HPH Task Force Migration Equity Diversity Ensuring Equity


















- Slides: 24

HPH Task Force Migration, Equity & Diversity Ensuring Equity in Health Care Organisations: The Contribution of the HPH – TF MED Dr Antonio Chiarenza Leader of HPH-TF MED Coordinator of the HPH network of Emilia-Romagna Simposium Embedding Health Equity in Policy, Practice and Participation October, 11 -12 2017, Montreal

Outline of the presentation § What is the TF MED: where does it come from and where is it going § The changing context for responsiveness to diversity § The impact of the refugee crisis on EU health care systems § What defines a health care organisation as being responsive to diversity § Ensuring effective implementation of policy measures through the Equity standards § Future steps for the TF MED

Migrant-Friendly Hospitals (www. mfh-net) a European initiative to promote health and health literacy of migrants and ethnic minorities AT DE DK EL ES FI FR IR IT NL SV UK Kaiser-Franz-Josef-Spital, Vienna, Austria Immanuel-Krankenhaus Gmb. H, Rheumaklinik Berlin-Wannsee, Berlin, Germany Kolding Hospital, Velje-Kolding, Denmark Hospital ”Spiliopoulio Agia Eleni”, Athens, Greece Hospital Punta de Europa, Algeciras-Cádiz, Spain Turku University Hospital, Turku, Finland Hôptial Avicenne, Paris, France James Connolly Memorial Hospital, Dublin, Ireland Azienda Unità sanitaria Locale di Reggio Emilia, Italy Academic Medical Centre, Amsterdam, The Netherlands Uppsala University Hospital, Psychiatric Centre, Uppsala, Sweden Bradford Hospitals NHS Trust, Bradford, U. K. HPH TASK FORCE ON MIGRATION, EQUITY& DIVERSITY (MED) HEALTH PROMOTING HOSPITALS NETWORK OF EMILIA – ROMAGNA AZIENDA USL DI REGGIO EMILIA – DIREZIONE GENERALE 3

The HPH Task Force on Migrant Friendly & Culturally Competent Health Care is established within the WHO-HPH Network in 2005 Aims of the Task Force • To create a framework for continuity after the conclusion of the MFH project • To share and disseminate best policies and practice (e. g. MFH concepts, models and tools) • To foster co-operation and alliances between healthcare organisations • To support health care organisations in becoming MF & CC organisations as indicated in the Amsterdam Declaration HPH TASK FORCE ON MIGRATION, EQUITY& DIVERSITY (MED) HEALTH PROMOTING HOSPITALS NETWORK OF EMILIA – ROMAGNA AZIENDA USL DI REGGIO EMILIA – DIREZIONE GENERALE 4

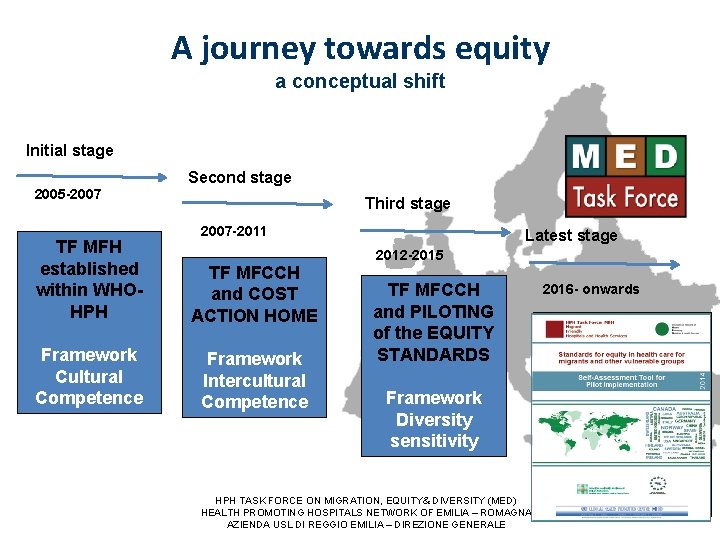
A journey towards equity a conceptual shift Initial stage 2005 -2007 Second stage Third stage 2007 -2011 TF MFH established within WHOHPH TF MFCCH and COST ACTION HOME Framework Cultural Competence Framework Intercultural Competence Latest stage 2012 -2015 TF MFCCH and PILOTING of the EQUITY STANDARDS Framework Diversity sensitivity HPH TASK FORCE ON MIGRATION, EQUITY& DIVERSITY (MED) HEALTH PROMOTING HOSPITALS NETWORK OF EMILIA – ROMAGNA AZIENDA USL DI REGGIO EMILIA – DIREZIONE GENERALE 2016 - onwards TF MED and IMPLEMENTATION of the EQUITY STANDARDS Framework Equity 5

