How to manage P aeruginosa infections Francesco Menichetti













- Slides: 20

How to manage P. aeruginosa infections Francesco Menichetti, MD Professor of Infectious Diseases, University of Pisa Director, Infectious Diseases Department, Cisanello Hospital, Pisa President, Italian Group for Antimicrobial Stewardship (GISA)

Clinical Disease in both normal & ICH • • Pulmonary Infections (VAP, HAP) Bloodstream infections (CVC, neutropenia) Burn Wound Infections Other skin and soft tissue infections UTI (catheter) External Otitis (malignant OE, swimmer’s ear) Eye Infections and corneal ulceration via contaminated contact lens cleaning fluids


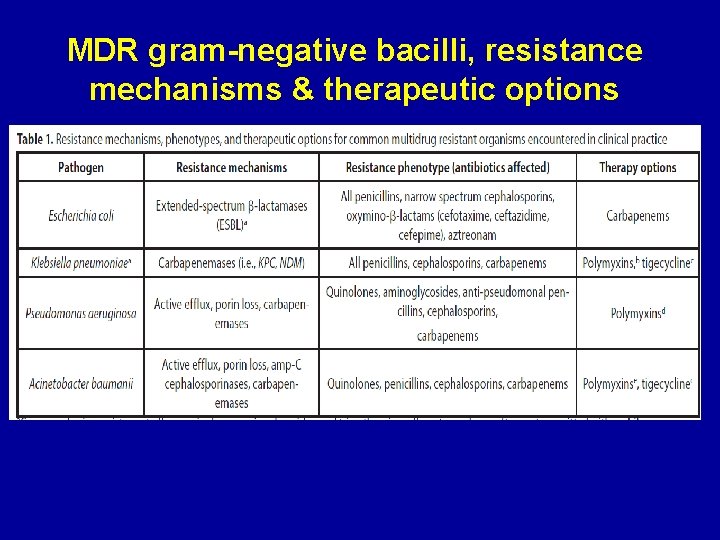
MDR gram-negative bacilli, resistance mechanisms & therapeutic options Pop-Vicas A & Opal SM Virulence 2013

P. aeruginosa: antibacterial resistance mechanisms • • Extended spectrum beta-lactamases Carbapenemases Presence of efflux pumps Decrease in cell wall permeability

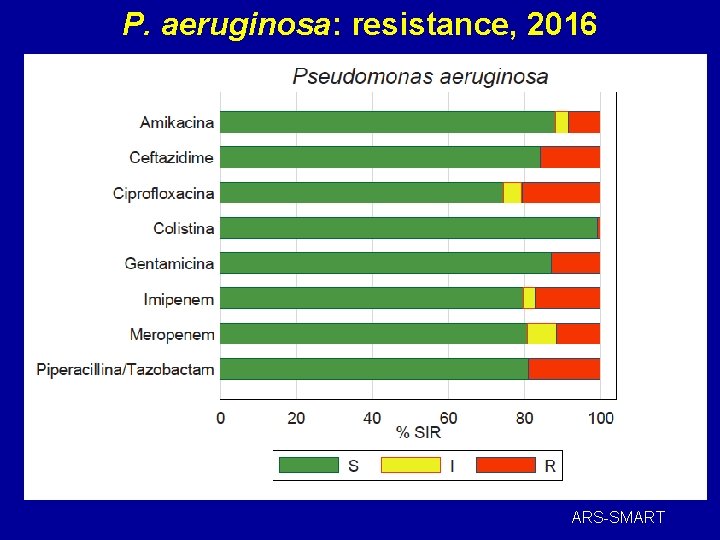
P. aeruginosa: resistance, 2016 ARS-SMART

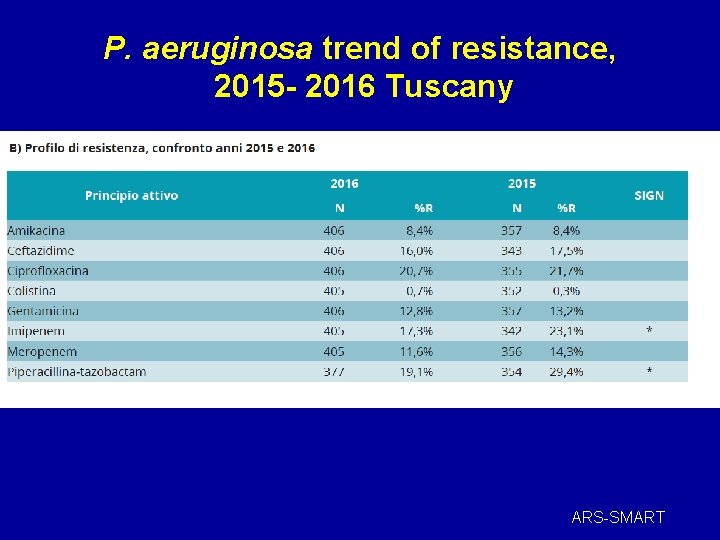
P. aeruginosa trend of resistance, 2015 - 2016 Tuscany ARS-SMART

