Hot Topics in Obesity Treatment Prevalence of Overweight

Hot Topics in Obesity Treatment
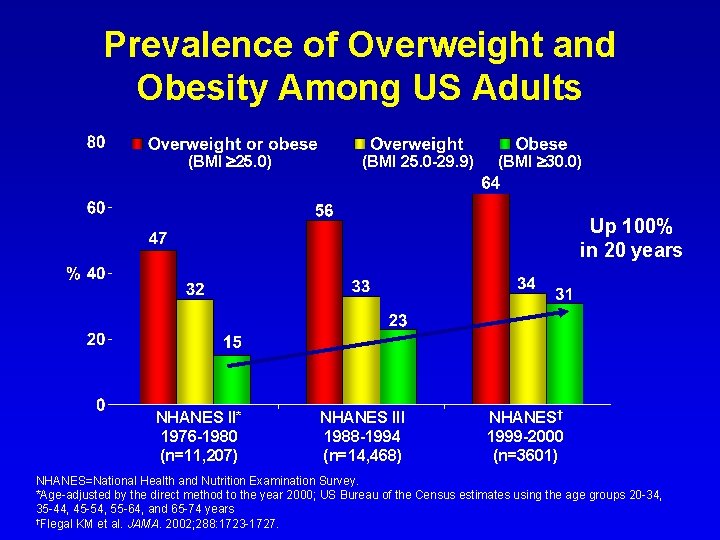
Prevalence of Overweight and Obesity Among US Adults (BMI 25. 0) (BMI 25. 0 -29. 9) (BMI 30. 0) Up 100% in 20 years NHANES II* 1976 -1980 (n=11, 207) NHANES III 1988 -1994 (n=14, 468) NHANES† 1999 -2000 (n=3601) NHANES=National Health and Nutrition Examination Survey. *Age-adjusted by the direct method to the year 2000; US Bureau of the Census estimates using the age groups 20 -34, 35 -44, 45 -54, 55 -64, and 65 -74 years †Flegal KM et al. JAMA. 2002; 288: 1723 -1727.

Binge Eating • Could there be a survival advantage to being able to binge or eat more in an environment with limited food?
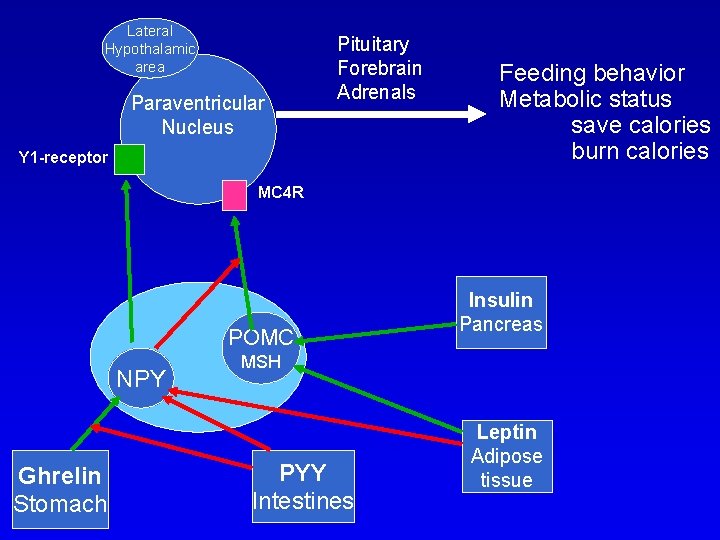
Lateral Hypothalamic area Paraventricular Nucleus Pituitary Forebrain Adrenals Y 1 -receptor Feeding behavior Metabolic status save calories burn calories MC 4 R POMC NPY Ghrelin Stomach Insulin Pancreas MSH PYY Intestines Leptin Adipose tissue

Binge and MC 4 R Gene • Two articles in the NEJM March 2003 – Branson: 5. 1% of obese had MC 4 R gene mutations – Farooqi: 5. 8 % of obese had MC 4 R gene mutations • All mutation carriers reported binge eating

Binge Eating • 469 morbid obese Caucasian patients • 79% female • Found 24 pts (5. 1%) with a mutation of the MC 4 R – Basically a defective receptor • All 24 of these pts (100%) had binge eating • Only 14% of matched controls had binging NEJM 348: 12, 2003.

