How Bundled Payments Change Reimbursement Landscape Jeff Peters

How Bundled Payments Change Reimbursement Landscape Jeff Peters CEO, Surgical Directions

Agenda How the business of perioperative services is changing Why bundles are here to stay Will bundles change under the new administration How reimbursement changes under bundles How should perioperative services be organized How the role of the OR Business Manager is evolving Case Study • New Hanover Client logo placeholder
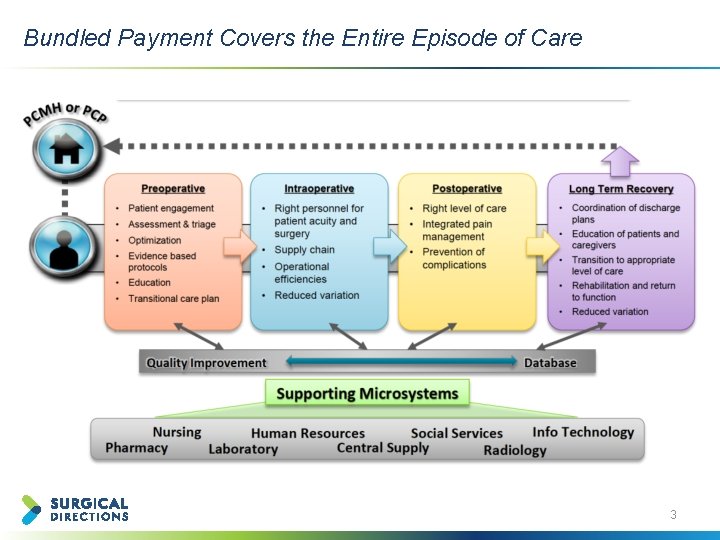
Bundled Payment Covers the Entire Episode of Care 3

Bundled Payments Client logo placeholder Politically Agnostic Hospitals Survival in New Value Based Payment Environment Essential Competency
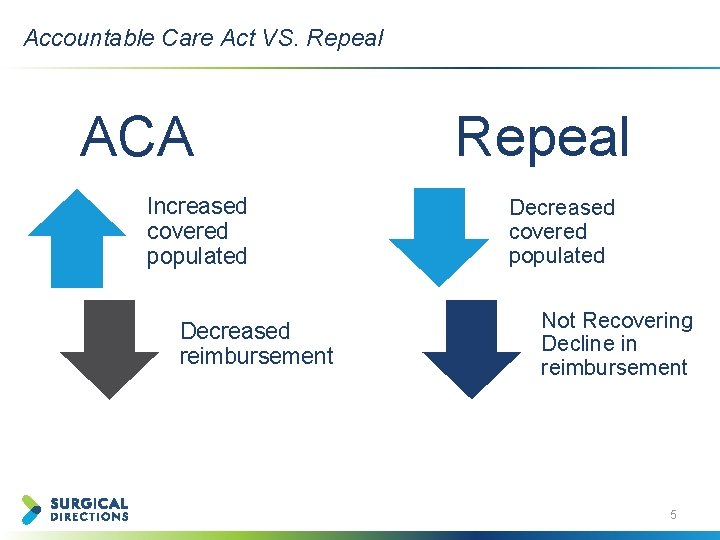
Accountable Care Act VS. Repeal ACA Increased covered populated Decreased reimbursement Repeal Decreased covered populated Not Recovering Decline in reimbursement 5

“We can’t solve the problems of healthcare with incremental add-on solutions, we have to change the very structure of how we deliver and think about healthcare” ASA National Meeting 2016— Michael Porter Ph. D
Adapting Perioperative Services to a Value Based Model Cost Outcome Value 7

