Hospitals Cant Live With Them Cant Live Without























- Slides: 26

Hospitals: Can’t Live With Them Can’t Live Without Them Georgia Medical Group Management Association Hilton Head, SC May 2, 2016 1

Objectives • Identify and analyze medical practice alliance models. • Learn how recently trained physicians will impact the practice. • Understand where health care may be “headed”. 2

Things I believe to be true • All health care is local • Things typically get worse before they get better (at least it feels that way) • Darwin’s theory • Nothing lasts forever 3

New Alliances – Why? • We’re broke! • Cost • Quality • Access • A New Deal • FFS to P 4 P • Transparency 4

New Expectations 5

Transparency • www. healthgrades. com • www. rate. MDs. com • www. vitals. com • www. drscore. com • www. Physician. Reports. com • www. consumerhealthratings. com • www. doctorpricing. com • www. medicare. gov/physiciancompare/ • www. zocdoc. com • www. angieslist. com 6

Changing Payment Models QUALITY/COST LOW COST AVERAGE COST HIGH QUALITY $$ $ MFS AVG QUALITY $ MFS -$ LOW QUALITY MFS -$ -$$ Medicare Value-Based Payment Modifier Coming to a physician near you soon. 7

Some Alliance Models • Ownership – Physician (single or multi-specialty) – Hospital – Faculty Practice Plan – Insurance company – PPM (Team. Health, Em. Care, etc. ) – Conglomerate (Mc. Kesson) – Private equity firm – Wal. Mart, Walgreens, CVS 8

Some Alliance Models • Affiliation – MSO – JV – Co-management agreement – Clinically Integrated Network – ACO – BPCI – CJR – IPA 9

So Many Choices! What’s a Doctor to Do? • Assessment factors – Local environment – Physician age, years to retirement, readiness – Partnership objectives – Risk assessment • Don’t wait until you have limited choices • Don’t try to hammer a square peg in a round hole 10

Hospital Employment? 11

The Cost/Payoff for Integration HIGH O V E R H E A D LOW HIGH AUTONOMY LOW 12

Medical Practice Alliances • “Change before you have to. If the environment changes faster than you do, you will be out of business” Jack Welch • “The best way to manage change is to lead it” Peter Drucker, Ph. D • “If you don’t like change, you are going to like irrelevance even less” General Eric Shinseki 13

Training physicians • 1700’s – 1910 – Apprenticeship – No organized education or standards – Wide variation of practice, expertise, and outcomes • 1910 – 1999 – Flexner Report (1910) – Birth of the organized medical staff (American Surgical Society Minimum Standards for Hospitals – 1919) 14

Training physicians • 1910 – 1999 (continued) – “Cottage industry” with individual proprietors – Wide variation of practice, expertise, and outcomes • 1999 • Institute of Medicine – To Err is Human • Wide variation of practice, expertise, and outcomes • 2013 – ACGME Next Accreditation System 15

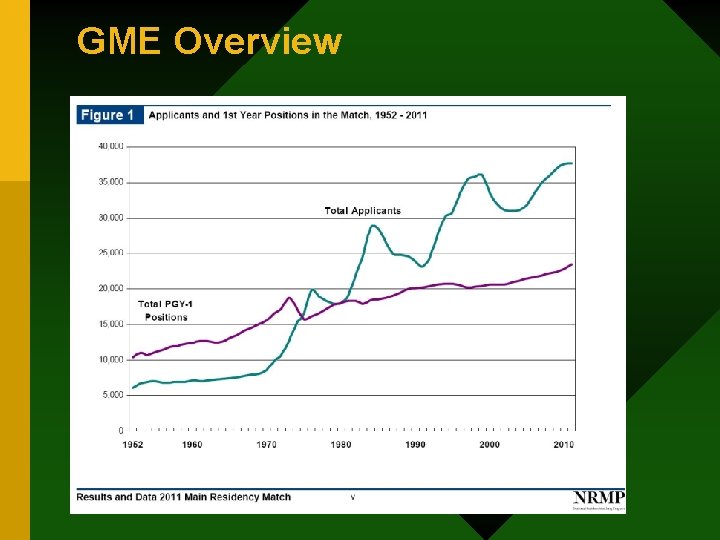
GME Overview

What’s Different? • EBP – rate of medical knowledge • Work-life expectations • Computer literate • Team approach – MLPs • Interpersonal skills 17

How will recently trained physicians impact the practice? 18

Where is health care headed? 19

High Deductible Health Plans 20

High Deductible Health Plans • ~$6, 000 to $12, 000 • Shared decision making • Pricing transparency • Insurance websites 21

Narrow Networks • Access points – Open access • PCMH • ICD-10 • CAHPS 22

What Do I Do? • Know what plans you are in and OUT • Assess your capacity to add new patients • Each visit check eligibility, coinsurance/copays, and deductibles • Script staff to discuss out of pocket expenses and overall cost of care • Utilize PATOS, prompt pay discounts, and payment plans 23

“The greatest danger in times of turbulence is not the turbulence; it is to act with yesterday’s logic. ” Peter Drucker, Ph. D 24

Questions? 25

Mickey Smith, FACMPE, FACHE, FHFMA CEO Oak Hill Hospital 11375 Cortez Blvd Brooksville, FL 34613 352 -597 -3099 352 -597 -3024 fax mickey. smith@oakhillhospital. com “I’ve never seen a successful hospital that wasn’t surrounded by successful physicians” 26