P. aeruginosa: resistance to carbapenems, 2016 ARS-SMART

P. aeruginosa MDR, 2016 ARS-SMART

P. aeruginosa Primary Targeted Regimens NO IN VITRO RESISTANCE • Piperacillin-tazobactam 4. 5 gm iv q 6 h EI, after a LD • Ceftazidime 2 gm IV q 8 h or • Cefepime 2 gm IV q 8 -12 h • Aztreonam 2 gm IV q 6 h (for Ig. E-mediated betalactam allergy) • Combination therapy may be considered The Sanford Guide 2018


P. aeruginosa Primary Targeted Regimens Amp-C producing strain • Meropenem 1 -2 gm IV q 8 h • Ceftolozane-tazobactam 1. 5 g q 8 h Serine based carbapenemase (KPC) rare • Ceftazidime-avibactam 2. 5 g over 2 hrs q 8 h • Meropenem-vaborbactam 4 gm IV over 3 hrs q 8 h Metallo-carbapenemase production • Ceftazidime-avibactam 2. 5 g over 2 hrs q 8 h plus Aztreonam 2 g IV q 6 hrs (colistin if no response) MBL plus ESBLs & FQ-R, AG-R • as above The Sanford Guide 2018


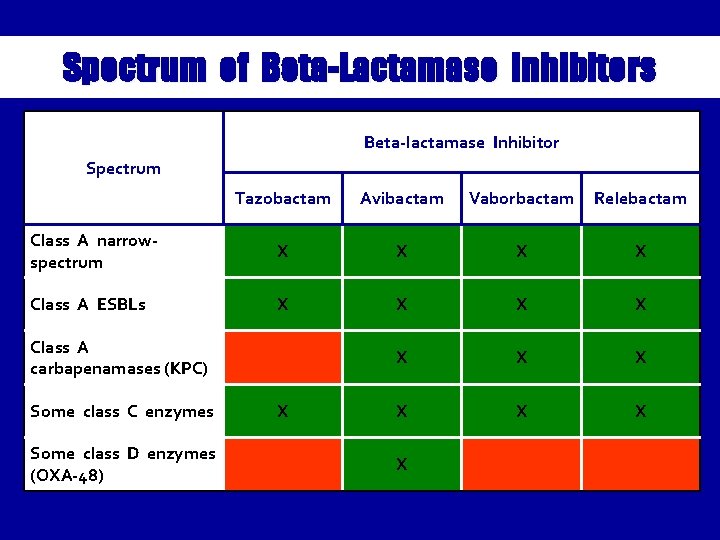
Spectrum of Beta-Lactamase Inhibitors Beta-lactamase Inhibitor Spectrum Tazobactam Avibactam Vaborbactam Relebactam Class A narrowspectrum X X Class A ESBLs X X X X X Class A carbapenamases (KPC) Some class C enzymes Some class D enzymes (OXA-48) X X

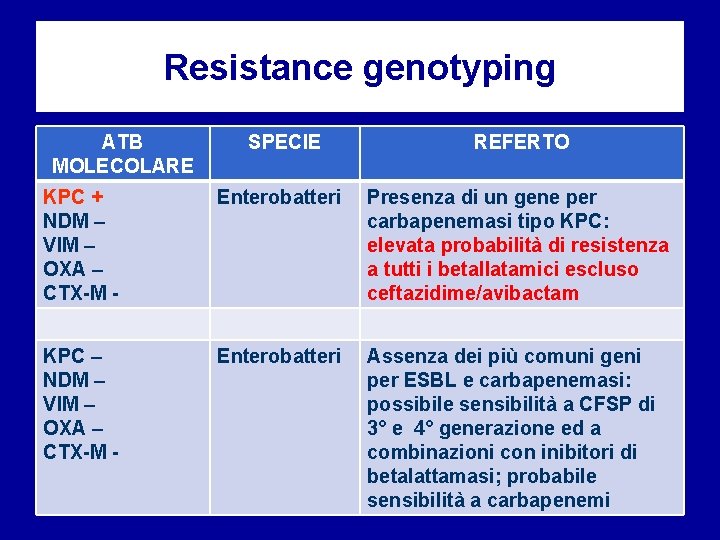
Resistance genotyping ATB MOLECOLARE SPECIE REFERTO KPC + NDM – VIM – OXA – CTX-M - Enterobatteri Presenza di un gene per carbapenemasi tipo KPC: elevata probabilità di resistenza a tutti i betallatamici escluso ceftazidime/avibactam KPC – NDM – VIM – OXA – CTX-M - Enterobatteri Assenza dei più comuni geni per ESBL e carbapenemasi: possibile sensibilità a CFSP di 3° e 4° generazione ed a combinazioni con inibitori di betalattamasi; probabile sensibilità a carbapenemi