Value Based Payments Now 26% of hospital patients are currently in value based payments Commercial carriers are moving to bundles Humana Tennessee Healthleaders 5/18/2017 8
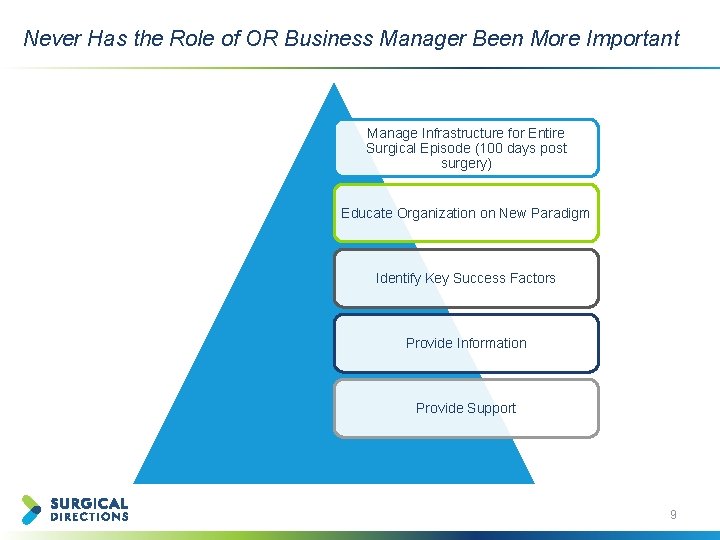
Never Has the Role of OR Business Manager Been More Important Manage Infrastructure for Entire Surgical Episode (100 days post surgery) Educate Organization on New Paradigm Identify Key Success Factors Provide Information Provide Support 9

Key Pillars for Success Under Bundles Governance • Multidisciplinary Steering Committee • Daily Huddle Commitment • Physician Leadership • Resources Information • • Cost Quality Patient Satisfaction Surgeon Score Cards Clinical Redesign • • PAT ERAs Clinical Pathway Post Discharge 10

Perioperative Organization Needs to Change OR Director Historical Under Value Based Payment Span of Control Scheduling PAT OR PACU Surgical Floor SICU Title OR Director VP of Surgical Services Duties & Details 11
Keys to Success Case Time Information Surgeon Education Metrics Physician Leadership Anesthesia P. I. T. 12

New Hanover Medical Center Case Study Goal • Create strategic alignment between Orthopedic & Colorectal Surgeons • Become provider of choice for Orthopedic surgeons and their patients Strategy • Surgical Home • Co-Management Agreement 13

