-in-One (& in renal risk patients ++) - Check DEXA & BMD at PN start & annually - Check bone markers : osteocalcin & cross laps / deoxypyridinoline • Specific treatments of osteoporosis : - Biphoshonates ° : positive moderate results at lumbar site, be careful with Ca & vit D status before treatment to avoid deficits - Near future : trophic factors (GLP 2*) or r. H-PTH** * Haderslev KV Scand J Gastroenterol 2002; ° Haderslev KV et al Am J Clin Nutr 2002, D ’aoust L et al Clin Nutr 2002 (A) ** Khosla S. N Eng J Med. 2003 (editorial)
- Slides: 16