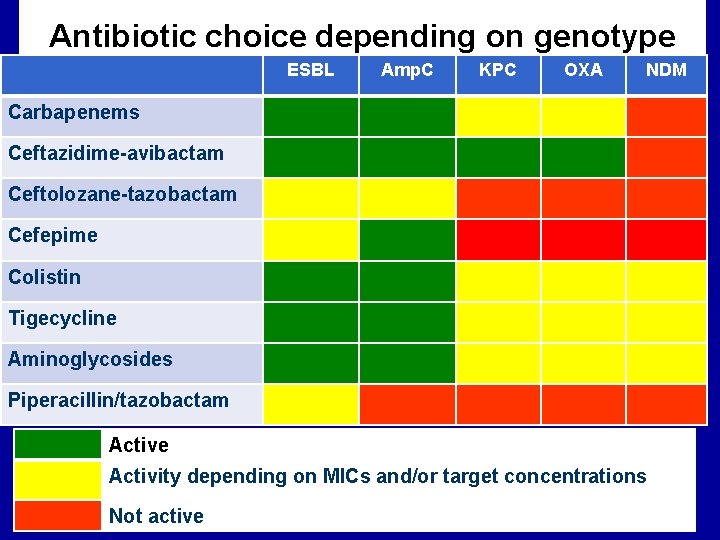
Antibiotic choice depending on genotype ESBL Amp. C KPC OXA NDM Carbapenems Ceftazidime-avibactam Ceftolozane-tazobactam Cefepime Colistin Tigecycline Aminoglycosides Piperacillin/tazobactam Active Activity depending on MICs and/or target concentrations Not active

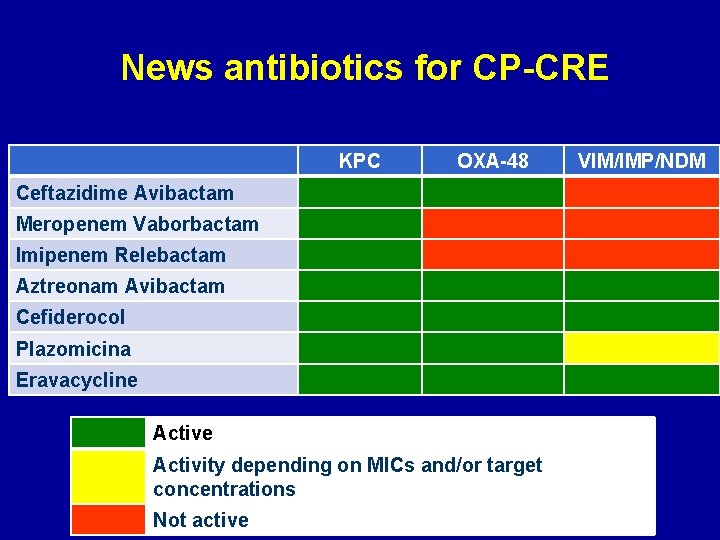
News antibiotics for CP-CRE KPC OXA-48 Ceftazidime Avibactam Meropenem Vaborbactam Imipenem Relebactam Aztreonam Avibactam Cefiderocol Plazomicina Eravacycline Activity depending on MICs and/or target concentrations Not active VIM/IMP/NDM

New approach to MDR gram-neg. infections Infections due to KPC-CP Colistin no more !! Meropenem/v aborbactam Plazomicin Ceftazidime/a vibactam

New approach to MDR gram-neg. infections MBL producers or Acinetobacter spp. cefiderocol Ceftazidime/a vibactam/aztr eonam

Conclusions • • P. aeruginosa: still a challenge in clinical practice Invasive infections in compromised host Difficult-to-treat site of infection New antimicrobials: ceftolozane/tazobactam, ceftazidime/avibactam • Precision medicine: a real chance for modern antimicrobial chemotherapy