The changing context of diversity responsiveness Two fundamental shifts § Recognition of the limits of “cultural competence” when implemented in practice. § Changes in the dimensions of “diversity” regarded as relevant in health care.

Limitations in the use of cultural competence in practice n Assumption that culture can be reduced to a technical skill. (Kleinman & Benson, 2006) n Existing models of CC interpret culture as if it only had to do with ethnicity and race (Kumas-Tan et al. 2007) n Simplistic representations of culture are by definition stereotypical (Johnson & Munch, 2009). n Focusing on cultural differences has detracted attention from the role of socio-economic factors (Simon and Mosavel, 2008)

Changes in the dimensions of “diversity” regarded as relevant in health care. New migration has brought with it an increased level of diversity that calls for an equity approach to address the multiple factors that contribute to variation in health care experience. n Different origins: increased diversification in countries of origin n Diverse socioeconomic backgrounds: migrant groups are less organised, more legally differentiated, and more socially stratified n Different immigrant status: economic workers, undocumented migrants, asylum seekers, refugees, . . . n Intra-group diversity: diversity within the same national or ethnic group

THE IMPACT OF THE REFUGEE CRISIS ON EUROPEAN HEALTH CARE SYSTEMS (2015 -2016) The refugee crisis in Europe has made it evident that we need to address the issue of multiple diversity and vulnerability in order to respond effectively to migrants’ needs

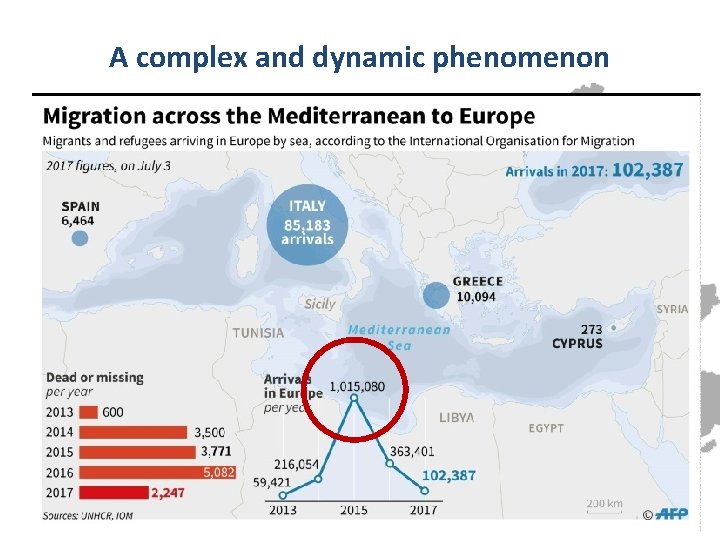
A complex and dynamic phenomenon

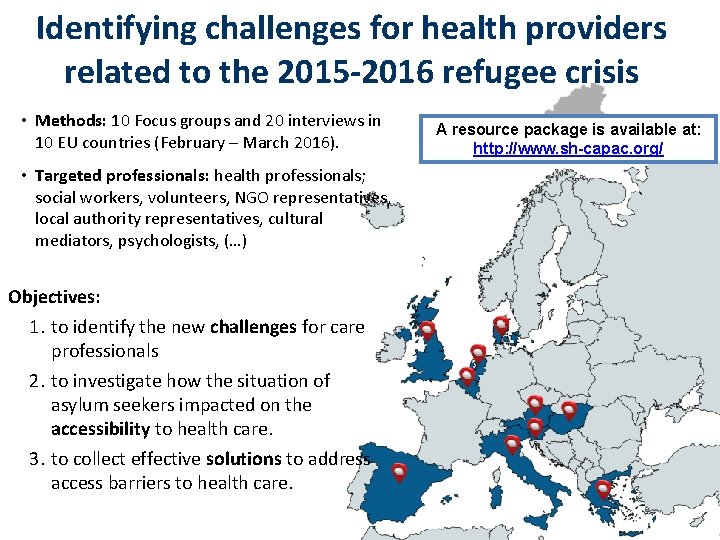
Identifying challenges for health providers related to the 2015 -2016 refugee crisis • Methods: 10 Focus groups and 20 interviews in 10 EU countries (February – March 2016). • Targeted professionals: health professionals; social workers, volunteers, NGO representatives, local authority representatives, cultural mediators, psychologists, (…) Objectives: 1. to identify the new challenges for care professionals 2. to investigate how the situation of asylum seekers impacted on the accessibility to health care. 3. to collect effective solutions to address access barriers to health care. A resource package is available at: http: //www. sh-capac. org/