Binge Eating • 500 morbid obese children • Found 29 pts (5. 8%) with a mutation of the MC 4 R – Basically a defective receptor • All 29 of these patients had “hyperphagia” • Compared to unaffected siblings they ate three times as much food at a single meal – Meal size corrected for lean body mass NEJM 348: 12, 2003.
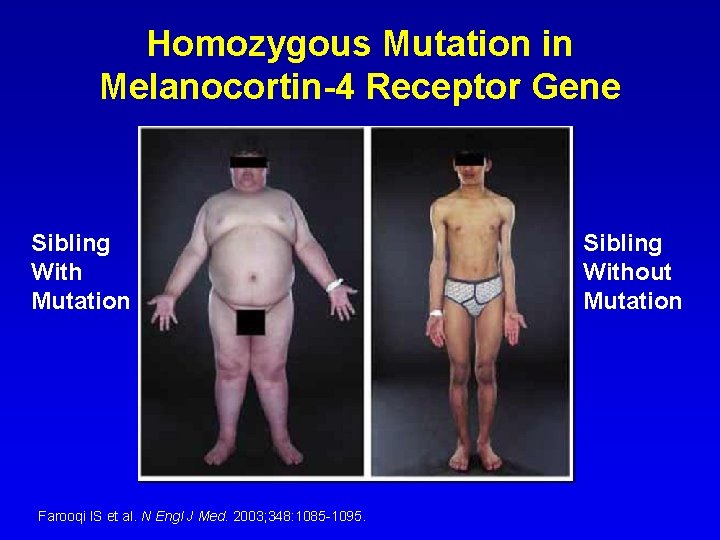
Homozygous Mutation in Melanocortin-4 Receptor Gene Sibling With Mutation Farooqi IS et al. N Engl J Med. 2003; 348: 1085 -1095. Sibling Without Mutation

MC 4 R Mutations • Mutations carriers were: – Severely obese – Increased lean mass – Increased linear growth – Severe hyper-insulinemia • Homozygotes were more severely effected than heterozygotes

Binge Eating Disorder Definition of a Binge Episode • Eating an amount of food that is definitely larger than most people would eat in similar circumstances during a similar period of time (eg, 2 x a normal portion in 2 hours) • A sense of lack of control during the episodes – Sense of inability to stop or control eating • Marked distress about the binge eating – Women yes, men often not • Binge eating is a provisional DSM code at this time

Secondary Binge Criteria • Eat alone (closet eating) • Eat when not hungry • Eat fast • Eats until uncomfortably full • Feeling of guilt or un-happiness after eating • Loose criteria different for men and women

Questions for the Clinician to Ask Patients Who Might Have Binge Eating Disorder • Do you ever have episodes of eating where you feel out of control or that you just could not stop yourself? • Do you ever eat large portions of food that would clearly be larger portions that other persons might eat in a similar circumstance?

Diagnostic Criteria for Bulimia Nervosa (BN) • Recurrent episodes of binge eating with loss of control • Recurrent inappropriate compensatory behavior to prevent weight gain • Binge eating and inappropriate compensatory behavior both occur, on average, at least twice a week for 3 months • Self-evaluation is unduly influenced by body shape and weight
Prevalence of BED in Community Samples • BED is found in ~ 2% to 3% of adults – About half are obese Bruce B, Agras WS. Int J Eat Disord. 1992; 12: 365 -373. Spitzer RL et al. Int J Eat Disord. 1992; 11: 191 -203.

