Hot Topics in Newborn Care Neonatal Abstinence Syndrome

Hot Topics in Newborn Care: Neonatal Abstinence Syndrome & Breastfeeding Special Populations Caitlin Vanini C-PNP, C-NNP & Stephanie Solpietro C-PNP

NEONATAL ABSTINENCE SYNDROME

OBJECTIVES • UNDERSTAND THE CURRENT STATUS OF MATERNAL OPIOD USE AND NEONATAL ABSTINENCE SYNDROME (NAS) AND ITS’ AFFECT ON COST AND LENGTH OF STAY • DESCRIBE NAS AND ITS’ CLINICAL MANIFESTATIONS • DESCRIBE MONITORING, EVALUATION OF AND TREATMENT OF NAS • DESCRIBE THE PRIMARY CARE PROVIDERS ROLE IN FOLLOW UP FOR PATIENTS WHO HAVE EXPERIENCED NAS

What is Neonatal Abstinence Syndrome The clinical findings in the neonate associated with opioid exposure and withdrawal Hudak, M. L. , & Tan, R. C. (2012). Neonatal Drug Withdrawal. Pediatrics, 129(2).
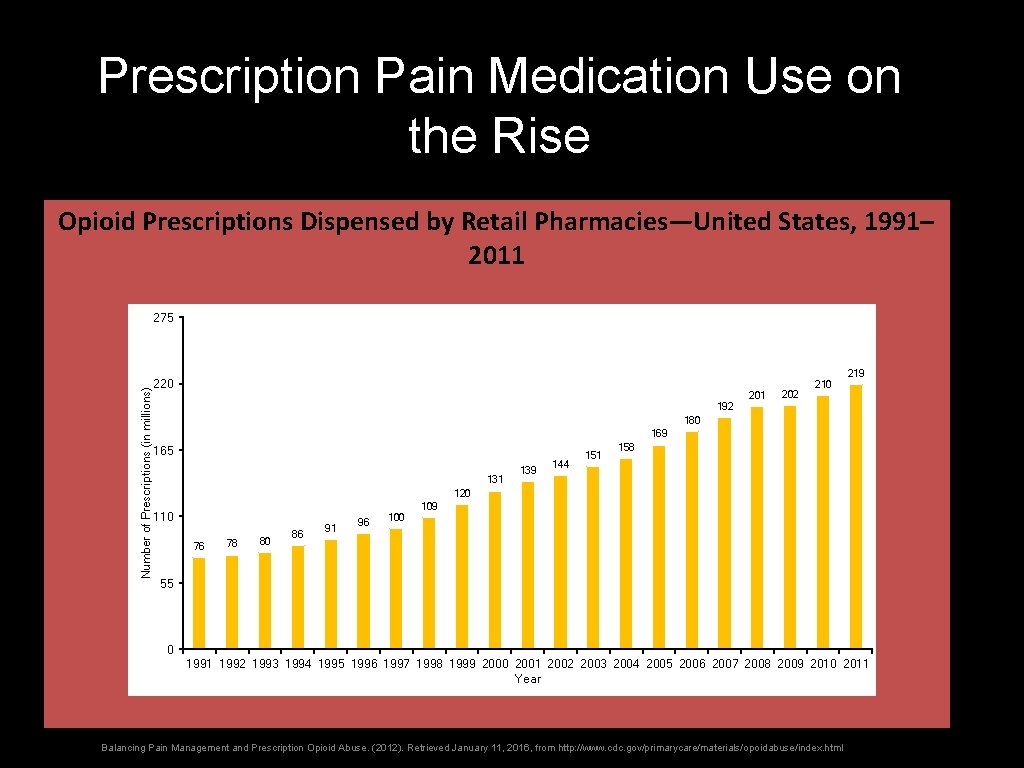
Prescription Pain Medication Use on the Rise Opioid Prescriptions Dispensed by Retail Pharmacies—United States, 1991– 2011 Number of Prescriptions (in millions) 275 INCIDENCE 220 192 201 202 210 219 180 169 165 131 139 144 151 158 120 110 76 78 80 86 91 96 100 109 55 0 1991 1992 1993 1994 1995 1996 1997 1998 1999 2000 2001 2002 2003 2004 2005 2006 2007 2008 2009 2010 2011 Year Balancing Pain Management and Prescription Opioid Abuse. (2012). Retrieved January 11, 2016, from http: //www. cdc. gov/primarycare/materials/opoidabuse/index. html
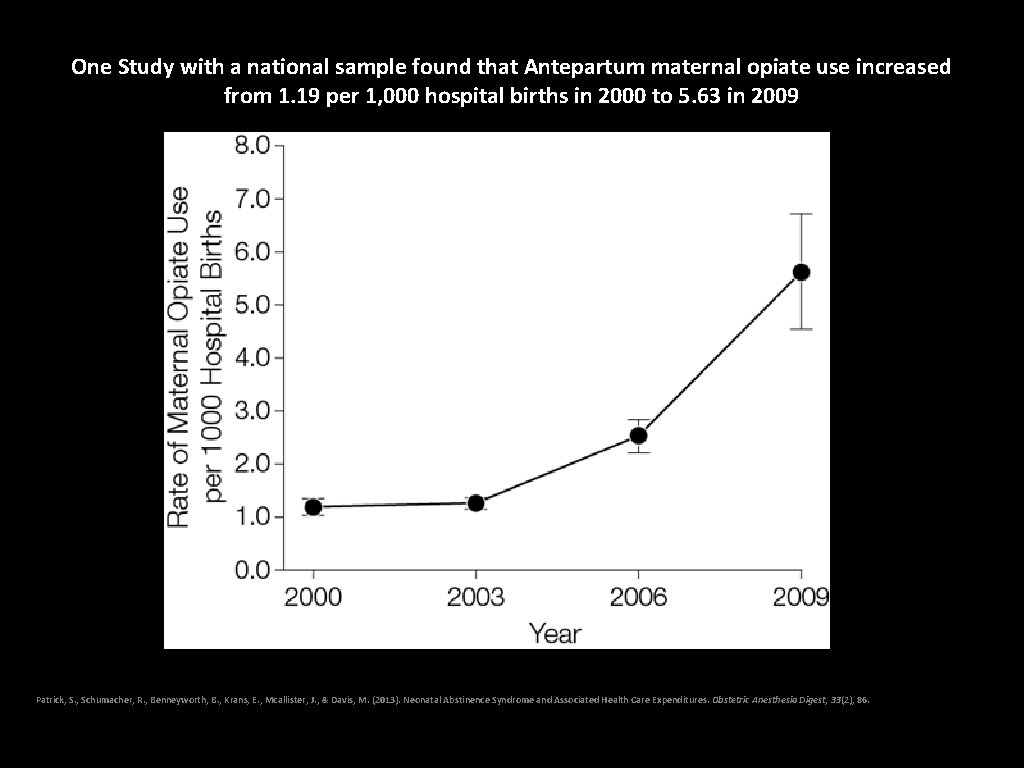
One Study with a national sample found that Antepartum maternal opiate use increased from 1. 19 per 1, 000 hospital births in 2000 to 5. 63 in 2009 Patrick, S. , Schumacher, R. , Benneyworth, B. , Krans, E. , Mcallister, J. , & Davis, M. (2013). Neonatal Abstinence Syndrome and Associated Health Care Expenditures. Obstetric Anesthesia Digest, 33(2), 86.

