How to decrease barriers to physician helpseeking Primary

How to decrease barriers to physician help-seeking Primary Authors: Version 1. 0: Updated June 2020 Sansea Jacobson, MD Julie Chilton, MD Andres Martin, MD

How to use the WELL Toolkit slides These slide decks were created by the WELL Toolkit Workgroup in 2020. You may use these slides individually or as a set for non-commercial purposes. You are welcome to edit this slide deck to customize it to your setting, including the use of your own logo, but please do not substantively change the content of the work. If you present, reproduce, or distribute these slides, please acknowledge our resource, “WELL Toolkit (2020). ” For additional information and related resources, please visit: https: //gmewellness. upmc. com/

Agenda • Barriers to care for physicians • What institutions can do • What physician leaders can do

Learning Objectives 1. Be aware of reasons why physicians may not seek help for themselves when they are struggling 2. Be able to name career implications of receiving mental health care at both state and institutional level 3. Learn how leaders can destigmatize help-seeking, assure confidentiality, improve transparency, and advocate for a work culture that values physician wellbeing

Physicians are not immune to mental illness Depression Estimated prevalence of depression in physicians exceeds rates in the general population: – 12% of male physicians – 19. 5% of female physicians Suicide While suicide remains relatively rare, physicians are at: – 1. 41 x the risk of the general male population – 2. 27 x the risk of the general female population Substance use disorders Physicians have a lifetime prevalence of substance use disorders similar to the general population: – 10% to 12% (Flaherty & Richman, 1993; SAMHSA, 2006; Medscape 2018)
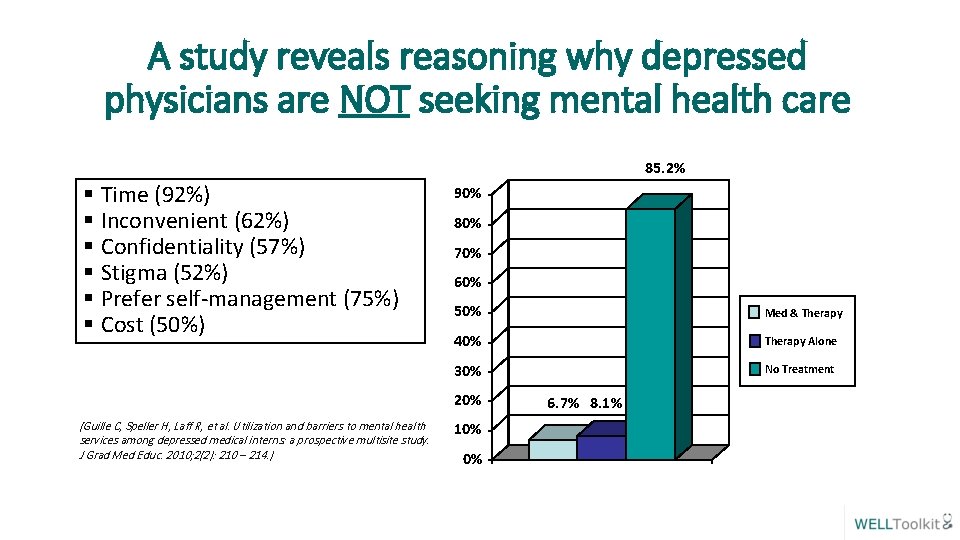
A study reveals reasoning why depressed physicians are NOT seeking mental health care 85. 2% § Time (92%) § Inconvenient (62%) § Confidentiality (57%) § Stigma (52%) § Prefer self-management (75%) § Cost (50%) 90% 80% 70% 60% 50% Med & Therapy 40% Therapy Alone 30% No Treatment 20% (Guille C, Speller H, Laff R, et al. Utilization and barriers to mental health services among depressed medical interns: a prospective multisite study. J Grad Med Educ. 2010; 2(2): 210 – 214. ) 6. 7% 8. 1% 10% 0% 6

Consequences of help-seeking Physicians not only need to know HOW to access help, but they need to know the practical implications for doing so.
Help-Seeking by Physicians often do not engage in help-seeking (i. e. pursuing professional support when they are struggling with personal, professional and/or mental health issues) Institutions can help change the culture of maladaptive perfectionism in medicine by destigmatizing and demystifying the process of help-seeking by physicians

What can institutions do?