Prevalence of BED in Clinical Samples • BED in obese treatment seekers – ~ 7. 6% to 18. 8% (rigorously defined) – ~ 20% to 40% (broadly defined) • BED in Overeaters Anonymous: ~ 70% • BED in bariatric surgery seekers: ~ 25% to 50% Stunkard AJ. In: Handbook of Obesity Treatment. 2002. Wadden TA et al. Surg Clin N Am. 2001; 81: 1001 -1014. Williamson DA, Martin CK. Eat Weight Disord. 1999; 4: 103 -114.
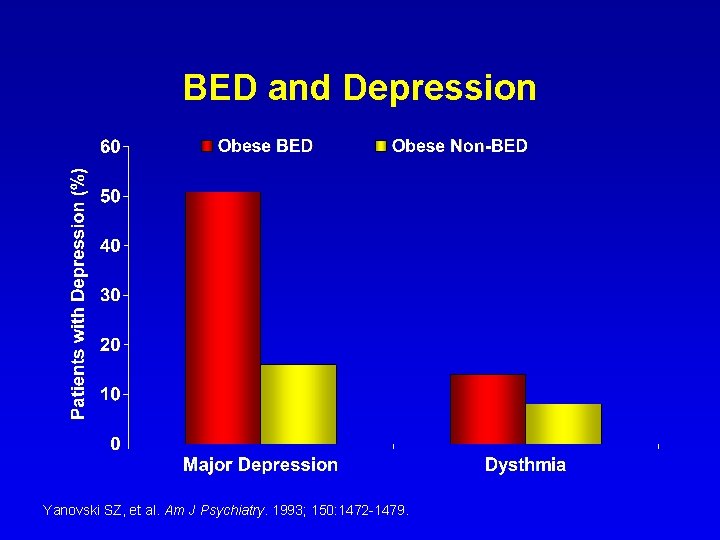
BED and Depression Yanovski SZ, et al. Am J Psychiatry. 1993; 150: 1472 -1479.
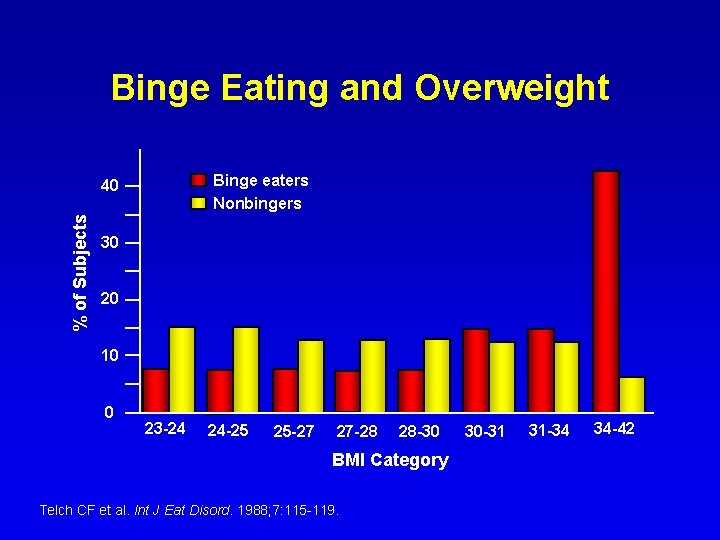
Binge Eating and Overweight Binge eaters Nonbingers % of Subjects 40 30 20 10 0 23 -24 24 -25 25 -27 27 -28 28 -30 BMI Category Telch CF et al. Int J Eat Disord. 1988; 7: 115 -119. 30 -31 31 -34 34 -42
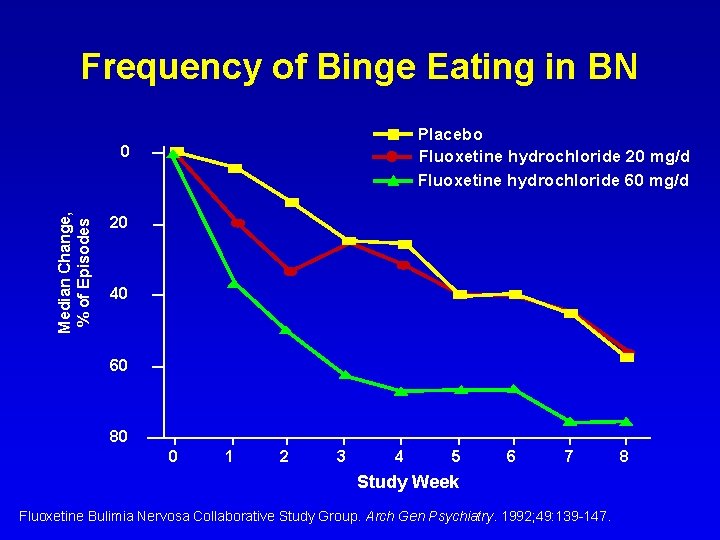
Frequency of Binge Eating in BN Placebo Fluoxetine hydrochloride 20 mg/d Fluoxetine hydrochloride 60 mg/d Median Change, % of Episodes 0 20 40 60 80 0 1 2 3 4 5 6 7 Study Week Fluoxetine Bulimia Nervosa Collaborative Study Group. Arch Gen Psychiatry. 1992; 49: 139 -147. 8
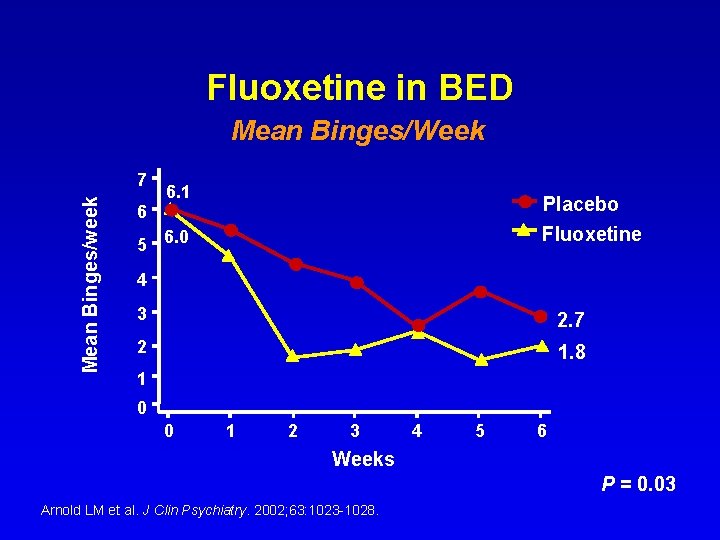
Fluoxetine in BED Mean Binges/Week Mean Binges/week 7 6 6. 1 Placebo Fluoxetine 5 6. 0 4 3 2. 7 2 1. 8 1 0 0 1 2 3 4 5 6 Weeks P = 0. 03 Arnold LM et al. J Clin Psychiatry. 2002; 63: 1023 -1028.