U. S. Heroin Epidemic • Heroin use more than doubled among young adults ages 18– 25 in the past decade. • More than 9 in 10 people who used heroin also used at least one other drug. • 45% of people who used heroin were also addicted to prescription opioid painkillers. Today’s Heroin Epidemic. (2015). Retrieved January 11, 2016, from http: //www. cdc. gov/vitalsigns/heroin/
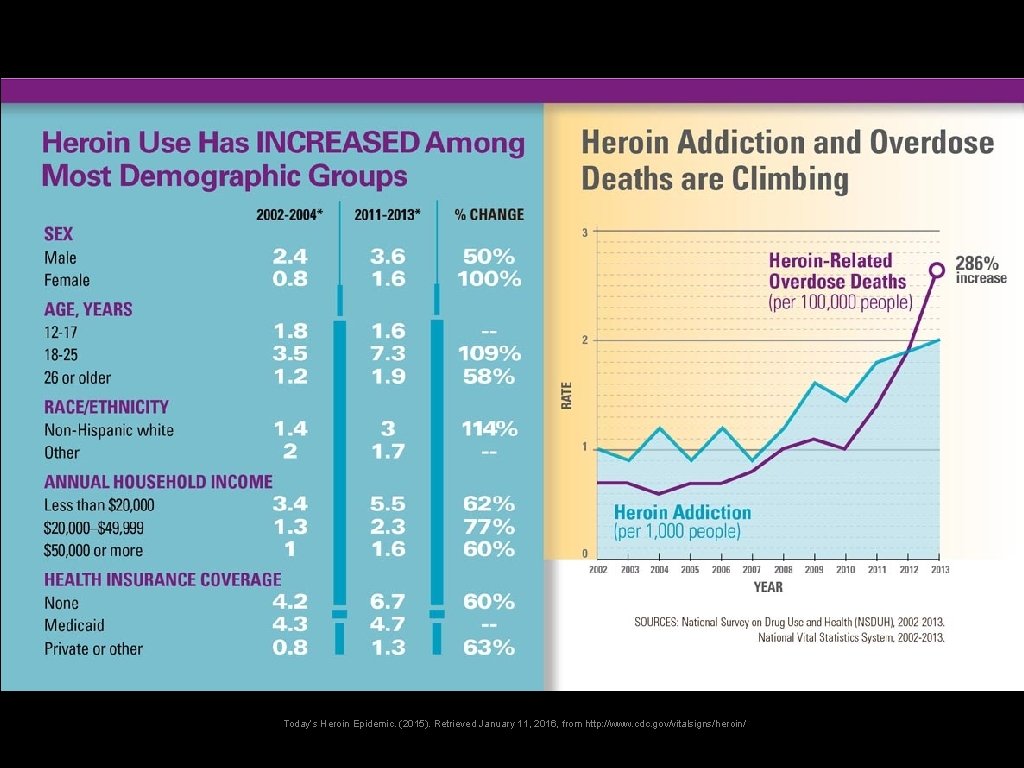
Today’s Heroin Epidemic. (2015). Retrieved January 11, 2016, from http: //www. cdc. gov/vitalsigns/heroin/

Commonly Used Opioids Methadone – Commonly used in treatment program Buprenorphine – Commonly used in treatment program Morphine Oxycodone Hydromorphone Hydrocodone Fentanyl Heroin Hudak, M. L. , & Tan, R. C. (2012). Neonatal Drug Withdrawal. Pediatrics, 129(2).
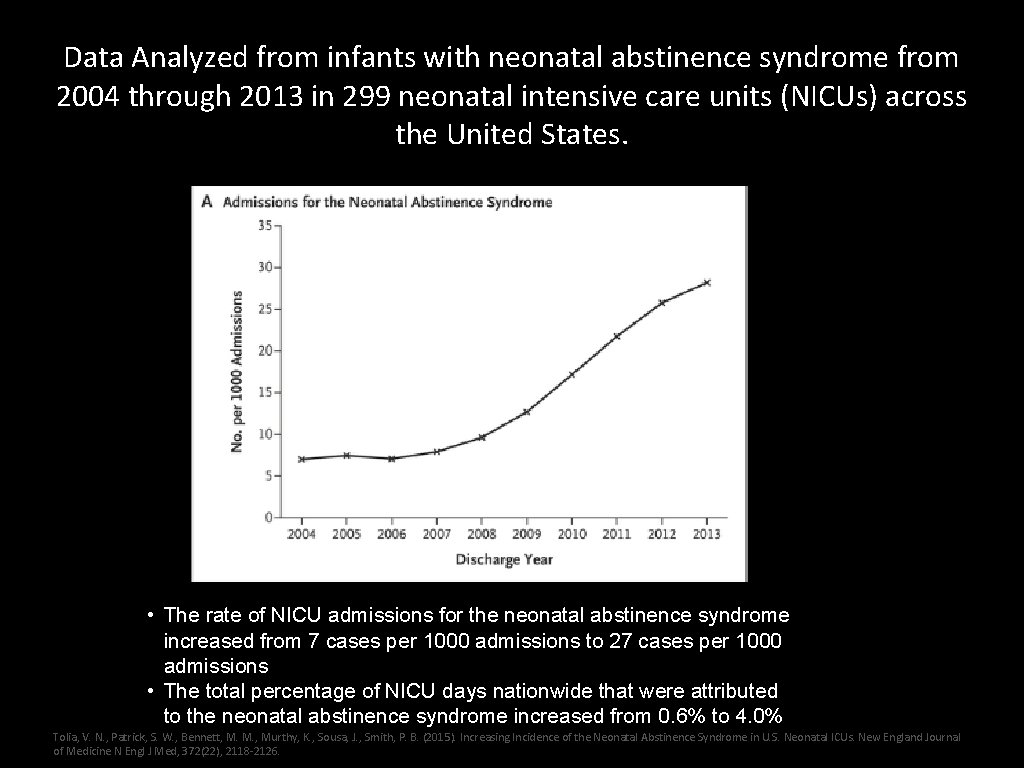
Data Analyzed from infants with neonatal abstinence syndrome from 2004 through 2013 in 299 neonatal intensive care units (NICUs) across the United States. • The rate of NICU admissions for the neonatal abstinence syndrome increased from 7 cases per 1000 admissions to 27 cases per 1000 admissions • The total percentage of NICU days nationwide that were attributed to the neonatal abstinence syndrome increased from 0. 6% to 4. 0% Tolia, V. N. , Patrick, S. W. , Bennett, M. M. , Murthy, K. , Sousa, J. , Smith, P. B. (2015). Increasing Incidence of the Neonatal Abstinence Syndrome in U. S. Neonatal ICUs. New England Journal of Medicine N Engl J Med, 372(22), 2118 -2126.