What Institutions can do: List/Describe/Assure üLIST the actual mental health questions from the state licensure forms, hospital credentialing, and insurance/malpractice forms üDESCRIBE confidentiality and circumstances when other parties might be involved and for what? (e. g. Physician Assistance Program? Human Resources? Legal? State Physician Health Program? ) üASSURE relevant institutional policies (e. g. sick leave, FMLA, disability) and resources are easily available and up-to-date

Align with the Americans with Disabilities Act Under the ADA, employers are only allowed to ask about CURRENT impairment • NOT whether a condition hypothetically could cause impairment • NOT about specific diagnoses and treatment without impairment Many medical state licensing questions remain in violation of the ADA • Nearly half still ask mental health questions beyond current impairment • One-third of states are ADA-compliant for both initial applications and renewal
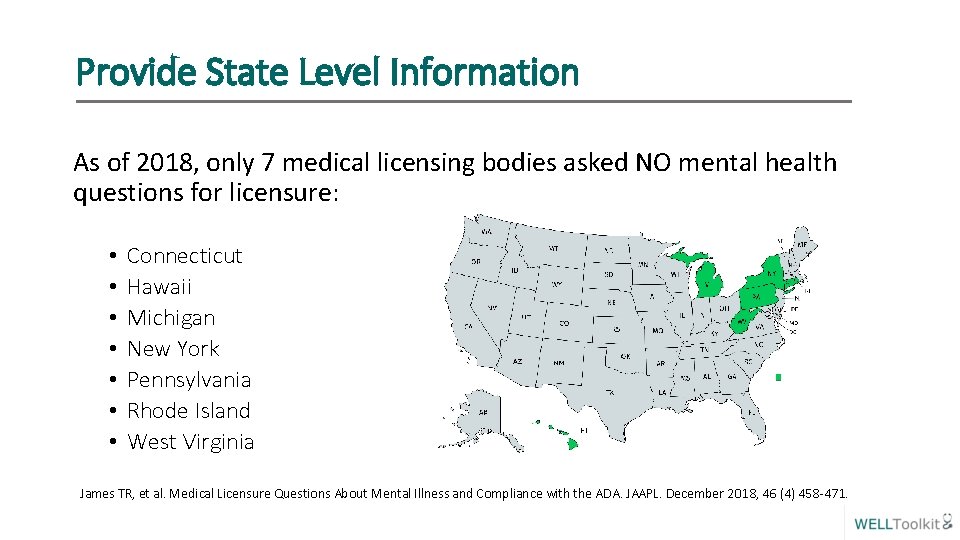
Provide State Level Information As of 2018, only 7 medical licensing bodies asked NO mental health questions for licensure: • • Connecticut Hawaii Michigan New York Pennsylvania Rhode Island West Virginia James TR, et al. Medical Licensure Questions About Mental Illness and Compliance with the ADA. JAAPL. December 2018, 46 (4) 458 -471.

Provide Institution. Level Information It is important to make the questions easily accessible This is an example of a hospital credentialing form. Do you know what questions are asked at your institution? 1. Are you currently using any chemical substance(s) which in any way may impair or limit your ability to practice medicine with reasonable skill and safety? � Yes � No 2. Are you currently engaged in illegal use of controlled dangerous substances? � Yes � No 3. Are you currently participating in a supervised rehabilitation program or professional assistance program which monitors or treats you? � Yes � No 4. Do you have a medical or psychiatric condition which in any way may impair or limit your ability to practice medicine with reasonable skill and safety with or without reasonable accommodation? � Yes � No

Provide Details of Mental Health Provider Contracts (1 of 2) Provider Payment Contact Name of therapist/provider, degree, training background, license #, modality of treatment, description of purpose, length of treatment, # of sessions, transition process Method and amount of charge, cancellation window, option to not be billed to insurance (if preferred), if therapist salary pre-paid by institution client identity is not released for billing Phone calls returned within specific amount of time, secure email for scheduling or other purposes, an on-call crisis system Provider information