Sibutramine in BED • Placebo-controlled, randomized, double-blind trial • 15 mg/d • 4 -week placebo run-in; 6 -month double-blind treatment – Placebo run-in – Randomized – Completed n = 549 n = 304 n = 189 • Baseline values determined after placebo run-in • Outcome measures: – Binge frequency and weight • A significant difference from placebo was achieved for both outcomes Wilfley DE et al. Presented at: the Eating Disorders Research Society Annual Meeting; Charleston, South Carolina; November 20 -22, 2002.
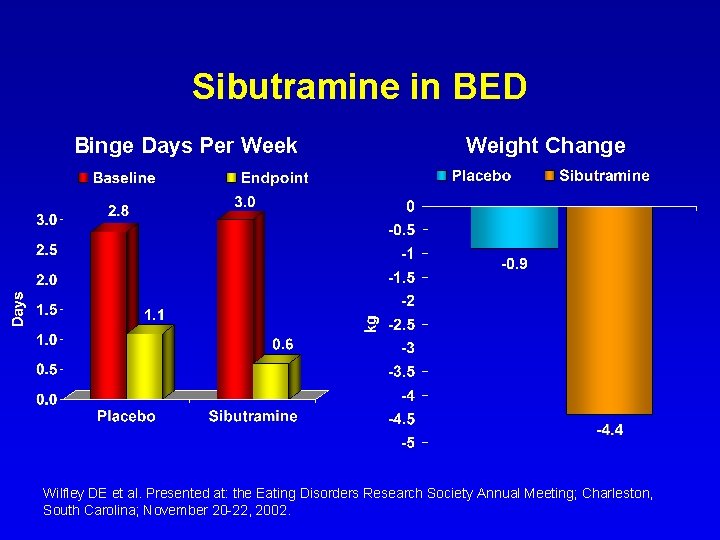
Sibutramine in BED Binge Days Per Week Weight Change Wilfley DE et al. Presented at: the Eating Disorders Research Society Annual Meeting; Charleston, South Carolina; November 20 -22, 2002.