Increased Risk of Readmission A study in NYS from 2006 to 2009 showed when compared with uncomplicated term infants, infants diagnosed with NAS were more than 2 x as likely to be readmitted to the hospital 30 days of birth hospitalizations. Patrick, S. W. , Burke, J. F. , Biel, T. J. , Auger, K. A. , Goyal, N. K. , & Cooper, W. O. (2015). Risk of Hospital Readmission Among Infants With Neonatal Abstinence Syndrome. Hospital Pediatrics, 5(10), 513 -519.

Dramatic Increases in Maternal Opioid Use and Neonatal Abstinence Syndrome. (2015). Retrieved January 11, 2016, from http: //www. drugabuse. gov/relatedtopics/trends-statistics/infographics/dramaticincreases-in-maternal-opioid-use-neonatalabstinence-syndrome
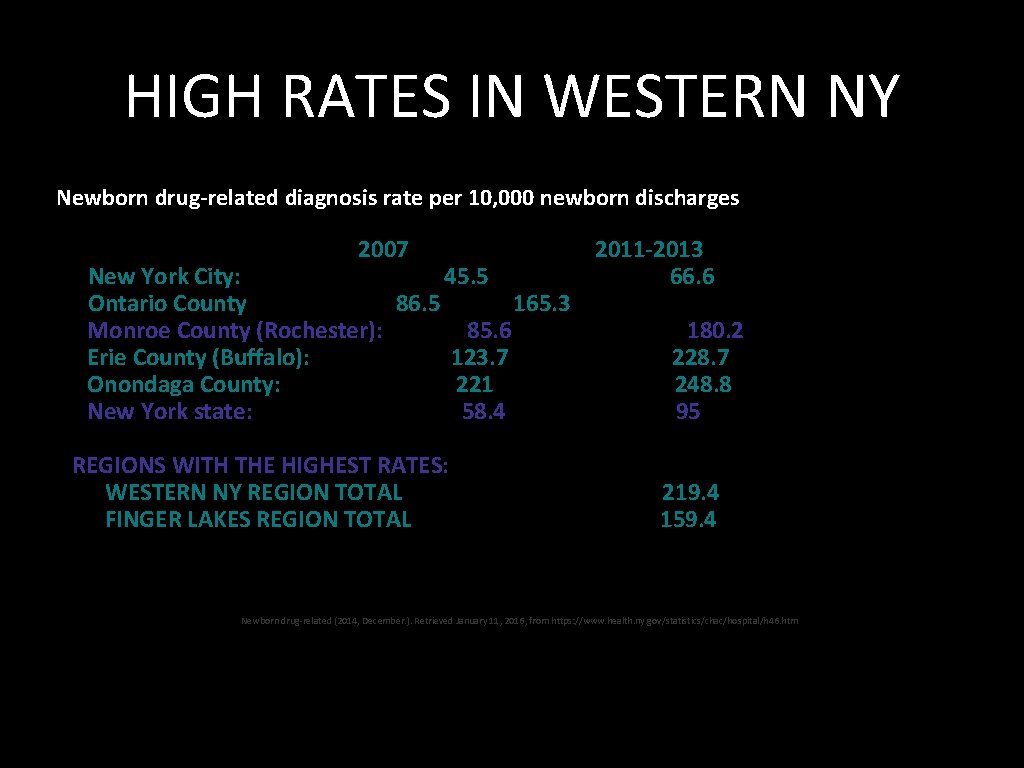
HIGH RATES IN WESTERN NY Newborn drug-related diagnosis rate per 10, 000 newborn discharges 2007 New York City: 45. 5 Ontario County 86. 5 165. 3 Monroe County (Rochester): 85. 6 Erie County (Buffalo): 123. 7 Onondaga County: 221 New York state: 58. 4 REGIONS WITH THE HIGHEST RATES: WESTERN NY REGION TOTAL FINGER LAKES REGION TOTAL 2011 -2013 66. 6 180. 2 228. 7 248. 8 95 219. 4 159. 4 Newborn drug-related (2014, December. ). Retrieved January 11, 2016, from https: //www. health. ny. gov/statistics/chac/hospital/h 46. htm
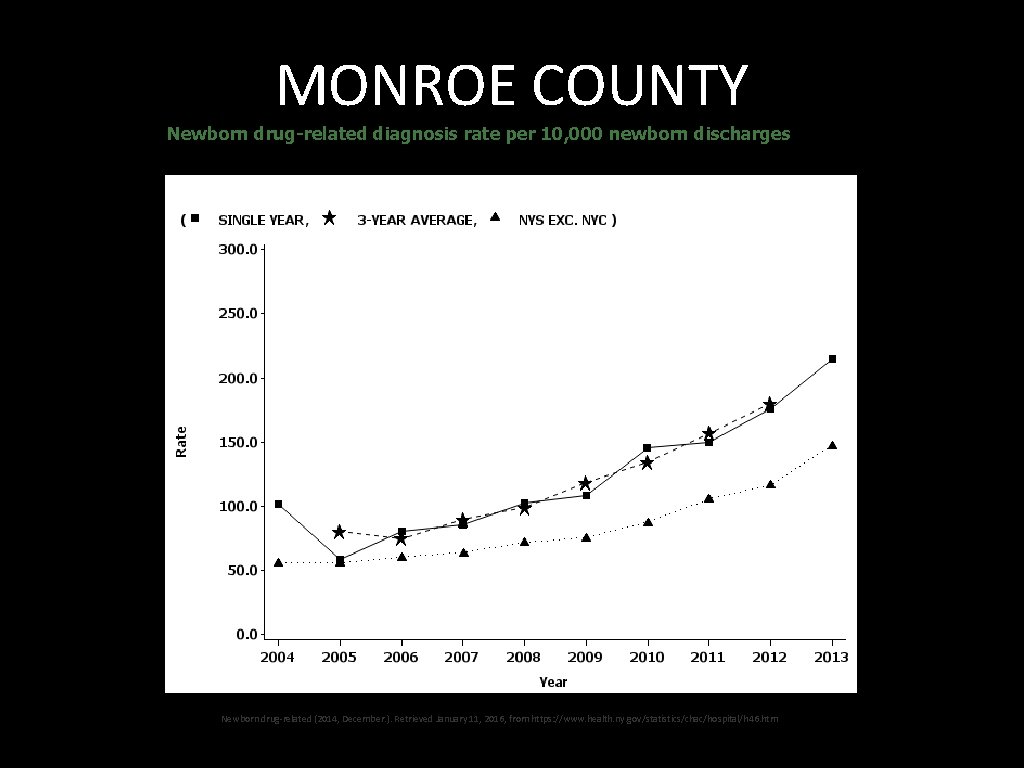
MONROE COUNTY Newborn drug-related diagnosis rate per 10, 000 newborn discharges Newborn drug-related (2014, December. ). Retrieved January 11, 2016, from https: //www. health. ny. gov/statistics/chac/hospital/h 46. htm