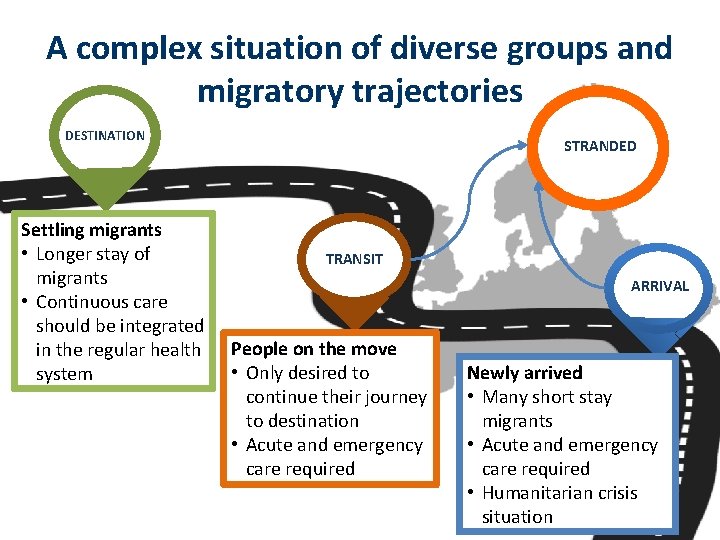
A complex situation of diverse groups and migratory trajectories DESTINATION Settling migrants • Longer stay of migrants • Continuous care should be integrated in the regular health system STRANDED TRANSIT ARRIVAL People on the move • Only desired to continue their journey to destination • Acute and emergency care required Newly arrived • Many short stay migrants • Acute and emergency care required • Humanitarian crisis situation

Different levels of entitlement to access to health services The legal status linked to the migration trajectory stage as well as outcomes of the asylum seeking procedure play an important role in migrants’ access to health care • Newly arrived migrants are in principle “irregular migrants” • Migrants in transit do not claim asylum • Asylum seekers at destination (may be lodging an application, awaiting a decision, awaiting an appeal) • Migrants granted refugee or protected status • Failed asylum seekers (awaiting deportation) • Irregular (undocumented) migrants

Legislative and administrative barriers • Different procedures depending on the status of the asylum seeker (e. g. : sexual and reproductive care; family planning; child care) • Prolonged waiting time before receiving refugee status has an impact on health and mental health • Poor knowledge and different interpretations of legislation Linguistic and cultural barriers • Lack of interpreters has a negative impact on the quality of care • Linguistic barriers make it difficult to handle cultural barriers (e. g. : woman’s health, mental health, child care. . . ) • Concern about confidentiality and ethnic concordance (mental health; care for victims of violence)

Organisational barriers and lack of coordination • Limited availability of services; unequal distribution of facilities; • Specialist care is hard to reach (e. g. : mental health; dental care); complex appointment systems; • Lack of coordination between different care providers (e. g. : care of victims of violence). Lack of information for both providers and migrants • Lack of health records (e. g. : vaccination status of children ); • Absence of exchange of information within and between countries; • Lack of information and knowledge on how to navigate the system.

Lessons learned § Health systems have been affected differently, depending on whether migrants were at the arrival, transit or destination. § Health-care systems have still not adapted to respond adequately to their diverse needs. § Diverse needs should be identified according to the intersection of individual/family characteristics and social position (e. g. : gender-migrant status-economic situation-health situation). § Cultural competence needs to be integrated with alternative concepts such as equity, intersectionality, person-centered care.