Intermittent Drug Therapy
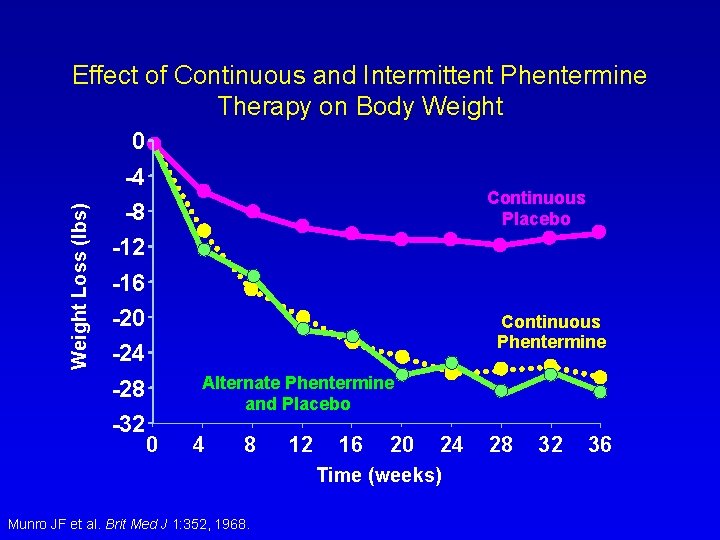
Effect of Continuous and Intermittent Phentermine Therapy on Body Weight 0 Weight Loss (lbs) -4 Continuous Placebo -8 -12 -16 -20 Continuous Phentermine -24 Alternate Phentermine and Placebo -28 -32 0 4 8 12 16 20 24 Time (weeks) Munro JF et al. Brit Med J 1: 352, 1968. 28 32 36
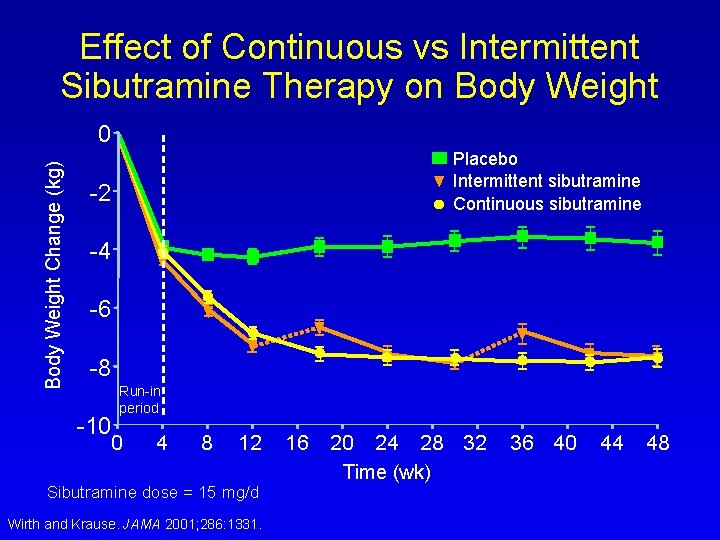
Effect of Continuous vs Intermittent Sibutramine Therapy on Body Weight Change (kg) 0 Placebo Intermittent sibutramine Continuous sibutramine -2 -4 -6 -8 -10 Run-in period 0 4 8 12 Sibutramine dose = 15 mg/d Wirth and Krause. JAMA 2001; 286: 1331. 16 20 24 28 32 Time (wk) 36 40 44 48

Pharmacologic and Surgical Management of Obesity in Primary Care: A Clinical Practice Guideline from the ACP Ann Intern Med 2005; 142: 525 -531.

Medications Used for Weight Loss • • Phentermine* Diethylpropion* Sibutramine# Orlistat# * Approved by the FDA for short term weight loss # Approved by the FDA for weight loss and weight maintenance

“Off-label” Use of Medications for Weight Loss • Bupropion • Fluoxetine • Sertraline • Topiramate • Zonisamide

Coverage of Weight Loss Medications • Typically not covered as a general rule • Although see 30% to 40% coverage • Typically covered medical conditions that get coverage of weight loss medications – Morbid obesity: − With the threat of bariatric surgery – Diabetes – Patients with BMI of ≥ 35 with co-morbid condition – Metabolic syndrome

Paperwork: Billing Codes • Very rarely covered by health insurances – Obesity – 278. 00 • Usually paid billing codes – – Morbid obesity – 278. 01 Dysmetabolic Syndrome – 277. 7 Impaired fasting glucose – 790. 21 Impaired GTT – 790. 22

ACP Guidelines • 5 recommendations based on the evidence report and accompanying background papers developed by the Southern California Evidence-Based Practice Center • The ACP recommends all clinicians refer to these guidelines as part of an overall strategy for managing overweight and obese patients • Overall strategy should always include appropriate diet and exercise • Target audience is patients with BMIs of above 30

ACP Guidelines Recommendation #1 • Clinicians should counsel all patients with a BMI above 30 on lifestyle and behavior modifications such as appropriate diet and exercise • Patient goals should be individually determined