State Medicaid Programs Paying the Majority of the Cost is 15 to 16 times higher than healthy infants Cost is rising –Mean hospital charges for discharges with NAS increased from $39, 400 in 2000 to $53, 400 in 2009 Patrick, S. , Schumacher, R. , Benneyworth, B. , Krans, E. , Mcallister, J. , & Davis, M. (2013). Neonatal Abstinence Syndrome and Associated Health Care Expenditures. Obstetric Anesthesia Digest, 33(2), 86. Roussos-Ross, K. , Reisfield, G. , Elliot, I. , Dalton, S. , & Gold, M. (2015). Opioid Use in Pregnant Women and the Increase in Neonatal Abstinence Syndrome. Journal of Addiction Medicine, 9(3), 222 -225.
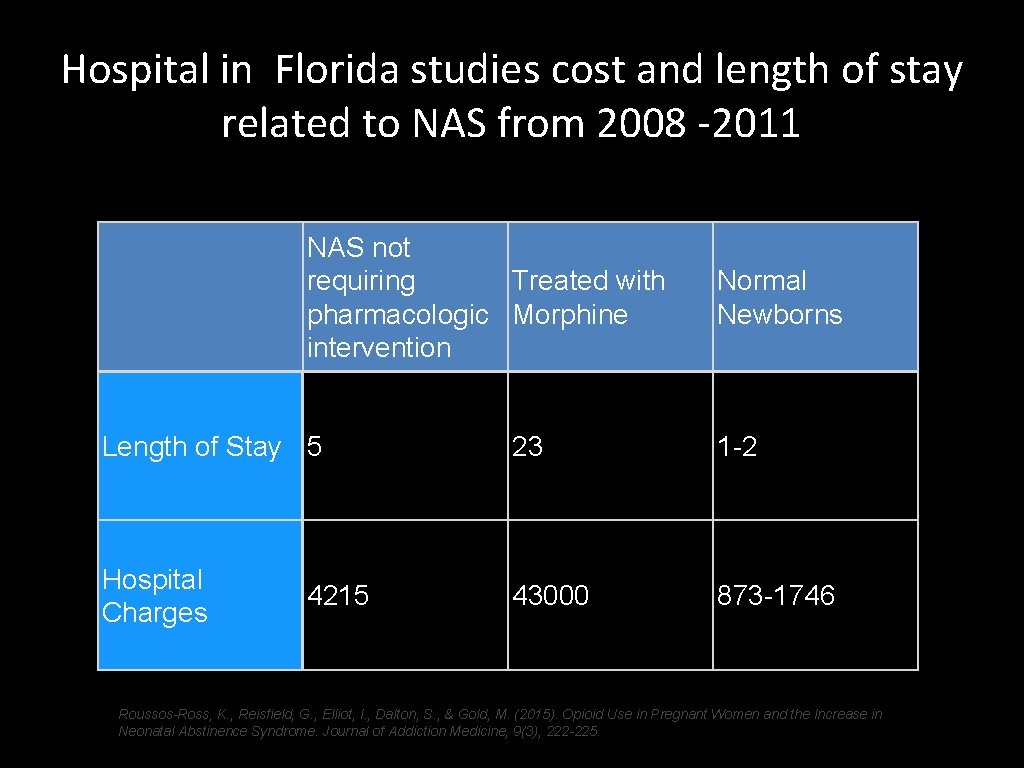
Hospital in Florida studies cost and length of stay related to NAS from 2008 -2011 NAS not requiring Treated with pharmacologic Morphine intervention Normal Newborns Length of Stay 5 23 1 -2 Hospital Charges 43000 873 -1746 4215 Roussos-Ross, K. , Reisfield, G. , Elliot, I. , Dalton, S. , & Gold, M. (2015). Opioid Use in Pregnant Women and the Increase in Neonatal Abstinence Syndrome. Journal of Addiction Medicine, 9(3), 222 -225.

Screening • Maternal History • Maternal Urine Drug Screen • Infant Drug Screen - can have false negative as it requires recent exposure to be accurate • Meconium testing - often not available at hospitals and not practical as it delays diagnosis Bio, L. L. , Siu, A. , & Poon, C. Y. (2011). Update on the pharmacologic management of neonatal abstinence syndrome. J Perinatol Journal of Perinatology, 31(11), 692 -701. Hudak, M. L. , & Tan, R. C. (2012). Neonatal Drug Withdrawal. Pediatrics, 129(2).

SIGNS OF WITHDRAWAL IN NEWBORNS Onset, severity, presentation and signs of withdrawal vary greatly among each infant Increased Temperature Skin Mottling Yawning Sneezing Nasal Stuffiness Tachypnea Increased Metabolic Rate with High Calorie Requirements

SIGNS OF WITHDRAWAL IN NEWBORNS Excessive sucking/uncoordinated suck Poor feeding Weight loss/Poor Gain Reflux Loose watery stools —> diaper rash

SIGNS OF WITHDRAWAL IN NEWBORNS High pitched Cry/Excessive Crying Irritability Excoriation Poor Sleep Hypertonia Tremors disturbed or undisturbed Seizures

Onset of Withdrawal Methadone Heroin Buprenorphine 24 -72 hours Within 24 hours from ~ 40 hours birth Infants are typically monitored for a minimum of 72 -96 hours for signs of Withdrawal onset can be delayed for up to 5 -7 days Hudak, M. L. , & Tan, R. C. (2012). Neonatal Drug Withdrawal. Pediatrics, 129(2).