Surgical Home Steering Committee Member: Responsibility: Surgeon • • • Clinical Metrics Dashboard Monitor Drive Change Address Issues Anesthesia • • • Organizational Qualitative Redesign Nursing • • Consensus Goals 14
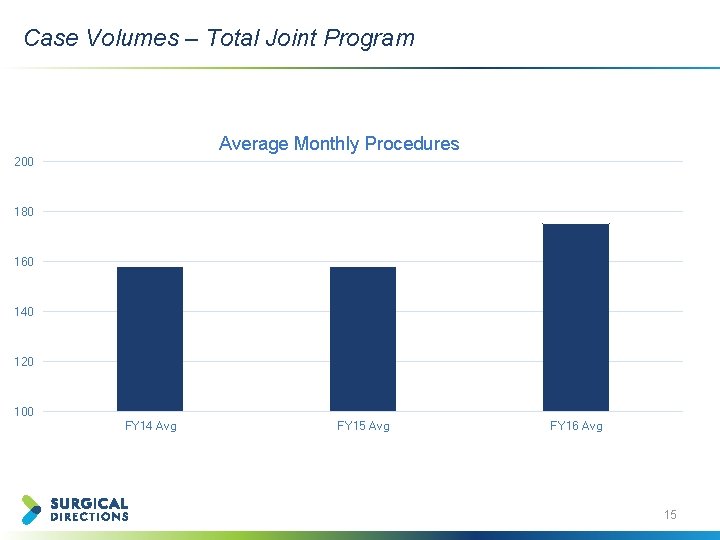
Case Volumes – Total Joint Program Average Monthly Procedures 200 180 160 140 120 100 FY 14 Avg FY 15 Avg FY 16 Avg 15
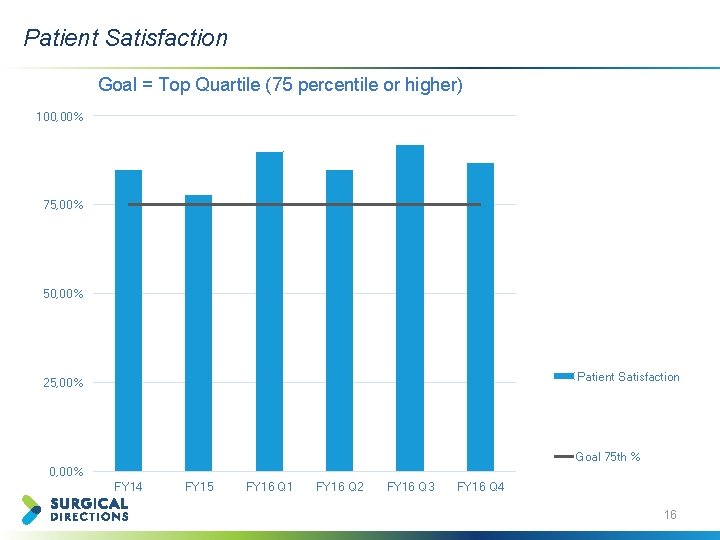
Patient Satisfaction Goal = Top Quartile (75 percentile or higher) 100, 00% 75, 00% 50, 00% Patient Satisfaction 25, 00% Goal 75 th % 0, 00% FY 14 FY 15 FY 16 Q 1 FY 16 Q 2 FY 16 Q 3 FY 16 Q 4 16
