Host defense mechanism Dr Enas Razzoqi B D


Host defense mechanism Dr. Enas Razzoqi B. D. S. , M. Sc. , Ph. D in Periodontics

It is recognized that host responses play a role in most forms of P. d. disease. In gingivitis, periodontitis, the development of the disease depends on the interaction between the resident microbiota and host response. In other types of P. d. disease. , such as desquamative gingivitis, the lesions frequently result from a host response.

Clinically healthy gingiva appears to deal with microbial challenges without progressing to a diseased state, probably because of several defensive factors which include: 1. Regular shedding of epithelial cells into the oral cavity 2. Intact epithelial barrier 3. Positive fluid flow of the gingival crevice which may remove non-attached microorganisms and noxious products 4. Antimicrobial effect of antibodies 5. Phagocytic function of neutrophils and macrophages 6. Detrimental effect of complement on the microbiota
Inflammatory cells, molecules and processes: -
Mast cells: Contain cytoplasmic granules that contain: • Histamine. • Heparin. • Bradykinin. Vasodilatation. Increased vascular permeability. Bone resorption. mast cell interleukin has been shown to enhance collagenase activity

Neutrophils: polymorphonuclear leukocytes Attracted by chemotactic factors to areas of inflammation particularly in the more acute lesions, 1. IL-8 chemotactic for neutrophils and increases their adherence to endothelial cells 2. interferon-γ (IFN- γ). 3. complement factors (C 5 a). Chemotaxis is the directed movement of a cell along a chemical gradient, as a response to chemical signals (chemotaxins) from multiple sources, after attraction of the cells to the area they phagocytose bacteria and remove damaged tissue

then engulf (phagocytosis) and subsequently kill and digest most microorganisms and neutralize other noxious substances. Opsonization: Is referred to the process of coating a particle with recognizable molecules to enable phagocytic ingestion Neutrophils Protective Destruction Lysozomal collagenase enzymes elastase • leukocytes abnormalities, including chemotactic defects, deficiencies in adhesion and lack of specific granules, can lead to more severe P. d. disease.

Macrophages: - Mononuclear cells Macrophages develop from blood monocytes attracted to sites of inflammation Phagocytose and kill bacteria. • The efficiency of bacterial phagocytosis by the macrophages is enhanced by the reaction of the antibody with the antigen and subsequent complement activation. Remove damaged host tissue during inflammation. Antigen-presenting cell macrophages B cells. dendritic cells Langerhans cells

In response to stimulation by bacterial endotoxin, immune complexes, or lymphokines. They secrete interleukin-I (IL-I), IL-6, IL-8, IL-10, tumor necrosis factor -α(TNF- α). • They produce prostaglandins and collagenase
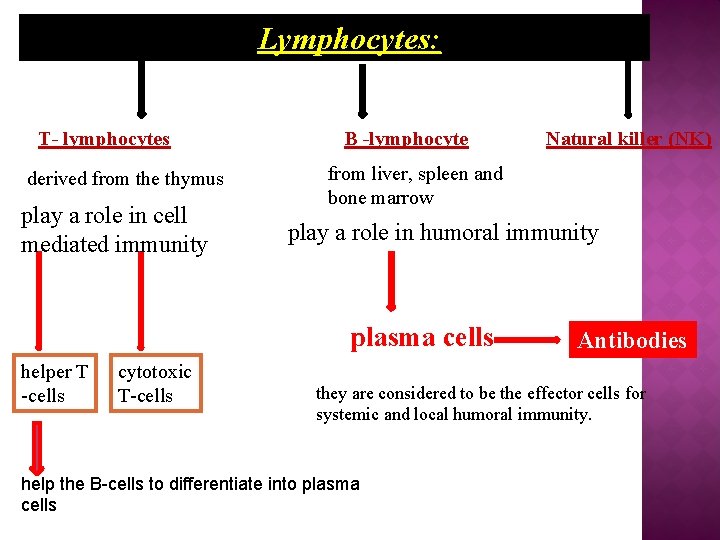
Lymphocytes: T- lymphocytes derived from the thymus play a role in cell mediated immunity B -lymphocyte from liver, spleen and bone marrow play a role in humoral immunity plasma cells helper T -cells cytotoxic T-cells Natural killer (NK) Antibodies they are considered to be the effector cells for systemic and local humoral immunity. help the B-cells to differentiate into plasma cells
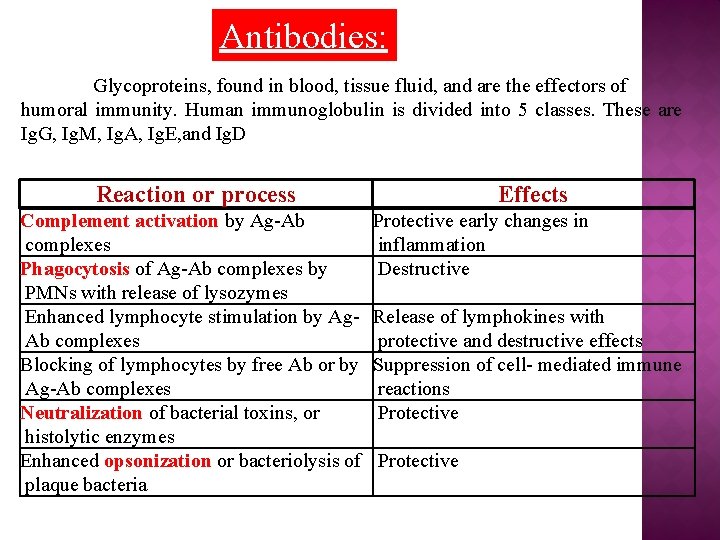
Antibodies: Glycoproteins, found in blood, tissue fluid, and are the effectors of humoral immunity. Human immunoglobulin is divided into 5 classes. These are Ig. G, Ig. M, Ig. A, Ig. E, and Ig. D Reaction or process Complement activation by Ag-Ab complexes Phagocytosis of Ag-Ab complexes by PMNs with release of lysozymes Enhanced lymphocyte stimulation by Ag. Ab complexes Blocking of lymphocytes by free Ab or by Ag-Ab complexes Neutralization of bacterial toxins, or histolytic enzymes Enhanced opsonization or bacteriolysis of plaque bacteria Effects Protective early changes in inflammation Destructive Release of lymphokines with protective and destructive effects Suppression of cell- mediated immune reactions Protective

Serum complement system: The serum complement system is composed of more than 20 serum proteins, that when activated, have potent biological activity. The system is important in both inflammation and immunity. • the classical pathway, follows binding of Ab to bacterial cell wall surfaces. • The alternate pathway, can be activated directly by constituents of cell walls of certain G-ve bacteria (e. g. endotoxins).

Biologic effects of complement: Activity Cytolytic and cytotoxic damage to cells Chemotactic activity for leukocytes Histamine release from mast cells Increased vascular permeability Lysosomal enzyme release from leukocytes Promotion of phagocytosis Enhancement of blood clotting Promotion of clot lysis Inactivation of bacterial lipopolysaccharide
- Slides: 14