FINNEGAN SCORING SYSTEM • Most widely used tool in the US • Scores are used to help quantify the severity of the withdrawal and they are used as a guide to start, wean and discontinue treatment • A normal newborn can have scores as high as 8 • At SMH treatment is typically initiated with consistent scores > 8 • Training of staff completing scoring very important • Examination of infant just as important as evaluation of scores as scores can be somewhat subjective • Scores are a reflection of a period of time and not one moment in time • Trending scores over time is important in determining management
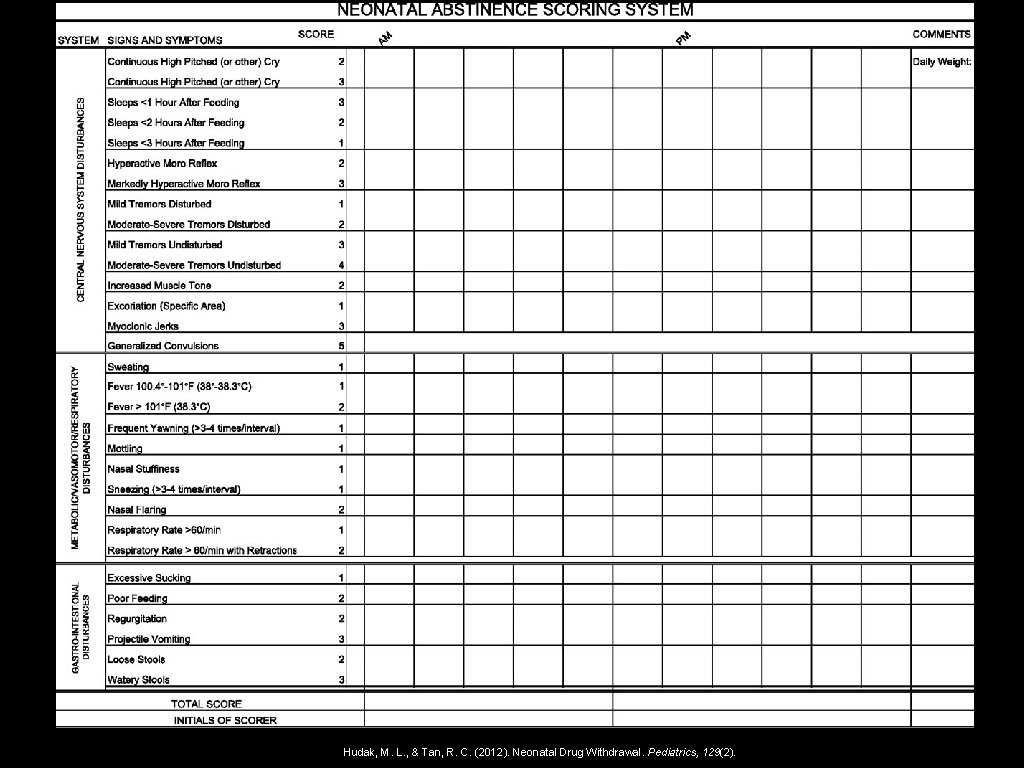
Hudak, M. L. , & Tan, R. C. (2012). Neonatal Drug Withdrawal. Pediatrics, 129(2).

Goal of Therapy To alleviate the symptoms of NAS and to prevent complications including fevers, seizures, discomfort, weight loss etc. Attain sufficient sleep and nutrition Establish pattern of weight gain The goal is NOT to eliminate every single symptom Hudak, M. L. , & Tan, R. C. (2012). Neonatal Drug Withdrawal. Pediatrics, 129(2).

NON-PHARMACOLOGIC MANAGEMENT Decrease Environmental Stimuli Dim lighting Quiet environment Swaddling Decreased Handling Pacifier Firm prolonged touch vs frequent stroking etc.

Multidisciplinary Approach • • Medical Providers Nurses Parents Social work

CAN THESE INFANTS BREASTFEED? • YES! As long as the mother is in a supervised treatment program • There may be other medications or diseases that may be contraindicated, however most of the infant’s treated at SMH can breastfeed if desired! • If mother is unable to breastfeed or desires to use formula then often Gentlease or it’s equivalent is used given the GI symptoms that occur with NAS • Mother’s need to be reassured that despite being on prescribed opioids there is still overall benefit! • Methadone and Buprenorphine transfer to breast milk is very small • BF has been associated with less severe NAS with later onset of withdrawal and less need for pharmacologic treatment • If mother hepatitis C positive – this is not a contraindication unless mother has bleeding or cracked nipples Hudak, M. L. , & Tan, R. C. (2012). Neonatal Drug Withdrawal. Pediatrics, 129(2).

PHARMACOLOGIC MANAGEMENT - MORPHINE Short half life allows for weaning, shorter half life than Methadone Dosed every 4 hours Infant needs to be monitored during initial therapy for signs of respiratory depression Due to decreased responsiveness to carbon dioxide tension Opioids decrease pain perception and cause euphoria and sedation. They also decrease GI motility resulting in constipation and anorexia. At SMH - Once infant “captured” on dose with stable scores for ~ 48 hours then the dose is weaned 10 -20% every 1 -3 days until discontinued At SMH - Once discontinued infant is monitored in the hospital for an additional 24 -48 hours to ensure there is no rebound withdrawal Bio, L. L. , Siu, A. , & Poon, C. Y. (2011). Update on the pharmacologic management of neonatal abstinence syndrome. J Perinatol Journal of Perinatology, 31(11), 692 -701. Hudak, M. L. , & Tan, R. C. (2012). Neonatal Drug Withdrawal. Pediatrics, 129(2).

PHARMACOLOGIC MANAGEMENT – nd PHENOBARBITAL 2 line agent • Most commonly used when there is history of poly -substance use • May be used with severe NAS or when morphine is very difficult to wean • suppresses hyperactivity, decreases CNS activity, helps to control insomnia and irritability. Does not have any affect on opioid specific withdrawal symptoms such as diarrhea and poor feeding • Long half life - drug may not need to be given every day • Infant may be discharged on Phenobarbital with pre-planned taper and close follow up by PCP Bio, L. L. , Siu, A. , & Poon, C. Y. (2011). Update on the pharmacologic management of neonatal abstinence syndrome. J Perinatol Journal of Perinatology, 31(11), 692 -701. Hudak, M. L. , & Tan, R. C. (2012). Neonatal Drug Withdrawal. Pediatrics, 129(2).