Provide Details of Mental Health Provider Contracts (2 of 2) Privacy Records Confidentiality protected by state law, information only shared with written consent or in rare circumstances (e. g. court ordered, protection from harm, child/elder abuse, if active and impairing addictive disease) Ideally does NOT utilize the institutional EMR, client has right to review records (unless detrimental to health in which case provider would share with a mental health professional of the individual's choice) Client information

Advocate for a Culture that Values Physician Well-Being Ia. Access to Care: WELL Resource Guide High-quality resources exist to support well-being advocacy • This is page from the APA Wellbeing Ambassador Toolkit, which is just one of many helpful online resources • Check out the National Academy of Medicine (NAM) Clinician Well-Being Knowledge Hub to find more: https: //nam. edu/clinicianwellbeing

10 Tips for Physician Supervisors Ia. Access to Care: WELL Resource Guide 1. Avoid making assumptions. When concerning behaviors arise in physicians, inquire with that individual whether they are doing okay, prior to assuming they are simply acting in an unprofessional manner. 2. Defer conversations about competence. Avoid making decisions related to goodness of fit around career-choice or assumptions about potential for success or failure within a specialty while a physician is in crisis. 3. Decrease barriers. Problem solve with the physician around barriers to help-seeking and assure that the individual will be supported as confidentially and professionally as possible in the process. 4. Offer accommodations. Prioritize appropriate follow-up for physician mental health concerns and, when indicated, provide accommodations and flexibility. 5. Describe details related to taking leave. Explain options for taking time away from work to get professional help when necessary. Describe the practical implications and reassure that clinical coverage will be handled in their absence.

10 Tips for Physician Supervisors Ia. Access to Care: WELL Resource Guide 6. Be aware of relevant policies. Supervisors must know how the specifics of institutional policies (e. g. FMLA, Short-Term Disability, Paid Time Off, etc. ) impact physicians. 7. Know who can answer practical questions. Supervisors need to know how to contact internal representatives in Human Resources, Legal Department, and the Graduate Medical Education Office. 8. Know how to make a referral. Be aware of workplace supports and mental health referral sources for physicians (e. g. Physicians Assistance Programs). 9. Know about crisis services. Supervisors must know how to connect a physician with local crisis services and national hotlines in an emergency. 10. Post a flyer. Spread the word by posting a highly recognizable one-page flyer of local physician resources at your institution in physician lounges, call rooms, online sites, and wherever physicians can access this information discretely.

Summarize Local Resources Ia. Access to Care: WELL Resource Guide Improve access to mental health and supportive resources for physicians by creating and distributing a easily recognizable, one-page flyer of local resources. A sample UPMC flyer may be found at the WELL website: https: //gmewellness. upmc. com

Spread the Word on National Resources

What can physician leaders do?

We all struggle (but historically physicians often struggle alone) Physician leaders have the power to change the culture of maladaptive perfectionism. • • • What if trainees knew attendings for their HUMANITY? What if attendings MODELED what it really takes to thrive? What if trainees knew that some of their mentors struggled too, and that they are thriving BECAUSE they sought help?

May 30, 2017 Dear Members of the Graduate Medical Education Community, In addition to our efforts around the clinical learning and working environment, it may require evolution of our culture, where admitting needs or weakness has been often seen as a sign of Lack of commitment. … We must model the behaviors we wish to instill in our residents… Enhance mentoring by senior peers and faculty. Mentors can help to destigmatize asking for help related to depression, burnout, and feelings of inadequacy. Most sincerely, Thomas J. Nasca, MD, MACP Chief Executive Officer Accreditation Council for Graduate Medical Education (ACGME)

91% of medical students surveyed (N=43) agreed or strongly agreed with the statement: “knowing doctors further along in their careers who struggled with mental health issues, got treatment, and are now doing well would make me more likely to access care if I needed it. ”

What can you do next? https: //www. seeonedooneteachone. net/3 -steps

For more information: Thank you! The WELL Website https: //gmewellness. upmc. com Please email questions to: Sansea Jacobson, M. D. jacobsonsl@upmc. edu Vu Nguyen, M. D. nguyenvt 3@upmc. edu
- Slides: 26