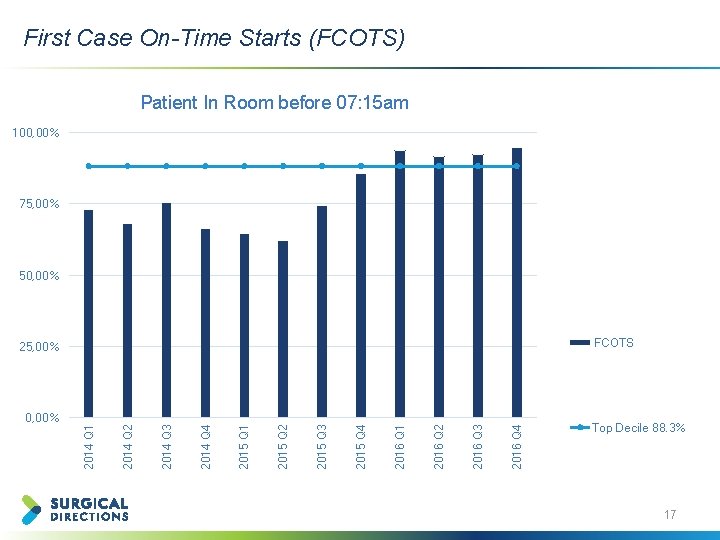
First Case On-Time Starts (FCOTS) Patient In Room before 07: 15 am 100, 00% 75, 00% 50, 00% FCOTS 2016 Q 4 2016 Q 3 2016 Q 2 2016 Q 1 2015 Q 4 2015 Q 3 2015 Q 2 2015 Q 1 2014 Q 4 2014 Q 3 2014 Q 2 0, 00% 2014 Q 1 25, 00% Top Decile 88. 3% 17
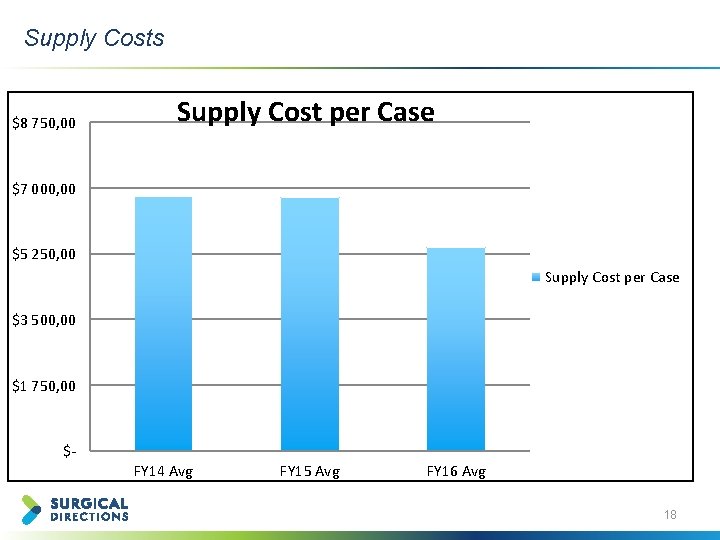
Supply Costs $8 750, 00 Supply Cost per Case $7 000, 00 $5 250, 00 Supply Cost per Case $3 500, 00 $1 750, 00 $FY 14 Avg FY 15 Avg FY 16 Avg 18
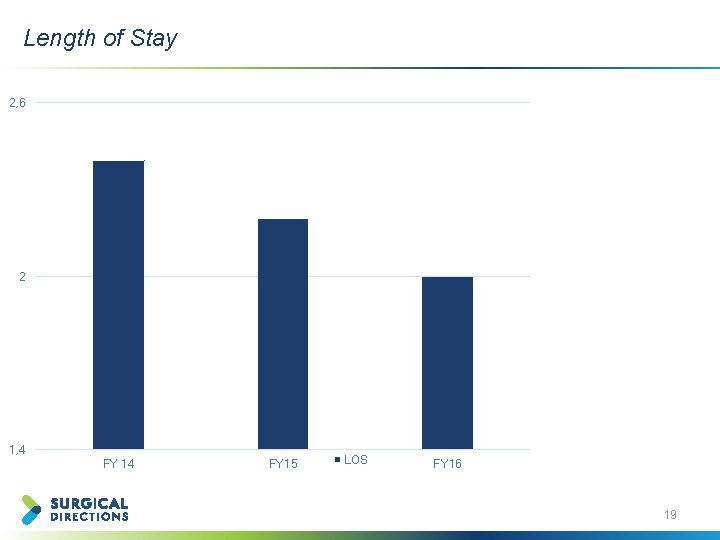
Length of Stay 2, 6 2 1, 4 FY 15 LOS FY 16 19
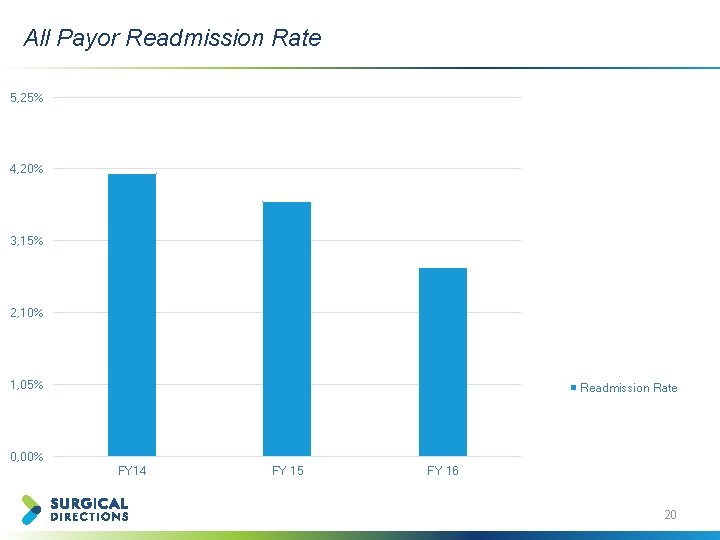