ACP Guidelines Recommendation #2 • Pharmacologic therapy can be offered to patients who have failed diet and exercise alone • Doctor-patient discussion of side effects, long term safety data, and temporary nature of weight loss achieved with medications should occur before medication initiation

ACP Guidelines Recommendation #3 • Medication choices for the obese patient include: sibutramine, orlistat, phentermine, diethylpropion, fluoxetine and bupropion • The choice of drug should be dependent on the side effect profile and the patients tolerance of the side effects

ACP Guidelines Recommendation #4 • Surgery should be considered as a treatment option for patients with a BMI over 40 who: – Instituted but failed an adequate exercise and diet program (with or without adjunctive drug therapy) AND – Present with obesity-related comorbid conditions such as hypertension, impaired glucose tolerance, diabetes mellitus, hyperlipidemia and obstructive sleep apnea • Doctor-patient discussion of surgery should include long term side effects

ACP Guidelines Recommendation #5 • Patients should be referred to high-volume centers with surgeons experienced in bariatric surgery

Bariatric Surgery

Recommendations for Patient Selection • Between ages 18 and 50 • Stable preoperative weight for 3 -5 years • Smoking cessation for at least 6 weeks • Those with psychiatric history require careful assessment • Tests to predict success of surgery: – Personality factors – Eating habits – Motivation Grace DM. Gastroenterol Clin North Am. 1987; 16: 399.

Types of Surgery: Gastric Bypass • Roux-en-Y gastric bypass is the most popular in the US • Pouch can be created with staples or complete division • Long-term weight loss of 50% of excess body weight • Moving Roux limbs distally creates more rapid weight loss – Malabsorption problems may be exacerbated
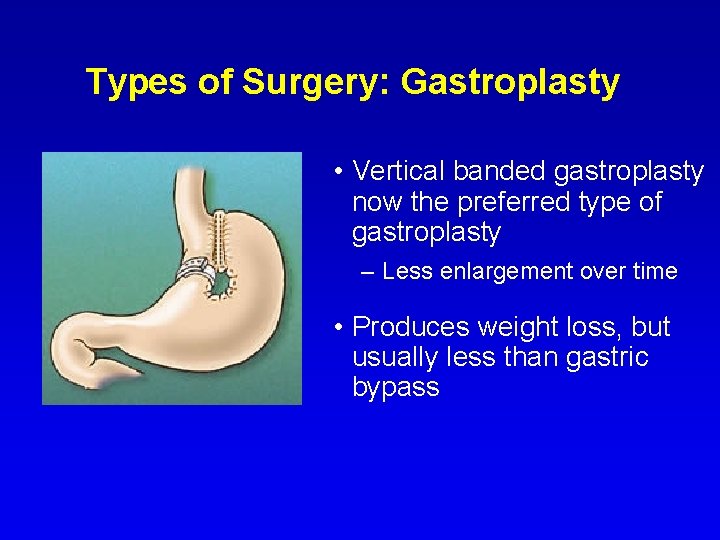
Types of Surgery: Gastroplasty • Vertical banded gastroplasty now the preferred type of gastroplasty – Less enlargement over time • Produces weight loss, but usually less than gastric bypass

Types of Surgery: Gastric Banding • Problems with original gastric band – Pouch too large or small • Adjustable gastric band developed in the 1980 s – Controls restriction by injection/withdrawal of saline • May be performed laparoscopically

Mechanisms • Operations dramatically restrict gastric size, reducing nutritional intake • Some types of surgery decrease the absorption efficiency of nutrients – Roux-en-Y gastric bypass – Biliopancreatic diversion (BPD) • Malabsorption procedures create a greater risk for nutritional deficiencies

Side Effects & Complications 1 in 200 -300 patients in the US die from bariatric surgery • • • Iron deficiency Vitamin B 12 deficiency Folic Acid deficiency Dehydration Vitamin A deficiency Electrolyte deficiency Protein deficiency Hyperparathyroidism Follow up of nutritional and metabolic problems after bariatric surgery K. Fujioka Diabetes Care 28: 481 -484, 2005 • • Nausea Vomiting Abdominal pain Constipation Marginal ulceration Gallstones Bleeding ulcer Obstruction of the stomach outlet Shikora SA. Nutrition in Clinical Practice. 2000; 15: 13. www. mayoclinic. com. Surgery for obesity: What is it and is it for you? . Accessed February 15, 2005.
- Slides: 42