PHARMACOLOGIC MANAGEMENT - Other Therapies That Have Been Used • Tincture of opium • Methadone • Clonidine - for poly-substance • diazepam - for poly-substance • Buprenorphine has recently been under investigation as an option to consider in the management of NAS Bio, L. L. , Siu, A. , & Poon, C. Y. (2011). Update on the pharmacologic management of neonatal abstinence syndrome. J Perinatol Journal of Perinatology, 31(11), 692 -701. Hudak, M. L. , & Tan, R. C. (2012). Neonatal Drug Withdrawal. Pediatrics, 129(2).
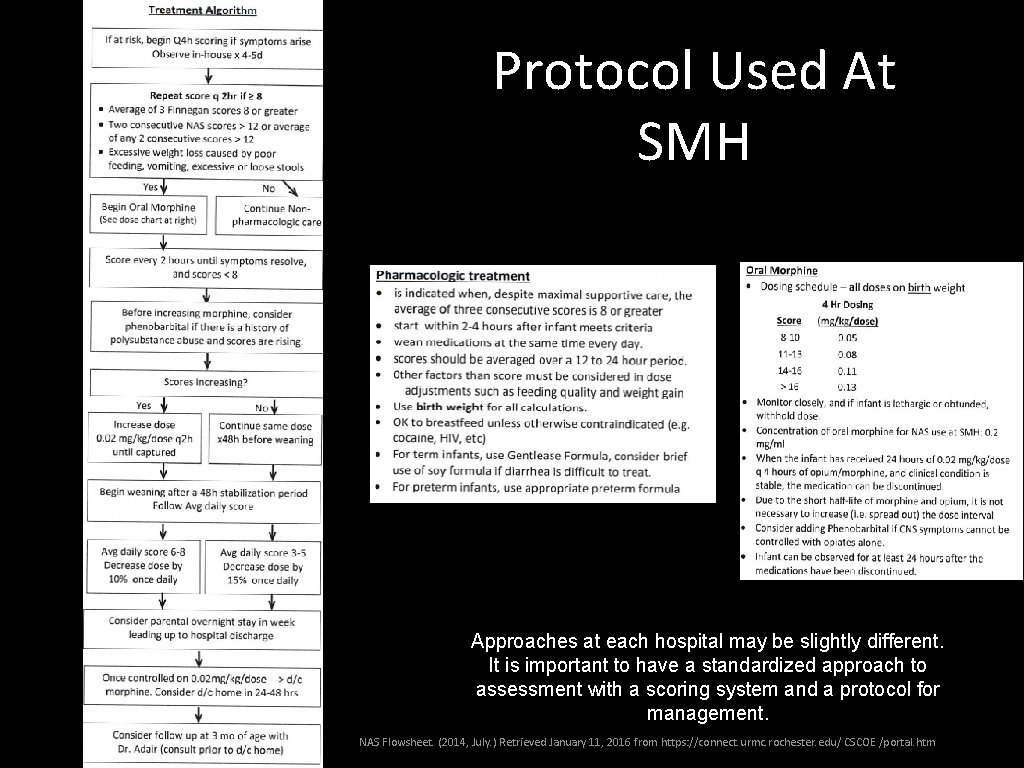

Protocol Used At SMH Approaches at each hospital may be slightly different. It is important to have a standardized approach to assessment with a scoring system and a protocol for management. NAS Flowsheet. (2014, July. ) Retrieved January 11, 2016 from https: //connect. urmc. rochester. edu/ CSCOE /portal. htm

Decreased Risk Of Withdrawal After Opioid Exposure In Preterm Infants • Immature central nervous system • Decreased fat deposition of drug • Decreased length of drug exposure in utero • Inability to express motor dysfunction as compared to term infants i. e. tremors Hudak, M. L. , & Tan, R. C. (2012). Neonatal Drug Withdrawal. Pediatrics, 129(2). Dysart, K. , Hsieh, H. , Kaltenbach, K. , & Greenspan, J. S. (2007). Sequela of preterm versus term infants born to mothers on a methadone maintenance program: Differential course of neonatal abstinence syndrome. Journal of Perinatal Medicine, 35(4).

FOLLOW UP • A visiting nurse often sent to infant’s home in the first few days after discharge to assess weight, feeding and vital signs. Close follow up in the first few days after discharge is indicated to evaluate for continued withdrawal. • At SMH all infants are seen in the Kirch Pediatric Developmental Clinic at 3 months of age • CPS involvement often ongoing after discharge. Note: If mother in a treatment program at time of delivery then CPS will not be notified • Mother may be given referral for outpatient social worker

THE PRIMARY CARE PROVIDERS ROLE • Monitor weight gain closely given high metabolic demands • Determine if infant requires increased caloric density or if infant has stable or excessive weight gain they can be transitioned off higher calorie formula or BM • Advocate for child if parental substance use is suspected to be continuing by reporting to CPS • Work with in-patient clinician on weaning phenobarbital if infant is to go home on medication • Understand the clinical manifestations of NAS and determine if infant experiencing clinically significant withdrawal that would require initial admission or readmission • Understand that withdrawal can occur after hospital discharge and still may require hospitalization • Many times mothers also have a diagnosis of hepatitis C at time of delivery. Be sure to screen at risk infant’s for disease according to Red Book guidelines • Continue to follow infant’s development and refer for evaluation as indicated

OUTCOMES • More research needs to be done! Very limited data on long term outcomes of in utero exposed infants. • Dysfunctional caregivers and other environmental variables make interpretation of outcomes difficult Hudak, M. L. , & Tan, R. C. (2012). Neonatal Drug Withdrawal. Pediatrics, 129(2).

The Breastfeeding Newborn: Special Populations

Objectives - State AAP recommendations for breastfeeding newborns Identify Healthy People 2020 goals for breastfeeding Identify important interview points for the breastfeeding mother Identify special considerations necessary when caring for late preterm infant - Create a feeding plan to optimize growth in the late preterm infant, infant with significant weight loss, and infant with tongue tie - Recognize newborn with tongue tie and make necessary referral and feeding plan to optimize growth - Identify resources for mothers to obtain breast pumps and lactation support

Breast Feeding Recommendations - AAP recommends exclusive breast feeding for the first 6 months of life, then continued breast feeding with the introduction of complimentary foods - According to the CDC 2014 Breast Feeding Report Card: “In 2011, 79% of newborn infants started to breastfeed. Yet breastfeeding did not continue for as long as recommended. Of infants born in 2011, 49% were breastfeeding at 6 months and 27% at 12 months. ”

What makes breast milk optimal nutrition? • Breast milk is a “complex and dynamic fluid that supports ideal infant growth and immune function development. The composition of human milk changes over time, and contains live cells along with macronutrients and micronutrients and bioactive factors. ” (Denne 2015) • Colostrum is the first milk, it begins to produced during the second trimester of pregnancy and is available in relatively low volumes during the first days following delivery. It is rich in secretory Ig. A, lactoferrin, leukocytes, and epidermal growth factor • Breast milk transitions to mature milk during over the next 2 -4 weeks. I t is rich in lactose, fat, immunoglobulins and total proteins (Denne 2015)

Important questions for breast feeding mothers • • • - Complete history: Medical and obstetric history Daily medications and supplements Did she experience breast changes during the first trimester of pregnancy Maternal breast feeding goals How long does mother want to breast feed for? Does she wish to feed at the breast or pump breast milk for bottle feeding What is her previous breast feeding experience and does she have support at home Maternal access to breast pumps thanks to the Affordable Care Act, most new mothers will be able to attain an electric breast pump through insurance, these are generally available through a durable medical equipment supply Mothers with WIC may be able to obtain a breast pump through the WIC peer counselor

Special populations • Late Preterm or Small Infants • Tongue Tie • Significant Weight Loss