All Payor Readmission Rate 5, 25% 4, 20% 3, 15% 2, 10% 1, 05% Readmission Rate 0, 00% FY 14 FY 15 FY 16 20
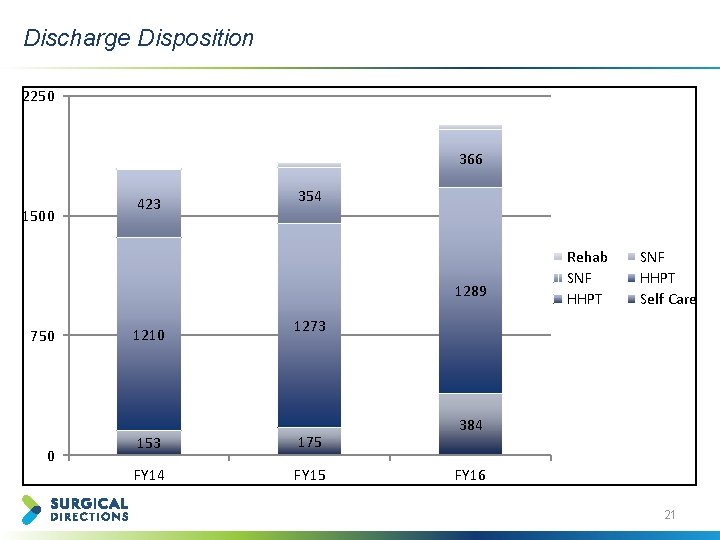
Discharge Disposition 2250 366 1500 423 354 1289 750 0 1210 Rehab SNF HHPT Self Care 1273 153 175 FY 14 FY 15 384 FY 16 21
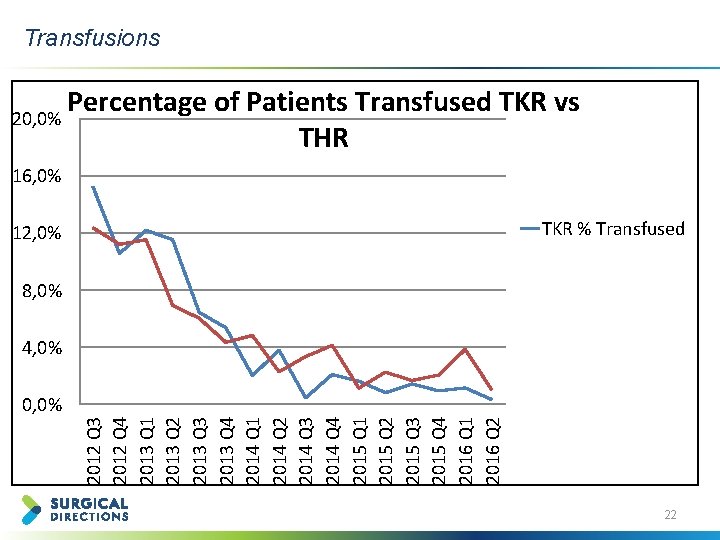
2012 Q 3 2012 Q 4 2013 Q 1 2013 Q 2 2013 Q 3 2013 Q 4 2014 Q 1 2014 Q 2 2014 Q 3 2014 Q 4 2015 Q 1 2015 Q 2 2015 Q 3 2015 Q 4 2016 Q 1 2016 Q 2 Transfusions Percentage of Patients Transfused TKR vs 20, 0% THR 16, 0% 12, 0% TKR % Transfused 8, 0% 4, 0% 0, 0% 22
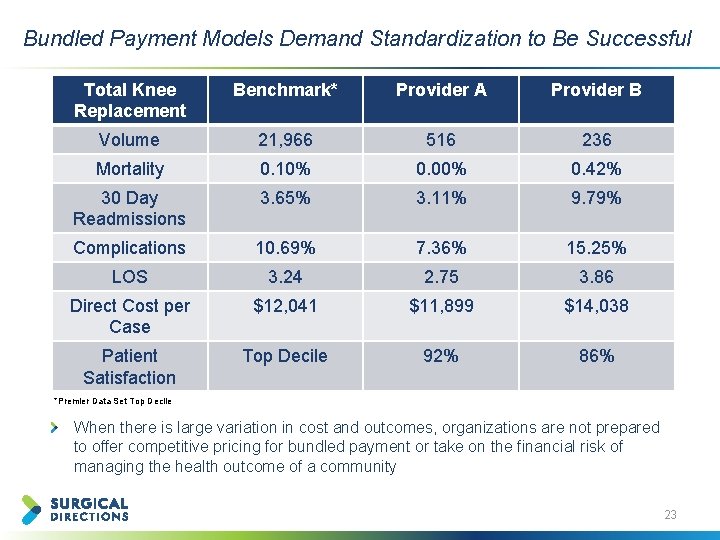