WHAT DEFINES A HEALTH CARE ORGANISATION AS BEING RESPONSIVE TO DIVERSITY ?

How should health professionals work effectively with diversity? n They should avoid a “recipe” approach. n They should be able to work across differences n They should learn from the patient, n They should favour a case-by-case assessment of needs and priorities n They should engage in self-reflection and selfcritique 18

How should health organisations work effectively with diversity? n Develop specific policies and programmes that address equity and diversity priorities n Link health data to socio-demographic information n Build staff capacity at all levels to address equity and diversity n Address all barriers which prevent or limit people accessing health care n Provide person and family-centred care n Promote equitable participation of users/community. 19

HOW DO HEALTH CARE ORGANISATIONS ENSURE EFFECTIVE IMPLEMENTATION AND ASSESSMENT OF THESE POLICIES AND MEASURES ?

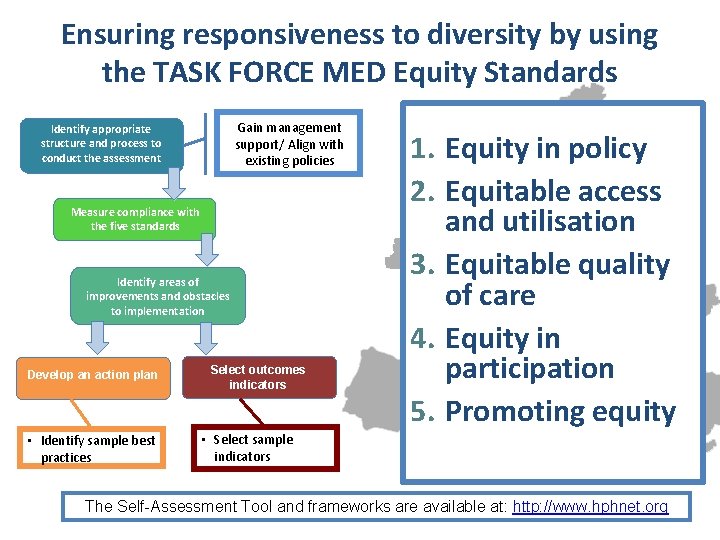
Ensuring responsiveness to diversity by using the TASK FORCE MED Equity Standards Gain management support/ Align with existing policies Identify appropriate structure and process to conduct the assessment Measure compliance with the five standards Identify areas of improvements and obstacles to implementation Develop an action plan • Identify sample best practices Select outcomes indicators 1. Equity in policy 2. Equitable access and utilisation 3. Equitable quality of care 4. Equity in participation 5. Promoting equity • Select sample indicators The Self-Assessment Tool and frameworks are available at: http: //www. hphnet. org

Task Force MED programme (2017 -2019) From pilot to effective implementation of equity in health care WORK PLAN & Working Groups • WG 1: Develop a Rapid Assessment Tool • WG 2: Promote the tool to as wide a range of audiences as possible and expand the network • WG 3: Develop an online self-assessment tool including an evidence gathering system for country reporting • WG 4: Develop a manual for implementation, including standards, outcome indicators and examples of best practice 22

Scientific committee of the TF MED • Bernadette Nirmal Kumar and Ragnhild Spilker, The Norwegian Centre for Migration and Minority Health, NAKMI, Norway • • • David Ingleby, University of Amsterdam, The Netherlands • • • Karima Karmali, The Hospital for Sick Children, Toronto, Canada • • Manuel Fernandez Gonzalez, Uppsala University Hospital, Sweden Eeva Hakkinen, Mikkeli Central Hospital, Finland Laura Mc. Hugh, Galway University Hospital, Ireland James Glover, Community Health, Dublin, Ireland Marie Serdynska, Montreal Children’s Hospital, Mc. Gill University Health Centre, Canada Elizabeth Abraham, Critical Link International, Canada Lidia Horvat, Department of Health and Human Services, Melbourne, Australia Hans Verrept, FPS Health, Food Chain Safety and Environment, Belgium Manuel Garcia-Ramirez, CESPYD, University of Seville, Spain Antonio Chiarenza, Task Force Chair, AUSL of Reggio Emilia, Italy

24