Breastfeeding the late preterm infant • Infants born between 34 0/7 weeks and 36 6/7 weeks gestation are: 75% of preterm births and they: “lag behind in terms of their cardiorespiratory, metabolic, immunologic, neurologic, and motor development” “ 4 times more likely than term infants to be diagnosed with jaundice, respiratory distress, poor feeding, temperature instability, or hypoglycemia during the birth hospitalization” - Breast fed late preterm infants are more likely to be readmitted to hospital than formula fed counterparts due to failure to thrive, jaundice and dehydration (Radtke 2011)
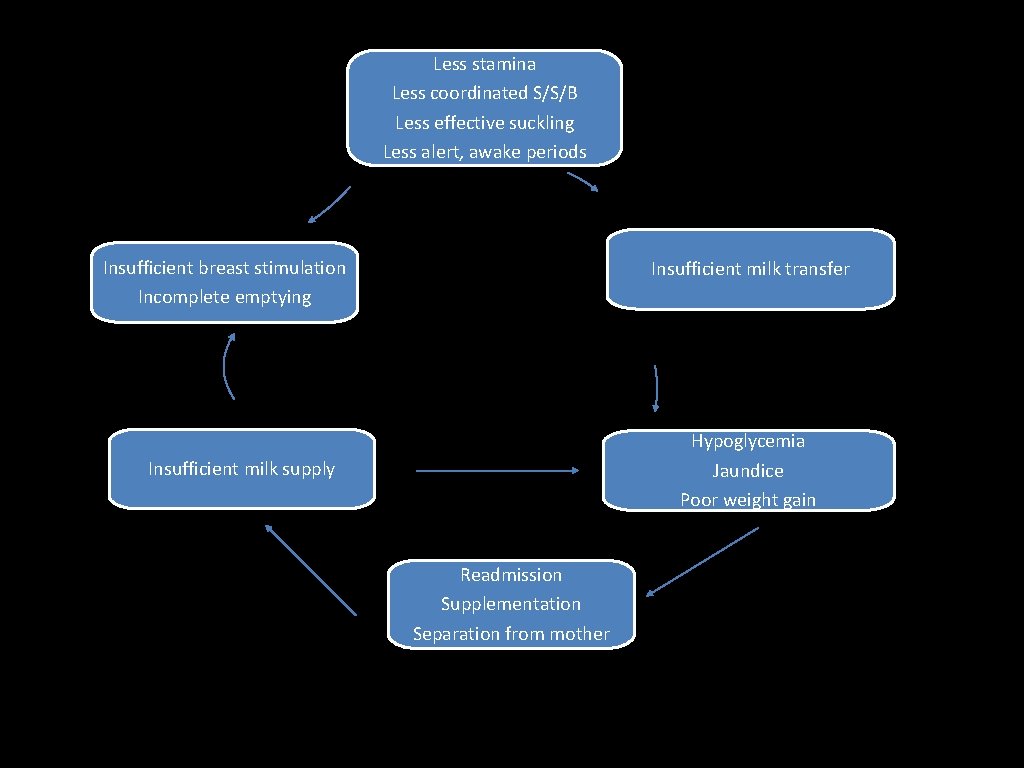
Less stamina Less coordinated S/S/B Less effective suckling Less alert, awake periods Insufficient breast stimulation Incomplete emptying Insufficient milk transfer Hypoglycemia Jaundice Poor weight gain Insufficient milk supply Readmission Supplementation Separation from mother Wight, Pediatric Annals 2003; 3

Breastfeeding the late preterm infant American Academy of Breastfeeding Medicine Guideline Inpatient: • Communicate feeding plan with late preterm order set and modify daily as needed given infant status (weight loss, physiologic stability) • Encourage rooming in and ad lib breast feeding (at least every 23 hours) • Educate parents about waking techniques, ways to facilitate effective latch and hold • Ensure daily formal breast feeding assessment • If supplementation is required: 5 -10 ml/feed on day 1 and 1030 ml/feed day 2 and on. Mother should pump if supplementation is required (Academy of Breastfeeding Medicine, 2011)

Breastfeeding the late preterm infant Role of the Primary Care Provider • Before hospital discharge: - Ensure effective at breast feeding with daily evaluation of feeding quality by hospital lactation services Closely monitor weight and bilirubin Create home breast feeding plan based on weight/weight loss and bilirubin, as well as maternal factors and desires • In Pc. P office - First visit 24 -48 hrs following hospital discharge Continued close monitoring of weight, bilirubin and hydration Identification of lactation support (private Lactation support company, La Leche League, WIC) Modification of home breast feeding plan (Academy of Breastfeeding Medicine, 2011)

Breastfeeding & tongue tie - Congenital condition causing a short, thick lingual frenulum - Effects 1. 7 -4. 7% of newborns, causes feeding difficulties in 44% of these infants - There are potential for both short and long term sequelae of anykyloglossia, including speech difficulties, orthodontic and mandibular abnormalities and psychological problems (Academy of Breastfeeding Medicine)
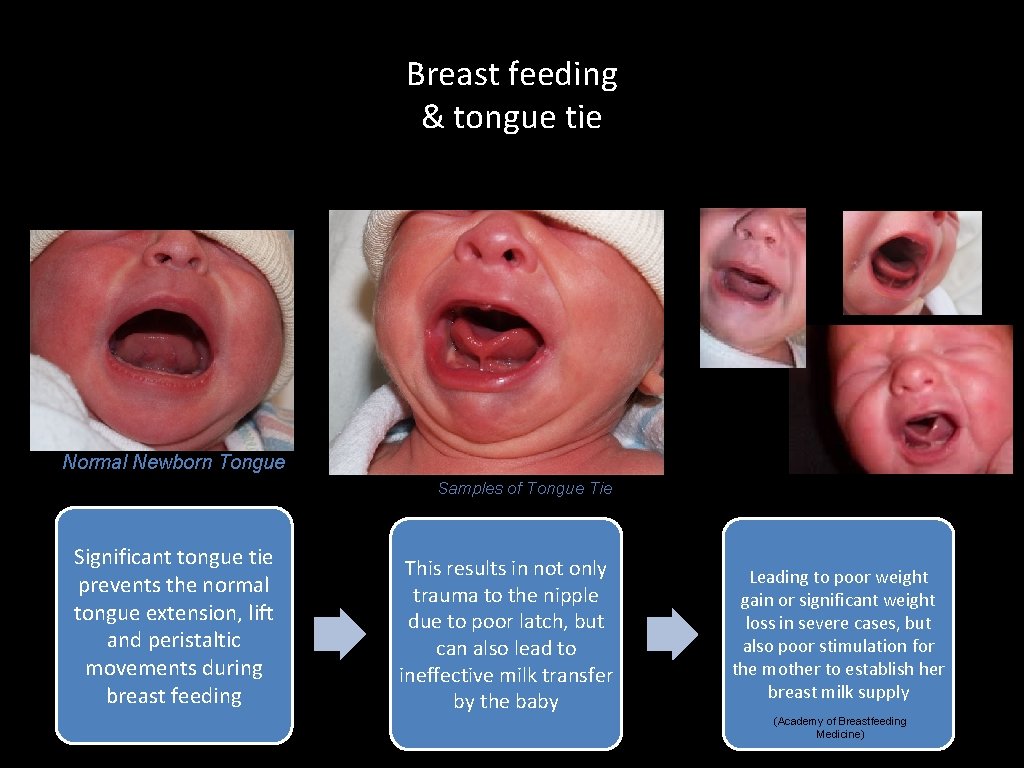
Breast feeding & tongue tie Normal Newborn Tongue Samples of Tongue Tie Significant tongue tie prevents the normal tongue extension, lift and peristaltic movements during breast feeding This results in not only trauma to the nipple due to poor latch, but can also lead to ineffective milk transfer by the baby Leading to poor weight gain or significant weight loss in severe cases, but also poor stimulation for the mother to establish her breast milk supply (Academy of Breastfeeding Medicine)