Bundled Payment Models Demand Standardization to Be Successful Total Knee Replacement Benchmark* Provider A Provider B Volume 21, 966 516 236 Mortality 0. 10% 0. 00% 0. 42% 30 Day Readmissions 3. 65% 3. 11% 9. 79% Complications 10. 69% 7. 36% 15. 25% LOS 3. 24 2. 75 3. 86 Direct Cost per Case $12, 041 $11, 899 $14, 038 Patient Satisfaction Top Decile 92% 86% *Premier Data Set Top Decile When there is large variation in cost and outcomes, organizations are not prepared to offer competitive pricing for bundled payment or take on the financial risk of managing the health outcome of a community 23
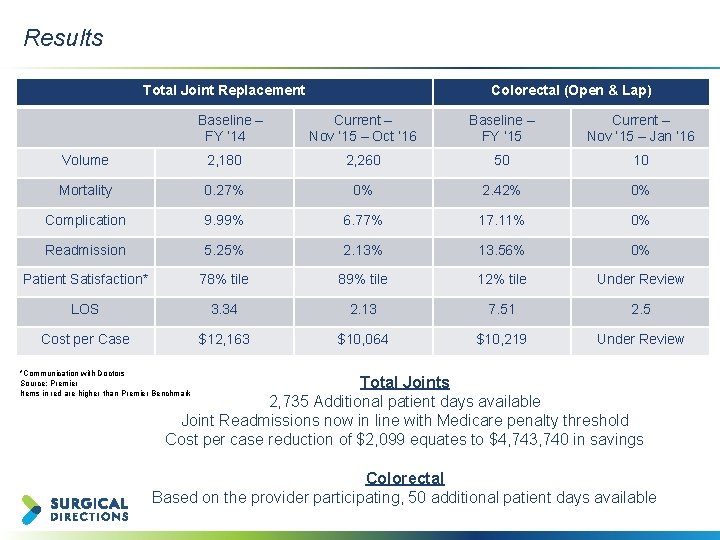
Results Client logo placeholder Total Joint Replacement Baseline – FY ’ 14 Colorectal (Open & Lap) Current – Nov ‘ 15 – Oct ’ 16 Baseline – FY ’ 15 Current – Nov ‘ 15 – Jan ‘ 16 Volume 2, 180 2, 260 50 10 Mortality 0. 27% 0% 2. 42% 0% Complication 9. 99% 6. 77% 17. 11% 0% Readmission 5. 25% 2. 13% 13. 56% 0% Patient Satisfaction* 78% tile 89% tile 12% tile Under Review LOS 3. 34 2. 13 7. 51 2. 5 Cost per Case $12, 163 $10, 064 $10, 219 Under Review *Communication with Doctors Source: Premier Items in red are higher than Premier Benchmark Total Joints 2, 735 Additional patient days available Joint Readmissions now in line with Medicare penalty threshold Cost per case reduction of $2, 099 equates to $4, 743, 740 in savings Colorectal Based on the provider participating, 50 additional patient days available

Outcome Growth in Orthopedic Volume Increased Financial Performance 25

Surgical Directions 541 N. Fairbanks Court Suite 2740 Chicago, IL 60611 T 312. 870. 5600 F 312. 870. 5601 www. Surgical. Directions. com
- Slides: 26