Breastfeeding & tongue tie • What to do? ? - Frenotomy is the procedure during which the tongue is released by clipping the restrictive lingual frenulum - Though some evidence reports decreased maternal nipple pain and improvements in the infants ability to latch and transfer milk – there are very few randomized controlled trials that report this procedure to be effective treatment although there is a tendency toward performing this procedure to protect breastfeeding. - If concern for tongue tie exists and is thought to be affecting feeding and weight gain, referral to ENT can be made or tongue can be clipped AND a feeding plan can be created to optimize milk transfer and weight gain, this will generally include supplementation and maternal pumping (Academy of Breastfeeding Medicine)

Breast feeding & significant weight loss What defines significant weight loss in newborn • In late preterm infant, weight loss of > 3% in first 24 hrs or >7% by day 3 of life Factors to consider: - Gestational age at birth as well as birth weight Immediate postpartum course – has infant been rooming in and exclusively breast fed? Was first feeding delayed for any reason? Maternal breast feeding history as well as past medical history that could affect breastfeeding (breast surgery, polycystic ovary syndrome, etc. ) Maternal medications (many medications can delay or hinder breastmilk production) Experienced mother vs first time breast feeding mother Delivery modality- vaginal vs c-section

Breast feeding & significant weight loss What to do? ? • Significant weight loss during the newborn period can easily be remedied by providing the infant feeding via supplementary or complementary feeds, but what is the difference… - Supplementary feedings: Feedings provided in place of breastfeeding. - Complementary feedings: Feedings provided in addition to breastfeeding when breastmilk alone is no longer sufficient. What to supplement with? ? - Best to supplement/complement at breast feedings with either expressed breast milk, however in many cases formula is required to bridge the volume gap

Breast feeding & significant weight loss • Appropriate weight gain of a normal healthy newborn is 28 -34 g/day poor weight gain is defined as <20 g/day How to manage significant weight loss… - Establish clear feeding plan, generally this means giving the mother a period of time during the day (4, 6, 8 or 12 hours) during which the infant may exclusively breast feed • during the remaining hours of the day the infant may breast feed but these feedings must be supplemented with formula or expressed breast milk - Identify available lactation support - Mothers are encouraged to pump if the infant is receiving supplemented feeds or has significant weight loss to stimulate an increased supply - Follow up for this group of infants should be done frequently, at least weekly until appropriate weight gain is established. Once infant is gaining weight appropriately the feeding plan can be altered to include more hours of exclusive at breast feeding

Future breastfeeding objectives Healthy People 2020

References • Balancing Pain Management and Prescription Opioid Abuse. (2012). Retrieved January 11, 2016, from http: //www. cdc. gov/primarycare/materials/opoidabuse/index. html • Bio, L. L. , Siu, A. , & Poon, C. Y. (2011). Update on the pharmacologic management of neonatal abstinence syndrome. J Perinatol Journal of Perinatology, 31(11), 692 -701. • Denne, S. C. (2015) Neonatal Nutrition. Pediatr Clin N Am 62 (2015) 427– 438. doi. 1016 j. pcl. 2014. 11. 006 • Dramatic Increases in Maternal Opioid Use and Neonatal Abstinence Syndrome. (2015). Retrieved January 11, 2016, from http: //www. drugabuse. gov/related-topics/trendsstatistics/infographics/dramatic-increases-in-maternal-opioid-use-neonatal-abstinence-syndrome • Dysart, K. , Hsieh, H. , Kaltenbach, K. , & Greenspan, J. S. (2007). Sequela of preterm versus term infants born to mothers on a methadone maintenance program: Differential course of neonatal abstinence syndrome. Journal of Perinatal Medicine, 35(4). • Healthy People 2020 Objectives. http: //www. cdc. gov/breastfeeding/policy/hp 2010. htm • Hudak, M. L. , & Tan, R. C. (2012). Neonatal Drug Withdrawal. Pediatrics, 129(2). • NAS Flowsheet. (2014, July. ) Retrieved January 11, 2016 from https: //connect. urmc. rochester. edu/ CSCOE /portal. htm • Newborn drug-related (2014, December. ). Retrieved January 11, 2016, from https: //www. health. ny. gov/statistics/chac/hospital/h 46. htm • Patrick, S. , Schumacher, R. , Benneyworth, B. , Krans, E. , Mcallister, J. , & Davis, M. (2013). Neonatal Abstinence Syndrome and Associated Health Care Expenditures. Obstetric Anesthesia Digest, 33(2), 86. • Radtke, J. V. (2011). The Paradox of Breastfeeding – Associated Morbidity Among Late Preterm Infants. Journal of Gynocyologic and Neonatal Nursing, 40, 9 -24. • Roussos-Ross, K. , Reisfield, G. , Elliot, I. , Dalton, S. , & Gold, M. (2015). Opioid Use in Pregnant Women and the Increase in Neonatal Abstinence Syndrome. Journal of Addiction Medicine, 9(3), 222225. • The Academy of Breastfeeding Medicine. ABM Clinical Protocol #11: Guidelines for the evaluation and management of neonatal ankyloglossia and its complications in the breastfeeding dyad. Breastfeeding Medicine • The Academy of Breastfeeding Medicine (2009). ABM Clinical Protocol #3. Hospital Guidelines for the Use of Supplementary Feedings in the Healthy Term Breastfed Neonate, Revised 2009. Breastfeeding Medicine, 4 (3) 175 -182 • The Academy of Breastfeeding Medicine (2011). ABM Clinical Protocol #10: Breastfeeding the Late Preterm Infant (34 0/7 to 36 6/7 Weeks Gestation). Breastfeeding Medicine, 6 (3) 151 -156 • Today’s Heroin Epidemic. (2015). Retrieved January 11, 2016, from http: //www. cdc. gov/vitalsigns/heroin/ • Tolia, V. N. , Patrick, S. W. , Bennett, M. M. , Murthy, K. , Sousa, J. , Smith, P. B. (2015). Increasing Incidence of the Neonatal Abstinence Syndrome in U. S. Neonatal ICUs. New England Journal of Medicine N Engl J Med, 372(22), 2118 -2126. • Wight, NE (2003). Breastfeeding the borderline (near-term) preterm infant. Pediatric Annals, 32 (5): 329 -336
- Slides: 53